POMALIDOMIDE- pomalidomide capsule
Pomalidomide by
Drug Labeling and Warnings
Pomalidomide by is a Prescription medication manufactured, distributed, or labeled by Camber Pharmaceuticals, Inc., Hetero Labs Limited Unit V. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
-
HIGHLIGHTS OF PRESCRIBING INFORMATION
These highlights do not include all the information needed to use POMALIDOMIDE CAPSULES safely and effectively. See full prescribing information for POMALIDOMIDE CAPSULES.
POMALIDOMIDE capsules, for oral use
Initial U.S. Approval: 2013See full prescribing information for complete boxed warning
EMBRYO-FETAL TOXICITY
Pomalidomide is contraindicated in pregnancy. Pomalidomide is a thalidomide analogue. Thalidomide is a known human teratogen that causes severe life-threatening birth defects ( 4, 5.1, 8.1).
For females of reproductive potential: Exclude pregnancy before start of treatment. Prevent pregnancy during treatment by the use of 2 reliable methods of contraception ( 5.1, 8.3).
Pomalidomide is available only through a restricted program called PS-Pomalidomide REMS ( 5.2).
VENOUS AND ARTERIAL THROMBOEMBOLISM
Deep venous thrombosis (DVT), pulmonary embolism (PE), myocardial infarction, and stroke occur in patients with multiple myeloma treated with pomalidomide. Antithrombotic prophylaxis is recommended ( 5.3).
INDICATIONS AND USAGE
Pomalidomide is a thalidomide analogue indicated for the treatment of adult patients:
in combination with dexamethasone, for patients with multiple myeloma (MM) who have received at least two prior therapies including lenalidomide and a proteasome inhibitor and have demonstrated disease progression on or within 60 days of completion of the last therapy ( 1.1).
DOSAGE AND ADMINISTRATION
WARNINGS AND PRECAUTIONS
Increased Mortality: Observed in patients with MM when pembrolizumab was added to dexamethasone and a thalidomide analogue ( 5.4).
Hematologic Toxicity: Neutropenia was the most frequently reported Grade 3/4 adverse event. Monitor patients for hematologic toxicities, especially neutropenia ( 5.5).
Hepatotoxicity: Hepatic failure including fatalities; monitor liver function tests monthly ( 5.6).
Severe Cutaneous Reactions: Discontinue pomalidomide for severe reactions ( 5.7).
Tumor Lysis Syndrome (TLS): Monitor patients at risk of TLS (i.e., those with high tumor burden) and take appropriate precautions ( 5.11).
Hypersensitivity: Monitor patients for potential hypersensitivity. Discontinue pomalidomide for angioedema and anaphylaxis ( 5.12).ADVERSE REACTIONS
MM: Most common adverse reactions (≥30%) included fatigue and asthenia, neutropenia, anemia, constipation, nausea, diarrhea, dyspnea, upper-respiratory tract infections, back pain, and pyrexia ( 6.1).
To report SUSPECTED ADVERSE REACTIONS, contact Hetero Labs Limited at 1-866-495-1995 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.DRUG INTERACTIONS
USE IN SPECIFIC POPULATIONS
Lactation: Advise women not to breastfeed ( 8.2).
See 17 for PATIENT COUNSELING INFORMATION and Medication Guide.
Revised: 11/2025
-
Table of Contents
FULL PRESCRIBING INFORMATION: CONTENTS*
WARNING: EMBRYO-FETAL TOXICITY and VENOUS AND ARTERIAL THROMBOEMBOLISM
1 INDICATIONS AND USAGE
1.1 Multiple Myeloma
2 DOSAGE AND ADMINISTRATION
2.1 Pregnancy Testing Prior to Administration
2.2 Recommended Dosage for Multiple Myeloma
2.4 Dosage Modifications for Hematologic Adverse Reactions
2.5 Dosage Modifications for Non-Hematologic Adverse Reactions
2.6 Dosage Modifications for Strong CYP1A2 Inhibitors
2.7 Dosage Modification for Severe Renal Impairment on Hemodialysis
2.8 Dosage Modification for Hepatic Impairment
2.9 Administration
3 DOSAGE FORMS AND STRENGTHS
4 CONTRAINDICATIONS
4.1 Pregnancy
4.2 Hypersensitivity
5 WARNINGS AND PRECAUTIONS
5.1 Embryo-Fetal Toxicity
5.2 PS-Pomalidomide REMS
5.3 Venous and Arterial Thromboembolism
5.4 Increased Mortality in Patients with Multiple Myeloma When Pembrolizumab Is Added to a Thalidomide Analogue and Dexamethasone
5.5 Hematologic Toxicity
5.6 Hepatotoxicity
5.7 Severe Cutaneous Reactions
5.8 Dizziness and Confusional State
5.9 Neuropathy
5.10 Risk of Second Primary Malignancies
5.11 Tumor Lysis Syndrome
5.12 Hypersensitivity
6 ADVERSE REACTIONS
6.1 Clinical Trials Experience
6.2 Postmarketing Experience
7 DRUG INTERACTIONS
7.1 Drugs That Affect Pomalidomide Plasma Concentrations
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
8.2 Lactation
8.3 Females and Males of Reproductive Potential
8.4 Pediatric Use
8.5 Geriatric Use
8.6 Renal Impairment
8.7 Hepatic Impairment
8.8 Smoking Tobacco
10 OVERDOSAGE
11 DESCRIPTION
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
12.2 Pharmacodynamics
12.3 Pharmacokinetics
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
14 CLINICAL STUDIES
14.1 Multiple Myeloma
15 REFERENCES
16 HOW SUPPLIED/STORAGE AND HANDLING
17 PATIENT COUNSELING INFORMATION
- * Sections or subsections omitted from the full prescribing information are not listed.
-
BOXED WARNING
(What is this?)
WARNING: EMBRYO-FETAL TOXICITY and VENOUS AND ARTERIAL THROMBOEMBOLISM
WARNING: EMBRYO-FETAL TOXICITY and VENOUS AND ARTERIAL THROMBOEMBOLISM
Embryo-Fetal Toxicity
Pomalidomideis contraindicated in pregnancy. Pomalidomide is a thalidomide analogue. Thalidomide is a known human teratogen that causes severe birth defects or embryo-fetal death. In females of reproductive potential, obtain 2 negative pregnancy tests before starting pomalidomide treatment.
Females of reproductive potential must use 2 forms of contraception or continuously abstain from heterosexual sex during and for 4 weeks after stopping pomalidomide treatment [see Contraindications (4),Warnings and Precautions (5.1)and Use in Specific Populations (8.1, 8.3)].
Pomalidomide is only available through a restricted distribution program called PS-Pomalidomide REMS [see Warnings and Precautions (5.2)] . Information about PS-Pomalidomide REMS is available at www.PS-PomalidomideREMS.com or by calling the REMS Call Center at 1-888-423-5436.
Venous and Arterial Thromboembolism
Deep venous thrombosis (DVT), pulmonary embolism (PE), myocardial infarction, and stroke occur in patients with multiple myeloma treated with pomalidomide. Prophylactic antithrombotic measures were employed in clinical trials. Thromboprophylaxis is recommended, and the choice of regimen should be based on assessment of the patient's underlying risk factors [see Warnings and Precautions (5.3)]. -
1 INDICATIONS AND USAGE
1.1 Multiple Myeloma
Pomalidomide capsules, in combination with dexamethasone, is indicated for adult patients with multiple myeloma (MM) who have received at least two prior therapies including lenalidomide and a proteasome inhibitor and have demonstrated disease progression on or within 60 days of completion of the last therapy.
-
2 DOSAGE AND ADMINISTRATION
2.1 Pregnancy Testing Prior to Administration
Females of reproductive potential must have negative pregnancy testing and use contraception methods before initiating pomalidomide capsules [see Warnings and Precautions (5.1)and Use in Specific Populations (8.1, 8.3)].
2.2 Recommended Dosage for Multiple Myeloma
The recommended dosage of pomalidomide capsules is 4 mg once daily orally with or without food on Days 1 through 21 of each 28-day cycle until disease progression. Give pomalidomide capsules in combination with dexamethasone [see Clinical Studies (14.1)].
2.4 Dosage Modifications for Hematologic Adverse Reactions
Multiple Myeloma: Dosage Modifications for Hematologic Adverse Reactions
Initiate a new cycle of pomalidomide capsules in patients with multiple myeloma (MM) when the neutrophil count is at least 500 per mcL and the platelet count is at least 50,000 per mcL.
Dosage modification for pomalidomide capsules for hematologic adverse reactions in patients with MM are summarized in Table 1.
Table 1: Dosage Modifications for Pomalidomide Capsules for Hematologic in MM
Adverse Reaction
Severity
Dosage Modification
Neutropenia [see Warnings and Precautions (5.5)]
- ANC less than 500 per mcL or febrile neutropenia (fever greater than or equal to 38.5°C and ANC less than 1,000 per mcL)
- Withhold pomalidomide capsules until ANC is greater than or equal to 500 per mcL; follow CBC weekly.
- Resume pomalidomide capsules dose at 1 mg less than the previous dose.*
- For each subsequent drop of ANC less than 500 per mcL
- Withhold pomalidomide capsules until ANC is greater than or equal to 500 mcL.
- Resume pomalidomide capsules dose at 1 mg less than the previous dose.*
Thrombocytopenia [see Warnings and Precautions (5.5)]
- Platelets less than 25,000 per mcL
- Withhold pomalidomide capsules until platelets are greater than or equal to 50,000 per mcL; follow CBC weekly.
- Resume pomalidomide capsules dose at 1 mg less than the previous dose.*
- For each subsequent drop of platelets less than 25,000 per mcL
- Withhold pomalidomide capsules until platelets are greater than or equal to 50,000 per mcL.
- Resume pomalidomide capsules at 1 mg less than the previous dose.*
* Permanently discontinue pomalidomide capsules if unable to tolerate 1 mg once daily.
ANC= absolute neutrophil count2.5 Dosage Modifications for Non-Hematologic Adverse Reactions
Permanently discontinue pomalidomide capsules for angioedema, anaphylaxis, Grade 4 rash, skin exfoliation, bullae, or any other severe dermatologic reaction [See Warnings and Precautions (5.7, 5.12)].
For other Grade 3 or 4 toxicities, hold treatment and restart treatment at 1 mg less than the previous dose when toxicity has resolved to less than or equal to Grade 2 at the physician’s discretion.
2.6 Dosage Modifications for Strong CYP1A2 Inhibitors
Avoid concomitant use of pomalidomide capsules with strong CYP1A2 inhibitors. If concomitant use of a strong CYP1A2 inhibitor is unavoidable, reduce pomalidomide capsules dose to 2 mg [see Drug Interactions (7.1) and Clinical Pharmacology (12.3)].
2.7 Dosage Modification for Severe Renal Impairment on Hemodialysis
Take pomalidomide capsules after completion of dialysis procedure on hemodialysis days [see Use in Specific Populations (8.6) and Clinical Pharmacology (12.3)].
For patients with MM with severe renal impairment requiring dialysis, reduce the recommended dosage to 3 mg orally daily.2.8 Dosage Modification for Hepatic Impairment
Multiple Myeloma
For patients with MM with mild or moderate hepatic impairment (Child-Pugh A or B), reduce the recommended dosage to 3 mg orally daily.
For patients with MM with severe hepatic impairment (Child-Pugh C), reduce the recommended dosage to 2 mg [see Use in Specific Populations (8.7) and Clinical Pharmacology (12.3)]. -
3 DOSAGE FORMS AND STRENGTHS
Pomalidomide capsules are available in the following capsule strengths:
1 mg: Opaque, white cap and opaque white body, hard gelatin capsules imprinted with 'H' on cap and 'P1' on body, filled with pale yellow to yellowish color powder.
2 mg: Opaque, white cap and opaque brown body, hard gelatin capsules imprinted with 'H' on cap and 'P2' on body, filled with pale yellow to yellowish color powder.
3 mg: Opaque, white cap and opaque pink body, hard gelatin capsules imprinted with 'H' on cap and 'P3' on body, filled with pale yellow to yellowish color powder.
4 mg: Opaque, white cap and opaque white body, hard gelatin capsules imprinted with 'H' on cap and 'P4' on body, filled with pale yellow to yellowish color powder. -
4 CONTRAINDICATIONS
4.1 Pregnancy
Pomalidomide is contraindicated in females who are pregnant. Pomalidomide can cause fetal harm when administered to a pregnant female [see Warnings and Precautions (5.1)and Use in Specific Populations (8.1)] . Pomalidomide is a thalidomide analogue and is teratogenic in both rats and rabbits when administered during the period of organogenesis. If the patient becomes pregnant while taking this drug, the patient should be apprised of the potential risk to a fetus.
4.2 Hypersensitivity
Pomalidomide is contraindicated in patients who have demonstrated severe hypersensitivity (e.g., angioedema, anaphylaxis) to pomalidomide or any of the excipients [see Warnings and Precautions (5.7), Description (11)].
-
5 WARNINGS AND PRECAUTIONS
5.1 Embryo-Fetal Toxicity
Pomalidomide is a thalidomide analogue and is contraindicated for use during pregnancy. Thalidomide is a known human teratogen that causes severe birth defects or embryo-fetal death [see Use in Specific Populations ( 8.1)]. Pomalidomide is only available through the PS-Pomalidomide REMS program [see Warnings and Precautions ( 5.2)].
Females of Reproductive Potential
Females of reproductive potential must avoid pregnancy for at least 4weeksbefore beginning pomalidomide therapy, during therapy, during dose interruptions and for at least 4 weeks after completing therapy.
Females must commit either to abstain continuously from heterosexual sexual intercourse or to use 2 methods of reliable birth control, beginning 4 weeks prior to initiating treatment with pomalidomide, during therapy, during dose interruptions, and continuing for 4 weeks following discontinuation of pomalidomide therapy.
Two negative pregnancy tests must be obtained prior to initiating therapy. The first test should be performed within 10 to 14 days and the second test within 24 hours prior to prescribing pomalidomide therapy and then weekly during the first month, then monthly thereafter in females with regular menstrual cycles, or every 2 weeks in females with irregular menstrual cycles [see Use in Specific Populations ( 8.3)].
Males
Pomalidomide is present in the semen of patients receiving the drug. Therefore, males must always use a latex or synthetic condom during any sexual contact with females of reproductive potential while taking pomalidomide and for up to 4 weeks after discontinuing pomalidomide, even if they have undergone a successful vasectomy. Male patients taking pomalidomide must not donate sperm [see Use in Specific Populations ( 8.3)].Blood Donation
Patients must not donate blood during treatment with pomalidomide and for 4 weeks following discontinuation of the drug because the blood might be given to a pregnant female patient whose fetus must not be exposed to pomalidomide.5.2 PS-Pomalidomide REMS
Because of the embryo-fetal risk [see Warnings and Precautions (5.1)] , pomalidomide is available only through a restricted program under a Risk Evaluationand Mitigation Strategy (REMS), “PS-Pomalidomide REMS”.
Required componentsof PS-Pomalidomide REMSinclude the following:
Prescribers must be certified with PS-Pomalidomide REMSby enrolling and complying with the REMS requirements.
Patients must signaPatient-Physician Agreement Form and comply with the REMS requirements. In particular, female patients of reproductive potential who are not pregnant must comply with the pregnancy testing and contraception requirements [see Use in Specific Populations (8.3)] and males must comply with contraception requirements [see Use in Specific Populations (8.3)].
Pharmacies mustbe certified with PS-Pomalidomide REMS, must only dispense to patients who are authorized to receive pomalidomide and comply with REMS requirements.
Further information about PS-Pomalidomide REMSis availableat www.PS-PomalidomideREMS.com or by telephone at 1-888-423-5436.5.3 Venous and Arterial Thromboembolism
Venous thromboembolic events (deep venous thrombosis and pulmonary embolism) and arterial thromboembolic events (myocardial infarction and stroke) have been observed in patients treated with pomalidomide. In Trial 2, where anticoagulant therapies were mandated, thromboembolic events occurred in 8.0% of patients treated with pomalidomide and low dose-dexamethasone (Low-dose Dex), and 3.3% of patients treated with high-dose dexamethasone. Venous thromboembolic events (VTE) occurred in 4.7% of patients treated with pomalidomide and Low-dose Dex, and 1.3% of patients treated with high-dose dexamethasone. Arterial thromboembolic events include terms for arterial thromboembolic events, ischemic cerebrovascular conditions, and ischemic heart disease. Arterial thromboembolic events occurred in 3.0% of patients treated with pomalidomide and Low-dose Dex, and 1.3% of patients treated with high-dose dexamethasone.
Patients with known risk factors, including prior thrombosis, may be at greater risk, and actions should be taken to try to minimize all modifiable factors (e.g., hyperlipidemia, hypertension, smoking). Thromboprophylaxis is recommended, and the choice of regimen should be based on assessment of the patient's underlying risk factors.
5.4 Increased Mortality in Patients with Multiple Myeloma When Pembrolizumab Is Added to a Thalidomide Analogue and Dexamethasone
In two randomized clinical trials in patients with MM, the addition of pembrolizumab to a thalidomide analogue plus dexamethasone, a use for which no PD-1 or PD-L1 blocking antibody is indicated, resulted in increased mortality. Treatment of patients with MM with a PD-1 or PD-L1 blocking antibody in combination with a thalidomide analogue plus dexamethasone is not recommended outside of controlled clinical trials.
5.5 Hematologic Toxicity
Multiple Myeloma
In trials 1 and 2 in patients who received pomalidomide + Low-dose Dex, neutropenia was the most frequently reported Grade 3 or 4 adverse reaction, followed by anemia and thrombocytopenia. Neutropenia of any grade was reported in 51% of patients in both trials. The rate of Grade 3 or 4 neutropenia was 46%. The rate of febrile neutropenia was 8%.
Monitor patients for hematologic toxicities, especially neutropenia. Monitor complete blood counts weekly for the first 8 weeks and monthly thereafter. Patients may require dose interruption and/or modification [see Dosage and Administration (2.4)].5.6 Hepatotoxicity
Hepatic failure, including fatal cases, has occurred in patients treated with pomalidomide. Elevated levels of alanine aminotransferase and bilirubin have also been observed in patients treated with pomalidomide. Monitor liver function tests monthly. Stop pomalidomide upon elevation of liver enzymes and evaluate. After return to baseline values, treatment at a lower dose may be considered.
5.7 Severe Cutaneous Reactions
Severe cutaneous reactions including Stevens-Johnson syndrome (SJS), toxic epidermal necrolysis (TEN), and drug reaction with eosinophilia and systemic symptoms (DRESS) have been reported. DRESS may present with a cutaneous reaction (such as rash or exfoliative dermatitis), eosinophilia, fever, and/or lymphadenopathy with systemic complications such as hepatitis, nephritis, pneumonitis, myocarditis, and/or pericarditis. These reactions can be fatal. Consider pomalidomide interruption or discontinuation for Grade 2 or 3 skin rash. Permanently discontinue pomalidomide for Grade 4 rash, exfoliative or bullous rash, or for other severe cutaneous reactions such as SJS, TEN or DRESS [see Dosage and Administration (2.5)].
5.8 Dizziness and Confusional State
In trials 1 and 2 in patients who received pomalidomide + Low-dose Dex, 14% of patients experienced dizziness and 7% of patients experienced a confusional state; 1% of patients experienced Grade 3 or 4 dizziness, and 3% of patients experienced Grade 3 or 4 confusional state. Instruct patients to avoid situations where dizziness or confusional state may be a problem and not to take other medications that may cause dizziness or confusional state without adequate medical advice.
5.9 Neuropathy
In trials 1 and 2 in patients who received pomalidomide + Low-dose Dex, 18% of patients experienced neuropathy, with approximately 12% of the patients experiencing peripheral neuropathy. Two percent of patients experienced Grade 3 neuropathy in trial 2. There were no cases of Grade 4 neuropathy adverse reactions reported in either trial.
5.10 Risk of Second Primary Malignancies
Cases of acute myelogenous leukemia have been reported in patients receiving pomalidomide as an investigational therapy outside of MM.
5.11 Tumor Lysis Syndrome
Tumor lysis syndrome (TLS) may occur in patients treated with pomalidomide. Patients at risk for TLS are those with high tumor burden prior to treatment. These patients should be monitored closely and appropriate precautions taken.
5.12 Hypersensitivity
Hypersensitivity, including angioedema, anaphylaxis, and anaphylactic reactions to pomalidomide have been reported. Permanently discontinue pomalidomide for angioedema or anaphylaxis [see Dosage and Administration (2.5)].
-
6 ADVERSE REACTIONS
The following clinically significant adverse reactions are described in detail in other labeling sections:
Embryo-Fetal Toxicity [see Warnings and Precautions (5.1, 5.2)]
Venous and Arterial Thromboembolism [see Warnings and Precautions ( 5.3)]
Increased Mortality in Patients with Multiple Myeloma When Pembrolizumab Is Added to a Thalidomide Analogue and Dexamethasone [see Warnings and Precautions ( 5.4)]
Hematologic Toxicity [see Warnings and Precautions ( 5.5)]
Hepatotoxicity [see Warnings and Precautions ( 5.6)]
Severe Cutaneous Reactions [see Warnings and Precautions ( 5.7)]
Dizziness and Confusional State [see Warnings and Precautions ( 5.8)]
Neuropathy [see Warnings and Precautions ( 5.9)]
Risk of Second Primary Malignancies [see Warnings and Precautions ( 5.10)]
Tumor Lysis Syndrome [see Warnings and Precautions ( 5.11)]Hypersensitivity [see Warnings and Precautions (5.12)]
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Multiple Myeloma (MM)
In Trial 1, data were evaluated from 219 patients (safety population) who received treatment with pomalidomide + Low-dose Dex (112 patients) or pomalidomide alone (107 patients). Median number of treatment cycles was 5. Sixty-seven percent of patients in the study had a dose interruption of either drug due to adverse reactions. Forty-two percent of patients in the study had a dose reduction of either drug due to adverse reactions. The discontinuation rate due to adverse reactions was 11%.
In Trial 2, data were evaluated from 450 patients (safety population) who received treatment with pomalidomide + Low-dose Dex (300 patients) or High-dose Dexamethasone (High-dose Dex) (150 patients). The median number of treatment cycles for the pomalidomide + Low-dose Dex arm was 5. In the pomalidomide + Low-dose Dex arm, 67% of patients had a dose interruption of pomalidomide, the median time to the first dose interruption of pomalidomide was 4.1 weeks. Twenty-seven percent of patients had a dose reduction of pomalidomide, the median time to the first dose reduction of pomalidomide was 4.5 weeks. Eight percent of patients discontinued pomalidomide due to adverse reactions.
Tables 3 and 4 summarize the adverse reactions reported in Trials 1 and 2, respectively.
Table 3: Adverse Reactions in Any Pomalidomide Treatment Arm in Trial 1*
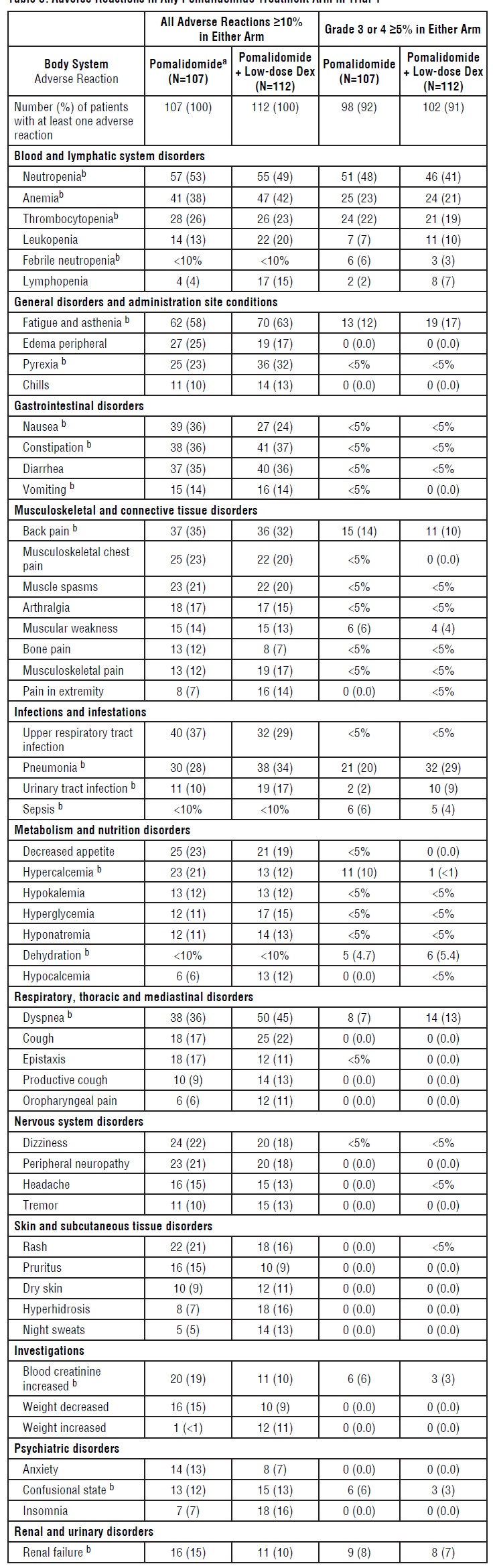
*Regardless of attribution of relatedness to pomalidomide.
aPomalidomide alone arm includes all patients randomized to the pomalidomide alone arm who took study drug; 61 of the 107 patients had dexamethasone added during the treatment period.
bSerious adverse reactions were reported in at least 2 patients in any pomalidomide treatment arm.
Data cutoff: 01 March 2013
Table 4: Adverse Reactions in Trial 2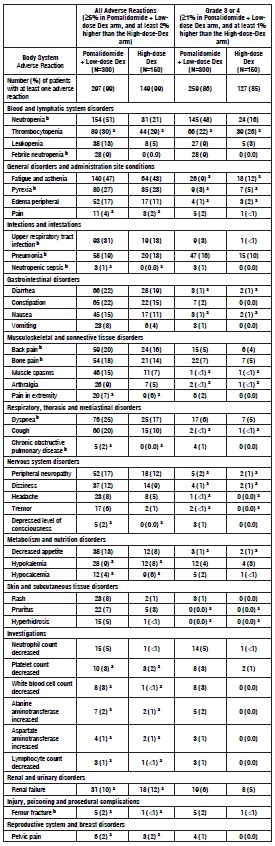
aPercentage did not meet the criteria to be considered as an adverse reaction for pomalidomide for that category of event (i.e., all adverse events or Grade 3 or 4 adverse events).
bSerious adverse reactions were reported in at least 3 patients in the POM + Low-dose Dex arm, AND at least 1% higher than the High-dose-Dex arm percentage.
Data cutoff: 01 March 2013
Other Adverse Reactions
Other adverse reactions of pomalidomide in patients with MM, not described above, and considered important:
Cardiac Disorders:Myocardial infarction, Atrial fibrillation, Angina pectoris, Cardiac failure congestive
Ear and Labyrinth Disorders: Vertigo
Gastrointestinal disorders: Abdominal pain
General Disorders and Administration Site Conditions:General physical health deterioration, Non-cardiac chest pain, Multi-organ failure
Hepatobiliary Disorders:Hyperbilirubinemia
Infections and Infestations: Pneumocystis jiroveci pneumonia, Respiratory syncytial virus infection, Neutropenic sepsis, Bacteremia, Pneumonia respiratory syncytial viral, Cellulitis, Urosepsis, Septic shock, Clostridium difficile colitis, Pneumonia streptococcal, Lobar pneumonia, Viral infection, Lung infection
Investigations:Alanine aminotransferase increased, Hemoglobin decreased
Injury, poisoning and procedural complications:Fall, Compression fracture, Spinal compression fracture
Metabolism and nutritional disorders:Hyperkalemia, Failure to thrive
Nervous system disorders:Depressed level of consciousness, Syncope
Psychiatric disorders:Mental status change
Renal and urinary disorders:Urinary retention, Hyponatremia
Reproductive system and breast disorders:Pelvic pain
Respiratory, thoracic, and mediastinal disorders: Interstitial lung disease, Pulmonary embolism, Respiratory failure, Bronchospasm
Vascular disorders:Hypotension6.2 Postmarketing Experience
The following adverse reactions have been identified during postapproval use of pomalidomide. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Blood and Lymphatic System Disorders:Pancytopenia
Endocrine Disorders:Hypothyroidism, hyperthyroidism
Gastrointestinal Disorders:Gastrointestinal hemorrhage
Hepatobiliary Disorders:Hepatic failure (including fatal cases), elevated liver enzymes
Immune system Disorders:Allergic reactions (e.g., angioedema, anaphylaxis, urticaria), solid organ transplant rejection
Infections and Infestations:Hepatitis B virus reactivation, Herpes zoster, progressive multifocal leukoencephalopathy (PML)
Neoplasms benign, malignant and unspecified (incl cysts and polyps):Tumor lysis syndrome, basal cell carcinoma, and squamous cell carcinoma of the skin
Skin and Subcutaneous Tissue Disorders:Stevens-Johnson Syndrome, toxic epidermal necrolysis, drug reaction with eosinophilia and systemic symptoms (DRESS)
-
7 DRUG INTERACTIONS
7.1 Drugs That Affect Pomalidomide Plasma Concentrations
CYP1A2 inhibitors:
In healthy subjects, co-administration of fluvoxamine, a strong CYP1A2 inhibitor, increased C maxand AUC of pomalidomide by 24% and 125% respectively [see Clinical Pharmacology (12.3)]. Increased pomalidomide exposure may increase the risk of exposure related toxicities. Avoid co-administration of strong CYP1A2 inhibitors (e.g. ciprofloxacin and fluvoxamine). If co-administration is unavoidable, reduce the pomalidomide dose [see Dosage and Administration (2.6)]. -
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Pregnancy Exposure Registry
There is a pregnancy exposure registry that monitors pregnancy outcomes in females exposed to pomalidomide during pregnancy as well as female partners of male patients who are exposed to pomalidomide. This registry is also used to understand the root cause for the pregnancy. Report any suspected fetal exposure to pomalidomide to the FDA via the MedWatch program at 1-800-FDA-1088 and also to the REMS Call Center at 1-888-423-5436.
Risk Summary
Based on the mechanism of action [see Clinical Pharmacology (12.1)] and findings from animal studies, pomalidomide can cause embryo-fetal harm when administered to a pregnant female and is contraindicated during pregnancy [ see Contraindications (4), and Warnings and Precautions (5.1)].
Pomalidomide is a thalidomide analogue. Thalidomide is a human teratogen, inducing a high frequency of severe and life-threatening birth defects such as amelia (absence of limbs), phocomelia (short limbs), hypoplasticity of the bones, absence of bones, external ear abnormalities (including anotia, micropinna, small or absent external auditory canals), facial palsy, eye abnormalities (anophthalmos, microphthalmos), and congenital heart defects. Alimentary tract, urinary tract, and genital malformations have also been documented, and mortality at or shortly after birth has been reported in about 40% of infants.
Pomalidomide was teratogenic in both rats and rabbits when administered during the period of organogenesis. Pomalidomide crossed the placenta after administration to pregnant rabbits (see Data). If this drug is used during pregnancy or if the patient becomes pregnant while taking this drug, the patient should be apprised of the potential risk to a fetus.
If pregnancy does occur during treatment, immediately discontinue the drug. Under these conditions, refer patient to an obstetrician/gynecologist experienced in reproductive toxicity for further evaluation and counseling. Report any suspected fetal exposure to pomalidomide to the FDA via the MedWatch program at 1-800-FDA-1088 and also to the REMS Call Center at 1-888-423-5436.
The estimated background risk of major birth defects and miscarriage for the indicated population is unknown. The estimated background risk in the U.S. general population of major birth defects is 2% to 4% and of miscarriage is 15% to 20% of clinically recognized pregnancies.
Data
Animal Data
Pomalidomide was teratogenic in both rats and rabbits in the embryo-fetal developmental studies when administered during the period of organogenesis.
In rats, pomalidomide was administered orally to pregnant animals at doses of 25 to 1000 mg/kg/day. Malformations or absence of urinary bladder, absence of thyroid gland, and fusion and misalignment of lumbar and thoracic vertebral elements (vertebral, central, and/or neural arches) were observed at all dose levels. There was no maternal toxicity observed in this study. The lowest dose in rats resulted in an exposure (AUC) approximately 85-fold of the human exposure at the recommended dose of 4 mg/day. Other embryo-fetal toxicities included increased resorptions leading to decreased number of viable fetuses.
In rabbits, pomalidomide was administered orally to pregnant animals at doses of 10 to 250 mg/kg/day. Increased cardiac malformations such as interventricular septal defect were seen at all doses with significant increases at 250 mg/kg/day. Additional malformations observed at 250 mg/kg/day included anomalies in limbs (flexed and/or rotated fore - and/or hindlimbs, unattached or absent digit) and associated skeletal malformations (not ossified metacarpal, misaligned phalanx and metacarpal, absent digit, not ossified phalanx, and short not ossified or bent tibia), moderate dilation of the lateral ventricle in the brain, abnormal placement of the right subclavian artery, absent intermediate lobe in the lungs, low-set kidney, altered liver morphology, incompletely or not ossified pelvis, an increased average for supernumerary thoracic ribs, and a reduced average for ossified tarsals. No maternal toxicity was observed at the low dose (10 mg/kg/day) that resulted in cardiac anomalies in fetuses; this dose resulted in an exposure (AUC) approximately equal to that reported in humans at the recommended dose of 4 mg/day. Additional embryo-fetal toxicity included increased resorption.
Following daily oral administration of pomalidomide from Gestation Day 7 through Gestation Day 20 in pregnant rabbits, fetal plasma pomalidomide concentrations were approximately 50% of the maternal Cmax at all dosages (5 to 250 mg/kg/day), indicating that pomalidomide crossed the placenta.8.2 Lactation
Risk Summary
There is no information regarding the presence of pomalidomide in human milk, the effects of pomalidomide on the breastfed child, or the effects of pomalidomide on milk production. Pomalidomide was excreted in the milk of lactating rats ( see Data).Because many drugs are excreted in human milk and because of the potential for adverse reactions in a breastfed child from pomalidomide, advise women not to breastfeed during treatment with pomalidomide.
Data
Animal Data
Following a single oral administration of pomalidomide to lactating rats approximately 14 days postpartum, pomalidomide was transferred into milk, with milk to plasma ratios of 0.63 to 1.46.8.3 Females and Males of Reproductive Potential
Pregnancy Testing
Pomalidomide can cause fetal harm when administered during pregnancy [see Use in Specific Populations (8.1)]. Verify the pregnancy status of females of reproductive potential prior to initiating pomalidomide therapy and during therapy. Advise females of reproductive potential that they must avoid pregnancy 4 weeks before therapy, while taking pomalidomide, during dose interruptions and for at least 4 weeks after completing therapy.
Females of reproductive potential must have 2 negative pregnancy tests before initiating pomalidomide. The first test should be performed within 10 to 14 days, and the second test within 24 hours prior to prescribing pomalidomide. Once treatment has started and during dose interruptions, pregnancy testing for females of reproductive potential should occur weekly during the first 4 weeks of use, then pregnancy testing should be repeated every 4 weeks in females with regular menstrual cycles. If menstrual cycles are irregular, the pregnancy testing should occur every 2 weeks. Pregnancy testing and counseling should be performed if a patient misses her period or if there is any abnormality in her menstrual bleeding. Pomalidomide treatment must be discontinued during this evaluation.
Contraception
Females
Females of reproductive potential must commit either to abstain continuously from heterosexual sexual intercourse or to use 2 methods of reliable birth control simultaneously: one highly effective form of contraception – tubal ligation, IUD, hormonal (birth control pills, injections, hormonal patches, vaginal rings, or implants), or partner’s vasectomy, and 1 additional effective contraceptive method – male latex or synthetic condom, diaphragm, or cervical cap. Contraception must begin 4 weeks prior to initiating treatment with pomalidomide, during therapy, during dose interruptions, and continuing for 4 weeks following discontinuation of pomalidomide therapy. Reliable contraception is indicated even where there has been a history of infertility, unless due to hysterectomy. Females of reproductive potential should be referred to a qualified provider of contraceptive methods, if needed.
Males
Pomalidomide is present in the semen of males who take pomalidomide capsules. Therefore, males must always use a latex or synthetic condom during any sexual contact with females of reproductive potential while taking pomalidomide capsules and for up to 4 weeks after discontinuing pomalidomide capsules, even if they have undergone a successful vasectomy. Male patients taking pomalidomide capsules must not donate sperm.
Infertility
Based on findings in animals, female fertility may be compromised by treatment with pomalidomide [see Nonclinical Toxicology ( 13.1)].8.4 Pediatric Use
The safety and effectiveness of pomalidomide have not been established in pediatric patients. The safety and effectiveness were assessed but not established in two open-label studies: a dose escalation study in 25 pediatric patients aged 5 to <17 with recurrent, progressive or refractory CNS tumors [NCT02415153] and a parallel-group study conducted in 47 pediatric patients aged 4 to <17 years with recurrent or progressive high-grade glioma, medulloblastoma, ependymoma, or diffuse intrinsic pontine glioma (DIPG) [NCT03257631]. No new safety signals were observed in pediatric patients across these studies.
At the same dose by body surface area, pomalidomide exposure in 55 pediatric patients aged 4 to < 17 years old was within the range observed in adult patients with MM but higher than the exposure observed in adult patients with KS [see Clinical Pharmacology (12.3)].8.5 Geriatric Use
Multiple Myeloma
Of the total number of patients in clinical studies of pomalidomide, 44% were aged older than 65 years, while 10% were aged older than 75 years. No overall differences in effectiveness were observed between these patients and younger patients. In these studies, patients older than 65 years were more likely than patients less than or equal to 65 years of age to experience pneumonia.8.6 Renal Impairment
In patients with severe renal impairment requiring dialysis, the AUC of pomalidomide increased by 38% and the rate of SAE increased by 64% relative to patients with normal renal function; therefore, starting dose adjustment is recommended. For patients with severe renal impairment requiring dialysis, administer pomalidomide after the completion of hemodialysis on dialysis days because exposure of pomalidomide could be significantly decreased during dialysis [see Dosage and Administration (2.7) and Clinical Pharmacology (12.3)].
8.7 Hepatic Impairment
Pomalidomide is metabolized primarily by the liver. Following single dose administration, the AUC of pomalidomide increased 51%, 58%, and 72% in subjects with mild (Child-Pugh class A), moderate (Child-Pugh class B), and severe (Child-Pugh class C) hepatic impairment, respectively compared to subjects with normal liver function. Dose adjustment is recommended in patients with hepatic impairment [see Dosage and Administration (2.8) and Clinical Pharmacology (12.3)].
8.8 Smoking Tobacco
Cigarette smoking reduces pomalidomide AUC due to CYP1A2 induction. Advise patients that smoking may reduce the efficacy of pomalidomide [see Clinical Pharmacology (12.3)].
- 10 OVERDOSAGE
-
11 DESCRIPTION
Pomalidomide is a thalidomide analog. The chemical name is (RS)-4-Amino-2-(2,6-dioxo-piperidin-3-yl)-1H-isoindoline-1,3-dione and it has the following chemical structure:
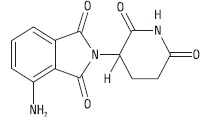
The molecular formula for pomalidomide is C 13H 11N 3O 4and the gram molecular weight is 273.24.
Pomalidomide is a pale yellow to yellow color powder. Soluble in dimethylformamide and in dimethylsulfoxide. Pomalidomide has a chiral carbon atom which exists as a racemic mixture of the R(+) and S(-) enantiomers.
Pomalidomide is available in 1 mg, 2 mg, 3 mg, and 4 mg capsules for oral administration. Each capsule contains pomalidomide as the active ingredient and the following inactive ingredients: black iron oxide, gelatin, mannitol, microcrystalline cellulose, potassium hydroxide, pregelatinized starch, propylene glycol, shellac, sodium stearyl fumarate, strong ammonia solution and titanium dioxide. In addition, the 2 mg and 3 mg capsules also contain iron oxide red. The 2 mg capsule also contains iron oxide yellow.
The botanical source for pregelatinized starch is corn starch. -
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Pomalidomide is an analogue of thalidomide with immunomodulatory, antiangiogenic, and antineoplastic properties. Cellular activities of pomalidomide are mediated through its target cereblon, a component of a cullin ring E3 ubiquitin ligase enzyme complex. In vitro, in the presence of drug, substrate proteins (including Aiolos and Ikaros) are targeted for ubiquitination and subsequent degradation leading to direct cytotoxic and immunomodulatory effects. In in vitrocellular assays, pomalidomide inhibited proliferation and induced apoptosis of hematopoietic tumor cells. Additionally, pomalidomide inhibited the proliferation of lenalidomide-resistant multiple myeloma (MM) cell lines and synergized with dexamethasone in both lenalidomide-sensitive and lenalidomide-resistant cell lines to induce tumor cell apoptosis. Pomalidomide enhanced T cell- and natural killer (NK) cell-mediated immunity and inhibited production of pro-inflammatory cytokines (e.g., TNF-α and IL-6) by monocytes. Pomalidomide demonstrated anti-angiogenic activity in a mouse tumor model and in the in vitroumbilical cord model.
12.2 Pharmacodynamics
Pomalidomide exposure-response analyses showed that there was no relationship between systemic pomalidomide exposure level and efficacy or safety following pomalidomide dose of 4 mg.
Cardiac Electrophysiology
The QTc prolongation potential of pomalidomide was evaluated in a single center, randomized, double-blind crossover study (N=72) using 4 mg pomalidomide, 20 mg pomalidomide, placebo, and 400 mg moxifloxacin (positive control). No significant QTc prolongation effect of pomalidomide was observed following pomalidomide doses of 4 and 20 mg.12.3 Pharmacokinetics
In patients with MM who received pomalidomide 4 mg daily alone or in combination with dexamethasone, pomalidomide steady-state drug exposure was characterized by AUC (CV%) of 860 (37%) ng.h/mL and C max (CV%) of 75 (32%) ng/mL.
Absorption
Following administration of single oral doses of pomalidomide, the maximum plasma concentration (C max) for pomalidomide occurs at 2 to 3 hours postdose in patients with MM.
Effect of Food
Co-administration of pomalidomide with a high-fat meal (approximately 50% of the total caloric content) and high-calorie meal (approximately 800 to 1000 calories) (the meal contained approximately 150, 250, and 500 to 600 calories from protein, carbohydrates, and fat, respectively) delays the T maxby 2.5 hours, decreased mean plasma C maxand AUC in healthy subjects by about 27% and 8%, respectively.
Distribution
Pomalidomide has a mean apparent volume of distribution (Vd/F) between 62 and 138 L at steady state in patients with MM.
Pomalidomide is distributed in semen of healthy subjects at a concentration of approximately 67% of plasma level at 4 hours postdose (~T max) after 4 days of 2 mg once-daily dosing.
Human plasma protein binding of pomalidomide ranges from 12% to 44% and is not concentration dependent. Pomalidomide is a substrate for P-gp.
Elimination
Pomalidomide has a mean total body clearance (CL/F) of 7 to 10 L/h in patients with MM. Pomalidomide is eliminated with a median plasma half-life of 9.5 hours in healthy subjects and 7.5 hours in patients with MM.
Metabolism
Pomalidomide is primarily metabolized in the liver by CYP1A2 and CYP3A4. Minor contributions from CYP2C19 and CYP2D6 were also observed in vitro.
Excretion
Following a single oral administration of [ 14C]-pomalidomide to healthy subjects, approximately 73% and 15% of the radioactive dose was eliminated in urine and feces, respectively, with approximately 2% and 8% of the radiolabeled dose eliminated unchanged as pomalidomide in urine and feces.
Specific Populations
Age (61 to 85 years old), sex and race have no clinically significant effect on the systemic exposure of pomalidomide.
Patients with Renal Impairment
Pomalidomide pharmacokinetic parameters were not significantly affected in patients with moderate (30 mL/min ≤ CLcr< 60 mL/min) or severe (15 mL/min ≤ CLcr< 30 mL/min) renal impairment relative to patients with normal renal function (CLcr ≥ 60 mL/min). Mean exposure (AUC) to pomalidomide increased by 38% in patients with severe renal impairment requiring dialysis (CLcr< 30 mL/min requiring dialysis) and 40% in patients with end stage renal disease (CLcr< 15 mL/min) on non-dialysis days. In patients with severe renal impairment requiring dialysis, the estimated dialysis clearance is approximately 12 L/h which is higher than pomalidomide total body clearance, indicating hemodialysis will remove pomalidomide from the blood circulation.
Patients with Hepatic Impairment
Mean exposure (AUC) of pomalidomide increased by 51%, 58% and 72% in subjects with mild, moderate or severe hepatic impairment as defined by Child-Pugh criteria, respectively.
Drug Interaction Studies
Clinical Studies
Co-administration of pomalidomide with the following drugs did not increase pomalidomide exposure to a clinically significant extent: ketoconazole (a strong CYP3A4 and P-gp inhibitor), carbamazepine (a strong CYP3A4 inducer) and dexamethasone (a weak to moderate CYP3A4 inducer). Co-administration of pomalidomide with drugs that are CYP1A2 inducers has not been studied.
CYP1A2Inhibitors: Co-administration of fluvoxamine (a strong CYP1A2 inhibitor) with pomalidomide increased mean [90% confidence interval] pomalidomide exposure by 125% [98% to 157%] compared to pomalidomide alone in healthy subjects. Co-administration of fluvoxamine in the presence of ketoconazole (a strong CYP3A4 and P-gp inhibitor) with pomalidomide capsules increased mean pomalidomide exposure by 146% [126% to 167%] compared to pomalidomide capsules administered alone in healthy subjects, indicating the predominant effect of CYP1A2 inhibition in the increase of pomalidomide exposure [see Dosage and Administration (2.6) and Drug Interactions (7.1)].
Strong CYP3A4 and P-gp Inhibitors: Co-administration of ketoconazole (a strong CYP3A4 and P-gp inhibitor) in 16 healthy male subjects increased AUC of pomalidomide by 19% compared to pomalidomide administered alone.
Strong CYP1A2 Inducers:Co-administration of pomalidomide with drugs that are CYP1A2 inducers has not been studied and may reduce pomalidomide exposure.
Strong CYP3A4 Inducers:Co-administration of carbamazepine to 16 healthy male subjects decreased AUC of pomalidomide by 20% with a 90% confidence interval [13% to 27%] compared to when pomalidomide was administered alone.
Dexamethasone:Co-administration of multiple doses of 4 mg pomalidomide with 20 mg to 40 mg dexamethasone (a weak to moderate inducer of CYP3A4) to patients with MM had no effect on the pharmacokinetics of pomalidomide compared to when pomalidomide was administered alone.
Smoking:In 14 healthy male subjects who smoked 25 cigarettes per day for a total of 10 days, after single oral dose of 4 mg pomalidomide, C maxof pomalidomide increased 14% while AUC of pomalidomide decreased 32%, compared to that in 13 healthy male subjects who were non-smokers.
In Vitro Studies
Pomalidomide does not inhibit or induce cytochrome p450 enzymes or transporters i n vitro. -
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Studies examining the carcinogenic potential of pomalidomide have not been conducted. One of 12 monkeys dosed with 1 mg/kg of pomalidomide (an exposure approximately 15-fold of the exposure in patients at the recommended dose of 4 mg/day) developed acute myeloid leukemia in a 9-month repeat-dose toxicology study.
Pomalidomide was not mutagenic or clastogenic in a battery of tests, including the bacteria reverse mutation assay (Ames test), the in vitroassay using human peripheral blood lymphocytes, and the micronucleus test in orally treated rats administered doses up to 2000 mg/kg/day.
In a fertility and early embryonic development study in rats, drug-treated males were mated with untreated or treated females. Pomalidomide was administered to males and females at doses of 25 to 1000 mg/kg/day. When treated males were mated with treated females, there was an increase in post-implantation loss and a decrease in mean number of viable embryos at all dose levels. There were no other effects on reproductive functions or the number of pregnancies. The lowest dose tested in animals resulted in an exposure (AUC) approximately 100-fold of the exposure in patients at the recommended dose of 4 mg/day. When treated males in this study were mated with untreated females, all uterine parameters were comparable to the controls. Based on these results, the observed effects were attributed to the treatment of females. -
14 CLINICAL STUDIES
14.1 Multiple Myeloma
Trial 1
Trial 1 was a phase 2, multicenter, randomized open-label study in patients with relapsed multiple myeloma (MM) who were refractory to their last myeloma therapy and had received lenalidomide and bortezomib. Patients were considered relapsed if they had achieved at least stable disease for at least 1 cycle of treatment to at least 1 prior regimen and then developed progressive disease. Patients were considered refractory if they experienced disease progression on or within 60 days of their last therapy. A total of 221 patients were randomized to receive pomalidomide alone or pomalidomide with Low-dose Dex. In Trial 1, the safety and efficacy of pomalidomide 4 mg, once daily for 21 of 28 days, until disease progression, were evaluated alone and in combination with Low-dose Dex (40 mg/day given only on Days 1, 8, 15, and 22 of each 28-day cycle for patients aged 75 years or younger, or 20 mg/day given only on Days 1, 8, 15, and 22 of each 28-day cycle for patients aged greater than 75 years). Patients in the pomalidomide alone arm were allowed to add Low-dose Dex upon disease progression.
Table 7 summarizes the baseline patient and disease characteristics in Trial 1. The baseline demographics and disease characteristics were balanced and comparable between the study arms.
Table 7: Baseline Demographic and Disease-Related Characteristics – Trial 1
Pomalidomide
(n=108)
Pomalidomide
+ Low-dose Dex
(n=113)
Patient Characteristics
Median age, years (range)
61 (37 to 88)
64 (34 to 88)
Age distribution, n (%)
<65 years
≥65 years
65 (60.2)
43 (39.8)
60 (53.1)
53 (46.9)
Sex, n (%)
Male
Female
57 (52.8)
51 (47.2)
62 (54.9)
51 (45.1)
Race/ethnicity, n (%)
White
Black or African American
All other race
86 (79.6)
16 (14.8)
6 (5.6)
92 (81.4)
17 (15)
4 (3.6)
ECOG Performance, n (%)
Status 0 to 1
95 (87.9)
100 (88.5)
Disease Characteristics
Number of prior therapies
Median (min, max)
5 (2, 12)
5 (2, 13)
Prior transplant, n (%)
82 (75.9)
84 (74.3)
Refractory to bortezomib and lenalidomide, n (%)
64 (59.3)
69 (61.1)
Data cutoff: 01 April 2011
Table 8 summarizes the analysis results of overall response rate (ORR) and duration of response (DOR), based on assessments by the Independent Review Adjudication Committee for the treatment arms in Trial 1. ORR did not differ based on type of prior antimyeloma therapy.
Table 8: Trial 1 Results
Pomalidomide a
(n=108)
Pomalidomide
+ Low-dose Dex
(n=113)
Response
Overall Response Rate
(ORR), bn (%)
8 (7.4)
33 (29.2)
95% CI for ORR (%)
(3.3, 14.1)
(21.0, 38.5)
Complete Response (CR), n (%)
0 (0.0)
1 (0.9)
Partial Response (PR), n (%)
8 (7.4)
32 (28.3)
Duration of Response (DOR)
Median, months
NE
7.4
95% CI for DOR (months)
NE
(5.1, 9.2)
aResults are prior to the addition of dexamethasone.
bORR = PR + CR per EBMT criteria.
CI, confidence interval; NE, not established (the median has not yet been reached).
Data cutoff: 01 April 2011
Trial 2
Trial 2 was a Phase 3 multi-center, randomized, open-label study, where pomalidomide + Low-dose Dex therapy was compared to High-dose Dex in adult patients with relapsed and refractory MM, who had received at least two prior treatment regimens, including lenalidomide and bortezomib, and demonstrated disease progression on or within 60 days of the last therapy. Patients with creatinine clearance ≥ 45mL/min qualified for the trial. A total of 455 patients were enrolled in the trial: 302 in the pomalidomide + Low-dose Dex arm and 153 in the High-dose Dex arm. Patients in the pomalidomide + Low-dose Dex arm were administered 4 mg pomalidomide orally on Days 1 to 21 of each 28-day cycle. Dexamethasone (40 mg) was administered once per day on Days 1, 8, 15 and 22 of a 28-day cycle. Patients > 75 years of age started treatment with 20 mg dexamethasone using the same schedule. For the High-dose Dex arm, dexamethasone (40 mg) was administered once per day on Days 1 through 4, 9 through 12, and 17 through 20 of a 28-day cycle. Patients > 75 years of age started treatment with 20 mg dexamethasone using the same schedule. Treatment continued until patients had disease progression.
Baseline patient and disease characteristics were balanced and comparable between the study arms, as summarized in Table 9. Overall, 94% of patients had disease refractory to lenalidomide, 79% had disease refractory to bortezomib and 74% had disease refractory to both lenalidomide and bortezomib.
Table 9: Baseline Demographic and Disease-Related Characteristics – Trial 2
Pomalidomide + Low-dose Dex
(N=302)
High-dose Dex
(N=153)
Patient Characteristics
Median Age, years (range)
64 (35, 84)
65 (35, 87)
Age Distribution n (%)
< 65 years
≥ 65 years
158 (52)
144 (48)
74 (48)
79 (52)
Sex n (%)
Male
Female
181 (60)
121 (40)
87 (57)
66 (43)
Race/Ethnicity n (%)
White
Black or African American
Asian
Other Race
Not Collected
244 (81)
4 (1)
4 (1)
2 (1)
48 (16)
113 (74)
3 (2)
0 (0)
2 (1)
35 (23)
ECOG Performance n (%)
Status 0
Status 1
Status 2
Status 3
Missing
110 (36)
138 (46)
52 (17)
0 (0)
2 (1)
36 (24)
86 (56)
25 (16)
3 (2)
3 (2)
Disease Characteristics
Number of Prior Therapies Median, (Min, Max)
5 (2, 14)
5 (2, 17)
Prior stem cell transplant n (%)
214 (71)
105 (69)
Refractory to bortezomib and lenalidomide n (%)
225 (75)
113 (74)
Data cutoff: 01March 2013
Table 10 summarizes the progression free survival (PFS) and overall response rate (ORR) based on the assessment by the Independent Review Adjudication Committee (IRAC) review at the final PFS analysis and overall survival (OS) at the OS analysis. PFS was significantly longer with pomalidomide + Low-dose Dex than High-dose Dex: HR 0.45 (95% CI: 0.35 to 0.59 p < 0.001). OS was also significantly longer with pomalidomide + Low-dose Dex than High-dose Dex: HR 0.70 (95% CI: 0.54 to 0.92 p = 0.009). The Kaplan-Meier curves for PFS and OS for the ITT population are provided in Figures 1 and 2, respectively.
Table 10: Trial 2 Results
Pomalidomide
+ Low-dose Dex
(N=302)
High-dose Dex
(N=153)
Progression Free Survival Time
Number (%) of events
164 (54.3)
103 (67.3)
Median a(2-sided 95% CI) (months )
3.6 [3.0, 4.6]
1.8 [1.6, 2.1]
Hazard Ratio (Pom+LD-Dex:HD-Dex) 2-Sided 95% CI b
0.45 [0.35, 0.59]
Log-Rank Test 2-sided P-Value c
<0.001
Overall Survival Time d
Number (%) of deaths
147 (48.7)
86 (56.2)
Median a(2-sided 95% CI) (months )
12.4 [10.4, 15.3]
8.0 [6.9, 9.0]
Hazard Ratio (Pom+LD-Dex:HD-Dex) 2-Sided 95% CI e
0.70 [0.54, 0.92]
Log-Rank Test 2-sided P-Value f, g
0.009
Overall Response Rate, n (%)
71 (23.5)
6 (3.9)
Complete Response
1 (0.3)
0
Very Good Partial Response
8 (2.6)
1 (0.7)
Partial Response
62 (20.5)
5 (3.3)
Note: CI=Confidence interval; HD-Dex=High dose dexamethasone; IRAC=Independent Review Adjudication Committee; LD-Dex=Low dose dexamethasone.
aThe median is based on Kaplan-Meier estimate.
bBased on Cox proportional hazards model comparing the hazard functions associated with treatment groups, stratified by age (≤75 vs >75), diseases population (refractory to both Lenalidomide and Bortezomib vs not refractory to both drugs), and prior number of antimyeloma therapy (=2 vs >2), stratification factors for the trial.
cThe p-value is based on a stratified log-rank test with the same stratification factors as the above Cox model.
d53% of patients in the High-dose Dex arm subsequently received pomalidomide.
eBased on Cox proportional hazards model (unstratified) comparing the hazard functions associated with treatment groups.
fThe p-value is based on an unstratified log-rank test.
gAlpha control for PFS and OS.
Data cutoff: 07 Sep 2012 for PFS
Data cutoff: 01 Mar 2013 for OS and ORR
Figure 1: Progression Free Survival Based on IRAC Review of Response by IMWG Criteria (Stratified Log Rank Test) (ITT Population)
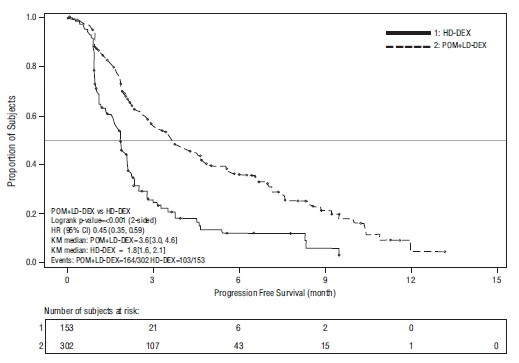
Data cut-off: 07 Sep 2012
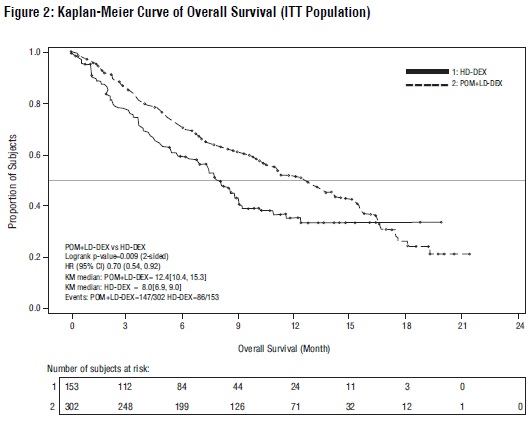
Data cutoff: 01 Mar 2013
- 15 REFERENCES
-
16 HOW SUPPLIED/STORAGE AND HANDLING
Pomalidomide Capsules, 1 mg are opaque, white cap and opaque white body, hard gelatin capsules imprinted with 'H' on cap and 'P1' on body, filled with pale yellow to yellowish color powder. They are supplied as follows:
Bottles of 21 Capsules NDC: 31722-770-21
Bottles of 100 Capsules NDC: 31722-770-01
Carton of 60 capsules (6 x 10 unit-dose) NDC: 31722-770-32
Pomalidomide Capsules, 2 mg are opaque, white cap and opaque brown body, hard gelatin capsules imprinted with 'H' on cap and 'P2' on body, filled with pale yellow to yellowish color powder. They are supplied as follows:
Bottles of 21 Capsules NDC: 31722-771-21
Bottles of 100 Capsules NDC: 31722-771-01
Carton of 60 capsules (6 x 10 unit-dose) NDC: 31722-771-32
Pomalidomide Capsules, 3 mg are opaque, white cap and opaque pink body, hard gelatin capsules imprinted with 'H' on cap and 'P3' on body, filled with pale yellow to yellowish color powder. They are supplied as follows:
Bottles of 21 Capsules NDC: 31722-772-21
Bottles of 100 Capsules NDC: 31722-772-01
Carton of 60 capsules (6 x 10 unit-dose) NDC: 31722-772-32
Pomalidomide Capsules, 4 mg are opaque, white cap and opaque white body, hard gelatin capsules imprinted with 'H' on cap and 'P4' on body, filled with pale yellow to yellowish color powder. They are supplied as follows:
Bottles of 21 Capsules NDC: 31722-773-21
Bottles of 100 Capsules NDC: 31722-773-01
Carton of 60 capsules (6 x 10 unit-dose) NDC: 31722-773-32
Store at 20°C to 25°C (68°F to 77°F); excursions permitted to 15°C to 30°C (59°F to 86°F). [see USP Controlled Room Temperature].
Care should be exercised in handling of pomalidomide. Do not open or crush pomalidomide capsules. If powder from pomalidomide capsules contacts the skin, wash the skin immediately and thoroughly with soap and water. If pomalidomide contacts the mucous membranes, flush thoroughly with water.
Follow procedures for proper handling and disposal of hazardous drugs.1 -
17 PATIENT COUNSELING INFORMATION
Advise the patient to read the FDA-approved patient labeling ( Medication Guide).
Embryo-Fetal Toxicity
Advise patients that pomalidomide is contraindicated in pregnancy [see Contraindications (4)]. Pomalidomide is a thalidomide analogue and may cause serious birth defects or death to a developing baby [see Warnings and Precautions (5.1) and Use in Specific Populations (8.1)].
Advise females of reproductive potential that they must avoid pregnancy while taking pomalidomide capsules and for at least 4 weeks after completing therapy.
Initiate pomalidomide treatment in females of reproductive potential only following a negative pregnancy test.
Advise females of reproductive potential of the importance of monthly pregnancy tests and the need to use 2 different forms of contraception, including at least 1 highly effective form, simultaneously during pomalidomide therapy, during dose interruptions, and for 4 weeks after she has completely finished taking pomalidomide capsules. Highly effective forms of contraception other than tubal ligation include IUD and hormonal (birth control pills, injections, patch, or implants) and a partner’s vasectomy. Additional effective contraceptive methods include latex or synthetic condom, diaphragm, and cervical cap.
Instruct patient to immediately stop taking pomalidomide capsules and contact her healthcare provider if she becomes pregnant while taking this drug, if she misses her menstrual period or experiences unusual menstrual bleeding, if she stops taking birth control, or if she thinks FOR ANY REASON that she may be pregnant.
Advise patient that if her healthcare provider is not available, she should call the REMS Call Center at 1-888-423-5436 [see Warnings and Precautions (5.1) and Use in Specific Populations (8.3)].
Advise males to always use a latex or synthetic condom during any sexual contact with females of reproductive potential while taking pomalidomide capsules and for up to 4 weeks after discontinuing pomalidomide capsules, even if they have undergone a successful vasectomy.
Advise male patients taking pomalidomide capsules that they must not donate sperm [see Warnings and Precautions (5.1) and Use in Specific Populations (8.3)].
All patients must be instructed to not donate blood while taking pomalidomide capsules and for 4 weeks following discontinuation of pomalidomide capsules [see Warnings and Precautions (5.1)].
PS-Pomalidomide REMS
Because of the risk of embryo-fetal toxicity, pomalidomide is only available through a restricted program called PS-Pomalidomide REMS [see Warnings and Precautions (5.2)].
Patients must sign a Patient-Physician Agreement Form and comply with the requirements to receive pomalidomide capsules. In particular, females of reproductive potential must comply with the pregnancy testing, contraception requirements, and participate in monthly telephone surveys. Males must comply with the contraception requirements [see Use in Specific Populations (8.3)].
Pomalidomide capsules are available only from pharmacies that are certified in PS-Pomalidomide REMS. Provide patients with the telephone number and website for information on how to obtain the product.
Pregnancy Exposure Registry
Inform females that there is a Pregnancy Exposure Registry that monitors pregnancy outcomes in females exposed to pomalidomide during pregnancy and that they can contact the Pregnancy Exposure Registry by calling 1-888-423-5436 [see Use in Specific Populations (8.1)].
Venous and Arterial Thromboembolism
Inform patients of the risk of developing DVT, PE, MI, and stroke and to report immediately any signs and symptoms suggestive of these events for evaluation [see Warnings and Precautions (5.3)].
Hematologic Toxicities
Inform patients on the risks of developing neutropenia, thrombocytopenia, and anemia and the need to report signs and symptoms associated with these events to their healthcare provider for further evaluation [see Warnings and Precautions (5.5)].
Hepatotoxicity
Inform patients on the risks of developing hepatotoxicity, including hepatic failure and death, and to report signs and symptoms associated with these events to their healthcare provider for evaluation [see Warnings and Precautions (5.6)].
Severe Cutaneous Reactions
Inform patients of the potential risk for severe skin reactions such as SJS, TEN and DRESS and to report any signs and symptoms associated with these reactions to their healthcare provider for evaluation [see Warnings and Precautions (5.7)].
Dizziness and Confusional State
Inform patients of the potential risk of dizziness and confusional state with the drug, to avoid situations where dizziness or confusional state may be a problem, and not to take other medications that may cause dizziness or confusional state without adequate medical advice [see Warnings and Precautions (5.8)].
Neuropathy
Inform patients of the risk of neuropathy and to report the signs and symptoms associated with these events to their healthcare provider for further evaluation [see Warnings and Precautions (5.9)].
Second Primary Malignancies
Inform the patient that the potential risk of developing acute myelogenous leukemia during treatment with pomalidomide is unknown [see Warnings and Precautions (5.10)].
Tumor Lysis Syndrome
Inform patients of the potential risk of tumor lysis syndrome and to report any signs and symptoms associated with this event to their healthcare provider for evaluation [see Warnings and Precautions (5.11)] .
Hypersensitivity
Inform patients of the potential for severe hypersensitivity reactions such as angioedema and anaphylaxis to pomalidomide. Instruct patients to contact their healthcare provider right away for any signs and symptoms of these reactions. Advise patients to seek emergency medical attention for signs or symptoms of severe hypersensitivity reactions [see Warnings and Precautions (5.12)].
Smoking Tobacco
Advise patients that smoking tobacco may reduce the efficacy of pomalidomide [see Use in Specific Populations (8.8) and Clinical Pharmacology (12.3)].
Dosing Instructions
Inform patients on how to take pomalidomide capsules [see Dosage and Administration (2.2, 2.3, 2.9)]
Pomalidomide capsules should be taken once daily at about the same time each day.
Patients on hemodialysis should take pomalidomide capsules following hemodialysis, on hemodialysis days.
Pomalidomide capsules may be taken with or without food.
The capsules should not be opened, broken, or chewed. Pomalidomide capsules should be swallowed whole with water.
Instruct patients that if they miss a dose of pomalidomide capsules, they may still take it up to 12 hours after the time they would normally take it. If more than 12 hours have elapsed, they should be instructed to skip the dose for that day. The next day, they should take pomalidomide capsules at the usual time. Warn patients not to take 2 doses to make up for the one that they missed.

Manufactured for:
Camber Pharmaceuticals, Inc.
Piscataway, NJ 08854.By: HETERO TM
Hetero Labs Limited, Unit V, Polepally, Jadcherla,
Mahabubnagar - 509 301, India.
All brand names listed are registered trademarks of their respective owners and are not trademarks of Hetero Labs Limited.
Revised:11/2025 -
MEDICATION GUIDE
Pomalidomide (poe” ma lid' oh mide)
capsules
What is the most important information I should know about pomalidomide capsules?
Before you begin taking pomalidomide capsules, you must read and agree to all of the instructions in PS-Pomalidomide REMS. For more information, call 1-888-423-5436 or go to www.PS-PomalidomideREMS.com. Before prescribing pomalidomide capsules, your healthcare provider will explain PS-Pomalidomide REMS to you and have you sign the Patient-Physician Agreement Form.
Pomalidomide capsules can cause serious side effects including:
Possible birth defects (deformed babies) or death of an unborn baby.Females who are pregnant or who plan to become pregnant must not take pomalidomide capsules.
Pomalidomide capsules are similar to the medicine thalidomide (THALOMID).We know thalidomide can cause severe life-threatening birth defects. Pomalidomide capsules have not been tested in pregnant females. Pomalidomide capsules have harmed unborn animals in animal testing.
Females must not get pregnant:
o For at least 4 weeks before starting pomalidomide capsules
o While taking pomalidomide capsules
o During any breaks (interruptions) in your treatment with pomalidomide capsules
o For at least 4 weeks after stopping pomalidomide capsules
Females who can become pregnant:
o Will have pregnancy tests weekly for 4 weeks, then every 4 weeks if your menstrual cycle is regular, or every 2 weeks if your menstrual cycle is irregular.
If you miss your period or have unusual bleeding, you will need to have a pregnancy test and receive counseling.
o Must agree to use two acceptable forms of birth control at the same time, for at least 4 weeks before, while taking, during any breaks (interruptions) in your treatment, and for at least 4 weeks after stopping pomalidomide capsules.
o Talk with your healthcare provider to find out about options for acceptable forms of birth control that you may use to prevent pregnancy before, during, and after treatment with pomalidomide capsules.
If you become pregnant while taking pomalidomide capsules, stop taking it right away and call your healthcare provider.
If your healthcare provider is not available, you can call the REMS Call Center at 1-888-423-5436. Healthcare providers and patients should report all cases of pregnancy to:
o FDA MedWatch at 1-800-FDA-1088, and
o REMS Call Center at 1-888-423-5436
There is a pregnancy exposure registry that monitors the outcomes of females who take pomalidomide capsules during pregnancy, or if their male partner takes pomalidomide capsules and they are exposed during pregnancy. You can enroll in this registry by calling the REMS Call Center at the phone number listed above.
Pomalidomide can pass into human semen:
o Males, including those who have had a vasectomy, must always use a latex or synthetic condom during any sexual contact with a pregnant female or a female that can become pregnant while taking pomalidomide capsules, during any breaks (interruptions) in your treatment with pomalidomide capsules, and for 4 weeks after stopping pomalidomide capsules.
o Do not have unprotected sexual contact with a female who is or could become pregnant. Tell your healthcare provider if you do have unprotected sexual contact with a female who is or could become pregnant.
o Do not donate sperm while taking pomalidomide capsules, during any breaks (interruptions) in your treatment, and for 4 weeks after stopping pomalidomide capsules. If a female becomes pregnant with your sperm, the baby may be exposed to pomalidomide and may be born with birth defects.
Men, if your female partner becomes pregnant, you should call your healthcare provider right away.
Blood clots in your arteries, veins, and lungs, heart attack, and stroke can happen if you take pomalidomide capsules.Most people who take pomalidomide capsules will also take a blood thinner medicine to help prevent blood clots.
Before taking pomalidomide capsules, tell your healthcare provider:
o If you have had a blood clot in the past
o If you have high blood pressure, smoke, or if you have been told you have a high level of fat in your blood (hyperlipidemia)
o About all the medicines you take. Certain other medicines can also increase your risk for blood clots
Call your healthcare provider or get medical help right away if you get any of the following during treatment with pomalidomide capsules:
Signs or symptoms of a blood clot in the lung, arm, or leg may include:shortness of breath, chest pain, or arm or leg swelling
Signs or symptoms of a heart attack may include:chest pain that may spread to the arms, neck, jaw, back, or stomach area (abdomen), feeling sweaty, shortness of breath, feeling sick or vomiting
Signs or symptoms of stroke may include:sudden numbness or weakness, especially on one side of the body, severe headache or confusion, or problems with vision, speech, or balance.
What are pomalidomide capsules?
Pomalidomide capsules are a prescription medicine used to treat adults with:
Multiple myeloma.Pomalidomide capsules are taken along with the medicine dexamethasone, in people who:
o have received at least 2 prior medicines to treat multiple myeloma, including a type of medicine known as a proteasome inhibitor and lenalidomide, and
o their disease has become worse during treatment or within 60 days of finishing the last treatment.
It is not known if pomalidomide capsules are safe and effective in children.
Who should not take pomalidomide capsules?
Do not take pomalidomide capsules if you:
are pregnant, plan to become pregnant, or become pregnant during treatment with pomalidomide capsules. See “What is the most important information I should know about pomalidomide capsules?”
are allergic to pomalidomide or any of the ingredients in pomalidomide capsules. See the end of this Medication Guide for a complete list of ingredients in pomalidomide capsules.
What should I tell my healthcare provider before taking pomalidomide capsules?
Before you take pomalidomide capsules, tell your healthcare provider if you:
smoke cigarettes. Pomalidomide may not work as well in people who smoke
have liver problems
have kidney problems and are receiving hemodialysis treatment
have any other medical conditions
are breastfeeding. You should notbreastfeed during treatment with pomalidomide capsules. It is not known if pomalidomide passes into your breast milk and can harm your baby.
Tell your healthcare provider about all the medicines you take,including prescription and over-the-counter medicines, vitamins, and herbal supplements. Pomalidomide capsules and other medicines may affect each other, causing serious side effects. Talk with your healthcare provider before taking any new medicines.
Know the medicines you take. Keep a list of them to show your healthcare provider and pharmacist.
How should I take pomalidomide capsules?
Take pomalidomide capsules exactly as prescribed and follow all the instructions of PS-Pomalidomide REMS.
Swallow pomalidomide capsules whole with water 1 time a day. Do not break, chew, or open your capsules.
Pomalidomide capsules may be taken with or without food.
Take pomalidomide capsules at about the same time each day.
If you are on hemodialysis, take pomalidomide capsules after hemodialysis, on hemodialysis days.
Do not open the pomalidomide capsules or handle them any more than needed. If you touch a broken pomalidomide capsules or the medicine in the capsule, wash the area of your body right away with soap and water.
If you miss a dose of pomalidomide capsules and it has been less than 12 hours since your regular time, take it as soon as you remember. If it has been more than 12 hours, just skip your missed dose. Do not take 2 doses at the same time.
If you take too much pomalidomide, call your healthcare provider right away.What should I avoid while taking pomalidomide capsules?
See “What is the most important information I should know about pomalidomide capsules?”
Females: Do not get pregnant and do not breastfeed while taking pomalidomide capsules.
Males: Do not donate sperm.
Do not share pomalidomide capsules with other people. It may cause birth defects and other serious problems.
Do not donate bloodwhile you take pomalidomide capsules, during any breaks (interruptions) in your treatment, and for 4 weeks after stopping pomalidomide capsules. If someone who is pregnant gets your donated blood, her baby may be exposed to pomalidomide capsules and may be born with birth defects.
Pomalidomide capsules can cause dizziness and confusion. Avoid taking other medicines that may cause dizziness and confusion during treatment with pomalidomide capsules. Avoid situations that require you to be alert until you know how pomalidomide capsules affect you.What are the possible side effects of pomalidomide capsules?
Pomalidomide capsules can cause serious side effects, including:
See “What is the most important information I should know about pomalidomide capsules?”
Low white blood cells (neutropenia), low platelets (thrombocytopenia), and low red blood cells (anemia) are common with pomalidomide capsules, but can also be serious.You may need a blood transfusion or certain medicines if your blood counts drop too low. Your blood counts should be checked weekly for the first 8 weeks of treatment and monthly after that.
Severe liver problems, including liver failure and death. Your healthcare provider should do blood tests to check your liver function during your treatment with pomalidomide capsules. Tell your healthcare provider right away if you develop any of the following symptoms of liver problems:
o Yellowing of your skin or the white part of your eyes (jaundice) o Pain on the upper right side of your stomach area (abdomen)
o Dark or brown (tea-colored) urine o Bleeding or bruising more easily than normal
o Feeling very tired
Severe allergic reactions and severe skin reactionscan happen with pomalidomide capsules and may cause death.
Call your healthcare provider if you develop any of the following signs or symptoms during treatment with pomalidomide capsules:
o a red, itchy, skin rash o peeling of your skin or blisters o severe itching
o fever
Get emergency medical help right away if you develop any of the following signs or symptoms during treatment with pomalidomide capsules:
o swelling of your lips, mouth, tongue, or throat
o trouble breathing or swallowing
o raised red areas on your skin (hives) o a very fast heartbeat
o you feel dizzy or faint
Dizziness and confusion. See “What should I avoid while taking pomalidomide capsules?”
Nerve damage. Stop taking pomalidomide capsules and call your healthcare provider if you develop symptoms of nerve damage including: numbness, tingling, pain, burning sensation in your hands, legs, or feet.
Risk of new cancers (malignancies).New cancers, including certain blood cancers (acute myelogenous leukemia or AML) have been seen in people who received pomalidomide capsules. Talk with your healthcare provider about your risk of developing new cancers if you take pomalidomide capsules.
Tumor lysis syndrome (TLS).TLS is caused by the fast breakdown of cancer cells. TLS can cause kidney failure and the need for dialysis treatment, abnormal heart rhythm, seizure, and sometimes death. Your healthcare provider may do blood tests to check you for TLS.
Your healthcare provider may tell you to stop taking pomalidomide capsules if you develop certain serious side effects during treatment.
The most common side effects of pomalidomide in people with Multiple Myeloma include:
o tiredness and weakness o diarrhea o back pain
o constipation o shortness of breath o fever
o nausea o upper respiratory tract infection
These are not all the possible side effects of pomalidomide capsules.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.How should I store pomalidomide capsules?
Store pomalidomide capsules at room temperature between 68°F to 77°F (20°C to 25°C).
Return any unused pomalidomide capsules to PS-Pomalidomide REMS by calling 1-888-423-5436 or your healthcare provider.
Keep pomalidomide capsules and all medicines out of the reach of children.General information about the safe and effective use of pomalidomide capsules.
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not take pomalidomide capsules for conditions for which it was not prescribed. Do not give pomalidomide capsules to other people, even if they have the same symptoms you have. They may harm them and may cause birth defects.
If you would like more information, talk with your healthcare provider. You can ask your healthcare provider or pharmacist for information about pomalidomide capsules that is written for health professionals.
For more information, call 1-888-423-5436 or go to www.PS-PomalidomideREMS.com.What are the ingredients in pomalidomide capsules?
Active ingredient: pomalidomide
Inactive ingredients:black iron oxide, gelatin, mannitol, microcrystalline cellulose, potassium hydroxide, pregelatinized starch, propylene glycol, shellac, sodium stearyl fumarate, strong ammonia solution and titanium dioxide. In addition, the 2 mg and 3 mg capsules also contain iron oxide red. The 2 mg capsule also contains iron oxide yellow.
Medication Guide available at http://camberpharma.com/medication-guides

Manufactured for:
Camber Pharmaceuticals, Inc.
Piscataway, NJ 08854.
By: HETEROTM
Hetero Labs Limited, Unit V, Polepally, Jadcherla,
Mahabubnagar - 509 301, India.
All brand names listed are registered trademarks of their respective owners and are not trademarks of Hetero Labs Limited.This Medication Guide has been approved by the U.S. Food and Drug Administration.
Revised: 11/2025
- PACKAGE LABEL.PRINCIPAL DISPLAY PANEL
-
INGREDIENTS AND APPEARANCE
POMALIDOMIDE
pomalidomide capsuleProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 31722-771 Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength POMALIDOMIDE (UNII: D2UX06XLB5) (POMALIDOMIDE - UNII:D2UX06XLB5) POMALIDOMIDE 2 mg Inactive Ingredients Ingredient Name Strength FERROSOFERRIC OXIDE (UNII: XM0M87F357) GELATIN, UNSPECIFIED (UNII: 2G86QN327L) MANNITOL (UNII: 3OWL53L36A) MICROCRYSTALLINE CELLULOSE 101 (UNII: 7T9FYH5QMK) POTASSIUM HYDROXIDE (UNII: WZH3C48M4T) PROPYLENE GLYCOL (UNII: 6DC9Q167V3) SHELLAC (UNII: 46N107B71O) SODIUM STEARYL FUMARATE (UNII: 7CV7WJK4UI) AMMONIA (UNII: 5138Q19F1X) TITANIUM DIOXIDE (UNII: 15FIX9V2JP) STARCH, CORN (UNII: O8232NY3SJ) FERRIC OXIDE RED (UNII: 1K09F3G675) FERRIC OXIDE YELLOW (UNII: EX438O2MRT) Product Characteristics Color white (opaque white cap) , brown (opaque brown body) Score no score Shape CAPSULE Size 14mm Flavor Imprint Code H;P2 Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 31722-771-21 21 in 1 BOTTLE; Type 0: Not a Combination Product 02/28/2026 2 NDC: 31722-771-01 100 in 1 BOTTLE; Type 0: Not a Combination Product 02/28/2026 3 NDC: 31722-771-32 6 in 1 CARTON 02/28/2026 3 10 in 1 BLISTER PACK; Type 0: Not a Combination Product Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA210236 02/28/2026 POMALIDOMIDE
pomalidomide capsuleProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 31722-772 Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength POMALIDOMIDE (UNII: D2UX06XLB5) (POMALIDOMIDE - UNII:D2UX06XLB5) POMALIDOMIDE 3 mg Inactive Ingredients Ingredient Name Strength GELATIN, UNSPECIFIED (UNII: 2G86QN327L) MANNITOL (UNII: 3OWL53L36A) MICROCRYSTALLINE CELLULOSE 101 (UNII: 7T9FYH5QMK) POTASSIUM HYDROXIDE (UNII: WZH3C48M4T) PROPYLENE GLYCOL (UNII: 6DC9Q167V3) SHELLAC (UNII: 46N107B71O) SODIUM STEARYL FUMARATE (UNII: 7CV7WJK4UI) AMMONIA (UNII: 5138Q19F1X) TITANIUM DIOXIDE (UNII: 15FIX9V2JP) STARCH, CORN (UNII: O8232NY3SJ) FERRIC OXIDE RED (UNII: 1K09F3G675) FERROSOFERRIC OXIDE (UNII: XM0M87F357) Product Characteristics Color white (opaque white cap) , pink (opaque pink body) Score no score Shape CAPSULE Size 16mm Flavor Imprint Code H;P3 Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 31722-772-21 21 in 1 BOTTLE; Type 0: Not a Combination Product 02/28/2026 2 NDC: 31722-772-01 100 in 1 BOTTLE; Type 0: Not a Combination Product 02/28/2026 3 NDC: 31722-772-32 6 in 1 CARTON 02/28/2026 3 10 in 1 BLISTER PACK; Type 0: Not a Combination Product Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA210236 02/28/2026 POMALIDOMIDE
pomalidomide capsuleProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 31722-773 Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength POMALIDOMIDE (UNII: D2UX06XLB5) (POMALIDOMIDE - UNII:D2UX06XLB5) POMALIDOMIDE 4 mg Inactive Ingredients Ingredient Name Strength FERROSOFERRIC OXIDE (UNII: XM0M87F357) GELATIN, UNSPECIFIED (UNII: 2G86QN327L) MANNITOL (UNII: 3OWL53L36A) MICROCRYSTALLINE CELLULOSE 101 (UNII: 7T9FYH5QMK) POTASSIUM HYDROXIDE (UNII: WZH3C48M4T) PROPYLENE GLYCOL (UNII: 6DC9Q167V3) SHELLAC (UNII: 46N107B71O) SODIUM STEARYL FUMARATE (UNII: 7CV7WJK4UI) AMMONIA (UNII: 5138Q19F1X) TITANIUM DIOXIDE (UNII: 15FIX9V2JP) STARCH, CORN (UNII: O8232NY3SJ) Product Characteristics Color white (opaque white cap and body) Score no score Shape CAPSULE Size 18mm Flavor Imprint Code H;P4 Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 31722-773-21 21 in 1 BOTTLE; Type 0: Not a Combination Product 02/28/2026 2 NDC: 31722-773-01 100 in 1 BOTTLE; Type 0: Not a Combination Product 02/28/2026 3 NDC: 31722-773-32 6 in 1 CARTON 02/28/2026 3 10 in 1 BLISTER PACK; Type 0: Not a Combination Product Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA210236 02/28/2026 POMALIDOMIDE
pomalidomide capsuleProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 31722-770 Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength POMALIDOMIDE (UNII: D2UX06XLB5) (POMALIDOMIDE - UNII:D2UX06XLB5) POMALIDOMIDE 1 mg Inactive Ingredients Ingredient Name Strength FERROSOFERRIC OXIDE (UNII: XM0M87F357) GELATIN, UNSPECIFIED (UNII: 2G86QN327L) MANNITOL (UNII: 3OWL53L36A) MICROCRYSTALLINE CELLULOSE 101 (UNII: 7T9FYH5QMK) POTASSIUM HYDROXIDE (UNII: WZH3C48M4T) PROPYLENE GLYCOL (UNII: 6DC9Q167V3) SHELLAC (UNII: 46N107B71O) SODIUM STEARYL FUMARATE (UNII: 7CV7WJK4UI) AMMONIA (UNII: 5138Q19F1X) TITANIUM DIOXIDE (UNII: 15FIX9V2JP) STARCH, CORN (UNII: O8232NY3SJ) Product Characteristics Color white (opaque white cap and body) Score no score Shape CAPSULE Size 11mm Flavor Imprint Code H;P1 Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 31722-770-21 21 in 1 BOTTLE; Type 0: Not a Combination Product 02/28/2026 2 NDC: 31722-770-01 100 in 1 BOTTLE; Type 0: Not a Combination Product 02/28/2026 3 NDC: 31722-770-32 6 in 1 CARTON 02/28/2026 3 10 in 1 BLISTER PACK; Type 0: Not a Combination Product Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA210236 02/28/2026 Labeler - Camber Pharmaceuticals, Inc. (826774775) Establishment Name Address ID/FEI Business Operations Hetero Labs Limited Unit V 650452530 manufacture(31722-770, 31722-771, 31722-772, 31722-773)
© 2026 FDA.report
This site is not affiliated with or endorsed by the FDA.



