These highlights do not include all the information needed to use Ciclesonide Inhalation Aerosol safely and effectively. See full prescribing information for Ciclesonide Inhalation Aerosol. Ciclesonide Inhalation Aerosol 80 mcg, 160 mcg For Oral Inhalation Only Initial U.S. Approval: 2006
Ciclesonide by
Drug Labeling and Warnings
Ciclesonide by is a Prescription medication manufactured, distributed, or labeled by Prasco Laboratories. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
CICLESONIDE- ciclesonide aerosol, metered
Prasco Laboratories
----------
HIGHLIGHTS OF PRESCRIBING INFORMATIONThese highlights do not include all the information needed to use Ciclesonide Inhalation Aerosol safely and effectively. See full prescribing information for Ciclesonide Inhalation Aerosol.
Ciclesonide Inhalation Aerosol 80 mcg, 160 mcg For Oral Inhalation Only Initial U.S. Approval: 2006 INDICATIONS AND USAGEDOSAGE AND ADMINISTRATIONFOR ORAL INHALATION ONLY (2)
1 Prednisone should be reduced gradually, no faster than 2.5 mg/day on a weekly basis, beginning after at least 1 week of therapy with Ciclesonide Inhalation Aerosol. Patients should be carefully monitored for signs of asthma instability, including monitoring of serial objective measures of airflow, and for signs of adrenal insufficiency during steroid taper and following discontinuation of oral corticosteroid therapy [see Warnings and Precautions (5.1)]. DOSAGE FORMS AND STRENGTHSInhalation Aerosol 80 mcg/actuation or 160 mcg/actuation (3) CONTRAINDICATIONSWARNINGS AND PRECAUTIONS
ADVERSE REACTIONSMost common adverse reactions (≥ 3%) are headache, nasopharyngitis, sinusitis, pharyngolaryngeal pain, upper respiratory infection, arthralgia, nasal congestion, pain in extremity and back pain. (6) Other adverse reactions have been reported. (6) To report SUSPECTED ADVERSE REACTIONS, contact Prasco Laboratories at 1-866-525-0688 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch. See 17 for PATIENT COUNSELING INFORMATION and FDA-approved patient labeling. Revised: 8/2020 |
FULL PRESCRIBING INFORMATION
1 INDICATIONS AND USAGE
1.1 Treatment of Asthma
Ciclesonide Inhalation Aerosol is indicated for the maintenance treatment of asthma as prophylactic therapy in adult and adolescent patients 12 years of age and older.
Important Limitations of Use:
Ciclesonide Inhalation Aerosol is NOT indicated for the relief of acute bronchospasm.
Ciclesonide Inhalation Aerosol is NOT indicated for children under 12 years of age.
2 DOSAGE AND ADMINISTRATION
Ciclesonide Inhalation Aerosol should be administered by the orally inhaled route. Prime Ciclesonide Inhalation Aerosol before using for the first time by actuating 3 times prior to using the first dose from a new canister or when the inhaler has not been used for more than 10 days. Individual patients will experience a variable time to onset and degree of symptom relief. Maximum benefit may not be achieved for four weeks or longer after initiation. After asthma stability has been achieved, it is desirable to titrate to the lowest effective dosage to reduce the possibility of side effects. For patients who do not respond adequately to the starting dose after 4 weeks of therapy, higher doses may provide additional asthma control. The safety and efficacy of Ciclesonide Inhalation Aerosol when administered in excess of the highest recommended doses has not been established.
Recommended Dosages
The recommended starting dose and the highest recommended dose of Ciclesonide Inhalation Aerosol are listed in the following table.
| Previous Therapy |
Recommended | Highest Recommended Dose |
| Patients ≥ 12 years who received bronchodilators alone | 80 mcg twice daily | 160 mcg twice daily |
| Patients ≥ 12 years who received inhaled corticosteroids | 80 mcg twice daily | 320 mcg twice daily |
| Patients ≥ 12 years who received oral corticosteroids1 | 320 mcg twice daily | 320 mcg twice daily |
1 Prednisone should be reduced gradually, no faster than 2.5 mg/day on a weekly basis, beginning after at least 1 week of therapy with Ciclesonide Inhalation Aerosol. Patients should be carefully monitored for signs of asthma instability, including monitoring of serial objective measures of airflow, and for signs of adrenal insufficiency during steroid taper and following discontinuation of oral corticosteroid therapy [see Warnings and Precautions (5.1)].
3 DOSAGE FORMS AND STRENGTHS
Ciclesonide Inhalation Aerosol is available in the following two strengths: 80 mcg/actuation, and 160 mcg/actuation. The 80 mcg/actuation strength contains 60 actuations fill/canister, and the 160 mcg/actuation strength contains 60 actuations fill/canister.
Ciclesonide Inhalation Aerosol 80 mcg is supplied with a brown plastic actuator with a red dust cap.
Ciclesonide Inhalation Aerosol 160 mcg is supplied with a red plastic actuator with a red dust cap.
4 CONTRAINDICATIONS
4.1 Status Asthmaticus
Ciclesonide Inhalation Aerosol is contraindicated in the primary treatment of status asthmaticus or other acute episodes of asthma where intensive measures are required.
4.2 Hypersensitivity
Ciclesonide Inhalation Aerosol is contraindicated in patients with known hypersensitivity to ciclesonide or any of the ingredients of Ciclesonide Inhalation Aerosol. Rare cases of hypersensitivity reactions with manifestations such as angioedema, with swelling of the lips, tongue and pharynx, have been reported.
5 WARNINGS AND PRECAUTIONS
5.1 Local Effects
In clinical trials, the development of localized infections of the mouth and pharynx with Candida albicans occurred in 32 of 3038 patients treated with Ciclesonide Inhalation Aerosol. Of the 32 reported cases, 20 occurred in 1394 patients treated with a total daily dose of 320 mcg of Ciclesonide Inhalation Aerosol or higher. Most cases of Candida infection were mild to moderate. When such an infection develops, it should be treated with appropriate local or systemic (i.e., oral antifungal) therapy while remaining on treatment with Ciclesonide Inhalation Aerosol, but at times therapy with Ciclesonide Inhalation Aerosol may need to be interrupted. Patients should rinse the mouth after inhalation of Ciclesonide Inhalation Aerosol.
5.2 Acute Asthma Episodes
Ciclesonide Inhalation Aerosol is not a bronchodilator and is not indicated for rapid relief of bronchospasm or other acute episodes of asthma. Patients should be instructed to contact their physician immediately if episodes of asthma not responsive to their usual doses of bronchodilators occur during the course of treatment with Ciclesonide Inhalation Aerosol. During such episodes, patients may require therapy with oral corticosteroids.
5.3 Immunosuppression
Persons who are using drugs that suppress the immune system are more susceptible to infections than healthy individuals. Chickenpox and measles, for example, can have a more serious or even fatal course in susceptible children or adults using corticosteroids. In such children or adults who have not had these diseases or been properly immunized, particular care should be taken to avoid exposure. How the dose, route, and duration of corticosteroid administration affect the risk of developing a disseminated infection is not known. The contribution of the underlying disease and/or prior corticosteroid treatment to the risk is also not known. If exposed to chickenpox, prophylaxis with varicella zoster immune globulin (VZIG) may be indicated. If exposed to measles, prophylaxis with pooled intramuscular immunoglobulin (IG) may be indicated. (See the respective package inserts for complete VZIG and IG prescribing information.) If chickenpox develops, treatment with antiviral agents may be considered.
Inhaled corticosteroids should be used with caution, if at all, in patients with active or quiescent tuberculosis infection of the respiratory tract; untreated systemic fungal, bacterial, viral, or parasitic infections; or ocular herpes simplex.
5.4 Transferring Patients from Systemic Corticosteroid Therapy
Particular care is needed for patients who are transferred from systemically active corticosteroids to Ciclesonide Inhalation Aerosol because deaths due to adrenal insufficiency have occurred in asthmatic patients during and after transfer from systemic corticosteroids to less systemically-available inhaled corticosteroids. After withdrawal from systemic corticosteroids, a number of months are required for recovery of hypothalamic-pituitary-adrenal (HPA) function.
Patients who have been previously maintained on 20 mg or more per day of prednisone (or its equivalent) may be most susceptible, particularly when their systemic corticosteroids have been almost completely withdrawn. During this period of HPA suppression, patients may exhibit signs and symptoms of adrenal insufficiency when exposed to trauma, surgery, or infection (particularly gastroenteritis) or other conditions associated with severe electrolyte loss. Although Ciclesonide Inhalation Aerosol may provide control of asthma symptoms during these episodes, in recommended doses it supplies less than normal physiological amounts of corticosteroid systemically and does NOT provide the mineralocorticoid activity that is necessary for coping with these emergencies.
During periods of stress or a severe asthma attack, patients who have been withdrawn from systemic corticosteroids should be instructed to resume oral corticosteroids (in large doses) immediately and to contact their physicians for further instruction. These patients should also be instructed to carry a medical identification card indicating that they may need supplementary systemic corticosteroids during periods of stress or a severe asthma attack.
Patients requiring oral corticosteroids should be weaned slowly from systemic corticosteroid use after transferring to Ciclesonide Inhalation Aerosol. Prednisone reduction can be accomplished by reducing the daily prednisone dose by 2.5 mg on a weekly basis during Ciclesonide Inhalation Aerosol therapy [see Dosage and Administration (2)]. Lung function (FEV1 or AM PEFR), beta-agonist use, and asthma symptoms should be carefully monitored during withdrawal of oral corticosteroids. In addition to monitoring asthma signs and symptoms, patients should be observed for signs and symptoms of adrenal insufficiency, such as fatigue, lassitude, weakness, nausea and vomiting, and hypotension.
Transfer of patients from systemic steroid therapy to Ciclesonide Inhalation Aerosol may unmask allergic conditions previously suppressed by the systemic steroid therapy, e.g., rhinitis, conjunctivitis, eczema, arthritis, and eosinophilic conditions.
During withdrawal from oral steroids, some patients may experience symptoms of systemically active steroid withdrawal, e.g., joint and/or muscular pain, lassitude, and depression, despite maintenance or even improvement of respiratory function.
5.5 Hypercorticism and Adrenal Suppression
Ciclesonide Inhalation Aerosol will often help control asthma symptoms with less suppression of HPA function than therapeutically similar oral doses of prednisone. Since individual sensitivity to effects on cortisol production exists, physicians should consider this information when prescribing Ciclesonide Inhalation Aerosol. Particular care should be taken in observing patients postoperatively or during periods of stress for evidence of inadequate adrenal response. It is possible that systemic corticosteroid effects such as hypercorticism and adrenal suppression may appear in a small number of patients particularly when Ciclesonide Inhalation Aerosol is administered at higher than recommended doses over prolonged periods of time. If such effects occur, the dosage of Ciclesonide Inhalation Aerosol should be reduced slowly, consistent with accepted procedures for reducing systemic corticosteroids and for management of asthma.
5.6 Reduction in Bone Mineral Density
Decreases in bone mineral density (BMD) have been observed with long-term administration of products containing inhaled corticosteroids. The clinical significance of small changes in BMD with regard to long-term outcomes is unknown. Patients with major risk factors for decreased bone mineral content, such as prolonged immobilization, family history of osteoporosis, or chronic use of drugs that can reduce bone mass (e.g., anticonvulsants and oral corticosteroids) should be monitored and treated with established standards of care.
5.7 Effect on Growth
Orally inhaled corticosteroids may cause a reduction in growth velocity when administered to pediatric patients. Monitor the growth of pediatric patients receiving Ciclesonide Inhalation Aerosol routinely (e.g., via stadiometry). To minimize the systemic effects of orally inhaled corticosteroids, including Ciclesonide Inhalation Aerosol, titrate each patient’s dose to the lowest dosage that effectively controls his/her symptoms [see Use in Specific Populations (8.4)].
5.8 Glaucoma and Cataracts
Glaucoma, increased intraocular pressure, and cataracts have been reported following the administration of inhaled corticosteroids including Ciclesonide Inhalation Aerosol. Therefore, close monitoring is warranted in patients with a change in vision or with a history of increased intraocular pressure, glaucoma, and/or cataracts.
In a comparator control study of one-year treatment duration, 743 patients 18 years of age and older (mean age 43.1 years) with moderate persistent asthma were treated with Ciclesonide Inhalation Aerosol 320 mcg twice daily and 742 were treated with a labeled dose of a comparator-inhaled corticosteroid appropriate for the patient population. Patients had an ophthalmology examination that included visual acuity, intraocular pressure measurement, and a slit lamp examination at baseline, 4, 8 and 12 months. Lens opacities were graded using the Lens Opacification System III. After 52 weeks, CLASS I effects (minimally detected changes) were recorded in 36.1% of the Ciclesonide Inhalation Aerosol-treated patients and in 38.4% of patients treated with the comparator-inhaled corticosteroid. The more severe CLASS III effects were recorded in 8.1% of the Ciclesonide Inhalation Aerosol-treated patients and 9.2% of patients treated with the comparator-inhaled corticosteroid. Of those patients having a CLASS III effect, the incidence of posterior sub-capsular opacities was 0.9% and 0.5% in the Ciclesonide Inhalation Aerosol- and comparator-treated patients, respectively.
5.9 Bronchospasm
As with other inhaled asthma medications, bronchospasm, with an immediate increase in wheezing, may occur after dosing. If bronchospasm occurs following dosing with Ciclesonide Inhalation Aerosol, it should be treated immediately with a fast-acting inhaled bronchodilator. Treatment with Ciclesonide Inhalation Aerosol should be discontinued and alternative treatment should be instituted.
6 ADVERSE REACTIONS
Systemic and local corticosteroid use may result in the following:
- Candida albicans infection [see Warnings and Precautions (5.1)]
- Immunosuppression [see Warnings and Precautions (5.3)]
- Hypercorticism and adrenal suppression [see Warnings and Precautions (5.5)]
- Growth effects [see Warnings and Precautions (5.7)]
- Glaucoma and cataracts [see Warnings and Precautions (5.8)]
6.1 Clinical Trial Experience
The safety data described below for adults and adolescents 12 years of age and older reflect exposure to Ciclesonide Inhalation Aerosol in doses ranging from 80 mcg to 640 mcg twice daily in five double-blind placebo-controlled clinical trials. Studies with once daily dosing are omitted from the safety database because the doses studied once daily are lower than the highest recommended twice daily doses. The five studies were of 12 to 16 weeks treatment duration, one of which included a safety extension follow-up of one year. In the 12 to 16 week treatment studies, 720 patients (298 males and 422 females) aged 12 years and older were exposed to Ciclesonide Inhalation Aerosol. In the long-term safety trial, 197 patients (82 males and 115 females) with severe persistent asthma from one of the 12-week trials were re-randomized and treated for up to one year with Ciclesonide Inhalation Aerosol 320 mcg twice daily. Safety information for pediatric patients 4 to 11 years of age, is obtained from once daily dosing studies. Two of these studies were designed with a 12-week double-blind treatment period followed by a long-term open label safety extension of one year, and one study was an open-label safety study of one-year duration [see Pediatric Use (8.4)].
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Adults and Adolescents 12 Years of Age and Older
Four of the five trials included a total of 624 patients ages 12 years and older (359 females and 265 males) with asthma of varying severity who were treated with Ciclesonide Inhalation Aerosol 80 mcg, 160 mcg, or 320 mcg twice daily for 12 to 16 weeks. These studies included patients previously using either controller therapy (predominantly inhaled corticosteroids) or reliever therapy (bronchodilator therapy alone). In these trials, the mean age was 39.1 years, and the majority of the patients (79.0%) were Caucasian. In these trials, 52.3%, 59.8% and 54.1% of the patients in the Ciclesonide Inhalation Aerosol 80 mcg, 160 mcg, and 320 mcg treatment groups, respectively, had at least one adverse event compared to 58.0% in the placebo group.
Table 1 includes adverse reactions for the recommended doses of Ciclesonide Inhalation Aerosol that occurred at an incidence of ≥ 3% in any of the Ciclesonide Inhalation Aerosol groups and which were more frequent with Ciclesonide Inhalation Aerosol compared to placebo.
| Adverse Reaction | Placebo (N=507) % | Ciclesonide Inhalation Aerosol | ||
| 80 mcg BID (N=325) % | 160 mcg BID (N=127) % |
320 mcg BID |
||
| Headache | 7.3 | 4.9 | 11.0 | 8.7 |
| Nasopharyngitis | 7.5 | 10.5 | 8.7 | 7.0 |
| Sinusitis | 3.0 | 3.1 | 5.5 | 5.2 |
| Pharyngolaryngeal pain | 4.3 | 4.3 | 2.4 | 4.7 |
| Upper respiratory Inf. | 6.5 | 7.1 | 8.7 | 4.1 |
| Arthralgia | 1.0 | 0.9 | 2.4 | 3.5 |
| Nasal congestion | 1.6 | 1.8 | 5.5 | 2.9 |
| Pain in extremity | 1.0 | 0.3 | 3.1 | 2.3 |
| Back pain | 2.0 | 0.6 | 3.1 | 1.2 |
The following adverse reactions occurred in these clinical trials using Ciclesonide Inhalation Aerosol with an incidence of less than 1% and occurred at a greater incidence with Ciclesonide Inhalation Aerosol than with placebo.
Infections and Infestations: Oral candidiasis
Respiratory Disorders: Cough
Gastrointestinal Disorders: Dry mouth, nausea
General Disorders and Administrative Site Conditions: Chest discomfort
Respiratory, Thoracic, and Mediastinal Disorders: Dysphonia, dry throat
The fifth study was a 12-week clinical trial in asthma patients 12 years of age and older who previously required oral corticosteroids (average daily dose of oral prednisone of 12 mg/day), in which the effects of Ciclesonide Inhalation Aerosol 320 mcg twice daily (n = 47) and 640 mcg twice daily (n = 49) were compared with placebo (n = 45) for the frequency of reported adverse reactions. The following adverse reactions occurred at an incidence of ≥ 3% in the Ciclesonide Inhalation Aerosol-treated patients and were more frequent compared to placebo: sinusitis, hoarseness, oral candidiasis, influenza, pneumonia, nasopharyngitis, arthralgia, back pain, musculoskeletal chest pain, headache, urticaria, dizziness, gastroenteritis, face edema, fatigue, and conjunctivitis.
Pediatric Patients less than 12 Years of Age
The safety of Ciclesonide Inhalation Aerosol in pediatric patients 4 to 11 years of age was evaluated in two studies in which Ciclesonide Inhalation Aerosol 40 mcg, 80 mcg, and 160 mcg was administered once daily for 12 weeks and in one study in pediatric patients 2 to 6 years of age in which Ciclesonide Inhalation Aerosol 40 mcg, 80 mcg, and 160 mcg was administered once daily for 24 weeks. Studies have not been conducted in patients less than 2 years of age [see Pediatric Use (8.4)].
Long-Term Clinical Trials Experience
A total of 197 patients 12 years of age and older (82 males and 115 females) from one of the 12-week treatment placebo-controlled studies were re-randomized to ciclesonide 320 mcg twice daily and followed for one year. The safety profile from the one-year follow-up was similar to that seen in the 12- and 16-week treatment studies. Long-term safety information for pediatric patients 4 to 11 years of age is obtained from three open-label one-year safety studies [see Pediatric Use (8.4)].
6.2 Post-marketing Experience
In addition to adverse reactions identified from clinical trials, the following adverse reactions have been identified during worldwide post-marketing use of ciclesonide oral inhalation. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Immune System Disorders: Immediate or delayed hypersensitivity reactions such as angioedema with swelling of the lips, tongue and pharynx.
7 DRUG INTERACTIONS
In clinical studies, concurrent administration of ciclesonide and other drugs commonly used in the treatment of asthma (albuterol, formoterol) had no effect on pharmacokinetics of des-ciclesonide [see Clinical Pharmacology (12.3)].
In vitro studies and clinical pharmacology studies suggested that des-ciclesonide has no potential for metabolic drug interactions or protein binding-based drug interactions [see Clinical Pharmacology (12.3)].
In a drug interaction study, co-administration of orally inhaled ciclesonide and oral ketoconazole, a potent inhibitor of cytochrome P450 3A4, increased the exposure (AUC) of des-ciclesonide by approximately 3.6-fold at steady state, while levels of ciclesonide remained unchanged.
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Teratogenic Effects: Pregnancy Category C
Oral administration of ciclesonide in rats up to 900 mcg/kg/day (approximately 10 times the maximum human daily inhalation dose based on mcg/m2/day) produced no teratogenicity or other fetal effects. However, subcutaneous administration of ciclesonide in rabbits at 5 mcg/kg/day (less than the maximum human daily inhalation dose based on mcg/m2/day) or greater produced fetal toxicity. This included fetal loss, reduced fetal weight, cleft palate, skeletal abnormalities including incomplete ossifications, and skin effects. No toxicity was observed at 1 mcg/kg (less than the maximum human daily inhalation dose based on mcg/m2).
There are no adequate and well-controlled studies in pregnant women. Ciclesonide Inhalation Aerosol should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus. Experience with oral corticosteroids since their introduction in pharmacologic as opposed to physiologic doses suggests that rodents are more prone to teratogenic effects from corticosteroids than humans. In addition, because there is a natural increase in corticosteroid production during pregnancy, most women will require a lower exogenous corticosteroid dose and many will not need corticosteroid treatment during pregnancy.
Non-teratogenic Effects: Hypoadrenalism may occur in infants born of mothers receiving corticosteroids during pregnancy. Such infants should be carefully monitored.
8.3 Nursing Mothers
It is not known if ciclesonide is secreted in human milk. However, other corticosteroids are excreted in human milk. In a study with lactating rats, minimal, but detectable levels of ciclesonide were recovered in milk. Caution should be used when Ciclesonide Inhalation Aerosol is administered to nursing women.
8.4 Pediatric Use
The safety and effectiveness of Ciclesonide Inhalation Aerosol in children under 12 years of age have not been established.
Two randomized, double-blind, placebo-controlled studies were conducted to evaluate the efficacy of Ciclesonide Inhalation Aerosol 40, 80, or 160 mcg administered once daily for 12 weeks in patients 4 to 11 years of age with asthma. These studies included 1018 patients previously using either controller therapy (predominately inhaled corticosteroids) or reliever therapy (bronchodilator therapy alone). The patients had a mean baseline percent predicted FEV1 of 68%. The primary efficacy endpoint was morning pre-dose FEV1. Other measures of efficacy included AM PEF, asthma symptoms, and rescue albuterol use. The studies showed inconsistent results and do not establish the efficacy of Ciclesonide Inhalation Aerosol in patients 4 to 11 years of age.
One randomized, double-blind, placebo-controlled study was conducted to evaluate the efficacy of Ciclesonide Inhalation Aerosol 40, 80, and 160 mcg administered once daily for 24 weeks in 992 patients 2 to 6 years of age with persistent asthma. The primary efficacy endpoint was time to the first severe asthma exacerbation [defined as worsening of asthma which required treatment with systemic (including oral) steroids or any other asthma medication besides treatment medication and rescue medication] or lack of improvement, whichever occurred first. No statistically significant differences were observed for the individual comparisons of Ciclesonide Inhalation Aerosol 40, 80, and 160 mcg to placebo. Results from this study did not establish efficacy of Ciclesonide Inhalation Aerosol in patients 2 to 6 years of age.
The safety of Ciclesonide Inhalation Aerosol was evaluated in 957 children between the ages of 4 and 11 and 747 children between the ages of 2 and 6 years of age who were treated with Ciclesonide Inhalation Aerosol in the three controlled clinical studies, two open-label one-year safety extensions of the controlled clinical studies, and one open-label safety study. In the controlled studies, the distribution of adverse events in the Ciclesonide Inhalation Aerosol and placebo groups was similar. The type of adverse events reported were similar to events reported in this patient population with other inhaled corticosteroids. The open-label safety studies in children 4 to 11 years of age compared the safety of Ciclesonide Inhalation Aerosol in doses up to 160 mcg once daily with an orally inhaled corticosteroid comparator. The types of adverse events seen were similar to those seen in the 12-week controlled studies.
Studies in children under 2 years of age have not been conducted given the lack of efficacy observed in patients 2 to 11 years of age.
Controlled clinical studies have shown that orally inhaled corticosteroids may cause a reduction in growth velocity in pediatric patients. In these studies, the mean reduction in growth velocity was approximately one centimeter per year (range 0.3 to 1.8 cm per year) and appears to be related to dose and duration of exposure. This effect has been observed in the absence of laboratory evidence of hypothalamic-pituitary-adrenal (HPA) axis suppression, suggesting that growth velocity is a more sensitive indicator of systemic corticosteroid exposure in pediatric patients than some commonly used tests of HPA axis function. The long-term effects of this reduction in growth velocity associated with orally inhaled corticosteroids, including the impact on final adult height, are unknown. The potential for "catch up" growth following discontinuation of treatment with orally inhaled corticosteroids has not been adequately studied. The growth of pediatric patients receiving orally inhaled corticosteroids, including Ciclesonide Inhalation Aerosol, should be monitored routinely (e.g., via stadiometry).
A 52-week, multi-center, double-blind, randomized, placebo-controlled, parallel-group study was conducted to assess the effect of orally inhaled ciclesonide on growth rate in 609 pediatric patients with mild persistent asthma, aged 5 to 8.5 years. Treatment groups included orally inhaled ciclesonide 40 mcg or 160 mcg or placebo given once daily. Growth was measured by stadiometer height during the baseline, treatment and follow-up periods. The primary comparison was the difference in growth rates between ciclesonide 40 mcg and 160 mcg and placebo groups. Conclusions cannot be drawn from this study because compliance could not be assured. There was no difference in efficacy measures between the placebo and the Ciclesonide Inhalation Aerosol groups. Ciclesonide blood levels were also not measured during the one-year treatment period.
The potential growth effects of prolonged treatment with orally inhaled corticosteroids should be weighed against clinical benefits obtained and the availability of safe and effective noncorticosteroid treatment alternatives. To minimize the systemic effects of orally inhaled corticosteroids, including Ciclesonide Inhalation Aerosol, each patient should be titrated to his/her lowest effective dose.
8.5 Geriatric Use
Clinical studies of Ciclesonide Inhalation Aerosol did not include sufficient numbers of patients aged 65 years and older to determine whether they respond differently than younger patients. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range reflecting the greater frequency of decreased hepatic, renal, or cardiac function and of concomitant disease or other drug therapy.
10 OVERDOSAGE
Chronic overdosage may result in signs/symptoms of hypercorticism [see Warnings and Precautions (5.5)]. Ciclesonide Inhalation Aerosol was well tolerated following inhalation by healthy subjects of single doses of 2880 mcg. A single oral dose of up to 10 mg of ciclesonide in healthy subjects was well tolerated and serum cortisol levels were virtually unchanged in comparison with placebo treatment. Adverse reactions were of mild or moderate severity.
The median lethal doses in mice and rats after single oral and intraperitoneal administration were > 2000 mg/kg and > 200 mg/kg, respectively. These doses are > 12000 and > 2500 times the maximum recommended daily inhalation dose in adults on a mg/m2 basis.
11 DESCRIPTION
The active component of Ciclesonide Inhalation Aerosol 80 mcg, and Ciclesonide Inhalation Aerosol 160 mcg is ciclesonide, a non-halogenated glucocorticoid having the chemical name pregna-1,4-diene-3,20-dione, 16,17-[[(R)-cyclohexylmethylene]bis(oxy)]-11-hydroxy-21-(2-methyl-1-oxopropoxy)-,(11β,16α). The empirical formula is C32H44O7 and its molecular weight is 540.7. Its structural formula is as follows:
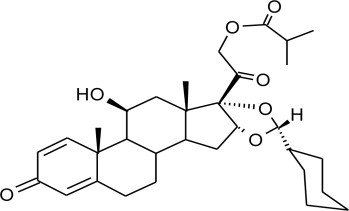
Ciclesonide is a white to yellow-white powder. It is soluble in dehydrated alcohol, acetone, dichloromethane, and chloroform.
Ciclesonide Inhalation Aerosol 80 mcg and Ciclesonide Inhalation Aerosol 160 mcg are pressurized, metered-dose aerosol units fitted with a dose indicator. Ciclesonide Inhalation Aerosol is intended for oral inhalation only. Each unit contains a solution of ciclesonide in propellant HFA-134a (1,1,1,2 tetrafluoroethane) and ethanol. After priming, Ciclesonide Inhalation Aerosol 80 mcg delivers 100 mcg from the valve and 80 mcg of ciclesonide from the actuator. Ciclesonide Inhalation Aerosol 160 mcg delivers 200 mcg from the valve and 160 mcg of ciclesonide from the actuator. This product delivers 50 microliters (59.3 milligrams) of solution as a fine particle mist from the valve with each actuation. The actual amount of drug delivered to the lung may depend on patient factors, such as the coordination between the actuation of the device and inspiration through the delivery system. Ciclesonide Inhalation Aerosol should be “primed” by actuating 3 times prior to using the first dose from a new canister or when the inhaler has not been used for more than 10 days. Avoid spraying in the eyes or face while priming Ciclesonide Inhalation Aerosol.
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Ciclesonide is a prodrug that is enzymatically hydrolyzed to a pharmacologically active metabolite, C21-desisobutyryl-ciclesonide (des-ciclesonide or RM1) following oral inhalation. Des-ciclesonide has anti-inflammatory activity with affinity for glucocorticoid receptors that is 120 times greater than the parent compound and 12 times greater than dexamethasone. The clinical significance of these findings is unknown.
The precise mechanisms of corticosteroid action in asthma are unknown. Inflammation is recognized as an important component in the pathogenesis of asthma. Corticosteroids have been shown to have a wide range of inhibitory activities against multiple cell types (e.g., mast cells, eosinophils, basophils, lymphocytes, macrophages, and neutrophils) and mediators (e.g., histamine, eicosanoids, leukotrienes, and cytokines) involved in the asthmatic response. These anti-inflammatory actions of corticosteroids may contribute to their efficacy in asthma. Though effective for the treatment of asthma, corticosteroids do not affect asthma symptoms immediately. Individual patients will experience a variable time to onset and degree of symptom relief. Maximum benefit may not be achieved for four weeks or longer after starting treatment. When corticosteroids are discontinued, asthma stability may persist for several days or longer.
12.2 Pharmacodynamics
The effect of ciclesonide by oral inhalation on the HPA axis was assessed in adults with mild asthma in a 29-day placebo-controlled study. Twenty-four-hour urinary-free cortisol was assessed in a total of 59 adults who were randomized to 320 mcg or 640 mcg Ciclesonide Inhalation Aerosol, a comparator corticosteroid, or placebo twice daily. At the end of 29 days of treatment, the mean (SE) change from baseline in 24-hr urinary-free cortisol was -8.69 (5.6) mcg/day, -4.01 (5.03) mcg/day, and -8.84 (5.02) mcg/day for the placebo, Ciclesonide Inhalation Aerosol 640 mcg/day, and Ciclesonide Inhalation Aerosol 1280 mcg/day, respectively. The difference from placebo for the change from baseline in 24-hr urinary-free cortisol was +4.7 mcg/day [95% CI: -10.58; 19.93] and -0.16 mcg/day [95% CI: -15.20; 14.89] for the 640 mcg/day or 1280 mcg/day treatments, respectively. The effects observed with the comparator corticosteroid validate the sensitivity of the study to assess the effect of ciclesonide on the HPA axis.
12.3 Pharmacokinetics
Absorption
Ciclesonide and des-ciclesonide have negligible oral bioavailability (both are less than 1%) due to low gastrointestinal absorption and high first-pass metabolism. Serum concentrations of ciclesonide and des-ciclesonide were measured and compared following oral inhalation of 1280 mcg Ciclesonide Inhalation Aerosol and intravenous administration of 800 mcg ciclesonide. The absolute bioavailability of ciclesonide was 22% and the relative systemic exposure of des-ciclesonide was 63%. The mean Cmax for des-ciclesonide was 1.02 ng/mL (range 0.6-1.5 ng/mL) in asthmatic patients following a single dose of 1280 mcg by oral inhalation. The mean Cmax (0.369 ng/mL) and AUC0-∞ (2.18 nghr/mL) of des‑ciclesonide following multiple dose administration of ciclesonide 320 mcg once daily increased up to 26% compared to single dose administration.
Distribution
Following intravenous administration of 800 mcg of ciclesonide, the volumes of distribution of ciclesonide and des-ciclesonide was approximately 2.9 L/kg and 12.1 L/kg, respectively. The percentage of ciclesonide and des-ciclesonide bound to human plasma proteins averaged ≥ 99% each, with ≤ 1% of unbound drug detected in the systemic circulation. Des-ciclesonide is not significantly bound to human transcortin.
Metabolism
Ciclesonide is hydrolyzed to a biologically active metabolite, des-ciclesonide, by esterases. Des-ciclesonide undergoes further metabolism in the liver to additional metabolites mainly by the cytochrome P450 (CYP) 3A4 isozyme and to a lesser extent by CYP 2D6. The full range of potentially active metabolites of ciclesonide has not been characterized. After intravenous administration of 14C-ciclesonide, 19.3% of the resulting radioactivity in the plasma is accounted for by ciclesonide or des-ciclesonide; the remainder may be a result of other, as yet, unidentified multiple metabolites.
Elimination
Following intravenous administration of 800 mcg of ciclesonide, the clearances of ciclesonide and des-ciclesonide were high (approximately 152 L/L/hr and 228 L/L/hr, respectively). 14C-labeled ciclesonide was predominantly excreted via the feces after intravenous administration (66%) indicating that excretion through bile is the major route of elimination. Approximately 20% or less of des-ciclesonide was excreted in the urine. The mean half-life of ciclesonide and des-ciclesonide was 0.71 hours and 6 to 7 hours, respectively. Tmax of des-ciclesonide occurs at 1.04 hours following inhalation of ciclesonide.
Special Populations
Population pharmacokinetic analysis showed that characteristics of des-ciclesonide after oral inhalation of ciclesonide were not appreciably influenced by a variety of subject characteristics such as body weight, age, race, and gender.
Renal Insufficiency
Studies in renally-impaired patients were not conducted since renal excretion of des-ciclesonide is a minor route of elimination (≤ 20%).
Hepatic Insufficiency
Compared to healthy subjects, the systemic exposure of des-ciclesonide (Cmax and AUC) in patients with moderate to severe liver impairment increased in the range of 1.4 to 2.7 fold after 1280 mcg ex-actuator ciclesonide by oral inhalation. Dose adjustment in patients with liver impairment is not necessary.
Pediatric
In two clinical safety and efficacy studies conducted in patients 4 to 11 years of age with asthma, population pharmacokinetic samples were obtained in 53 patients for pharmacokinetic analysis. In these pediatric patients, treated with daily doses of 40, 80 or 160 mcg of Ciclesonide Inhalation Aerosol, the median (min, max) Cmax values of des-ciclesonide were 41 pg/mL (not detectable, 146 pg/mL) (n=11), 113 pg/mL (35, 237 pg/mL) (n=13) and 128 pg/mL (12, 357 pg/mL) (n=14), respectively.
Drug-Drug Interactions
In a drug interaction study, co-administration of orally inhaled ciclesonide and oral ketoconazole, a potent inhibitor of cytochrome P450 3A4, increased the exposure (AUC) of ciclesonide active metabolite, des-ciclesonide, by approximately 3.6-fold at steady state, while levels of ciclesonide remained unchanged [see Drug Interactions (7)].
In another single-dose drug interaction study, co-administration of orally inhaled ciclesonide and oral erythromycin, an inhibitor of cytochrome P450 3A4, had no effect on the pharmacokinetics of either ciclesonide and the active metabolite, des-ciclesonide, or erythromycin.
Based on in vitro studies in human liver microsomes, des-ciclesonide had no significant potential to inhibit or induce the metabolism of other drugs metabolized by CYP450 enzymes. The inhibitory potential of ciclesonide on CYP450 isoenzymes has not been studied. Based on in vitro human hepatocyte studies, ciclesonide and des-ciclesonide had no potential to induce major CYP450 isozymes.
In vitro studies demonstrated that the plasma protein binding of des-ciclesonide was not affected by warfarin or salicylic acid, indicating no potential for protein binding-based drug interactions.
In a population pharmacokinetic analysis including 98 subjects, co-administration of Ciclesonide Inhalation Aerosol and albuterol had no effect on the pharmacokinetics of des-ciclesonide.
Concomitant administration of Ciclesonide Inhalation Aerosol (640 mcg) and formoterol (24 mcg) did not change the pharmacokinetics of either des-ciclesonide or formoterol.
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Ciclesonide demonstrated no carcinogenic potential in a study of oral doses up to 900 mcg/kg/day (approximately 6 times the maximum human daily inhalation dose based on mcg/m2/day) in mice for 104 weeks and in a study of inhalation doses up to 193 mcg/kg/day (approximately 2 times the maximum human daily inhalation dose based on mcg/m2/day) in rats for 104 weeks.
Ciclesonide was not mutagenic in an Ames test or in a forward mutation assay and was not clastogenic in a human lymphocyte assay or in an in vitro micronucleus test. However, ciclesonide was clastogenic in the in vivo mouse micronucleus test. The concurrent reference corticosteroid (dexamethasone) in this study showed similar findings.
No evidence of impairment of fertility was observed in a reproductive study conducted in male and female rats both dosed orally up to 900 mcg/kg/day (approximately 10 times the maximum human daily inhalation dose based on mcg/m2/day).
14 CLINICAL STUDIES
14.1 Asthma
Adults and Adolescents 12 Years of Age and Older
The efficacy of Ciclesonide Inhalation Aerosol was evaluated in six randomized, double-blind, placebo-controlled, parallel-group clinical trials in adult and adolescent patients 12 years of age and older with mild persistent to severe persistent asthma. The six trials included two trials in which patients were treated with Ciclesonide Inhalation Aerosol administered once daily for 12 weeks, two trials in which patients were treated with Ciclesonide Inhalation Aerosol twice daily for 12 weeks, and two trials in which patients were treated with Ciclesonide Inhalation Aerosol using once daily and twice daily dosing regimens for 12 or 16 weeks. These trials included a total of 2843 patients (1167 males and 1676 females) of whom 296 were adolescents 12-17 years of age. The primary efficacy endpoint in four of the six trials was the mean change from baseline in pre-dose FEV1 at endpoint (last observation). FEV1 was measured prior to the morning dose of study medication (at the end of the 24-hour dosing interval for once daily administration, and at the end of the 12-hour dosing interval for twice daily administration). In one of the six trials, the primary endpoint was the change from baseline in the average of the pre-dose FEV1 at Weeks 12 and 16, and in another trial, reduction of oral corticosteroid use was the primary efficacy endpoint. Additional efficacy variables were asthma symptoms, use of albuterol for rescue, AM PEF, nighttime awakenings, and withdrawal due to asthma worsening.
The two once daily dosing trials were identically designed and were conducted to evaluate the efficacy of Ciclesonide Inhalation Aerosol 80, 160, and 320 mcg given once daily in the morning for 12 weeks in patients with mild to moderate asthma maintained on inhaled bronchodilators and/or corticosteroids. The results of these trials, along with other trials that explored twice daily dosing, indicate that once daily dosing is not the optimum dosing regimen for Ciclesonide Inhalation Aerosol .
Four trials were designed to evaluate the efficacy of Ciclesonide Inhalation Aerosol administered twice daily in patients with asthma who were previously maintained on bronchodilators alone, patients who were previously maintained on inhaled corticosteroids, and patients who were previously maintained on oral corticosteroids.
Patients Previously Maintained on Bronchodilators Alone
The efficacy of Ciclesonide Inhalation Aerosol was studied in a randomized, double-blind, placebo-controlled trial in 691 patients with mild-to-moderate persistent asthma (mean baseline percent predicted FEV1 of 72%) previously using reliever therapy (bronchodilator therapy alone). In this trial, patients were treated with Ciclesonide Inhalation Aerosol 160 mcg once daily in the morning for 16 weeks, Ciclesonide Inhalation Aerosol 80 mcg twice daily for 16 weeks, or Ciclesonide Inhalation Aerosol 80 mcg twice daily for 4 weeks followed by Ciclesonide Inhalation Aerosol 160 mcg once daily in the morning for 12 weeks or placebo for 16 weeks. Compared to placebo, all Ciclesonide Inhalation Aerosol doses showed statistically significant improvement at Week 16 in AM pre-dose FEV1. However, the increase in AM pre-dose FEV1 in the patients treated with Ciclesonide Inhalation Aerosol 80 mcg twice daily was significantly greater than that observed in patients treated with Ciclesonide Inhalation Aerosol 160 mcg administered once daily. Compared to placebo, increases in AM pre-dose FEV1 were 0.12 L or 5.0% for Ciclesonide Inhalation Aerosol 160 mcg once daily, 0.24 L or 10.4% for Ciclesonide Inhalation Aerosol 80 mcg twice daily, 0.13 L or 5.0% for Ciclesonide Inhalation Aerosol 80 mcg twice daily for 4 weeks followed by Ciclesonide Inhalation Aerosol 160 mcg once daily. Other measures of asthma control, AM PEF, and need for rescue albuterol also improved in all the Ciclesonide Inhalation Aerosol treatment groups compared to placebo but the improvement was greatest with the Ciclesonide Inhalation Aerosol 80 mcg twice daily treatment arm. Discontinuations from the study for lack of efficacy were lower in the Ciclesonide Inhalation Aerosol treatment groups compared to placebo. Fewer patients receiving Ciclesonide Inhalation Aerosol experienced asthma worsening than did patients receiving placebo. The AM pre-dose FEV1 results are shown in Figure 1 below.
Figure 1: A 16-Week Double-Blind Clinical Trial Evaluating Ciclesonide Inhalation Aerosol Administered Once Daily, Twice Daily, or Twice Daily Initially for 4 Weeks Followed by Once Daily for 12 Weeks, in Adult and Adolescent Patients with Mild-to-Moderate Asthma Previously Maintained on Bronchodilators Alone:
Mean Change from Baseline in FEV1 (L) prior to AM dose
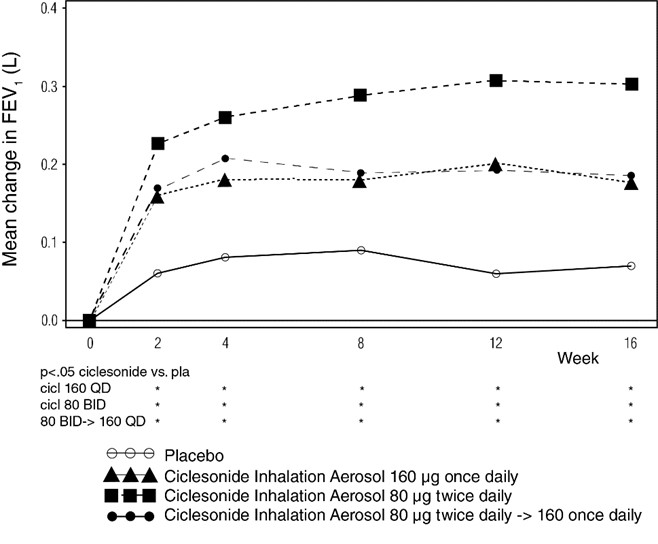
Patients Previously Maintained on Inhaled Corticosteroids
The efficacy of Ciclesonide Inhalation Aerosol in asthma patients previously maintained on inhaled corticosteroids was evaluated in two randomized, double-blind, placebo-controlled trials of 12-weeks treatment duration. In one trial, asthmatic patients with mild to moderate persistent asthma (mean baseline percent predicted FEV1 of 79%), previously maintained on controller therapy (predominantly inhaled corticosteroids) were treated with Ciclesonide Inhalation Aerosol 160 mcg once daily in the morning, Ciclesonide Inhalation Aerosol 80 mcg twice daily or placebo.
The AM pre-dose FEV1 results are shown in Figure 2 below.
Figure 2: A 12-Week Double-Blind Clinical Trial Evaluating Ciclesonide Inhalation Aerosol Administered Once and Twice Daily in Adult and Adolescent Patients with Mild-to-Moderate Asthma Previously Maintained on Inhaled Corticosteroids:
Mean Change from Baseline in FEV1 (L) prior to AM dose
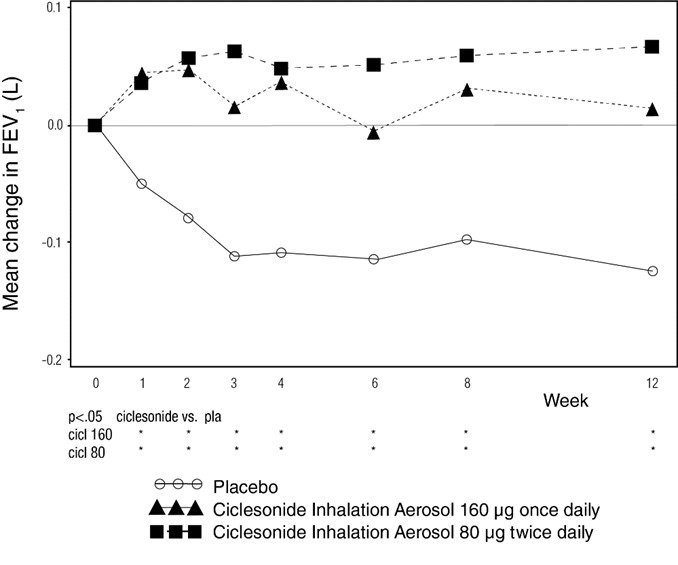
Statistically significantly more increases in AM pre-dose FEV1 compared to placebo were seen at 12 weeks for Ciclesonide Inhalation Aerosol 160 mcg once daily (0.14 L or 5.7%) and Ciclesonide Inhalation Aerosol 80 mcg twice daily (0.19 L or 7.5%). Asthma symptoms scores, AM PEF, and decreased need for rescue albuterol remained relatively stable in the Ciclesonide Inhalation Aerosol treatment groups compared to slight worsening in the placebo. Compared to placebo, fewer patients receiving Ciclesonide Inhalation Aerosol experienced worsening of asthma.
In the other trial, 257 patients with moderate to severe persistent asthma (mean baseline percent predicted FEV1 of 54%) were treated with Ciclesonide Inhalation Aerosol 160 or 320 mcg twice daily for 12 weeks. The AM pre-dose FEV1 results are shown in Figure 3 below.
Figure 3: A 12-Week Double-Blind Clinical Trial Evaluating Ciclesonide Inhalation Aerosol Administered Twice Daily in Adult and Adolescent Patients with Severe Asthma:
Mean Change from Baseline in FEV1 (L) prior to AM dose
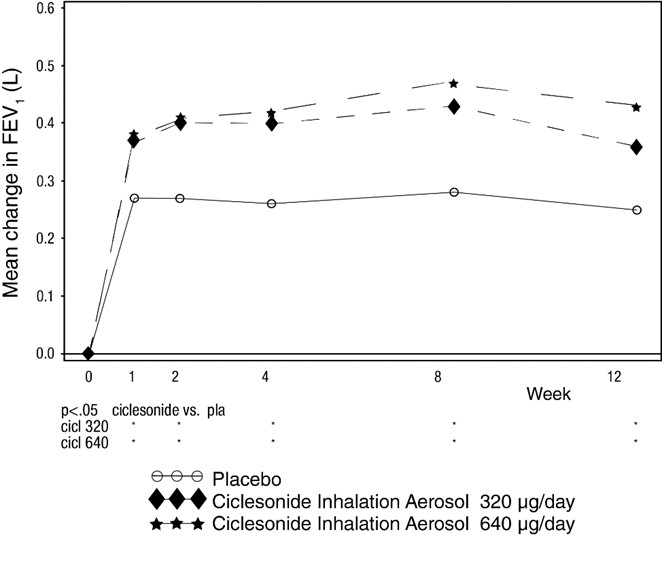
Compared to placebo, both Ciclesonide Inhalation Aerosol doses showed statistically significantly more improvement in pre-dose FEV1 (0.11 L or 8.6% and 0.18 L or 11.8%). Other measures of asthma control, AM PEF, symptoms, and need for rescue albuterol also showed improvement compared to placebo. Compared to placebo, fewer patients treated with Ciclesonide Inhalation Aerosol experienced worsening of asthma.
Patients treated with Ciclesonide Inhalation Aerosol were also less likely to discontinue study participation due to asthma deterioration.
Patients Previously Maintained on Oral Corticosteroids
In a 12-week double-blind clinical trial, 140 patients with severe persistent asthma (mean FEV1 at baseline 53% predicted) who had failed prior efforts to eliminate oral prednisone use and had established their lowest effective prednisone dose were randomized to Ciclesonide Inhalation Aerosol given by inhalation aerosol at doses of 320 or 640 mcg twice daily or placebo. The average prednisone dose at baseline was approximately 12 mg/day. Compared to patients on placebo whose prednisone requirements increased by 4%, those treated with Ciclesonide Inhalation Aerosol 320 mcg and 640 mcg twice daily significantly reduced their prednisone requirements by 47% and 62%, respectively. At the same time, patients on Ciclesonide Inhalation Aerosol maintained asthma control as reflected by lung function, symptoms, and need for rescue albuterol. A significantly larger percentage of patients on Ciclesonide Inhalation Aerosol were able to reduce oral prednisone use by 50% or more as compared to placebo (64% and 77% of the patients treated with 320 mcg and 640 mcg, respectively twice daily as compared with 33% of patients on placebo). There was no statistically significant difference observed with Ciclesonide Inhalation Aerosol 640 mcg twice daily compared to Ciclesonide Inhalation Aerosol 320 mcg twice daily.
Pediatric Patients less than 12 Years of Age
Two identically designed randomized, double-blind, parallel, placebo-controlled clinical trials of 12-weeks treatment duration were conducted in 1018 patients aged 4 to 11 years with asthma but efficacy was not established. In addition, one randomized, double-blind, parallel, placebo-controlled clinical trial did not establish efficacy in 992 patients aged 2 to 6 years with asthma. Clinical trials have not been conducted in pediatric patients less than 2 years of age [see Pediatric Use (8.4)].
16 HOW SUPPLIED/STORAGE AND HANDLING
Ciclesonide Inhalation Aerosol is available in the following strengths and canister presentations.
|
Micrograms per Actuation
|
Number of
|
Canister Weight
|
Canister per Box
|
NDC Number
|
| Ciclesonide Inhalation Aerosol 80 mcg | 60 | 6.1 g | 1 | 66993-571-64 |
| Ciclesonide Inhalation Aerosol 160 mcg | 60 | 6.1 g | 1 | 66993-572-64 |
Ciclesonide Inhalation Aerosol 80 mcg Inhalation Aerosol is supplied with a brown plastic actuator with a red dust cap. Each actuation of the inhaler delivers 80 mcg of ciclesonide from the actuator.
Ciclesonide Inhalation Aerosol 160 mcg Inhalation Aerosol is supplied with a red plastic actuator with a red dust cap. Each actuation of the inhaler delivers 160 mcg of ciclesonide from the actuator.
Ciclesonide Inhalation Aerosol canisters are for use with Ciclesonide Inhalation Aerosol Inhalation Aerosol actuators only. The actuators are fitted with a dose indicator and should not be used with other inhalation aerosol medications. The correct amount of medication in each actuation cannot be assured from the canister labeled to contain 60 actuations when the dose indicator display window shows zero even though the canister is not completely empty. The canister should be discarded when the dose indicator display window shows zero.
Store at 25°C (77°F).
Excursions between 15° and 30°C (59° and 86°F) are permitted (see USP). For optimal results, the canister should be at room temperature when used. Keep out of reach of children.
CONTENTS UNDER PRESSURE
Do not puncture. Do not use or store near heat or open flame. Exposure to temperatures above 49°C (120°F) may cause bursting. Never throw canister into fire or incinerator.
17 PATIENT COUNSELING INFORMATION
See FDA-Approved Patient Labeling accompanying the product.
17.1 Oral Candidiasis
Patients should be advised that localized infections with Candida albicans occurred in the mouth and pharynx in some patients. If oropharyngeal candidiasis develops, it should be treated with appropriate local or systemic (i.e., oral) antifungal therapy while still continuing with Ciclesonide Inhalation Aerosol therapy, but at times therapy with the Ciclesonide Inhalation Aerosol inhaler may need to be temporarily interrupted under close medical supervision. Rinsing the mouth after inhalation is advised.
17.2 Status Asthmaticus and Acute Asthma Symptoms
Patients should be advised that Ciclesonide Inhalation Aerosol is not a bronchodilator and is not intended for use as rescue medication for acute asthma exacerbations. Acute asthma symptoms should be treated with an inhaled, short-acting beta2-agonist such as albuterol. The patient should be instructed to contact their physician immediately if there is deterioration of their asthma.
17.3 Immunosuppression
Patients who are on immunosuppressant doses of corticosteroids should be warned to avoid exposure to chickenpox or measles and, if exposed, to consult their physician without delay. Patients should be informed of potential worsening of existing tuberculosis, fungal, bacterial, viral, or parasitic infections, or ocular herpes simplex.
17.4 Hypercorticism and Adrenal Suppression
Patients should be advised that Ciclesonide Inhalation Aerosol may cause systemic corticosteroid effects of hypercorticism and adrenal suppression. Additionally, patients should be instructed that deaths due to adrenal insufficiency have occurred during and after transfer from systemic corticosteroids. Patients should taper slowly from systemic corticosteroids if transferring to Ciclesonide Inhalation Aerosol.
17.5 Reduction in Bone Mineral Density
Patients who are at an increased risk for decreased BMD should be advised that the use of corticosteroids may pose an additional risk and should be monitored and where appropriate, be treated for this condition.
17.6 Reduced Growth Velocity
Patients should be informed that orally inhaled corticosteroids, including Ciclesonide Inhalation Aerosol, may cause a reduction in growth velocity when administered to pediatric patients. Physicians should closely follow the growth of children and adolescents taking corticosteroids by any route.
17.7 Use Daily for Best Effect
Patients should be advised to use Ciclesonide Inhalation Aerosol at regular intervals, since its effectiveness depends on regular use. Maximum benefit may not be achieved for four weeks or longer after starting treatment. The patient should not increase the prescribed dosage but should contact their physician if symptoms do not improve or if the condition worsens. Patients should be instructed not to stop Ciclesonide Inhalation Aerosol use abruptly. Patients should contact their physician immediately if use of Ciclesonide Inhalaiton Aerosol is discontinued.
17.8 How to Use Ciclesonide Inhalation Aerosol
Patients should use Ciclesonide Inhalation Aerosol only with the actuator supplied with the product. When the dose indicator display window shows a red zone, approximately 20 inhalations are left, and a refill is required. Discard the inhaler when the indicator shows zero.
Manufactured for:
Prasco Laboratories
Mason, OH 45040 USA
Made in United Kingdom
Revised August 2020
Patient Information
Ciclesonide Inhalation Aerosol
Note: For Oral Inhalation Only
Do not use your Ciclesonide Inhalation Aerosol near heat or an open flame.
Read this Patient Information leaflet before you start using Ciclesonide Inhalation Aerosol Inhalation Aerosol and each time you get a refill. There may be new information. This information does not take the place of talking with your healthcare provider about your medical condition or your treatment. If you have any questions about Ciclesonide Inhalation Aerosol, ask your healthcare provider or pharmacist.
What is Ciclesonide Inhalation Aerosol?
Ciclesonide Inhalation Aerosol is a prescription medicine used for the control and prevention of asthma in adults and children 12 years of age and older.
Ciclesonide Inhalation Aerosol contains ciclesonide, which is a man-made (synthetic) corticosteroid. Corticosteroids are natural substances found in the body and reduce inflammation. When you inhale Ciclesonide Inhalation Aerosol it may help to control and prevent your symptoms of asthma by reducing your airway inflammation.
Ciclesonide Inhalation Aerosol is not for the relief of acute bronchospasm. Ciclesonide Inhalation Aerosol is not a bronchodilator and does not treat sudden symptoms of an asthma attack such as wheezing, cough, shortness of breath, and chest pain or tightness. Always have a fast-acting bronchodilator medicine (rescue inhaler) with you to treat sudden symptoms.
It is not known if Ciclesonide Inhalation Aerosol is safe and effective in children 11 years of age and younger.
Who should not use Ciclesonide Inhalation Aerosol?
Do not use Ciclesonide Inhalation Aerosol:
- to treat status asthmaticus or other sudden symptoms of asthma. Ciclesonide Inhalation Aerosol is not a rescue inhaler and should not be used to give you fast relief from your asthma attack. Always use a rescue inhaler such as albuterol, during a sudden asthma attack.
- if you are allergic to ciclesonide or any of the ingredients in Ciclesonide Inhalation Aerosol Inhalation Aerosol. See the end of this Patient Information leaflet for a complete list of ingredients in Ciclesonide Inhalation Aerosol Inhalation Aerosol.
What should I tell my healthcare provider before using Ciclesonide Inhalation Aerosol?
Before you use Ciclesonide Inhalation Aerosol tell your healthcare provider if you:
- have or have had eye problems such as increased ocular pressure, glaucoma, or cataracts.
- have any infections including tuberculosis or ocular herpes simplex.
- have not had or been vaccinated for chicken pox or measles.
- are pregnant or plan to become pregnant. It is not known if Ciclesonide Inhalation Aerosol will harm your unborn baby. Talk to your healthcare provider if you are pregnant or plan to become pregnant.
- are breastfeeding or plan to breastfeed. It is not known if Ciclesonide Inhalation Aerosol passes into your breast milk. Talk to your healthcare provider about the best way to feed your baby if you are using Ciclesonide Inhalation Aerosol.
Tell your healthcare provider about all the medicines you take, including prescription and non-prescription medicines, vitamins and herbal supplements.
Know the medicines you take. Keep a list of them to show your healthcare provider and pharmacist when you get a new medicine.
How should I use Ciclesonide Inhalation Aerosol?
- Read the Instructions for Use at the end of this leaflet for specific information about the right way to use Ciclesonide Inhalation Aerosol.
- Use Ciclesonide Inhalation Aerosol exactly as your healthcare provider tells you to use it. Do not take more of your medicine, or take it more often than your healthcare provider tells you.
- You must use Ciclesonide Inhalation Aerosol regularly. It may take 4 weeks or longer after you start using Ciclesonide Inhalation Aerosol for your asthma symptoms to get better. Do not stop using Ciclesonide Inhalation Aerosol even if you are feeling better, unless your healthcare provider tells you to.
- If your symptoms do not improve or get worse, call your healthcare provider.
- Your healthcare provider may prescribe a rescue inhaler for emergency relief of sudden asthma attacks. Call your healthcare provider if you have:
an asthma attack that does not respond to your rescue inhaler or
you need more of your rescue inhaler than usual.
- If you use another inhaled medicine, ask your healthcare provider for instructions on how to use it while you use Ciclesonide Inhalation Aerosol.
What are the possible side effects of Ciclesonide Inhalation Aerosol?
Ciclesonide Inhalation Aerosol may cause serious side effects, including:
-
Thrush (Candida), a fungal infection of your nose, mouth, or throat. Tell your healthcare provider if you have discomfort or pain in your throat, have hoarseness in your voice or have any redness or white colored patches in your mouth or throat. Rinse your mouth after you use your Ciclesonide Inhalation Aerosol.
-
Immune system problems that may increase your risk of infections. You are more likely to get infections if you take medicines that may weaken your body’s ability to fight infections. Avoid contact with people who have contagious diseases such as chicken pox or measles while you use Ciclesonide Inhalation Aerosol. Symptoms of an infection may include:
fever
pain
aches
chills
feeling tired
nausea
vomiting
-
Adrenal insufficiency. Adrenal insufficiency is a condition in which the adrenal glands do not make enough steroid hormones. Your healthcare provider will follow you closely if you take steroids by mouth and are having them decreased (tapered) or you are being switched to Ciclesonide Inhalation Aerosol. People have died while steroids are being decreased and when people have been switched from steroids by mouth to inhaled steroids like Ciclesonide Inhalation Aerosol. If you are under stress, such as with surgery, after surgery or trauma, you may need steroids by mouth again.
Call your healthcare provider right away if you have the following symptoms of adrenal insufficiency:
tiredness
weakness
dizziness
nausea that does not go away
vomiting that does not go away
-
Decreased bone mass (bone mineral density). People who use inhaled steroid medicines for a long time may have an increased risk of decreased bone mass which can affect bone strength. Talk to your healthcare provider about any concerns you may have about bone health.
-
Slowed or delayed growth in children. A child’s growth should be checked regularly while using Ciclesonide Inhalation Aerosol.
-
Eye problems such as glaucoma and cataracts. If you have a history of glaucoma or cataracts or have a family history of eye problems, you should have regular eye exams while you use Ciclesonide Inhalation Aerosol.
-
Increased wheezing (bronchospasm) can happen right away after using Ciclesonide Inhalation Aerosol. Stop using Ciclesonide Inhalation Aerosol and use an inhaled fast-acting bronchodilator (rescue inhaler) right away.
Tell your healthcare provider right away so that a new medicine can be prescribed to control your asthma.
The most common side effects with Ciclesonide Inhalation Aerosol include: - headache
- swelling of nose and throat (nasopharyngitis)
- swelling of the sinuses (sinusitis)
- throat pain
- upper respiratory infection
- joint pain (arthralgia)
- nasal congestion
- pain in arms, legs, and back
Tell your healthcare provider about any side effect that bothers you or that does not go away.
These are not all of the possible side effects with Ciclesonide Inhalation Aerosol. For more information, ask your healthcare provider or pharmacist.
Call your healthcare provider for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
How should I store Ciclesonide Inhalation Aerosol?
- Store Ciclesonide Inhalation Aerosol at room temperature between 59°F to 86°F (15°C to 30°C)
-
Do not puncture the Ciclesonide Inhalation Aerosol canister
-
Do not store the Ciclesonide Inhalation Aerosol canister near heat or a flame. Temperatures above 120°F (49°C) may cause the canister to burst.
-
Do not throw the Ciclesonide Inhalation Aerosol Inhalation into a fire or an incinerator.
- Safely throw away medicine that is out of date or no longer needed.
- Keep Ciclesonide Inhalation Aerosol clean and dry at all times.
Keep Ciclesonide Inhalation Aerosol and all medicines out of reach of children.
General Information About the Safe and Effective use of Ciclesonide Inhalation Aerosol
Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. Do not use Ciclesonide Inhalation Aerosol for a condition for which it is not prescribed. Do not give Ciclesonide Inhalation Aerosol to other people, even if they have the same symptoms that you have. It may harm them.
This Patient Information summarizes the most important information about Ciclesonide Inhalation Aerosol. If you would like more information, talk with your healthcare provider. You can ask your pharmacist or healthcare provider for information about Ciclesonide Inhalation Aerosol that is written for health professionals.
What are the ingredients in Ciclesonide Inhalation Aerosol?
Active ingredient: ciclesonide
Inactive ingredients: propellant HFA-134a and ethanol
Instructions for Use
Ciclesonide Inhalation Aerosol
Read this Instructions for Use for Ciclesonide Inhalation Aerosol before you start using it and each time you get a refill. There may be new information. This leaflet does not take the place of talking to your healthcare provider about your medical condition or treatment.
Note: For Oral Inhalation Only
Do not use your Ciclesonide Inhalation Aerosol Inhalation Aerosol near heat or an open flame.
The parts of your Ciclesonide Inhalation Aerosol
Ciclesonide Inhalation Aerosol comes as a canister that fits into an actuator with a dose indicator. Do not use the actuator with a canister of medicine from any other inhaler. Do not use Ciclesonide Inhalation Aerosol canister with an actuator from any other inhaler. (See Figure A)
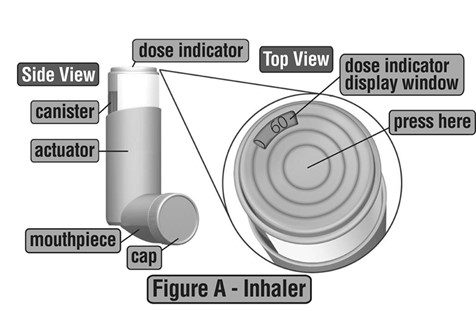
Priming your Ciclesonide Inhalation Aerosol for use
- Remove your Ciclesonide Inhalation Aerosol from its package.
-
Before you use Ciclesonide Inhalation Aerosol for the first time or if you have not used your medicine for 10 days in a row, you will need to prime your Ciclesonide Inhalation Aerosol unit.
- Remove the plastic cap. Look at the dose indicator on top of the inhaler. Make sure that the dose indicator display window pointer is before the “60” inhalation mark before you use your Ciclesonide Inhalation Aerosol for the first time.
- Hold the actuator upright. Spray 3 times into the air away from the face, by pressing down fully onto the center of the dose indicator button. (See Figure B)
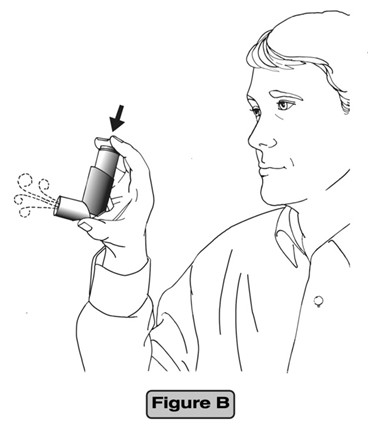
- Check the dose indicator display window after the priming sprays and before the first use to make sure it shows that there are 60 sprays left in your Ciclesonide Inhalation Aerosol unit. If there are not 60 sprays left in your Ciclesonide Inhalation Aerosol after the first use priming spray, return it to the pharmacy.
- Make sure the canister is firmly placed in the mouthpiece each time you use your Ciclesonide Inhalation Aerosol.
- You do not need to shake your Ciclesonide Inhalation Aerosol unit before you use it.
Using Your Ciclesonide Inhalation Aerosol
Step 1. Remove the cap from the mouthpiece. (See Figure C)
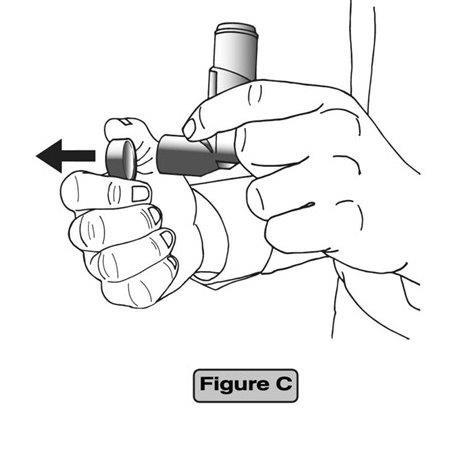
Step 2. Hold the actuator upright, between your thumb, forefinger, and middle finger with the mouthpiece pointing towards you. (See Figure D)
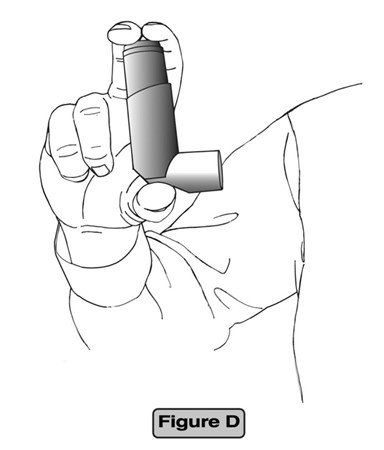
Step 3. Breathe out as fully as you comfortably can. Close your lips around the mouthpiece, keeping your tongue below it. (See Figure E)
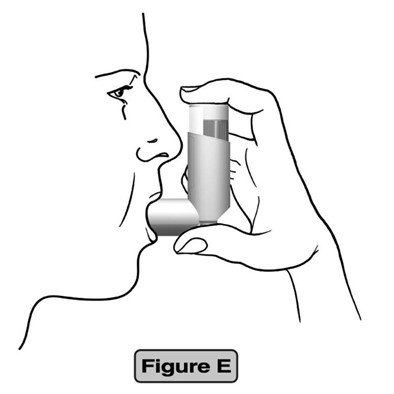
Step 4.
- While breathing in deeply and slowly, press down on the center of the dose indicator with your finger. Press down fully on the canister until it stops moving in the actuator while delivering your dose.
- When you have finished breathing in, hold your breath for about 10 seconds, or for as long as is comfortable.
- Note: It is normal to hear a soft click from the indicator as it counts down during use.
Step 5.
Take your finger completely off the center of the dose indicator and remove the inhaler from your mouth. Breathe out gently. (See Figure F)
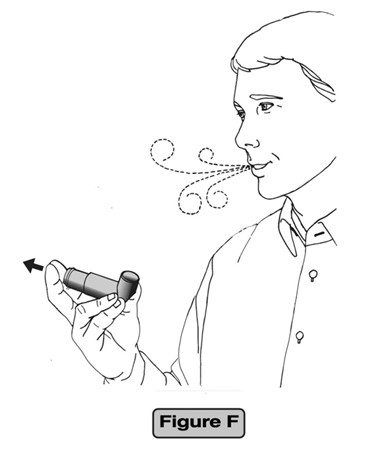
Step 6. Replace the cap to keep the mouthpiece clean.
Step 7. Rinse your mouth with water and spit it out. Do not swallow.
Cleaning your Ciclesonide Inhalation Aerosol unit
- Clean the mouthpiece weekly with a clean dry tissue, both inside and out. (See Figure G)
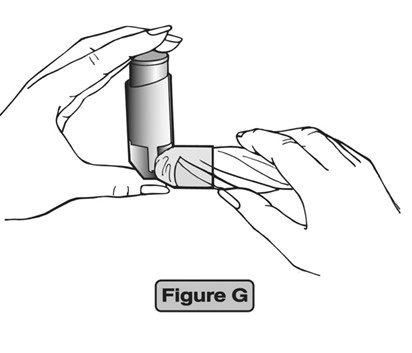
- Wipe over the front of the small hole where the medicine comes out with a dry, folded tissue. (See Figure H)
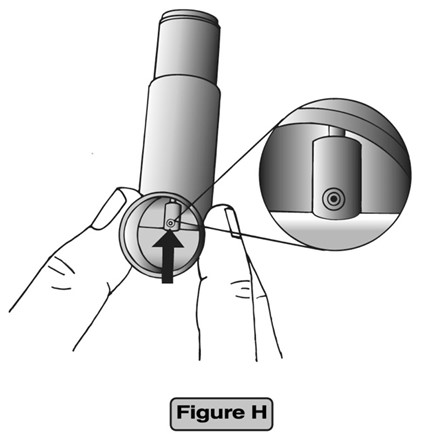
- Do not wash or put any part of your Ciclesonide Inhalation Aerosol unit in water or any other liquids.
How to tell if your Ciclesonide Inhalation Aerosol canister is empty
- Your Ciclesonide Inhalation Aerosol unit is fitted with a dose indicator display which shows you how much of your medicine is left after each use.
- Each canister of Ciclesonide Inhalation Aerosol contains enough medicine for you to spray your medicine 60 times. This does not count the first sprays used for priming.
- The dose indicator display counts down by 10 and will move every tenth time you take a puff (i.e., 60-50-40, etc.).
- The dose indicator display window will turn red when there are only 20 sprays left. This means that you need to replace your inhaler soon.
- When the dose indicator display window reads “0” you should throw away your Ciclesonide Inhalation Aerosol unit. (See Figure I)
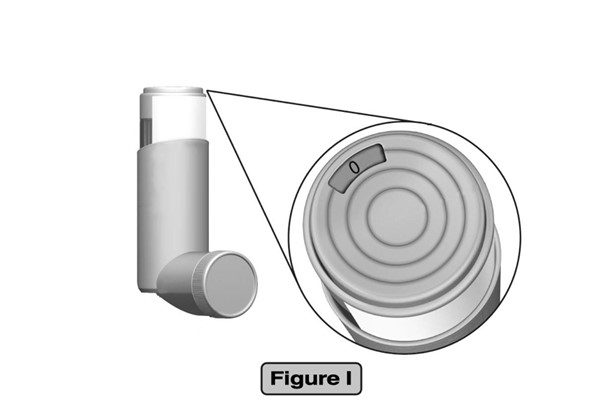
- Although your Ciclesonide Inhalation Aerosol unit is fitted with a dose indicator display to help determine the number of sprays left, you should keep track of the number of sprays used from each canister of your Ciclesonide Inhalation Aerosol unit.
This PPI and Instructions for Use has been approved by the U.S. Food and Drug Administration.
Manufactured for:
Prasco Laboratories
Mason, OH 45040 USA
Made in United Kingdom
Revised August 2020
PRINCIPAL DISPLAY PANEL - 80 mcg CARTON

PRASCO
NDC: 66993-571-64
Net Contents: 6.1 g
Ciclesonide
Inhalation
Aerosol
80 mcg/actuation
60 Metered Actuations
FOR ORAL INHALATION WITH CICLESONIDE INHALATION AEROSOL ACTUATOR ONLY
Rx Only
PRINCIPAL DISPLAY PANEL - 160 mcg CARTON

PRASCO
NDC: 66993-572-64
Net Contents: 6.1 g
Ciclesonide
Inhalation
Aerosol
160 mcg/actuation
60 Metered Actuations
FOR ORAL INHALATION WITH CICLESONIDE INHALATION AEROSOL ACTUATOR ONLY
Rx Only
| CICLESONIDE
ciclesonide aerosol, metered |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| CICLESONIDE
ciclesonide aerosol, metered |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| Labeler - Prasco Laboratories (065969375) |
© 2026 FDA.report
This site is not affiliated with or endorsed by the FDA.