DILTIAZEM HYDROCHLORIDE capsule, extended release
Diltiazem Hydrochloride by
Drug Labeling and Warnings
Diltiazem Hydrochloride by is a Prescription medication manufactured, distributed, or labeled by Dispensing Solutions, Inc., PSS World Medical, Inc.. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
- SPL UNCLASSIFIED SECTION
-
DESCRIPTION
Diltiazem hydrochloride, USP is a calcium ion cellular influx inhibitor (slow channel blocker or calcium antagonist). Chemically, diltiazem hydrochloride is 1,5-benzothiazepin-4(5H)one,3-(acetyloxy)-5-[2-(dimethylamino)ethyl]-2,3-dihydro-2-(4-methoxyphenyl)-, monohydrochloride,(+)-cis-. The chemical structure is:
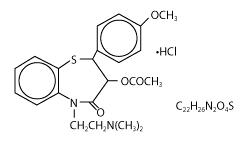
Diltiazem hydrochloride, USP is a white to off-white crystalline powder with a bitter taste. It is soluble in water, methanol, and chloroform. It has a molecular weight of 450.98. Diltiazem hydrochloride, USP is formulated as a once-a-day extended release capsule containing either 120 mg, 180 mg, 240 mg, or 300 mg diltiazem hydrochloride.
Each diltiazem extended-release capsule, for oral administration, contains the following inactive ingredients:
120 mg — ammonio methacrylate copolymer NF, type A, ammonio methacrylate copolymer NF, type B, ammonium hydroxide, black iron oxide, gelatin, hydroxypropyl cellulose, pharmaceutical glaze, propylene glycol, silicon dioxide, simethicone, sodium lauryl sulfate, sugar spheres, talc, titanium dioxide, triethyl citrate
180 mg — ammonio methacrylate copolymer NF, type A, ammonio methacrylate copolymer NF, type B, ammonium hydroxide, D and C yellow #10, FD and C blue #1, FD and C green #3, gelatin, hydroxypropyl cellulose, pharmaceutical glaze, propylene glycol, silicon dioxide, simethicone, sodium lauryl sulfate, sugar spheres, talc, titanium dioxide, triethyl citrate
240 mg — ammonio methacrylate copolymer NF, type A, ammonio methacrylate copolymer NF, type B, ammonium hydroxide, D and C yellow #10, FD and C green #3, gelatin, hydroxypropyl cellulose, pharmaceutical glaze, propylene glycol, silicon dioxide, simethicone, sodium lauryl sulfate, sugar spheres, talc, titanium dioxide, triethyl citrate
300 mg— ammonio methacrylate copolymer NF, type A, ammonio methacrylate copolymer NF, type B, ammonium hydroxide, black iron oxide, D and C yellow #10, FD and C green #3, gelatin, hydroxypropyl cellulose, pharmaceutical glaze, propylene glycol, silicon dioxide, simethicone, sodium lauryl sulfate, sugar spheres, talc, titanium dioxide, triethyl citrate
This drug product conforms to USP Drug release test #11. -
CLINICAL PHARMACOLOGY
The therapeutic effects of diltiazem hydrochloride are believed to be related to its ability to inhibit the cellular influx of calcium ions during membrane depolarization of cardiac and vascular smooth muscle.
Hypertension: Diltiazem hydrochloride produces its antihypertensive effect primarily by relaxation of vascular smooth muscle and the resultant decrease in peripheral vascular resistance. The magnitude of blood pressure reduction is related to the degree of hypertension; thus hypertensive individuals experience an antihypertensive effect, whereas there is only a modest fall in blood pressure in normotensives.
Angina: Diltiazem hydrochloride has been shown to produce increases in exercise tolerance, probably due to its ability to reduce myocardial oxygen demand. This is accomplished via reductions in heart rate and systemic blood pressure at submaximal and maximal work loads. Diltiazem has been shown to be a potent dilator of coronary arteries, both epicardial and subendocardial. Spontaneous and ergonovine-induced coronary artery spasm are inhibited by diltiazem.
In animal models, diltiazem interferes with the slow inward (depolarizing) current in excitable tissue. It causes excitation-contraction uncoupling in various myocardial tissues without changes in the configuration of the action potential. Diltiazem produces relaxation of coronary vascular smooth muscle and dilation of both large and small coronary arteries at drug levels which cause little or no negative inotropic effect. The resultant increases in coronary blood flow (epicardial and subendocardial) occur in ischemic and nonischemic models and are accompanied by dose-dependent decreases in systemic blood pressure and decreases in peripheral resistance.
Like other calcium channel antagonists, diltiazem decreases sinoatrial and atrioventricular conduction in isolated tissues and has a negative inotropic effect in isolated preparations. In the intact animal, prolongation of the AH interval can be seen at higher doses.
In man, diltiazem prevents spontaneous and ergonovine-provoked coronary artery spasm. It causes a decrease in peripheral vascular resistance and a modest fall in blood pressure in normotensive individuals and, in exercise tolerance studies in patients with ischemic heart disease, reduces the heart rate-blood pressure product for any given work load. Studies to date, primarily in patients with good ventricular function, have not revealed evidence of a negative inotropic effect cardiac output, ejection fraction, and left ventricular end diastolic pressure have not been affected. Such data have no predictive value with respect to effects in patients with poor ventricular function, and increased heart failure has been reported in patients with preexisting impairment of ventricular function. There are as yet few data on the interaction of diltiazem and beta-blockers in patients with poor ventricular function. Resting heart rate is usually slightly reduced by diltiazem.
In hypertensive patients, diltiazem hydrochloride extended-release produces antihypertensive effects both in the supine and standing positions. In a double-blind, parallel, dose-response study utilizing doses ranging from 90 to 540 mg once daily, diltiazem hydrochloride lowered supine diastolic blood pressure in an apparent linear manner over the entire dose range studied. The changes in diastolic blood pressure, measured at trough, for placebo, 90 mg, 180 mg, 360 mg, and 540 mg were -2.9, -4.5, -6.1, -9.5, and -10.5 mm Hg, respectively. Postural hypotension is infrequently noted upon suddenly assuming an upright position. No reflex tachycardia is associated with the chronic antihypertensive effects. Diltiazem hydrochloride decreases vascular resistance, increases cardiac output (by increasing stroke volume), and produces a slight decrease or no change in heart rate. During dynamic exercise, increases in diastolic pressure are inhibited, while maximum achievable systolic pressure is usually reduced. Chronic therapy with diltiazem hydrochloride produces no change or an increase in plasma catecholamines. No increased activity of the renin-angiotensin-aldosterone axis has been observed. Diltiazem reduces the renal and peripheral effects of angiotensin II. Hypertensive animal models respond to diltiazem hydrochloride with reductions in blood pressure and increased urinary output and natriuresis without a change in urinary sodium/potassium ratio.
In a double-blind, parallel dose-response study of doses from 60 mg to 480 mg once daily, diltiazem hydrochloride increased time to termination of exercise in a linear manner over the entire dose range studied. The improvement in time to termination of exercise utilizing a Bruce exercise protocol, measured at trough, for placebo, 60 mg, 120 mg, 240 mg, 360 mg, and 480 mg was 29, 40, 56, 51, 69 and 68 seconds, respectively. As doses of diltiazem hydrochloride were increased, overall angina frequency was decreased. Diltiazem hydrochloride, 180 mg once daily, or placebo was administered in a double-blind study to patients receiving concomitant treatment with long-acting nitrates and/or beta-blockers. A significant increase in time to termination of exercise and a significant decrease in overall angina frequency was observed. In this trial the overall frequency of adverse events in the diltiazem treatment group was the same as the placebo group.
Intravenous diltiazem hydrochloride in doses of 20 mg prolongs AH conduction time and AV node functional and effective refractory periods by approximately 20%. In a study involving single oral doses of 300 mg of diltiazem hydrochloride in six normal volunteers, the average maximum PR prolongation was 14% with no instances of greater than first-degree AV block. Diltiazem-associated prolongation of the AH interval is not more pronounced in patients with first-degree heart block. In patients with sick sinus syndrome, diltiazem significantly prolongs sinus cycle length (up to 50% in some cases).
Chronic oral administration of diltiazem hydrochloride to patients in doses of up to 540 mg/day has resulted in small increases in PR interval and on occasion produces abnormal prolongation (see WARNINGS).
Diltiazem is well absorbed from the gastrointestinal tract and is subject to an extensive first-pass effect, giving an absolute bioavailability (compared to intravenous administration) of about 40%. Diltiazem undergoes extensive metabolism in which only 2% to 4% of the unchanged drug appears in the urine. Drugs which induce or inhibit hepatic microsomal enzymes may alter diltiazem disposition.
Total radioactivity measurement following short IV administration in healthy volunteers suggests the presence of other unidentified metabolites, which attain higher concentrations than those of diltiazem and are more slowly eliminated; half-life of total radioactivity is about 20 hours compared to 2 to 5 hours for diltiazem.
In vitro binding studies show diltiazem is 70% to 80% bound to plasma proteins. Competitive in vitro ligand binding studies have also shown diltiazem binding is not altered by therapeutic concentrations of digoxin, hydrochlorothiazide, phenylbutazone, propranolol, salicylic acid, or warfarin. The plasma elimination half-life following single or multiple drug administration is approximately 3.0 to 4.5 hours. Desacetyl diltiazem is also present in the plasma at levels of 10% to 20% of the parent drug and is 25% to 50% as potent as a coronary vasodilator as diltiazem. Minimum therapeutic plasma diltiazem concentrations appear to be in the range of 50 to 200 ng/mL. There is a departure from linearity when dose strengths are increased; the half-life is slightly increased with dose. A study that compared patients with normal hepatic function to patients with cirrhosis found an increase in half-life and a 69% increase in bioavailability in the hepatically impaired patients. A single study in nine patients with severely impaired renal function showed no difference in the pharmacokinetic profile of diltiazem compared to patients with normal renal function.
Diltiazem Hydrochloride Extended-Release Capsules: When compared to a regimen of diltiazem hydrochloride tablets at steady-state, more than 95% of drug is absorbed from the diltiazem hydrochloride extended-release capsules formulation. A single 360-mg dose of the capsule results in detectable plasma levels within 2 hours and peak plasma levels between 10 and 14 hours; absorption occurs throughout the dosing interval. When diltiazem hydrochloride extended-release capsules were coadministered with a high fat content breakfast, the extent of diltiazem absorption was not affected. Dose-dumping does not occur. The apparent elimination half-life after single or multiple dosing is 5 to 8 hours. A departure from linearity similar to that seen with diltiazem hydrochloride tablets and diltiazem hydrochloride sustained-release capsules is observed. As the dose of diltiazem hydrochloride extended-release capsules is increased from a daily dose of 120 mg to 240 mg, there is an increase in the area-under-the-curve of 2.7 times. When the dose is increased from 240 mg to 360 mg there is an increase in the area-under-the-curve of 1.6 times.
-
INDICATIONS & USAGE
Diltiazem hydrochloride extended-release capsules, USP are indicated for the treatment of hypertension. It may be used alone or in combination with other antihypertensive medications.
Diltiazem hydrochloride extended-release capsules, USP are indicated for the management of chronic stable angina and angina due to coronary artery spasm.
-
CONTRAINDICATIONS
Diltiazem hydrochloride is contraindicated in (1) patients with sick sinus syndrome except in the presence of a functioning ventricular pacemaker, (2) patients with second-or third-degree AV block except in the presence of a functioning ventricular pacemaker, (3) patients with hypotension (less than 90 mm Hg systolic), (4) patients who have demonstrated hypersensitivity to the drug, and (5) patients with acute myocardial infarction and pulmonary congestion documented by x-ray on admission.
-
WARNINGS
-
Cardiac Conduction: Diltiazem
prolongs AV node refractory periods without significantly prolonging
sinus node recovery time, except in patients with sick sinus syndrome.
This effect may rarely result in abnormally slow heart rates
(particularly in patients with sick sinus syndrome) or second- or
third-degree AV block (13 of 3290 patients or 0.40%). Concomitant use
of diltiazem with beta-blockers or digitalis may result in additive
effects on cardiac conduction. A patient with Prinzmetal’s angina
developed periods of asystole (2 to 5 seconds) after a single dose of
60 mg of diltiazem (see ADVERSE REACTIONS).
- Congestive Heart Failure: Although diltiazem has a negative inotropic effect in isolated animal tissue preparations, hemodynamic studies in humans with normal ventricular function have not shown a reduction in cardiac index nor consistent negative effects on contractility (dp/dt). An acute study of oral diltiazem in patients with impaired ventricular function (ejection fraction 24% ± 6%) showed improvement in indices of ventricular function without significant decrease in contractile function (dp/dt). Worsening of congestive heart failure has been reported in patients with preexisting impairment of ventricular function. Experience with the use of diltiazem hydrochloride in combination with beta-blockers in patients with impaired ventricular function is limited. Caution should be exercised when using this combination.
- Hypotension: Decreases in blood pressure associated with diltiazem therapy may occasionally result in symptomatic hypotension.
- Acute Hepatic Injury: Mild elevations of transaminases with and without concomitant elevation in alkaline phosphatase and bilirubin have been observed in clinical studies. Such elevations were usually transient and frequently resolved even with continued diltiazem treatment. In rare instances, significant elevations in enzymes such as alkaline phosphatase, LDH, SGOT, SGPT, and other phenomena consistent with acute hepatic injury have been noted. These reactions tended to occur early after therapy initiation (1 to 8 weeks) and have been reversible upon discontinuation of drug therapy. The relationship to diltiazem is uncertain in some cases, but probable in some (see PRECAUTIONS).
-
Cardiac Conduction: Diltiazem
prolongs AV node refractory periods without significantly prolonging
sinus node recovery time, except in patients with sick sinus syndrome.
This effect may rarely result in abnormally slow heart rates
(particularly in patients with sick sinus syndrome) or second- or
third-degree AV block (13 of 3290 patients or 0.40%). Concomitant use
of diltiazem with beta-blockers or digitalis may result in additive
effects on cardiac conduction. A patient with Prinzmetal’s angina
developed periods of asystole (2 to 5 seconds) after a single dose of
60 mg of diltiazem (see ADVERSE REACTIONS).
-
ADVERSE REACTIONS
Serious adverse reactions have been rare in studies carried out to date, but it should be recognized that patients with impaired ventricular function and cardiac conduction abnormalities have usually been excluded from these studies.
The following table presents the most common adverse reactions reported in placebo-controlled angina and hypertension trials in patients receiving diltiazem hydrochloride extended-release capsules up to 360 mg with rates in placebo patients shown for comparison.
DILTIAZEM HYDROCHLORIDE EXTENDED-RELEASE CAPSULE PLACEBO-CONTROLLED ANGINA ANDHYPERTENSION TRIALS COMBINED
Diltiazem
Hydrochloride
Extended-Release Capsules Placebo Adverse Reaction n=607 n=301 Headache 5.4% 5.0% Dizziness 3.0% 3.0% Bradycardia 3.3% 1.3% AV Block First Degree 3.3% 0.0% Edema 2.6% 1.3% ECG Abnormality 1.6% 2.3% Asthenia 1.8% 1.7% In clinical trials of diltiazem hydrochloride extended-release capsules, diltiazem hydrochloride tablets, and diltiazem hydrochloride sustained-release capsules involving over 3200 patients, the most common events (ie, greater than 1%) were edema (4.6%), headache (4.6%), dizziness (3.5%), asthenia (2.6%), first degree AV block (2.4%), bradycardia (1.7%), flushing (1.4%), nausea (1.4%), and rash (1.2%).
In addition, the following events were reported infrequently (less than 1%) in angina or hypertension trials:
Cardiovascular: Angina, arrhythmia, AV block (second- or third-degree), bundle branch block, congestive heart failure, ECG abnormalities, hypotension, palpitations, syncope, tachycardia, ventricular extrasystoles.
Nervous System: Abnormal dreams, amnesia, depression, gait abnormality, hallucinations, insomnia, nervousness, paresthesia, personality change, somnolence, tinnitus, tremor.
Gastrointestinal: Anorexia, constipation, diarrhea, dry mouth, dysgeusia, dyspepsia, mild elevations of SGOT, SGPT, LDH, and alkaline phosphatase (see WARNINGS, Acute Hepatic Injury), thirst, vomiting, weight increase
Dermatological: Petechiae, photosensitivity, pruritus, urticaria.
Other: Amblyopia, CPK increase, dyspnea, epistaxis, eye irritation, hyperglycemia, hyperuricemia, impotence, muscle cramps, nasal congestion, nocturia, osteoarticular pain, polyuria, sexual difficulties.
The following postmarketing events have been reported infrequently in patients receiving diltiazem hydrochloride: acute generalized exanthematous pustulosis, allergic reactions, alopecia, angioedema (including facial or periorbital edema), asystole, erythema multiforme (including Stevens-Johnson syndrome, toxic epidermal necrolysis), exfoliative dermatitis, extrapyramidal symptoms, gingival hyperplasia, hemolytic anemia, increased bleeding time, leukopenia, photosensitivity (including lichenoid keratosis and hyperpigmentation at sun-exposed skin areas), purpura, retinopathy, myopathy and thrombocytopenia. In addition, events such as myocardial infarction have been observed which are not readily distinguishable from the natural history of the disease in these patients. A number of well-documented cases of generalized rash, some characterized as leukocytoclastic vasculitis, have been reported. However, a definitive cause and effect relationship between these events and diltiazem therapy is yet to be established.
-
OVERDOSAGE
The oral LD50’s in mice and rats range from 415 to 740 mg/kg and from 560 to 810 mg/kg, respectively. The intravenous LD50’s in these species were 60 and 38 mg/kg, respectively. The oral LD50 in dogs is considered to be in excess of 50 mg/kg, while lethality was seen in monkeys at 360 mg/kg.
The toxic dose in man is not known. Due to extensive metabolism, blood levels after a standard dose of diltiazem can vary over tenfold, limiting the usefulness of blood levels in overdose cases.
There have been reports of diltiazem overdose in amounts ranging from less than 1 g to 18 g. Of cases with known outcome, most patients recovered and in cases with a fatal outcome, the majority involved multiple drug ingestion.
Events observed following diltiazem overdose included bradycardia, hypotension, heart block, and cardiac failure. Most reports of overdose described some supportive medical measure and/or drug treatment. Bradycardia frequently responded favorably to atropine, as did heart block, although cardiac pacing was also frequently utilized to treat heart block. Fluids and vasopressors were used to maintain blood pressure and in cases of cardiac failure, inotropic agents were administered. In addition, some patients received treatment with ventilatory support, gastric lavage, activated charcoal, and/or intravenous calcium.
The effectiveness of intravenous calcium administration to reverse the pharmacological effects of diltiazem overdose has been inconsistent. In a few reported cases, overdose with calcium channel blockers associated with hypotension and bradycardia that was initially refractory to atropine became more responsive to atropine after the patients received intravenous calcium. In some cases, intravenous calcium has been administered (1 g calcium chloride or 3 g calcium gluconate) over 5 minutes and repeated every 10 to 20 minutes as necessary. Calcium gluconate has also been administered as a continuous infusion at a rate of 2 g per hour for 10 hours. Infusions of calcium for 24 hours or more may be required. Patients should be monitored for signs of hypercalcemia.
In the event of overdose or exaggerated response, appropriate supportive measures should be employed in addition to gastrointestinal decontamination. Diltiazem does not appear to be removed by peritoneal or hemodialysis. Limited data suggest that plasmapheresis or charcoal hemoperfusion may hasten diltiazem elimination following overdose. Based on the known pharmacological effects of diltiazem and/or reported clinical experiences, the following measures may be considered:
Bradycardia: Administer atropine (0.60 to 1.0 mg). If there is no response to vagal blockade, administer isoproterenol cautiously.
High-degree AV Block: Treat as for bradycardia above. Fixed high-degree AV block should be treated with cardiac pacing.
Cardiac Failure: Administer inotropic agents (isoproterenol, dopamine, or dobutamine) and diuretics.
Hypotension: Vasopressors (e.g., dopamine or norepinephrine).
Actual treatment and dosage should depend on the severity of the clinical situation and the judgment and experience of the treating physician. -
DOSAGE & ADMINISTRATION
Patients controlled on diltiazem alone or in combination with other medications may be switched to diltiazem hydrochloride extended-release capsules at the nearest equivalent total daily dose. Higher doses of diltiazem hydrochloride extended-release capsules may be needed in some patients. Patients should be closely monitored. Subsequent titration to higher or lower doses may be necessary and should be initiated as clinically warranted. There is limited general clinical experience with doses above 360 mg, but doses to 540 mg have been studied in clinical trials. The incidence of side effects increases as the dose increases with first-degree AV block, dizziness, and sinus bradycardia bearing the strongest relationship to dose.
Hypertension: Dosage needs to be adjusted by titration to individual patient needs. When used as monotherapy, reasonable starting doses are 180 to 240 mg once daily, although some patients may respond to lower doses. Maximum antihypertensive effect is usually observed by 14 days of chronic therapy; therefore, dosage adjustments should be scheduled accordingly. The usual dosage range studied in clinical trials was 240 to 360 mg once daily. Individual patients may respond to higher doses of up to 480 mg once daily.
Angina: Dosages for the treatment of angina should be adjusted to each patient’s needs, starting with a dose of 120 or 180 mg once daily. Individual patients may respond to higher doses of up to 480 mg once daily. When necessary, titration may be carried out over a 7- to 14-day period.
Concomitant Use With Other Cardiovascular Agents
-
Sublingual NTG - May be taken as required to abort acute anginal attacks during diltiazem hydrochloride extended-release capsules therapy.
-
Prophylactic Nitrate Therapy - Diltiazem hydrochloride extended-release capsules may be safely coadministered with short-and long-acting nitrates.
-
Beta-Blockers - (See WARNINGS and PRECAUTIONS).
- Antihypertensives - Diltiazem hydrochloride extended-release capsules have an additive antihypertensive effect when used with other antihypertensive agents. Therefore, the dosage of diltiazem hydrochloride extended-release capsules or the concomitant antihypertensives may need to be adjusted when adding one to the other.
-
Sublingual NTG - May be taken as required to abort acute anginal attacks during diltiazem hydrochloride extended-release capsules therapy.
-
HOW SUPPLIED
Diltiazem Hydrochloride Extended-release Capsules, USP are supplied as follows:
120 mg — Each #2 capsule with light gray opaque cap and body printed with
 and 2588 on both cap and body in white ink contains 120 mg of diltiazem
hydrochloride, USP. Capsules are supplied in bottles of 30 (NDC
0228-2588-03), 90 (NDC: 0228-2588-09) and 500 (NDC: 0228-2588-50).
and 2588 on both cap and body in white ink contains 120 mg of diltiazem
hydrochloride, USP. Capsules are supplied in bottles of 30 (NDC
0228-2588-03), 90 (NDC: 0228-2588-09) and 500 (NDC: 0228-2588-50).180 mg — Each #0 capsule with dark green opaque cap and aqua blue opaque body printed with
 and 2577 on both cap and body in white ink contains 180 mg of diltiazem
hydrochloride, USP. Capsules are supplied in bottles of 30 (NDC
0228-2577-03), 90 (NDC: 0228-2577-09) and 500 (NDC: 0228-2577-50).
and 2577 on both cap and body in white ink contains 180 mg of diltiazem
hydrochloride, USP. Capsules are supplied in bottles of 30 (NDC
0228-2577-03), 90 (NDC: 0228-2577-09) and 500 (NDC: 0228-2577-50).240 mg — Each #0EL capsule with dark green opaque cap and body printed with
 and 2578 on both cap and body in white ink contains 240 mg of diltiazem
hydrochloride, USP. Capsules are supplied in bottles of 30 (NDC
0228-2578-03), 90 (NDC: 0228-2578-09) and 500 (NDC: 0228-2578-50).
and 2578 on both cap and body in white ink contains 240 mg of diltiazem
hydrochloride, USP. Capsules are supplied in bottles of 30 (NDC
0228-2578-03), 90 (NDC: 0228-2578-09) and 500 (NDC: 0228-2578-50).300 mg — Each #00 capsule with dark green opaque cap and light gray opaque body printed with
 and 2579 on both cap and body in white ink contains 300 mg of diltiazem
hydrochloride, USP. Capsules are supplied in bottles of 30 (NDC
0228-2579-03), 90 (NDC: 0228-2579-09) and 500 (NDC: 0228-2579-50).
and 2579 on both cap and body in white ink contains 300 mg of diltiazem
hydrochloride, USP. Capsules are supplied in bottles of 30 (NDC
0228-2579-03), 90 (NDC: 0228-2579-09) and 500 (NDC: 0228-2579-50).Dispense in tight, light-resistant containers as defined in the USP.
Store at 25°C (77°F); excursions permitted to 15° to 30°C (59° to 86°F).
Avoid excessive humidity.
Manufactured by:
Actavis Elizabeth LLC
200 Elmora Avenue
Elizabeth, NJ 07207 USA
40-8791
Revised — June 2011
- PRINCIPAL DISPLAY PANEL
-
INGREDIENTS AND APPEARANCE
DILTIAZEM HYDROCHLORIDE
diltiazem hydrochloride capsule, extended releaseProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 68258-6046(NDC: 0228-2577) Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength DILTIAZEM HYDROCHLORIDE (UNII: OLH94387TE) (DILTIAZEM - UNII:EE92BBP03H) DILTIAZEM HYDROCHLORIDE 180 mg Inactive Ingredients Ingredient Name Strength METHACRYLIC ACID - METHYL METHACRYLATE COPOLYMER (1:1) (UNII: 74G4R6TH13) METHACRYLIC ACID - METHYL METHACRYLATE COPOLYMER (1:2) (UNII: 5KY68S2577) AMMONIA (UNII: 5138Q19F1X) GELATIN (UNII: 2G86QN327L) HYDROXYPROPYL CELLULOSE (UNII: RFW2ET671P) PROPYLENE GLYCOL (UNII: 6DC9Q167V3) SILICON DIOXIDE (UNII: ETJ7Z6XBU4) SODIUM LAURYL SULFATE (UNII: 368GB5141J) SUCROSE (UNII: C151H8M554) STARCH, CORN (UNII: O8232NY3SJ) TALC (UNII: 7SEV7J4R1U) TITANIUM DIOXIDE (UNII: 15FIX9V2JP) TRIETHYL CITRATE (UNII: 8Z96QXD6UM) D&C YELLOW NO. 10 (UNII: 35SW5USQ3G) FD&C BLUE NO. 1 (UNII: H3R47K3TBD) FD&C GREEN NO. 3 (UNII: 3P3ONR6O1S) Product Characteristics Color green (DARK) , blue (AQUA) Score no score Shape CAPSULE Size 22mm Flavor Imprint Code R;2577 Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 68258-6046-3 30 in 1 BOTTLE Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA074984 12/20/1999 Labeler - Dispensing Solutions, Inc. (066070785) Registrant - PSS World Medical, Inc. (101822682) Establishment Name Address ID/FEI Business Operations Dispensing Solutions, Inc. 066070785 relabel, repack
© 2026 FDA.report
This site is not affiliated with or endorsed by the FDA.
