Methocarbamol Tablets USP
Methocarbamol by
Drug Labeling and Warnings
Methocarbamol by is a Prescription medication manufactured, distributed, or labeled by Westminster Pharmaceuticals, LLC, AustarPharma LLC. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
METHOCARBAMOL- methocarbamol tablet, coated
Westminster Pharmaceuticals, LLC
----------
Methocarbamol Tablets USP
DESCRIPTION
Methocarbamol Tablets USP, 500 mg and 750 mg, a carbamate derivative of gualfenesin, is a central nervous system (CNS) depressant with sedative and musculoskeletal relaxant properties.
The chemical name of methocarbamol is a 3-(2 methoxyphenoxy)-1,2-propanediol 1-carbamate and has the empirical formula C11H15NO5. Its molecular weight is 241.24. The structural formula is shown below.
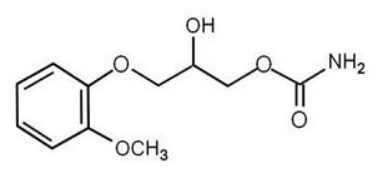
Methocarbamol is a white powder, sparingly soluble in water and chloroform, soluble in alcohol (only with heating) and propylene glycol, and insoluble in benzene and n-hexane.
Methocarbamol Tablet, 500 mg is available as an orange, film coated, round concave tablet containing 500 mg of methocarbamol, USP for oral administration. The inactive ingredients present are microcrystalline cellulose, croscarmellose sodium, FD&C Yellow 6 aluminum lake, hydroxypropyl cellulose, hypromellose, magnesium stearate, polyethylene glycol, triacetin, titanium dioxide.
Methocarbamol Tablet, 750 mg is available as a yellow, film coated, modified capsule shaped tablet containing 750 mg of methocarbamol, USP for oral administration. The inactive ingredients present are microcrystalline cellulose, croscarmellose sodium, iron oxide yellow, iron oxide red, hydroxypropyl cellulose, hypromellose, magnesium stearate, polyethylene glycol, triacetin, titanium dioxide.
Clinical Pharmacology
The mechanism of action of methocarbamol in humans has not been established, but may be due to general CNS depression. It has no direct action on the contractile mechanism of striated muscle, the motor end plate or the nerve fiber.
Pharmacokinetics
In healthy volunteers, the plasma clearance of methocarbamol ranges between 0.20 and 0.80 L/h/kg, the mean plasma elimination half-life ranges between 1 and 2 hours, and the plasma protein binding ranges between 46% and 50%.
Methocarbamol is metabolized via dealkylation and hydroxylation. Conjugation of methocarbamol also is likely. Essentially all methocarbamol metabolites are eliminated in the urine. Small amounts of unchanged methocarbamol also are excreted in the urine.
Special populations
Elderly
The mean (± SD) elimination half-life of methocarbamol in elderly healthy volunteers (mean (± SD) age, 69 (± 4) years) was slightly prolonged compared to a younger (mean (± SD) age, 53.3 (± 8.8) years), healthy population (1.5 (± 0.4) hours versus 1.1 (± 0.27) hours, respectively). The fraction of bound methocarbamol was slightly decreased in the elderly versus younger volunteers (41% to 43% versus 46% to 50%, respectively).
Preclinical studies (in male rats) show that alendronate transiently distributes to soft tissues following 1 mg/kg IV administration but is then rapidly redistributed to bone or excreted in the urine. The mean steady-state volume of distribution, exclusive of bone, is at least 28 L in humans. Concentrations of drug in plasma following therapeutic oral doses are too low (less than 5 ng/mL) for analytical detection. Protein binding in human plasma is approximately 78%.
Renally impaired
The clearance of methocarbamol in 8 renally-impaired patients on maintenance hemodialysis was reduced about 40% compared to 17 normal subjects, although the mean (± SD) elimination half-life in these two groups was similar: 1.2 (± 0.6) versus 1.1 (± 0.3) hours, respectively.
Hepatically impaired
In 8 patients with cirrhosis secondary to alcohol abuse, the mean total clearance of methocarbamol was reduced approximately 70% compared to that obtained in 8 age- and weight-matched normal subjects. The mean (± SD) elimination half-life in the cirrhotic patients and the normal subjects was 3.38 (± 1.62) hours and 1.11 (± 0.27) hours, respectively. The percent of methocarbamol bound to plasma proteins was decreased to approximately 40% to 45% compared to 46% to 50% in the normal subjects.
INDICATIONS AND USAGE
Methocarbamol is indicated as an adjunct to rest, physical therapy, and other measures for the relief of discomfort associated with acute, painful musculoskeletal conditions. The mode of action of methocarbamol has not been clearly identified, but may be related to its sedative properties. Methocarbamol does not directly relax tense skeletal muscles in man.
CONTRAINDICATIONS
Methocarbamol is contraindicated in patients hypersensitive to methocarbamol or to any of the tablet components.
WARNINGS
Since methocarbamol may possess a general CNS depressant effect, patients receiving methocarbamol tablets should be cautioned about combined effects with alcohol and other CNS depressants.
Safe use of methocarbamol has not been established with regard to possible adverse effects upon fetal development. There have been reports of fetal and congenital abnormalities following in utero exposure to methocarbamol. Therefore, methocarbamol tablets should not be used in women who are or may become pregnant and particularly during early pregnancy unless in the judgment of the physician the potential benefits outweigh the possible hazards (see PRECAUTIONS, Pregnancy).
Use in Activities Requiring Mental Alertness
Methocarbamol may impair mental and/or physical abilities required for performance of hazardous tasks, such as operating machinery or driving a motor vehicle. Patients should be cautioned about operating machinery, including automobiles, until they are reasonably certain that methocarbamol therapy does not adversely affect their ability to engage in such activities.
PRECAUTIONS
Information for Patients
Patients should be cautioned that methocarbamol may cause drowsiness or dizziness, which may impair their ability to operate motor vehicles or machinery. Because methocarbamol may possess a general CNS-depressant effect, patients should be cautioned about combined effects with alcohol and other CNS depressants.
Drug Interactions
See WARNINGS and PRECAUTIONS for interaction with CNS drugs and alcohol.
Methocarbamol may inhibit the effect of pyridostigmine bromide. Therefore, methocarbamol should be used with caution in patients with myasthenia gravis receiving anticholinesterase agents.
Drug/Laboratory Test Interactions
Methocarbamol may cause a color interference in certain screening tests for 5-hydroxyindoleacetic acid (5-HIAA) using nitrosonaphthol reagent and in screening tests for urinary vanillylmandelic acid (VMA) using the Gitlow method.
Carcinogenesis, Mutagenesis, Impairment of Fertility
Long-term studies to evaluate the carcinogenic potential of methocarbamol have not been performed. No studies have been conducted to assess the effect of methocarbamol on mutagenesis or its potential to impair fertility.
Pregnancy
Teratogenic Effects
Pregnancy Category C
Animal reproduction studies have not been conducted with methocarbamol. It is also not known whether methocarbamol can cause fetal harm when administered to a pregnant woman or can affect reproduction capacity. Methocarbamol should be given to a pregnant woman only if clearly needed.
Safe use of methocarbamol has not been established with regard to possible adverse effects upon fetal development. There have been reports of fetal and congenital abnormalities following in utero exposure to methocarbamol. Therefore, methocarbamol should not be used in women who are or may become pregnant and particularly during early pregnancy unless in the judgment of the physician the potential benefits outweigh the possible hazards (see WARNINGS).
Nursing Mothers
Methocarbamol and/or its metabolites are excreted in the milk of dogs; however, it is not known whether methocarbamol or its metabolites are excreted in human milk. Because many drugs are excreted in human milk, caution should be exercised when methocarbamol is administered to a nursing woman.
ADVERSE REACTIONS
Adverse reactions reported coincident with the administration of methocarbamol include:
Body as a whole: Anaphylactic reaction, angioneurotic edema, fever, headache
Cardiovascular system: Bradycardia, flushing, hypotension, syncope, thrombophlebitis
Digestive system: Dyspepsia, jaundice (including cholestatic jaundice), nausea and vomiting
Hemic and lymphatic system: Leukopenia
Immune system: Hypersensitivity reactions
Nervous system: Amnesia, confusion, diplopia, dizziness or lightheadedness, drowsiness, insomnia, mild muscular incoordination, nystagmus, sedation, seizures (including grand mal), vertigo
Skin and special senses: Blurred vision, conjunctivitis, nasal congestion, metallic taste, pruritus, rash, urticaria
To report SUSPECTED ADVERSE REACTIONS, contact Westminster Pharmaceuticals, LLC at 1-844-221-7294 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch
OVERDOSAGE
Limited information is available on the acute toxicity of methocarbamol. Overdose of methocarbamol is frequently in conjunction with alcohol or other CNS depressants and includes the following symptoms: nausea, drowsiness, blurred vision, hypotension, seizures, and coma.
In post-marketing experience, deaths have been reported with an overdose of methocarbamol alone or in the presence of other CNS depressants, alcohol or psychotropic drugs.
Treatment
Management of overdose includes symptomatic and supportive treatment. Supportive measures include maintenance of an adequate airway, monitoring urinary output and vital signs, and administration of intravenous fluids if necessary. The usefulness of hemodialysis in managing overdose is unknown.
DOSAGE AND ADMINISTRATION
Methocarbamol, 500 mg — Adults:
Initial dosage: 3 tablets q.i.d.
Maintenance dosage: 2 tablets q.i.d.
Methocarbamol, 750 mg — Adults:
Initial dosage: 2 tablets q.i.d.
Maintenance dosage: 1 tablet q.4h. or 2 tablets t.i.d.
Six grams a day are recommended for the first 48 to 72 hours of treatment. (For severe conditions 8 grams a day may be administered). Thereafter, the dosage can usually be reduced to approximately 4 grams a day.
HOW SUPPLIED
Methocarbamol Tablets USP, 500 mg — Orange, film coated, round concave tablets with one side debossed 'AP212', the other side bisected. They
are supplied as follows:
Bottles of 100, NDC: 69367-255-01
Bottles of 500, NDC: 69367-255-05
Methocarbamol Tablets USP, 750 mg — Yellow, film coated, modified capsule shaped tablets; one side debossed 'AP211' and other side blank. They are supplied as follows:
Bottles of 100, NDC: 69367-256-01
Bottles of 500, NDC: 69367-256-05
Store at 20° to 25°C (68° to 77°F) [See USP controlled room temperature].
Dispense in a tight container.
LBL378
REV062220
Revised: June, 2020
Manufactured by:
Hangzhou Minsheng Binjiang
Pharmaceutical Co., Ltd.
Hangzhou, 310051, China
Distributed by:
Westminster Pharmaceuticals, LLC
Nashville, TN 37217
Principal Display Panel - 500mg 100 counts
NDC: 69367-255-01
Methocarbamol
500mg 100 tablet (s)
RX only

Principal Display Panel - 500mg 500counts
NDC: 69367-255-05
Methocarbamol
500mg 500 tablet (s)
RX only

Principal Display Panel - 750mg 100counts
NDC: 69367-256-01
Methocarbamol
750mg 100 tablet (s)
RX only

Principal Display Panel - 750mg 500counts
NDC: 69367-256-05
Methocarbamol
750mg 500tablet (s)
RX only

| METHOCARBAMOL
methocarbamol tablet, coated |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| METHOCARBAMOL
methocarbamol tablet, coated |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| Labeler - Westminster Pharmaceuticals, LLC (079516651) |
| Registrant - AustarPharma LLC (362785011) |