Paroxetine by ANI Pharmaceuticals, Inc. / Novitium Pharma LLC PAROXETINE suspension
Paroxetine by
Drug Labeling and Warnings
Paroxetine by is a Prescription medication manufactured, distributed, or labeled by ANI Pharmaceuticals, Inc., Novitium Pharma LLC. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
-
HIGHLIGHTS OF PRESCRIBING INFORMATION
These highlights do not include all the information needed to use PAROXETINE ORAL SUSPENSION safely and effectively. See full prescribing information for PAROXETINE ORAL SUSPENSION.
PAROXETINE oral suspension
Initial U.S. Approval: 1992
WARNING: SUICIDAL THOUGHTS AND BEHAVIORS
See full prescribing information for complete boxed warning.
Increased risk of suicidal thoughts and behavior in pediatric and young adult patients taking antidepressants. Closely monitor all antidepressant-treated patients for clinical worsening and emergence of suicidal thoughts and behaviors. Paroxetine is not approved for use in pediatric patients. (5.1, 8.4)
RECENT MAJOR CHANGES
Warnings and Precautions (5.4) 11/2024
INDICATIONS AND USAGE
Paroxetine is a selective serotonin reuptake inhibitor (SSRI) indicated in adults for the treatment of (1): (1)
- Major Depressive Disorder (MDD)
- Obsessive Compulsive Disorder (OCD)
- Panic Disorder (PD)
- Social Anxiety Disorder (SAD)
- Generalized Anxiety Disorder (GAD)
- Posttraumatic Stress Disorder (PTSD)
DOSAGE AND ADMINISTRATION
- Shake oral suspension well before administration (2.1)
- Recommended starting and maximum daily dosage for MDD, OCD, PD, and PTSD: (2.2)
Indication
Starting Dose
Maximum Dose
MDD
20 mg
50 mg
OCD
20 mg
60 mg
PD
10 mg
60 mg
PTSD
20 mg
50 mg
- Recommended starting dosage for SAD and GAD is 20 mg daily. (2.3)
- Elderly patients, patients with severe renal impairment or severe hepatic impairment: Starting dosage is 10 mg daily. Maximum dosage is 40 mg daily. (2.4)
- When discontinuing paroxetine, reduce dosage gradually. (2.6, 5.7)
DOSAGE FORMS AND STRENGTHS
- Oral suspension: 10 mg/5 mL. (3)
CONTRAINDICATIONS
- Concomitant use of monoamine oxidase inhibitors (MAOIs) or use within 14 days of discontinuing a MAOI. (4, 5.3, 7)
- Concomitant use of pimozide or thioridazine. (4, 5.3,7)
- Known hypersensitivity to paroxetine or to any of the inactive ingredients in paroxetine oral suspension. (4)
WARNINGS AND PRECAUTIONS
- Serotonin Syndrome: Increased risk when co-administered with other serotonergic agents, but also when taken alone. If occurs, discontinue paroxetine oral suspension and serotonergic agents and initiate supportive measures. (5.2)
- Embryofetal Toxicity: May cause fetal harm. Meta-analyses of epidemiological studies have shown increased risk (less than 2-fold) of cardiovascular malformations with exposure during the first trimester. (5.4, 8.1)
- Increased Risk of Bleeding: Concomitant use of aspirin, nonsteroidal anti-inflammatory drugs, other antiplatelet drugs, warfarin, and other anticoagulant drugs may increase risk. (5.5)
- Activation of Mania/Hypomania: Screen patients for bipolar disorder. (5.6)
- Seizures: Use with caution in patients with seizure disorders. (5.8)
- Angle-Closure Glaucoma: Angle-closure glaucoma has occurred in patients with untreated anatomically narrow angles treated with antidepressants. (5.9)
- Sexual Dysfunction: Paroxetine oral suspension may cause symptoms of sexual dysfunction. (5.13)
ADVERSE REACTIONS
Most common adverse reactions (≥5% and at least twice placebo) are abnormal ejaculation, asthenia, constipation, decreased appetite, diarrhea, dizziness, dry mouth, female genital disorder, impotence, infection, insomnia, libido decreased, male genital disorder, nausea, nervousness, somnolence, sweating, tremor, yawn. (6) (6)
To report SUSPECTED ADVERSE REACTIONS, contact Novitium Pharma LLC at 1-855-204-1431 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch. (6)
DRUG INTERACTIONS
- Drugs Highly Bound to Plasma Protein: Monitor for adverse reactions and reduce dosage of paroxetine oral suspension or other protein-bound drugs (e.g., warfarin) as warranted. (7)
- Drugs Metabolized by CYP2D6: Reduce dosage of drugs metabolized by CYP2D6 as warranted. (7)
- Concomitant use with tamoxifen: Consider use of an alternative antidepressant with little or no CYP2D6 inhibition. (5.11, 7)
USE IN SPECIFIC POPULATIONS
- Pregnancy: SSRI use, particularly later in pregnancy, may increase the risk for persistent pulmonary hypertension and symptoms of poor adaptation (respiratory distress, temperature instability, feeding difficulty, hypotonia, irritability) in the neonate. (8.1)
See 17 for PATIENT COUNSELING INFORMATION and Medication Guide.
Revised: 3/2025
-
Table of Contents
FULL PRESCRIBING INFORMATION: CONTENTS*
BOXED WARNING
1 INDICATIONS & USAGE
2 DOSAGE & ADMINISTRATION
2.1 Administration Information
2.2 Recommended Dosage for MDD, OCD, PD, and PTSD
2.3 Recommended Dosage for SAD and GAD
2.4 Screen for Bipolar Disorder Prior to Starting Paroxetine Oral Suspension
2.5 Recommended Dosage for Elderly Patients, Patients with Severe Renal Impairment, and Patients with Severe Hepatic Impairment
2.6 Switching Patients to or From a Monoamine Oxidase Inhibitor (MAOI)
2.7 Discontinuation of Treatment With Paroxetine Oral Suspension
3 DOSAGE FORMS & STRENGTHS
4 CONTRAINDICATIONS
5 WARNINGS AND PRECAUTIONS
5.1 Suicidal Thoughts and Behaviors in Adolescents and Young Adults
5.2 Serotonin Syndrome
5.3 Drug Interactions Leading to QT Prolongation
5.4 Embryofetal Toxicity
5.5 Increased Risk of Bleeding
5.6 Activation of Mania or Hypomania
5.7 Discontinuation Syndrome
5.8 Seizures
5.9 Angle-Closure Glaucoma
5.10 Hyponatremia
5.11 Reduction of Efficacy of Tamoxifen
5.12 Bone Fracture
5.13 Sexual Dysfunction
6 ADVERSE REACTIONS
6.1 Clinical Trials Experience
6.2 Postmarketing Experience
7 DRUG INTERACTIONS
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
8.2 Lactation
8.3 Females and Males of Reproductive Potential
8.4 Pediatric Use
8.5 Geriatric Use
8.6 Renal and Hepatic Impairment
10 OVERDOSAGE
11 DESCRIPTION
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
12.2 Pharmacodynamics
12.3 Pharmacokinetics
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis & Mutagenesis & Impairment Of Fertility
14 CLINICAL STUDIES
14.1 Major Depressive Disorder
14.2 Obsessive Compulsive Disorder
14.3 Panic Disorder
14.4 Social Anxiety Disorder
14.5 Generalized Anxiety Disorder
14.6 Posttraumatic Stress Disorder
16 HOW SUPPLIED/STORAGE AND HANDLING
17 PATIENT COUNSELING INFORMATION
- * Sections or subsections omitted from the full prescribing information are not listed.
-
BOXED WARNING
(What is this?)
BOXED WARNING
WARNING: SUICIDAL THOUGHTS AND BEHAVIORS
Antidepressants increased the risk of suicidal thoughts and behaviors in pediatric and young adult patients in short-term studies. Closely monitor all antidepressant-treated patients for clinical worsening, and for emergence of suicidal thoughts and behaviors [see Warnings and Precautions (5.1)]. Paroxetine is not approved for use in pediatric patients [see Use in Specific Populations (8.4)].
- 1 INDICATIONS & USAGE
-
2 DOSAGE & ADMINISTRATION
2.1 Administration Information
Administer paroxetine oral suspension as a single daily dose in the morning, with or without food.
Shake the oral suspension well before administration.
2.2 Recommended Dosage for MDD, OCD, PD, and PTSD
The recommended starting dosages and maximum dosages of paroxetine oral suspension in patients with MDD, OCD, PD, and PTSD are presented in Table 1.
In patients with an inadequate response, increase dosage in increments of 10 mg per day at intervals of at least 1 week, depending on tolerability.
Table 1: Recommended Daily Dosage of Paroxetine Oral Suspension in Patients with MDD, OCD, PD, and PTSD
Indication
Starting Dose
Maximum Dose
MDD
20 mg
50 mg
OCD
20 mg
60 mg
PD
10 mg
60 mg
PTSD
20 mg
50 mg
2.3 Recommended Dosage for SAD and GAD
SAD
The starting and recommended dosage in patients with SAD is 20 mg daily. In clinical trials the effectiveness of paroxetine oral suspension was demonstrated in patients dosed in a range of 20 mg to 60 mg daily. While the safety of paroxetine oral suspension has been evaluated in patients with SAD at doses up to 60 mg daily, available information does not suggest any additional benefit for doses above 20 mg daily [see Clinical Studies (14.4)].
GAD
The starting and recommended dosage in patients with GAD is 20 mg daily. In clinical trials the effectiveness of paroxetine oral suspension in GAD was demonstrated in patients dosed in a range of 20 mg to 50 mg daily. There is not sufficient evidence to suggest a greater benefit to doses higher than 20 mg daily [see Clinical Studies (14.5)].
In patients with an inadequate response, increase dosage in increments of 10 mg per day at intervals of at least 1 week, depending on tolerability.
2.4 Screen for Bipolar Disorder Prior to Starting Paroxetine Oral Suspension
Prior to initiating treatment with paroxetine oral suspension or another antidepressant, screen patients for a personal or family history of bipolar disorder, mania, or hypomania [see Warnings and Precautions (5.6)].
2.5 Recommended Dosage for Elderly Patients, Patients with Severe Renal Impairment, and Patients with Severe Hepatic Impairment
The recommended initial dosage is 10 mg per day for elderly patients, patients with severe renal impairment, and patients with severe hepatic impairment. Dosage should not exceed 40 mg/day.
2.6 Switching Patients to or From a Monoamine Oxidase Inhibitor (MAOI)
At least 14 days must elapse between discontinuation of a monoamine oxidase inhibitor (MAOI and initiation of paroxetine oral suspension. In addition, at least 14 days must elapse after stopping paroxetine oral suspension before starting an MAOI antidepressant [see Contraindications (4), Warnings and Precautions (5.2)].
- 3 DOSAGE FORMS & STRENGTHS
-
4 CONTRAINDICATIONS
Paroxetine oral suspension is contraindicated in patients:
- Taking, or within 14 days of stopping, MAOIs (including the MAOIs linezolid and intravenous methylene blue) because of an increased risk of serotonin syndrome [see Warnings and Precautions (5.2), Drug Interactions (7)].
- Taking thioridazine because of risk of QT prolongation [see Warnings and Precautions (5.3), Drug Interactions (7)].
- Taking pimozide because of risk of QT prolongation [see Warnings and Precautions (5.3), Drug Interactions (7)].
- With known hypersensitivity (e.g., anaphylaxis, angioedema, Stevens-Johnson syndrome) to paroxetine or any of the inactive ingredients in paroxetine oral suspension [see Adverse Reactions (6.1), (6.2)].
-
5 WARNINGS AND PRECAUTIONS
5.1 Suicidal Thoughts and Behaviors in Adolescents and Young Adults
In pooled analyses of placebo-controlled trials of antidepressant drugs (SSRIs and other antidepressant classes) that included approximately 77,000 adult patients and 4,500 pediatric patients, the incidence of suicidal thoughts and behaviors in antidepressant-treated patients age 24 years and younger was greater than in placebo-treated patients. There was considerable variation in risk of suicidal thoughts and behaviors among drugs, but there was an increased risk identified in young patients for most drugs studied. There were differences in absolute risk of suicidal thoughts and behaviors across the different indications, with the highest incidence in patients with MDD. The drug-placebo differences in the number of cases of suicidal thoughts and behaviors per 1,000 patients treated are provided in Table 2.
Table 2: Risk Differences of the Number of Patients with Suicidal Thoughts and Behaviors in the Pooled Placebo-Controlled Trials of Antidepressants in Pediatric and Adult Patients
Age Range
Drug-Placebo Difference in Number of Patients with Suicidal Thoughts and Behaviors per 1,000 Patients Treated
Increases Compared to Placebo
<18 years old
14 additional cases
18-24 years old
5 additional cases
Decreases Compared to Placebo
25-64 years old
1 fewer case
≥65 years old
6 fewer cases
Paroxetine oral suspension is not approved for use in pediatric patients.
It is unknown whether the risk of suicidal thoughts and behaviors in children, adolescents, and young adults extends to longer-term use, i.e., beyond four months. However, there is substantial evidence from placebo-controlled maintenance trials in adults with MDD that antidepressants delay the recurrence of depression and that depression itself is a risk factor for suicidal thoughts and behaviors.
Monitor all antidepressant-treated patients for any indication for clinical worsening and emergence of suicidal thoughts and behaviors, especially during the initial few months of drug therapy, and at times of dosage changes. Counsel family members or caregivers of patients to monitor for changes in behavior and to alert the healthcare provider. Consider changing the therapeutic regimen, including possibly discontinuing paroxetine oral suspension , in patients whose depression is persistently worse, or who are experiencing emergent suicidal thoughts or behaviors.
5.2 Serotonin Syndrome
SSRIs, including paroxetine, can precipitate serotonin syndrome, a potentially life-threatening condition. The risk is increased with concomitant use of other serotonergic drugs (including triptans, tricyclic antidepressants, fentanyl, lithium, tramadol, meperidine, methadone, tryptophan, buspirone, amphetamines and St. John’s Wort) and with drugs that impair metabolism of serotonin, i.e., MAOIs [see Contraindications (4), Drug Interactions (7.1)]. Serotonin syndrome can also occur when these drugs are used alone.
Serotonin syndrome symptoms may include mental status changes (e.g., agitation, hallucinations, delirium, and coma), autonomic instability (e.g., tachycardia, labile blood pressure, dizziness, diaphoresis, flushing, hyperthermia), neuromuscular symptoms (e.g., tremor, rigidity, myoclonus, hyperreflexia, incoordination), seizures, and/or gastrointestinal symptoms (e.g., nausea, vomiting, diarrhea).
The concomitant use of paroxetine oral suspension with MAOIs is contraindicated. In addition, do not initiate paroxetine oral suspension in a patient being treated with MAOIs such as linezolid or intravenous methylene blue. No reports involved the administration of methylene blue by other routes (such as oral tablets or local tissue injection) or at lower doses. If it is necessary to initiate treatment with an MAOI such as linezolid or intravenous methylene blue in a patient taking paroxetine oral suspension , discontinue paroxetine oral suspension before initiating treatment with the MAOI [see Contraindications (4), Drug Interactions (7)].
Monitor all patients taking paroxetine oral suspension for the emergence of serotonin syndrome. Discontinue treatment with paroxetine oral suspension and any concomitant serotonergic agents immediately if the above symptoms occur, and initiate supportive symptomatic treatment. If concomitant use of paroxetine oral suspension with other serotonergic drugs is clinically warranted, inform patients of the increased risk for serotonin syndrome and monitor for symptoms.
5.3 Drug Interactions Leading to QT Prolongation
The CYP2D6 inhibitory properties of paroxetine can elevate plasma levels of thioridazine and pimozide. Since thioridazine and pimozide given alone produce prolongation of the QTc interval and increase the risk of serious ventricular arrhythmias, the use of paroxetine is contraindicated in combination with thioridazine and pimozide [see Contraindications (4), Drug Interactions (7), Clinical Pharmacology (12.3)].
5.4 Embryofetal Toxicity
Based on meta-analyses of epidemiological studies, exposure to paroxetine in the first trimester of pregnancy is associated with a less than 2-fold increase in the rate of cardiovascular malformations among infants. For women who intend to become pregnant or who are in their first trimester of pregnancy, paroxetine oral suspension should be initiated only after consideration of the other available treatment options [see Use in Specific Populations (8.1)].
5.5 Increased Risk of Bleeding
Drugs that interfere with serotonin reuptake inhibition, including paroxetine, increase the risk of bleeding events. Concomitant use of aspirin, nonsteroidal anti-inflammatory drugs (NSAIDS), other antiplatelet drugs, warfarin, and other anticoagulants may add to this risk. Case reports and epidemiological studies (case-control and cohort design) have demonstrated an association between use of drugs that interfere with serotonin reuptake and the occurrence of gastrointestinal bleeding. Based on data from the published observational studies, exposure to SSRIs, particularly in the month before delivery, has been associated with a less than 2-fold increase in the risk of postpartum hemorrhage [see Use in Specific Populations (8.1)]. Bleeding events related to drugs that interfere with serotonin reuptake have ranged from ecchymoses, hematomas, epistaxis, and petechiae to life-threatening hemorrhages.
Inform patients about the increased risk of bleeding associated with the concomitant use of paroxetine oral suspension and antiplatelet agents or anticoagulants. For patients taking warfarin, carefully monitor the international normalized ratio.
5.6 Activation of Mania or Hypomania
In patients with bipolar disorder, treating a depressive episode with paroxetine oral suspension or another antidepressant may precipitate a mixed/manic episode. During controlled clinical trials of paroxetine oral suspension, hypomania or mania occurred in approximately 1% of paroxetine oral suspension-treated unipolar patients compared to 1.1% of active-control and 0.3% of placebo-treated unipolar patients. Prior to initiating treatment with paroxetine oral suspension, screen patients for any personal or family history of bipolar disorder, mania, or hypomania.
5.7 Discontinuation Syndrome
Adverse reactions after discontinuation of serotonergic antidepressants, particularly after abrupt discontinuation, include: nausea, sweating, dysphoric mood, irritability, agitation, dizziness, sensory disturbances (e.g., paresthesia, such as electric shock sensations), tremor, anxiety, confusion, headache, lethargy, emotional lability, insomnia, hypomania, tinnitus, and seizures. A gradual reduction in dosage rather than abrupt cessation is recommended whenever possible [see Dosage and Administration (2.7)].
During clinical trials of GAD and PTSD, gradual decreases in the daily dose by 10 mg/day at weekly intervals followed by 1 week at 20 mg/day was used before treatment was discontinued. The following adverse reactions were reported at an incidence of 2% or greater for paroxetine and were at least twice that reported for placebo: Abnormal dreams, paresthesia, and dizziness. Adverse reactions have been reported upon discontinuation of treatment with paroxetine in pediatric patients. The safety and effectiveness of paroxetine in pediatric patients have not been established [see Boxed Warning, Warnings and Precautions (5.1), Use in Specific Populations (8.4)].
5.8 Seizures
Paroxetine oral suspension has not been systematically evaluated in patients with seizure disorders. Patients with history of seizures were excluded from clinical studies. During clinical studies, seizures occurred in 0.1% of patients treated with paroxetine. Paroxetine should be prescribed with caution in patients with a seizure disorder. Discontinue paroxetine oral suspension in any patient who develops seizures.
5.9 Angle-Closure Glaucoma
The pupillary dilation that occurs following use of many antidepressant drugs including paroxetine may trigger an angle closure attack in a patient with anatomically narrow angles who does not have a patent iridectomy. Cases of angle-closure glaucoma associated with use of paroxetine have been reported. Avoid use of antidepressants, including paroxetine oral suspension in patients with untreated anatomically narrow angles.
5.10 Hyponatremia
Hyponatremia may occur as a result of treatment with SSRIs, including paroxetine. Cases with serum sodium lower than 110 mmol/L have been reported. Signs and symptoms of hyponatremia include headache, difficulty concentrating, memory impairment, confusion, weakness, and unsteadiness, which may lead to falls. Signs and symptoms associated with more severe and/or acute cases have included hallucination, syncope, seizure, coma, respiratory arrest, and death. In many cases, this hyponatremia appears to be the result of the syndrome of inappropriate antidiuretic hormone secretion (SIADH).
In patients with symptomatic hyponatremia, discontinue paroxetine oral suspension and institute appropriate medical intervention. Elderly patients, patients taking diuretics, and those who are volume-depleted may be at greater risk of developing hyponatremia with SSRIs [see Use in Specific Populations (8.5)].
5.11 Reduction of Efficacy of Tamoxifen
Some studies have shown that the efficacy of tamoxifen, as measured by the risk of breast cancer relapse/mortality, may be reduced with concomitant use of paroxetine oral suspension as a result of paroxetine’s irreversible inhibition of CYP2D6 and lower blood levels of tamoxifen [see Drug Interactions (7)]. One study suggests that the risk may increase with longer duration of coadministration. However, other studies have failed to demonstrate such a risk. When tamoxifen is used for the treatment or prevention of breast cancer, prescribers should consider using an alternative antidepressant with little or no CYP2D6 inhibition.
5.12 Bone Fracture
Epidemiological studies on bone fracture risk during exposure to some antidepressants, including SSRIs, have reported an association between antidepressant treatment and fractures. There are multiple possible causes for this observation and it is unknown to what extent fracture risk is directly attributable to SSRI treatment.
5.13 Sexual Dysfunction
Use of SSRIs, including paroxetine, may cause symptoms of sexual dysfunction [see Adverse Reactions (6.1)]. In male patients, SSRI use may result in ejaculatory delay or failure, decreased libido, and erectile dysfunction. In female patients, SSRI use may result in decreased libido and delayed or absent orgasm. It is important for prescribers to inquire about sexual function prior to initiation of paroxetine oral suspension and to inquire specifically about changes in sexual function during treatment, because sexual function may not be spontaneously reported. When evaluating changes in sexual function, obtaining a detailed history (including timing of symptom onset) is important because sexual symptoms may have other causes, including the underlying psychiatric disorder. Discuss potential management strategies to support patients in making informed decisions about treatment.
-
6 ADVERSE REACTIONS
The following adverse reactions are included in more detail in other sections of the prescribing information:
- Hypersensitivity reactions to paroxetine [see Contraindications (4)]
- Suicidal Thoughts and Behaviors [see Warnings and Precautions (5.1)]
- Serotonin Syndrome [see Warnings and Precautions (5.2)]
- Embryofetal Toxicity [see Warnings and Precautions (5.4)]
- Increased Risk of Bleeding [see Warnings and Precautions (5.5)]
- Activation of Mania/Hypomania [see Warnings and Precautions (5.6)]
- Discontinuation Syndrome [see Warnings and Precautions (5.7)]
- Seizures [see Warnings and Precautions (5.8)]
- Angle-closure Glaucoma [see Warnings and Precautions (5.9)]
- Hyponatremia [see Warnings and Precautions (5.10)]
- Bone Fracture [see Warnings and Precautions (5.12)]
- Sexual Dysfunction [see Warnings and Precautions (5.13)]
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
The safety data for paroxetine are from:
- 6-week clinical trials in MDD patients who received paroxetine 20 mg to 50 mg once daily
- 12-week clinical trials in OCD patients who received paroxetine 20 mg to 60 mg once daily
- 10- to 12-week clinical trials in PD patients who received paroxetine 10 mg to 60 mg once daily
- 12-week clinical trials in SAD patients who received paroxetine 20 mg to 50 mg once daily
- 8-week clinical trials in GAD patients who received paroxetine 10 mg to 50 mg once daily
- 12-week clinical trials in PTSD patients who received paroxetine 20 mg to 50 mg once daily
Adverse Reactions Leading to Discontinuation
Twenty percent (1,199/6,145) of patients treated with paroxetine in clinical trials in MDD and 16.1% (84/522), 11.8% (64/542), 9.4% (44/469), 10.7% (79/735), and 11.7% (79/676) of patients treated with paroxetine in clinical trials in SAD, OCD, PD, GAD, and PTSD, respectively, discontinued treatment due to an adverse reaction. The most common adverse reactions (>1%) associated with discontinuation (i.e., those adverse reactions associated with dropout at a rate approximately twice or greater for paroxetine compared to placebo) are presented in Table 3:
Table 3: Adverse Reactions Reported as Leading to Discontinuation (≥1% of Paroxetine -Treated Patients and Greater than Placebo) in MDD, OCD, PD, SAD, GAD, and PTSD Trials
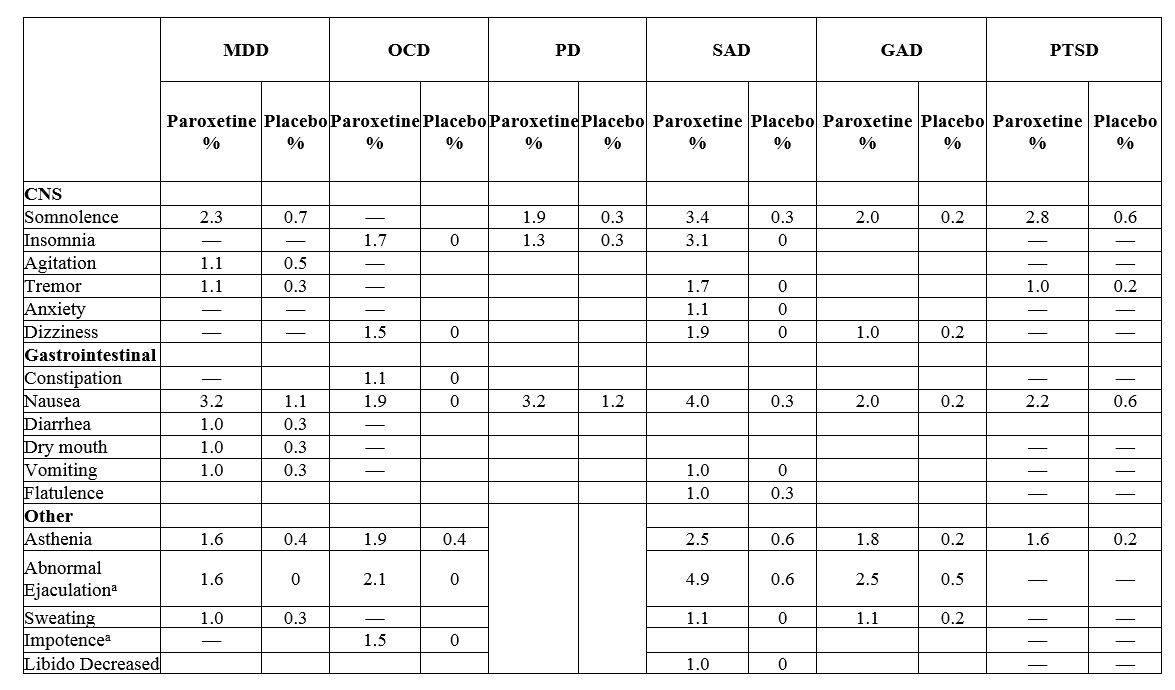
Where numbers are not provided the incidence of the adverse reactions in patients treated with paroxetine was not >1% or was not greater than or equal to 2 times the incidence of placebo.
a. Incidence corrected for gender.
Most Common Adverse Reactions
The most commonly observed adverse reactions associated with the use of paroxetine (incidence of 5% or greater and at least twice that for placebo) were:
MDD: Asthenia, sweating, nausea, decreased appetite, somnolence, dizziness, insomnia, tremor, nervousness, ejaculatory disturbance, and other male genital disorders.
OCD: Nausea, dry mouth, decreased appetite, constipation, dizziness, somnolence, tremor, sweating, impotence, and abnormal ejaculation.
PD: Asthenia, sweating, decreased appetite, libido decreased, tremor, abnormal ejaculation, female genital disorders, and impotence.
SAD: Sweating, nausea, dry mouth, constipation, decreased appetite, somnolence, tremor, libido decreased, yawn, abnormal ejaculation, female genital disorders, and impotence.
GAD: Asthenia, infection, constipation, decreased appetite, dry mouth, nausea, libido decreased, somnolence, tremor, sweating, and abnormal ejaculation.
PTSD: Asthenia, sweating, nausea, dry mouth, diarrhea, decreased appetite, somnolence, libido decreased, abnormal ejaculation, female genital disorders, and impotence.
Adverse Reactions in Patients with MDD
Table 4 presents the adverse reactions that occurred at an incidence of 1% or more and greater than placebo in clinical trials of paroxetine-treated patients with MDD.
Table 4: Adverse Reactions (≥1% of Paroxetine-Treated Patients and Greater than Placebo) in 6-Week Clinical Trials for MDD
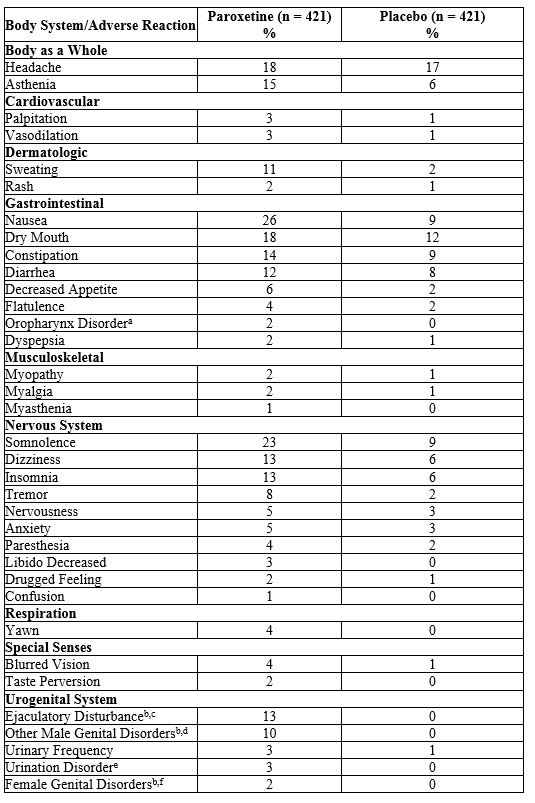
a. Includes mostly “lump in throat” and “tightness in throat.”
b. Percentage corrected for gender.
c. Mostly “ejaculatory delay.”
d. Includes “anorgasmia,” “erectile difficulties,” “delayed ejaculation/orgasm,” and “sexual dysfunction,” and “impotence.”
e. Includes mostly “difficulty with micturition” and “urinary hesitancy.”
f. Includes mostly “anorgasmia” and “difficulty reaching climax/orgasm.”
Adverse Reactions in Patients with OCD, PD, and SAD
Table 5 presents adverse reactions that occurred at a frequency of 2% or more in clinical trials in patients with OCD, PD, and SAD
Table 5. Adverse Reactions (≥2% of Paroxetine-Treated Patients and Greater than Placebo) in 10 to 12-Week Clinical Trials for OCD, PD, and SAD
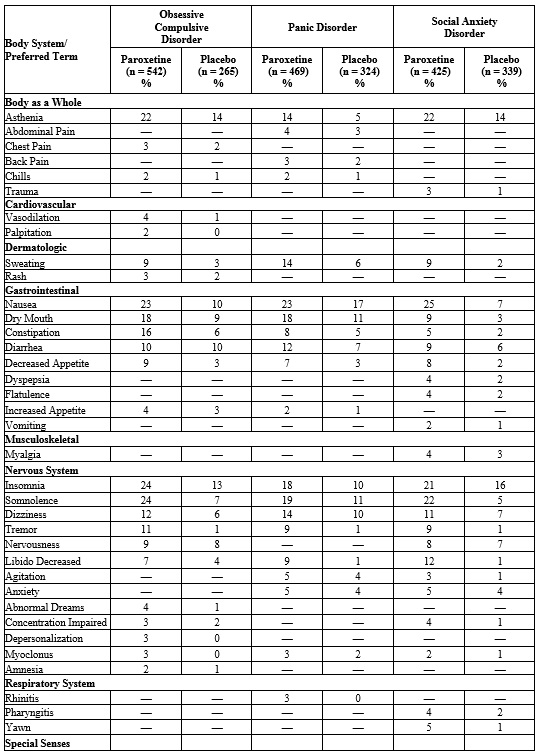
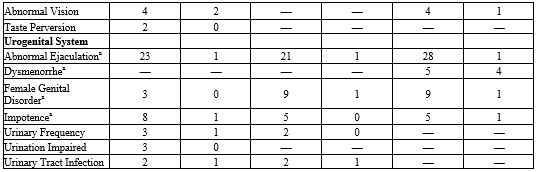
a. Percentage corrected for gender.
Adverse Reactions in Patients with GAD and PTSD
Table 6 presents adverse reactions that occurred at a frequency of 2% or more in clinical trials in patients with GAD and PTSD.
Table 6.Adverse Reactions (≥2% of Paroxetine-Treated Patients and Greater than Placebo) in 8- to 12-Week Clinical Trials for GAD and PTSDa
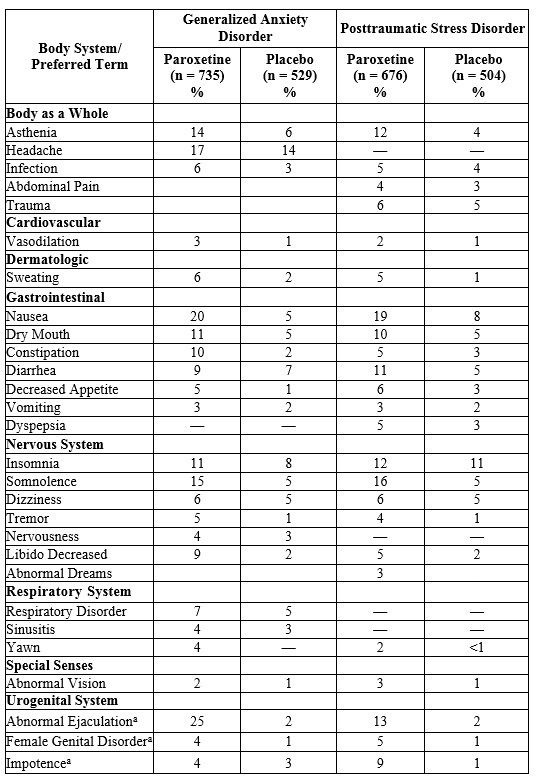
a. Percentage corrected for gender.
Dose Dependent Adverse Reactions
MDD
A comparison of adverse reaction rates in a fixed-dose study comparing paroxetine 10 mg, 20 mg, 30 mg, and 40 mg once daily with placebo in the treatment of MDD revealed dose dependent adverse reactions, as shown in Table 7:
Table 7. Adverse Reactions (≥5% of Paroxetine-Treated Patients and ≥ Twice the Rate of Placebo) in a Dose-Comparison Trial in the Treatment of MDD
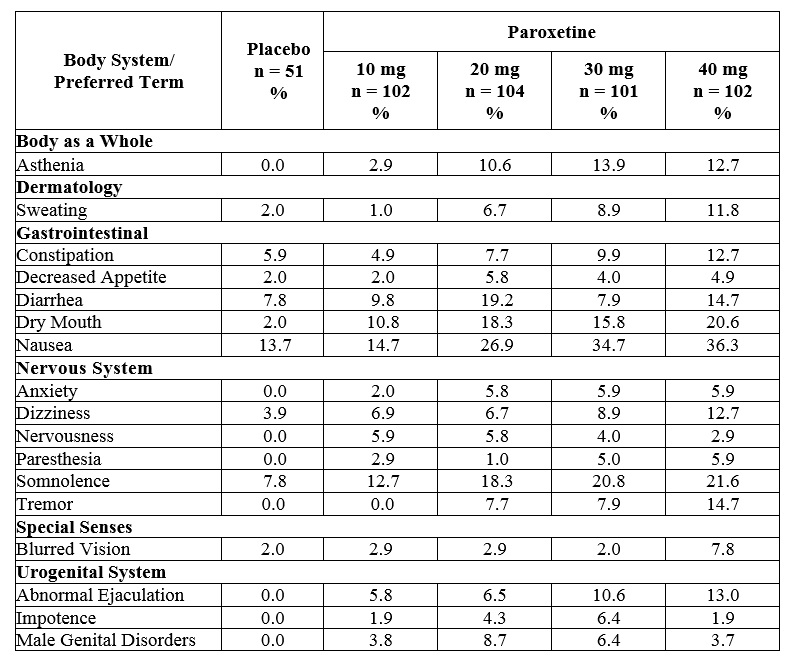
OCDIn a fixed-dose study comparing placebo and paroxetine 20 mg, 40 mg, and 60 mg in the treatment of OCD, there was no clear relationship between adverse reactions and the dose of paroxetine to which patients were assigned.
PD
In a fixed-dose study comparing placebo and paroxetine 10 mg, 20 mg, and 40 mg in the treatment of PD, the following adverse reactions were shown to be dose-dependent: asthenia, dry mouth, anxiety, libido decreased, tremor, and abnormal ejaculation.
SAD
In a fixed-dose study comparing placebo and paroxetine 20 mg, 40 mg and 60 mg in the treatment of SAD, for most of the adverse reactions, there was no clear relationship between adverse reactions and the dose of paroxetine to which patients were assigned.
GAD
In a fixed-dose study comparing placebo and paroxetine 20 mg and 40 mg in the treatment of GAD, the following adverse reactions were shown to be dose-dependent: asthenia, constipation, and abnormal ejaculation.
PTSD
In a fixed-dose study comparing placebo and paroxetine 20 mg and 40 mg in the treatment of PTSD, the following adverse reactions were shown to be dose-dependent: impotence and abnormal ejaculation.
Male and Female Sexual Dysfunction
Although changes in sexual desire, sexual performance, and sexual satisfaction often occur as manifestations of a psychiatric disorder, they may also be a consequence of SSRI treatment. However, reliable estimates of the incidence and severity of untoward experiences involving sexual desire, performance, and satisfaction are difficult to obtain, however, in part because patients and healthcare providers may be reluctant to discuss them. Accordingly, estimates of the incidence of untoward sexual experience and performance cited in labeling may underestimate their actual incidence.
The percentage of patients reporting symptoms of sexual dysfunction in males and females with MDD, OCD, PD, SAD, GAD, and PTSD are displayed in Table 8.
Table 8. Adverse Reactions Related to Sexual Dysfunction in Patients Treated with Paroxetine in Clinical Trials of MDD, OCD, PD, SAD, GAD, and PTSD
Paroxetine
Placebo
n (males)
1446 %
1042 %
Decreased Libido
6 to 15
0 to 5
Ejaculatory Disturbance
13 to 28
0 to 2
Impotence
2 to 9
0 to 3
n (females)
1822 %
1340 %
Decreased Libido
0 to 9
0 to 2
Orgasmic Disturbance
2 to 9
0 to 1
Paroxetine treatment has been associated with several cases of priapism. In those cases with a known outcome, patients recovered without sequelae.
Hallucinations
In pooled clinical trials of paroxetine, hallucinations were observed in 0.2% of paroxetine-treated patients compared to 0.1% of patients receiving placebo.
Less Common Adverse Reactions
The following adverse reactions occurred during the clinical studies of paroxetine and are not included elsewhere in the labeling.
Adverse reactions are categorized by body system and listed in order of decreasing frequency according to the following definitions: Frequent adverse reactions are those occurring on 1 or more occasions in at least 1/100 patients; infrequent adverse reactions are those occurring in 1/100 to 1/1,000 patients; rare adverse reactions are those occurring in fewer than 1/1,000 patients.
Body as a Whole
Infrequent: Allergic reaction, chills, face edema, malaise, neck pain; rare: Adrenergic syndrome, cellulitis, moniliasis, neck rigidity, pelvic pain, peritonitis, sepsis, ulcer.
Cardiovascular System Frequent: Hypertension, tachycardia; infrequent: Bradycardia, hematoma, hypotension, migraine, postural hypotension, syncope; rare: Angina pectoris, arrhythmia nodal, atrial fibrillation, bundle branch block, cerebral ischemia, cerebrovascular accident, congestive heart failure, heart block, low cardiac output, myocardial infarct, myocardial ischemia, pallor,phlebitis, pulmonary embolus, supraventricular extrasystoles, thrombophlebitis, thrombosis, varicose vein, vascular headache, ventricular extrasystoles.
Digestive System
Infrequent: Bruxism, colitis, dysphagia, eructation, gastritis, gastroenteritis, gingivitis, glossitis, increased salivation, abnormal liver function tests, rectal hemorrhage, ulcerative stomatitis; rare: Aphthous stomatitis, bloody diarrhea, bulimia, cardiospasm, cholelithiasis, duodenitis, enteritis, esophagitis, fecal impactions, fecal incontinence, gum hemorrhage, hematemesis, hepatitis, ileitis, ileus, intestinal obstruction, jaundice, melena, mouth ulceration, peptic ulcer, salivary gland enlargement, sialadenitis, stomach ulcer, stomatitis, tongue discoloration, tongue edema, tooth caries.
Endocrine System
Rare: Diabetes mellitus, goiter, hyperthyroidism, hypothyroidism, thyroiditis.
Hemic and Lymphatic SystemsInfrequent: Anemia, leukopenia, lymphadenopathy, purpura; rare: Abnormal erythrocytes, basophilia, bleeding time increased, eosinophilia, hypochromic anemia, iron deficiency anemia, leukocytosis, lymphedema, abnormal lymphocytes, lymphocytosis, microcytic anemia, monocytosis, normocytic anemia, thrombocythemia, thrombocytopenia.
Metabolic and Nutritional
Frequent: Weight gain; infrequent: Edema, peripheral edema, SGOT increased, SGPT increased, thirst, weight loss; rare: Alkaline phosphatase increased, bilirubinemia, BUN increased, creatinine phosphokinase increased, dehydration, gamma globulins increased, gout, hypercalcemia, hypercholesteremia, hyperglycemia, hyperkalemia, hyperphosphatemia, hypocalcemia, hypoglycemia, hypokalemia, hyponatremia, ketosis, lactic dehydrogenase increased, non-protein nitrogen (NPN) increased.
Musculoskeletal System
Frequent: Arthralgia; infrequent: Arthritis, arthrosis; rare: Bursitis, myositis, osteoporosis, generalized spasm, tenosynovitis, tetany.
Nervous System
Frequent: Emotional lability, vertigo; infrequent: Abnormal thinking, alcohol abuse, ataxia, dystonia, dyskinesia, euphoria, hostility, hypertonia, hypesthesia, hypokinesia, incoordination, lack of emotion, libido increased, manic reaction, neurosis, paralysis, paranoid reaction; rare: Abnormal gait, akinesia, antisocial reaction, aphasia, choreoathetosis, circumoral paresthesias, convulsion, delirium, delusions, diplopia, drug dependence, dysarthria, extrapyramidal syndrome, fasciculations, grand mal convulsion, hyperalgesia, hysteria, manic-depressivereaction, meningitis, myelitis, neuralgia, neuropathy, nystagmus, peripheral neuritis, psychotic depression, psychosis, reflexes decreased, reflexes increased, stupor, torticollis, trismus, withdrawal syndrome.
Respiratory System
Infrequent: Asthma, bronchitis, dyspnea, epistaxis, hyperventilation, pneumonia, respiratory flu; rare: Emphysema, hemoptysis, hiccups, lung fibrosis, pulmonary edema, sputum increased, stridor, voice alteration.
Skin and Appendages
Frequent: Pruritus; infrequent: Acne, alopecia, contact dermatitis, dry skin, ecchymosis, eczema, herpes simplex, photosensitivity, urticaria; rare: Angioedema, erythema nodosum, erythema multiforme, exfoliative dermatitis, fungal dermatitis, furunculosis; herpes zoster, hirsutism, maculopapular rash, seborrhea, skin discoloration, skin hypertrophy, skin ulcer, sweating decreased, vesiculobullous rash.
Special SensesFrequent: Tinnitus; infrequent: Abnormality of accommodation, conjunctivitis, ear pain, eye pain, keratoconjunctivitis, mydriasis, otitis media; rare: Amblyopia, anisocoria, blepharitis, cataract, conjunctival edema, corneal ulcer, deafness, exophthalmos, eye hemorrhage, glaucoma, hyperacusis, night blindness, otitis externa, parosmia, photophobia, ptosis, retinal hemorrhage, taste loss, visual field defect.
Urogenital System
Infrequent: Amenorrhea, breast pain, cystitis, dysuria, hematuria, menorrhagia, nocturia, polyuria, pyuria, urinary incontinence, urinary retention, urinary urgency, vaginitis; rare: Abortion, breast atrophy, breast enlargement, endometrial disorder, epididymitis, female lactation, fibrocystic breast, kidney calculus, kidney pain, leukorrhea, mastitis, metrorrhagia, nephritis, oliguria, salpingitis, urethritis, urinary casts, uterine spasm, urolith, vaginal hemorrhage, vaginal moniliasis.
6.2 Postmarketing Experience
The following reactions have been identified during post approval use of paroxetine. Because these reactions are reported voluntarily from a population of unknown size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Acute pancreatitis, elevated liver function tests (the most severe cases were deaths due to liver necrosis, and grossly elevated transaminases associated with severe liver dysfunction), Guillain-Barré syndrome, Stevens-Johnson syndrome, toxic epidermal necrolysis, drug reaction with eosinophilia and systemic symptoms (DRESS), syndrome of inappropriate ADH secretion, prolactinemia and galactorrhea; extrapyramidal symptoms which have included akathisia, bradykinesia, cogwheel rigidity, oculogyric crisis which has been associated with concomitant use of pimozide; status epilepticus, acute renal failure, pulmonary hypertension, allergic alveolitis, anosmia, hyposmia, anaphylaxis, eclampsia, laryngismus, optic neuritis, porphyria, restless legs syndrome (RLS), ventricular fibrillation, ventricular tachycardia (including torsade de pointes), hemolytic anemia, events related to impaired hematopoiesis (including aplastic anemia, pancytopenia, bone marrow aplasia, and agranulocytosis), vasculitic syndromes (such as Henoch-Schönlein purpura), and premature births in pregnant women. There has been a case report of severe hypotension when paroxetine was added to chronic metoprolol treatment.
-
7 DRUG INTERACTIONS
Table 9 presents clinically significant drug interactions with paroxetine.
Table 9: Clinically Significant Drug Interactions with Paroxetine
Monoamine Oxidase Inhibitors (MAOIs)
Clinical Impact
The concomitant use of SSRIs, including paroxetine, and MAOIs increases the risk of serotonin syndrome.
Intervention
Paroxetine is contraindicated in patients taking MAOIs, including MAOIs such as linezolid or intravenous methylene blue [see Dosage and Administration (2.5), Contraindications (4), Warnings and Precautions (5.2)].
Examples
selegiline, tranylcypromine, isocarboxazid, phenelzine, linezolid, methylene blue
Pimozide and Thioridazine
Clinical Impact
Increased plasma concentrations of pimozide and thioridazine, drugs with a narrow therapeutic index, may increase the risk of QTc prolongation and ventricular arrhythmias.
Intervention
Paroxetine is contraindicated in patients taking pimozide or thioridazine [see Contraindications (4)].
Other Serotonergic Drugs
Clinical Impact
The concomitant use of serotonergic drugs with paroxetine increases the risk of serotonin syndrome.
Intervention
Monitor patients for signs and symptoms of serotonin syndrome, particularly during treatment initiation and dosage increases. If serotonin syndrome occurs, consider discontinuation of paroxetine and/or concomitant serotonergic drugs [see Warnings and Precautions (5.2)].
Examples
other SSRIs, SNRIs, triptans, tricyclic antidepressants, opioids, lithium, tryptophan, buspirone, amphetamines, and St. John’s Wort
Drugs that Interfere with Hemostasis (antiplatelet agents and anticoagulants)
Clinical Impact
Theconcurrentuse of anantiplateletagentoranticoagulant with paroxetine maypotentiate the risk ofbleeding.
Intervention
Informpatientsofthe increasedrisk of bleedingassociated with the concomitantuse ofparoxetine andantiplateletagentsand anticoagulants. For patients takingwarfarin,carefullymonitor the international normalizedratio [seeWarningsand Precautions(5.5)].
Examples
aspirin, clopidogrel, heparin,warfarin
Drugs HighlyBound toPlasmaProtein
Clinical Impact
Paroxetine is highlybound to plasma protein. The concomitant useof paroxetine with another drugthat ishighlyboundto plasma protein may increasefreeconcentrationsofparoxetine or othertightly-bound drugs in plasma.
Intervention
Monitor foradversereactionsandreducedosageof paroxetine orother protein-bound drugs as warranted.
Examples
warfarin
Drugs Metabolized by CYP2D6
Clinical Impact
Paroxetine is a CYP2D6inhibitor [see Clinical Pharmacology(12.3)].The concomitant use of paroxetine with a CYP2D6substrate may increasetheexposure of the CYP2D6substrate.
Intervention
Decreasethe dosage of a CYP2D6substrate if neededwith concomitantparoxetine use.Conversely,anincreaseindosageof a CYP2D6substratemay be needed if paroxetine is discontinued.
Examples
propafenone,flecainide,atomoxetine, desipramine, dextromethorphan,metoprolol,nebivolol,perphenazine,tolterodine,venlafaxine, risperidone.
Tamoxifen
Clinical Impact
Concomitant use oftamoxifen with paroxetine maylead to reduced plasmaconcentrations ofthe active metabolite (endoxifen)andreducedefficacyoftamoxifen.
Intervention
Consideruse ofanalternativeantidepressantwithlittle or noCYP2D6 inhibition [seeWarningsand Precautions(5.11)].
Fosamprenavir/Ritonavir
Clinical Impact
Co-administration of fosamprenavir/ritonavir withparoxetine significantly decreased plasmalevels of paroxetine.
Intervention
Anydose adjustment should be guidedbyclinicaleffect (tolerabilityandefficacy).
-
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Pregnancy Exposure Registry
There is a pregnancy exposure registry that monitors pregnancy outcomes in women exposed to antidepressants, including paroxetine, during pregnancy. Healthcare providers are encouraged to advise patients to register by calling the National Pregnancy Registry for Antidepressants 1-866- 961-2388 or visiting online at https://womensmentalhealth.org/ clinical-and-research-programs/pregnancyregistry/antidepressants/.
Risk Summary
Based on data from published observational studies, exposure to SSRIs, particularly in the month before delivery, has been associated with a less than 2-fold increase in the risk of postpartum hemorrhage [see Warnings and Precautions (5.5) and Clinical Considerations].
Paroxetine is associated with a less than 2-fold increase in cardiovascular malformations when administered to a pregnant woman during the first trimester. While individual epidemiological studies on the association between paroxetine use and cardiac malformations have reported inconsistent findings, some meta-analyses of epidemiological studies have identified an increased risk of cardiovascular malformations (see Data). There are risks of persistent pulmonary hypertension of the newborn (PPHN) (see Data) and/or poor neonatal adaptation with exposure to selective serotonin reuptake inhibitors (SSRIs), including paroxetine during pregnancy. There also are risks associated with untreated depression in pregnancy (see Clinical Considerations). For women who intend to become pregnant or who are in their first trimester of pregnancy, paroxetine should be initiated only after consideration of the other available treatment options.
No evidence of treatment related malformations was observed in animal reproduction studies, when paroxetine was administered during the period of organogenesis at doses up to 50 mg/kg/day in rats and 6 mg/kg/day in rabbits. These doses are approximately 8 (rat) and less than 2 (rabbit) times the maximum recommended human dose (MRHD – 60 mg) on an mg/m2 basis. When paroxetine was administered to female rats during the last trimester of gestation and continued through lactation, there was an increase in the number of pup deaths during the first four days of lactation. This effect occurred at a dose of 1 mg/kg/day which is less than the MRHD on an mg/m2 basis (See Data).
The background risks of major birth defects and miscarriage for the indicated populations are unknown. All pregnancies have a background risk of birth defect, loss, or other adverse outcomes. In the US general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2 to 4% and 15 to 20%, respectively.
Clinical Considerations
Disease-associated maternal and/or embryofetal risk
Women who discontinue antidepressants during pregnancy are more likely to experience a relapse of major depression than women who continue antidepressants. This finding is from a prospective, longitudinal study of 201 pregnant women with a history of major depressive disorder who were euthymic and taking antidepressants at the beginning of pregnancy. Consider the risk of untreated depression when discontinuing or changing treatment with antidepressant medication during pregnancy and the postpartum.
Maternal Adverse Reactions
Use of paroxetine in the month before delivery may be associated with an increased risk of postpartum hemorrhage [see Warnings and Precautions (5.5)].
Fetal/Neonatal adverse reactions
Neonates exposed to paroxetine and other SSRIs late in the third trimester have developed complications requiring prolonged hospitalization, respiratory support, and tube feeding. Such complications can arise immediately upon delivery. Reported clinical findings have included respiratory distress, cyanosis, apnea, seizures, temperature instability, feeding difficulty, vomiting, hypoglycemia, hypotonia, hypertonia, hyperreflexia, tremors, jitteriness, irritability, and constant crying. These findings are consistent with either a direct toxic effect of SSRIs or possibly a drug discontinuation syndrome. It should be noted that, in some cases, the clinical picture is consistent with serotonin syndrome [see Warnings and Precautions (5.2)].
Data
Human Data
Published epidemiological studies on the association between first trimester paroxetine use and cardiovascular malformations have reported inconsistent results; however, meta-analyses of population-based cohort studies published between 1996 – 2017 indicate a less than 2-fold increased risk for overall cardiovascular malformations. Specific cardiac malformations identified in two meta-analyses include an approximately 2 to 2.5-fold increased risk for right ventricular outflow tract defects. One meta-analysis also identified an increased risk (less than 2-fold) for bulbus cordis anomalies and anomalies of cardiac septal closure, and an increased risk for atrial septal defect (pooled OR 2.38, 95% CI 1.14-4.97). Important limitations of the studies included in these meta-analyses include potential confounding by indication, depression severity, and potential exposure misclassification.
Exposure to SSRIs, particularly later in pregnancy, may have an increased risk for PPHN. PPHN occurs in 1-2 per 1000 live births in the general population and is associated with substantial neonatal morbidity and mortality.
Animal Data
Reproduction studies were performed at doses up to 50 mg/kg/day in rats and 6 mg/kg/day in rabbits administered during organogenesis. These doses are approximately 8 (rat) and less than 2 (rabbit) times the maximum recommended human dose (MRHD – 60 mg) on an mg/m2 basis. These studies have revealed no evidence of developmental effects. However, in rats, there was an increase in pup deaths during the first 4 days of lactation when dosing occurred during the last trimester of gestation and continued throughout lactation. This effect occurred at a dose of 1 mg/kg/day which is less than the MRHD on an mg/m2 basis. The no-effect dose for rat pup mortality was not determined. The cause of these deaths is not known.
8.2 Lactation
Risk Summary
Data from the published literature report the presence of paroxetine in human milk (see Data). There are reports of agitation, irritability, poor feeding and poor weight gain in infants exposed to paroxetine through breast milk (see Clinical Considerations). There are no data on the effect of paroxetine on milk production. The developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for paroxetine and any potential adverse effects on the breastfed child from paroxetine or from underlying maternal condition.
Clinical Considerations
Infants exposed to paroxetine should be monitored for agitation, irritability, poor feeding and poor weight gain.
Data
Published literature suggests the presence of paroxetine in human milk with relative infant doses ranging between 0.4% to 2.2%, and a milk/plasma ratio of <1. No significant amounts were detected in the plasma of infants after breastfeeding.
8.3 Females and Males of Reproductive Potential
Infertility
Male
Based on findings from clinical studies, paroxetine may affect sperm quality which may impair fertility; it is not known if this effect is reversible [see Nonclinical Toxicology (13.1)].
8.4 Pediatric Use
The safety and effectiveness of paroxetine oral suspension in pediatric patients have not been established [see Box Warning]. Effectiveness was not demonstrated in three placebo-controlled trials in 752 paroxetine-treated pediatric patients with MDD.
Antidepressants increase the risk of suicidal thoughts and behaviors in pediatric patients [see Boxed Warning, Warnings and Precautions (5.1)]. Decreased appetite and weight loss have been observed in association with the use of SSRIs.
In placebo-controlled clinical trials conducted with pediatric patients, the following adverse reactions were reported in at least 2% of pediatric patients treated with paroxetine and occurred at a rate at least twice that for pediatric patients receiving placebo: emotional lability (including self-harm, suicidal thoughts, attempted suicide, crying, and mood fluctuations), hostility, decreased appetite, tremor, sweating, hyperkinesia, and agitation.
Adverse reactions upon discontinuation of treatment with paroxetine in the pediatric clinical trials that included a taper phase regimen, which occurred in at least 2% of patients and at a rate at least twice that of placebo, were: emotional lability (including suicidal ideation, suicide attempt, mood changes, and tearfulness), nervousness, dizziness, nausea, and abdominal pain.
8.5 Geriatric Use
In premarketing clinical trials with paroxetine, 17% of patients treated with paroxetine (approximately 700) were 65 years of age or older. Pharmacokinetic studies revealed a decreased clearance in the elderly, and a lower starting dose is recommended; however, no overall differences in safety or effectiveness were observed between elderly and younger patients [see Dosage and Administration (2.4), Clinical Pharmacology (12.3)].
SSRIs including paroxetine, have been associated with cases of clinically significant hyponatremia in elderly patients, who may be at greater risk for this adverse reaction [see Warnings and Precautions (5.7)].
8.6 Renal and Hepatic Impairment
Increased plasma concentrations of paroxetine oral suspension occur in patients with renal and hepatic impairment. The initial dosage of paroxetine oral suspension should be reduced in patients with severe renal impairment and in patients with severe hepatic impairment [see Dosage and Administration (2.4), Clinical Pharmacology (12.3)].
-
10 OVERDOSAGE
The following have been reported with paroxetine overdosage:
- Seizures, which may be delayed, and altered mental status including coma.
- Cardiovascular toxicity, which may be delayed, including QRS and QTc interval prolongation. Hypertension most commonly seen, but rarely can see hypotension alone or with co-ingestants including alcohol.
- Serotonin syndrome (patients with a multiple drug overdosage with other proserotonergic drugs may have a higher risk).
Gastrointestinal decontamination with activated charcoal should be considered in patients who present early after a paroxetine overdose.
Consider contacting a poison center (1-800-222-1222) or a medical toxicologist for additional overdosage management recommendations.
-
11 DESCRIPTION
Paroxetine Oral Suspension contains paroxetine hydrochloride, an SSRI. It is the hydrochloride salt of a phenylpiperidine compound identified chemically as (-)-trans-4R-(4'-fluorophenyl)-3S-[(3',4'methylenedioxyphenoxy) methyl] piperidine hydrochloride hemihydrate and has the empirical formula of C19H20FNO3HCl1/2H2O. The molecular weight is 374.8 (329.4 as free base). The structural formula of paroxetine hydrochloride is:
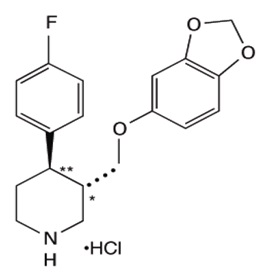
Paroxetine hydrochloride is an odorless, off-white powder, having a melting point range of 120° to 138°C and a solubility of 5.4 mg/mL in water.
Paroxetine Oral Suspension
Paroxetine Oral Suspension is for oral administration. Each 5 mL contains 10 mg of paroxetine equivalent to 11.1 mg of paroxetine hydrochloride.
Inactive ingredients consist of polacrilin potassium, microcrystalline cellulose, carboxymethyl cellulose sodium, propylene glycol, glycerin, sorbitol, methylparaben, propylparaben, sodium citrate dihydrate, citric acid anhydrous, sodium saccharin, orange flavor (triacetin, propylene glycol, natural and artificial flavor), FD&C Yellow No. 6, simethicone emulsion and purified water.
-
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
The mechanism of action of paroxetine in the treatment of MDD, SAD, OCD, PD, GAD, and PTSD is unknown, but is presumed to be linked to potentiation of serotonergic activity in the central nervous system resulting from inhibition of neuronal reuptake of serotonin (5-hydroxy-tryptamine, 5-HT).
12.2 Pharmacodynamics
Studies at clinically relevant doses in humans have demonstrated that paroxetine blocks the uptake of serotonin into human platelets. In vitro studies in animals also suggest that paroxetine is a potent and highly selective inhibitor of neuronal serotonin reuptake (SSRI) and has only very weak effects on norepinephrine and dopamine neuronal reuptake.
12.3 Pharmacokinetics
Nonlinearity in pharmacokinetics is observed with increasing doses of paroxetine.
In a meta-analysis of paroxetine from 4 studies done in healthy volunteers following multiple dosing of 20 mg/day to 40 mg/day, males did not exhibit a significantly lower Cmax or AUC than females.
Absorption
Paroxetine hydrochloride is completely absorbed after oral dosing of a solution of the hydrochloride salt. In a study in which normal male subjects (n = 15) received 30 mg tablets daily for 30 days, steady-state paroxetine concentrations were achieved by approximately 10 days for most subjects, although it may take substantially longer in an occasional patient. At steady state, mean values of Cmax, Tmax, Cmin, and T½ were 61.7 ng/mL (CV 45%), 5.2 hr. (CV 10%), 30.7 ng/mL (CV 67%), and 21 hours (CV 32%), respectively. The steady-state Cmax and Cmin values were about 6 and 14 times what would be predicted from single-dose studies. Steady-state drug exposure based on AUC0-24 was about 8 times greater than would have been predicted from single-dose data in these subjects. The excess accumulation is a consequence of the fact that 1 of the enzymes that metabolizes paroxetine is readily saturable.
Paroxetine is equally bioavailable from the oral suspension and tablet.
Effect of Food
The effects of food on the bioavailability of paroxetine were studied in subjects administered a single dose with and without food. AUC was only slightly increased (6%) when drug was administered with food but the Cmax was 29% greater, while the time to reach peak plasma concentration decreased from 6.4 hours post-dosing to 4.9 hours.
Distribution
Paroxetine distributes throughout the body, including the CNS, with only 1% remaining in the plasma.
Approximately 95% and 93% of paroxetine is bound to plasma protein at 100 ng/mL and 400 ng/mL, respectively. Under clinical conditions, paroxetine concentrations would normally be less than 400 ng/mL. Paroxetine does not alter the in vitro protein binding of phenytoin or warfarin.
Elimination
Metabolism
The mean elimination half-life is approximately 21 hours (CV 32%) after oral dosing of 30 mg tablets daily for 30 days of paroxetine.
In steady-state dose proportionality studies involving elderly and nonelderly patients, at doses of 20 mg to 40 mg daily for the elderly and 20 mg to 50 mg daily for the nonelderly, some nonlinearity was observed in both populations, again reflecting a saturable metabolic pathway. In comparison to Cmin values after 20 mg daily, values after 40 mg daily were only about 2 to 3 times greater than doubled.
Paroxetine is extensively metabolized after oral administration. The principal metabolites are polar and conjugated products of oxidation and methylation, which are readily cleared. Conjugates with glucuronic acid and sulfate predominate, and major metabolites have been isolated and identified. Data indicate that the metabolites have no more than 1/50 the potency of the parent compound at inhibiting serotonin uptake. The metabolism of paroxetine is accomplished in part by CYP2D6. Saturation of this enzyme at clinical doses appears to account for the nonlinearity of paroxetine kinetics with increasing dose and increasing duration of treatment. The role of this enzyme in paroxetine metabolism also suggests potential drug-drug interactions [see Drug Interactions (7)]. Pharmacokinetic behavior of paroxetine has not been evaluated in subjects who are deficient in CYP2D6 (poor metabolizers).
Excretion
Approximately 64% of a 30-mg oral solution dose of paroxetine was excreted in the urine with 2% as the parent compound and 62% as metabolites over a 10-day post-dosing period. About 36% was excreted in the feces (probably via the bile), mostly as metabolites and less than 1% as the parent compound over the 10-day post-dosing period.
Drug Interaction Studies
There are clinically significant, known drug interactions between paroxetine and other drugs [see Drug Interactions (7)].
Figure 1. Impact of Paroxetine on the Pharmacokinetics of Co-Administered Drugs (log scale)
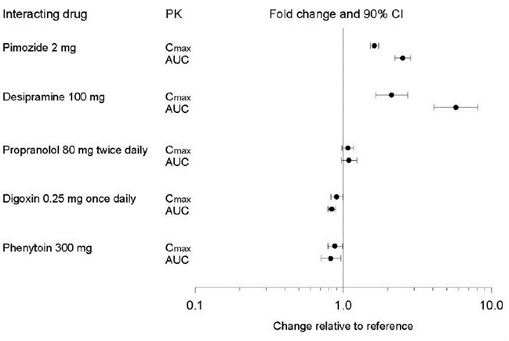
Figure 2. Impact of Co-Administered Drugs on the Pharmacokinetics of Paroxetine
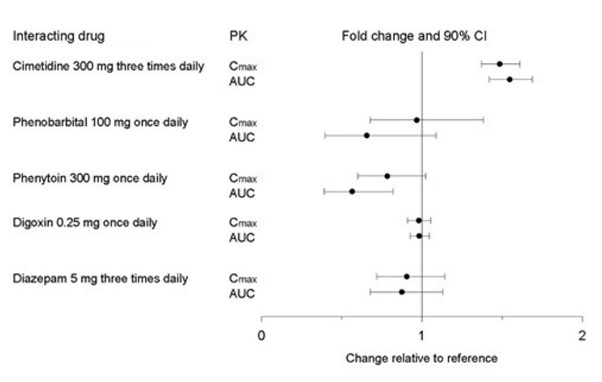
Theophylline: Reports of elevated theophylline levels associated with paroxetine treatment have been reported. While this interaction has not been formally studied, it is recommended that theophylline levels be monitored when these drugs are concurrently administered.
Drugs Metabolized by Cytochrome CYP3A4
An in vivo interaction study involving the coadministration under steady-state conditions of paroxetine and terfenadine, a substrate for CYP3A4, revealed no effect of paroxetine on terfenadine pharmacokinetics. In addition, in vitro studies have shown ketoconazole, a potent inhibitor of CYP3A4 activity, to be at least 100 times more potent than paroxetine as an inhibitor of the metabolism of several substrates for this enzyme, including terfenadine, triazolam, and cyclosporine. Paroxetine’s extent of inhibition of CYP3A4 activity is not expected to be of clinical significance.
Specific Populations
The impact of specific populations on the pharmacokinetics of paroxetine are shown in Figure 3.
The recommended starting dosage and maximum dosage of paroxetine is reduced in elderly patients, patients with severe renal impairment, and patients with severe hepatic impairment [see Dosage and Administration (2.4)].
Figure 3. Impact of Specific Population on the Pharmacokinetics of Paroxetine (log scale)
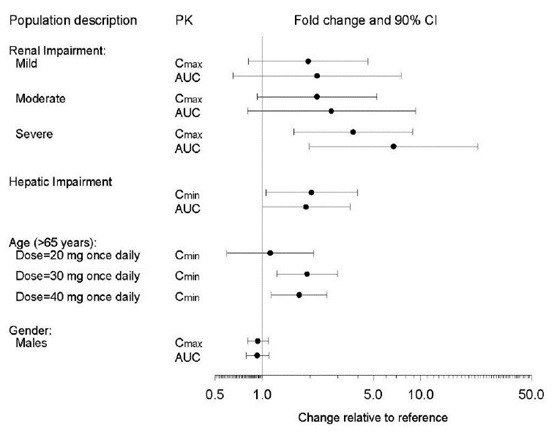
-
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis & Mutagenesis & Impairment Of Fertility
Carcinogenesis
Two-year carcinogenicity studies were conducted in rodents given paroxetine in the diet at 1, 5, and 25 mg/kg/day (mice) and 1, 5, and 20 mg/kg/day (rats). These doses are up to 2 (mouse) and 3 (rat) times the MRHD of 60 mg on a mg/m2 basis. There was a significantly greater number of male rats in the high-dose group with reticulum cell sarcomas (1/100, 0/50, 0/50, and 4/50 for control, low-, middle-, and high-dose groups, respectively) and a significantly increased linear trend across dose groups for the occurrence of lymphoreticular tumors in male rats. Female rats were not affected. Although there was a dose-related increase in the number of tumors in mice, there was no drug-related increase in the number of mice with tumors. The relevance of these findings to humans is unknown.
Mutagenesis
Paroxetine produced no genotoxic effects in a battery of 5 in vitro and 2 in vivo assays that included the following: Bacterial mutation assay, mouse lymphoma mutation assay, unscheduled DNA synthesis assay, and tests for cytogenetic aberrations in vivo in mouse bone marrow and in vitro in human lymphocytes and in a dominant lethal test in rats.
Impairment of Fertility
A reduced pregnancy rate was found in reproduction studies in rats at a dose of paroxetine of 15 mg/kg/day, which is 2 times the MRHD of 60 mg on a mg/m2 basis. Irreversible lesions occurred in the reproductive tract of male rats after dosing in toxicity studies for 2 to 52 weeks. These lesions consisted of vacuolation of epididymal tubular epithelium at 50 mg/kg/day and atrophic changes in the seminiferous tubules of the testes with arrested spermatogenesis at 25 mg/kg/day (8 and 4 times the MRHD of 60 mg on a mg/m2 basis).
-
14 CLINICAL STUDIES
14.1 Major Depressive Disorder
The efficacy of paroxetine as a treatment for major depressive disorder (MDD) has been established in 6 placebo-controlled studies of patients with MDD (aged 18 to 73). In these studies, paroxetine was shown to be statistically significantly more effective than placebo in treating MDD by at least 2 of the following measures: Hamilton Depression Rating Scale (HDRS), the Hamilton depressed mood item, and the Clinical Global Impression (CGI)-Severity of Illness. Paroxetine was statistically significantly better than placebo in improvement of the HDRS sub-factor scores, including the depressed mood item, sleep disturbance factor, and anxiety factor.
Long-term efficacy of paroxetine for treatment of MDD in outpatients was demonstrated in a randomized withdrawal study. Patients who responded to paroxetine (HDRS total score <8) during an initial 8-week open-label treatment phase were then randomized to continue paroxetine or placebo, for up to 1 year. Patients treated with paroxetine demonstrated a statistically significant lower relapse rate during the withdrawal phase (15%) compared to those on placebo (39%). Effectiveness was similar for male and female patients.
14.2 Obsessive Compulsive Disorder
The effectiveness of paroxetine in the treatment of obsessive compulsive disorder (OCD) was demonstrated in two 12-week multicenter placebo-controlled studies of adult outpatients (Studies 1 and 2). Patients had moderate to severe OCD (DSM-IIIR) with mean baseline ratings on the Yale Brown Obsessive Compulsive Scale (YBOCS) total score ranging from 23 to 26. In study 1, a dose-range finding study, patients received fixed daily doses of paroxetine 20 mg, 40 mg, or 60 mg. Study 1 demonstrated that daily doses of paroxetine 40 mg and 60 mg are effective in the treatment of OCD. Patients receiving doses of paroxetine 40 mg and 60 mg experienced a mean reduction of approximately 6 and 7 points, respectively, on the YBOCS total score which was statistically significantly greater than the approximate 4-point reduction at 20 mg and a 3-point reduction in the placebo-treated patients. Study 2 was a flexible-dose study comparing paroxetine 20 mg to 60 mg daily with clomipramine 25 mg to 250 mg daily or placebo). In this study, patients receiving paroxetine experienced a mean reduction of approximately 7 points on the YBOCS total score, which was statistically significantly greater than the mean reduction of approximately 4 points in placebo-treated patients.
The following table provides the outcome classification by treatment group on Global Improvement items of the Clinical Global Impression (CGI) scale for Study 1.
Table 10: Outcome Classification (%) on CGI-Global Improvement Item for Completers in Study 1 in Patients with OCD
Outcome Classification
Placebo
(n = 74)
%
Paroxetine
20 mg
(n = 75)
%
Paroxetine
40 mg
(n = 66)
%
Paroxetine
60 mg
(n = 66)
%
Worse
14
7
7
3
No Change
44
35
22
19
Minimally Improved
24
33
29
34
Much Improved
11
18
22
24
Very Much Improved
7
7
20
20
Subgroup analyses did not indicate that there were any differences in treatment outcomes as a function of age or gender.
The long-term efficacy of paroxetine for the treatment of OCD was established in a long-term extension to Study 1. Patients who responded to paroxetine during the 3-month double-blind phase and a 6-month extension on open-label paroxetine 20 mg to 60 mg daily were randomized to either paroxetine or placebo in a 6-month double-blind relapse prevention phase. Patients randomized to paroxetine were statistically significantly less likely to relapse than placebo-treated patients.
14.3 Panic Disorder
The effectiveness of paroxetine in the treatment of panic disorder (PD) was demonstrated in three 10- to 12-week multicenter, placebo-controlled studies of adult outpatients (Studies 1, 2, and 3). Patients had PD (DSM-IIIR), with or without agoraphobia. In these studies, paroxetine was shown to be statistically significantly more effective than placebo in treating PD by at least 2 out of 3 measures of panic attack frequency and on the Clinical Global Impression Severity of Illness score.
Study 1 was a 10-week dose-range finding study; patients received fixed doses of paroxetine 10 mg, 20 mg, or 40 mg daily or placebo. A statistically significant difference from placebo was observed only for the paroxetine 40 mg daily group. At endpoint, 76% of patients receiving paroxetine 40 mg daily were free of panic attacks, compared to 44% of placebo-treated patients.
Study 2 was a 12-week flexible-dose study comparing paroxetine 10 mg to 60 mg daily and placebo. At endpoint, 51% of paroxetine-treated patients were free of panic attacks compared to 32% of placebo-treated patients.
Study 3 was a 12-week flexible-dose study comparing paroxetine 10 mg to 60 mg daily to placebo in patients concurrently receiving standardized cognitive behavioral therapy. At endpoint, 33% of the paroxetine-treated patients showed a reduction to 0 or 1 panic attacks compared to 14% of placebo-treated patients.
In Studies 2 and 3, the mean paroxetine dose for completers at endpoint was approximately 40 mg daily.
Long-term efficacy of paroxetine in PD was demonstrated in an extension to Study 1. Patients who responded to paroxetine during the 10-week double-blind phase and during a 3-month double-blind extension phase were randomized to either paroxetine 10 mg, 20 mg, or 40 mg daily or placebo in a 3-month double-blind relapse prevention phase. Patients randomized to paroxetine were statistically significantly less likely to relapse than placebo-treated patients.
Subgroup analyses did not indicate that there were any differences in treatment outcomes as a function of age or gender.
14.4 Social Anxiety Disorder
The effectiveness of paroxetine in the treatment of social anxiety disorder (SAD) was demonstrated in three 12-week, multicenter, placebo-controlled studies (Studies 1, 2, and 3) of adult outpatients with SAD (DSM-IV). In these studies, the effectiveness of paroxetine compared to placebo was evaluated on the basis of (1) the proportion of responders, as defined by a Clinical Global Impression (CGI) Improvement score of 1 (very much improved) or 2 (much improved), and (2) change from baseline in the Liebowitz Social Anxiety Scale (LSAS).
Studies 1 and 2 were flexible-dose studies comparing paroxetine 20 mg to 50 mg daily and placebo. Paroxetine demonstrated statistically significant superiority over placebo on both the CGI Improvement responder criterion and the Liebowitz Social Anxiety Scale (LSAS). In Study 1, for patients who completed to week 12, 69% of paroxetine-treated patients compared to 29% of placebo-treated patients were CGI Improvement responders. In Study 2, CGI Improvement responders were 77% and 42% for the paroxetine- and placebo-treated patients, respectively.
Study 3 was a 12-week study comparing fixed doses of paroxetine 20 mg, 40 mg, or 60 mg daily with placebo. Paroxetine 20 mg was statistically significantly superior to placebo on both the LSAS Total Score and the CGI Improvement responder criterion; there were trends for superiority over placebo for the paroxetine 40 mg and 60 mg daily dose groups. There was no indication in this study of any additional benefit for doses higher than 20 mg daily.
Subgroup analyses generally did not indicate differences in treatment outcomes as a function of age, race, or gender.
14.5 Generalized Anxiety Disorder
The effectiveness of paroxetine in the treatment of generalized anxiety disorder (GAD) was demonstrated in two 8-week, multicenter, placebo-controlled studies (Studies 1 and 2) of adult outpatients with GAD (DSM-IV).
Study 1 was an 8-week study comparing fixed doses of paroxetine 20 mg or 40 mg daily with placebo. Doses of paroxetine 20 mg or 40 mg were both demonstrated to be statistically significantly superior to placebo on the Hamilton Rating Scale for Anxiety (HAM-A) total score. There was not sufficient evidence in this study to suggest a greater benefit for the paroxetine 40 mg daily dose compared to the 20 mg daily dose.
Study 2 was a flexible-dose study comparing paroxetine 20 mg to 50 mg daily and placebo. Paroxetine demonstrated statistically significant superiority over placebo on the Hamilton Rating Scale for Anxiety (HAM-A) total score.
A third study, a flexible-dose study comparing paroxetine 20 mg to 50 mg daily to placebo, did not demonstrate statistically significant superiority of paroxetine over placebo on the Hamilton Rating Scale for Anxiety (HAM-A) total score, the primary outcome.
Subgroup analyses did not indicate differences in treatment outcomes as a function of race or gender. There were insufficient elderly patients to conduct subgroup analyses on the basis of age.
In a long-term trial, 566 patients meeting DSM-IV criteria for GAD, who had responded during a single-blind, 8-week acute treatment phase with paroxetine 20 mg to 50 mg daily, were randomized to continuation of paroxetine at their same dose, or to placebo, for up to 24 weeks of observation for relapse. Response during the single-blind phase was defined by having a decrease of >2 points compared to baseline on the CGI-Severity of Illness scale, to a score of <3. Relapse during the double-blind phase was defined as an increase of >2 points compared to baseline on the CGI-Severity of Illness scale to a score of >4, or withdrawal due to lack of efficacy. Patients continuing to receive paroxetine experienced a statistically significantly lower relapse rate over the subsequent 24 weeks compared to those receiving placebo.
14.6 Posttraumatic Stress Disorder
The effectiveness of paroxetine in the treatment of Posttraumatic Stress Disorder (PTSD) was demonstrated in two 12-week, multicenter, placebo-controlled studies (Studies 1 and 2) of adult outpatients who met DSM-IV criteria for PTSD. The mean duration of PTSD symptoms for the 2 studies combined was 13 years (ranging from 0.1 year to 57 years). The percentage of patients with secondary MDD or non-PTSD anxiety disorders in the combined 2 studies was 41% (356 out of 858 patients) and 40% (345 out of 858 patients), respectively. Study outcome was assessed by (1) the Clinician-Administered PTSD Scale Part 2 (CAPS-2) score and (2) the Clinical Global Impression-Global Improvement Scale (CGI-I). The CAPS-2 is a multi-item instrument that measures 3 aspects of PTSD with the following symptom clusters: Reexperiencing/intrusion, avoidance/numbing and hyperarousal. The 2 primary outcomes for each trial were (1) change from baseline to endpoint on the CAPS-2 total score (17 items), and (2) proportion of responders on the CGI-I, where responders were defined as patients having a score of 1 (very much improved) or 2 (much improved).
Study 1 was a 12-week study comparing fixed doses of paroxetine 20 mg or 40 mg daily to placebo. Doses of paroxetine 20 mg and 40 mg were demonstrated to be statistically significantly superior to placebo on change from baseline for the CAPS-2 total score and on proportion of responders on the CGI-I. There was not sufficient evidence in this study to suggest a greater benefit for the 40 mg daily dose compared to the 20 mg daily dose.
Study 2 was a 12-week flexible-dose study comparing paroxetine 20 mg to 50 mg daily to placebo. Paroxetine was demonstrated to be significantly superior to placebo on change from baseline for the CAPS-2 total score and on proportion of responders on the CGI-I.
A third study, a flexible-dose study comparing paroxetine 20 mg to 50 mg daily to placebo, demonstrated paroxetine to be statistically significantly superior to placebo on change from baseline for CAPS-2 total score, but not on proportion of responders on the CGI-I.
The majority of patients in these trials were women (68% women: 377 out of 551 subjects in Study 1 and 66% women: 202 out of 303 subjects in Study 2). Subgroup analyses did not indicate differences in treatment outcomes as a function of gender. There were an insufficient number of patients who were 65 years and older or were non-Caucasian to conduct subgroup analyses on the basis of age or race, respectively.
- 16 HOW SUPPLIED/STORAGE AND HANDLING
-
17 PATIENT COUNSELING INFORMATION
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
Suicidal Thoughts and Behaviors
Advise patients and caregivers to look for the emergence of suicidality, especially early during treatment and when the dosage is adjusted up or down, and instruct them to report such symptoms to the healthcare provider [see Boxed Warning and Warnings and Precautions (5.1)].
Serotonin Syndrome
Caution patients about the risk of serotonin syndrome, particularly with the concomitant use of paroxetine oral suspension with other serotonergic drugs including triptans, tricyclic antidepressants, opioids, lithium, tryptophan, buspirone, amphetamines, St. John’s Wort, and with drugs that impair metabolism of serotonin (in particular, MAOIs, both those intended to treat psychiatric disorders and also others, such as linezolid). Instruct patients to contact their health care provider or report to the emergency room if they experience signs or symptoms of serotonin syndrome [see Warnings and Precautions (5.2), Drug Interactions (7)].
Concomitant Medications
Advise patients to inform their physician if they are taking, or plan to take, any prescription or over-the-counter drugs, since there is a potential for drug-drug interactions [see Warning and Precautions (5.3), Drug Interactions (7)].
Increased Risk of Bleeding
Inform patients about the concomitant use of paroxetine oral suspension with aspirin, NSAIDs, other antiplatelet drugs, warfarin, or other anticoagulants because the combined use has been associated with an increased risk of bleeding. Advise patients to inform their health care providers if they are taking or planning to take any prescription or over-the counter medications that increase the risk of bleeding [see Warnings and Precautions (5.5)].
Activation of Mania/Hypomania
Advise patients and their caregivers to observe for signs of activation of mania/hypomania and instruct them to report such symptoms to the healthcare provider [see Warnings and Precautions (5.6)].
Discontinuation Syndrome
Advise patients not to abruptly discontinue paroxetine oral suspension and to discuss any tapering regimen with their healthcare provider. Inform patients that adverse reactions can occur when paroxetine oral suspension is discontinued [See Warnings and Precautions (5.7)].
Sexual Dysfunction
Advise patients that use of paroxetine may cause symptoms of sexual dysfunction in both male and female patients. Inform patients that they should discuss any changes in sexual function and potential management strategies with their healthcare provider [see Warnings and Precautions (5.13)].
Administration Information for Oral Suspension
Instruct patients to shake the oral suspension well before administration [see Dosage and Administration (2.1)].
Allergic Reactions
Advise patients to notify their healthcare provider if they develop an allergic reaction such as rash, hives, swelling, or difficulty breathing [see Adverse Reactions (6.1, 6.2)].
EmbryoFetal Toxicity
Advise women to notify their healthcare provider if they become pregnant or intend to become pregnant during treatment with paroxetine. Advise women of risks associated with first trimester use of paroxetine and that use later in pregnancy may lead to an increased risk for neonatal complications requiring prolonged hospitalization, respiratory support, tube feeding, and/or persistent pulmonary hypertension of the newborn (PPHN) [see Warnings and Precautions (5.4), Use in Specific Populations (8.1)]. Advise women that there is a pregnancy exposure registry that monitors pregnancy outcomes in women exposed to paroxetine during pregnancy [see Warnings and Precautions (5.4), Use in Specific Populations (8.1)].
Lactation
Advise breastfeeding women using paroxetine to monitor infants for agitation, irritability, poor feeding, and poor weight gain and to seek medical care if they notice these signs [see Use in Specific Populations (8.2)].
Females and Males of Reproductive Potential
Advise men that paroxetine may affect sperm quality, which may impair fertility; it is not known if this effect is reversible [see Use in Specific Populations (8.3)].
All trademarks are the property of their respective owners.
Manufactured by:
Novitium Pharma LLC
70 Lake Drive, East Windsor
New Jersey 08520
Issued: 03/2025
LB4256-06
-
SPL MEDGUIDE SECTION
MEDICATION GUIDE
Paroxetine (pa rox’ e teen)
Oral Suspension
What is the most important information I should know about paroxetine oral suspension?
Paroxetine oral suspension can cause serious side effects, including:
- Increased risk of suicidal thoughts or actions. Paroxetine oral suspension and other antidepressant medicines may increase suicidal thoughts and actions in some people 24 years of age and younger, especially within the first few months of treatment or when the dose is changed. Paroxetine oral suspension is not for use in children.
- Depression or other mental illnesses are the most important causes of suicidal thoughts and actions.
- Pay close attention to any changes, especially sudden changes in mood, behavior, thoughts or feelings or if you develop suicidal thoughts or actions. This is very important when an antidepressant medicine is started or when the dose is changed.
- Call your healthcare provider right away to report new or sudden changes in mood, behavior, thoughts or feelings or if you develop suicidal thoughts or actions.
- Keep all follow-up visits with your healthcare provider as scheduled. Call your healthcare provider between visits as needed, especially if you have concerns about symptoms.

What is paroxetine oral suspension?
Paroxetine oral suspension is a prescription medicine used in adults to treat:
- A certain type of depression called Major Depressive Disorder (MDD)
- Obsessive Compulsive Disorder (OCD)
- Panic Disorder (PD)
- Social Anxiety Disorder (SAD)
- Generalized Anxiety Disorder (GAD)
- Posttraumatic Stress Disorder (PTSD)
Do not take paroxetine oral suspension if you:
- take a monoamine oxidase inhibitor (MAOI)
- have stopped taking an MAOI in the last 14 days
- are being treated with the antibiotic linezolid or the intravenous methylene blue
- are taking pimozide
- are taking thioridazine
- are allergic to paroxetine or any of the ingredients in paroxetine oral suspension. See the end of this Medication Guide for a complete list of ingredients in paroxetine oral suspension.
Ask your healthcare provider or pharmacist if you are not sure if you take an MAOI or one of these medicines, including the antibiotic linezolid or intravenous methylene blue.
Do not start taking an MAOI for at least 14 days after you stop treatment with paroxetine oral suspension.
Before taking paroxetine oral suspension, tell your healthcare provider about all your medical conditions, including if you:
- have heart problemshave or had bleeding problems
- have, or have a family history of, bipolar disorder, mania or hypomania
- have or had seizures or convulsions
- have glaucoma (high pressure in the eye)
- have low sodium levels in your blood
- have bone problems
- have kidney or liver problems
- are pregnant or plan to become pregnant. Paroxetine may harm your unborn baby.
- Taking paroxetine oral suspension during your first trimester of pregnancy may cause your baby to be at an increased risk of having a heart problem (cardiac malformations) at birth.
- Taking paroxetine oral suspension during your third trimester of pregnancy may cause your baby to have breathing, temperature, and feeding problems, low muscle tone, and irritability after birth and may cause your baby to be at an increased risk of a serious lung problem at birth. Talk to your healthcare provider about the risk to your unborn baby if you take paroxetine during pregnancy.
- Tell your healthcare provider right away if you become pregnant or think you are pregnant during treatment with paroxetine oral suspension.
- There is a pregnancy registry for females who are exposed to paroxetine during pregnancy. The purpose of the registry is to collect information about the health of females exposed to paroxetine and their baby. If you become pregnant during treatment with paroxetine oral suspension, talk to your healthcare provider about registering with the National Pregnancy Registry for Antidepressants at 1-866-961-2388 or visit online at https://womensmentalhealth.org/clinical-and-research-programs/pregnancyregistry /antidepressants/.
- are breastfeeding or plan to breastfeed. Paroxetine passes into your breast milk. Talk to your healthcare provider about the best way to feed your baby during treatment with paroxetine oral suspension.
Paroxetine oral suspension and some other medicines may affect each other causing possible serious side effects. Paroxetine oral suspension may affect the way other medicines work and other medicines may affect the way paroxetine oral suspension works.
Especially tell your healthcare provider if you take:
- medicines used to treat migraine headaches called triptans
- tricyclic antidepressants
- lithium
- tramadol, fentanyl, meperidine, methadone, or other opioids
- tryptophan
- buspirone
- amphetamines
- St. John’s Wort
- medicines that can affect blood clotting such as aspirin, nonsteroidal anti-inflammatory drugs (NSAIDs), warfarin
- diuretics
- tamoxifen
- medicines used to treat mood, anxiety, psychotic, or thought disorders, including selective serontonin reuptake (SSRIs) and serotonin norepinephrine reuptake inhibitors (SNRIs)
Do not start or stop any other medicines during treatment with paroxetine oral suspension without talking to your healthcare provider first. Stopping paroxetine oral suspension suddenly may cause you to have serious side effects. See, “What are the possible side effects of paroxetine oral suspension?”.
Know the medicines you take. Keep a list of them to show to your healthcare provider and pharmacist when you get a new medicine.
How should I take paroxetine oral suspension?
- Take paroxetine oral suspension exactly as prescribed. Your healthcare provider may need to change the dose of paroxetine oral suspension until it is the right dose for you.
- Take paroxetine oral suspension 1 time each day in the morning.
- Paroxetine oral suspension may be taken with or without food.
- If you are taking paroxetine oral suspension, shake the suspension well before taking.
- If you take too much paroxetine oral suspension, call your poison control center at 1-800-222-1222 or go to the nearest hospital emergency room right away.
What are possible side effects of paroxetine oral suspension?
Paroxetine oral suspension can cause serious side effects, including:
- See, “What is the most important information I should know about paroxetine oral suspension?”
- Serotonin syndrome. A potentially life-threatening problem called serotonin syndrome can happen when you take paroxetine oral suspension with certain other medicines. See, “Who should not take paroxetine oral suspension?” Call your healthcare provider or go to the nearest hospital emergency room right away if you have any of the following signs and symptoms of serotonin syndrome:

-
Eye problems (angle-closure glaucoma). Paroxetine oral suspension may cause a type of eye problem called angle-closure glaucoma in people with certain other eye conditions. You may want to undergo an eye examination to see if you are at risk and receive preventative treatment if you are. Call your healthcare provider if you have eye pain, changes in your vision, or swelling or redness in or around the eye.
- Medicine interactions. Taking paroxetine oral suspension with certain other medicines including thioridazine and pimozide may increase the risk of developing a serious heart problem called QT prolongation.
- Seizures (convulsions).
-
Manic episodes. Manic episodes may happen in people with bipolar disorder who take paroxetine oral suspension. Symptoms may include:

-
Discontinuation syndrome. Suddenly stopping paroxetine oral suspension may cause you to have serious side effects. Your healthcare provider may want to decrease your dose slowly. Symptoms may include:

- Low sodium levels in your blood (hyponatremia). Low sodium levels in your blood that may be serious and may cause death, can happen during treatment with paroxetine oral suspension. Elderly people and people who take certain medicines may be at a greater risk for developing low sodium levels in your blood. Signs and symptoms may include:
- headache
- difficulty concentrating
- memory changes
- confusion
- weakness and unsteadiness on your feet which can lead to falls
- seeing or hearing things that are not real (hallucinations)
- fainting
- seizures
- coma
- stopping breathing (respiratory arrest)
- Abnormal bleeding. Taking paroxetine oral suspension with aspirin, NSAIDs, or blood thinners may increase this risk. Tell your healthcare provider about any unusual bleeding or bruising.
- Bonefractures.
-
Sexual problems (dysfunction). Taking selective serotonin reuptake inhibitors (SSRIs), including paroxetine oral suspension, may cause sexual problems.
- Delayed ejaculation or inability to have an ejaculation
- Decreased sex drive
- Problems getting or keeping an erection
Symptoms in females may include:- Decreased sex drive
- Delayed orgasm or inability to have an orgasm
The most common side effects of paroxetine oral suspension include:

These are not all the possible side effects of paroxetine oral suspension.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
How should I store paroxetine oral suspension?
- Store paroxetine oral suspension at 68° to 77ºF (20° to 25ºC).
General information about the safe and effective use of paroxetine oral suspension.
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not take paroxetine oral suspension for a condition for which it was not prescribed. Do not give paroxetine oral suspension to other people, even if they have the same symptoms that you have. It may harm them. You may ask your healthcare provider or pharmacist for information about paroxetine oral suspension that is written for healthcare professionals.
What are the ingredients in paroxetine oral suspension?
Active ingredient: Paroxetine hydrochloride
Inactive ingredients:
Oral suspension: polacrilin potassium, microcrystalline cellulose, carboxymethyl cellulose sodium, propylene glycol, glycerin, sorbitol, methylparaben, propylparaben, sodium citrate dihydrate, citric acid anhydrous, sodium saccharin, orange flavor (triacetin, propylene glycol, natural and artificial flavor), FD&C Yellow No. 6, simethicone emulsion and purified water.
All trademarks are the property of their respective owners.
Manufactured by:
Novitium Pharma LLC
70 Lake Drive, East Windsor
New Jersey 08520
For more information about paroxetine oral suspension, call 1-855-204-1431.
This Medication Guide has been approved by the U.S. Food and Drug Administration.
Issued: 03/2025
LB4256-06
- PACKAGE LABEL.PRINCIPAL DISPLAY PANEL
-
INGREDIENTS AND APPEARANCE
PAROXETINE
paroxetine suspensionProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 70954-319 Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength PAROXETINE HYDROCHLORIDE HEMIHYDRATE (UNII: X2ELS050D8) (PAROXETINE - UNII:41VRH5220H) PAROXETINE 10 mg in 5 mL Inactive Ingredients Ingredient Name Strength POLACRILIN POTASSIUM (UNII: 0BZ5A00FQU) CELLULOSE, MICROCRYSTALLINE (UNII: OP1R32D61U) CARBOXYMETHYLCELLULOSE SODIUM (UNII: K679OBS311) PROPYLENE GLYCOL (UNII: 6DC9Q167V3) GLYCERIN (UNII: PDC6A3C0OX) SORBITOL (UNII: 506T60A25R) METHYLPARABEN (UNII: A2I8C7HI9T) PROPYLPARABEN (UNII: Z8IX2SC1OH) TRISODIUM CITRATE DIHYDRATE (UNII: B22547B95K) ANHYDROUS CITRIC ACID (UNII: XF417D3PSL) SACCHARIN SODIUM MONOHYDRATE (UNII: A9CO00M9HV) TRIACETIN (UNII: XHX3C3X673) FD&C YELLOW NO. 6 (UNII: H77VEI93A8) DIMETHICONE (UNII: 92RU3N3Y1O) WATER (UNII: 059QF0KO0R) Product Characteristics Color ORANGE Score Shape Size Flavor ORANGE Imprint Code Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 70954-319-10 250 mL in 1 BOTTLE; Type 0: Not a Combination Product 09/03/2021 Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA215003 09/03/2021 Labeler - ANI Pharmaceuticals, Inc. (145588013) Establishment Name Address ID/FEI Business Operations Novitium Pharma LLC 080301870 ANALYSIS(70954-319) , LABEL(70954-319) , MANUFACTURE(70954-319) , PACK(70954-319)
© 2026 FDA.report
This site is not affiliated with or endorsed by the FDA.
