These highlights do not include all the information needed to use Oxaliplatin for Injection safely and effectively. See full prescribing information for Oxaliplatin for Injection. OXALIPLATIN FOR INJECTION powder, for solution for intravenous use Initial U.S. Approval: 2002
OXALIPLATIN by
Drug Labeling and Warnings
OXALIPLATIN by is a Prescription medication manufactured, distributed, or labeled by APP Pharmaceuticals, LLC, Cipla Limited. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
OXALIPLATIN- oxaliplatin injection, powder, lyophilized, for solution
Fresenius Kabi USA, LLC
----------
HIGHLIGHTS OF PRESCRIBING INFORMATIONThese highlights do not include all the information needed to use Oxaliplatin for Injection safely and effectively. See full prescribing information for Oxaliplatin for Injection.
OXALIPLATIN FOR INJECTION powder, for solution for intravenous use Initial U.S. Approval: 2002 WARNING: ANAPHYLACTIC REACTIONSSee full prescribing information for complete boxed warning.Anaphylactic reactions to Oxaliplatin have been reported, and may occur within minutes of Oxaliplatin administration. Epinephrine, corticosteroids, and antihistamines have been employed to alleviate symptoms. (5.1) INDICATIONS AND USAGEOxaliplatin is a platinum-based drug used in combination with infusional 5-fluorouracil (5-FU)/leucovorin (LV), which is indicated for:
DOSAGE AND ADMINISTRATION
DOSAGE FORMS AND STRENGTHSSingle-use vials of 50 mg or 100 mg oxaliplatin as a sterile, preservative-free lyophilized powder for reconstitution. ( 3) WARNINGS AND PRECAUTIONS
ADVERSE REACTIONSMost common adverse reactions (incidence ≥ 40%) were peripheral sensory neuropathy, neutropenia, thrombocytopenia, anemia, nausea, increase in transaminases and alkaline phosphatase, diarrhea, emesis, fatigue and stomatitis. Other adverse reactions, including serious adverse reactions, have been reported. ( 6.1) To report SUSPECTED ADVERSE REACTIONS, contact APP Pharmaceuticals, LLC, Medical Information and Safety Department at 1-800-551-7176 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch. See 17 for PATIENT COUNSELING INFORMATION. Revised: 9/2009 |
FULL PRESCRIBING INFORMATION
WARNING
WARNING: ANAPHYLACTIC REACTIONS
Anaphylactic reactions to Oxaliplatin have been reported, and may occur within minutes of Oxaliplatin administration. Epinephrine, corticosteroids, and antihistamines have been employed to alleviate symptoms of anaphylaxis
[see Warnings and Precautions (5.1)].
1 INDICATIONS AND USAGE
Oxaliplatin, used in combination with infusional 5-fluorouracil/leucovorin, is indicated for
- adjuvant treatment of stage III colon cancer in patients who have undergone complete resection of the primary tumor.
- treatment of advanced colorectal cancer.
2 DOSAGE AND ADMINISTRATION
Oxaliplatin for Injection should be administered under the supervision of a qualified physician experienced in the use of cancer chemotherapeutic agents. Appropriate management of therapy and complications is possible only when adequate diagnostic and treatment facilities are readily available.
2.1 Dosage
Administer oxaliplatin in combination with 5-fluorouracil (5-FU)/leucovorin (LV) every 2 weeks. For advanced disease, treatment is recommended until disease progression or unacceptable toxicity. For adjuvant use, treatment is recommended for a total of 6 months (12 cycles):
Day 1: Oxaliplatin 85 mg/m 2intravenous (IV) infusion in 250 to 500 mL 5% Dextrose injection, USP (D5W) and leucovorin 200 mg/m 2 IV infusion in D5W both given over 120 minutes at the same time in separate bags using a Y-line, followed by 5-FU 400 mg/m 2 IV bolus given over 2 to 4 minutes, followed by 5-FU 600 mg/m 2 IV infusion in 500 mL D5W (recommended) as a 22-hour continuous infusion.
Day 2: Leucovorin 200 mg/m 2 IV infusion over 120 minutes, followed by 5-FU 400 mg/m 2 IV bolus given over 2 to 4 minutes, followed by 5-FU 600 mg/m 2 IV infusion in 500 mL D5W (recommended) as a 22-hour continuous infusion.
Figure 1
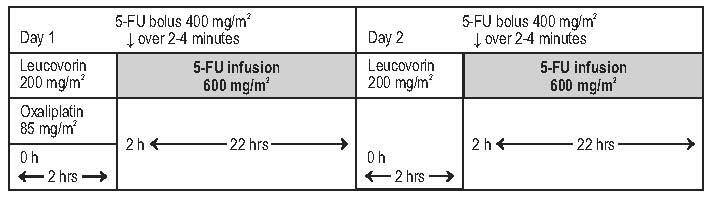
The administration of oxaliplatin does not require prehydration. Premedication with antiemetics, including 5-HT 3 blockers with or without dexamethasone, is recommended.
For information on 5-fluorouracil and leucovorin, see the respective package inserts.
2.2 Dose Modification Recommendations
Prior to subsequent therapy cycles, patients should be evaluated for clinical toxicities and recommended laboratory tests [see Warnings and Precautions (5.6)] . Prolongation of infusion time for oxaliplatin from 2 hours to 6 hours may mitigate acute toxicities. The infusion times for 5-FU and leucovorin do not need to be changed.
Adjuvant Therapy in Patients with Stage III Colon Cancer
Neuropathy and other toxicities were graded using the NCI CTC scale version 1 [see Warnings and Precautions (5.2)] .
For patients who experience persistent Grade 2 neurosensory events that do not resolve, a dose reduction of oxaliplatin to 75 mg/m 2 should be considered. For patients with persistent Grade 3 neurosensory events, discontinuing therapy should be considered. The infusional 5-FU/LV regimen need not be altered.
A dose reduction of oxaliplatin to 75 mg/m 2 and infusional 5-FU to 300 mg/m 2 bolus and 500 mg/m 2 22 hour infusion is recommended for patients after recovery from grade 3/4 gastrointestinal (despite prophylactic treatment) or grade 4 neutropenia or grade 3/4 thrombocytopenia. The next dose should be delayed until: neutrophils ≥1.5 x 10 9/L and platelets ≥75 x 10 9/L.
Dose Modifications in Therapy in Previously Untreated and Previously Treated Patients with Advanced Colorectal Cancer
Neuropathy was graded using a study-specific neurotoxicity scale [see Warnings and Precautions (5.2)] . Other toxicities were graded by the NCI CTC, Version 2.0.
For patients who experience persistent Grade 2 neurosensory events that do not resolve, a dose reduction of oxaliplatin to 65 mg/m 2 should be considered. For patients with persistent Grade 3 neurosensory events, discontinuing therapy should be considered. The 5-fluorouracil /leucovorin regimen need not be altered.
A dose reduction of oxaliplatin to 65 mg/m 2 and 5-FU by 20% (300 mg/m 2 bolus and 500 mg/m 2 22-hour infusion) is recommended for patients after recovery from grade 3/4 gastrointestinal (despite prophylactic treatment) or grade 4 neutropenia or grade 3/4 thrombocytopenia. The next dose should be delayed until: neutrophils ≥1.5 x 10 9/L and platelets ≥75 x 10 9/L.
2.3 Preparation of Infusion Solution
Reconstitution or final dilution must never be performed with a sodium chloride solution or other chloride containing solutions.
The lyophilized powder is reconstituted by adding 10 mL (for the 50 mg vial) or 20 mL (for the 100 mg vial) of Water for Injection, USP or 5% Dextrose Injection, USP. Do not administer the reconstituted solution without further dilution. The reconstituted solution must be further diluted in an infusion solution of 250 to 500 mL of 5% Dextrose Injection, USP.
After reconstitution in the original vial, the solution may be stored up to 24 hours under refrigeration [2º to 8°C (36º to 46° F)]. After final dilution with 250 to 500 mL of 5% Dextrose Injection, USP, the shelf life is 6 hours at room temperature [20º to 25°C (68º to 77°F)] or up to 24 hours under refrigeration [2º to 8°C (36º to 46°F)].
Oxaliplatin for Injection is not light sensitive.
Oxaliplatin is incompatible in solution with alkaline medications or media (such as basic solutions of 5-FU) and must not be mixed with these or administered simultaneously through the same infusion line. The infusion line should be flushed with 5% Dextrose Injection, USP prior to administration of any concomitant medication.
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration and discarded if present.
Needles or intravenous administration sets containing aluminum parts that may come in contact with oxaliplatin should not be used for the preparation or mixing of the drug. Aluminum has been reported to cause degradation of platinum compounds.
3 DOSAGE FORMS AND STRENGTHS
Oxaliplatin for Injection is supplied in single-use vials containing 50 mg or 100 mg of oxaliplatin as a sterile, preservative-free lyophilized powder for reconstitution.
4 CONTRAINDICATIONS
Oxaliplatin should not be administered to patients with a history of known allergy to oxaliplatin or other platinum compounds [see Warnings and Precautions (5.1)] .
5 WARNINGS AND PRECAUTIONS
5.1 Allergic Reactions
See boxed warning
Grade 3/4 hypersensitivity, including anaphylactic/anaphylactoid reactions, to oxaliplatin has been observed in 2 to 3% of colon cancer patients. These allergic reactions which can be fatal, can occur within minutes of administration and at any cycle, and were similar in nature and severity to those reported with other platinum-containing compounds, such as rash, urticaria, erythema, pruritus, and, rarely, bronchospasm and hypotension. The symptoms associated with hypersensitivity reactions reported in the previously untreated patients were urticaria, pruritus, flushing of the face, diarrhea associated with oxaliplatin infusion, shortness of breath, bronchospasm, diaphoresis, chest pains, hypotension, disorientation and syncope. These reactions are usually managed with standard epinephrine, corticosteroid, antihistamine therapy, and may require discontinuation of therapy. Drug-related deaths associated with platinum compounds from anaphylaxis have been reported.
5.2 Neuropathy
Oxaliplatin is associated with two types of neuropathy:
An acute, reversible, primarily peripheral, sensory neuropathy that is of early onset, occurring within hours or one to two days of dosing, that resolves within 14 days, and that frequently recurs with further dosing. The symptoms may be precipitated or exacerbated by exposure to cold temperature or cold objects and they usually present as transient paresthesia, dysesthesia and hypoesthesia in the hands, feet, perioral area, or throat. Jaw spasm, abnormal tongue sensation, dysarthria, eye pain, and a feeling of chest pressure have also been observed. The acute, reversible pattern of sensory neuropathy was observed in about 56% of study patients who received oxaliplatin with 5-fluorouracil (5-FU)/leucovorin (LV). In any individual cycle acute neurotoxicity was observed in approximately 30% of patients. In adjuvant patients the median cycle of onset for grade 3 peripheral sensory neuropathy was 9 in the previously treated patients the median number of cycles administered on the oxaliplatin with 5 FU/LV combination arm was 6.
An acute syndrome of pharyngolaryngeal dysesthesia seen in 1 to 2% (grade 3/4) of patients previously untreated for advanced colorectal cancer, and the previously treated patients, is characterized by subjective sensations of dysphagia or dyspnea, without any laryngospasm or bronchospasm (no stridor or wheezing). Ice (mucositis prophylaxis) should be avoided during the infusion of oxaliplatin because cold temperature can exacerbate acute neurological symptoms.
A persistent (>14 days), primarily peripheral, sensory neuropathy that is usually characterized by paresthesias, dysesthesias, hypoesthesias, but may also include deficits in proprioception that can interfere with daily activities (e.g., writing, buttoning, swallowing, and difficulty walking from impaired proprioception). These forms of neuropathy occurred in 48% of the study patients receiving oxaliplatin with 5-FU/LV. Persistent neuropathy can occur without any prior acute neuropathy event. The majority of the patients (80%) who developed grade 3 persistent neuropathy progressed from prior Grade 1 or 2 events. These symptoms may improve in some patients upon discontinuation of oxaliplatin.
In the adjuvant colon cancer trial, neuropathy was graded using a prelisted module derived from the Neuro-Sensory section of the National Cancer Institute Common Toxicity Criteria (NCI CTC) scale, Version 1, as follows:
Table 1 - NCI CTC Grading for Neuropathy in Adjuvant Patients
| Grade | Definition
|
| Grade 0 | No change or none
|
| Grade 1
| Mild paresthesias, loss of deep tendon reflexes
|
| Grade 2
| Mild or moderate objective sensory loss, moderate paresthesias
|
| Grade 3
| Severe objective sensory loss or paresthesias that interfere with function
|
| Grade 4
| Not applicable
|
Peripheral sensory neuropathy was reported in adjuvant patients treated with the oxaliplatin combination with a frequency of 92% (all grades) and 13% (grade 3). At the 28-day follow-up after the last treatment cycle, 60% of all patients had any grade (Grade 1= 40%, Grade 2=16%, Grade 3=5%) peripheral sensory neuropathy decreasing to 39% at 6 months follow-up (Grade 1=31%, Grade 2=7%, Grade 3=1%) and 21% at 18 months of follow-up (Grade 1=17%, Grade 2=3%, Grade 3=1%).
In the advanced colorectal cancer studies, neuropathy was graded using a study-specific neurotoxicity scale, which was different from the NCI CTC scale, Version 2.0 (see below).
Table 2 - Grading Scale for Paresthesias/Dysesthesias in Advanced Colorectal Cancer Patients
| Grade | Definition
|
| Grade 1
| Resolved and did not interfere with functioning
|
| Grade 2
| Interfered with function but not daily activities
|
| Grade 3
| Pain or functional impairment that interfered with daily activities
|
| Grade 4
| Persistent impairment that is disabling or life-threatening
|
Overall, neuropathy was reported in patients previously untreated for advanced colorectal cancer in 82% (all grades) and 19% (grade 3/4), and in the previously treated patients in 74% (all grades) and 7% (grade 3/4) events. Information regarding reversibility of neuropathy was not available from the trial for patients who had not been previously treated for colorectal cancer.
5.3 Pulmonary Toxicity
Oxaliplatin has been associated with pulmonary fibrosis (<1% of study patients), which may be fatal. The combined incidence of cough and dyspnea was 7.4% (any grade) and <1% (grade 3) with no grade 4 events in the oxaliplatin plus infusional 5-FU/LV arm compared to 4.5% (any grade) and no grade 3 and 0.1% grade 4 events in the infusional 5-FU/LV alone arm in adjuvant colon cancer patients. In this study, one patient died from eosinophilic pneumonia in the oxaliplatin combination arm. The combined incidence of cough, dyspnea and hypoxia was 43% (any grade) and 7% (grade 3 and 4) in the oxaliplatin plus 5-FU/LV arm compared to 32% (any grade) and 5% (grade 3 and 4) in the irinotecan plus 5-FU/LV arm of unknown duration for patients with previously untreated colorectal cancer. In case of unexplained respiratory symptoms such as non-productive cough, dyspnea, crackles, or radiological pulmonary infiltrates, oxaliplatin should be discontinued until further pulmonary investigation excludes interstitial lung disease or pulmonary fibrosis.
5.4 Hepatotoxicity
Hepatotoxicity as evidenced in the adjuvant study, by increase in transaminases (57% vs. 34%) and alkaline phosphatase (42% vs. 20%) was observed more commonly in the oxaliplatin combination arm than in the control arm. The incidence of increased bilirubin was similar on both arms. Changes noted on liver biopsies include: peliosis, nodular regenerative hyperplasia or sinusoidal alterations, perisinusoidal fibrosis, and veno-occlusive lesions. Hepatic vascular disorders should be considered, and if appropriate, should be investigated in case of abnormal liver function test results or portal hypertension, which cannot be explained by liver metastases [see Clinical Trials Experience (6.1)] .
5.5 Use in Pregnancy
Pregnancy Category D
Oxaliplatin may cause fetal harm when administered to a pregnant woman. There are no adequate and well-controlled studies of oxaliplatin in pregnant women. Women of childbearing potential should be advised to avoid becoming pregnant while receiving treatment with oxaliplatin.
5.6 Recommended Laboratory Tests
Standard monitoring of the white blood cell count with differential, hemoglobin, platelet count, and blood chemistries (including ALT, AST, bilirubin and creatinine) is recommended before each oxaliplatin cycle [see Dosage and Administration (2)] .
There have been reports while on study and from post-marketing surveillance of prolonged prothrombin time and INR occasionally associated with hemorrhage in patients who received oxaliplatin plus 5-FU/LV while on anticoagulants. Patients receiving oxaliplatin plus 5-FU/LV and requiring oral anticoagulants may require closer monitoring.
6 ADVERSE REACTIONS
6.1 Clinical Trials Experience
Serious adverse reactions including anaphylaxis and allergic reactions, neuropathy, pulmonary toxicities and hepatotoxicities can occur [see Warnings and Precautions (5.1)] .
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
More than 1100 patients with stage II or III colon cancer and more than 4,000 patients with advanced colorectal cancer have been treated in clinical studies with oxaliplatin. The most common adverse reactions in patients with stage II or III colon cancer receiving adjuvant therapy were peripheral sensory neuropathy, neutropenia, thrombocytopenia, anemia, nausea, increase in transaminases and alkaline phosphatase, diarrhea, emesis, fatigue and stomatitis. The most common adverse reactions in previously untreated and treated patients were peripheral sensory neuropathies, fatigue, neutropenia, nausea, emesis, and diarrhea [see Warnings and Precautions (5)] .
Combination Adjuvant Therapy with Oxaliplatin and Infusional 5-fluorouracil/leucovorin in Patients with Colon Cancer
One thousand one hundred and eight patients with stage II or III colon cancer, who had undergone complete resection of the primary tumor, have been treated in a clinical study with oxaliplatin in combination with infusional 5-fluorouracil (5-FU)/leucovorin (LV) [see Clinical Studies (14)] . The incidence of grade 3 or 4 adverse reactions was 70% on the oxaliplatin combination arm, and 31% on the infusional 5-FU/LV arm. The adverse reactions in this trial are shown in the tables below. Discontinuation of treatment due to adverse reactions occurred in 15% of the patients receiving oxaliplatin and infusional 5-FU/LV. Both 5-FU/LV and oxaliplatin are associated with gastrointestinal or hematologic adverse reactions. When oxaliplatin is administered in combination with infusional 5-FU/LV, the incidence of these events is increased.
The incidence of death within 28 days of last treatment, regardless of causality, was 0.5% (n=6) in both the oxaliplatin combination and infusional 5-FU/LV arms, respectively. Deaths within 60 days from initiation of therapy were 0.3% (n=3) in both the oxaliplatin combination and infusional 5-FU/LV arms, respectively. On the oxaliplatin combination arm, 3 deaths were due to sepsis/neutropenic sepsis, 2 from intracerebral bleeding and one from eosinophilic pneumonia. On the 5-FU/LV arm, one death was due to suicide, 2 from Stevens-Johnson Syndrome (1 patient also had sepsis), 1 unknown cause, 1 anoxic cerebral infarction and 1 probable abdominal aorta rupture.
The following table provides adverse reactions reported in the adjuvant therapy colon cancer clinical trial [see Clinical Studies (14)] by body system and decreasing order of frequency in the oxaliplatin and infusional 5-FU/LV arm for events with overall incidences ≥ 5% and for NCI grade 3/4 events with incidences ≥ 1%.
|
|
||||
| Adverse reaction
(WHO/Pref) | Oxaliplatin + 5-FU/LV
N=1108 | 5-FU/LV
N=1111 |
||
| All Grades
(%) | Grade 3/4
(%) | All Grades
(%) | Grade 3/4
(%) |
|
| Any Event
| 100
| 70
| 99
| 31
|
| Allergy/Immunology
|
||||
| Allergic Reaction
| 10
| 3
| 2
| <1
|
| Constitutional Symptoms/Pain
|
||||
| Fatigue
| 44
| 4
| 38
| 1
|
| Abdominal Pain
| 18
| 1
| 17
| 2
|
| Dermatology/Skin
|
||||
| Skin Disorder
| 32
| 2
| 36
| 2
|
| Injection Site Reaction
*
| 11
| 3
| 10
| 3
|
| Gastrointestinal
|
||||
| Nausea
| 74
| 5
| 61
| 2
|
| Diarrhea
| 56
| 11
| 48
| 7
|
| Vomiting
| 47
| 6
| 24
| 1
|
| Stomatitis
| 42
| 3
| 40
| 2
|
| Anorexia
| 13
| 1
| 8
| <1
|
| Fever/Infection
|
||||
| Fever
| 27
| 1
| 12
| 1
|
| Infection
| 25
| 4
| 25
| 3
|
| Neurology
|
||||
| Overall Peripheral Sensory Neuropathy
| 92
| 12
| 16
| <1
|
The following table provides adverse reactions reported in the adjuvant therapy colon cancer clinical trial [see Clinical Studies (14)] by body system and decreasing order of frequency in the oxaliplatin and infusional 5-FU/LV arm for events with overall incidences ≥5% but with incidences <1% NCI grade 3/4 events.
| Adverse reaction
(WHO/Pref) | Oxaliplatin + 5-FU/LV
N=1108 | 5-FU/LV
N=1111 |
| All Grades (%)
| All Grades (%)
|
|
| Allergy/Immunology
|
||
| Rhinitis
| 6
| 8
|
| Constitutional Symptoms/Pain/Ocular/Visual
|
||
| Epistaxis
| 16
| 12
|
| Weight Increase
| 10
| 10
|
| Conjunctivitis
| 9
| 15
|
| Headache
| 7
| 5
|
| Dyspnea
| 5
| 3
|
| Pain
| 5
| 5
|
| Lacrimation Abnormal
| 4
| 12
|
| Dermatology/Skin
|
||
| Alopecia
| 30
| 28
|
| Gastrointestinal
|
||
| Constipation
| 22
| 19
|
| Taste Perversion
| 12
| 8
|
| Dyspepsia
| 8
| 5
|
| Metabolic
|
||
| Phosphate Alkaline increased
| 42
| 20
|
| Neurology
|
||
| Sensory Disturbance
| 8
| 1
|
Although specific events can vary, the overall frequency of adverse reactions was similar in men and women and in patients <65 and ≥65 years. However, the following grade 3/4 events were more common in females: diarrhea, fatigue, granulocytopenia, nausea and vomiting. In patients ≥65 years old, the incidence of grade 3/4 diarrhea and granulocytopenia was higher than in younger patients. Insufficient subgroup sizes prevented analysis of safety by race. The following additional adverse reactions, were reported in ≥2% and <5% of the patients in the oxaliplatin and infusional 5-FU/LV combination arm (listed in decreasing order of frequency): pain, leukopenia, weight decrease, coughing.
The number of patients who developed secondary malignancies was similar; 62 in the oxaliplatin combination arm and 68 in the infusional 5-FU/LV arm. An exploratory analysis showed that the number of deaths due to secondary malignancies was 1.96% in the oxaliplatin combination arm and 0.98% in infusional 5-FU/LV arm. In addition, the number of cardiovascular deaths was 1.4% in the oxaliplatin combination arm as compared to 0.7% in the infusional 5-FU/LV arm. Clinical significance of these findings is unknown.
Patients Previously Untreated for Advanced Colorectal Cancer
Two hundred and fifty-nine patients were treated in the oxaliplatin and 5-FU/LV combination arm of the randomized trial in patients previously untreated for advanced colorectal cancer [see Clinical Studies (14)] . The adverse reaction profile in this study was similar to that seen in other studies and the adverse reactions in this trial are shown in the tables below.
Both 5-FU and oxaliplatin are associated with gastrointestinal and hematologic adverse reactions. When oxaliplatin is administered in combination with 5-FU, the incidence of these events is increased.
The incidence of death within 30 days of treatment in the previously untreated for advanced colorectal cancer study, regardless of causality, was 3% with the Oxaliplatin and 5-FU/LV combination, 5% with irinotecan plus 5-FU/LV, and 3% with Oxaliplatin plus irinotecan. Deaths within 60 days from initiation of therapy were 2.3% with the oxaliplatin and 5-FU/LV combination, 5.1% with irinotecan plus 5-FU/LV, and 3.1% with oxaliplatin plus irinotecan.
The following table provides adverse reactions reported in the previously untreated for advanced colorectal cancer study [see Clinical Studies (14)] by body system and decreasing order of frequency in the oxaliplatin and 5-FU/LV combination arm for events with overall incidences ≥5% and for grade 3/4 events with incidences ≥1%.
|
|
||||||
| Adverse
Reaction (WHO/Pref) | Oxaliplatin +
5-FU/LV N=259 | irinotecan +
5-FU/LV N=256 | Oxaliplatin +
irinotecan N=258 |
|||
| All Grades
(%) | Grade 3/4
(%) | All Grades
(%) | Grade 3/4
(%) | All Grades
(%) | Grade 3/4
(%) |
|
| Any Event
| 99
| 82
| 98
| 70
| 99
| 76
|
| Allergy/Immunology
|
||||||
| Hypersensitivity
| 12
| 2
| 5
| 0
| 6
| 1
|
| Cardiovascular
|
||||||
| Thrombosis
| 6
| 5
| 6
| 6
| 3
| 3
|
| Hypotension
| 5
| 3
| 6
| 3
| 4
| 3
|
| Constitutional Symptoms/Pain/Ocular/Visual
|
||||||
| Fatigue
| 70
| 7
| 58
| 11
| 66
| 16
|
| Abdominal Pain
| 29
| 8
| 31
| 7
| 39
| 10
|
| Myalgia
| 14
| 2
| 6
| 0
| 9
| 2
|
| Pain
| 7
| 1
| 5
| 1
| 6
| 1
|
| Vision abnormal
| 5
| 0
| 2
| 1
| 6
| 1
|
| Neuralgia
| 5
| 0
| 0
| 0
| 2
| 1
|
| Dermatology/Skin
|
||||||
| Skin reaction – hand/foot
| 7
| 1
| 2
| 1
| 1
| 0
|
| Injection site reaction
| 6
| 0
| 1
| 0
| 4
| 1
|
| Gastrointestinal
|
||||||
| Nausea
| 71
| 6
| 67
| 15
| 83
| 19
|
| Diarrhea
| 56
| 12
| 65
| 29
| 76
| 25
|
| Vomiting
| 41
| 4
| 43
| 13
| 64
| 23
|
| Stomatitis
| 38
| 0
| 25
| 1
| 19
| 1
|
| Anorexia
| 35
| 2
| 25
| 4
| 27
| 5
|
| Constipation
| 32
| 4
| 27
| 2
| 21
| 2
|
| Diarrhea-colostomy
| 13
| 2
| 16
| 7
| 16
| 3
|
| Gastrointestinal NOS
*
| 5
| 2
| 4
| 2
| 3
| 2
|
| Hematology/Infection
|
||||||
| Infection normal ANC
†
| 10
| 4
| 5
| 1
| 7
| 2
|
| Infection low ANC
†
| 8
| 8
| 12
| 11
| 9
| 8
|
| Lymphopenia
| 6
| 2
| 4
| 1
| 5
| 2
|
| Febrile neutropenia
| 4
| 4
| 15
| 14
| 12
| 11
|
| Hepatic/Metabolic/Laboratory/Renal
|
||||||
| Hyperglycemia
| 14
| 2
| 11
| 3
| 12
| 3
|
| Hypokalemia
| 11
| 3
| 7
| 4
| 6
| 2
|
| Dehydration
| 9
| 5
| 16
| 11
| 14
| 7
|
| Hypoalbuminemia
| 8
| 0
| 5
| 2
| 9
| 1
|
| Hyponatremia
| 8
| 2
| 7
| 4
| 4
| 1
|
| Urinary frequency
| 5
| 1
| 2
| 1
| 3
| 1
|
| Neurology
|
||||||
| Overall Neuropathy
| 82
| 19
| 18
| 2
| 69
| 7
|
| Paresthesias
| 77
| 18
| 16
| 2
| 62
| 6
|
| Pharyngo-laryngeal dysesthesias
| 38
| 2
| 1
| 0
| 28
| 1
|
| Neuro-sensory
| 12
| 1
| 2
| 0
| 9
| 1
|
| Neuro NOS
*
| 1
| 0
| 1
| 0
| 1
| 0
|
| Pulmonary
|
||||||
| Cough
| 35
| 1
| 25
| 2
| 17
| 1
|
| Dyspnea
| 18
| 7
| 14
| 3
| 11
| 2
|
| Hiccups
| 5
| 1
| 2
| 0
| 3
| 2
|
The following table provides adverse reactions reported in the previously untreated for advanced colorectal cancer study [see Clinical Studies (14)] by body system and decreasing order of frequency in the oxaliplatin and 5-FU/LV combination arm for events with overall incidences ≥5% but with incidences <1% NCI Grade 3/4 events.
|
|
|||
| Adverse reaction
(WHO/Pref) | Oxaliplatin +
5-FU/LV N=259 | Irinotecan +
5-FU/LV N=256 | Oxaliplatin +
irinotecan N=258 |
| All Grades
(%) | All Grades
(%) | All Grades
(%) |
|
| Allergy/Immunology
|
|||
| Rash
| 11
| 4
| 7
|
| Rhinitis allergic
| 10
| 6
| 6
|
| Cardiovascular
|
|||
| Edema
| 15
| 13
| 10
|
| Constitutional Symptoms/Pain/Ocular/Visual
|
|||
| Headache
| 13
| 6
| 9
|
| Weight loss
| 11
| 9
| 11
|
| Epistaxis
| 10
| 2
| 2
|
| Tearing
| 9
| 1
| 2
|
| Rigors
| 8
| 2
| 7
|
| Dysphasia
| 5
| 3
| 3
|
| Sweating
| 5
| 6
| 12
|
| Arthralgia
| 5
| 5
| 8
|
| Dermatology/Skin
|
|||
| Alopecia
| 38
| 44
| 67
|
| Flushing
| 7
| 2
| 5
|
| Pruritus
| 6
| 4
| 2
|
| Dry Skin
| 6
| 2
| 5
|
| Gastrointestinal
|
|||
| Taste perversion
| 14
| 6
| 8
|
| Dyspepsia
| 12
| 7
| 5
|
| Flatulence
| 9
| 6
| 5
|
| Mouth Dryness
| 5
| 2
| 3
|
| Hematology/Infection
|
|||
| Fever normal ANC
*
| 16
| 9
| 9
|
| Hepatic/Metabolic/Laboratory/Renal
|
|||
| Hypocalcemia
| 7
| 5
| 4
|
| Elevated Creatinine
| 4
| 4
| 5
|
| Neurology
|
|||
| Insomnia
| 13
| 9
| 11
|
| Depression
| 9
| 5
| 7
|
| Dizziness
| 8
| 6
| 10
|
| Anxiety
| 5
| 2
| 6
|
Adverse reactions were similar in men and women and in patients <65 and ≥65 years, but older patients may have been more susceptible to diarrhea, dehydration, hypokalemia, leukopenia, fatigue and syncope. The following additional adverse reactions, at least possibly related to treatment and potentially important, were reported in ≥2% and <5% of the patients in the oxaliplatin and 5-FU/LV combination arm (listed in decreasing order of frequency): metabolic, pneumonitis, catheter infection, vertigo, prothrombin time, pulmonary, rectal bleeding, dysuria, nail changes, chest pain, rectal pain, syncope, hypertension, hypoxia, unknown infection, bone pain, pigmentation changes, and urticaria.
Previously Treated Patients with Advanced Colorectal Cancer
Four hundred and fifty patients (about 150 receiving the combination of oxaliplatin and 5-FU/LV) were studied in a randomized trial in patients with refractory and relapsed colorectal cancer [see Clinical Studies (14)] . The adverse reaction profile in this study was similar to that seen in other studies and the adverse reactions in this trial are shown in the tables below. Thirteen percent of patients in the oxaliplatin and 5-FU/LV combination arm and 18% in the 5-FU/LV arm of the previously treated study had to discontinue treatment because of adverse effects related to gastrointestinal, or hematologic adverse reactions, or neuropathies. Both 5-FU and oxaliplatin are associated with gastrointestinal and hematologic adverse reactions. When oxaliplatin is administered in combination with 5-FU, the incidence of these events is increased.
The incidence of death within 30 days of treatment in the previously treated study, regardless of causality, was 5% with the oxaliplatin and 5-FU/LV combination, 8% with oxaliplatin alone, and 7% with 5-FU/LV. Of the 7 deaths that occurred on the oxaliplatin and 5-FU/LV combination arm within 30 days of stopping treatment, 3 may have been treatment related, associated with gastrointestinal bleeding or dehydration.
The following table provides adverse reactions reported in the previously treated study [see Clinical Studies (14)] by body system and in decreasing order of frequency in the oxaliplatin and 5-FU/LV combination arm for events with overall incidences ≥5% and for grade 3/4 events with incidences ≥1%. This table does not include hematologic and blood chemistry abnormalities; these are shown separately below.
| Adverse reaction
(WHO/Pref) | 5-FU/LV
(N=142) | Oxaliplatin
(N=153) | Oxaliplatin + 5-FU/LV
(N=150) |
|||
| All Grades
(%) | Grade 3/4
(%) | All Grades
(%) | Grade 3/4
(%) | All Grades
(%) | Grade 3/4
(%) |
|
| Any Event
| 98
| 41
| 100
| 46
| 99
| 73
|
| Cardiovascular
|
||||||
| Dyspnea
| 11
| 2
| 13
| 7
| 20
| 4
|
| Coughing
| 9
| 0
| 11
| 0
| 19
| 1
|
| Edema
| 13
| 1
| 10
| 1
| 15
| 1
|
| Thromboembolism
| 4
| 2
| 2
| 1
| 9
| 8
|
| Chest Pain
| 4
| 1
| 5
| 1
| 8
| 1
|
| Constitutional Symptoms/Pain
|
||||||
| Fatigue
| 52
| 6
| 61
| 9
| 68
| 7
|
| Back Pain
| 16
| 4
| 11
| 0
| 19
| 3
|
| Pain
| 9
| 3
| 14
| 3
| 15
| 2
|
| Dermatology/Skin
|
||||||
| Injection Site Reaction
| 5
| 1
| 9
| 0
| 10
| 3
|
| Gastrointestinal
|
||||||
| Diarrhea
| 44
| 3
| 46
| 4
| 67
| 11
|
| Nausea
| 59
| 4
| 64
| 4
| 65
| 11
|
| Vomiting
| 27
| 4
| 37
| 4
| 40
| 9
|
| Stomatitis
| 32
| 3
| 14
| 0
| 37
| 3
|
| Abdominal Pain
| 31
| 5
| 31
| 7
| 33
| 4
|
| Anorexia
| 20
| 1
| 20
| 2
| 29
| 3
|
| Gastroesophageal Reflux
| 3
| 0
| 1
| 0
| 5
| 2
|
| Hematology/Infection
|
||||||
| Fever
| 23
| 1
| 25
| 1
| 29
| 1
|
| Febrile Neutropenia
| 1
| 1
| 0
| 0
| 6
| 6
|
| Hepatic/Metabolic/Laboratory/Renal
|
||||||
| Hypokalemia
| 3
| 1
| 3
| 2
| 9
| 4
|
| Dehydration
| 6
| 4
| 5
| 3
| 8
| 3
|
| Neurology
|
||||||
| Neuropathy
| 17
| 0
| 76
| 7
| 74
| 7
|
| Acute
| 10
| 0
| 65
| 5
| 56
| 2
|
| Persistent
| 9
| 0
| 43
| 3
| 48
| 6
|
The following table provides adverse reactions reported in the previously treated study [see Clinical Studies (14)] by body system and in decreasing order of frequency in the oxaliplatin and 5-FU/LV combination arm for events with overall incidences ≥5% but with incidences <1% NCI Grade 3/4 events.
| Adverse reaction
(WHO/Pref) | 5-FU/LV
(N=142) | Oxaliplatin
(N=153) | Oxaliplatin +
5-FU/LV (N=150) |
| All Grades (%)
| All Grades (%)
| All Grades (%)
|
|
| Allergy/Immunology
|
|||
| Rhinitis
| 4
| 6
| 15
|
| Allergic Reaction
| 1
| 3
| 10
|
| Rash
| 5
| 5
| 9
|
| Cardiovascular
|
|||
| Peripheral Edema
| 11
| 5
| 10
|
| Constitutional Symptoms/Pain/Ocular/Visual
|
|||
| Headache
| 8
| 13
| 17
|
| Arthralgia
| 10
| 7
| 10
|
| Epistaxis
| 1
| 2
| 9
|
| Abnormal Lacrimation
| 6
| 1
| 7
|
| Rigors
| 6
| 9
| 7
|
| Dermatology/Skin
|
|||
| Hand-Foot Syndrome
| 13
| 1
| 11
|
| Flushing
| 2
| 3
| 10
|
| Alopecia
| 3
| 3
| 7
|
| Gastrointestinal
|
|||
| Constipation
| 23
| 31
| 32
|
| Dyspepsia
| 10
| 7
| 14
|
| Taste Perversion
| 1
| 5
| 13
|
| Mucositis
| 10
| 2
| 7
|
| Flatulence
| 6
| 3
| 5
|
| Hepatic/Metabolic/Laboratory/Renal
|
|||
| Hematuria
| 4
| 0
| 6
|
| Dysuria
| 1
| 1
| 6
|
| Neurology
|
|||
| Dizziness
| 8
| 7
| 13
|
| Insomnia
| 4
| 11
| 9
|
| Pulmonary
|
|||
| Upper Resp Tract Infection
| 4
| 7
| 10
|
| Pharyngitis
| 10
| 2
| 9
|
| Hiccup
| 0
| 2
| 5
|
Adverse reactions were similar in men and women and in patients <65 and ≥65 years, but older patients may have been more susceptible to dehydration, diarrhea, hypokalemia and fatigue. The following additional adverse reactions, at least possibly related to treatment and potentially important, were reported in ≥2% and <5% of the patients in the oxaliplatin and 5-FU/LV combination arm (listed in decreasing order of frequency): anxiety, myalgia, erythematous rash, increased sweating, conjunctivitis, weight decrease, dry mouth, rectal hemorrhage, depression, ataxia, ascites, hemorrhoids, muscle weakness, nervousness, tachycardia, abnormal micturition frequency, dry skin, pruritus, hemoptysis, purpura, vaginal hemorrhage, melena, somnolence, pneumonia, proctitis, involuntary muscle contractions, intestinal obstruction, gingivitis, tenesmus, hot flashes, enlarged abdomen, urinary incontinence.
Hematologic Changes
The following tables list the hematologic changes occurring in ≥5% of patients, based on laboratory values and NCI grade, with the exception of those events occurring in adjuvant patients and anemia in the patients previously untreated for advanced colorectal cancer, respectively, which are based on AE reporting and NCI grade alone.
| Hematology
Parameter | Oxaliplatin + 5-FU/LV
(N=1108) | 5-FU/LV
(N=1111) |
||
| All Grades
(%) | Grade 3/4
(%) | All Grades
(%) | Grade 3/4
(%) |
|
| Anemia
| 76
| 1
| 67
| <1
|
| Neutropenia
| 79
| 41
| 40
| 5
|
| Thrombocytopenia
| 77
| 2
| 19
| <1
|
| Hematology
Parameter | Oxaliplatin +
5-FU/LV N=259 | Irinotecan +
5-FU/LV N=256 | Oxaliplatin +
Irinotecan N=258 |
|||
| All Grades
(%) | Grade 3/4
(%) | All Grades
(%) | Grade 3/4
(%) | All Grades
(%) | Grade 3/4
(%) |
|
| Anemia
| 27
| 3
| 28
| 4
| 25
| 3
|
| Leukopenia
| 85
| 20
| 84
| 23
| 76
| 24
|
| Neutropenia
| 81
| 53
| 77
| 44
| 71
| 36
|
| Thrombocytopenia
| 71
| 5
| 26
| 2
| 44
| 4
|
| Hematology
Parameter | 5-FU/LV
(N=142) | Oxaliplatin
(N=153) | Oxaliplatin +
5-FU/LV (N=150) |
|||
| All Grades
(%) | Grade 3/4
(%) | All Grades
(%) | Grade 3/4
(%) | All Grades
(%) | Grade 3/4
(%) |
|
| Anemia
| 68
| 2
| 64
| 1
| 81
| 2
|
| Leukopenia
| 34
| 1
| 13
| 0
| 76
| 19
|
| Neutropenia
| 25
| 5
| 7
| 0
| 73
| 44
|
| Thrombocytopenia
| 20
| 0
| 30
| 3
| 64
| 4
|
Thrombocytopenia and Bleeding
Thrombocytopenia was frequently reported with the combination of oxaliplatin and infusional 5-FU/LV. The incidence of all hemorrhagic events in the adjuvant and previously treated patients was higher on the oxaliplatin combination arm compared to the infusional 5-FU/LV arm. These events included gastrointestinal bleeding, hematuria, and epistaxis. In the adjuvant trial, two patients died from intracerebral hemorrhages.
The incidence of Grade 3/4 thrombocytopenia was 2% in adjuvant patients with colon cancer. In patients treated for advanced colorectal cancer the incidence of Grade 3/4 thrombocytopenia was 3 to 5%, and the incidence of these events was greater for the combination of oxaliplatin and 5-FU/LV over the irinotecan plus 5-FU/LV or 5-FU/LV control groups. Grade 3/4 gastrointestinal bleeding was reported in 0.2% of adjuvant patients receiving oxaliplatin and 5-FU/LV. In the previously untreated patients, the incidence of epistaxis was 10% in the Oxaliplatin and 5-FU/LV arm, and 2% and 1%, respectively, in the irinotecan plus 5-FU/LV or irinotecan plus oxaliplatin arms.
Neutropenia
Neutropenia was frequently observed with the combination of oxaliplatin and 5-FU/LV, with Grade 3 and 4 events reported in 29% and 12% of adjuvant patients with colon cancer, respectively. In the adjuvant trial, 3 patients died from sepsis/neutropenic sepsis. Grade 3 and 4 events were reported in 35% and 18% of the patients previously untreated for advanced colorectal cancer, respectively. Grade 3 and 4 events were reported in 27% and 17% of previously treated patients, respectively. In adjuvant patients the incidence of either febrile neutropenia (0.7%) or documented infection with concomitant grade 3/4 neutropenia (1.1%) was 1.8% in the oxaliplatin and 5-FU/LV arm. The incidence of febrile neutropenia in the patients previously untreated for advanced colorectal cancer was 15% (3% of cycles) in the irinotecan plus 5-FU/LV arm and 4% (less than 1% of cycles) in the oxaliplatin and 5-FU/LV combination arm. Additionally, in this same population, infection with grade 3 or 4 neutropenia was 12% in the irinotecan plus 5-FU/LV, and 8% in the oxaliplatin and 5-FU/LV combination. The incidence of febrile neutropenia in the previously treated patients was 1% in the 5-FU/LV arm and 6% (less than 1% of cycles) in the oxaliplatin and 5-FU/LV combination arm.
Gastrointestinal
In patients receiving the combination of oxaliplatin plus infusional 5-FU/LV for adjuvant treatment for colon cancer the incidence of Grade 3/4 nausea and vomiting was greater than those receiving infusional 5-FU/LV alone (see table). In patients previously untreated for advanced colorectal cancer receiving the combination of oxaliplatin and 5-FU/LV, the incidence of Grade 3 and 4 vomiting and diarrhea was less compared to irinotecan plus 5-FU/LV controls (see table). In previously treated patients receiving the combination of oxaliplatin and 5-FU/LV, the incidence of Grade 3 and 4 nausea, vomiting, diarrhea, and mucositis/stomatitis increased compared to 5-FU/LV controls (see table).
The incidence of gastrointestinal adverse reactions in the previously untreated and previously treated patients appears to be similar across cycles. Premedication with antiemetics, including 5-HT 3 blockers, is recommended. Diarrhea and mucositis may be exacerbated by the addition of oxaliplatin to 5-FU/LV, and should be managed with appropriate supportive care. Since cold temperature can exacerbate acute neurological symptoms, ice (mucositis prophylaxis) should be avoided during the infusion of oxaliplatin.
Dermatologic
Oxaliplatin did not increase the incidence of alopecia compared to 5-FU/LV alone. No complete alopecia was reported. The incidence of Grade 3/4 skin disorders was 2% in both the oxaliplatin plus infusional 5-FU/LV and the infusional 5-FU/LV alone arms in the adjuvant colon cancer patients. The incidence of hand-foot syndrome in patients previously untreated for advanced colorectal cancer was 2% in the irinotecan plus 5-FU/LV arm and 7% in the oxaliplatin and 5-FU/LV combination arm. The incidence of hand-foot syndrome in previously treated patients was 13% in the 5-FU/LV arm and 11% in the oxaliplatin and 5-FU/LV combination arm.
Intravenous Site Reactions
Extravasation, in some cases including necrosis, has been reported.
Injection site reaction, including redness, swelling, and pain, has been reported.
Anticoagulation and Hemorrhage
There have been reports while on study and from post-marketing surveillance of prolonged prothrombin time and INR occasionally associated with hemorrhage in patients who received oxaliplatin plus 5-FU/LV while on anticoagulants. Patients receiving oxaliplatin plus 5-FU/LV and requiring oral anticoagulants may require closer monitoring.
Renal
About 5-10% of patients in all groups had some degree of elevation of serum creatinine. The incidence of Grade 3/4 elevations in serum creatinine in the oxaliplatin and 5-FU/LV combination arm was 1% in the previously treated patients. Serum creatinine measurements were not reported in the adjuvant trial.
Hepatic
Hepatotoxicity (defined as elevation of liver enzymes) appears to be related to oxaliplatin combination therapy [see Warnings and Precautions (5.4)] . The following tables list the clinical chemistry changes associated with hepatic toxicity occurring in ≥5% of patients, based on adverse reactions reported and NCI CTC grade for adjuvant patients and patients previously untreated for advanced colorectal cancer, laboratory values and NCI CTC grade for previously treated patients.
| Hepatic Parameter
| Oxaliplatin +5-FU/LV
(N=1108) | 5-FU/LV
(N=1111) |
||
| All Grades
(%) | Grade 3/4
(%) | All Grades
(%) | Grade 3/4
(%) |
|
| Increase in transaminases
| 57
| 2
| 34
| 1
|
| ALP increased
| 42
| <1
| 20
| <1
|
| Bilirubinaemia
| 20
| 4
| 20
| 5
|
| Clinical
Chemistry | Oxaliplatin + 5-FU/LV.
N=259 | irinotecan + 5-FU/LV
N=256 | Oxaliplatin + irinotecan
N=258 |
|||
| All Grades
(%) | Grade 3/4
(%) | All Grades
(%) | Grade 3/4
(%) | All Grades
(%) | Grade 3/4
(%) |
|
| ALT (SGPT-
ALAT) | 6
| 1
| 2
| 0
| 5
| 2
|
| AST (SGOT-
ASAT) | 17
| 1
| 2
| 1
| 11
| 1
|
| Alkaline
Phosphatase | 16
| 0
| 8
| 0
| 14
| 2
|
| Total Bilirubin
| 6
| 1
| 3
| 1
| 3
| 2
|
| Clinical Chemistry
| 5-FU/LV
(N=142) | Oxaliplatin
(N=153) | Oxaliplatin +
5-FU/LV (N=150) |
|||
| All Grades
(%) | Grade 3/4
(%) | All Grades
(%) | Grade 3/4
(%) | All Grades
(%) | Grade 3/4
(%) |
|
| ALT (SGPT-ALAT)
| 28
| 3
| 36
| 1
| 31
| 0
|
| AST (SGOT-ASAT)
| 39
| 2
| 54
| 4
| 47
| 0
|
| Total Bilirubin
| 22
| 6
| 13
| 5
| 13
| 1
|
Thromboembolism
The incidence of thromboembolic events in adjuvant patients with colon cancer was 6% (1.8% grade 3/4) in the infusional 5-FU/LV arm and 6% (1.2% grade 3/4) in the oxaliplatin and infusional 5-FU/LV combined arm, respectively. The incidence was 6 and 9% of the patients previously untreated for advanced colorectal cancer and previously treated patients in the oxaliplatin and 5-FU/LV combination arm, respectively.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of oxaliplatin. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Body as a whole:
angioedema, anaphylactic shock
Central and peripheral nervous system disorders:
loss of deep tendon reflexes, dysarthria, Lhermitte’s sign, cranial nerve palsies, fasciculations, convulsion
Liver and Gastrointestinal system disorders:
severe diarrhea/vomiting resulting in hypokalemia, colitis (including Clostridium difficile diarrhea), metabolic acidosis; ileus; intestinal obstruction, pancreatitis; veno-occlusive disease of liver also known as sinusoidal obstruction syndrome, and perisinusoidal fibrosis which rarely may progress.
Hearing and vestibular system disorders:
deafness
Platelet, bleeding, and clotting disorders:
immuno-allergic thrombocytopenia
prolongation of prothrombin time and of INR in patients receiving anticoagulants
Red Blood Cell disorders:
hemolytic uremic syndrome, immuno-allergic hemolytic anemia
Renal disorders:
Acute tubular necrosis, acute interstitial nephritis and acute renal failure.
Respiratory system disorders:
pulmonary fibrosis, and other interstitial lung diseases (sometimes fatal)
Vision disorders:
decrease of visual acuity, visual field disturbance, optic neuritis and transient vision loss (reversible following therapy discontinuation)
7 DRUG INTERACTIONS
No specific cytochrome P-450-based drug interaction studies have been conducted. No pharmacokinetic interaction between 85 mg/m 2 oxaliplatin and 5-fluorouracil (5-FU)/leucovorin (LV) has been observed in patients treated every 2 weeks. Increases of 5-FU plasma concentrations by approximately 20% have been observed with doses of 130 mg/m 2 oxaliplatin dosed every 3 weeks. Because platinum-containing species are eliminated primarily through the kidney, clearance of these products may be decreased by coadministration of potentially nephrotoxic compounds; although, this has not been specifically studied [see Clinical Pharmacology (12.3)].
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Pregnancy Category D
Based on direct interaction with DNA, oxaliplatin may cause fetal harm when administered to a pregnant woman. There are no adequate and well-controlled studies of oxaliplatin in pregnant women. Reproductive toxicity studies in rats demonstrated adverse effects on fertility and embryo-fetal development at maternal doses that were below the recommended human dose based on body surface area. If this drug is used during pregnancy or if the patient becomes pregnant while taking this drug, the patient should be apprised of the potential hazard to the fetus. Women of childbearing potential should be advised to avoid becoming pregnant and use effective contraception while receiving treatment with oxaliplatin.
Pregnant rats were administered oxaliplatin at less than one-tenth the recommended human dose based on body surface area during gestation days 1 to 5 (pre-implantation), 6 to 10, or 11 to 16 (during organogenesis). Oxaliplatin caused developmental mortality (increased early resorptions) when administered on days 6 to 10 and 11 to 16 and adversely affected fetal growth (decreased fetal weight, delayed ossification) when administered on days 6 to 10. Administration of oxaliplatin to male and female rats prior to mating resulted in 97% post-implantation loss in animals that received approximately one-seventh the recommended human dose based on the body surface area.
8.3 Nursing Mothers
It is not known whether oxaliplatin or its derivatives are excreted in human milk. Because many drugs are excreted in human milk and because of the potential for serious adverse reactions in nursing infants from oxaliplatin, a decision should be made whether to discontinue nursing or discontinue the use of the drug, taking into account the importance of the drug to the mother.
8.4 Pediatric Use
The effectiveness of oxaliplatin in children has not been established. Oxaliplatin has been tested in 2 Phase I and 2 Phase II trials in 159 patients ages 7 months to 22 years with solid tumors (see below) and no significant activity observed.
In a Phase I/II study, oxaliplatin was administered as a 2-hour IV infusion on days 1, 8 and 15 every 4 weeks (1 cycle), for a maximum of 6 cycles, to 43 patients with refractory or relapsed malignant solid tumors, mainly neuroblastoma and osteosarcoma. Twenty-eight pediatric patients in the Phase I study received oxaliplatin at 6 dose levels starting at 40 mg/m 2 with escalation to 110 mg/m 2. The dose limiting toxicity (DLT) was sensory neuropathy at the 110 mg/m 2 dose. Fifteen patients received oxaliplatin at a dose of 90 mg/m 2 IV in the Phase II portion of the study. At this dose, paresthesia (60%, G3/4: 7%), fever (40%, G3/4: 7%) and thrombocytopenia (40%, G3/4: 27%) were the main adverse reactions. No responses were observed.
In a second Phase I study, oxaliplatin was administered to 26 pediatric patients as a 2-hour IV infusion on day 1 every 3 weeks (1 cycle) at 5 dose levels starting at 100 mg/m 2 with escalation to 160 mg/m 2, for a maximum of 6 cycles. In a separate cohort, oxaliplatin 85 mg/m 2 was administered on day 1 every 2 weeks, for a maximum of 9 doses. Patients had metastatic or unresectable solid tumors mainly neuroblastoma and ganglioneuroblastoma. No responses were observed. The DLT was sensory neuropathy at the 160 mg/m 2 dose. Based on these studies, oxaliplatin 130 mg/m 2 as a 2-hour IV infusion on day 1 every 3 weeks (1 cycle) was used in subsequent Phase II studies. A dose of 85 mg/m 2 on day 1 every 2 weeks was also found to be tolerable.
In one Phase II study, 43 pediatric patients with recurrent or refractory embryonal CNS tumors received oxaliplatin 130 mg/m 2 every 3 weeks for a maximum of 12 months in absence of progressive disease or unacceptable toxicity. In patients < 10 kg the oxaliplatin dose used was 4.3 mg/kg. The most common adverse reactions reported were leukopenia (67%, G3/4: 12%), anemia (65%, G3/4: 5%), thrombocytopenia (65%, G3/4: 26%), vomiting (65%, G3/4: 7%), neutropenia (58%, G3/4: 16%) and sensory neuropathy (40%, G3/4: 5%). One partial response was observed.
In a second Phase II study, 47 pediatric patients with recurrent solid tumors, including Ewing sarcoma or peripheral PNET, osteosarcoma, rhabdomyosarcoma and neuroblastoma, received oxaliplatin 130 mg/m 2 every 3 weeks for a maximum of 12 months or 17 cycles. In patients ≤ 12 months old the oxaliplatin dose used was 4.3 mg/kg. The most common adverse reactions reported were sensory neuropathy (53%, G3/4: 15%), thrombocytopenia (40%, G3/4: 26%), anemia (40%, G3/4: 15%), vomiting (32%, G3/4: 0%), nausea (30%, G3/4: 2%) and AST increased (26%, G3/4: 4%). No responses were observed.
The pharmacokinetic parameters of ultrafiltrable platinum have been evaluated in 105 pediatric patients during the first cycle. The mean clearance in pediatric patients estimated by the population pharmacokinetic analysis was 4.7 L/h. The inter-patient variability of platinum clearance in pediatric cancer patients was 41%. Mean platinum pharmacokinetic parameters in ultrafiltrate were C max of 0.75 ± 0.24 mcg/mL, AUC 0-48 of 7.52 ± 5.07 mcgh/mL and AUC inf of 8.83±1.57 mcgh/mL at 85 mg/m 2 of oxaliplatin and C max of 1.1 ± 0.43 mcg/mL, AUC 0-48 of 9.74 ± 2.52 mcgh/mL and AUC inf of 17.3 ± 5.34 mcgh/mL at 130 mg/m 2 of oxaliplatin.
8.5 Geriatric Use
No significant effect of age on the clearance of ultrafilterable platinum has been observed.
In the adjuvant therapy colon cancer randomized clinical trial, [see Clinical Studies (14)] 723 patients treated with oxaliplatin and infusional 5-fluorouracil (5-FU)/leucovorin (LV) were <65 years and 400 patients were ≥65 years. A descriptive subgroup analysis demonstrated that the improvement in DFS for the oxaliplatin combination arm compared to the infusional 5-FU/LV alone arm appeared to be maintained across genders. The effect of oxaliplatin in patients ≥65 years of age was not conclusive. Insufficient subgroup sizes prevented analysis by race. Patients ≥65 years of age receiving the oxaliplatin combination therapy experienced more grade 3-4 granulocytopenia than patients < 65 years of age (45% versus 39%).
In the previously untreated for advanced colorectal cancer randomized clinical trial [see Clinical Studies (14)] of oxaliplatin, 160 patients treated with oxaliplatin and 5-FU/LV were < 65 years and 99 patients were ≥65 years. The same efficacy improvements in response rate, time to tumor progression, and overall survival were observed in the ≥65 year old patients as in the overall study population. In the previously treated for advanced colorectal cancer randomized clinical trial [see Clinical Studies (14)] of oxaliplatin, 95 patients treated with oxaliplatin and 5-FU/LV were <65 years and 55 patients were ≥65 years. The rates of overall adverse reactions, including grade 3 and 4 events, were similar across and within arms in the different age groups in all studies. The incidence of diarrhea, dehydration, hypokalemia, leukopenia, fatigue and syncope were higher in patients ≥65 years old. No adjustment to starting dose was required in patients ≥65 years old.
8.6 Patients with Renal Impairment
The safety and effectiveness of the combination of oxaliplatin and 5-FU/LV in patients with renal impairment have not been evaluated. The combination of oxaliplatin and 5-FU/LV should be used with caution in patients with preexisting renal impairment since the primary route of platinum elimination is renal. Clearance of ultrafilterable platinum is decreased in patients with mild, moderate, and severe renal impairment. A pharmacodynamic relationship between platinum ultrafiltrate levels and clinical safety and effectiveness has not been established [see Adverse Reactions (6.1)and Clinical Pharmacology (12.3)] .
10 OVERDOSAGE
There is no known antidote for oxaliplatin overdose. In addition to thrombocytopenia, the anticipated complications of an oxaliplatin overdose include hypersensitivity reaction, myelosuppression, nausea, vomiting, diarrhea and neurotoxicity.
Several cases of overdoses have been reported with oxaliplatin. Adverse reactions observed were Grade 4 thrombocytopenia (<25,000/mm 3) without any bleeding, anemia, sensory neuropathy such as paresthesia, dysesthesia, laryngospasm and facial muscle spasms, gastrointestinal disorders such as nausea, vomiting, stomatitis, flatulence, abdomen enlarged and Grade 4 intestinal obstruction, Grade 4 dehydration, dyspnea, wheezing, chest pain, respiratory failure, severe bradycardia and death.
Patients suspected of receiving an overdose should be monitored, and supportive treatment should be administered. The maximum dose of oxaliplatin that has been administered in a single infusion is 825 mg.
11 DESCRIPTION
Oxaliplatin is an antineoplastic agent with the molecular formula C 8H 14N 2O 4Pt and the chemical name of cis-[(1 R,2 R)-1,2-cyclohexanediamine- N,N’] [oxalato(2-)- O,O’] platinum. Oxaliplatin is an organoplatinum complex in which the platinum atom is complexed with 1,2-diaminocyclohexane(DACH) and with an oxalate ligand as a leaving group.
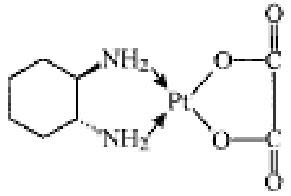
The molecular weight is 397.3. Oxaliplatin is slightly soluble in water at 6 mg/mL, very slightly soluble in methanol, and practically insoluble in ethanol and acetone.
Oxaliplatin for Injection is supplied in vials containing 50 mg or 100 mg of oxaliplatin as a sterile, preservative-free lyophilized powder for reconstitution. Lactose monohydrate is present as an inactive ingredient.
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Oxaliplatin undergoes nonenzymatic conversion in physiologic solutions to active derivatives via displacement of the labile oxalate ligand. Several transient reactive species are formed, including monoaquo and diaquo DACH platinum, which covalently bind with macromolecules. Both inter- and intrastrand Pt-DNA crosslinks are formed. Crosslinks are formed between the N7 positions of two adjacent guanines (GG), adjacent adenine-guanines (AG), and guanines separated by an intervening nucleotide (GNG). These crosslinks inhibit DNA replication and transcription. Cytotoxicity is cell-cycle nonspecific. In vivo studies have shown antitumor activity of oxaliplatin against colon carcinoma. In combination with 5-fluorouracil (5-FU), oxaliplatin exhibits in vitro and in vivo antiproliferative activity greater than either compound alone in several tumor models [HT29 (colon), GR (mammary), and L1210 (leukemia)].
12.3 Pharmacokinetics
The reactive oxaliplatin derivatives are present as a fraction of the unbound platinum in plasma ultrafiltrate. The decline of ultrafilterable platinum levels following oxaliplatin administration is triphasic, characterized by two relatively short distribution phases (t 1/2α; 0.43 hours and t 1/2β; 16.8 hours) and a long terminal elimination phase (t 1/2γ; 391 hours). Pharmacokinetic parameters obtained after a single 2-hour IV infusion of oxaliplatin at a dose of 85 mg/m 2 expressed as ultrafilterable platinum were C max of 0.814 mcg /mL and volume of distribution of 440 L.
Interpatient and intrapatient variability in ultrafilterable platinum exposure (AUC 0-48hr) assessed over 3 cycles was moderate to low (23% and 6%, respectively). A pharmacodynamic relationship between platinum ultrafiltrate levels and clinical safety and effectiveness has not been established.
Distribution
At the end of a 2-hour infusion of oxaliplatin, approximately 15% of the administered platinum is present in the systemic circulation. The remaining 85% is rapidly distributed into tissues or eliminated in the urine. In patients, plasma protein binding of platinum is irreversible and is greater than 90%. The main binding proteins are albumin and gamma-globulins. Platinum also binds irreversibly and accumulates (approximately 2-fold) in erythrocytes, where it appears to have no relevant activity. No platinum accumulation was observed in plasma ultrafiltrate following 85 mg/m 2 every two weeks.
Metabolism
Oxaliplatin undergoes rapid and extensive nonenzymatic biotransformation. There is no evidence of cytochrome P450-mediated metabolism in vitro.
Up to 17 platinum-containing derivatives have been observed in plasma ultrafiltrate samples from patients, including several cytotoxic species (monochloro DACH platinum, dichloro DACH platinum, and monoaquo and diaquo DACH platinum) and a number of noncytotoxic, conjugated species.
Elimination
The major route of platinum elimination is renal excretion. At five days after a single 2-hour infusion of oxaliplatin, urinary elimination accounted for about 54% of the platinum eliminated, with fecal excretion accounting for only about 2%. Platinum was cleared from plasma at a rate (10 to 17 L/h) that was similar to or exceeded the average human glomerular filtration rate (GFR; 7.5 L/h). There was no significant effect of gender on the clearance of ultrafilterable platinum. The renal clearance of ultrafilterable platinum is significantly correlated with GFR.
Pharmacokinetics in Special Populations
Pediatric
[See Use In Specific Patient Populations (8.4)] .
Renal Impairment
The AUC 0-48hr of platinum in the plasma ultrafiltrate increases as renal function decreases. The AUC 0-48hr of platinum in patients with mild (creatinine clearance, CL cr 50 to 80 mL/min), moderate (CL cr 30 to <50 mL/min) and severe renal (CL cr <30 mL/min) impairment is increased by about 60, 140 and 190%, respectively, compared to patients with normal renal function (CL cr >80 mL/min) [see Adverse Reactions (6), Drug Interactions (7) and Use In Specific Patient Populations (8.6)].
Drug - Drug Interactions
No pharmacokinetic interaction between 85 mg/m 2 of Oxaliplatin and infusional 5-FU has been observed in patients treated every 2 weeks, but increases of 5-FU plasma concentrations by approximately 20% have been observed with doses of 130 mg/m 2 of oxaliplatin administered every 3 weeks. In vitro, platinum was not displaced from plasma proteins by the following medications: erythromycin, salicylate, sodium valproate, granisetron, and paclitaxel. In vitro, oxaliplatin is not metabolized by, nor does it inhibit, human cytochrome P450 isoenzymes. No P450-mediated drug-drug interactions are therefore anticipated in patients.
Since platinum-containing species are eliminated primarily through the kidney, clearance of these products may be decreased by co-administration of potentially nephrotoxic compounds, although this has not been specifically studied.
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment Of Fertility
Long-term animal studies have not been performed to evaluate the carcinogenic potential of oxaliplatin. Oxaliplatin was not mutagenic to bacteria (Ames test) but was mutagenic to mammalian cells in vitro (L5178Y mouse lymphoma assay). Oxaliplatin was clastogenic both in vitro (chromosome aberration in human lymphocytes) and in vivo (mouse bone marrow micronucleus assay).
In a fertility study, male rats were given oxaliplatin at 0, 0.5, 1, or 2 mg/kg/day for five days every 21 days for a total of three cycles prior to mating with females that received two cycles of oxaliplatin on the same schedule. A dose of 2 mg/kg/day (less than one-seventh the recommended human dose on a body surface area basis) did not affect pregnancy rate, but caused developmental mortality (increased early resorptions, decreased live fetuses, decreased live births) and delayed growth (decreased fetal weight).
Testicular damage, characterized by degeneration, hypoplasia, and atrophy, was observed in dogs administered oxaliplatin at 0.75 mg/kg/day x 5 days every 28 days for three cycles. A no effect level was not identified. This daily dose is approximately one-sixth of the recommended human dose on a body surface area basis.
14 CLINICAL STUDIES
14.1 Combination Adjuvant Therapy with Oxaliplatin and Infusional 5-fluorouracil/leucovorin in Patients with Colon Cancer
An international, multicenter, randomized study compared the efficacy and evaluated the safety of oxaliplatin in combination with an infusional schedule of 5-fluorouracil (5-FU)/leucovorin (LV)to infusional 5-FU/LV alone, in patients with stage II (Dukes’ B2) or III (Dukes’ C) colon cancer who had undergone complete resection of the primary tumor. The primary objective of the study was to compare the 3-year disease-free survival (DFS) in patients receiving oxaliplatin and infusional 5-FU/LV to those receiving 5-FU/LV alone. Patients were to be treated for a total of 6 months (i.e., 12 cycles). A total of 2246 patients were randomized; 1123 patients per study arm. Patients in the study had to be between 18 and 75 years of age, have histologically proven stage II (T 3-T 4 N0 M0; Dukes’ B2) or III (any T N 1-2 M0; Dukes’ C) colon carcinoma (with the inferior pole of the tumor above the peritoneal reflection, i.e., ≥15 cm from the anal margin) and undergone (within 7 weeks prior to randomization) complete resection of the primary tumor without gross or microscopic evidence of residual disease. Patients had to have had no prior chemotherapy, immunotherapy or radiotherapy, and have an ECOG performance status of 0,1, or 2 (KPS ≥ 60%), absolute neutrophil count (ANC) > 1.5x10 9/L, platelets ≥100x10 9/L, serum creatinine < 1.25 x ULN total bilirubin < 2 x ULN, AST/ALT < 2 x ULN and carcino-embyrogenic antigen (CEA) < 10 ng/mL. Patients with preexisting peripheral neuropathy (NCI grade ≥ 1) were ineligible for this trial.
The following table shows the dosing regimens for the two arms of the study.
Table 15 - Dosing Regimens in Adjuvant Therapy Study
| Treatment Arm
| Dose
| Regimen
|
| Oxaliplatin + 5-FU/LV
(FOLFOX4) (N =1123) | Day 1: Oxaliplatin: 85 mg/m
2 (2-hour infusion) + LV:
200 mg/m 2 (2-hour infusion), followed by 5-FU: 400 mg/m 2 (bolus), 600 mg/m 2 (22-hour infusion) Day 2: LV: 200 mg/m 2 (2-hour infusion), followed by 5-FU: 400 mg/m 2 (bolus), 600 mg/m 2 (22-hour infusion) | every 2 weeks
12 cycles |
| 5-FU/LV
(N=1123) | Day 1: LV: 200 mg/m
2 (2-hour infusion), followed by
5-FU: 400 mg/m 2 (bolus), 600 mg/m 2 (22-hour infusion) Day 2: LV: 200 mg/m 2 (2-hour infusion), followed by 5-FU: 400 mg/m 2 (bolus), 600 mg/m 2 (22-hour infusion) | every 2 weeks
12 cycles |
The following tables show the baseline characteristics and dosing of the patient population entered into this study. The baseline characteristics were well balanced between arms.
Table 16 - Patient Characteristics in Adjuvant Therapy Study
| Oxaliplatin + infusional 5-FU/LV
N=1123 | Infusional 5-FU/LV
N=1123 |
|
| Sex: Male (%) | 56.1
| 52.4
|
| Female (%) | 43.9
| 47.6
|
| Median age (years) | 61
| 60
|
| <65 years of age (%) | 64.4
| 66.2
|
| ≥65 years of age (%) | 35.6
| 33.8
|
| Karnofsky Performance Status (KPS) (%)
|
||
| 100
| 29.7
| 30.5
|
| 90
| 52.2
| 53.9
|
| 80
| 4.4
| 3.3
|
| 70
| 13.2
| 11.9
|
| <60
| 0.6
| 0.4
|
| Primary site (%)
|
||
| Colon including cecum | 54.6
| 54.4
|
| Sigmoid | 31.9
| 33.8
|
| Recto sigmoid | 12.9
| 10.9
|
| Other including rectum | 0.6
| 0.9
|
| Bowel obstruction (%)
|
||
| Yes
| 17.9
| 19.3
|
| Perforation (%)
|
||
| Yes
| 6.9
| 6.9
|
| Stage at Randomization (%)
|
||
| II (T=3,4 N=0, M=0) | 40.1
| 39.9
|
| III (T=any, N=1,2, M=0) | 59.6
| 59.3
|
| IV (T=any, N=any, M=1) | 0.4
| 0.8
|
| Staging – T (%)
|
||
| T1
| 0.5
| 0.7
|
| T2
| 4.5
| 4.8
|
| T3
| 76
| 75.9
|
| T4
| 19
| 18.5
|
| Staging – N (%)
|
||
| N0
| 40.2
| 39.9
|
| N1
| 39.4
| 39.4
|
| N2
| 20.4
| 20.7
|
| Staging – M (%)
|
||
| M1
| 0.4
| 0.8
|
Table 17 - Dosing in Adjuvant Therapy Study
|
| Oxaliplatin + infusional
5-FU/LV N=1108 | Infusional
5-FU/LV N=1111 |
| Median Relative Dose Intensity (%) | ||
| 5-FU | 84.4
| 97.7
|
| Oxaliplatin | 80.5
| N/A
|
| Median Number of Cycles | 12
| 12
|
| Median Number of cycles with Oxaliplatin | 11
| N/A
|
The following table and figures summarize the disease-free survival (DFS) results in the overall randomized population and in patients with stage II and III disease based on an ITT analysis. The median duration of follow-up was approximately 77 months.
Table 18 - Summary of DFS analysis - ITT analysis
| Parameter | Oxaliplatin +Infusional
5-FU/LV | Infusional
5-FU/LV |
| Overall
|
||
| N
| 1123
| 1123
|
| Number of events – relapse or death (%) | 304 (27.1)
| 360 (32.1)
|
| Disease-free survival % [95% CI] * | 73.3 [70.7, 76]
| 67.4 [64.6, 70.2]
|
| Hazard ratio [95% CI] ** | 0.8 [0.68, 0.93]
|
|
| Stratified Logrank test | p=0.003
|
|
| Stage III (Dukes’ C)
|
||
| N
| 672
| 675
|
| Number of events –relapse or death (%) | 226 (33.6)
| 271 (40.1)
|
| Disease-free survival % [95% CI] * | 66.4 [62.7, 70]
| 58.9 [55.2, 62.7]
|
| Hazard ratio [95% CI] ** | 0.78 [0.65, 0.93]
|
|
| Logrank test | p=0.005
|
|
| Stage II (Dukes’ B2)
|
||
| N
| 451
| 448
|
| Number of events – relapse or death (%) | 78 (17.3)
| 89 (19.9)
|
| Disease-free survival % [95% CI] * | 83.7 [80.2, 87.1]
| 79.9 [76.2, 83.7]
|
| Hazard ratio [95% CI] ** | 0.84 [0.62, 1.14]
|
|
| Logrank test | p=0.258
|
|
Data cut off for disease free survival 1 June 2006
* Disease-free survival at 5 years
**A hazard ratio of less than 1 favors Oxaliplatin + Infusional 5-FU/LV
In the overall and stage III colon cancer populations DFS was statistically significantly improved in the oxaliplatin combination arm compared to infusional 5-FU/LV alone. However, a statistically significant improvement in DFS was not noted in Stage II patients.
Figure 2 shows the DFS Kaplan-Meier curves for the comparison of oxaliplatin and infusional 5-FU/LV combination and infusional 5-FU/LV alone for the overall population (ITT analysis).
Figure 3 shows the DFS Kaplan-Meier curves for the comparison of oxaliplatin and infusional 5-FU/LV combination and infusional 5-FU/LV alone in Stage III patients.
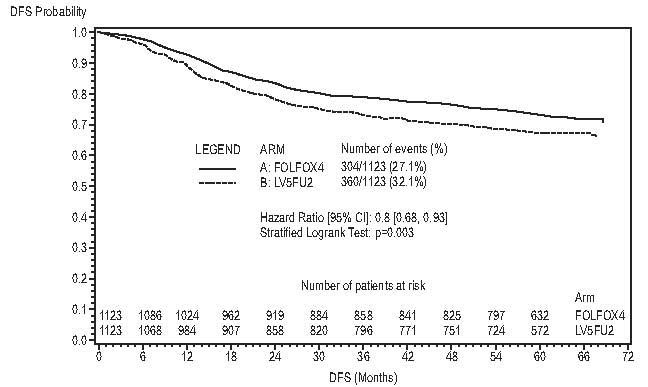
Figure 2 - DFS Kaplan-Meier curves by treatment arm (cutoff: 1 June 2006) – ITT population
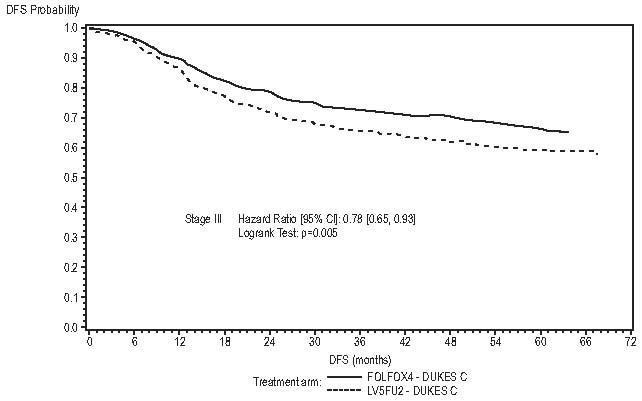
Figure 3 - DFS Kaplan-Meier curves by treatment arm in Stage III patients (cutoff: 1 June 2006) – ITT population
The following table summarizes the overall survival (OS) results in the overall randomized population and in patients with stage II and III disease, based on the ITT analysis.
Table 19 - Summary of OS analysis - ITT analysis
| Parameter | Oxaliplatin +
Infusional 5-FU/LV | Infusional 5-FU/LV
|
| Overall
|
||
| N
| 1123
| 1123
|
| Number of death events (%)
| 245 (21.8)
| 283 (25.2)
|
| Hazard ratio* [95% CI]
| 0.84 [0.71, 1]
|
|
| Stage III (Dukes’ C)
|
||
| N
| 672
| 675
|
| Number of death events (%)
| 182 (27.1)
| 220 (32.6)
|
| Hazard ratio* [95% CI]
| 0.8 [0.65, 0.97]
|
|
| Stage II (Dukes’ B2)
|
||
| N
| 451
| 448
|
| Number of death events (%)
| 63 (14)
| 63 (14.1)
|
| Hazard ratio* [95% CI]
| 1 [0.7, 1.41]
|
|
*A hazard ratio of less than 1 favors Oxaliplatin + Infusional 5-FU/LV
Data cut off for overall survival 16 January 2007
14.2 Combination Therapy with Oxaliplatin and 5-fluorouracil/leucovorin in Patients Previously Untreated for Advanced Colorectal Cancer
A North American, multicenter, open-label, randomized controlled study was sponsored by the National Cancer Institute (NCI) as an intergroup study led by the North Central Cancer Treatment Group (NCCTG). The study had 7 arms at different times during its conduct, four of which were closed due to either changes in the standard of care, toxicity, or simplification. During the study, the control arm was changed to irinotecan plus 5-fluorouracil (5-FU)/leucovorin (LV). The results reported below compared the efficacy and safety of two experimental regimens, oxaliplatin in combination with infusional 5-FU/LV and a combination of oxaliplatin plus irinotecan, to an approved control regimen of irinotecan plus 5-FU/LV in 795 concurrently randomized patients previously untreated for locally advanced or metastatic colorectal cancer. After completion of enrollment, the dose of irinotecan plus 5-FU/LV was decreased due to toxicity. Patients had to be at least 18 years of age, have known locally advanced, locally recurrent, or metastatic colorectal adenocarcinoma not curable by surgery or amenable to radiation therapy with curative intent, histologically proven colorectal adenocarcinoma, measurable or evaluable disease, with an ECOG performance status 0, 1, or 2. Patients had to have granulocyte count ≥1.5 x 10 9/L, platelets ≥ 100 x 10 9/L, hemoglobin ≥9 gm/dL, creatinine <1.5 x ULN, total bilirubin < 1.5 mg/dL, AST <5 x ULN, and alkaline phosphatase < 5 x ULN. Patients may have received adjuvant therapy for resected Stage II or III disease without recurrence within 12 months. The patients were stratified for ECOG performance status (0, 1 vs. 2), prior adjuvant chemotherapy (yes vs. no), prior immunotherapy (yes vs. no), and age (<65 vs. ≥65 years). Although no post study treatment was specified in the protocol, 65 to 72% of patients received additional post study chemotherapy after study treatment discontinuation on all arms. Fifty-eight percent of patients on the oxaliplatin plus 5-FU/LV arm received an irinotecan-containing regimen and 23% of patients on the irinotecan plus 5-FU/LV arm received oxaliplatin-containing regimens. Oxaliplatin was not commercially available during the trial.
The following table presents the dosing regimens of the three arms of the study.
Table 20 – Dosing Regimens in Patients Previously Untreated for Advanced Colorectal Cancer Clinical Trial
| Treatment Arm
| Dose
| Regimen
|
| Oxaliplatin +
5-FU/LV (FOLFOX4) (N=267) | Day 1: Oxaliplatin: 85 mg/m
2 (2-hour infusion) +
LV 200 mg/m 2 (2-hour infusion), followed by 5-FU: 400 mg/m 2 (bolus), 600 mg/m 2 (22-hour infusion) Day 2: LV 200 mg/m 2 (2-hour infusion), followed by 5-FU: 400 mg/m 2 (bolus), 600 mg/m 2 (22-hour infusion) | every 2 weeks
|
| Irinotecan +
5-FU/LV (IFL) (N=264) | Day 1: irinotecan 125 mg/m
2 as a 90–min
infusion + LV 20 mg/m 2 as a 15-min infusion or intravenous push, followed by 5-FU 500 mg/m 2 intravenous bolus weekly x 4 | Every 6 weeks
|
| Oxaliplatin
+ Irinotecan (IROX) (N=264) | Day 1: Oxaliplatin: 85 mg/m
2 intravenous (2-
hour infusion) + irinotecan 200 mg/m 2 intravenous over 30 minutes | every 3 weeks
|
The following table presents the demographics of the patient population entered into this study.
Table 21 – Patient Demographics in Patients Previously Untreated for Advanced Colorectal Cancer Clinical Trial
|
| Oxaliplatin +
5-FU/LV N=267 | Irinotecan +
5-FU/LV N=264 | Oxaliplatin + irinotecan
N=264 |
| Sex: Male (%) | 58.8
| 65.2
| 61
|
| Female (%) | 41.2
| 34.8
| 39
|
| Median age (years) | 61
| 61
| 61
|
| <65 years of age (%) | 61
| 62
| 63
|
| ≥65 years of age (%) | 39
| 38
| 37
|
| ECOG (%)
|
|||
| 0.1 | 94.4
| 95.5
| 94.7
|
| 2 | 5.6
| 4.5
| 5.3
|
| Involved organs (%)
|
|||
| Colon only | 0.7
| 0.8
| 0.4
|
| Liver only | 39.3
| 44.3
| 39
|
| Liver + other | 41.2
| 38.6
| 40.9
|
| Lung only | 6.4
| 3.8
| 5.3
|
| Other (including lymph nodes) | 11.6
| 11
| 12.9
|
| Not reported | 0.7
| 1.5
| 1.5
|
| Prior radiation (%) | 3
| 1.5
| 3
|
| Prior surgery (%) | 74.5
| 79.2
| 81.8
|
| Prior adjuvant (%) | 15.7
| 14.8
| 15.2
|
The length of a treatment cycle was 2 weeks for the oxaliplatin and 5-FU/LV regimen; 6 weeks for the irinotecan plus 5-FU/LV regimen; and 3 weeks for the oxaliplatin plus irinotecan regimen. The median number of cycles administered per patient was 10 (23.9 weeks) for the oxaliplatin and 5-FU/LV regimen, 4 (23.6 weeks) for the irinotecan plus 5-FU/LV regimen, and 7 (21 weeks) for the oxaliplatin plus irinotecan regimen. Patients treated with the oxaliplatin and 5-FU/LV combination had a significantly longer time to tumor progression based on investigator assessment, longer overall survival, and a significantly higher confirmed response rate based on investigator assessment compared to patients given irinotecan plus 5-FU/LV. The following table summarizes the efficacy results.
Table 22 – Summary of Efficacy
|
| Oxaliplatin +
5-FU/LV N=267 | irinotecan +
5-FU/LV N=264 | Oxaliplatin +
Irinotecan N=264 |
| Survival (ITT)
|
|||
| Number of deaths N (%) | 155 (58.1)
| 192 (72.7)
| 175 (66.3)
|
| Median survival (months) | 19.4
| 14.6
| 17.6
|
| Hazard Ratio and (95% confidence interval) | 0.65 (0.53-0.8)*
| ||
| P-value | <0.0001*
| -
| -
|
| TTP (ITT, investigator assessment)
|
|||
| Percentage of progressors | 82.8
| 81.8
| 89.4
|
| Median TTP (months) | 8.7
| 6.9
| 6.5
|
| Hazard Ratio and (95% confidence interval) *** | 0.74 (0.61-0.89)*
| ||
| P-value | 0.0014*
| -
| -
|
| Response Rate (investigator assessment)**
|
|||
| Patients with measurable disease | 210
| 212
| 215
|
| Complete response N (%) | 13 (6.2)
| 5 (2.4)
| 7 (3.3)
|
| Partial response N (%) | 82 (39)
| 64 (30.2)
| 67 (31.2)
|
| Complete and partial response N (%) | 95 (45.2)
| 69 (32.5)
| 74 (34.4)
|
| 95% confidence interval | (38.5 – 52)
| (26.2 – 38.9)
| (28.1 – 40.8)
|
| P-value | 0.008*
| -
| -
|
* Compared to irinotecan plus 5-FU/LV (IFL) arm
** Based on all patients with measurable disease at baseline
The numbers in the response rate and TTP analysis are based on unblinded investigator assessment.
*** A hazard ratio of less than 1 favors Oxaliplatin + Infusional 5-FU/LV
Figure 4 illustrates the Kaplan-Meier survival curves for the comparison of oxaliplatin and 5-FU/LV combination and oxaliplatin plus irinotecan to irinotecan plus 5-FU/LV.
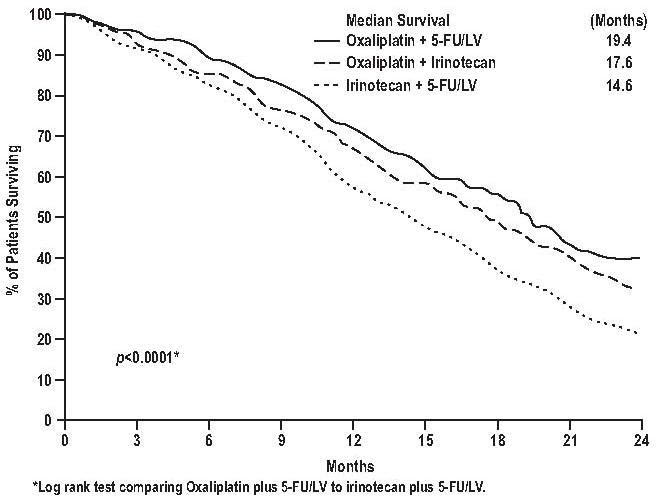
Figure 4 – Kaplan-Meier Overall Survival by treatment arm
A descriptive subgroup analysis demonstrated that the improvement in survival for oxaliplatin plus 5-FU/LV compared to irinotecan plus 5-FU/LV appeared to be maintained across age groups, prior adjuvant therapy, and number of organs involved. An estimated survival advantage in oxaliplatin plus 5-FU/LV versus irinotecan plus 5-FU/LV was seen in both genders; however it was greater among women than men. Insufficient subgroup sizes prevented analysis by race.
14.3 Combination Therapy with Oxaliplatin and 5-fluorouracil/leucovorin in Previously Treated Patients with Advanced Colorectal Cancer
A multicenter, open-label, randomized, three-arm controlled study was conducted in the US and Canada comparing the efficacy and safety of oxaliplatin in combination with an infusional schedule of 5-fluorouracil (5-FU)/leucovorin (LV)to the same dose and schedule of 5-FU/LV alone and to single agent oxaliplatin in patients with advanced colorectal cancer who had relapsed/progressed during or within 6 months of first-line therapy with bolus 5-FU/LV and irinotecan. The study was intended to be analyzed for response rate after 450 patients were enrolled. Survival will be subsequently assessed in all patients enrolled in the completed study. Accrual to this study is complete, with 821 patients enrolled. Patients in the study had to be at least 18 years of age, have unresectable, measurable, histologically proven colorectal adenocarcinoma, with a Karnofsky performance status >50%. Patients had to have SGOT (AST) and SGPT (ALT) <2x the institution’s upper limit of normal (ULN), unless liver metastases were present and documented at baseline by CT or MRI scan, in which case <5x ULN was permitted. Patients had to have alkaline phosphatase ≤2x the institution’s ULN, unless liver metastases were present and documented at baseline by CT or MRI scan, in which cases <5x ULN was permitted. Prior radiotherapy was permitted if it had been completed at least 3 weeks before randomization.
The dosing regimens of the three arms of the study are presented in the table below.
Table 23 – Dosing Regimens in Refractory and Relapsed Colorectal Cancer Clinical Trial
| Treatment Arm
| Dose
| Regimen
|
|
Oxaliplatin + 5-FU/LV (N =152) | Day 1: Oxaliplatin: 85 mg/m
2 (2-hour infusion) + LV 200 mg/m
2
(2-hour infusion), followed by 5-FU: 400 mg/m 2 (bolus), 600 mg/m 2 (22-hour infusion) Day 2: LV 200 mg/m 2 (2-hour infusion), followed by 5-FU: 400 mg/m 2 (bolus), 600 mg/m 2 (22-hour infusion) | every 2 weeks
|
|
5-FU/LV (N=151) | Day 1: LV 200 mg/m
2 (2-hour infusion), followed by 5-FU:
400 mg/m 2 (bolus), 600 mg/m 2 (22-hour infusion) Day 2: LV 200 mg/m 2 (2-hour infusion), followed by 5-FU: 400 mg/m 2 (bolus), 600 mg/m 2 (22-hour infusion) | every 2 weeks
|
| Oxaliplatin
(N=156) | Day 1: Oxaliplatin 85 mg/m
2 (2-hour infusion)
| every 2 weeks
|
Patients entered into the study for evaluation of response must have had at least one unidimensional lesion measuring ≥20 mm using conventional CT or MRI scans, or ≥10 mm using a spiral CT scan. Tumor response and progression were assessed every 3 cycles (6 weeks) using the Response Evaluation Criteria in Solid Tumors (RECIST) until radiological documentation of progression or for 13 months following the first dose of study drug(s), whichever came first. Confirmed responses were based on two tumor assessments separated by at least 4 weeks.
The demographics of the patient population entered into this study are shown in the table below.
Table 24 – Patient Demographics in Refractory and Relapsed Colorectal Cancer Clinical Trial
|
| 5-FU/LV
(N = 151) | Oxaliplatin
(N = 156) | Oxaliplatin +
5-FU/LV (N = 152) |
| Sex: Male (%) | 54.3
| 60.9
| 57.2
|
| Female (%) | 45.7
| 39.1
| 42.8
|
| Median age (years) | 60
| 61
| 59
|
| Range | 21-80
| 27-79
| 22-88
|
| Race (%)
|
|||
| Caucasian | 87.4
| 84.6
| 88.8
|
| Black | 7.9
| 7.1
| 5.9
|
| Asian | 1.3
| 2.6
| 2.6
|
| Other | 3.3
| 5.8
| 2.6
|
| KPS (%)
|
|||
| 70 – 100 | 94.7
| 92.3
| 95.4
|
| 50 – 60 | 2.6
| 4.5
| 2
|
| Not reported | 2.6
| 3.2
| 2.6
|
| Prior radiotherapy (%) | 25.2
| 19.2
| 25
|
| Prior pelvic radiation (%) | 18.5
| 13.5
| 21.1
|
| Number of metastatic sites (%)
|
|||
| 1 | 27.2
| 31.4
| 25.7
|
| ≥2 | 72.2
| 67.9
| 74.3
|
| Liver involvement (%)
|
|||
| Liver only | 22.5
| 25.6
| 18.4
|
| Liver + other | 60.3
| 59
| 53.3
|
The median number of cycles administered per patient was 6 for the oxaliplatin and 5-FU/LV combination and 3 each for 5-FU/LV alone and oxaliplatin alone.
Patients treated with the combination of oxaliplatin and 5-FU/LV had an increased response rate compared to patients given 5-FU/LV or oxaliplatin alone. The efficacy results are summarized in the tables below.
Table 25 - Response Rates (ITT Analysis)
| Best Response
| 5-FU/LV
(N=151) | Oxaliplatin
(N=156) | Oxaliplatin + 5-FU/LV
(N=152) |
| CR | 0
| 0
| 0
|
| PR | 0
| 2 (1%)
| 13 (9%)
|
| p-value | 0.0002 for 5-FU/LV vs. Oxaliplatin + 5 FU/LV
|
||
| 95%CI | 0-2.4%
| 0.2-4.6%
| 4.6-14.2%
|
Table 26 - Summary of Radiographic Time to Progression*
| Arm
| 5-FU/LV
(N=151) | Oxaliplatin
(N=156) | Oxaliplatin + 5-FU/LV
(N=152) |
| No. of Progressors | 74
| 101
| 50
|
| No. of patients with no
radiological evaluation beyond baseline |
22 (15%) |
16 (10%) |
17 (11%) |
| Median TTP (months) | 2.7
| 1.6
| 4.6
|
| 95% CI | 1.8-3
| 1.4-2.7
| 4.2-6.1
|
*This is not an ITT analysis. Events were limited to radiographic disease progression documented by independent review of radiographs. Clinical progression was not included in this analysis, and 18% of patients were excluded from the analysis based on unavailability of the radiographs for independent review.
At the time of the interim analysis 49% of the radiographic progression events had occurred. In this interim analysis an estimated 2-month increase in median time to radiographic progression was observed compared to 5-FU/LV alone.
Of the 13 patients who had tumor response to the combination of oxaliplatin and 5-FU/LV, 5 were female and 8 were male, and responders included patients <65 years old and ≥65 years old. The small number of non-Caucasian participants made efficacy analyses in these populations uninterpretable.
15 REFERENCES
- NIOSH Alert: Preventing occupational exposures to antineoplastic and other hazardous drugs in healthcare settings. 2004. U.S. Department of Health and Human Services, Public Health Service, Centers for Disease Control and Prevention, National Institute for Occupational Safety and Health, DHHS (NIOSH) Publication No. 2004-165.
- OSHA Technical Manual, TED 1-0.15A, Section VI: Chapter 2. Controlling Occupational Exposure to Hazardous Drugs. OSHA, 1999. http://www.osha.gov/dts/osta/otm/otm_vi/otm_vi_2.html
- American Society of Health-System Pharmacists. (2006) ASHP Guidelines on Handling Hazardous Drugs.
- Polovich, M., White, J. M., & Kelleher, L.O. (eds.) 2005. Chemotherapy and biotherapy guidelines and recommendations for practice (2nd. ed.) Pittsburgh, PA: Oncology Nursing Society.
16 HOW SUPPLIED/STORAGE AND HANDLING
16.1 How Supplied
Oxaliplatin for injection is available in single use vials containing 50 mg or 100 mg of oxaliplatin as a sterile, preservative-free lyophilized powder for reconstitution. Lactose monohydrate is also present as an inactive ingredient.
Product NDC
No. No.
107530 63323-175-30 Packaged individually.
107650 63323-176-50 Packaged individually.
16.2 Storage
Store under normal lighting conditions at 25°C (77°F); excursions permitted to 15º to 30°C (59º to 86°F) [see USP Controlled Room Temperature].
16.3 Handling and Disposal
As with other potentially toxic anticancer agents, care should be exercised in the handling and preparation of infusion solutions prepared from oxaliplatin for injection. The use of gloves is recommended. If a solution of oxaliplatin for injection contacts the skin, wash the skin immediately and thoroughly with soap and water. If oxaliplatin contacts the mucous membranes, flush thoroughly with water.
Procedures for the handling and disposal of anticancer drugs should be considered. Several guidelines on the subject have been published [see References (15)] . There is no general agreement that all of the procedures recommended in the guidelines are necessary or appropriate.
17 PATIENT COUNSELING INFORMATION
17.1 Information for Patients
Patients and patients’ caregivers should be informed of the expected side effects of oxaliplatin for injection, particularly its neurologic effects, both the acute, reversible effects and the persistent neurosensory toxicity. Patients should be informed that the acute neurosensory toxicity may be precipitated or exacerbated by exposure to cold or cold objects. Patients should be instructed to avoid cold drinks, use of ice, and should cover exposed skin prior to exposure to cold temperature or cold objects.
Patients must be adequately informed of the risk of low blood cell counts and instructed to contact their physician immediately should fever, particularly if associated with persistent diarrhea, or evidence of infection develop.
Patients should be instructed to contact their physician if persistent vomiting, diarrhea, signs of dehydration, cough or breathing difficulties occur, or signs of allergic reaction appear.
No studies on the effects on the ability to drive and use machines have been performed. However oxaliplatin treatment resulting in an increase risk of dizziness, nausea and vomiting, and other neurologic symptoms that affect gait and balance may lead to a minor or moderate influence on the ability to drive and use machines.
Vision abnormalities, in particular transient vision loss (reversible following therapy discontinuation), may affect patients' ability to drive and use machines. Therefore, patients should be warned of the potential effect of these events on the ability to drive or use machines.
17.2 FDA-Approved Patient Labeling
Patient Information
OXALIPLATIN
FOR INJECTION
powder, for solution for intravenous use
Read this information carefully before you start using oxaliplatin for injection. It will help you learn more about oxaliplatin for injection.
This information does not take the place of talking to your doctor about your medical condition or your treatment. Ask your doctor about any questions you have.
What is the most important information I should know about Oxaliplatin for Injection?
Oxaliplatin for Injection can cause serious allergic reactions.
In people who get severe allergic reactions while taking platinum medicines, death can occur.
Get emergency help right away if you:
- suddenly have trouble breathing.
- feel like your throat is closing up.
Call your doctor right away if you have any signs of allergic reaction:
- rash
- flushed face
- hives
- itching
- swelling of your lips or tongue
- sudden cough
- dizziness or feel faint
- sweating
- chest pain
If you have vision problems while taking oxaliplatin for injection
- do not drive, operate heavy machines, or engage in dangerous activities.
See “What are the possible side effects of Oxaliplatin for Injection” for information on other serious side effects.
What is Oxaliplatin for Injection?
Oxaliplatin for injection is an anti-cancer (chemotherapy) medicine that is used with other anti-cancer medicines called 5-fluorouracil (5-FU) and leucovorin (LV) to treat adults with:
- stage III colon cancer after surgery to remove the tumor
- advanced colon or rectal cancer (colo-rectal cancer).
Oxaliplatin for injection with infusional 5-FU and LV was shown to lower the chance of colon cancer returning when given to patients with stage III colon cancer after surgery to remove the tumor. Oxaliplatin for injection also increases survival in patients with stage III colon cancer. Oxaliplatin for injection with infusional 5-FU and LV was also shown to increase survival, shrink tumors and delay growth of tumors in some patients with advanced colorectal cancer.
It is not known if oxaliplatin for injection works in children.
Who should not use Oxaliplatin for Injection?
Do not use oxaliplatin for injection if you are allergic to any of the ingredients in oxaliplatin for injection or other medicines that contain platinum. Cisplatin (Platinol ®) and carboplatin (Paraplatin ®) are other chemotherapy medicines that also contain platinum. See the end of this leaflet for a list of the ingredients in oxaliplatin for injection.
What should I tell my doctor before treatment with Oxaliplatin for Injection?
Tell your doctor about all your medical conditions including, if you are:
- pregnant or planning to become pregnant. Oxaliplatin may harm your unborn child. You should avoid becoming pregnant while taking oxaliplatin for injection. Talk with your doctor about how to avoid pregnancy.
- breast feeding or plan to breast feed. We do not know if oxaliplatin for injection can pass through your milk and if it can harm your baby. You will need to decide whether to stop breast feeding or not to take oxaliplatin for injection.
Tell your doctor about all the medicines you take, including prescription and non-prescription medicines, vitamins, and herbal supplements. Oxaliplatin for injection may affect how other medicines work in your body.
Know the medicines you take. Keep a list of them and show it to your doctor and pharmacist when you get a new medicine.
How is Oxaliplatin for Injection given to me?
Oxaliplatin for injection is given to you through your veins (blood vessels).
- Your doctor will prescribe oxaliplatin for injection in an amount that is right for you.
- Your doctor will treat you with several medicines for your cancer.
- It is very important that you do exactly what your doctor and nurse have taught you to do.
- Some medicines may be given to you before oxaliplatin for injection to help prevent nausea and vomiting.
- Oxaliplatin for injection is given with 2 other chemotherapy medicines, leucovorin and 5-FU.
- Each treatment course is given to you over 2 days. You will receive oxaliplatin for injection on the first day only.
- There are usually 14 days between each chemotherapy treatment course.
Treatment Day 1:
Oxaliplatin for injection and leucovorin are given through a thin plastic tube put into a vein (intravenous infusion or I.V.) and given for 2 hours. You will be watched by a healthcare provider during this time.
Right after the oxaliplatin for injection and leucovorin are finished, 2 doses of 5-FU will be given. The first dose is given right away into your I.V. tube. The second dose will be given into your I.V. tube over the next 22 hours, using a pump device.
Treatment Day 2:
You will not get oxaliplatin for injection on Day 2. Leucovorin and 5-FU will be given the same way as on Day 1.
During your treatment with Oxaliplatinfor Injection:
- It is important for you to keep all appointments. Call your doctor if you must miss an appointment. There may be special instructions for you.
- Your doctor may change how often you get oxaliplatin for injection, how much you get, or how long the infusion will take.
- You and your doctor will discuss how many times you will get oxaliplatin for injection.
The 5-FU will be given through your I.V. with a pump. If you have any problems with the pump or the tube, call your doctor, your nurse, or the person who is responsible for your pump. Do not let anyone other than a healthcare provider touch your infusion pump or tubing.
What activities should I avoid while on treatment with Oxaliplatin for Injection?
- Avoid cold temperatures and cold objects. Cover your skin if you must go outside in cold temperatures.
- Do not drink cold drinks or use ice cubes in drinks.
- Do not put ice or ice packs on your body.
See the end of this leaflet (“How can I reduce the side effects caused by cold temperatures?”) for more information.
Talk with your doctor and nurse about your level of activity during treatment with oxaliplatin for injection. Follow their instructions.
What are the possible side effects of Oxaliplatinfor Injection?
Oxaliplatin for injection can cause serious side effects:
- Serious allergic reactions. See “What is the most important information I should know about oxaliplatin for injection?”
- Nerve problems (peripheral neuropathy). Oxaliplatin for injection can affect how your nerves work and make you feel. Tell your doctor right away if you get any signs of nerve problems listed below:
Very sensitive to cold temperatures and cold objects
Trouble breathing, swallowing, or saying words, jaw tightness, odd feelings in your tongue, or chest pressure
Pain, tingling, burning (pins and needles, numb feeling) in your hands, feet, or around your
mouth or throat, which may cause problems walking or performing activities of daily living.
The first signs of nerve problems may happen with the first treatment. The nerve problems can also start up to 2 days after treatment. If you develop nerve problems, the amount of oxaliplatin for injection in your next treatment may be changed or oxaliplatin for injection treatment may be stopped.
For information on ways to lessen or help with the nerve problems, see the end of this leaflet, “How can I reduce the side effects caused by cold temperatures?”
-
Lung problems (interstitial fibrosis). Tell your doctor if you get a dry cough and have trouble breathing (shortness of breath) before your next treatment. These may be signs of a serious lung disease.
-
Liver problems (hepatotoxicity).Your doctor will do blood tests to watch for this.
- Harm to an unborn baby. Oxaliplatin for injection may cause harm to your unborn baby. See “What should I tell my doctor before treatment with oxaliplatin for injection?”
Common side effects with oxaliplatin for injection include:
- decreased blood counts: oxaliplatin for injection can cause a decrease in neutrophils (a type of white blood cells important in fighting in bacterial infections), red blood cells (blood cells that carry oxygen to the tissues), and platelets (important for clotting and to control bleeding).
Call your doctor right away if you get any of the following signs of infection:
- Fever (temperature of 100.5ºF or greater)
- Chills or shivering
- Cough that brings up mucus
- Burning or pain on urination
- Pain on swallowing
- Sore throat
- Redness or swelling at intravenous site
- Tell your doctor about any bleeding or bruising.
- nausea
- vomiting
- diarrhea
- constipation
- mouth sores
- stomach pain
- decreased appetite
- tiredness
- eyesight (visual) problems including reversible short-term loss of vision. Tell your doctor about any eyesight changes
- injection site reactions. Reactions may include redness, swelling, pain, tissue damage
- hair loss (alopecia)
Call your doctor if you get any of the following:
- Vomiting that does not go away
- Frequent, loose, watery bowel movements (Diarrhea)
- Signs of dehydration (too much water loss)
o tiredness
o thirst
o dry mouth
o lightheadedness (dizziness)
o decreased urination
Tell your doctor if you have any side effect that bothers you or that does not go away. These are not all the possible side effects of oxaliplatin for injection. For more information, ask your doctor or pharmacist.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
How can I reduce the side effects caused by cold temperatures?
- Cover yourself with a blanket while you are getting your oxaliplatin for injection infusion.
- Do not breathe deeply when exposed to cold air.
- Wear warm clothing in cold weather at all times. Cover your mouth and nose with a scarf or a pull-down cap (ski cap) to warm the air that goes to your lungs.
- Wear gloves when taking things from the freezer or refrigerator.
- Drink fluids warm or at room temperature.
- Always drink through a straw.
- Do not use ice chips if you have nausea or mouth sores. Ask your nurse about what you can use.
- Be aware that most metals are cold to touch, especially in the winter. These include your car door and mailbox. Wear gloves to touch cold objects.
- Do not run the air-conditioning at high levels in the house or in the car in hot weather.
- If your body gets cold, warm-up the affected part. If your hands get cold, wash them with warm water.
- Always let your nurse and doctor know before your next treatment how well you did since your last visit.
This list is not complete and your healthcare provider may have other useful tips for helping you with these side effects.
General information about the safe and effective use of Oxaliplatin for Injection
Medicines are sometimes prescribed for conditions that are not mentioned in patient information leaflets.
This leaflet summarizes the most important information about oxaliplatin for injection. If you would like more information, talk with your doctor. You can ask your doctor or pharmacist for information about oxaliplatin for Injection that is written for health professionals.
What are the ingredients in Oxaliplatin for Injection?
Active ingredient: oxaliplatin
Inactive ingredients: lactose monohydrate
Manufactured for:

APP Pharmaceuticals, LLC
Schaumburg, IL 60173
Made in India
For Product Inquiry:
1-800-551-7176 or www.APPpharma.com
451177/Issued: July 2009
PACKAGE LABEL.PRINCIPAL DISPLAY PANEL - OXALIPLATIN 50 mg Single Use Vial Carton Label
NDC 63323-175-30
107530
OXALIPLATIN
FOR INJECTION
50 mg
FOR INTRAVENOUS USE ONLY
SINGLE USE VIAL
Sterile Lyophilized Powder-Preservative Free
Must be reconstituted and diluted before use.
DO NOT RECONSTITUTE WITH SODIUM CHLORIDE/CHLORIDE-CONTAINING SOLUTIONS
Rx only

PACKAGE LABEL.PRINCIPAL DISPLAY PANEL - OXALIPLATIN 50 mg Single Use Vial Label
NDC 63323-175-30
107530
OXALIPLATIN
FOR INJECTION
50 mg
FOR INTRAVENOUS USE ONLY
SINGLE USE VIAL
Sterile Lyophilized Powder-Preservative Free
Must be reconstituted and diluted before use.
DO NOT RECONSTITUTE WITH SODIUM CHLORIDE/CHLORIDE-CONTAINING SOLUTIONS
Rx only

PACKAGE LABEL.PRINCIPAL DISPLAY PANEL - OXALIPLATIN 100 mg Single Use Vial Carton Label
NDC 66323-176-50
107650
OXALIPLATIN
FOR INJECTION
100 mg
FOR INTRAVENOUS USE ONLY
SINGLE USE VIAL
Sterile Lyophilized Powder-Preservative Free
Must be reconstituted and diluted before use.
DO NOT RECONSTITUTE WITH SODIUM CHLORIDE/CHLORIDE-CONTAINING SOLUTIONS
Rx only

PACKAGE LABEL.PRINCIPAL DISPLAY PANEL - OXALIPLATIN 100 mg Single Use Vial Label
NDC 63323-176-50
107650
OXALIPLATIN
FOR INJECTION
100 mg
FOR INTRAVENOUS USE ONLY
SINGLE USE VIAL
Sterile Lyophilized Powder-Preservative Free
Must be reconstituted and diluted before use.
DO NOT RECONSTITUTE WITH SODIUM CHLORIDE/CHLORIDE-CONTAINING SOLUTIONS
Rx only

| OXALIPLATIN
oxaliplatin injection, powder, lyophilized, for solution |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| OXALIPLATIN
oxaliplatin injection, powder, lyophilized, for solution |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| Labeler - Fresenius Kabi USA, LLC (608775388) |
| Establishment | |||
| Name | Address | ID/FEI | Business Operations |
|---|---|---|---|
| Cipla Ltd. | 650072015 | manufacture(63323-175, 63323-176) | |