SUMATRIPTAN SUCCINATE injection
Sumatriptan Succinate by
Drug Labeling and Warnings
Sumatriptan Succinate by is a Prescription medication manufactured, distributed, or labeled by Fresenius Kabi USA, LLC , Fresenius Kabi USA, LLC. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
-
HIGHLIGHTS OF PRESCRIBING INFORMATION
These highlights do not include all the information needed to use SUMATRIPTAN SUCCINATE INJECTION safely and effectively. See full prescribing information for SUMATRIPTAN SUCCINATE INJECTION.
SUMATRIPTAN SUCCINATE INJECTION, for subcutaneous use
Initial U.S. Approval: 1992
INDICATIONS AND USAGE
DOSAGE AND ADMINISTRATION
- For subcutaneous use only. ( 2.1)
- Acute treatment of migraine: 1 to 6 mg Single dose. ( 2.1)
- Acute treatment of cluster headache: 6 mg Single dose. ( 2.1)
- Maximum dose in a 24-hour period: 12 mg, Separate doses by at least 1 hour. ( 2.1)
- Patients receiving doses other than 6 mg: Use the 6 mg single-dose vial. ( 2.2)
DOSAGE FORMS AND STRENGTHS
- Injection: 6 mg single-dose vial. ( 3)
CONTRAINDICATIONS
- Coronary artery disease or coronary vasospasm ( 4)
- Wolff-Parkinson-White syndrome or other cardiac accessory conduction pathway disorders ( 4)
- History of stroke, transient ischemic attack, or hemiplegic or basilar migraine ( 4)
- Peripheral vascular disease ( 4)
- Ischemic bowel disease ( 4)
- Uncontrolled hypertension ( 4)
- Recent (within 24 hours) use of another 5-HT 1 agonist (e.g., another triptan) or of an ergotamine-containing medication ( 4)
- Current or recent (past 2 weeks) use of monoamine oxidase-A inhibitor ( 4)
- Known hypersensitivity to sumatriptan ( 4)
- Severe hepatic impairment ( 4)
WARNINGS AND PRECAUTIONS
- Myocardial ischemia/infarction and Prinzmetal’s angina: Perform cardiac evaluation in patients with multiple cardiovascular risk factors. ( 5.1)
- Arrhythmias: Discontinue sumatriptan succinate if occurs. ( 5.2)
- Chest/throat/neck/jaw pain, tightness, pressure, or heaviness: Generally not associated with myocardial ischemia; evaluate for coronary artery disease in patients at high risk. ( 5.3)
- Cerebral hemorrhage, subarachnoid hemorrhage, and stroke: Discontinue sumatriptan succinate if occurs. ( 5.4)
- Gastrointestinal ischemia and infarction events, peripheral vasospastic reactions: Discontinue sumatriptan succinate if occurs. ( 5.5)
- Medication overuse headache: Detoxification may be necessary. ( 5.6)
- Serotonin syndrome: Discontinue sumatriptan succinate if occurs. ( 5.7)
- Increase in blood pressure: Monitor blood pressure. ( 5.8)
- Anaphylactic/anaphylactoid reactions: Discontinue sumatriptan succinate if occurs. ( 5.9)
- Seizures: Use with caution in patients with epilepsy or a lowered seizure threshold. ( 5.10)
ADVERSE REACTIONS
Most common adverse reactions (≥ 5% and > placebo) were injection site reactions, tingling, dizziness/vertigo, warm/hot sensation, burning sensation, feeling of heaviness, pressure sensation, flushing, feeling of tightness, and numbness. ( 6.1)
To report SUSPECTED ADVERSE REACTIONS, contact Fresenius Kabi USA, LLC, Vigilance & Medical Affairs at 1-800-551-7176 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
USE IN SPECIFIC POPULATIONS
See 17 for PATIENT COUNSELING INFORMATION and FDA-approved patient labeling.
Revised: 4/2015
-
Table of Contents
FULL PRESCRIBING INFORMATION: CONTENTS*
1 INDICATIONS AND USAGE
2 DOSAGE AND ADMINISTRATION
2.1 Dosing Information
2.2 Administration of Doses of Sumatriptan Succinate Injection Other than 6 mg
3 DOSAGE FORMS AND STRENGTHS
4 CONTRAINDICATIONS
5 WARNINGS AND PRECAUTIONS
5.1 Myocardial Ischemia, Myocardial Infarction, and Prinzmetal's Angina
5.2 Arrhythmias
5.3 Chest, Throat, Neck, and/or Jaw Pain/Tightness/Pressure
5.4 Cerebrovascular Events
5.5 Other Vasospasm Reactions
5.6 Medication Overuse Headache
5.7 Serotonin Syndrome
5.8 Increase in Blood Pressure
5.9 Anaphylactic/Anaphylactoid Reactions
5.10 Seizures
6 ADVERSE REACTIONS
6.1 Clinical Trials Experience
6.2 Postmarketing Experience
7 DRUG INTERACTIONS
7.1 Ergot-Containing Drugs
7.2 Monoamine Oxidase-A Inhibitors
7.3 Other 5-HT1 Agonists
7.4 Selective Serotonin Reuptake Inhibitors/Serotonin Norepinephrine Reuptake Inhibitors and Serotonin Syndrome
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
8.3 Nursing Mothers
8.4 Pediatric Use
8.5 Geriatric Use
10 OVERDOSAGE
11 DESCRIPTION
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
12.2 Pharmacodynamics
12.3 Pharmacokinetics
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
13.2 Animal Toxicology and/or Pharmacology
14 CLINICAL STUDIES
14.1 Migraine
14.2 Cluster Headache
16 HOW SUPPLIED/STORAGE AND HANDLING
17 PATIENT COUNSELING INFORMATION
- * Sections or subsections omitted from the full prescribing information are not listed.
-
1 INDICATIONS AND USAGE
Sumatriptan succinate injection is indicated in adults for (1) the acute treatment of migraine, with or without aura, and (2) the acute treatment of cluster headache.
Limitations of Use:
- Use only if a clear diagnosis of migraine or cluster headache has been established.
- If a patient has no response to the first migraine attack treated with sumatriptan succinate injection, reconsider the diagnosis of migraine before sumatriptan succinate injection is administered to treat any subsequent attacks.
- Sumatriptan succinate injection is not indicated for the prevention of migraine attacks.
-
2 DOSAGE AND ADMINISTRATION
2.1 Dosing Information
The maximum single recommended adult dose of sumatriptan succinate injection for the acute treatment of migraine or cluster headache is 6 mg injected subcutaneously. For the treatment of migraine, if side effects are dose limiting, lower doses (1 to 5 mg) may be used [see Clinical Studies ( 14.1)] . For the treatment of cluster headache, the efficacy of lower doses has not been established.
The maximum cumulative dose that may be given in 24 hours is 12 mg, two 6 mg injections separated by at least 1 hour. A second 6 mg dose should only be considered if some response to a first injection was observed.2.2 Administration of Doses of Sumatriptan Succinate Injection Other than 6 mg
In patients receiving doses other than 6 mg, use the 6 mg single-dose vial. Visually inspect the vial for particulate matter and discoloration before administration. Do not use if particulates and discolorations are noted.
- 3 DOSAGE FORMS AND STRENGTHS
-
4 CONTRAINDICATIONS
Sumatriptan succinate injection is contraindicated in patients with:
- Ischemic coronary artery disease (CAD) (angina pectoris, history of myocardial infarction, or documented silent ischemia) or coronary artery vasospasm, including Prinzmetal’s angina [see Warnings and Precautions ( 5.1)] .
- Wolff-Parkinson-White syndrome or arrhythmias associated with other cardiac accessory conduction pathway disorders [see Warnings and Precautions ( 5.2)] .
- History of stroke or transient ischemic attack (TIA) because these patients are at a higher risk of stroke [see Warnings and Precautions ( 5.4)] .
- History of hemiplegic or basilar migraine.
- Peripheral vascular disease [see Warnings and Precautions ( 5.5)] .
- Ischemic bowel disease [see Warnings and Precautions ( 5.5) ].
- Uncontrolled hypertension [see Warnings and Precautions ( 5.8)] .
- Recent (i.e., within 24 hours) use of ergotamine-containing medication, ergot-type medication (such as dihydroergotamine or methysergide), or another 5‑hydroxytryptamine 1 (5-HT 1) agonist [see Drug Interactions ( 7.1, 7.3)] .
- Concurrent administration of an MAO-A inhibitor or recent (within 2 weeks) use of an MAO-A inhibitor [see Drug Interactions ( 7.2) and Clinical Pharmacology ( 12.3)] .
- Known hypersensitivity to sumatriptan [see Warnings and Precautions ( 5.9) and Adverse Reactions ( 6.2)] .
- Severe hepatic impairment [see Clinical Pharmacology ( 12.3)] .
-
5 WARNINGS AND PRECAUTIONS
5.1 Myocardial Ischemia, Myocardial Infarction, and Prinzmetal's Angina
The use of sumatriptan succinate injection is contraindicated in patients with ischemic or vasospastic CAD. There have been rare reports of serious cardiac adverse reactions, including acute myocardial infarction, occurring within a few hours following administration of sumatriptan succinate injection. Some of these reactions occurred in patients without known CAD. 5-HT 1 agonists, including sumatriptan succinate injection, may cause coronary artery vasospasm (Prinzmetal’s angina), even in patients without a history of CAD.
Perform a cardiovascular evaluation in triptan-naive patients who have multiple cardiovascular risk factors (e.g., increased age, diabetes, hypertension, smoking, obesity, strong family history of CAD) prior to receiving sumatriptan succinate injection. If there is evidence of CAD or coronary artery vasospasm, sumatriptan succinate injection is contraindicated. For patients with multiple cardiovascular risk factors who have a negative cardiovascular evaluation, consider administering the first dose of sumatriptan succinate injection in a medically supervised setting and performing an electrocardiogram (ECG) immediately following sumatriptan succinate injection. For such patients, consider periodic cardiovascular evaluation in intermittent long-term users of sumatriptan succinate injection.
Evaluate patients with signs or symptoms suggestive of angina following sumatriptan succinate injection for the presence of CAD or Prinzmetal’s angina before receiving additional doses of sumatriptan succinate injection.5.2 Arrhythmias
Life-threatening disturbances of cardiac rhythm, including ventricular tachycardia and ventricular fibrillation leading to death, have been reported within a few hours following the administration of 5-HT 1 agonists. Discontinue sumatriptan succinate injection if these disturbances occur. Sumatriptan succinate injection is contraindicated in patients with Wolff-Parkinson-White syndrome or arrhythmias associated with other cardiac accessory conduction pathway disorders.
5.3 Chest, Throat, Neck, and/or Jaw Pain/Tightness/Pressure
As with other 5-HT 1 agonists, sensations of tightness, pain, pressure, and heaviness in the precordium, throat, neck, and jaw commonly occur after treatment with sumatriptan succinate injection and are usually non-cardiac in origin. However, perform a cardiac evaluation if these patients are at high cardiac risk. The use of sumatriptan succinate injection is contraindicated in patients shown to have CAD and those with Prinzmetal’s variant angina.
5.4 Cerebrovascular Events
Cerebral hemorrhage, subarachnoid hemorrhage, and stroke have occurred in patients treated with 5-HT 1 agonists, and some have resulted in fatalities. In a number of cases, it appears possible that the cerebrovascular events were primary, the 5-HT 1 agonist having been administered in the incorrect belief that the symptoms experienced were a consequence of migraine when they were not. Also, patients with migraine may be at increased risk of certain cerebrovascular events (e.g., stroke, hemorrhage, TIA). Discontinue sumatriptan succinate injection if a cerebrovascular event occurs.
As with other acute migraine therapies, before treating headaches in patients not previously diagnosed as migraineurs, and in migraineurs who present with atypical symptoms, exclude other potentially serious neurological conditions. Sumatriptan succinate injection is contraindicated in patients with a history of stroke or TIA.5.5 Other Vasospasm Reactions
5-HT 1 agonists, including sumatriptan succinate injection, may cause non-coronary vasospastic reactions, such as peripheral vascular ischemia, gastrointestinal vascular ischemia and infarction (presenting with abdominal pain and bloody diarrhea), splenic infarction, and Raynaud’s syndrome. Until further evaluation, sumatriptan succinate injection is contraindicated in patients who experience symptoms or signs suggestive of non-coronary vasospasm reaction following the use of any 5-HT 1 agonist.
Reports of transient and permanent blindness and significant partial vision loss have been reported with the use of 5-HT 1 agonists. Since visual disorders may be part of a migraine attack, a causal relationship between these events and the use of 5-HT 1 agonists have not been clearly established.5.6 Medication Overuse Headache
Overuse of acute migraine drugs (e.g., ergotamine, triptans, opioids, combination of drugs for 10 or more days per month) may lead to exacerbation of headache (medication overuse headache). Medication overuse headache may present as migraine-like daily headaches, or as a marked increase in frequency of migraine attacks. Detoxification of patients, including withdrawal of the overused drugs, and treatment of withdrawal symptoms (which often includes a transient worsening of headache) may be necessary.
5.7 Serotonin Syndrome
Serotonin syndrome may occur with triptans, including sumatriptan succinate injection, particularly during coadministration with selective serotonin reuptake inhibitors (SSRIs), serotonin norepinephrine reuptake inhibitors (SNRIs), tricyclic antidepressants (TCAs), and MAO inhibitors [see Drug Interactions ( 7.4)] . Serotonin syndrome symptoms may include mental status changes (e.g., agitation, hallucinations, coma), autonomic instability (e.g., tachycardia, labile blood pressure, hyperthermia), neuromuscular aberrations (e.g., hyperreflexia, incoordination), and/or gastrointestinal symptoms (e.g., nausea, vomiting, diarrhea). The onset of symptoms usually occurs within minutes to hours of receiving a new or a greater dose of a serotonergic medication. Discontinue sumatriptan succinate injection if serotonin syndrome is suspected.
5.8 Increase in Blood Pressure
Significant elevation in blood pressure, including hypertensive crisis with acute impairment of organ systems, has been reported on rare occasions in patients treated with 5-HT 1 agonists, including patients without a history of hypertension. Monitor blood pressure in patients treated with sumatriptan succinate. Sumatriptan succinate injection is contraindicated in patients with uncontrolled hypertension.
5.9 Anaphylactic/Anaphylactoid Reactions
Anaphylactic/anaphylactoid reactions have occurred in patients receiving sumatriptan. Such reactions can be life threatening or fatal. In general, anaphylactic reactions to drugs are more likely to occur in individuals with a history of sensitivity to multiple allergens. Sumatriptan succinate injection is contraindicated in patients with prior serious anaphylactic reaction.
5.10 Seizures
Seizures have been reported following administration of sumatriptan. Some have occurred in patients with either a history of seizures or concurrent conditions predisposing to seizures. There are also reports in patients where no such predisposing factors are apparent. Sumatriptan succinate injection should be used with caution in patients with a history of epilepsy or conditions associated with a lowered seizure threshold.
-
6 ADVERSE REACTIONS
The following adverse reactions are discussed in more detail in other sections of the labeling:
- Myocardial ischemia, myocardial infarction, and Prinzmetal’s angina [see Warnings and Precautions ( 5.1)]
- Arrhythmias [see Warnings and Precautions ( 5.2)]
- Chest, throat, neck, and/or jaw pain/tightness/pressure [see Warnings and Precautions ( 5.3)]
- Cerebrovascular events [see Warnings and Precautions ( 5.4)]
- Other vasospasm reactions [see Warnings and Precautions ( 5.5)]
- Medication overuse headache [see Warnings and Precautions ( 5.6)]
- Serotonin syndrome [see Warnings and Precautions ( 5.7)]
- Increase in blood pressure [see Warnings and Precautions ( 5.8)]
- Anaphylactic/anaphylactoid reactions [see Warnings and Precautions ( 5.9)]
- Seizures [see Warnings and Precautions ( 5.10)]
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared with rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Migraine Headache: Table 1 lists adverse reactions that occurred in 2 US placebo-controlled clinical trials in migraine subjects [Studies 2 and 3, see Clinical Studies ( 14.1)] following either a single 6 mg dose of sumatriptan succinate injection or placebo. Only reactions that occurred at a frequency of 2% or more in groups treated with sumatriptan succinate injection 6 mg and that occurred at a frequency greater than the placebo group are included in Table 1.
Table 1. Adverse Reactions Reported by at Least 2% of Subjects and at a Greater Frequency than Placebo in 2 Placebo-Controlled Migraine Clinical Trials (Studies 2 and 3) a
Adverse ReactionPercent of Subjects Reporting
Sumatriptan Succinate Injection
6 mg
Subcutaneous
(n = 547)
Placebo
(n=370)
Atypical sensations
Tingling
Warm/hot sensation
Burning sensation
Feeling of heaviness
Pressure sensation
Feeling of tightness
Numbness
Feeling strange
Tight feeling in head
42
14
11
7
7
7
5
5
2
2
9
3
4
< 1
1
2
< 1
2
< 1
< 1
Cardiovascular
Flushing
7
2
Chest discomfort
Tightness in chest
Pressure in chest
5
3
2
1
< 1
< 1
Ear, nose, and throat
Throat discomfort
Discomfort: nasal cavity/sinuses
3
2
< 1
< 1
Injection site reaction b
59
24
Miscellaneous
Jaw discomfort
2
0
Musculoskeletal
Weakness
Neck pain/stiffness
Myalgia
5
5
2
< 1
< 1
< 1
Neurological
Dizziness/vertigo
Drowsiness/sedation
Headache
12
3
2
4
2
< 1
Skin
Sweating
2
1
a The sum of the percentages cited is greater than 100% because subjects may have experienced more than 1 type of adverse reaction. Only reactions that occurred at a frequency of 2% or more in groups treated with sumatriptan succinate injection and occurred at a frequency greater than the placebo groups are included.
b Includes injection site pain, stinging/burning, swelling, erythema, bruising, bleeding.
The incidence of adverse reactions in controlled clinical trials was not affected by gender or age of the subjects. There were insufficient data to assess the impact of race on the incidence of adverse reactions.Cluster Headache: In the controlled clinical trials assessing the efficacy of sumatriptan succinate injection as a treatment for cluster headache [Studies 4 and 5, see Clinical Studies ( 14.2)] , no new significant adverse reactions were detected that had not already been identified in trials of sumatriptan succinate in subjects with migraine.
Overall, the frequency of adverse reactions reported in the trials of cluster headache was generally lower than in the migraine trials. Exceptions include reports of paresthesia (5% sumatriptan succinate, 0% placebo), nausea and vomiting (4% sumatriptan succinate, 0% placebo), and bronchospasm (1% sumatriptan succinate, 0% placebo).
Other Adverse Reactions: In the paragraphs that follow, the frequencies of less commonly reported adverse reactions are presented. Reaction frequencies were calculated as the number of subjects reporting a reaction divided by the total number of subjects (N = 6,218) exposed to subcutaneous sumatriptan succinate injection. All reported reactions are included except those already listed in the previous table. Reactions are further classified within body system categories and enumerated in order of decreasing frequency using the following definitions: frequent are defined as those occurring in at least 1/100 subjects, infrequent are those occurring in 1/100 to 1/1,000 subjects, and rare are those occurring in fewer than 1/1,000 subjects.
Cardiovascular: Infrequent were hypertension, hypotension, bradycardia, tachycardia, palpitations, and syncope. Rare was arrhythmia.
Gastrointestinal: Frequent was abdominal discomfort.
Musculoskeletal: Frequent were muscle cramps.
Neurological: Frequent was anxiety. Infrequent were mental confusion, euphoria, agitation, tremor. Rare were myoclonia, sleep disturbance, and dystonia.
Respiratory: Infrequent was dyspnea.
Skin: Infrequent were erythema, pruritus, and skin rashes.
Miscellaneous: Infrequent was “serotonin agonist effect”.
Adverse Events Observed with Other Formulations of Sumatriptan Succinate: The following adverse events occurred in clinical trials with sumatriptan succinate tablets and sumatriptan succinate nasal spray. Because the reports include events observed in open and uncontrolled trials, the role of sumatriptan succinate in their causation cannot be reliably determined. All reported events are included except those already listed, those too general to be informative, and those not reasonably associated with the use of the drug.
Cardiovascular: Angina, cerebrovascular lesion, heart block, peripheral cyanosis, phlebitis, thrombosis.
Gastrointestinal: Abdominal distention and colitis.
Neurological: Convulsions, hallucinations, syncope, suicide, and twitching.
Miscellaneous: Edema, hypersensitivity, swelling of extremities, and swelling of face.
6.2 Postmarketing Experience
The following adverse reactions have been identified during postapproval use of sumatriptan succinate tablets, sumatriptan succinate nasal spray, and sumatriptan succinate injection. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure. These reactions have been chosen for inclusion due to either their seriousness, frequency of reporting, or causal connection to sumatriptan succinate or a combination of these factors.
Blood: Hemolytic anemia, pancytopenia, thrombocytopenia.
Ear, Nose, and Throat: Deafness.
Eye: Ischemic optic neuropathy, retinal artery occlusion, retinal vein thrombosis.
Neurological: Central nervous system vasculitis, cerebrovascular accident, serotonin syndrome, subarachnoid hemorrhage.
Non-Site Specific: Angioedema, cyanosis, temporal arteritis.
Skin: Exacerbation of sunburn, hypersensitivity reactions (allergic vasculitis, erythema, pruritus, rash, shortness of breath, urticaria), photosensitivity. Following subcutaneous administration of sumatriptan succinate, pain, redness, stinging, induration, swelling, contusion, subcutaneous bleeding, and, on rare occasions, lipoatrophy (depression in the skin) or lipohypertrophy (enlargement or thickening of tissue) have been reported.
Urogenital: Acute renal failure.
-
7 DRUG INTERACTIONS
7.1 Ergot-Containing Drugs
Ergot-containing drugs have been reported to cause prolonged vasospastic reactions. Because these effects may be additive, use of ergotamine-containing or ergot-type medications (like dihydroergotamine or methysergide) and sumatriptan succinate injection within 24 hours of each other is contraindicated.
7.2 Monoamine Oxidase-A Inhibitors
MAO-A inhibitors increase systemic exposure by 2-fold. Therefore, the use of sumatriptan succinate injection in patients receiving MAO-A inhibitors is contraindicated [see Clinical Pharmacology ( 12.3)] .
7.3 Other 5-HT1 Agonists
Because their vasospastic effects may be additive, coadministration of sumatriptan succinate injection and other 5-HT 1 agonists (e.g., triptans) within 24 hours of each other is contraindicated.
7.4 Selective Serotonin Reuptake Inhibitors/Serotonin Norepinephrine Reuptake Inhibitors and Serotonin Syndrome
Cases of serotonin syndrome have been reported during coadministration of triptans and SSRIs, or SNRIs, SNRIs, TCAs, and MAO inhibitors [see Warnings and Precautions ( 5.7)] .
-
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Pregnancy Category C: There are no adequate and well-controlled trials of sumatriptan succinate injection in pregnant women. Sumatriptan succinate injection should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
When sumatriptan was administered intravenously to pregnant rabbits daily throughout the period of organogenesis, embryolethality was observed at doses at or close to those producing maternal toxicity. These doses were less than the maximum recommended human dose (MRHD) of 12 mg/day on a mg/m 2 basis. Oral administration of sumatriptan to rabbits during organogenesis was associated with increased incidences of fetal vascular and skeletal abnormalities. The highest no-effect dose for these effects was 15 mg/kg/day. The intravenous administration of sumatriptan to pregnant rats throughout organogenesis at doses that are approximately 10 times the MRHD on a mg/m 2 basis, did not produce evidence of embryolethality. The subcutaneous administration of sumatriptan to pregnant rats prior to and throughout pregnancy did not produce evidence of embryolethality or teratogenicity.8.3 Nursing Mothers
It is not known whether sumatriptan is excreted in human breast milk following subcutaneous administration. Because many drugs are excreted in human milk, and because of the potential for serious adverse reactions in nursing infants from sumatriptan succinate, a decision should be made whether to discontinue nursing or to discontinue the drug, taking into account the importance of the drug to the mother.
8.4 Pediatric Use
Safety and effectiveness of sumatriptan succinate injection in pediatric patients under 18 years of age have not been established; therefore, sumatriptan succinate injection is not recommended for use in patients under 18 years of age.
Two controlled clinical trials evaluated sumatriptan succinate nasal spray (5 to 20 mg) in 1,248 adolescent migraineurs aged 12 to 17 years who treated a single attack. The trials did not establish the efficacy of sumatriptan succinate nasal spray compared with placebo in the treatment of migraine in adolescents. Adverse reactions observed in these clinical trials were similar in nature to those reported in clinical trials in adults.
Five controlled clinical trials (2 single-attack trials, 3 multiple-attack trials) evaluating oral sumatriptan succinate (25 to 100 mg) in pediatric subjects aged 12 to 17 years enrolled a total of 701 adolescent migraineurs. These trials did not establish the efficacy of oral sumatriptan succinate compared with placebo in the treatment of migraine in adolescents. Adverse reactions observed in these clinical trials were similar in nature to those reported in clinical trials in adults. The frequency of all adverse reactions in these subjects appeared to be both dose- and age-dependent, with younger subjects reporting reactions more commonly than older adolescents.
Postmarketing experience documents that serious adverse reactions have occurred in the pediatric population after use of subcutaneous, oral, and/or intranasal sumatriptan succinate. These reports include reactions similar in nature to those reported rarely in adults, including stroke, visual loss, and death. A myocardial infarction has been reported in a 14-year-old male following the use of oral sumatriptan succinate; clinical signs occurred within 1 day of drug administration. Since clinical data to determine the frequency of serious adverse reactions in pediatric patients who might receive subcutaneous, oral, or intranasal sumatriptan succinate are not presently available, the use of sumatriptan succinate in patients under 18 years of age is not recommended.8.5 Geriatric Use
Clinical trials of sumatriptan succinate injection did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger subjects. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function and of concomitant disease or other drug therapy.
A cardiovascular evaluation is recommended for geriatric patients who have other cardiovascular risk factors (e.g., diabetes, hypertension, smoking, obesity, strong family history of CAD) prior to receiving sumatriptan succinate injection [see Warnings and Precautions ( 5.1)] . -
10 OVERDOSAGE
No gross overdoses in clinical practice have been reported. Coronary vasospasm was observed after intravenous administration of sumatriptan succinate injection [see Contraindications ( 4)] . Overdoses would be expected from animal data (dogs at 0.1 g/kg, rats at 2 g/kg) to possibly cause convulsions, tremor, inactivity, erythema of the extremities, reduced respiratory rate, cyanosis, ataxia, mydriasis, injection site reactions (desquamation, hair loss, and scab formation), and paralysis.
The elimination half-life of sumatriptan is about 2 hours [see Clinical Pharmacology ( 12.3)] , and therefore monitoring of patients after overdose with sumatriptan succinate injection should continue for at least 10 hours or while symptoms or signs persist. It is unknown what effect hemodialysis or peritoneal dialysis has on the serum concentrations of sumatriptan. -
11 DESCRIPTION
Sumatriptan succinate injection contains sumatriptan succinate, a selective 5-HT 1B/1D receptor agonist. Sumatriptan succinate is chemically designated as 3-[2-(dimethylamino)ethyl]-N-methyl-indole-5-methanesulfonamide succinate (1:1), and it has the following structure:
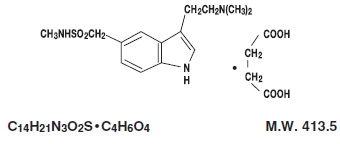
Sumatriptan succinate is a white to off-white powder that is readily soluble in water and in saline.
Sumatriptan succinate injection is a clear, colorless to pale yellow, sterile, nonpyrogenic solution for subcutaneous injection. Each 0.5 mL of sumatriptan succinate injection 12 mg/mL solution contains 6 mg of sumatriptan (base) as the succinate salt and 3.5 mg of sodium chloride in water for injection. The pH range of the solution is approximately 4.2 to 5.3. The osmolality of the injection is 291 mOsmol.
-
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Sumatriptan binds with high affinity to human cloned 5-HT 1B/1D receptors. Sumatriptan succinate presumably exerts its therapeutic effects in the treatment of migraine headache by binding to 5‑HT 1B/1D receptors located on intracranial blood vessels and sensory nerves of the trigeminal system.
Current theories proposed to explain the etiology of migraine headache suggest that symptoms are due to local cranial vasodilatation and/or to the release of sensory neuropeptides (including substance P and calcitonin gene-related peptide) through nerve endings in the trigeminal system. The therapeutic activity of sumatriptan succinate for the treatment of migraine and cluster headaches is thought to be due to the agonist effects at the 5-HT 1B/1D receptors on intracranial blood vessels (including the arterio-venous anastomoses) and sensory nerves of the trigeminal system, which result in cranial vessel constriction and inhibition of pro-inflammatory neuropeptide release.
12.2 Pharmacodynamics
Blood Pressure: Significant elevation in blood pressure, including hypertensive crisis, has been reported in patients with and without a history of hypertension [see Warnings and Precautions ( 5.8)] .
Peripheral (Small) Arteries: In healthy volunteers (N = 18), a trial evaluating the effects of sumatriptan on peripheral (small vessel) arterial reactivity failed to detect a clinically significant increase in peripheral resistance.
Heart Rate: Transient increases in blood pressure observed in some subjects in clinical trials carried out during sumatriptan’s development as a treatment for migraine were not accompanied by any clinically significant changes in heart rate.
12.3 Pharmacokinetics
Absorption and Bioavailability: The bioavailability of sumatriptan via subcutaneous site injection to 18 healthy male subjects was 97% ± 16% of that obtained following intravenous injection.
After a single 6 mg subcutaneous manual injection into the deltoid area of the arm in 18 healthy males (age: 24 ± 6 years, weight: 70 kg), the maximum serum concentration (C max) of sumatriptan was (mean ± standard deviation) 74 ± 15 ng/mL and the time to peak concentration (T max) was 12 minutes after injection (range: 5 to 20 minutes). In this trial, the same dose injected subcutaneously in the thigh gave a C max of 61 ± 15 ng/mL by manual injection versus 52 ± 15 ng/mL by autoinjector techniques. The T max or amount absorbed was not significantly altered by either the site or technique of injection.
Distribution: Protein binding, determined by equilibrium dialysis over the concentration range of 10 to 1,000 ng/mL, is low, approximately 14% to 21%. The effect of sumatriptan on the protein binding of other drugs has not been evaluated.
Following a 6 mg subcutaneous injection into the deltoid area of the arm in 9 males (mean age: 33 years, mean weight: 77 kg) the volume of distribution central compartment of sumatriptan was 50 ± 8 liters and the distribution half-life was 15 ± 2 minutes.
Metabolism: In vitro studies with human microsomes suggest that sumatriptan is metabolized by MAO, predominantly the A isoenzyme. Most of a radiolabeled dose of sumatriptan excreted in the urine is the major metabolite indole acetic acid (IAA) or the IAA glucuronide, both of which are inactive.
Elimination: After a single 6 mg subcutaneous dose, 22% ± 4% was excreted in the urine as unchanged sumatriptan and 38% ± 7% as the IAA metabolite.
Following a 6 mg subcutaneous injection into the deltoid area of the arm, the systemic clearance of sumatriptan was 1,194 ± 149 mL/min and the terminal half-life was 115 ± 19 minutes.
Special Populations: Age: The pharmacokinetics of sumatriptan in the elderly (mean age: 72 years, 2 males and 4 females) and in subjects with migraine (mean age: 38 years, 25 males and 155 females) were similar to that in healthy male subjects (mean age: 30 years).
Renal Impairment: The effect of renal impairment on the pharmacokinetics of sumatriptan has not been examined.
Hepatic Impairment: The effect of mild to moderate hepatic disease on the pharmacokinetics of subcutaneously administered sumatriptan has been evaluated. There were no significant differences in the pharmacokinetics of subcutaneously administered sumatriptan in moderately hepatically impaired subjects compared with healthy controls. The pharmacokinetics of subcutaneously administered sumatriptan in patients with severe hepatic impairment has not been studied. The use of sumatriptan succinate injection in this population is contraindicated [see Contraindications ( 4)] .
Race: The systemic clearance and C max of sumatriptan were similar in Black (n = 34) and Caucasian (n = 38) healthy male subjects.
Drug Interaction Studies: Monoamine Oxidase-A Inhibitors: In a trial of 14 healthy females, pretreatment with an MAO-A inhibitor decreased the clearance of sumatriptan, resulting in a 2-fold increase in the area under the sumatriptan plasma concentration-time curve (AUC), corresponding to a 40% increase in elimination half-life .
-
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis: In carcinogenicity studies, rats and mice were given sumatriptan by oral gavage. Mice were dosed for 78 weeks and rats were dosed for 104 weeks. Average exposures achieved in mice receiving the highest dose were approximately 110 times the exposure attained in humans after the maximum recommended single dose of 6 mg. The highest dose to rats was approximately 260 times the maximum single dose of 6 mg on a mg/m 2 basis. There was no evidence of an increase in tumors in either species related to sumatriptan administration.
Mutagenesis: Sumatriptan was not mutagenic in the presence or absence of metabolic activation when tested in 2 gene mutation assays (the Ames test and the in vitro mammalian Chinese hamster V79/HGPRT assay). It was not clastogenic in 2 cytogenetics assays (the in vitro human lymphocyte assay and the in vivo rat micronucleus assay).
Impairment of Fertility: A fertility study (Segment I) by the subcutaneous route, during which male and female rats were dosed daily with sumatriptan prior to and throughout the mating period, has shown no evidence of impaired fertility at doses equivalent to approximately 100 times the maximum recommended single human dose of 6 mg on a mg/m 2 basis. However, following oral administration, a treatment-related decrease in fertility, secondary to a decrease in mating, was seen for rats treated with 50 and 500 mg/kg/day. The no-effect dose for this finding was approximately 8 times the maximum recommended single human dose of 6 mg on a mg/m 2 basis. It is not clear whether the problem is associated with the treatment of males or females or both.
13.2 Animal Toxicology and/or Pharmacology
Corneal Opacities: Dogs receiving oral sumatriptan developed corneal opacities and defects in the corneal epithelium. Corneal opacities were seen at the lowest dosage tested,
2 mg/kg/day, and were present after 1 month of treatment. Defects in the corneal epithelium were noted in a 60-week study. Earlier examinations for these toxicities were not conducted and no-effect doses were not established; however, the relative exposure at the lowest dose tested was approximately 5 times the human exposure after a 100 mg oral dose or 3 times the human exposure after a 6 mg subcutaneous dose.Melanin Binding: In rats with a single subcutaneous dose (0.5 mg/kg) of radiolabeled sumatriptan, the elimination half-life of radioactivity from the eye was 15 days, suggesting that sumatriptan and its metabolites bind to the melanin of the eye. The clinical significance of this binding is unknown.
-
14 CLINICAL STUDIES
14.1 Migraine
In controlled clinical trials enrolling more than 1,000 subjects during migraine attacks who were experiencing moderate or severe pain and 1 or more of the symptoms enumerated in Table 3, onset of relief began as early as 10 minutes following a 6 mg sumatriptan succinate injection. Lower doses of sumatriptan succinate injection may also prove effective, although the proportion of subjects obtaining adequate relief was decreased and the latency to that relief is greater with lower doses.
In Study 1, 6 different doses of sumatriptan succinate injection (n = 30 each group) were compared with placebo (n = 62), in a single-attack, parallel-group design, the dose response relationship was found to be as shown in Table 2.
Table 2. Proportion of Subjects with Migraine Relief and Incidence of Adverse Events by Time and by Sumatriptan Succinate Dose in Study 1
Dose of Sumatriptan Injection
Percent Subjects with Relief a
Adverse Events Incidence (%)
at 10 Minutes
at 30 Minutes
at 1 Hour
at 2 Hours
Placebo
1 mg
2 mg
3 mg
4 mg
6 mg
8 mg
5
10
7
17
13
10
23
15
40
23
47
37
63
57
24
43
57
57
50
73
80
21
40
43
60
57
70
83
55
63
63
77
80
83
93
a Relief is defined as the reduction of moderate or severe pain to no or mild pain after dosing without use of rescue medication.
In 2 randomized, placebo-controlled clinical trials of sumatriptan succinate injection 6 mg in 1,104 subjects with moderate or severe migraine pain (Studies 2 and 3), the onset of relief was less than 10 minutes. Headache relief, as defined by a reduction in pain from severe or moderately severe to mild or no headache, was achieved in 70% of the subjects within 1 hour of a single 6 mg subcutaneous dose of sumatriptan succinate injection. Approximately 82% and 65% of subjects treated with sumatriptan succinate 6 mg had headache relief and were pain free within 2 hours, respectively.
Table 3 shows the 1- and 2-hour efficacy results for sumatriptan succinate injection 6 mg in Studies 2 and 3.
Table 3. Proportion of Subjects with Pain Relief and Relief of Migraine Symptoms after 1 and 2 Hours of Treatment in Studies 2 and 3
1-Hour Data
Study2
Study 3
Placebo
(n = 190)
Sumatriptan Succinate
6 mg
(n = 384)
Placebo
(n = 180)
Sumatriptan Succinate 6 mg (n = 350)
Subjects with pain relief (grade 0/1)
Subjects with no pain
Subjects without nausea
Subjects without photophobia
Subjects with little or no clinical disability b
18%
5%
48%
23%
34%
70% a
48% a
73% a
56% a
76% a
26%
13%
50%
25%
34%
70% a
49% a
73% a
58% a
76% a
2-Hour Data
Study2
Study 3
Placebo c
Sumatriptan Succinate 6 mg d
Placebo c
Sumatriptan Succinate 6 mg d
Subjects with pain relief (grade 0/1)
Subjects with no pain
Subjects without nausea
Subjects without photophobia
Subjects with little or no clinical disability b
31%
11%
56%
31%
42%
81% a
63% a
82% a
72% a
85% a
39%
19%
63%
35%
49%
82% a
65% a
81% a
71% a
84% a
a P<0.05 versus placebo.
b A successful outcome in terms of clinical disability was defined prospectively as ability to work mildly impaired or ability to work and function normally.
c Includes subjects that may have received an additional placebo injection 1 hour after the initial injection.
d Includes subjects that may have received an additional 6 mg of sumatriptan succinate injection 1 hour after the initial injection.
Sumatriptan succinate injection also relieved photophobia, phonophobia (sound sensitivity), nausea, and vomiting associated with migraine attacks.
The efficacy of sumatriptan succinate injection was unaffected by whether or not the migraine was associated with aura, duration of attack, gender or age of the subject, or concomitant use of common migraine prophylactic drugs (e.g., beta-blockers).
14.2 Cluster Headache
The efficacy of sumatriptan succinate injection in the acute treatment of cluster headache was demonstrated in 2 randomized, double-blind, placebo-controlled, 2-period crossover trials (Studies 4 and 5). Subjects aged 21 to 65 years were enrolled and were instructed to treat a moderate to very severe headache within 10 minutes of onset. Headache relief was defined as a reduction in headache severity to mild or no pain. In both trials, the proportion of individuals gaining relief at 10 or 15 minutes was significantly greater among subjects receiving 6 mg of sumatriptan succinate injection compared with those who received placebo (see Table 4).
Table 4. Proportion of Subjects with Cluster Headache Relief by Time in Studies 4 and 5
Study 4
Study 5
Placebo
(n = 39)
Sumatriptan Succinate
6 mg
(n = 39)
Placebo
(n = 88)
Sumatriptan Succinate 6 mg (n = 92)
Subjects with pain relief (no/mild)
5 Minutes post-injection
10 Minutes post-injection
15 Minutes post-injection
8%
10%
26%
21%
49% a
74% a
7%
25%
35%
23% a
49% a
75% a
a P<0.05.
(n = Number of headaches treated.)
An estimate of the cumulative probability of a subject with a cluster headache obtaining relief after being treated with either sumatriptan succinate injection or placebo is presented in Figure 1.
Figure 1. Time to Relief of Cluster Headache from Time of Injection a
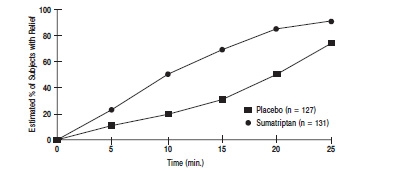
a The figure uses Kaplan-Meier (product limit) Survivorship Plot. Subjects taking rescue medication were censored at 15 minutes.
The plot was constructed with data from subjects who either experienced relief or did not require (request) rescue medication within a period of 2 hours following treatment. As a consequence, the data in the plot are derived from only a subset of the 258 headaches treated (rescue medication was required in 52 of the 127 placebo-treated headaches and 18 of the 131 headaches treated with sumatriptan succinate injection).
Other data suggest that treatment with sumatriptan succinate injection is not associated with an increase in early recurrence of headache and has little effect on the incidence of later-occurring headaches (i.e., those occurring after 2, but before 18 or 24 hours).
-
16 HOW SUPPLIED/STORAGE AND HANDLING
Sumatriptan succinate injection contains sumatriptan (base) as the succinate salt and is supplied as a clear, colorless to pale yellow, sterile, nonpyrogenic solution as follows:
Product
No.
NDC
No.
Strength
271301
63323-273-01
6 mg
(sumatriptan)
0.5 mL
0.5 mL single dose vial, packaged individually.
Store between 2° and 25°C (36° and 77°F). Protect from light.
The container closure is not made with natural rubber latex.
-
17 PATIENT COUNSELING INFORMATION
See FDA-approved patient labeling (Patient Information leaflet).
Risk of Myocardial Ischemia and/or Infarction, Prinzmetal’s Angina, Other Vasospasm-Related Events, Arrhythmias, and Cerebrovascular Events
Inform patients that sumatriptan succinate injection may cause serious cardiovascular side effects such as myocardial infarction or stroke. Although serious cardiovascular events can occur without warning symptoms, patients should be alert for the signs and symptoms of chest pain, shortness of breath, irregular heartbeat, significant rise in blood pressure, weakness, and slurring of speech and should ask for medical advice when observing any indicative sign or symptoms. Patients should be apprised of the importance of this follow-up [see Warnings and Precautions ( 5.1, 5.2, 5.4, 5.5, 5.8)] .
Anaphylactic/Anaphylactoid Reactions
Inform patients that anaphylactic/anaphylactoid reactions have occurred in patients receiving sumatriptan succinate injection. Such reactions can be life threatening or fatal. In general, anaphylactic reactions to drugs are more likely to occur in individuals with a history of sensitivity to multiple allergens [see Warnings and Precautions ( 5.9)] .
Medication Overuse Headache
Inform patients that use of acute migraine drugs for 10 or more days per month may lead to an exacerbation of headache and encourage patients to record headache frequency and drug use (e.g., by keeping a headache diary) [see Warnings and Precautions ( 5.6)] .
Pregnancy
Inform patients that sumatriptan succinate injection should not be used during pregnancy unless the potential benefit justifies the potential risk to the fetus [see Use in Specific Populations ( 8.1)] .
Nursing Mothers
Advise patients to notify their healthcare provider if they are breastfeeding or plan to breastfeed [see Use in Specific Populations ( 8.3)] .
Ability to Perform Complex TasksSince migraines or treatment with sumatriptan succinate injection may cause somnolence and dizziness, instruct patients to evaluate their ability to perform complex tasks during migraine attacks and after administration of sumatriptan succinate injection.
Serotonin SyndromePatients should be cautioned about the risk of serotonin syndrome with the use of sumatriptan succinate injection or other triptans, particularly during combined use with SSRIs, SNRIs, TCAs, and MAO inhibitors [see Warnings and Precautions (5.7) and Drug Interactions ( 7.4)] .
How to Use Sumatriptan Succinate Injection
Provide patients instruction on the proper use of sumatriptan succinate injection if they are able to self-administer sumatriptan succinate injection in medically unsupervised situation.
Inform patients that the injection is intended to be given subcutaneously and intramuscular or intravascular delivery should be avoided. Instruct patients to use injection sites with an adequate skin and subcutaneous thickness to accommodate the length of the needle.
-
PATIENT PACKAGE INSERT
SUMATRIPTAN SUCCINATE
(soo´mətrip´tan suk´sənāt´)
INJECTION
Read this Patient Information leaflet before you start taking sumatriptan succinate injection and each time you get a refill. There may be new information. This information does not take the place of talking with your healthcare provider about your medical condition or treatment.
What is the most important information I should know about sumatriptan succinate injection?
Sumatriptan succinate injection can cause serious side effects, including:
Heart attack and other heart problems. Heart problems may lead to death.
Stop taking sumatriptan succinate injection and get emergency medical help right away if you have any of the following symptoms of a heart attack:
- discomfort in the center of your chest that lasts for more than a few minutes, or that goes away and comes back
- severe tightness, pain, pressure, or heaviness in your chest, throat, neck, or jaw
- pain or discomfort in your arms, back, neck, jaw, or stomach
- shortness of breath with or without chest discomfort
- breaking out in a cold sweat
- nausea or vomiting
- feeling lightheaded
Sumatriptan succinate injection is not for people with risk factors for heart disease unless a heart exam is done and shows no problem. You have a higher risk for heart disease if you:
- have high blood pressure
- have high cholesterol levels
- smoke
- are overweight
- have diabetes
- have a family history of heart disease
What is sumatriptan succinate injection?
Sumatriptan succinate injection is a prescription medicine used to treat acute migraine headaches with or without aura and acute cluster headaches in adults who have been diagnosed with migraine or cluster headaches.
Sumatriptan succinate injection is not used to treat other types of headaches such as hemiplegic (that make you unable to move on one side of your body) or basilar (rare form of migraine with aura) migraines.
Sumatriptan succinate injection is not used to prevent or decrease the number of migraine or cluster headaches you have.
It is not known if sumatriptan succinate injection is safe and effective in children under 18 years of age.
Who should not take sumatriptan succinate injection?
Do not take sumatriptan succinate injection if you have:
- heart problems or a history of heart problems
- narrowing of blood vessels to your legs, arms, stomach, or kidney (peripheral vascular disease)
- uncontrolled high blood pressure
- hemiplegic migraines or basilar migraines. If you are not sure if you have these types of migraines, ask your healthcare provider.
- had a stroke, transient ischemic attacks (TIAs), or problems with your blood circulation
- taken any of the following medicines in the last 24 hours:
- almotriptan (AXERT ®)
- eletriptan (RELPAX ®)
- frovatriptan (FROVA ®)
- naratriptan (AMERGE ®)
- rizatriptan (MAXALT ®, MAXALT-MLT ®)
- sumatriptan and naproxen (TREXIMET ®)
- ergotamines (CAFERGOT ®, ERGOMAR ®, MIGERGOT ®)
- dihydroergotamine (D.H.E. 45 ®, MIGRANAL ®)
Ask your healthcare provider if you are not sure if your medicine is listed above.
- an allergy to sumatriptan or any of the ingredients in sumatriptan succinate injection. See the end of this leaflet for a complete list of ingredients in sumatriptan succinate injection.
What should I tell my healthcare provider before taking sumatriptan succinate injection?
Before you take sumatriptan succinate injection, tell your healthcare provider about all of your medical conditions, including if you:
- have high blood pressure
- have high cholesterol
- have diabetes
- smoke
- are overweight
- have heart problems or family history of heart problems or stroke
- have liver problems
- have had epilepsy or seizures
- are not using effective birth control
- become pregnant while taking sumatriptan succinate injection
- are breastfeeding or plan to breastfeed. Sumatriptan succinate injection passes into your breast milk and may harm your baby. Talk with your healthcare provider about the best way to feed your baby if you take sumatriptan succinate injection.
Tell your healthcare provider about all the medicines you take, including prescription and nonprescription medicines, vitamins, and herbal supplements.
Using sumatriptan succinate injection with certain other medicines can affect each other, causing serious side effects.
Especially tell your healthcare provider if you take anti-depressant medicines called:
- selective serotonin reuptake inhibitors (SSRIs)
- serotonin norepinephrine reuptake inhibitors (SNRIs)
- tricyclic antidepressants (TCAs)
- monoamine oxidase inhibitors (MAOIs)
Ask your healthcare provider or pharmacist for a list of these medicines if you are not sure.
Know the medicines you take. Keep a list of them to show your healthcare provider or pharmacist when you get a new medicine.
How should I take sumatriptan succinate injection?
- Certain people should take their first dose of sumatriptan succinate injection in their healthcare provider’s office or in another medical setting. Ask your healthcare provider if you should take your first dose in a medical setting.
- Use sumatriptan succinate injection exactly as your healthcare provider tells you to use it.
- Your healthcare provider may change your dose. Do not change your dose without first talking with your healthcare provider.
- For adults, the usual dose is a single injection given just below the skin.
- You should give an injection as soon as the symptoms of your headache start, but it may be given at any time during a migraine attack.
- If you did not get any relief after the first injection, do not give a second injection without first talking with your healthcare provider.
- You can take a second injection 1 hour after the first injection, but not sooner, if your headache came back after your first injection.
- Do not take more than 12 mg in a 24-hour period.
- If you use too much sumatriptan succinate injection, call your healthcare provider or go to the nearest hospital emergency room right away.
- You should write down when you have headaches and when you take sumatriptan succinate injection so you can talk with your healthcare provider about how sumatriptan succinate injection is working for you.
What should I avoid while taking sumatriptan succinate injection?
Sumatriptan succinate injection can cause dizziness, weakness, or drowsiness. If you have these symptoms, do not drive a car, use machinery, or do anything where you need to be alert.
What are the possible side effects of sumatriptan succinate injection?
Sumatriptan succinate injection may cause serious side effects. See “What is the most important information I should know about sumatriptan succinate injection?”
These serious side effects include:
- changes in color or sensation in your fingers and toes (Raynaud’s syndrome)
- stomach and intestinal problems (gastrointestinal and colonic ischemic events). Symptoms of gastrointestinal and colonic ischemic events include:
- sudden or severe stomach pain
- stomach pain after meals
- weight loss
- nausea or vomiting
- constipation or diarrhea
- bloody diarrhea
- fever
- problems with blood circulation to your legs and feet (peripheral vascular ischemia). Symptoms of peripheral vascular ischemia include:
- cramping and pain in your legs or hips
- feeling of heaviness or tightness in your leg muscles
- burning or aching pain in your feet or toes while resting
- numbness, tingling, or weakness in your legs
- cold feeling or color changes in 1 or both legs or feet
- medication overuse headaches. Some people who use too many sumatriptan succinate injections may have worse headaches (medication overuse headache). If your headaches get worse, your healthcare provider may decide to stop your treatment with sumatriptan succinate injection.
- serotonin syndrome. Serotonin syndrome is a rare but serious problem that can happen in people using sumatriptan succinate injection, especially if sumatriptan succinate injection is used with anti-depressant medicines called SSRIs or SNRIs.
Call your healthcare provider right away if you have any of the following symptoms of serotonin syndrome:
- mental changes such as seeing things that are not there (hallucinations), agitation, or coma
- fast heartbeat
- changes in blood pressure
- high body temperature
- tight muscles
- trouble walking
- seizures. Seizures have happened in people taking sumatriptan succinate injection who have never had seizures before. Talk with your healthcare provider about your chance of having seizures while you take sumatriptan succinate injection.
The most common side effects of sumatriptan succinate injection include:
- pain or redness at your injection site
- tingling or numbness in your fingers or toes
- dizziness
- warm, hot, burning feeling to your face (flushing)
- discomfort or stiffness in your neck
- feeling weak, drowsy, or tired
Tell your healthcare provider if you have any side effect that bothers you or that does not go away.
These are not all the possible side effects of sumatriptan succinate injection. For more information, ask your healthcare provider or pharmacist.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
How should I store sumatriptan succinate injection?
- Do not store at temperatures above 77°F (25°C).
- Store your medicine away from light.
- Keep your medicine in the packaging or carrying case provided with it.
Keep sumatriptan succinate injection and all medicines out of the reach of children.
General information about the safe and effective use of sumatriptan succinate injection
Medicines are sometimes prescribed for purposes other than those listed in Patient Information leaflets. Do not use sumatriptan succinate injection for a condition for which it was not prescribed. Do not give sumatriptan succinate injection to other people, even if they have the same symptoms you have. It may harm them.
This Patient Information leaflet summarizes the most important information about sumatriptan succinate injection. If you would like more information, talk with your healthcare provider. You can ask your healthcare provider or pharmacist for information about sumatriptan succinate injection that is written for healthcare professionals.
What are the ingredients in sumatriptan succinate injection?
Active ingredient: sumatriptan succinate
Inactive ingredients: sodium chloride, water for injection
This Patient Information leaflet has been approved by the U.S. Food and Drug Administration.
The brand names mentioned in this document are the trademarks of their respective owners.

451119C
Revised: April 2015
-
PRINCIPAL DISPLAY PANEL
PACKAGE LABEL - PRINCIPAL DISPLAY - Sumatriptan 0.5 mL Single Dose Vial Label
Sumatriptan Succinate Injection
6 mg (sumatriptan) per 0.5 mL
For subcutaneous injection only.
0.5 mL Single Dose Vial
Discard unused portion.

PACKAGE LABEL - PRINCIPAL DISPLAY - Sumatriptan 0.5 mL Single Dose Vial Carton Panel
NDC 63323-273-01
271301
Sumatriptan Succinate Injection
6 mg (sumatriptan) per 0.5 mL
For subcutaneous injection only.
Discard unused portion.
1 x 0.5 mL
Single Dose Vial
Rx only

-
INGREDIENTS AND APPEARANCE
SUMATRIPTAN SUCCINATE
sumatriptan succinate injectionProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 63323-273 Route of Administration SUBCUTANEOUS Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength SUMATRIPTAN SUCCINATE (UNII: J8BDZ68989) (SUMATRIPTAN - UNII:8R78F6L9VO) SUMATRIPTAN 6 mg in 0.5 mL Inactive Ingredients Ingredient Name Strength SODIUM CHLORIDE (UNII: 451W47IQ8X) 3.5 mg in 0.5 mL Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 63323-273-01 1 in 1 CARTON 04/12/2011 1 0.5 mL in 1 VIAL, SINGLE-DOSE; Type 0: Not a Combination Product Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA079242 04/12/2011 Labeler - Fresenius Kabi USA, LLC (608775388) Establishment Name Address ID/FEI Business Operations Fresenius Kabi USA, LLC 840771732 manufacture(63323-273)
© 2026 FDA.report
This site is not affiliated with or endorsed by the FDA.