BETAMETHASONE DIPROPIONATE cream
Betamethasone Dipropionate by
Drug Labeling and Warnings
Betamethasone Dipropionate by is a Prescription medication manufactured, distributed, or labeled by NuCare Pharmaceuticals,Inc., NuCare Pharmaceuticals, Inc.. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
-
HIGHLIGHTS OF PRESCRIBING INFORMATION
These highlights do not include all the information needed to use betamethasone dipropionate safely and effectively. See full prescribing information for betamethasone dipropionate.
BETAMETHASONE DIPROPIONATE Cream, 0.05% (Augmented*), for topical use
Initial U.S. Approval: 1983INDICATIONS AND USAGE
Betamethasone dipropionate cream, 0.05% (augmented) is a corticosteroid indicated for the relief of the inflammatory and pruritic manifestations of corticosteroid-responsive dermatoses in patients 13 years of age and older. ( 1)
DOSAGE AND ADMINISTRATION
- Apply a thin film to the affected skin areas once or twice daily. ( 2)
- Discontinue therapy when control is achieved. ( 2)
- Use no more than 50 g per week. ( 2)
- Do not use with occlusive dressings unless directed by a physician. ( 2)
- Avoid use on the face, groin, or axillae, or if skin atrophy is present at the treatment site. ( 2)
- Not for oral, ophthalmic, or intravaginal use. ( 2)
DOSAGE FORMS AND STRENGTHS
- Cream, 0.05% ( 3)
CONTRAINDICATIONS
- Hypersensitivity to any component of this medicine. ( 4)
WARNINGS AND PRECAUTIONS
- Effects on endocrine system: Betamethasone dipropionate cream, 0.5% (augmented) can cause reversible HPA axis suppression with the potential for glucocorticosteroid insufficiency during and after withdrawal of treatment. Risk factor(s) include the use of high-potency topical corticosteroids, use over a large surface area or to areas under occlusion, prolonged use, altered skin barrier, liver failure, and use in pediatric patients. Modify use should HPA axis suppression develop. ( 5.1, 8.4)
ADVERSE REACTIONS
- The most common adverse reaction reported in 0.4% of adult patients is stinging. ( 6.1)
- The most common adverse reactions reported in 10% of pediatric patients are signs of skin atrophy, telangiectasia, bruising, shininess. ( 6.1, 8.4)
To report SUSPECTED ADVERSE REACTIONS, contact Glenmark Pharmaceuticals Inc., USA at 1 (888)721-7115 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
See 17 for PATIENT COUNSELING INFORMATION.
Revised: 10/2015
-
Table of Contents
FULL PRESCRIBING INFORMATION: CONTENTS*
1 INDICATIONS AND USAGE
2 DOSAGE AND ADMINISTRATION
3 DOSAGE FORMS AND STRENGTHS
4 CONTRAINDICATIONS
5 WARNINGS AND PRECAUTIONS
5.1 Effects on Endocrine System
5.2 Allergic Contact Dermatitis
6 ADVERSE REACTIONS
6.1 Clinical Trials Experience
6.2 Postmarketing Experience
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
8.3 Nursing Mothers
8.4 Pediatric Use
8.5 Geriatric Use
11 DESCRIPTION
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
12.2 Pharmacodynamics
12.3 Pharmacokinetics
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
14 CLINICAL STUDIES
16 HOW SUPPLIED/STORAGE AND HANDLING
17 PATIENT COUNSELING INFORMATION
- * Sections or subsections omitted from the full prescribing information are not listed.
- 1 INDICATIONS AND USAGE
-
2 DOSAGE AND ADMINISTRATION
Apply a thin film of betamethasone dipropionate cream, 0.5% (augmented) to the affected skin areas once or twice daily. Therapy should be discontinued when control is achieved. Betamethasone dipropionate cream, 0.5% (augmented)is a high-potency corticosteroid. Treatment with betamethasone dipropionate cream, 0.5% (augmented)should not exceed 50 g per week because of the potential for the drug to suppress the hypothalamic-pituitary-adrenal (HPA) axis.
Betamethasone dipropionate cream, 0.5% (augmented)should not be used with occlusive dressings unless directed by a physician.
Betamethasone dipropionate cream, 0.5% (augmented)is for topical use only. It is not for oral, ophthalmic, or intravaginal use.
Avoid use on the face, groin, or axillae, or if skin atrophy is present at the treatment site.
- 3 DOSAGE FORMS AND STRENGTHS
- 4 CONTRAINDICATIONS
-
5 WARNINGS AND PRECAUTIONS
5.1 Effects on Endocrine System
Betamethasone dipropionate cream, 0.5% (augmented) can produce reversible hypothalamic-pituitary-adrenal (HPA) axis suppression with the potential for glucocorticosteroid insufficiency. This may occur during treatment or after withdrawal of treatment. Factors that predispose to HPA axis suppression include the use of high-potency steroids, large treatment surface areas, prolonged use, use of occlusive dressings, altered skin barrier, liver failure, and young age. Evaluation for HPA axis suppression may be done by using the adrenocorticotropic hormone (ACTH) stimulation test.
Betamethasone dipropionate cream, 0.5% (augmented) was applied once daily at 7 grams per day for 1 week to diseased skin, in adult subjects with psoriasis or atopic dermatitis, to study its effects on the HPA axis. The results suggested that the drug lowered adrenal corticosteroid secretion, although plasma cortisol levels did not go below the lower limit of the normal range.
In an open-label pediatric trial of 60 evaluable subjects (3 months to 12 years of age), 19 subjects showed evidence of HPA axis suppression. Four (4) subjects were tested 2 weeks after discontinuation of betamethasone dipropionate cream, 0.5% (augmented) and 3 of the 4 (75%) had complete rehcovery of HPA axis function. The proportion of subjects with adrenal suppression in this trial was progressively greater, the younger the age group.
If HPA axis suppression is documented, gradually withdraw the drug, reduce the frequency of application, or substitute with a less potent corticosteroid. Infrequently, signs and symptoms of steroid withdrawal may occur, requiring supplemental systemic corticosteroids.
Cushing’s syndrome and hyperglycemia may also occur with topical corticosteroids. These events are rare and generally occur after prolonged exposure to excessively large doses, especially of high-potency topical corticosteroids.
Pediatric patients may be more susceptible to systemic toxicity due to their larger skin surface to body mass ratios [see Use in Specific Populations (8.4)] .
5.2 Allergic Contact Dermatitis
Allergic contact dermatitis with corticosteroids is usually diagnosed by observing failure to heal rather than noting a clinical exacerbation. Such an observation should be corroborated with appropriate diagnostic patch testing. If irritation develops, topical corticosteroids should be discontinued and appropriate therapy instituted.
-
6 ADVERSE REACTIONS
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
In controlled clinical trials, involving 242 adult subjects, the adverse reaction associated with the use of betamethasone dipropionate cream, 0.5% (augmented)reported at a frequency of 0.4% was stinging. It occurred in 1 subject.
In a controlled clinical trial involving 67 pediatric subjects from 3 months to 12 years of age, the adverse reactions associated with the use of betamethasone dipropionate cream, 0.5% (augmented)occurred in 7 of 67 (10%) subjects. Reported reactions included signs of skin atrophy (telangiectasia, bruising, shininess).
6.2 Postmarketing Experience
Because adverse reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Postmarketing reports for local adverse reactions to topical corticosteroids may also include: burning, itching, irritation, dryness, folliculitis, acneiform eruptions, hypopigmentation, perioral dermatitis, allergic contact dermatitis, secondary infection, hypertrichosis, skin atrophy, striae, and miliaria.
Hypersensitivity reactions, consisting of predominantly skin signs and symptoms, e.g., contact dermatitis, pruritus, bullous dermatitis, and erythematous rash have been reported.
-
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Teratogenic Effects: Pregnancy Category C
There are no adequate and well-controlled studies in pregnant women. Betamethasone dipropionate cream, 0.5% (augmented)should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
Betamethasone dipropionate has been shown to be teratogenic in rabbits when given by the intramuscular route at doses of 0.05 mg/kg. The abnormalities observed included umbilical hernias, cephalocele, and cleft palate.
8.3 Nursing Mothers
Systemically administered corticosteroids appear in human milk and can suppress growth, interfere with endogenous corticosteroid production, or cause other untoward effects. It is not known whether topical administration of corticosteroids can result in sufficient systemic absorption to produce detectable quantities in human milk. Because many drugs are excreted in human milk, caution should be exercised when betamethasone dipropionate cream, 0.5% (augmented)is administered to a nursing woman.
8.4 Pediatric Use
Use of betamethasone dipropionate cream, 0.5% (augmented)in pediatric patients younger than 13 years of age is not recommended due to the potential for HPA axis suppression [see Warnings and Precautions (5.1)] .
In an open-label HPA axis safety trial in subjects 3 months to 12 years of age with atopic dermatitis, betamethasone dipropionate cream, 0.5% (augmented) was applied twice daily for 2 to 3 weeks over a mean body surface area of 58% (range 35% to 95%). In 19 of 60 (32%) evaluable subjects, adrenal suppression was indicated by either a ≤5 mcg/dL pre-stimulation cortisol, or a cosyntropin post-stimulation cortisol ≤18 mcg/dL and/or an increase of <7 mcg/dL from the baseline cortisol. Out of the 19 subjects with HPA axis suppression, 4 subjects were tested 2 weeks after discontinuation of betamethasone dipropionate cream, 0.5% (augmented) and 3 of the 4 (75%) had complete recovery of HPA axis function. The proportion of subjects with adrenal suppression in this trial was progressively greater, the younger the age group [see Warnings and Precautions (5.1)] .
Because of a higher ratio of skin surface area to body mass, pediatric patients are at a greater risk than adults of systemic toxicity when treated with topical drugs. They are, therefore, also at greater risk of HPA axis suppression and adrenal insufficiency upon the use of topical corticosteroids.
Rare systemic effects such as Cushing's syndrome, linear growth retardation, delayed weight gain, and intracranial hypertension have been reported in pediatric patients, especially those with prolonged exposure to large doses of high potency topical corticosteroids.
Local adverse reactions including skin atrophy have also been reported with use of topical corticosteroids in pediatric patients.
Avoid use of betamethasone dipropionate cream, 0.5% (augmented)in the treatment of diaper dermatitis.
8.5 Geriatric Use
Clinical trials of betamethasone dipropionate, 0.5% (augmented)included 104 subjects who were 65 years of age and over and 8 subjects who were 75 years of age and over. No overall differences in safety or effectiveness were observed between these subjects and younger subjects, and other reported clinical experience has not identified differences in responses between the elderly and younger patients. However, greater sensitivity of some older individuals cannot be ruled out.
-
11 DESCRIPTION
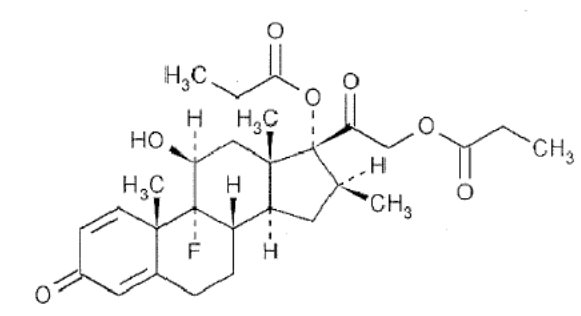
Betamethasone dipropionate cream, 0.05% (augmented) contains betamethasone dipropionate USP, a synthetic adrenocorticosteroid, for topical use in an emollient cream base. Betamethasone, an analog of prednisolone, has a high degree of corticosteroid activity and a slight degree of mineralocorticoid activity. Betamethasone dipropionate is the 17,21-dipropionate ester of betamethasone.
Chemically, betamethasone dipropionate USP is 9-fluoro-11β,17,21-trihydroxy-16β-methylpregna-1,4diene-3,20-dione 17,21-dipropionate, with the empirical formula C 28 H 37 FO 7, a molecular weight of 504.6, and the following structural formula:
Betamethasone dipropionate USP is a white or almost white crystalline powder, practically insoluble in water, freely soluble in acetone and in methylene chloride, sparingly soluble in alcohol.
Each gram of betamethasone dipropionate cream, 0.05% (augmented) contains: 0.643 mg betamethasone dipropionate USP (equivalent to 0.5 mg betamethasone) in a white to off-white emollient cream base of carbomer homopolymer, ceteareth-30, chlorocresol, cyclomethicone, glyceryl oleate/propylene glycol, purified water, propylene glycol, sodium hydroxide, sorbitol solution, white petrolatum and white wax.
-
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Corticosteroids play a role in cellular signaling, immune function, inflammation, and protein regulation; however, the precise mechanism of action of betamethasone dipropionate cream, 0.5% (augmented)in corticosteroid responsive dermatoses is unknown.
12.2 Pharmacodynamics
Vasoconstrictor Assay
Trials performed with betamethasone dipropionate cream, 0.5% (augmented) indicate that it is in the high range of potency as demonstrated in vasoconstrictor trials in healthy subjects when compared with other topical corticosteroids. However, similar blanching scores do not necessarily imply therapeutic equivalence.
12.3 Pharmacokinetics
No pharmacokinetics trials have been conducted with betamethasone dipropionate cream, 0.5% (augmented). The extent of percutaneous absorption of topical corticosteroids is determined by many factors including the vehicle, the integrity of the epidermal barrier, and the use of occlusive dressings [see Dosage and Administration (2)] .
Topical corticosteroids can be absorbed through normal intact skin. Inflammation and/or other disease processes in the skin may increase percutaneous absorption. Occlusive dressings substantially increase the percutaneous absorption of topical corticosteroids [see Dosage and Administration (2)] .
Once absorbed through the skin, topical corticosteroids enter pharmacokinetic pathways similar to systemically administered corticosteroids. Corticosteroids are bound to plasma proteins in varying degrees, are metabolized primarily in the liver, and excreted by the kidneys. Some of the topical corticosteroids and their metabolites are also excreted into the bile.
-
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Long-term animal studies have not been performed to evaluate the carcinogenic potential of betamethasone dipropionate.
Betamethasone was negative in the bacterial mutagenicity assay (Salmonella typhimurium and Escherichia coli), and in the mammalian cell mutagenicity assay (CHO/HGPRT). It was positive in the in vitro human lymphocyte chromosome aberration assay, and equivocal in the in vivo mouse bone marrow micronucleus assay.
Studies in rabbits, mice, and rats using intramuscular doses up to 1, 33, and 2 mg/kg, respectively, resulted in dose-related increases in fetal resorptions in rabbits and mice.
-
14 CLINICAL STUDIES
The safety and efficacy of betamethasone dipropionate cream, 0.5% (augmented)for the treatment of corticosteroid-responsive dermatoses have been established in two randomized and active controlled trials in subjects with chronic plaque psoriasis. A total of 81 subjects who received betamethasone dipropionate cream, 0.5% (augmented) were included in these trials. These trials evaluated betamethasone dipropionate cream, 0.5% (augmented)applied once or twice daily for 14 and 21 days, respectively, on bilateral paired psoriatic lesions. Betamethasone dipropionate cream, 0.5% (augmented)was shown to be effective in relieving the signs and symptoms of chronic plaque psoriasis.
-
16 HOW SUPPLIED/STORAGE AND HANDLING
Betamethasone dipropionate cream, 0.05% (augmented) is a white to off-white cream supplied in 15 g (NDC: 68071-1657-5)
Store at 25°C (77°F); excursions permitted to 15 to 30°C (59 to 86°F) [see USP Controlled Room Temperature].
-
17 PATIENT COUNSELING INFORMATION
Inform patients of the following:
- Discontinue therapy when control is achieved, unless directed otherwise by the physician.
- Use no more than 50 grams per week.
- Avoid contact with the eyes.
- Avoid use of betamethasone dipropionate cream, 0.5% (augmented)on the face, underarms, or groin areas unless directed by the physician.
- Do not occlude the treatment area with bandage or other covering, unless directed by the physician.
- Note that local reactions and skin atrophy are more likely to occur with occlusive use, prolonged use or use of higher potency corticosteroids.
Manufactured by:
Glenmark Pharmaceuticals Ltd.
Village: Kishanpura, Baddi Nalagarh Road
District: Solan, Himachal Pradesh – 174101, IndiaManufactured for:
Glenmark Pharmaceuticals Inc., USA
Mahwah, NJ 07430Questions? 1 (888)721-7115
www.glenmarkpharma.com/usaFebruary 2015
- PACKAGE/LABEL PRINCIPAL DISPLAY PANEL
-
INGREDIENTS AND APPEARANCE
BETAMETHASONE DIPROPIONATE
betamethasone dipropionate creamProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 68071-1657(NDC:68462-290) Route of Administration TOPICAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength BETAMETHASONE DIPROPIONATE (UNII: 826Y60901U) (BETAMETHASONE - UNII:9842X06Q6M) BETAMETHASONE 0.5 mg in 1 g Inactive Ingredients Ingredient Name Strength CARBOMER HOMOPOLYMER TYPE C (ALLYL PENTAERYTHRITOL CROSSLINKED) (UNII: 4Q93RCW27E) CETEARETH-30 (UNII: 1R9DCZ5FOX) CHLOROCRESOL (UNII: 36W53O7109) CYCLOMETHICONE (UNII: NMQ347994Z) PROPYLENE GLYCOL (UNII: 6DC9Q167V3) SODIUM HYDROXIDE (UNII: 55X04QC32I) SORBITOL (UNII: 506T60A25R) PETROLATUM (UNII: 4T6H12BN9U) WHITE WAX (UNII: 7G1J5DA97F) Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 68071-1657-5 15 g in 1 BOX; Type 0: Not a Combination Product 07/12/2017 Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA078930 09/23/2008 Labeler - NuCare Pharmaceuticals,Inc. (010632300) Establishment Name Address ID/FEI Business Operations NuCare Pharmaceuticals, Inc. 010632300 relabel(68071-1657)
© 2026 FDA.report
This site is not affiliated with or endorsed by the FDA.