LEVORA- levonorgestrel and ethinyl estradiol kit
Levora by
Drug Labeling and Warnings
Levora by is a Prescription medication manufactured, distributed, or labeled by RPK Pharmaceuticals, Inc.. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
- SPL UNCLASSIFIED SECTION
-
DESCRIPTION
21 white Levora® 0.15/30-28 tablets, each containing 0.15 mg of levonorgestrel, (d(-)-13 betaethyl-17- alpha-ethinyl-17-beta-hydroxygon-4-en-3-one), a totally synthetic progestogen, and 0.03 mg of ethinyl estradiol, (19-nor-17a-pregna-1,3,5 (10)-trien-20-yne-3,17-diol), and 7 peach inert tablets.
The white Levora® 0.15/30 tablets contain the following inactive ingredients: croscarmellose sodium, lactose, magnesium stearate, microcrystalline cellulose, and povidone.
The inactive peach tablets in the 28-day regimen of Levora® 0.15/30 contain the following inactive ingredients: FD&C Yellow No. 6 Lake, Lactose Anhydrous, Lactose Monohydrate, Magnesium Stearate and Microcrystalline Cellulose.
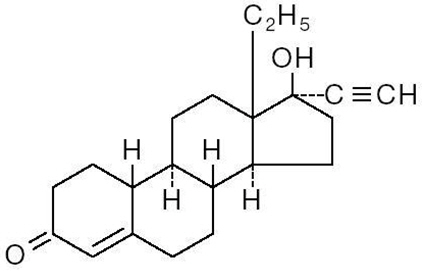
LEVONORGESTREL 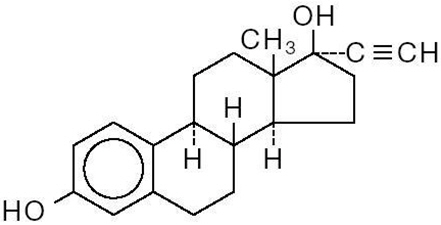
ETHINYL ESTRADIOL -
CLINICAL PHARMACOLOGY
Combination oral contraceptives act by suppression of gonadotropins. Although the primary mechanism of this action is inhibition of ovulation, other alterations include changes in the cervical mucus (which increase the difficulty of sperm entry into the uterus) and the endometrium (which reduce the likelihood of implantation).
-
INDICATIONS AND USAGE
Oral contraceptives are indicated for the prevention of pregnancy in women who elect to use this product as a method of contraception.
Oral contraceptives are highly effective. Table I lists the typical accidental pregnancy rates for users of combination oral contraceptives and other methods of contraception. The efficacy of these contraceptive methods, except sterilization and the IUD, depends upon the reliability with which they are used. Correct and consistent use of methods can result in lower failure rates.
TABLE I: PERCENTAGE OF WOMEN EXPERIENCING AN UNINTENDED PREGNANCY DURING THE FIRST YEAR OF USE OF A CONTRACEPTIVE METHOD Method Perfect Use Typical Use NA - not available - * Depending on method (calendar, ovulation, symptothermal, post-ovulation) Adapted from Hatcher RA et al, Contraceptive Technology: 17th Revised Edition. NY, NY: Ardent Media, Inc., 1998.
Levonorgestrel implants 0.05 0.05 Male sterilization 0.1 0.15 Female sterilization 0.5 0.5 Depo-Provera® (injectable progestogen) 0.3 0.3 Oral contraceptives 5 Combined 0.1 NA Progestin only 0.5 NA IUD Progesterone 1.5 2.0 Copper T 380A 0.6 0.8 Condom (male) without spermicide 3 14 (Female) without spermicide 5 21 Cervical cap Nulliparous women 9 20 Parous women 26 40 Vaginal sponge Nulliparous women 9 20 Parous women 20 40 Diaphragm with spermicidal cream or jelly 6 20 Spermicides alone (foam, creams, jellies, and vaginal suppositories) 6 26 Periodic abstinence (all methods) 1-9* 25 Withdrawal 4 19 No contraception (planned pregnancy) 85 85 -
CONTRAINDICATIONS
Combination oral contraceptives should not be used in women with any of the following conditions: Thrombophlebitis or thromboembolic disorders.
A past history of deep-vein thrombophlebitis or thromboembolic disorders.
Cerebral-vascular or coronary artery disease.
Thrombogenic valvulopathies. Thrombogenic rhythm disorders. Diabetes with vascular involvement.
Uncontrolled hypertension.
Known or suspected carcinoma of the breast.
Carcinoma of the endometrium or other known or suspected estrogen-dependent neoplasia. Undiagnosed abnormal genital bleeding.
Cholestatic jaundice of pregnancy or jaundice with prior pill use.
Hepatic adenomas or carcinomas, or active liver disease, as long as liver function has not returned to normal.
Known or suspected pregnancy.
Hypersensitivity to any of the components of Levora® 0.15/30-28 (levonorgestrel and ethinyl estradiol tablets).
Are receiving Hepatitis C drug combinations containing ombitasvir/paritaprevir/ritonavir, with or without dasabuvir, due to the potential for ALT elevations (see Warnings, RISK OF LIVER ENZYME ELEVATIONS WITH CONCOMITANT HEPATITIS C TREATMENT). -
WARNINGS
Cigarette smoking increases the risk of serious cardiovascular side effects from oral contraceptive use. This risk increases with age and with the extent of smoking (in epidemiologic studies, 15 or more cigarettes per day was associated with a significantly increased risk) and is quite marked in women over 35 years of age. Women who use oral contraceptives should be strongly advised not to smoke. The use of oral contraceptives is associated with increased risks of several serious conditions including venous and arterial thrombotic and thromboembolic events (such as myocardial infarction, thromboembolism, and stroke), hepatic neoplasia, gallbladder disease, and hypertension, although the risk of serious morbidity or mortality is very small in healthy women without underlying risk factors. The risk of morbidity and mortality increases significantly in the presence of other underlying risk factors such as certain inherited or acquired thrombophilias, hypertension, hyperlipidemias, obesity, and diabetes.
Practitioners prescribing oral contraceptives should be familiar with the following information relating to these risks.
The information contained in this package insert is based principally on studies carried out in patients who used oral contraceptives with higher formulations of estrogens and progestogens than those in common use today. The effect of long-term use of the oral contraceptives with lower formulations of both estrogens and progestogens remains to be determined.
Throughout this labeling, epidemiological studies reported are of two types: retrospective or case control studies and prospective or cohort studies. Case control studies provide a measure of the relative risk of disease, namely, a ratio of the incidence of a disease among oral contraceptive users to that among non-users. The relative risk does not provide information on the actual clinical occurrence of a disease. Cohort studies provide a measure of attributable risk, which is the difference in the incidence of disease between oral contraceptive users and non-users. The attributable risk does provide information about the actual occurrence of a disease in the population. For further information, the reader is referred to a text on epidemiological methods.
1. Thromboembolic Disorders and Other Vascular Problems
a. Myocardial Infarction
An increased risk of myocardial infarction has been attributed to oral contraceptive use. This risk is primarily in smokers or women with other underlying risk factors for coronary artery disease such as hypertension, hypercholesterolemia, morbid obesity, and diabetes. The relative risk of heart attack for current oral contraceptive users has been estimated to be two to six. The risk is very low under the age of 30.
Smoking in combination with oral contraceptive use has been shown to contribute substantially to the incidence of myocardial infarctions in women in their mid-thirties or older with smoking accounting for the majority of excess cases. Mortality rates associated with circulatory disease have been shown to increase substantially in smokers over the age of 35 and nonsmokers over the age of 40 (Table II) among women who use oral contraceptives.
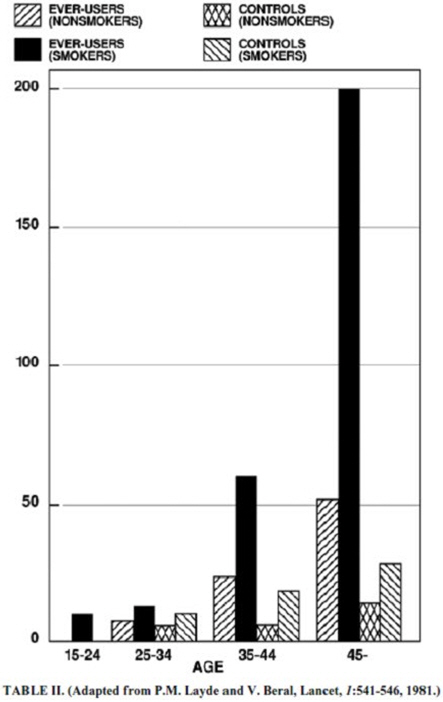
CIRCULATORY DISEASE MORTALITY RATES PER 100,000 WOMAN YEARS BY AGE, SMOKING STATUS AND ORAL CONTRACEPTIVE USE Oral contraceptives may compound the effects of well-known risk factors, such as hypertension, diabetes, hyperlipidemias, age, and obesity. In particular, some progestogens are known to decrease HDL cholesterol and cause glucose intolerance, while estrogens may create a state of hyperinsulinism. Oral contraceptives have been shown to increase blood pressure among users (see section 10 in WARNINGS). Similar effects on risk factors have been associated with an increased risk of heart disease. Oral contraceptives must be used with caution in women with cardiovascular disease risk factors.
b. Thromboembolism
An increased risk of venous thromboembolic and thrombotic disease associated with the use of oral contraceptives is well established. Case control studies have found the relative risk of users compared to non-users to be 3 for the first episode of superficial venous thrombosis, 4 to 11 for deep-vein thrombosis or pulmonary embolism, and 1.5 to 6 for women with predisposing conditions for venous thromboembolic disease. Cohort studies have shown the relative risk to be somewhat lower, about 3 for new cases and about 4.5 for new cases requiring hospitalization. The approximate incidence of deep- vein thrombosis and pulmonary embolism in users of low dose (<50µg ethinyl estradiol) combination oral contraceptives is up to 4 per 10,000 woman-years compared to 0.5 to 3 per 10,000 woman-years for non-users. However, the incidence is substantially less than that associated with pregnancy (6 per 10,000 woman-years). The risk of thromboembolic disease due to oral contraceptives is not related to length of use and disappears after pill use is stopped.
A two- to four-fold increase in relative risk of postoperative thromboembolic complications has been reported with the use of oral contraceptives. The relative risk of venous thrombosis in women who have predisposing conditions is twice that of women without such medical conditions. If feasible, oral contraceptives should be discontinued at least four weeks prior to and for two weeks after elective surgery of a type associated with an increase in risk of thromboembolism and during and following prolonged immobilization. Since the immediate postpartum period is also associated with an increased risk of thromboembolism, oral contraceptives should be started no earlier than four to six weeks after delivery in women who elect not to breast-feed, or a midtrimester pregnancy termination.
c. Cerebrovascular Diseases
Oral contraceptives have been shown to increase both the relative and attributable risks of cerebrovascular events (thrombotic and hemorrhagic strokes), although, in general, the risk is greatest among older (>35 years), hypertensive women who also smoke. Hypertension was found to be a risk factor for both users and non-users, for both types of strokes, while smoking interacted to increase the risk for hemorrhagic strokes.
In a large study, the relative risk of thrombotic strokes has been shown to range from 3 for normotensive users to 14 for users with severe hypertension. The relative risk of hemorrhagic stroke is reported to be 1.2 for nonsmokers who used oral contraceptives, 2.6 for smokers who did not use oral contraceptives, 7.6 for smokers who used oral contraceptives, 1.8 for normotensive users, and 25.7 for users with severe hypertension. The attributable risk is also greater in older women. Oral contraceptives also increase the risk for stroke in women with other underlying risk factors such as certain inherited or acquired thrombophilias, hyperlipidemias, and obesity. Women with migraine (particularly migraine with aura) who take combination oral contraceptives may be at an increased risk of stroke.
d. Dose-Related Risk of Vascular Disease from Oral Contraceptives
A positive association has been observed between the amount of estrogen and progestogen in oral contraceptives and the risk of vascular disease. A decline in serum high-density lipoproteins (HDL) has been reported with many progestational agents. A decline in serum high-density lipoproteins has been associated with an increased incidence of ischemic heart disease. Because estrogens increase HDL cholesterol, the net effect of an oral contraceptive depends on a balance achieved between doses of estrogen and progestogen and the nature and absolute amount of progestogen used in the contraceptive. The amount of both hormones should be considered in the choice of an oral contraceptive.
Minimizing exposure to estrogen and progestogen is in keeping with good principles of therapeutics. For any particular estrogen/progestogen combination, the dosage regimen prescribed should be one which contains the least amount of estrogen and progestogen that is compatible with a low failure rate and the needs of the individual patient. New acceptors of oral contraceptive agents should be started on preparations containing less than 50 mcg of estrogen.
e. Persistence of Risk of Vascular Disease
There are two studies which have shown persistence of risk of vascular disease for ever-users of oral contraceptives. In a study in the United States, the risk of developing myocardial infarction after discontinuing oral contraceptives persists for at least 9 years for women 40 to 49 years who had used oral contraceptives for five or more years, but this increased risk was not demonstrated in other age groups. In another study in Great Britain, the risk of developing cerebrovascular disease persisted for at least 6 years after discontinuation of oral contraceptives, although excess risk was very small.
However, both studies were performed with oral contraceptive formulations containing 50 micrograms or higher of estrogens.
2. Estimate of Mortality from Contraceptive Use
One study gathered data from a variety of sources which have estimated the mortality rate associated with different methods of contraception at different ages (Table III). These estimates include the combined risk of death associated with contraceptive methods plus the risk attributable to pregnancy in the event of method failure. Each method of contraception has its specific benefits and risks. The study concluded that with the exception of oral contraceptive users 35 and older who smoke and 40 and older who do not smoke, mortality associated with all methods of birth control is less than that associated with childbirth. The observation of a possible increase in risk of mortality with age for oral contraceptive users is based on data gathered in the 1970's—but not reported until 1983. However, current clinical practice involves the use of lower estrogen dose formulations combined with careful restriction of oral contraceptive use to women who do not have the various risk factors listed in this labeling.
Because of these changes in practice and, also, because of some limited new data which suggest that the risk of cardiovascular disease with the use of oral contraceptives may now be less than previously observed, the Fertility and Maternal Health Drugs Advisory Committee was asked to review the topic in 1989. The Committee concluded that although cardiovascular disease risks may be increased with oral contraceptive use after age 40 in healthy nonsmoking women (even with the newer low-dose formulations), there are greater potential health risks associated with pregnancy in older women and with the alternative surgical and medical procedures which may be necessary if such women do not have access to effective and acceptable means of contraception.
Therefore, the Committee recommended that the benefits of oral contraceptive use by healthy nonsmoking women over 40 may outweigh the possible risks. Of course, older women, as all women who take oral contraceptives, should take the lowest possible dose formulation that is effective.
TABLE III—ANNUAL NUMBER OF BIRTH-RELATED OR METHOD RELATED DEATHS ASSOCIATED WITH CONTROL OF FERTILITY PER 100,000 NONSTERILE WOMEN, BY FERTILITY-CONTROL METHOD AND ACCORDING TO AGE Method of control and outcome 15-19 20-24 25-29 30-34 35-39 40-44 Adapted from H.W. Ory, Family Planning Perspectives, 15:57-63, 1983. - * Deaths are birth related
- † Deaths are method related
No fertility- control methods* 7.0 7.4 9.1 14.8 25.7 28.2 Oral contraceptives nonsmoker† 0.3 0.5 0.9 1.9 13.8 31.6 Oral contraceptives smoker† 2.2 3.4 6.6 13.5 51.1 117.2 IUD† 0.8 0.8 1.0 1.0 1.4 1.4 Condom* 1.1 1.6 0.7 0.2 0.3 0.4 Diaphragm/ spermicide* 1.9 1.2 1.2 1.3 2.2 2.8 Periodic abstinence* 2.5 1.6 1.6 1.7 2.9 3.6 3. Carcinoma of the Reproductive Organs
A meta-analysis from 54 epidemiological studies reported that there is a slightly increased relative risk (RR=1.24) of having breast cancer diagnosed in women who are currently using combination oral contraceptives compared to never-users. The increased risk gradually disappears during the course of the 10 years after cessation of combination oral contraceptive use. These studies do not provide evidence for causation. The observed pattern of increased risk of breast cancer diagnosis may be due to earlier detection of breast cancer in combination oral contraceptive users, the biological effects of combination oral contraceptives, or a combination of both. Because breast cancer is rare in women under 40 years of age, the excess number of breast cancer diagnoses in current and recent combination oral contraceptive users is small in relation to the lifetime risk of breast cancer. Breast cancers diagnosed in ever-users tend to be less advanced clinically than the cancers diagnosed in never-users.
Some studies suggest that oral contraceptive use has been associated with an increase in the risk of cervical intraepithelial neoplasia or invasive cervical cancer in some populations of women. However, there continues to be controversy about the extent to which such findings may be due to differences in sexual behavior and other factors.
In spite of many studies of the relationship between oral contraceptive use and breast and cervical cancers, a cause-and-effect relationship has not been established.
4. Hepatic Neoplasia
Benign hepatic adenomas are associated with oral contraceptive use, although the incidence of benign tumors is rare in the United States. Indirect calculations have estimated the attributable risk to be in the range of 3.3 cases/100,000 for users, a risk that increases after four or more years of use. Rupture of rare, benign, hepatic adenomas may cause death through intra-abdominal hemorrhage.
Studies from Britain have shown an increased risk of developing hepatocellular carcinoma in long-term (>8 years) oral contraceptive users. However, these cancers are extremely rare in the U.S., and the attributable risk (the excess incidence) of liver cancers in oral contraceptive users approaches less than one per million users.
5. RISK OF LIVER ENZYME ELEVATIONS WITH CONCOMITANT HEPATITIS C TREATMENT
During clinical trials with the Hepatitis C combination drug regimen that contains ombitasvir/paritaprevir/ritonavir, with or without dasabuvir, ALT elevations greater than 5 times the upper limit of normal (ULN), including some cases greater than 20 times the ULN, were significantly more frequent in women using ethinyl estradiol-containing medications such as COCs. Discontinue Levora 0.15/30-28 tablets prior to starting therapy with the combination drug regimen ombitasvir/paritaprevir/ritonavir, with or without dasabuvir [see Contraindications]. Levora 0.15/30-28 tablets can be restarted approximately 2 weeks following completion of treatment with the combination drug regimen.
6. Ocular Lesions
There have been clinical case reports of retinal thrombosis associated with the use of oral contraceptives that may lead to partial or complete loss of vision. Oral contraceptives should be discontinued if there is unexplained partial or complete loss of vision; onset of proptosis or diplopia; papilledema; or retinal vascular lesions. Appropriate diagnostic and therapeutic measures should be undertaken immediately.
7. Oral Contraceptive Use Before or During Early Pregnancy
Extensive epidemiological studies have revealed no increased risk of birth defects in women who have used oral contraceptives prior to pregnancy. Studies also do not suggest a teratogenic effect, particularly insofar as cardiac anomalies and limb-reduction defects are concerned, when taken inadvertently during early pregnancy (see CONTRAINDICATIONS section).
The administration of oral contraceptives to induce withdrawal bleeding should not be used as a test for pregnancy. Oral contraceptives should not be used during pregnancy to treat threatened or habitual abortion.
It is recommended that for any patient who has missed two consecutive periods, pregnancy should be ruled out before continuing oral contraceptive use. If the patient has not adhered to the prescribed schedule, the possibility of pregnancy should be considered at the time of the first missed period. Oral contraceptive use should be discontinued if pregnancy is confirmed.
8. Gallbladder Disease
Earlier studies have reported an increased lifetime relative risk of gallbladder surgery in users of oral contraceptives and estrogens. More recent studies, however, have shown that the relative risk of developing gallbladder disease among oral contraceptive users may be minimal. The recent findings of minimal risk may be related to the use of oral contraceptive formulations containing lower hormonal doses of estrogens and progestogens.
9. Carbohydrate and Lipid Metabolic Effects
Oral contraceptives have been shown to cause glucose intolerance in a significant percentage of users.
Oral contraceptives containing greater than 75 micrograms of estrogens cause hyperinsulinism, while lower doses of estrogen cause less glucose intolerance. Progestogens increase insulin secretion and create insulin resistance, this effect varying with different progestational agents. However, in the nondiabetic woman, oral contraceptives appear to have no effect on fasting blood glucose. Because of these demonstrated effects, prediabetic and diabetic women should be carefully observed while taking oral contraceptives.
A small proportion of women will have persistent hypertriglyceridemia while on the pill. As discussed earlier (see WARNINGS, 1a. and 1d.), changes in serum triglycerides and lipoprotein levels have been reported in oral contraceptive users.
10. Elevated Blood Pressure
An increase in blood pressure has been reported in women taking oral contraceptives, and this increase is more likely in older oral contraceptive users and with continued use. Data from the Royal College of General Practitioners and subsequent randomized trials have shown that the incidence of hypertension increases with increasing quantities of progestogens.
Women with a history of hypertension or hypertension-related diseases, or renal disease, should be encouraged to use another method of contraception. If women with hypertension elect to use oral contraceptives, they should be monitored closely, and if significant elevation of blood pressure occurs, oral contraceptives should be discontinued (see CONTRAINDICATIONS section). For most women, elevated blood pressure will return to normal after stopping oral contraceptives, and there is no difference in the occurrence of hypertension among ever- and never-users.
11. Headache
The onset or exacerbation of migraine or development of headache with a new pattern that is recurrent, persistent, or severe requires discontinuation of oral contraceptives and evaluation of the cause. (See WARNINGS, 1c.)
12. Bleeding Irregularities
Breakthrough bleeding and spotting are sometimes encountered in patients on oral contraceptives, especially during the first three months of use. The type and dose of progestogen may be important. If bleeding persists or recurs, nonhormonal causes should be considered and adequate diagnostic measures taken to rule out malignancy or pregnancy in the event of breakthrough bleeding, as in the case of any abnormal vaginal bleeding. If pathology has been excluded, time or a change to another formulation may solve the problem. In the event of amenorrhea, pregnancy should be ruled out if the oral contraceptive has not been taken according to directions prior to the first missed withdrawal bleed or if two consecutive withdrawal bleeds have been missed.
Some women may encounter post-pill amenorrhea or oligomenorrhea (possibly with anovulation), especially when such a condition was preexistent.
-
PRECAUTIONS
1. General
Patients should be counseled that this product does not protect against HIV infection (AIDS) and other sexually transmitted diseases.
2. Physical Examination and Follow-Up
A periodic personal and family medical history and complete physical examination are appropriate for all women, including women using oral contraceptives. The physical examination, however, may be deferred until after initiation of oral contraceptives if requested by the woman and judged appropriate by the clinician. The physical examination should include special reference to blood pressure, breasts, abdomen and pelvic organs, including cervical cytology, and relevant laboratory tests. In the case of undiagnosed, persistent or recurrent abnormal vaginal bleeding, appropriate measures should be conducted to rule out malignancy. Women with a strong family history of breast cancer or who have breast nodules should be monitored with particular care.
3. Lipid Disorders
Women who are being treated for hyperlipidemias should be followed closely if they elect to use oral contraceptives. Some progestogens may elevate LDL levels and may render the control of hyperlipidemias more difficult. (See WARNINGS, 1d.)
In patients with familial defects of lipoprotein metabolism receiving estrogen-containing preparations, there have been case reports of significant elevations of plasma triglycerides leading to pancreatitis.
4. Liver Function
If jaundice develops in any woman receiving such drugs, the medication should be discontinued. Steroid hormones may be poorly metabolized in patients with impaired liver function.
5. Fluid Retention
Oral contraceptives may cause some degree of fluid retention. They should be prescribed with caution, and only with careful monitoring, in patients with conditions which might be aggravated by fluid retention.
6. Emotional Disorders
Patients becoming significantly depressed while taking oral contraceptives should stop the medication and use an alternate method of contraception in an attempt to determine whether the symptom is drug- related. Women with a history of depression should be carefully observed and the drug discontinued if depression recurs to a serious degree.
7. Contact Lenses
Contact-lens wearers who develop visual changes or changes in lens tolerance should be assessed by an ophthalmologist.
9. Drug Interactions
Interactions between ethinyl estradiol and other substances may lead to decreased or increased serum ethinyl estradiol concentrations. Decreased ethinyl estradiol plasma concentrations may cause an increased incidence of breakthrough bleeding and menstrual irregularities and may possibly reduce efficacy of the combination oral contraceptive.
Combined hormonal contraceptives have been shown to significantly decrease plasma concentrations of lamotrigine when co-administered, likely due to induction of lamotrigine glucuronidation. This may reduce seizure control; therefore, dosage adjustments of lamotrigine may be necessary.
Consult the labeling of concurrently-used drugs to obtain further information about interactions with hormonal contraceptives or the potential for enzyme alterations.
Reduced ethinyl estradiol concentrations have been associated with concomitant use of substances that induce hepatic microsomal enzymes, such as rifampin, rifabutin, barbiturates, phenylbutazone, phenytoin sodium, griseofulvin, topiramate, some protease inhibitors, modafinil, and possibly St. John's wort.
Substances that may decrease plasma ethinyl estradiol concentrations by other mechanisms include any substance that reduces gut transit time and certain antibiotics (e.g. ampicillin and other penicillins, tetracyclines) by a decrease of enterohepatic circulation of estrogens.
During concomitant use of ethinyl estradiol containing products and substances that may lead to decreased plasma steroid hormone concentrations, it is recommended that a nonhormonal back-up method of birth control be used in addition to the regular intake of Levora® 0.15/30-28 (levonorgestrel and ethinyl estradiol tablets). If the use of a substance which leads to decreased ethinyl estradiol plasma concentrations is required for a prolonged period of time, combination oral contraceptives should not be considered the primary contraceptive.
After discontinuation of substances that may lead to decreased ethinyl estradiol plasma concentrations, use of a nonhormonal back-up method of birth control is recommended for 7 days. Longer use of a back-up method is advisable after discontinuation of substances that have led to induction of hepatic microsomal enzymes, resulting in decreased ethinyl estradiol concentrations. It may take several weeks until enzyme induction has completely subsided, depending on dosage, duration of use, and rate of elimination of the inducing substance.
Some substances may increase plasma ethinyl estradiol concentrations. These include:
- Competitive inhibitors for sulfation of ethinyl estradiol in the gastrointestinal wall, such as ascorbic acid (vitamin C) and acetaminophen.
- Substances that inhibit cytochrome P450 3A4 isoenzymes such as indinavir, fluconazole, and troleandomycin. Troleandomycin may increase the risk of intrahepatic cholestasis during coadministration with combination oral contraceptives.
- Atorvastatin (unknown mechanism)
Ethinyl estradiol may interfere with the mechanism of other drugs by inhibiting hepatic microsomal enzymes or by inducing hepatic drug conjugation, particularly glucuronidation. Accordingly, tissue concentrations may be either increased (e.g. cyclosporine, theophylline, corticosteroids) or decreased.
The prescribing information of concomitant medications should be consulted to identify potential interactions.
Concomitant Use with HCV Combination Therapy-Liver Enzyme Elevation
Do not co-administer Levora 0.15/30-28 tablets with HCV drug combinations containing ombitasvir/paritaprevir/ritonavir, with or without dasabuvir, due to potential for ALT elevations (see Warnings, RISK OF LIVER ENZYME ELEVATIONS WITH CONCOMITANT HEPATITIS C TREATMENT).
10. Interactions with Laboratory Tests
Certain endocrine- and liver-function tests and blood components may be affected by oral contraceptives:
- Increased prothrombin and factors VII, VIII, IX, and X; decreased antithrombin 3; increased norepinephrine-induced platelet aggregability.
- Increased thyroid-binding globulin (TBG) leading to increased circulating total thyroid hormone, as measured by protein-bound iodine (PBI), T4 by column or by radioimmunoassay. Free T3 resin uptake is decreased, reflecting the elevated TBG; free T4 concentration is unaltered.
- Other binding proteins may be elevated in serum.
- Sex-binding globulins are increased and result in elevated levels of total circulating sex steroids and corticoids; however, free or biologically active levels remain unchanged.
- Triglycerides may be increased.
- Glucose tolerance may be decreased.
- Serum folate levels may be depressed by oral contraceptive therapy. This may be of clinical significance if a woman becomes pregnant shortly after discontinuing oral contraceptives.
13. Nursing Mothers
Small amounts of oral contraceptive steroids and/or metabolites have been identified in the milk of nursing mothers, and a few adverse effects on the child have been reported, including jaundice and breast enlargement. In addition, combination oral contraceptives given in the postpartum period may interfere with lactation by decreasing the quantity and quality of breast milk. If possible, the nursing mother should be advised not to use combination oral contraceptives but to use other forms of contraception until she has completely weaned her child.
14. Pediatric Use
Safety and efficacy of Levora® 0.15/30-28 (levonorgestrel and ethinyl estradiol tablets) have been established in women of reproductive age. Safety and efficacy are expected to be the same for postpubertal adolescents under the age of 16 and users 16 and older. Use of this product before menarche is not indicated.
- INFORMATION FOR THE PATIENT
-
ADVERSE REACTIONS
An increased risk of the following serious adverse reactions (see WARNINGS section for additional information) has been associated with the use of oral contraceptives:
Thromboembolic disorders and other vascular problems (including thrombophlebitis, arterial thromboembolism, pulmonary embolism, myocardial infarction, cerebral hemorrhage, cerebral thrombosis), carcinoma of the reproductive organs, hepatic neoplasia (including hepatic adenomas or benign liver tumors), ocular lesions (including retinal vascular thrombosis), gallbladder disease, carbohydrate and lipid effects, elevated blood pressure, and headache.
The following adverse reactions have been reported in patients receiving oral contraceptives and are believed to be drug-related:
Nausea
Vomiting Gastrointestinal symptoms (such as abdominal pain, cramps and bloating)
Breakthrough bleeding
Spotting
Change in menstrual flow
Amenorrhea
Temporary infertility after discontinuation of treatment
Edema/fluid retention
Melasma/chloasma which may persist
Breast changes: tenderness, pain, enlargement, secretion
Change in weight or appetite (increase or decrease)
Change in cervical erosion and secretion
Diminution in lactation when given immediately postpartum
Cholestatic jaundice
Rash (allergic)
Mood changes, including depression
Vaginitis, including candidiasis
Change in corneal curvature (steepening)
Intolerance to contact lenses
Mesenteric thrombosis
Decrease in serum folate levels
Exacerbation of systemic lupus erythematosus
Exacerbation of porphyria
Exacerbation of chorea
Aggravation of varicose veins
Anaphylactic/anaphylactoid reactions, including urticaria, angioedema, and severe reactions with respiratory and circulatory symptoms.The following adverse reactions have been reported in users of oral contraceptives, and the association has been neither confirmed nor refuted:
Congenital anomalies
Premenstrual syndrome
Cataracts
Optic neuritis, which may lead to partial or complete loss of vision
Cystitis-like syndrome
Nervousness
Dizziness
Hirsutism
Loss of scalp hair
Erythema multiforme
Erythema nodosum
Hemorrhagic eruption
Impaired renal function
Hemolytic uremic syndrome
Budd-Chiari syndrome
Acne
Changes in libido
Colitis
Sickle-cell disease
Cerebral-vascular disease with mitral valve prolapse
Lupus-like syndromes Pancreatitis
Dysmenorrhea - OVERDOSAGE
-
NONCONTRACEPTIVE HEALTH BENEFITS
The following noncontraceptive health benefits related to the use of oral contraceptives are supported by epidemiological studies which largely utilized oral contraceptive formulations containing doses exceeding 0.035 mg of ethinyl estradiol or 0.05 mg of mestranol.
Effects on menses
Increased menstrual cycle regularity.
Decreased blood loss and decreased incidence of iron-deficiency anemia.
Decreased incidence of dysmenorrhea. -
DOSAGE AND ADMINISTRATION
To achieve maximum contraceptive effectiveness, Levora® 0.15/30-28 (levonorgestrel and ethinyl estradiol tablets, 0.15mg/0.03mg) must be taken exactly as directed and at intervals not exceeding 24 hours.
The dosage of Levora® 0.15/30-28 is one white tablet daily for 21 consecutive days, followed by one peach inert tablet daily for 7 consecutive days, according to prescribed schedule.
It is recommended that tablets be taken at the same time each day, preferably after the evening meal or at bedtime.
During the first cycle of medication, the patient is instructed to begin taking Levora® 0.15/30-28 on the first Sunday after the onset of menstruation. If menstruation begins on a Sunday, the first tablet (white) is taken that day. One white tablet should be taken daily for 21 consecutive days, followed by one peach inert tablet daily for 7 consecutive days. Withdrawal bleeding should usually occur within three days following discontinuation of white tablets and may not have finished before the next pack is started.
During the first cycle, contraceptive reliance should not be placed on Levora® 0.15/30-28 until a white tablet has been taken daily for 7 consecutive days and a nonhormonal back-up method of birth control should be used during those 7 days. The possibility of ovulation and conception prior to initiation of medication should be considered.
The patient begins her next and all subsequent 28-day courses of tablets on the same day of the week (Sunday) on which she began her first course, following the same schedule: 21 days on white tablets—7 days on peach inert tablets. If in any cycle the patient starts tablets later than the proper day, she should protect herself by using another method of birth control until she has taken a white tablet daily for 7 consecutive days.
When the patient is switching from a 21-day regimen of tablets, she should wait 7 days after her last tablet before she starts Levora® 0.15/30-28. She will probably experience withdrawal bleeding during that week. She should be sure that no more than 7 days pass after her previous 21-day regimen. When the patient is switching from a 28-day regimen of tablets, she should start her first pack of Levora® 0.15/30-28 on the day after her last tablet. She should not wait any days between packs. The patient may switch any day from a progestin-only pill and should begin Levora® 0.15/30-28 the next day. If switching from an implant or injection, the patient should start Levora® 0.15/30-28 on the day of implant removal or, if using an injection, the day the next injection would be due. In switching from a progestin- only pill, injection or implant, the patient should be advised to use a nonhormonal back-up method of birth control for the first 7 days of tablet-taking.
If spotting or breakthrough bleeding occurs, the patient is instructed to continue on the same regimen. This type of bleeding is usually transient and without significance; however, if the bleeding is persistent or prolonged, the patient is advised to consult her physician. Although the occurrence of pregnancy is highly unlikely if Levora® 0.15/30-28 is taken according to directions, if withdrawal bleeding does not occur, the possibility of pregnancy must be considered. If the patient has not adhered to the prescribed schedule (missed one or more tablets or started taking them on a day later than she should have), the probability of pregnancy should be considered at the time of the first missed period and appropriate diagnostic measures taken before the medication is resumed. If the patient has adhered to the prescribed regimen and misses two consecutive periods, pregnancy should be ruled out before continuing the contraceptive regimen.
For additional patient instructions regarding missed pills, see the "WHAT TO DO IF YOU MISS PILLS" section in the DETAILED PATIENT LABELING below.
Any time the patient misses two or more white tablets, she should also use another method of contraception until she has taken a white tablet daily for seven consecutive days. If the patient misses one or more peach tablets, she is still protected against pregnancy provided she begins taking white tablets again on the proper day.
If breakthrough bleeding occurs following missed white tablets, it will usually be transient and of no consequence. While there is little likelihood of ovulation occurring if only one or two white tablets are missed, the possibility of ovulation increases with each successive day that scheduled white tablets are missed.
Levora® 0.15/30-28 may be initiated no earlier than day 28 postpartum in the non-lactating mother or after a second trimester abortion due to the increased risk for thromboembolism (see CONTRAINDICATONS, WARNINGS, and PRECAUTIONS concerning thromboembolic disease). The patient should be advised to use a nonhormonal back-up method for the first 7 days of tablet taking. However, if intercourse has already occurred, pregnancy should be excluded before the start of combined oral contraceptive use or the patient must wait for her first menstrual period.
In the case of first trimester abortion, if the patient starts Levora® 0.15/30-28 immediately, additional contraceptive measures are not needed. It is to be noted that early resumption of ovulation may occur if Parlodel® (bromocriptine mesylate) has been used for the prevention of lactation.
-
HOW SUPPLIED
Levora® 0.15/30-28 Tablets (levonorgestrel and ethinyl estradiol, 0.15mg/0.03mg) are available in packages of 6 compact dispensers, each containing 28 Tablets:
21 Active Tablets: White, round, unscored, debossed with 15/30 on one side and WATSON on the other side. 7 Inert Tablets: Peach, round, unscored, debossed with WATSON on one side and P1 on the other side. NDC: 51862-097-01 - SPL UNCLASSIFIED SECTION
-
BRIEF SUMMARY PATIENT PACKAGE INSERT
This product (like all oral contraceptives) is intended to prevent pregnancy. It does not protect against HIV infection (AIDS) and other sexually transmitted diseases.
Oral contraceptives, also known as "birth-control pills" or "the pill," are taken to prevent pregnancy, and when taken correctly, have a failure rate of less than 1% per year when used without missing any pills.
The average failure rate of large numbers of pill users is 5% per year when women who miss pills are included. For most women oral contraceptives are also free of serious or unpleasant side effects. However, forgetting to take pills considerably increases the chances of pregnancy.
For the majority of women, oral contraceptives can be taken safely. But there are some women who are at high risk of developing certain serious diseases that can be life-threatening or may cause temporary or permanent disability or death. The risks associated with taking oral contraceptives increase significantly if you:
- smoke
- have high blood pressure, diabetes, high cholesterol, or a tendency to form blood clots, or are obese
- have or have had clotting disorders, heart attack, stroke, angina pectoris, cancer of the breast or sex organs, jaundice, or malignant or benign liver tumors
You should not take the pill if you suspect you are pregnant or have unexplained vaginal bleeding.
Cigarette smoking increases the risk of serious adverse effects on the heart and blood vessels from oral contraceptive use. This risk increases with age and with the amount of smoking (15 or more cigarettes per day has been associated with a significantly increased risk) and is quite marked in women over 35 years of age. Women who use oral contraceptives should not smoke. Most side effects of the pill are not serious. The most common such effects are nausea, vomiting, bleeding between menstrual periods, weight gain, breast tenderness, and difficulty wearing contact lenses. These side effects, especially nausea and vomiting, may subside within the first three months of use.
The serious side effects of the pill occur very infrequently, especially if you are in good health and do not smoke. However, you should know that the following medical conditions have been associated with or made worse by the pill:
- Blood clots in the legs (thrombophlebitis), lungs (pulmonary embolism), stoppage or rupture of a blood vessel in the brain (stroke), blockage of blood vessels in the heart (heart attack and angina pectoris) or other organs of the body. As mentioned above, smoking increases the risk of heart attacks and strokes and subsequent serious medical consequences. Women with migraine also may be at increased risk of stroke.
- Liver tumors, which may rupture and cause severe bleeding. A possible but not definite association has been found with the pill and liver cancer. However, liver cancers are extremely rare. The chance of developing liver cancer from using the pill is thus even rarer.
- High blood pressure, although blood pressure usually returns to normal when the pill is stopped.
The symptoms associated with these serious side effects are discussed in the detailed leaflet given to you with your supply of pills. Notify your doctor or healthcare provider if you notice any unusual physical disturbances while taking the pill. In addition, drugs such as rifampin, as well as some anticonvulsants and some antibiotics, and possibly St. John's wort, may decrease oral contraceptive effectiveness.
Breast cancer has been diagnosed slightly more often in women who use the pill than in women of the same age who do not use the pill. This very small increase in the number of breast cancer diagnoses gradually disappears during the 10 years after stopping use of the pill. It is not known whether the difference is caused by the pill. It may be that women taking the pill were examined more often, so that breast cancer was more likely to be detected.
Some studies have found an increase in the incidence of cancer or precancerous lesions of the cervix in women who use the pill. However, this finding may be related to factors other than the use of the pill.
Taking the pill provides some important noncontraceptive benefits. These include less painful menstruation, less menstrual blood loss and anemia, fewer pelvic infections, and fewer cancers of the ovary and the lining of the uterus.
Be sure to discuss any medical condition you may have with your healthcare provider. Your healthcare provider will take a medical and family history before prescribing oral contraceptives and will examine you. The physical examination may be delayed to another time if you request it and the healthcare provider believes that it is appropriate to postpone it. You should be reexamined at least once a year while taking oral contraceptives. The detailed patient information leaflet gives you further information which you should read and discuss with your healthcare provider.
This product (like all oral contraceptives) is intended to prevent pregnancy. It does not protect against transmission of HIV (AIDS) and other sexually transmitted diseases such as chlamydia, genital herpes, genital warts, gonorrhea, hepatitis B, and syphilis.
DETAILED PATIENT LABELING
This product (like all oral contraceptives) is intended to prevent pregnancy. It does not protect against HIV infection (AIDS) and other sexually transmitted diseases.
INTRODUCTION
Any woman who considers using oral contraceptives (the birth-control pill or the pill) should understand the benefits and risks of using this form of birth control. This leaflet will give you much of the information you will need to make this decision and will also help you determine if you are at risk of developing any of the serious side effects of the pill. It will tell you how to use the pill properly so that it will be as effective as possible. However, this leaflet is not a replacement for a careful discussion between you and your healthcare provider. You should discuss the information provided in this leaflet with him or her, both when you first start taking the pill and during your revisits. You should also follow your healthcare provider's advice with regard to regular check-ups while you are on the pill.
EFFECTIVENESS OF ORAL CONTRACEPTIVES
Oral contraceptives or "birth-control pills" or "the pill" are used to prevent pregnancy and are more effective than other nonsurgical methods of birth control. When they are taken correctly, the chance of becoming pregnant is less than 1% when used perfectly, without missing any pills. Average failure rates are 5% per year. The chance of becoming pregnant increases with each missed pill during the menstrual cycle.
In comparison, average failure rates for other nonsurgical methods of birth control during the first year of use are as follows:
TABLE: PERCENTAGE OF WOMEN EXPERIENCING AN UNINTENDED PREGNANCY DURING THE FIRST YEAR OF USE OF A CONTRACEPTIVE METHOD Method Perfect Use Average Use NA - not available - * Depending on method (calendar, ovulation, symptothermal, post-ovulation) Adapted from Hatcher RA et al, Contraceptive Technology: 17th Revised Edition. NY, NY: Ardent Media, Inc., 1998.
Levonorgestrel implants 0.05 0.05 Male sterilization 0.1 0.15 Female sterilization 0.5 0.5 Depo-Provera® (injectable progestogen) 0.3 0.3 Oral contraceptives 5 Combined 0.1 NA Progestin only 0.5 NA IUD Progesterone 1.5 2.0 Copper T 380A 0.6 0.8 Condom (male) without spermicide 3 14 (Female) without spermicide 5 21 Cervical cap Never given birth 9 20 Given birth 26 40 Vaginal sponge Never given birth 9 20 Given birth 20 40 Diaphragm with spermicidal cream or jelly 6 20 Spermicides alone (foam, creams, jellies, and vaginal suppositories) 6 26 Periodic abstinence (all methods) 1-9* 25 Withdrawal 4 19 No contraception (planned pregnancy) 85 85 WHO SHOULD NOT TAKE ORAL CONTRACEPTIVES
Cigarette smoking increases the risk of serious adverse effects on the heart and blood vessels from oral contraceptive use. This risk increases with age and with the amount of smoking (15 or more cigarettes per day has been associated with a significantly increased risk) and is quite marked in women over 35 years of age. Women who use oral contraceptives should not smoke. Some women should not use the pill. For example, you should not take the pill if you are pregnant or think you may be pregnant. You should also not use the pill if you have had any of the following conditions:
- Heart attack or stroke
- Blood clots in the legs (thrombophlebitis), lungs (pulmonary embolism), or eyes
- Blood clots in the deep veins of your legs
- Known or suspected breast cancer or cancer of the lining of the uterus, cervix, or vagina, or certain hormonally-sensitive cancers
- Liver tumor (benign or cancerous)
Or, if you have any of the following:
- Chest pain (angina pectoris)
- Unexplained vaginal bleeding (until a diagnosis is reached by your doctor)
- Yellowing of the whites of the eyes or of the skin (jaundice) during pregnancy or during previous use of the pill
- Known or suspected pregnancy
- Heart valve or heart rhythm disorders that may be associated with formation of blood clots
- Diabetes affecting your circulation
- Uncontrolled high blood pressure
- Active liver disease with abnormal liver function tests
- Take any Hepatitis C drug combination containing ombitasvir/paritaprevir/ritonavir, with or without dasabuvir. This may increase levels of the liver enzyme "alanine aminotransferase" (ALT) in the blood.
- Allergy or hypersensitivity to any of the components of Levora® 0.15/30-28 (levonorgestrel and ethinyl estradiol tablets)
Tell your healthcare provider if you have ever had any of these conditions. Your healthcare provider can recommend another method of birth control.
OTHER CONSIDERATIONS BEFORE TAKING ORAL CONTRACEPTIVES
Tell your healthcare provider if you or any family member has ever had:
- Breast nodules, fibrocystic disease of the breast, an abnormal breast X-ray or mammogram
- Diabetes
- Elevated cholesterol or triglycerides
- High blood pressure
- A tendency to form blood clots
- Migraine or other headaches or epilepsy
- Mental depression
- Gallbladder, heart, or kidney disease
- History of scanty or irregular menstrual periods
Women with any of these conditions should be checked often by their healthcare provider if they choose to use oral contraceptives. Also, be sure to inform your doctor or healthcare provider if you smoke or are on any medications.
RISKS OF TAKING ORAL CONTRACEPTIVES
1. Risk of Developing Blood Clots
Blood clots and blockage of blood vessels are the most serious side effects of taking oral contraceptives and can be fatal. In particular, a clot in the legs can cause thrombophlebitis and a clot that travels to the lungs can cause a sudden blocking of the vessel carrying blood to the lungs. Rarely, clots occur in the blood vessels of the eye and may cause blindness, double vision, or impaired vision.
If you take oral contraceptives and need elective surgery, need to stay in bed for a prolonged illness, or have recently delivered a baby, you may be at risk of developing blood clots. You should consult your doctor about stopping oral contraceptives three to four weeks before surgery and not taking oral contraceptives for two weeks after surgery or during bed rest. You should also not take oral contraceptives soon after delivery of a baby or a midtrimester pregnancy termination. It is advisable to wait for at least four weeks after delivery if you are not breast-feeding. If you are breast-feeding, you should wait until you have weaned your child before using the pill. (See also the section on breast- feeding in GENERAL PRECAUTIONS.)
2. Heart Attacks and Strokes
Oral contraceptives may increase the tendency to develop strokes (stoppage or rupture of blood vessels in the brain) and angina pectoris and heart attacks (blockage of blood vessels in the heart). Any of these conditions can cause death or serious disability.
Smoking greatly increases the possibility of suffering heart attacks and strokes. Furthermore, smoking and the use of oral contraceptives greatly increase the chances of developing and dying of heart disease.
Women with migraine (especially migraine with aura) who take oral contraceptives also may be at higher risk of stroke.
3. Gallbladder Disease
Oral contraceptive users probably have a greater risk than non-users of having gallbladder disease, although this risk may be related to pills containing high doses of estrogens.
4. Liver Tumors
In rare cases, oral contraceptives can cause benign but dangerous liver tumors. These benign liver tumors can rupture and cause fatal internal bleeding. In addition, a possible but not definite association has been found with the pill and liver cancers in two studies in which a few women who developed these very rare cancers were found to have used oral contraceptives for long periods. However, liver cancers are extremely rare. The chance of developing liver cancer from using the pill is thus even rarer.
5. Cancer of the Reproductive Organs
Breast cancer has been diagnosed slightly more often in women who use the pill than in women of the same age who do not use the pill. This very small increase in the number of breast cancer diagnoses gradually disappears during the 10 years after stopping use of the pill. It is not known whether the difference is caused by the pill. It may be that women taking the pill were examined more often, so that breast cancer was more likely to be detected.
Some studies have found an increase in the incidence of cancer or precancerous lesions of the cervix in women who use oral contraceptives. However, this finding may be related to factors other than the use of oral contraceptives.
6. Lipid Metabolism and Inflammation of the Pancreas
In patients with inherited defects of lipid metabolism, there have been reports of significant elevations of plasma triglycerides during estrogen therapy. This has led to pancreatitis in some cases.
ESTIMATED RISK OF DEATH FROM A BIRTH CONTROL METHOD OR PREGNANCY
All methods of birth control and pregnancy are associated with a risk of developing certain diseases which may lead to disability or death. An estimate of the number of deaths associated with different methods of birth control and pregnancy has been calculated and is shown in the following table.
ANNUAL NUMBER OF BIRTH-RELATED OR METHOD-RELATED DEATHS ASSOCIATED WITH CONTROL OF FERTILITY PER 100,000 NONSTERILE WOMEN, BY FERTILITY-CONTROL METHOD AND ACCORDING TO AGE Method of control and outcome 15-19 20-24 25-29 30-34 35-39 40-44 - * Deaths are birth related
- † Deaths are method related
No fertility- control methods* 7.0 7.4 9.1 14.8 25.7 28.2 Oral contraceptives nonsmoker† 0.3 0.5 0.9 1.9 13.8 31.6 Oral contraceptives smoker† 2.2 3.4 6.6 13.5 51.1 117.2 IUD† 0.8 0.8 1.0 1.0 1.4 1.4 Condom* 1.1 1.6 0.7 0.2 0.3 0.4 Diaphragm/ spermicide* 1.9 1.2 1.2 1.3 2.2 2.8 Periodic abstinence* 2.5 1.6 1.6 1.7 2.9 3.6 In the above table, the risk of death from any birth control method is less than the risk of childbirth, except for oral contraceptive users over the age of 35 who smoke and pill users over the age of 40 even if they do not smoke. It can be seen in the table that for women aged 15 to 39, the risk of death was highest with pregnancy (7 to 26 deaths per 100,000 women, depending on age). Among pill users who do not smoke, the risk of death was always lower than that associated with pregnancy for any age group, except for those women over the age of 40, when the risk increases to 32 deaths per 100,000 women, compared to 28 associated with pregnancy at that age. However, for pill users who smoke and are over the age of 35, the estimated number of deaths exceeds those for other methods of birth control. If a woman is over the age of 40 and smokes, her estimated risk of death is four times higher (117/100,000 women) than the estimated risk associated with pregnancy (28/100,000 women) in that age group.
The suggestion that women over 40 who don't smoke should not take oral contraceptives is based on information from older high-dose pills and on less-selective use of pills than is practiced today. An Advisory Committee of the FDA discussed this issue in 1989 and recommended that the benefits of oral contraceptive use by healthy, nonsmoking women over 40 years of age may outweigh the possible risks. However, all women, especially older women, are cautioned to use the lowest-dose pill that is effective.
WARNING SIGNALS
If any of these adverse effects occur while you are taking oral contraceptives, call your doctor immediately:
- Sharp chest pain, coughing of blood, or sudden shortness of breath (indicating a possible clot in the lung).
- Pain in the calf (indicating a possible clot in the leg).
- Crushing chest pain or heaviness in the chest (indicating a possible heart attack).
- Sudden severe headache or vomiting, dizziness or fainting, disturbances of vision or speech, weakness, or numbness in an arm or leg (indicating a possible stroke).
- Sudden partial or complete loss of vision (indicating a possible clot in the eye).
- Breast lumps (indicating possible breast cancer or fibrocystic disease of the breast; ask your doctor or healthcare provider to show you how to examine your breasts).
- Severe pain or tenderness in the stomach area (indicating a possibly ruptured liver tumor).
- Difficulty in sleeping, weakness, lack of energy, fatigue, or change in mood (possibly indicating severe depression).
- Jaundice or a yellowing of the skin or eyeballs, accompanied frequently by fever, fatigue, loss of appetite, dark-colored urine, or light-colored bowel movements (indicating possible liver problems).
SIDE EFFECTS OF ORAL CONTRACEPTIVES
- Vaginal Bleeding Irregular vaginal bleeding or spotting may occur while you are taking the pills. Irregular bleeding may vary from slight staining between menstrual periods to breakthrough bleeding which is a flow much like a regular period. Irregular bleeding occurs most often during the first few months of oral contraceptive use, but may also occur after you have been taking the pill for some time. Such bleeding may be temporary and usually does not indicate any serious problems. It is important to continue taking your pills on schedule. If the bleeding occurs in more than one cycle or lasts for more than a few days, talk to your doctor or healthcare provider.
- Contact Lenses If you wear contact lenses and notice a change in vision or an inability to wear your lenses, contact your doctor or healthcare provider.
- Fluid Retention Oral contraceptives may cause edema (fluid retention) with swelling of the fingers or ankles and may raise your blood pressure. If you experience fluid retention, contact your doctor or healthcare provider.
- Melasma A spotty darkening of the skin is possible, particularly of the face.
- Other Side Effects Other side effects may include nausea, breast tenderness, change in appetite, headache, nervousness, depression, dizziness, loss of scalp hair, rash, vaginal infections, inflammation of the pancreas, and allergic reactions.
If any of these side effects bother you, call your doctor or healthcare provider.
GENERAL PRECAUTIONS
1. Missed Periods and Use of Oral Contraceptives Before or During Early Pregnancy
There may be times when you may not menstruate regularly after you have completed taking a cycle of pills. If you have taken your pills regularly and miss one menstrual period, continue taking your pills for the next cycle but be sure to inform your healthcare provider before doing so. If you have not taken the pills daily as instructed and missed a menstrual period, or if you missed two consecutive menstrual periods, you may be pregnant. Check with your healthcare provider immediately to determine whether you are pregnant. Do not continue to take oral contraceptives until you are sure you are not pregnant, but continue to use another method of contraception.
There is no conclusive evidence that oral contraceptive use is associated with an increase in birth defects when taken inadvertently during early pregnancy. Previously, a few studies had reported that oral contraceptives might be associated with birth defects, but these studies have not been confirmed. Nevertheless, oral contraceptives or any other drugs should not be used during pregnancy unless clearly necessary and prescribed by your doctor. You should check with your doctor about risks to your unborn child of any medication taken during pregnancy.
2. While Breast-Feeding
If you are breast-feeding, consult your doctor before starting oral contraceptives. Some of the drug will be passed on to the child in the milk. A few adverse effects on the child have been reported, including yellowing of the skin (jaundice) and breast enlargement. In addition, oral contraceptives may decrease the amount and quality of your milk. If possible, do not use oral contraceptives while breast- feeding. You should use another method of contraception since breast-feeding provides only partial protection from becoming pregnant, and this partial protection decreases significantly as you breast- feed for longer periods of time. You should consider starting oral contraceptives only after you have weaned your child completely.
3. Laboratory Tests
If you are scheduled for any laboratory tests, tell your doctor you are taking birth control pills. Certain blood tests may be affected by birth control pills.
4. Drug Interactions
Certain drugs may interact with birth control pills to make them less effective in preventing pregnancy or cause an increase in breakthrough bleeding. Such drugs include rifampin, drugs used for epilepsy such as barbiturates (for example, phenobarbital) and phenytoin (Dilantin® is one brand of this drug), primidone (Mysoline®), topiramate (Topamax®), phenylbutazone (Butazolidin® is one brand), some drugs used for HIV such as ritonavir (Norvir®), modafinil (Provigil®) and possibly certain antibiotics (such as ampicillin and other penicillins, and tetracyclines) and St. John's wort. You may need to use an additional method of contraception during any cycle in which you take drugs that can make oral contraceptives less effective.
Birth control pills may interact with lamotrigine, an anticonvulsant used for epilepsy. This may increase the risk of seizures, so your physician may need to adjust the dose of lamotrigine.
Some medicines may make birth control pill less effective, including:
- Barbiturates
- Bosentan
- Carbamazepine
- Felbamate
- Griseofulvin
- Oxcarbazepine
- Phenytoin
- Rifampin
- St. John's wort
- Topiramate
As with all prescription products, you should notify your healthcare provider of any other medicines and herbal products you are taking. You may need to use a barrier contraceptive when you take drugs or products that can make birth control pills less effective.
You should inform your healthcare provider about all medicines you are taking, including nonprescription products.
5. Sexually Transmitted Diseases
This product (like all oral contraceptives) is intended to prevent pregnancy. It does not protect against transmission of HIV (AIDS) and other sexually transmitted diseases such as chlamydia, genital herpes, genital warts, gonorrhea, hepatitis B, and syphilis.
HOW TO TAKE THE PILL
IMPORTANT POINTS TO REMEMBER
BEFORE YOU START TAKING YOUR PILLS:
- BE SURE TO READ THESE DIRECTIONS: Before you start taking your pills. Anytime you are not sure what to do.
- THE RIGHT WAY TO TAKE THE PILL IS TO TAKE ONE PILL EVERY DAY AT THE SAME TIME. If you miss pills you could get pregnant. This includes starting the pack late. The more pills you miss, the more likely you are to get pregnant.
- MANY WOMEN HAVE SPOTTING OR LIGHT BLEEDING, OR MAY FEEL SICK TO THEIR STOMACH DURING THE FIRST 1-3 PACKS OF PILLS. If you feel sick to your stomach, do not stop taking the pill. The problem will usually go away. If it doesn't go away, check with your doctor or clinic.
- MISSING PILLS CAN ALSO CAUSE SPOTTING OR LIGHT BLEEDING, even when you make up these missed pills. On the days you take 2 pills to make up for missed pills, you could also feel a little sick to your stomach.
- IF YOU HAVE VOMITING (within 3 to 4 hours after you take your pill), you should follow the instructions for WHAT TO DO IF YOU MISS PILLS. IF YOU HAVE DIARRHEA or IF YOU TAKE SOME MEDICINES, including some antibiotics, your pills may not work as well. Use a back-up method (such as condoms, spermicide, or sponge) until you check with your doctor or clinic.
- IF YOU HAVE TROUBLE REMEMBERING TO TAKE THE PILL, talk to your doctor or clinic about how to make pill taking easier or about using another method of birth control.
- IF YOU HAVE ANY QUESTIONS OR ARE UNSURE ABOUT THE INFORMATION IN THIS LEAFLET, call your doctor or clinic.
BEFORE YOU START TAKING YOUR PILLS
- DECIDE WHAT TIME OF DAY YOU WANT TO TAKE YOUR PILL. It is important to take it at about the same time every day.
- LOOK AT YOUR PILL PACK TO SEE IF IT HAS 28 PILLS: The 28-pill pack has 21 "active" white pills (with hormones) to take for 3 weeks, followed by 1 week of reminder peach pills (without hormones).
- ALSO FIND: 1) where on the pack to start taking pills, and 2) in what order to take the pills (follow the arrows).
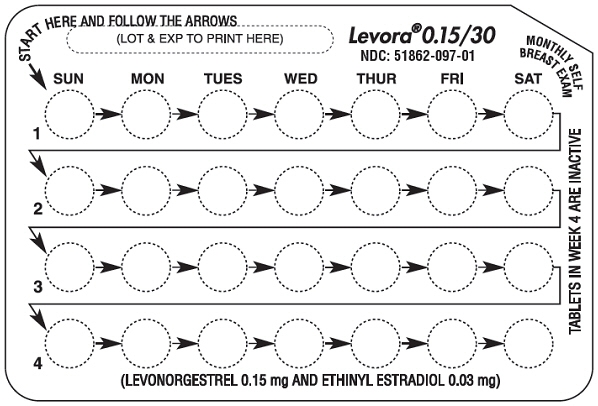
- BE SURE YOU HAVE READY AT ALL TIMES: ANOTHER KIND OF BIRTH CONTROL (such as condoms, spermicide, or sponge) to use as a back-up in case you miss pills. AN EXTRA, FULL PILL PACK.
WHEN TO START THE FIRST PACK OF PILLS
The 28-day pill pack accommodates a SUNDAY START only. Pick a time of day which will be easy to remember.
SUNDAY START:
These instructions are for the 28-day pill pack.
- Take the first "active" white pill of the first pack on the Sunday after your period starts, even if you are still bleeding. If your period begins on Sunday, start the pack that same day.
- Use another method of birth control as a back-up method if you have sex anytime from the Sunday you start your first pack until the next Sunday (7 days). Condoms, spermicide, or the sponge are good back-up methods of birth control.
WHAT TO DO DURING THE MONTH
- TAKE ONE PILL AT THE SAME TIME EVERY DAY UNTIL THE PACK IS EMPTY. Do not skip pills even if you are spotting or bleeding between monthly periods or feel sick to your stomach (nausea). Do not skip pills even if you do not have sex very often.
- WHEN YOU FINISH A PACK OR SWITCH YOUR BRAND OF PILLS: 28 pills: Start the next pack on the day after your last "reminder" pill. Do not wait any days between packs.
WHAT TO DO IF YOU MISS PILLS
The pill may not be as effective if you miss white "active" pills, and particularly if you miss the first few or the last few white "active" pills in a pack.
If you MISS 1 white "active" pill:
- Take it as soon as you remember. Take the next pill at your regular time. This means you may take 2 pills in 1 day.
- You do not need to use a back-up birth control method if you have sex. If you MISS 2 white "active" pills in a row in WEEK 1 OR WEEK 2 of your pack:
- Take 2 pills on the day you remember and 2 pills the next day.
- Then take 1 pill a day until you finish the pack.
- You MAY BECOME PREGNANT if you have sex in the 7 days after you miss pills. You MUST use another birth control method (such as condoms, spermicide, or sponge) as a backup for those 7 days.
If you MISS 2 white "active" pills in a row in THE 3rd WEEK:
The Sunday Starter instructions are for the 28-day pill pack.
- Sunday Starter: Keep taking 1 pill every day until Sunday. On Sunday, THROW OUT the rest of the pack and start a new pack of pills that same day.
- You may not have your period this month but this is expected. However, if you miss your period 2 months in a row, call your doctor or clinic because you might be pregnant.
- You MAY BECOME PREGNANT if you have sex in the 7 days after you miss pills. You MUST use another birth control method (such as condoms, spermicide, or sponge) as a backup for those 7 days.
If you MISS 3 OR MORE white "active" pills in a row (during the first 3 weeks):
The Sunday Starter instructions are for the 28-day pill pack.
- Sunday Starter: Keep taking 1 pill every day until Sunday. On Sunday, THROW OUT the rest of the pack and start a new pack of pills that same day.
- You may not have your period this month but this is expected. However, if you miss your period 2 months in a row, call your doctor or clinic because you might be pregnant.
- You MAY BECOME PREGNANT if you have sex in the 7 days after you miss pills. You MUST use another birth control method (such as condoms, spermicide, or sponge) as a backup for those 7 days.
A REMINDER FOR THOSE ON 28-DAY PACKS
If you forget any of the 7 peach "reminder" pills in Week 4:
THROW AWAY the pills you missed.
Keep taking 1 pill each day until the pack is empty.
You do not need a back-up method if you start your next pack on time.
FINALLY, IF YOU ARE STILL NOT SURE WHAT TO DO ABOUT THE PILLS YOU HAVE MISSED
Use a BACK-UP METHOD anytime you have sex.
KEEP TAKING ONE PILL EACH DAY until you can reach your doctor or clinic.
PREGNANCY DUE TO PILL FAILURE
The incidence of pill failure resulting in pregnancy is approximately less than 1% if taken every day as directed, but average failure rates are 5%. If you do become pregnant, the risk to the fetus is minimal, but you should stop taking your pills and discuss the pregnancy with your doctor.
PREGNANCY AFTER STOPPING THE PILL
There may be some delay in becoming pregnant after you stop using oral contraceptives, especially if you had irregular menstrual cycles before you used oral contraceptives. It may be advisable to postpone conception until you begin menstruating regularly once you have stopped taking the pill and desire pregnancy.
There does not appear to be any increase in birth defects in newborn babies when pregnancy occurs soon after stopping the pill.
OVERDOSAGE
Serious ill effects have not been reported following ingestion of large doses of oral contraceptives by young children. Overdosage may cause nausea and withdrawal bleeding in females. In case of overdosage, contact your healthcare provider or pharmacist.
OTHER INFORMATION
Your healthcare provider will take a medical and family history before prescribing oral contraceptives and will examine you. The physical examination may be delayed to another time if you request it and the healthcare provider believes that it is appropriate to postpone it. You should be reexamined at least once a year. Be sure to inform your healthcare provider if there is a family history of any of the conditions listed previously in this leaflet. Be sure to keep all appointments with your healthcare provider, because this is a time to determine if there are early signs of side effects of oral contraceptive use.
Do not use the drug for any condition other than the one for which it was prescribed. This drug has been prescribed specifically for you; do not give it to others who may want birth control pills.
HEALTH BENEFITS FROM ORAL CONTRACEPTIVES
In addition to preventing pregnancy, use of oral contraceptives may provide certain benefits. They are:
- Menstrual cycles may become more regular.
- Blood flow during menstruation may be lighter, and less iron may be lost. Therefore, anemia due
- to iron deficiency is less likely to occur.
- Pain or other symptoms during menstruation may be encountered less frequently. Ovarian
- cysts may occur less frequently.
- Ectopic (tubal) pregnancy may occur less frequently.
- Noncancerous cysts or lumps in the breast may occur less frequently. Acute
- pelvic inflammatory disease may occur less frequently.
- Oral contraceptive use may provide some protection against developing two forms of cancer: cancer of the ovaries and cancer of the lining of the uterus.
If you want more information about birth control pills, ask your doctor or pharmacist. They have a more technical leaflet called the Professional Labeling which you may wish to read.
Call your doctor for medical advice about side effects. You may need to report side effects to Mayne Pharma at 1-844-825-8500 or to FDA at 1-800-FDA-1088.
Manufactured by:
Patheon Inc.
Mississauga, Ontario L5N 7K9 CanadaDistributed by:
Mayne Pharma
Greenville, NC 27834Revised: April 2017
2000008167
- Levora 0.15/30 Tablets 28-Day Regimen
-
INGREDIENTS AND APPEARANCE
LEVORA
levonorgestrel and ethinyl estradiol kitProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 53002-1565(NDC:51862-097) Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 53002-1565-6 6 in 1 PACKAGE 09/01/2017 1 1 in 1 BLISTER PACK; Type 0: Not a Combination Product 2 NDC: 53002-1565-3 3 in 1 PACKAGE 09/01/2017 2 1 in 1 BLISTER PACK; Type 0: Not a Combination Product 3 NDC: 53002-1565-1 1 in 1 PACKAGE 09/01/2017 3 1 in 1 BLISTER PACK; Type 0: Not a Combination Product Quantity of Parts Part # Package Quantity Total Product Quantity Part 1 21 Part 2 7 Part 1 of 2 LEVORA
levonorgestrel and ethinyl estradiol tabletProduct Information Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength LEVONORGESTREL (UNII: 5W7SIA7YZW) (LEVONORGESTREL - UNII:5W7SIA7YZW) LEVONORGESTREL 0.15 mg ETHINYL ESTRADIOL (UNII: 423D2T571U) (ETHINYL ESTRADIOL - UNII:423D2T571U) ETHINYL ESTRADIOL 0.03 mg Inactive Ingredients Ingredient Name Strength CROSCARMELLOSE SODIUM (UNII: M28OL1HH48) LACTOSE, UNSPECIFIED FORM (UNII: J2B2A4N98G) MAGNESIUM STEARATE (UNII: 70097M6I30) MICROCRYSTALLINE CELLULOSE (UNII: OP1R32D61U) POVIDONE, UNSPECIFIED (UNII: FZ989GH94E) Product Characteristics Color WHITE Score no score Shape ROUND Size 6mm Flavor Imprint Code 15;30;WATSON Contains Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA073594 08/03/2016 Part 2 of 2 INERT
inert tabletProduct Information Route of Administration ORAL Inactive Ingredients Ingredient Name Strength ANHYDROUS LACTOSE (UNII: 3SY5LH9PMK) FD&C YELLOW NO. 6 (UNII: H77VEI93A8) LACTOSE MONOHYDRATE (UNII: EWQ57Q8I5X) Product Characteristics Color ORANGE (peach) Score no score Shape ROUND Size 6mm Flavor Imprint Code WATSON;P1 Contains Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA073594 08/03/2016 Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA073594 08/03/2016 Labeler - RPK Pharmaceuticals, Inc. (147096275) Establishment Name Address ID/FEI Business Operations RPK Pharmaceuticals, Inc. 147096275 RELABEL(53002-1565) , REPACK(53002-1565)
Trademark Results [Levora]
Mark Image Registration | Serial | Company Trademark Application Date |
|---|---|
 LEVORA 74034321 1746284 Live/Registered |
Syntex (F.P.) Inc. 1990-03-05 |
 LEVORA 74020808 not registered Dead/Abandoned |
Syntex General Products, Inc. 1990-01-22 |
© 2026 FDA.report
This site is not affiliated with or endorsed by the FDA.
