CHLOROTHIAZIDE SODIUM injection, powder, lyophilized, for solution
chlorothiazide sodium by
Drug Labeling and Warnings
chlorothiazide sodium by is a Prescription medication manufactured, distributed, or labeled by Sagent Pharmaceuticals. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
- SPL UNCLASSIFIED SECTION
-
DESCRIPTION
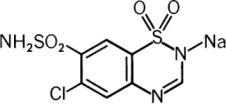
Chlorothiazide Sodium for Injection, USP is a diuretic and antihypertensive. It is 6-chloro-2H-1,2,4-benzothiadiazine-7-sulfonamide 1,1-dioxide monosodium salt and its molecular weight is 317.71. Its empirical formula is C7H5ClN3NaO4S2 and its structural formula is:
Chlorothiazide Sodium for Injection, USP is a sterile lyophilized white powder and is supplied in a vial containing: Chlorothiazide sodium equivalent to chlorothiazide 500 mg, and the inactive ingredient mannitol 250 mg with sodium hydroxide to adjust pH.
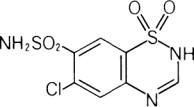
Chlorothiazide is a diuretic and antihypertensive. It is 6-chloro-2H-1,2,4-benzothiadiazine-7-sulfonamide 1,1-dioxide. Its empirical formula is C7H6ClN3O4S2 and its structural formula is:
It is a white, or practically white, crystalline powder with a molecular weight of 295.72, which is very slightly soluble in water, but readily soluble in dilute aqueous sodium hydroxide. It is soluble in urine to the extent of about 150 mg per 100 mL at pH 7.
-
CLINICAL PHARMACOLOGY
The mechanism of the antihypertensive effect of thiazides is unknown. Chlorothiazide does not usually affect normal blood pressure.
Chlorothiazide affects the distal renal tubular mechanism of electrolyte reabsorption. At maximal therapeutic dosage all thiazides are approximately equal in their diuretic efficacy.
Chlorothiazide increases excretion of sodium and chloride in approximately equivalent amounts. Natriuresis may be accompanied by some loss of potassium and bicarbonate.
After oral use diuresis begins within 2 hours, peaks in about 4 hours and lasts about 6 to 12 hours. Following intravenous use of chlorothiazide sodium, onset of the diuretic action occurs in 15 minutes and the maximal action in 30 minutes.
Pharmacokinetics and Metabolism
Chlorothiazide is not metabolized but is eliminated rapidly by the kidney; 96 percent of an intravenous dose is excreted unchanged in the urine within 23 hours. The plasma half-life of chlorothiazide is 45 to 120 minutes. Chlorothiazide crosses the placental but not the blood-brain barrier and is excreted in breast milk.
-
INDICATIONS AND USAGE
Chlorothiazide Sodium for Injection, USP is indicated as adjunctive therapy in edema associated with congestive heart failure, hepatic cirrhosis, and corticosteroid and estrogen therapy.
Chlorothiazide Sodium for Injection, USP has also been found useful in edema due to various forms of renal dysfunction such as nephrotic syndrome, acute glomerulonephritis, and chronic renal failure.
Use in Pregnancy
Routine use of diuretics during normal pregnancy is inappropriate and exposes mother and fetus to unnecessary hazard. Diuretics do not prevent development of toxemia of pregnancy and there is no satisfactory evidence that they are useful in the treatment of toxemia.
Edema during pregnancy may arise from pathologic causes or from the physiologic and mechanical consequences of pregnancy. Thiazides are indicated in pregnancy when edema is due to pathologic causes, just as they are in the absence of pregnancy (see PRECAUTIONS, Pregnancy). Dependent edema in pregnancy, resulting from restriction of venous return by the gravid uterus, is properly treated through elevation of the lower extremities and use of support stockings. Use of diuretics to lower intravascular volume in this instance is illogical and unnecessary. During normal pregnancy there is hypervolemia which is not harmful to the fetus or the mother in the absence of cardiovascular disease. However, it may be associated with edema, rarely generalized edema. If such edema causes discomfort, increased recumbency will often provide relief. Rarely this edema may cause extreme discomfort which is not relieved by rest. In these instances, a short course of diuretic therapy may provide relief and be appropriate.
- CONTRAINDICATIONS
-
WARNINGS
Intravenous use in infants and children has been limited and is not generally recommended.
Use with caution in severe renal disease. In patients with renal disease, thiazides may precipitate azotemia. Cumulative effects of the drug may develop in patients with impaired renal function.
Thiazides should be used with caution in patients with impaired hepatic function or progressive liver disease, since minor alterations of fluid and electrolyte balance may precipitate hepatic coma.
Thiazides may add to or potentiate the action of other antihypertensive drugs.
Sensitivity reactions may occur in patients with or without a history of allergy or bronchial asthma.
The possibility of exacerbation or activation of systemic lupus erythematosus has been reported.
Lithium generally should not be given with diuretics (see PRECAUTIONS, Drug Interactions).
-
PRECAUTIONS
General
All patients receiving diuretic therapy should be observed for evidence of fluid or electrolyte imbalance: namely, hyponatremia, hypochloremic alkalosis, and hypokalemia. Serum and urine electrolyte determinations are particularly important when the patient is vomiting excessively or receiving parenteral fluids. Warning signs or symptoms of fluid and electrolyte imbalance, irrespective of cause, include dryness of mouth, thirst, weakness, lethargy, drowsiness, restlessness, confusion, seizures, muscle pains or cramps, muscular fatigue, hypotension, oliguria, tachycardia, and gastrointestinal disturbances such as nausea and vomiting.
Hypokalemia may develop especially with brisk diuresis, when severe cirrhosis is present or after prolonged therapy.
Interference with adequate oral electrolyte intake will also contribute to hypokalemia. Hypokalemia may cause cardiac arrhythmias and may also sensitize or exaggerate the response of the heart to the toxic effects of digitalis (e.g., increased ventricular irritability). Hypokalemia may be avoided or treated by use of potassium-sparing diuretics or potassium supplements such as foods with a high potassium content.
Although any chloride deficit is generally mild and usually does not require specific treatment except under extraordinary circumstances (as in liver disease or renal disease), chloride replacement may be required in the treatment of metabolic alkalosis.
Dilutional hyponatremia may occur in edematous patients in hot weather; appropriate therapy is water restriction, rather than administration of salt, except in rare instances when the hyponatremia is life-threatening. In actual salt depletion, appropriate replacement is the therapy of choice.
Hyperuricemia may occur or acute gout may be precipitated in certain patients receiving thiazides.
In diabetic patients dosage adjustments of insulin or oral hypoglycemic agents may be required. Hyperglycemia may occur with thiazide diuretics. Thus latent diabetes mellitus may become manifest during thiazide therapy.
The antihypertensive effects of the drug may be enhanced in the postsympathectomy patient.
If progressive renal impairment becomes evident, consider withholding or discontinuing diuretic therapy.
Thiazides have been shown to increase the urinary excretion of magnesium; this may result in hypomagnesemia.
Thiazides may decrease urinary calcium excretion. Thiazides may cause intermittent and slight elevation of serum calcium in the absence of known disorders of calcium metabolism. Marked hypercalcemia may be evidence of hidden hyperparathyroidism. Thiazides should be discontinued before carrying out tests for parathyroid function.
Increases in cholesterol and triglyceride levels may be associated with thiazide diuretic therapy.
Laboratory Tests
Periodic determination of serum electrolytes to detect possible electrolyte imbalance should be done at appropriate intervals.
Drug Interactions
When given concurrently the following drugs may interact with thiazide diuretics.
Alcohol, barbiturates, or narcotics - potentiation of orthostatic hypotension may occur.
Antidiabetic drugs - (oral agents and insulin) - dosage adjustment of the antidiabetic drug may be required.
Other antihypertensive drugs - additive effect or potentiation.
Corticosteroids, ACTH - intensified electrolyte depletion, particularly hypokalemia.
Pressor amines (e.g., norepinephrine) - possible decreased response to pressor amines but not sufficient to preclude their use.
Skeletal muscle relaxants, nondepolarizing (e.g., tubocurarine) - possible increased responsiveness to the muscle relaxant.
Lithium - generally should not be given with diuretics. Diuretic agents reduce the renal clearance of lithium and add a high risk of lithium toxicity. Refer to the package insert for lithium preparations before use of such preparations with chlorothiazide sodium.
Non-steroidal Anti-inflammatory Drugs - In some patients, the administration of a non-steroidal anti-inflammatory agent can reduce the diuretic, natriuretic, and antihypertensive effects of loop, potassium-sparing and thiazide diuretics. Therefore, when chlorothiazide sodium and non-steroidal anti-inflammatory agents are used concomitantly, the patient should be observed closely to determine if the desired effect of the diuretic is obtained.
Drug/Laboratory Test Interactions
Thiazides should be discontinued before carrying out tests for parathyroid function (see PRECAUTIONS, General).
Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenicity studies have not been conducted with chlorothiazide.
Chlorothiazide was not mutagenic in vitro in the Ames microbial mutagen test (using a maximum concentration of 5 mg/plate and Salmonella typhimurium strains TA98 and TA100) and was not mutagenic and did not induce mitotic nondisjunction in diploid-strains of Aspergillus nidulans.
Chlorothiazide had no adverse effects on fertility in female rats at doses up to 60 mg/kg/day and no adverse effects on fertility in male rats at doses up to 40 mg/kg/day. These doses are 1.5 and 1.0 times** the recommended maximum human dose, respectively, when compared on a body weight basis.
Pregnancy
Teratogenic Effects - Pregnancy Category C: Although reproduction studies performed with chlorothiazide doses of 50 mg/kg/day in rabbits, 60 mg/kg/day in rats and 500 mg/kg/day in mice revealed no external abnormalities of the fetus or impairment of growth and survival of the fetus due to chlorothiazide, such studies did not include complete examinations for visceral and skeletal abnormalities. It is not known whether chlorothiazide can cause fetal harm when administered to a pregnant woman; however, thiazides cross the placental barrier and appear in cord blood. Chlorothiazide should be used during pregnancy only if clearly needed (see INDICATIONS AND USAGE).
Nursing Mothers
Because of the potential for serious adverse reactions in nursing infants from chlorothiazide sodium for injection, a decision should be made whether to discontinue nursing or to discontinue the drug, taking into account the importance of the drug to the mother.
Pediatric Use
Safety and effectiveness of chlorothiazide sodium for injection in pediatric patients have not been established.
Geriatric Use
Clinical studies of chlorothiazide sodium for injection did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy.
This drug is known to be substantially excreted by the kidney, and the risk of toxic reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and it may be useful to monitor renal function (see WARNINGS).
-
ADVERSE REACTIONS
The following adverse reactions have been reported and, within each category, are listed in order of decreasing severity.
Body as a Whole: Weakness.
Cardiovascular: Hypotension including orthostatic hypotension (may be aggravated by alcohol, barbiturates, narcotics or antihypertensive drugs).
Digestive: Pancreatitis, jaundice (intrahepatic cholestatic jaundice), diarrhea, vomiting, sialadenitis, cramping, constipation, gastric irritation, nausea, anorexia.
Hematologic: Aplastic anemia, agranulocytosis, leukopenia, hemolytic anemia, thrombocytopenia.
Hypersensitivity: Anaphylactic reactions, necrotizing angiitis (vasculitis and cutaneous vasculitis), respiratory distress including pneumonitis and pulmonary edema, photosensitivity, fever, urticaria, rash, purpura.
Metabolic: Electrolyte imbalance (see PRECAUTIONS), hyperglycemia, glycosuria, hyperuricemia.
Musculoskeletal: Muscle spasm.
Nervous System/Psychiatric: Vertigo, paresthesias, dizziness, headache, restlessness.
Skin: Erythema multiforme including Stevens-Johnson syndrome, exfoliative dermatitis including toxic epidermal necrolysis, alopecia.
Special Senses: Transient blurred vision, xanthopsia.
Renal: Renal failure, renal dysfunction, interstitial nephritis, (see WARNINGS); hematuria (following intravenous use).
Urogenital: Impotence.
Whenever adverse reactions are moderate or severe, thiazide dosage should be reduced or therapy withdrawn.
To report SUSPECTED ADVERSE REACTIONS, contact Sagent Pharmaceuticals, Inc. at 1-866-625-1618 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
-
OVERDOSAGE
The most common signs and symptoms observed are those caused by electrolyte depletion (hypokalemia, hypochloremia, hyponatremia) and dehydration resulting from excessive diuresis. If digitalis has also been administered, hypokalemia may accentuate cardiac arrhythmias.
In the event of overdosage, symptomatic and supportive measures should be employed. Correct dehydration, electrolyte imbalance, hepatic coma and hypotension by established procedures. If required, give oxygen or artificial respiration for respiratory impairment.
The degree to which chlorothiazide sodium is removed by hemodialysis has not been established.
The intravenous LD50 of chlorothiazide in the mouse is 1.1 g/kg.
-
DOSAGE AND ADMINISTRATION
Chlorothiazide Sodium for Injection, USP should be reserved for patients unable to take oral medication or for emergency situations.
Therapy should be individualized according to patient response. Use the smallest dosage necessary to achieve the required response.
Intravenous use in infants and children has been limited and is not generally recommended.
When medication can be taken orally, therapy with chlorothiazide tablets or oral suspension may be substituted for intravenous therapy, using the same dosage schedule as for the parenteral route.
Chlorothiazide Sodium for Injection, USP may be given slowly by direct intravenous injection or by intravenous infusion.
Extravasation must be rigidly avoided. Do not give subcutaneously or intramuscularly.
The usual adult dosage is 500 mg to 1 g once or twice a day. Many patients with edema respond to intermittent therapy, i.e., administration on alternate days or on three to five days each week. With an intermittent schedule, excessive response and the resulting undesirable electrolyte imbalance are less likely to occur.
Directions for Reconstitution
Use aseptic technique. Because Chlorothiazide Sodium for Injection, USP contains no preservative, a fresh solution should be prepared immediately prior to each administration, and the unused portion should be discarded.
Add 18 mL of Sterile Water for Injection to the vial to form an isotonic solution for intravenous injection. Never add less than 18 mL. When reconstituted with 18 mL of Sterile Water, the final concentration of Chlorothiazide Sodium for Injection, USP is 28 mg per mL. The reconstituted solution is clear and essentially free from visible particles. Parenteral drug products should be inspected visually for particulate matter and discoloration prior to use whenever solution and container permit. The solution is compatible with dextrose or sodium chloride solutions for intravenous infusion. Avoid simultaneous administration of solutions of chlorothiazide with whole blood or its derivatives.
-
HOW SUPPLIED
Chlorothiazide Sodium for Injection, USP is supplied as follows:
NDC Chlorothiazide Sodium for Injection, USP Package Factor 25021-305-20 500 mg Single-Dose Vial 1 vial per carton Chlorothiazide Sodium for Injection, USP is a dry, sterile lyophilized white powder usually in cake form, supplied in vials containing chlorothiazide sodium equivalent to 500 mg of chlorothiazide.
Storage Conditions
Store at 20° to 25°C (68° to 77°F). [See USP Controlled Room Temperature.]
For single dose only. Use solution immediately after reconstitution (see DOSAGE AND ADMINISTRATION, Directions for Reconstitution). Discard unused portion of the reconstituted solution.
Sterile, Nonpyrogenic, Preservative-free.
The container closure is not made with natural rubber latex.
** Calculations based on a human body weight of 50 kg.
SAGENT™
Mfd. for SAGENT Pharmaceuticals
Schaumburg, IL 60195 (USA)
Made in India
©2014 Sagent Pharmaceuticals, Inc.July 2014
-
PRINCIPAL DISPLAY PANEL
PACKAGE LABEL – PRINCIPAL DISPLAY PANEL – Vial Label
NDC: 25021-305-20
Rx only
Chlorothiazide Sodium for Injection, USP
500 mg per vial
FOR THE PREPARATION OF INTRAVENOUS SOLUTIONS
For Intravenous Use
Single-Dose Vial
-
INGREDIENTS AND APPEARANCE
CHLOROTHIAZIDE SODIUM
chlorothiazide sodium injection, powder, lyophilized, for solutionProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 25021-305 Route of Administration INTRAVENOUS Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength chlorothiazide sodium (UNII: SN86FG7N2K) (chlorothiazide - UNII:77W477J15H) chlorothiazide 500 mg in 18 mL Inactive Ingredients Ingredient Name Strength mannitol (UNII: 3OWL53L36A) sodium hydroxide (UNII: 55X04QC32I) Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 25021-305-20 1 in 1 CARTON 10/12/2015 1 18 mL in 1 VIAL; Type 0: Not a Combination Product Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA202462 10/12/2015 Labeler - Sagent Pharmaceuticals (796852890)
© 2026 FDA.report
This site is not affiliated with or endorsed by the FDA.