RYKINDO EXTENDED-RELEASE MICROSPHERES- risperidone kit
Rykindo by
Drug Labeling and Warnings
Rykindo by is a Prescription medication manufactured, distributed, or labeled by Shandong Luye Pharmaceutical Co., Ltd.. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
-
HIGHLIGHTS OF PRESCRIBING INFORMATION
These highlights do not include all the information needed to use RYKINDO® safely and effectively. See full prescribing information for RYKINDO®.
RYKINDO® (risperidone) for extended-release injectable suspension, for intramuscular use
Initial U.S. Approval: 1993WARNING: INCREASED MORTALITY IN ELDERLY PATIENTS WITH DEMENTIA-RELATED PSYCHOSIS
See full prescribing information for complete boxed warning.
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. RYKINDO is not approved for use in patients with dementia-related psychosis. (5.1)
INDICATIONS AND USAGE
DOSAGE AND ADMINISTRATION
- Establish tolerability with oral risperidone prior to initiating treatment with RYKINDO. (2.1)
- Administer RYKINDO by intramuscular (IM) injection in the gluteal muscle by a healthcare provider. Do not administer by any other route. (2.1)
- Recommended dosage of RYKINDO is 25 mg intramuscular (IM) every 2 weeks. Patients not responding to 25 mg may benefit from 37.5 mg or 50 mg. Dosage titration should not be made more frequently than every 4 weeks. The maximum recommended dosage should not exceed 50 mg every 2 weeks. (2.2, 2.3)
- Administer the first dose of RYKINDO along with 7 days of oral risperidone. (2.2, 2.3)
- Renal or Hepatic Impairment: Titrate with oral risperidone up to at least 2 mg prior to initiating treatment with RYKINDO. (2.6)
- See Full Prescribing Information for important preparation and administration instructions. (2.8)
DOSAGE FORMS AND STRENGTHS
For extended-release injectable suspension: 25 mg, 37.5 mg, and 50 mg. (3)
CONTRAINDICATIONS
Known hypersensitivity to risperidone, paliperidone, or to any components in RYKINDO. (4)
WARNINGS AND PRECAUTIONS
- Cerebrovascular Adverse Reactions in Elderly Patients with Dementia-Related Psychosis: Increased risk of cerebrovascular adverse reactions (e.g., stroke, transient ischemia attack). (5.2)
- Neuroleptic Malignant Syndrome (NMS): Manage with immediate discontinuation and close monitoring. (5.3)
- Tardive Dyskinesia: Discontinue treatment if clinically appropriate. (5.4)
- Metabolic Changes: Monitor for hyperglycemia/diabetes mellitus, dyslipidemia, and weight gain. (5.5)
- Hyperprolactinemia: Prolactin elevations occur and persist during chronic administration. Long-standing hyperprolactinemia, when associated with hypogonadism, can lead to decreased bone density in males and females. (5.6)
- Orthostatic Hypotension and Syncope: Monitor heart rate and blood pressure and warn patients with known cardiovascular disease or cerebrovascular disease, and risk of dehydration or syncope. (5.7)
- Leukopenia, Neutropenia, and Agranulocytosis: Perform complete blood cell counts (CBC) in patients with a history of clinically significant low white blood cell count (WBC) or history of leukopenia or neutropenia. Consider discontinuing RYKINDO if clinically significant decline in WBC occurs in the absence of other causative factors. (5.9)
- Potential for Cognitive and Motor Impairment: Use caution when operating machinery. (5.10)
- Seizures: Use cautiously in patients with a history of seizures or with conditions that potentially lower the seizure threshold. (5.11)
- Priapism: Priapism has been reported during postmarketing use of other risperidone products. Severe priapism may require surgical intervention. (5.13)
ADVERSE REACTIONS
The most common adverse reactions in patients with schizophrenia (≥ 5%) were headache, parkinsonism, dizziness, akathisia, fatigue, constipation, dyspepsia, sedation, weight increase, pain in extremity, and dry mouth. (6)
The most common adverse reactions in patients with bipolar disorder were (5% in monotherapy trial) weight increased and (≥ 10% in adjunctive therapy trial) tremor and parkinsonism. (6)
To report SUSPECTED ADVERSE REACTIONS, contact Shandong Luye Pharmaceutical Co., Ltd. at 1-800-548-9765 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
DRUG INTERACTIONS
USE IN SPECIFIC POPULATIONS
Pregnancy: May cause extrapyramidal and/or withdrawal symptoms in neonates with third trimester exposure. (8.1)
See 17 for PATIENT COUNSELING INFORMATION.
Revised: 1/2026
-
Table of Contents
FULL PRESCRIBING INFORMATION: CONTENTS*
WARNING: INCREASED MORTALITY IN ELDERLY PATIENTS WITH DEMENTIA-RELATED PSYCHOSIS
1 INDICATIONS AND USAGE
2 DOSAGE AND ADMINISTRATION
2.1 General Administration Information
2.2 Dosage Recommendations for the Treatment of Schizophrenia
2.3 Dosage Recommendations for Maintenance Treatment of Bipolar I Disorder
2.4 Patients Currently Receiving Risperidone Long-acting Injection 2-week Intramuscular Formulation (e.g., Risperdal Consta)
2.5 Reinitiation of Treatment in Patients Previously Discontinued
2.6 Dosage Recommendations for Patients with Renal or Hepatic Impairment
2.7 Dosage Recommendations for Concomitant Use of RYKINDO with Strong CYP2D6 Inhibitors and Strong CYP3A4 Inducers
2.8 Preparation and Administration Instructions
3 DOSAGE FORMS AND STRENGTHS
4 CONTRAINDICATIONS
5 WARNINGS AND PRECAUTIONS
5.1 Increased Mortality in Elderly Patients with Dementia-Related Psychosis
5.2 Cerebrovascular Adverse Reactions, Including Stroke, in Elderly Patients with Dementia-Related Psychosis
5.3 Neuroleptic Malignant Syndrome (NMS)
5.4 Tardive Dyskinesia
5.5 Metabolic Changes
5.6 Hyperprolactinemia
5.7 Orthostatic Hypotension and Syncope
5.8 Falls
5.9 Leukopenia, Neutropenia, and Agranulocytosis
5.10 Potential for Cognitive and Motor Impairment
5.11 Seizures
5.12 Dysphagia
5.13 Priapism
5.14 Body Temperature Dysregulation
5.15 Osteodystrophy and Tumors in Animals
6 ADVERSE REACTIONS
6.1 Clinical Trials Experience
6.2 Postmarketing Experience
7 DRUG INTERACTIONS
7.1 Drugs Having Clinically Significant Interactions with RYKINDO
7.2 Drugs Having No Clinically Important Interactions with RYKINDO
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
8.2 Lactation
8.3 Females and Males of Reproductive Potential
8.4 Pediatric Use
8.5 Geriatric Use
8.6 Renal Impairment
8.7 Hepatic Impairment
8.8 Patients with Parkinson's Disease or Dementia with Lewy Bodies
10 OVERDOSAGE
11 DESCRIPTION
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
12.2 Pharmacodynamics
12.3 Pharmacokinetics
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
14 CLINICAL STUDIES
14.1 Schizophrenia
14.2 Bipolar Disorder - Monotherapy
14.3 Bipolar Disorder - Adjunctive Therapy
16 HOW SUPPLIED/STORAGE AND HANDLING
17 PATIENT COUNSELING INFORMATION
- * Sections or subsections omitted from the full prescribing information are not listed.
-
BOXED WARNING
(What is this?)
WARNING: INCREASED MORTALITY IN ELDERLY PATIENTS WITH DEMENTIA-RELATED PSYCHOSIS
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. RYKINDO is not approved for the treatment of patients with dementia-related psychosis [see Warnings and Precautions (5.1)].
- 1 INDICATIONS AND USAGE
-
2 DOSAGE AND ADMINISTRATION
2.1 General Administration Information
For patients who have never taken oral risperidone, establish tolerability with oral risperidone prior to initiating RYKINDO.
RYKINDO should be administered every 2 weeks by intramuscular (IM) gluteal injection. Each injection should be administered by a health care professional. Do not administer by any other route. Alternate injections between the two buttocks. Do not combine two different dose strengths of RYKINDO in a single administration.
For detailed preparation and administration instructions, see Dosage and Administration (2.8).
2.2 Dosage Recommendations for the Treatment of Schizophrenia
The recommended dosage of RYKINDO for the treatment of schizophrenia is 25 mg every 2 weeks. Administer the first dose of RYKINDO along with 7 days of oral risperidone.
Patients not responding to 25 mg may benefit from a higher dose of 37.5 mg or 50 mg. The maximum dose should not exceed 50 mg every 2 weeks. No additional benefit was observed with dosages greater than 50 mg of risperidone long-acting injection (intramuscular); however, a higher incidence of adverse reactions was observed. Dose titration should not be made more frequently than every 4 weeks.
2.3 Dosage Recommendations for Maintenance Treatment of Bipolar I Disorder
The recommended dosage of RYKINDO for monotherapy or adjunctive therapy to lithium or valproate for the maintenance treatment of bipolar I disorder is 25 mg every 2 weeks. Administer the first dose of RYKINDO along with 7 days of oral risperidone.
Some patients may benefit from a higher dose of 37.5 mg or 50 mg. Dosages above 50 mg have not been studied in this population. Dose titration should not be made more frequently than every 4 weeks.
2.4 Patients Currently Receiving Risperidone Long-acting Injection 2-week Intramuscular Formulation (e.g., Risperdal Consta)
The RYKINDO dose for patients receiving a risperidone long-acting injection (intramuscular) every two week formulation (e.g., Risperdal Consta) should be the same as that of the previous treatment. The first injection of RYKINDO should be given 4 weeks (no later than 5 weeks) after the last injection of the previous treatment. Supplementation with oral risperidone is not recommended [see Clinical Pharmacology (12.3)]. Titration should not be made more frequently than every 4 weeks.
2.5 Reinitiation of Treatment in Patients Previously Discontinued
There are no data to specifically address reinitiation of treatment. When restarting patients who have had an interval off treatment with RYKINDO, the previously established dosage should be reinitiated if there has been no change in the patient's general medical condition. Supplementation with oral risperidone is also required.
2.6 Dosage Recommendations for Patients with Renal or Hepatic Impairment
Patients with renal or hepatic impairment should be treated with titrated oral risperidone prior to initiating treatment with RYKINDO [see Use in Specific Populations (8.6, 8.7) and Clinical Pharmacology (12.3)]. The recommended starting dose is 0.5 mg oral risperidone twice daily during the first week, which can be increased to 1 mg twice daily or 2 mg once daily during the second week. If a total daily dose of at least 2 mg oral risperidone is well tolerated, RYKINDO 25 mg can be administered every 2 weeks with oral supplementation for 7 days following the first injection [see Dosing and Administration (2.2, 2.3)]. In some patients, slower titration may be appropriate.
2.7 Dosage Recommendations for Concomitant Use of RYKINDO with Strong CYP2D6 Inhibitors and Strong CYP3A4 Inducers
Co-administration of carbamazepine and other CYP3A4 enzyme inducers (e.g., phenytoin, rifampin, phenobarbital) with risperidone would be expected to cause decreases in the plasma concentrations of the sum of risperidone and 9-hydroxyrisperidone combined, which could lead to decreased efficacy of RYKINDO treatment. The risperidone dose needs to be titrated accordingly for patients receiving these enzyme inducers, especially during initiation or discontinuation of therapy with these inducers [see Drug Interactions (7.1)]. At the initiation of therapy with carbamazepine or other known CYP3A4 hepatic enzyme inducers, patients should be closely monitored during the first 1 to 2 months because the dose of RYKINDO may need to be adjusted. A dose increase, or additional oral risperidone, needs to be considered. On discontinuation of carbamazepine or other CYP3A4 hepatic enzyme inducers, the dosage of RYKINDO should be re-evaluated and, if necessary, decreased. Patients may be placed on a lower dose of RYKINDO between 2 to 4 weeks before the planned discontinuation of carbamazepine or other CYP3A4 inducers to adjust for the expected increase in plasma concentrations of risperidone plus 9-hydroxyrisperidone. For patients treated with the recommended dose of 25 mg RYKINDO and discontinuing from carbamazepine or other CYP3A4 enzyme inducers, it is recommended to continue treatment with the 25-mg dose unless clinical judgment necessitates either lowering the dose to 12.5 mg, in which case a different risperidone long-acting injection intramuscular formulation should be used, or interruption of RYKINDO treatment.
Fluoxetine and paroxetine, CYP2D6 inhibitors, have been shown to increase the plasma concentration of risperidone by 2.5 to 2.8-fold and 3 to 9-fold, respectively. Fluoxetine did not affect the plasma concentration of 9-hydroxyrisperidone. Paroxetine lowered the concentration of 9-hydroxyrisperidone by about 10%. The dose of risperidone needs to be titrated accordingly when co-administering fluoxetine or paroxetine. When either concomitant fluoxetine or paroxetine is initiated or discontinued, the physician should re-evaluate the dose of RYKINDO. When initiation of fluoxetine or paroxetine is considered, patients may be placed on a lower dose of RYKINDO between 2 to 4 weeks before the planned start of fluoxetine or paroxetine therapy to adjust for the expected increase in plasma concentrations of risperidone. When fluoxetine or paroxetine is initiated in patients receiving the recommended dose of 25 mg RYKINDO it is recommended to continue treatment with the 25 mg dose unless clinical judgment necessitates either lowering the dose to 12.5 mg, in which case a different risperidone long-acting injection intramuscular formulation should be used, or interruption of RYKINDO treatment. The effects of discontinuation of concomitant fluoxetine or paroxetine therapy on the pharmacokinetics of risperidone and 9-hydroxyrisperidone have not been studied [see Drug Interactions (7.1)].
2.8 Preparation and Administration Instructions
- Read the instructions for preparation and administration below and consider referring to the separate Healthcare Provider "Instructions for Use" for additional preparation and administration considerations.
- For gluteal intramuscular injection only. Do not inject by any other route. Alternate injections between the two buttocks.
- Allow package to come to room temperature for at least 30 minutes prior to preparation. Prepare medication when you are ready to administer the dose.
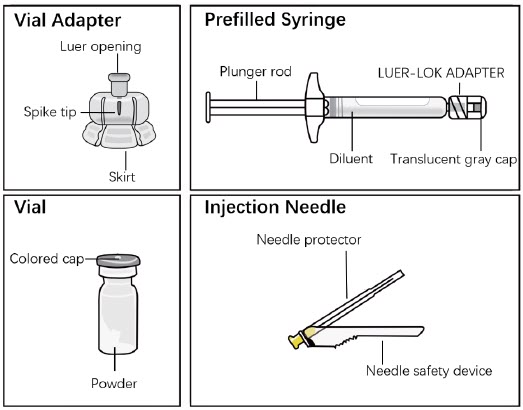
- The components in the single-dose kit are shown in Figure 1.
Figure 1. Single-dose Kit Components
Step 1. Take out kit and connect vial adapter to vial
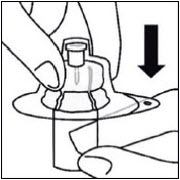
Wait 30 minutes
Remove dose pack from the refrigerator and allow to sit at room temperature for at least 30 minutes before reconstituting.
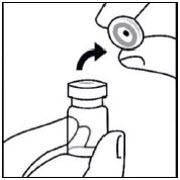
Do not warm any other way.Remove cap from vial
Flip off colored cap from vial.
Wipe top of the gray stopper with an alcohol swab. Allow to air dry.
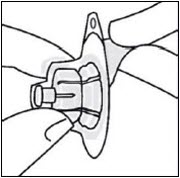
Do not remove gray rubber stopper.Prepare vial adapter
Hold sterile blister as shown. Peel back and remove paper backing.
Do not remove vial adapter from blister.
Do not touch spike tip at any time. This will result in contamination.Connect vial adapter to vial
Place vial on a hard surface and hold by the base. Center vial adapter over the gray rubber stopper. Push vial adapter straight down onto vial top until it snaps securely into place.
Do not place vial adapter on at an angle or diluent may leak upon transfer to the vial.
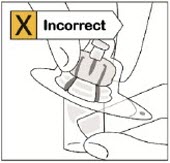
Step 2. Connect prefilled syringe to vial adapter
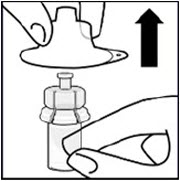
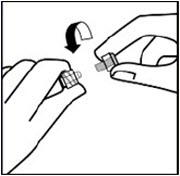
Remove sterile blister

Keep vial vertical to prevent leakage. Hold base of vial and pull up on the sterile blister to remove.
Do not shake.
Do not touch exposed luer opening on vial adapter.
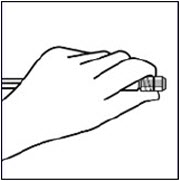
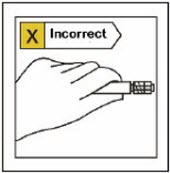
This will result in contamination.Use proper grip
Hold by the LUER-LOK ADAPTER at the tip of the syringe.
Do not hold syringe by the glass barrel during assembly.
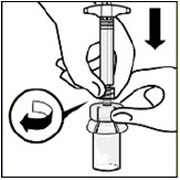
Remove cap
Holding the transparent LUER-LOK ADAPTER, unscrew the translucent gray cap
Do not snap or cut off the translucent gray cap
Do not touch syringe tip. This will result in contamination.
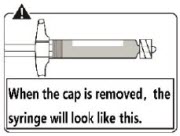
The unscrewed cap can be discarded.Connect syringe to vial adapter
Hold vial adapter by skirt to keep stationary.
Hold syringe by the LUER-LOK ADAPTER then turn it to connect with the luer opening of the vial adapter
Do not hold the glass syringe barrel. This may cause the LUER-LOK ADAPTER to loosen or detach.
Attach the syringe to the vial adapter with a firm clockwise twisting motion until it feels snug.
Do not over-tighten. Over-tightening may cause the syringe tip to break.Step 3. Reconstitute powder
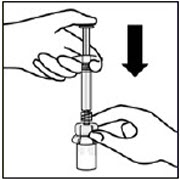
Inject diluent
Inject entire amount of diluent from syringe into the vial.

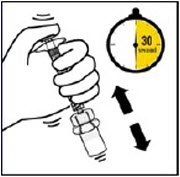
Suspend Powder in diluent
Continuing to hold down the plunger rod, shake vigorously for at least 30 seconds, as shown.
Check the suspension. When properly mixed, the suspension appears uniform, thick and milky in color.
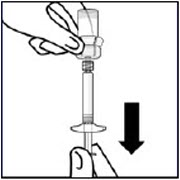
Immediately proceed to the next step so suspension does not settle.Transfer suspension to syringe
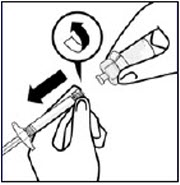
Invert vial completely. Slowly pull plunger rod down to withdraw entire contents from the vial into the syringe.Remove vial adapter
Hold LUER-LOK ADAPTER on the syringe and unscrew from vial adapter.
Tear section of the vial label at the perforation. Apply detached label to the syringe for identification purposes.
Discard both vial and vial adapter appropriately.Step 4. Attach Needle
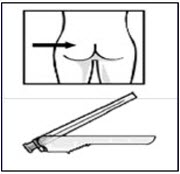
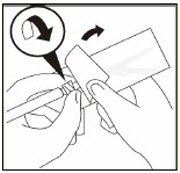
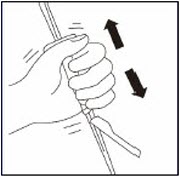
Take out needle
Take out needle for gluteal injection.Attach needle
Peel blister pouch open part way and use to grasp the base of the needle, as shown.
Holding the LUER-LOK ADAPTER on the syringe, attach syringe to needle luer connection with a firm clockwise twisting motion until snug.
Do not touch needle luer opening. This will result in contamination.Resuspend Powder
Fully remove the blister pouch.
Just before injection, shake syringe vigorously for 20 to 30 seconds until there is no deposition of powder, as some settling will have occurred.Step 5. Inject RYKINDO
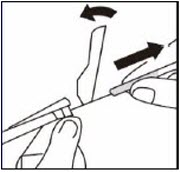
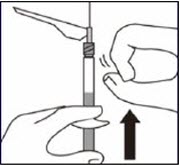
Remove transparent needle protector
Move the needle safety device back towards the syringe, as shown. Then hold the LUER-LOK ADAPTER on syringe and carefully pull the transparent needle protector straight off.
Do not twist transparent needle protector, as the luer connection may loosen.Remove air bubbles
Hold syringe upright and tap gently to make any air bubbles rise to the top.
Slowly and carefully press plunger rod upward to remove air.Inject
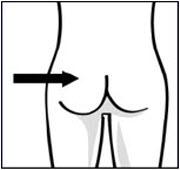
Immediately inject entire contents of syringe intramuscularly into the upper-outer quadrant of the gluteal muscle of the patient.Secure needle in safety device
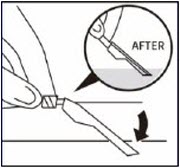
Using one hand, place needle safety device at a 45-degree angle on a hard, flat surface. Press down with a firm, quick motion until needle is fully engaged in safety device.Properly dispose of syringes
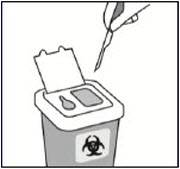
Check to confirm needle safety device is fully engaged.
Discard in an approved sharps container. -
3 DOSAGE FORMS AND STRENGTHS
RYKINDO (risperidone) for extended-release injectable suspension, for intramuscular use is available in strengths of 25 mg, 37.5 mg, and 50 mg.
Each strength is provided as a single-dose kit consisting of: a vial containing a white to almost white powder, a pre-filled syringe containing 2 mL of a colorless, clear diluent, a vial adapter, and a needle (20 gauge 2-inch needle with needle protection device).
- 4 CONTRAINDICATIONS
-
5 WARNINGS AND PRECAUTIONS
5.1 Increased Mortality in Elderly Patients with Dementia-Related Psychosis
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. Analyses of 17 placebo-controlled trials (modal duration of 10 weeks), largely in patients taking atypical antipsychotic drugs, revealed a risk of death in drug-treated patients that was 1.6 to 1.7 times the risk of death in placebo-treated patients. Over the course of a typical 10-week controlled trial, the rate of death in drug-treated patients was about 4.5% versus about 2.6% in the placebo group. Although the causes of death were varied, most of the deaths appeared to be either cardiovascular (e.g., heart failure, sudden death) or infectious (e.g., pneumonia) in nature. Observational studies suggest that, similar to atypical antipsychotic drugs, treatment with conventional antipsychotic drugs may increase mortality. The extent to which the findings of increased mortality in observational studies may be attributed to the antipsychotic drug as opposed to some characteristic(s) of the patients is not clear.
RYKINDO is not approved for the treatment of dementia-related psychosis [see Boxed Warning and Warnings and Precautions (5.2)].
5.2 Cerebrovascular Adverse Reactions, Including Stroke, in Elderly Patients with Dementia-Related Psychosis
Cerebrovascular adverse reactions (e.g., stroke, transient ischemic attack), including fatalities, were reported in patients (mean age 85 years; range 73 to 97) in trials of oral risperidone in elderly patients with dementia-related psychosis. In placebo-controlled trials, there was a significantly higher incidence of cerebrovascular adverse reactions in patients treated with oral risperidone compared to patients treated with placebo. RYKINDO is not approved for the treatment of patients with dementia-related psychosis [see Warnings and Precautions (5.1)].
5.3 Neuroleptic Malignant Syndrome (NMS)
NMS, a potentially fatal symptom complex, has been reported in association with antipsychotic drugs. Clinical manifestations of NMS are hyperpyrexia, muscle rigidity, altered mental status including delirium, and autonomic instability (irregular pulse or blood pressure, tachycardia, diaphoresis, and cardiac dysrhythmia). Additional signs may include elevated creatine phosphokinase, myoglobinuria (rhabdomyolysis), and acute renal failure.
If NMS is suspected, immediately discontinue RYKINDO and provide symptomatic treatment and monitoring.
5.4 Tardive Dyskinesia
Tardive dyskinesia, a syndrome consisting of potentially irreversible, involuntary, dyskinetic movements, may develop in patients treated with antipsychotic drugs. Although the prevalence of the syndrome appears to be highest among the elderly, especially elderly women, it is impossible to predict which patients will develop the syndrome. Whether antipsychotic drug products differ in their potential to cause tardive dyskinesia is unknown.
The risk of developing tardive dyskinesia and the likelihood that it will become irreversible increase with the duration of treatment and the cumulative dose. The syndrome can develop after relatively brief treatment periods, even at low doses. It may also occur after discontinuation of treatment.
Tardive dyskinesia may remit, partially or completely, if antipsychotic treatment is discontinued. Antipsychotic treatment, itself, however, may suppress (or partially suppress) the signs and symptoms of the syndrome, possibly masking the underlying process. The effect that symptomatic suppression has upon the long-term course of the syndrome is unknown.
Given these considerations, RYKINDO should be prescribed in a manner that is most likely to minimize the occurrence of tardive dyskinesia. Chronic antipsychotic treatment should generally be reserved for patients: (1) who suffer from a chronic illness that is known to respond to antipsychotic drugs, and (2) for whom alternative, equally effective, but potentially less harmful treatments are not available or appropriate. In patients who do require chronic treatment, the lowest dose and the shortest duration of treatment producing a satisfactory clinical response should be used. Periodically reassess the need for continued treatment.
If signs and symptoms of tardive dyskinesia appear in a patient treated with RYKINDO, drug discontinuation should be considered. However, some patients may require treatment with RYKINDO despite the presence of the syndrome.
5.5 Metabolic Changes
Atypical antipsychotic drugs have caused metabolic changes, including hyperglycemia, diabetes mellitus, dyslipidemia, and body weight gain. While all of the drugs in the class have been shown to produce some metabolic changes, each drug has its own specific risk profile.
Hyperglycemia and Diabetes Mellitus
Hyperglycemia and diabetes mellitus, sometimes extreme and associated with ketoacidosis or hyperosmolar coma or death, have been reported in patients treated with atypical antipsychotics including risperidone. Assessment of the relationship between atypical antipsychotic use and glucose abnormalities is complicated by the possibility of an increased background risk of diabetes mellitus in patients with schizophrenia and the increasing incidence of diabetes mellitus in the general population. Given these confounders, the relationship between atypical antipsychotic use and hyperglycemia-related adverse events is not completely understood. However, epidemiological studies suggest an increased risk of hyperglycemia-related events in patients treated with the atypical antipsychotics. Precise risk estimates for hyperglycemia-related events in patients treated with atypical antipsychotics are not available.
Patients with an established diagnosis of diabetes mellitus who are started on atypical antipsychotics, including RYKINDO, should be monitored regularly for worsening glucose control. Patients with risk factors for diabetes mellitus (e.g., obesity, family history of diabetes) who are starting treatment with atypical antipsychotics, including RYKINDO, should undergo fasting blood glucose testing at the beginning of treatment and periodically during treatment. Any patient treated with atypical antipsychotics, including RYKINDO, should be monitored for symptoms of hyperglycemia including polydipsia, polyuria, polyphagia, and weakness. Patients who develop symptoms of hyperglycemia during treatment with atypical antipsychotics, including RYKINDO, should undergo fasting blood glucose testing. In some cases, hyperglycemia resolved when the atypical antipsychotic, including risperidone, was discontinued; however, some patients required continuation of anti-diabetic treatment despite discontinuation of risperidone.
Pooled data from 3 double-blind, placebo-controlled studies in patients with schizophrenia and 4 double-blind, placebo-controlled monotherapy studies in patients with bipolar mania with oral risperidone are presented in Table 1.
Table 1. Change in Random Glucose from Seven Placebo-Controlled, 3- to 8-Week, Fixed- or Flexible-Dose Studies in Adult Patients with Schizophrenia or Bipolar Mania with Oral Risperidone Placebo Oral Risperidone 1–8 mg/day >8–16 mg/day Mean change from baseline (mg/dL) N=555 N=748 N=164 Serum Glucose -1.4 0.8 0.6 Proportion of patients with shifts Serum Glucose
(<140 mg/dL to ≥200 mg/dL)0.6%
(3/525)0.4%
(3/702)0%
(0/158)In longer-term, controlled and uncontrolled studies in adult patients, oral risperidone was associated with a mean change in glucose of +2.8 mg/dL at Week 24 (N=151) and +4.1 mg/dL at Week 48 (N=50).
Dyslipidemia
Undesirable alterations in lipids have been observed in patients treated with atypical antipsychotics. Before or soon after initiation of antipsychotic medications, obtain a fasting lipid profile at baseline and monitor periodically during treatment.
Pooled data from 7 placebo-controlled, 3- to 8- week, fixed- or flexible-dose studies in adult patients with schizophrenia or bipolar mania are presented in Table 2.
Table 2. Change in Random Lipids from Seven Placebo-Controlled, 3- to 8-Week, Fixed- or Flexible-Dose Studies in Adult Patients with Schizophrenia or Bipolar Mania with Oral Risperidone Placebo Oral Risperidone 1–8 mg/day >8–16 mg/day Mean Change from Baseline (mg/dL) N=559 N=742 N=156 Cholesterol Change from baseline 0.6 6.9 1.8 N=183 N=307 N=123 Triglycerides Change from baseline -17.4 -4.9 -8.3 Proportion of Patients with Shifts Cholesterol 2.7% 4.3% 6.3% (<200 mg/dL to ≥240 mg/dL) (10/368) (22/516) (6/96) Triglycerides 1.1% 2.7% 2.5% (<500 mg/dL to ≥500 mg/dL) (2/180) (8/301) (3/121) In longer-term, controlled and uncontrolled studies, oral risperidone was associated with a mean change in (a) non-fasting cholesterol of +4.4 mg/dL at Week 24 (N=231) and +5.5 mg/dL at Week 48 (N=86); and (b) non-fasting triglycerides of +19.9 mg/dL at Week 24 (N=52).
Weight Gain
Weight gain has been observed with atypical antipsychotic use. Clinical monitoring of weight is recommended. Monitor weight at baseline and frequently thereafter.
Data from a placebo-controlled, 12-week, fixed-dose study in adult patients with schizophrenia are presented in Table 3.
Table 3. Mean Change in Body Weight (kg) and the Proportion of Patients with ≥7% Gain in Body Weight from a Placebo-Controlled, 12-Week, Fixed-Dose Study in Adult Patients with Schizophrenia Placebo
(N=83)Risperidone Long-acting Injection (intramuscular) 25 mg
(N=90)50 mg
(N=87)Weight (kg)
Change from baseline-1.4 0.5 1.2 Weight Gain
≥7% increase from baseline6% 10% 8% In an uncontrolled, longer-term, open-label study, risperidone long-acting injection (intramuscular) was associated with a mean change in weight of +2.1 kg at Week 24 (N=268) and +2.8 kg at Week 50 (N=199).
5.6 Hyperprolactinemia
As with other dopamine D2 receptor antagonists, risperidone elevates prolactin levels and the elevation persists during chronic administration. Risperidone is associated with higher levels of prolactin elevation than other antipsychotic agents.
Hyperprolactinemia may suppress hypothalamic gonadotropin-releasing hormone (GnRH), resulting in reduced pituitary gonadotropin secretion. This, in turn, may inhibit reproductive function by impairing gonadal steroidogenesis in both female and male patients [see Use in Specific Populations (8.3)]. Galactorrhea, amenorrhea, gynecomastia, and impotence have been reported in patients receiving prolactin-elevating compounds. Long-standing hyperprolactinemia when associated with hypogonadism may lead to decreased bone density in both female and male patients.
Tissue culture experiments indicate that approximately one-third of human breast cancers are prolactin dependent in vitro, a factor of potential importance if the prescription of these drugs is contemplated in a patient with previously detected breast cancer. An increase in pituitary gland, mammary gland, and pancreatic islet cell neoplasia (mammary adenocarcinomas, pituitary and pancreatic adenomas) was observed in the risperidone carcinogenicity studies conducted in mice and rats [see Nonclinical Toxicology (13.1)]. Published epidemiologic studies have shown inconsistent results when exploring the potential association between hyperprolactinemia and breast cancer.
5.7 Orthostatic Hypotension and Syncope
RYKINDO may induce orthostatic hypotension associated with dizziness, tachycardia, and in some patients, syncope, especially during the initial dose-titration period, probably reflecting its alpha-adrenergic antagonistic properties. Syncope was reported in 0.8% (12/1499 patients) of patients treated with risperidone long-acting injection (intramuscular) in multiple-dose studies. Patients should be instructed in nonpharmacologic interventions that help to reduce the occurrence of orthostatic hypotension (e.g., sitting on the edge of the bed for several minutes before attempting to stand in the morning and slowly rising from a seated position).
RYKINDO should be used with particular caution in (1) patients with known cardiovascular disease (history of myocardial infarction or ischemia, heart failure, or conduction abnormalities), cerebrovascular disease, and conditions which would predispose patients to hypotension, e.g., dehydration and hypovolemia, and (2) in the elderly and patients with renal or hepatic impairment. Monitoring of orthostatic vital signs should be considered in all such patients, and a dose reduction should be considered if hypotension occurs. Clinically significant hypotension has been observed with concomitant use of oral risperidone and antihypertensive medication.
5.8 Falls
Somnolence, postural hypotension, motor and sensory instability have been reported with the use of antipsychotics, including RYKINDO, which may lead to falls and, consequently, fractures or other fall-related injuries. For patients, particularly the elderly, with diseases, conditions, or medications that could exacerbate these effects, assess the risk of falls when initiating antipsychotic treatment and recurrently for patients on long-term antipsychotic therapy.
5.9 Leukopenia, Neutropenia, and Agranulocytosis
In clinical trial and/or postmarketing experience, leukopenia/neutropenia have been reported in temporal association with antipsychotic agents, including risperidone. Agranulocytosis has also been reported.
Possible risk factors for leukopenia/neutropenia include pre-existing low white blood cell count (WBC) and a history of drug-induced leukopenia/neutropenia. Patients with a history of a clinically significant low WBC or past drug-induced leukopenia/neutropenia should have their complete blood count (CBC) monitored frequently during the first few months of therapy. Discontinuation of RYKINDO should be considered at the first sign of a clinically significant decline in WBC in the absence of other causative factors.
Monitor patients with clinically significant neutropenia for fever or other symptoms or signs of infection and treat promptly if such symptoms or signs occur. Discontinue RYKINDO in patients with absolute neutrophil count <1000/mm3 and follow their WBC until recovery.
5.10 Potential for Cognitive and Motor Impairment
RYKINDO, like other antipsychotics, may cause somnolence and has the potential to impair judgement, thinking, and motor skills. Somnolence was reported by 5% of patients treated with risperidone long-acting injection (intramuscular) in multiple-dose trials.
Patients should be cautioned about operating hazardous machinery, including motor vehicles, until they are reasonably certain that treatment with RYKINDO does not affect them adversely.
5.11 Seizures
During premarketing studies, seizure occurred in 0.3% of patients (5 out of 1, 499 patients) treated with risperidone long-acting injection (intramuscular). Use RYKINDO with caution in patients with a history of seizures or with conditions that lower the seizure threshold. Conditions that lower the seizure threshold may be more prevalent in older patients.
5.12 Dysphagia
Esophageal dysmotility and aspiration have been associated with antipsychotic drug use. Aspiration pneumonia is a common cause of morbidity and mortality in patients with advanced Alzheimer's dementia. Antipsychotic drugs, including RYKINDO should be used cautiously in patients at risk for aspiration [see Warnings and Precautions (5.1)].
5.13 Priapism
Priapism has been reported during postmarketing surveillance of other risperidone products. Severe priapism may require surgical intervention.
5.14 Body Temperature Dysregulation
Atypical antipsychotics may disrupt the body's ability to reduce core body temperature. Both hyperthermia and hypothermia have been reported in association with the use of oral risperidone or risperidone long-acting injection (intramuscular). Strenuous exercise, exposure to extreme heat, dehydration, and anticholinergic medications may contribute to an elevation in core body temperature; use RYKINDO with caution in patients who may experience these conditions.
5.15 Osteodystrophy and Tumors in Animals
Risperidone long-acting injection (intramuscular) produced osteodystrophy in male and female rats in a 1-year toxicity study and a 2-year carcinogenicity study at a dose of 40 mg/kg administered IM every 2 weeks.
Risperidone long-acting injection (intramuscular) produced renal tubular tumors (adenoma, adenocarcinoma) and adrenomedullary pheochromocytomas in male rats in the 2-year carcinogenicity study at 40 mg/kg administered IM every 2 weeks. In addition, risperidone long-acting injection (intramuscular) produced an increase in a marker of cellular proliferation in renal tissue in males in the 1-year toxicity study and in renal tumor-bearing males in the 2-year carcinogenicity study at 40 mg/kg administered IM every 2 weeks. Cellular proliferation was not measured at the low dose or in females in either study.
The effect dose for osteodystrophy and the tumor findings is 8 times the IM maximum recommended human dose (MRHD) (50 mg) on a mg/m2 basis and is associated with a plasma exposure (AUC) twice the expected plasma exposure (AUC) at the IM MRHD. The no-effect dose for these findings was 5 mg/kg (equal to the IM MRHD on a mg/m2 basis). Plasma exposure (AUC) at the no-effect dose was 33% of the expected plasma exposure (AUC) at the IM MRHD.
Neither the renal or adrenal tumors, nor osteodystrophy, were seen in studies of orally administered risperidone. Osteodystrophy was not observed in dogs at doses up to 14 times (based on AUC) the IM MRHD in a 1-year toxicity study.
The renal tubular and adrenomedullary tumors in male rats and other tumor findings are described in more detail in Section 13.1 (Carcinogenicity, Mutagenesis, Impairment of Fertility).
The relevance of these findings to humans is unknown.
-
6 ADVERSE REACTIONS
The following are discussed in more detail in other sections of the labeling:
- Increased mortality in elderly patients with dementia-related psychosis [see Boxed Warning and Warnings and Precautions (5.1)]
- Cerebrovascular adverse reactions, including stroke, in elderly patients with dementia-related psychosis [see Warnings and Precautions (5.2)]
- Neuroleptic malignant syndrome (NMS) [see Warnings and Precautions (5.3)]
- Tardive dyskinesia [see Warnings and Precautions (5.4)]
- Metabolic changes [see Warnings and Precautions (5.5)]
- Hyperprolactinemia [see Warnings and Precautions (5.6)]
- Orthostatic hypotension and syncope [see Warnings and Precautions (5.7)]
- Falls [see Warnings and Precautions (5.8)]
- Leukopenia, Neutropenia, and Agranulocytosis [see Warnings and Precautions (5.9)]
- Potential for cognitive and motor impairment [see Warnings and Precautions (5.10)]
- Seizures [see Warnings and Precautions (5.11)]
- Dysphagia [see Warnings and Precautions (5.12)]
- Priapism [see Warnings and Precautions (5.13)]
- Body temperature dysregulation [see Warnings and Precautions (5.14)]
- Osteodystrophy and tumors in animals [see Warnings and Precautions (5.15)]
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
The safety of RYKINDO for the treatment of schizophrenia in adults and as monotherapy or as adjunctive therapy to lithium or valproate for the maintenance treatment of Bipolar I Disorder in adults is based on adequate and well-controlled studies of risperidone long-acting injection (intramuscular).
The data described in this section are derived from a clinical trial database consisting of 2,392 patients exposed to one or more doses of risperidone long-acting injection (intramuscular) for the treatment of schizophrenia. Of these 2,392 patients, 332 patients received risperidone long-acting injection (intramuscular) while participating in a 12-week double-blind, placebo-controlled trial. Two hundred two (202) of the 332 were patients with schizophrenia who received 25 mg or 50 mg risperidone long-acting injection (intramuscular). The conditions and duration of treatment with risperidone long-acting injection (intramuscular) in the other clinical trials varied greatly and included (in overlapping categories) double-blind, fixed- and flexible dose, placebo- or active-controlled studies and open-label phases of studies, inpatients and outpatients, and short-term (up to 12 weeks) and longer-term (up to 4 years) exposures.
In addition to the studies in patients with schizophrenia, safety data are presented from a trial assessing the efficacy and safety of risperidone long-acting injection (intramuscular) when administered as monotherapy for maintenance treatment in patients with bipolar I disorder.
Safety data are also presented from a trial assessing the efficacy and safety of risperidone long-acting injection (intramuscular) administered as adjunctive maintenance treatment in patients with bipolar disorder (intramuscular).
The most common adverse reactions in clinical trials of risperidone long-acting injection (intramuscular) in patients with schizophrenia (≥ 5%) were headache, parkinsonism, dizziness, akathisia, fatigue, constipation, dyspepsia, sedation, weight increased, pain in extremity, and dry mouth.
The most common adverse reactions in the double-blind, placebo-controlled periods of the bipolar disorder trials of risperidone long-acting injection (intramuscular) were weight increased (5% in the monotherapy trial) and tremor and parkinsonism (≥ 10% in the adjunctive treatment trial).
Table 4 lists the adverse reactions reported in 2% or more of risperidone long-acting injection-treated patients with schizophrenia in one 12-week double-blind, placebo-controlled trial.
Table 4. Adverse Reactions Occurring in ≥2% of Risperidone Long-acting Injection (intramuscular)-Treated Patients (Adults) with Schizophrenia in a 12-Week Double-Blind, Placebo-Controlled Trial Risperidone Long-acting Injection (intramuscular) Placebo System/Organ Class
Adverse Reaction25 mg
%50 mg
%% (N=99) (N=103) (N=98) - * Fatigue includes fatigue and asthenia.
- † Parkinsonism includes extrapyramidal disorder, musculoskeletal stiffness, muscle rigidity, and bradykinesia.
- ‡ Akathisia includes akathisia and restlessness.
- § Sedation includes sedation and somnolence.
Eye disorders Vision blurred 2 3 0 Gastrointestinal disorders Constipation 5 7 1 Dry mouth 0 7 1 Dyspepsia 6 6 0 Nausea 3 4 5 Toothache 1 3 0 Salivary hypersecretion 4 1 0 General disorders and administration site conditions Fatigue* 3 9 0 Edema peripheral 2 3 1 Pain 4 1 0 Pyrexia 2 1 0 Infections and infestations Upper respiratory tract infection 2 0 1 Investigations Weight increased 5 4 2 Weight decreased 4 1 1 Musculoskeletal and connective tissue disorders Pain in extremity 6 2 1 Nervous system disorders Headache 15 21 12 Parkinsonism† 8 15 9 Dizziness 7 11 6 Akathisia‡ 4 11 6 Sedation§ 5 6 3 Tremor 0 3 0 Syncope 2 1 0 Hypoesthesia 2 0 0 Respiratory, thoracic and mediastinal disorders Cough 4 2 3 Sinus congestion 2 0 0 Skin and subcutaneous tissue disorders Acne 2 2 0 Dry skin 2 0 0 Adverse Reactions in Double-Blind, Placebo-Controlled Clinical Trials – Bipolar Disorder
Table 5 lists the adverse reactions reported in 2% or more of risperidone long-acting injection (intramuscular)-treated patients in the 24-month double-blind, placebo-controlled treatment period of the trial assessing the efficacy and safety of risperidone long-acting injection (intramuscular) when administered as monotherapy for maintenance treatment in patients with Bipolar I Disorder.
Table 5. Adverse Reactions in ≥2% of Adult Patients with Bipolar I Disorder Treated with Risperidone Long-acting Injection (intramuscular) as Monotherapy in a 24-Month Double-Blind, Placebo-Controlled Trial System/Organ Class
Adverse ReactionRisperidone Long-acting Injection (intramuscular)
(N=154)
%Placebo (N=149)
%Investigations Weight increased 5 1 Nervous system disorders Dizziness 3 1 Vascular disorders Hypertension 3 1 Table 6 lists the adverse reactions reported in 4% or more of patients in the 52-week double-blind, placebo-controlled treatment phase of a trial assessing the efficacy and safety of risperidone long-acting injection as adjunctive maintenance treatment in patients with bipolar disorder.
Table 6. Adverse Reactions Occurring in ≥ 4% of Adult Patients with Bipolar I Disorder Treated with Risperidone Long-acting Injection (intramuscular) as Adjunctive Therapy in a 52-Week Double-Blind, Placebo-Controlled Trial System/Organ Class
Adverse ReactionRisperidone Long-acting Injection (intramuscular) + Treatment as Usual*
(N=72)
%Placebo + Treatment as Usual*
(N=67)
%- * Patients received double-blind risperidone long-acting injection (intramuscular) or placebo in addition to continuing their treatment as usual, which included mood stabilizers, antidepressants, and/or anxiolytics.
- † Parkinsonism includes muscle rigidity, hypokinesia, cogwheel rigidity, and bradykinesia.
- ‡ Dyskinesia includes muscle twitching and dyskinesia.
- § Sedation includes sedation and somnolence.
General disorders and administration site conditions Gait abnormal 4 0 Infections and infestations Upper respiratory tract infection 6 3 Investigations Weight increased 7 1 Metabolism and nutrition disorders Decreased appetite 6 1 Increased appetite 4 0 Musculoskeletal and connective tissue disorders Arthralgia 4 3 Nervous system disorders Tremor 24 16 Parkinsonism† 15 6 Dyskinesia‡ 6 3 Sedation§ 7 1 Disturbance in attention 4 0 Reproductive system and breast disorders Amenorrhea 4 1 Respiratory, thoracic and mediastinal disorders Cough 4 1 Other Adverse Reactions Observed During the Clinical Trial Evaluation of Risperidone
The following additional adverse reactions occurred in < 2% of the risperidone long-acting injection (intramuscular)-treated patients in the above schizophrenia double-blind, placebo-controlled trial dataset, in < 2% of the risperidone long-acting injection (intramuscular) -treated patients in the above double-blind, placebo-controlled period of the monotherapy bipolar disorder trial dataset, or in < 4% of the risperidone long-acting injection (intramuscular)-treated patients in the above double-blind, placebo-controlled period of the adjunctive treatment bipolar disorder trial dataset. The following also includes additional adverse reactions reported at any frequency in risperidone long-acting injection (intramuscular)-treated patients who participated in the open-label phases of the above bipolar disorder studies and in other studies, including double-blind, active controlled, and open-label studies in schizophrenia and bipolar disorder.
Blood and lymphatic system disorders: anemia, neutropenia
Cardiac disorders: tachycardia, atrioventricular block first degree, palpitations, sinus bradycardia, bundle branch block left, bradycardia, sinus tachycardia, bundle branch block right
Ear and labyrinth disorders: ear pain, vertigo
Endocrine disorders: hyperprolactinemia
Eye disorders: conjunctivitis, visual acuity reduced
Gastrointestinal disorders: diarrhea, vomiting, abdominal pain upper, abdominal pain, stomach discomfort, gastritis
General disorders and administration site conditions: injection site pain, chest discomfort, chest pain, influenza like illness, sluggishness, malaise, induration, injection site induration, injection site swelling, injection site reaction, face edema
Immune system disorders: hypersensitivity
Infections and infestations: nasopharyngitis, influenza, bronchitis, urinary tract infection, rhinitis, respiratory tract infection, ear infection, pneumonia, lower respiratory tract infection, pharyngitis, sinusitis, viral infection, infection, localized infection, cystitis, gastroenteritis, subcutaneous abscess
Injury and poisoning: fall, procedural pain
Investigations: blood prolactin increased, alanine aminotransferase increased, electrocardiogram abnormal, gamma-glutamyl transferase increased, blood glucose increased, hepatic enzyme increased, aspartate aminotransferase increased, electrocardiogram QT prolonged, glucose urine present
Metabolism and nutritional disorders: anorexia, hyperglycemia
Musculoskeletal, connective tissue and bone disorders: posture abnormal, myalgia, back pain, buttock pain, muscular weakness, neck pain, musculoskeletal chest pain
Nervous system disorders: coordination abnormal, dystonia, tardive dyskinesia, drooling, paresthesia, dizziness postural, convulsion, akinesia, hypokinesia, dysarthria
Psychiatric disorders: insomnia, agitation, anxiety, sleep disorder, depression, initial insomnia, libido decreased, nervousness
Renal and urinary disorders: urinary incontinence
Reproductive system and breast disorders: galactorrhea, oligomenorrhea, erectile dysfunction, sexual dysfunction, ejaculation disorder, gynecomastia, breast discomfort, menstruation irregular, menstruation delayed, menstrual disorder, ejaculation delayed
Respiratory, thoracic and mediastinal disorders: nasal congestion, pharyngolaryngeal pain, dyspnea, rhinorrhea
Skin and subcutaneous tissue disorders: rash, eczema, pruritus generalized, pruritus
Vascular disorders: hypotension, orthostatic hypotension
Additional Adverse Reactions Reported with Oral Risperidone
Additional adverse reactions that have been reported during the clinical trial evaluation of oral risperidone, regardless of frequency of occurrence, include the following:
Blood and Lymphatic Disorders: granulocytopenia
Cardiac Disorders: atrioventricular block
Ear and Labyrinth Disorders: tinnitus
Eye Disorders: ocular hyperemia, eye discharge, eye rolling, eyelid edema, eye swelling, eyelid margin crusting, dry eye, lacrimation increased, photophobia, glaucoma
Gastrointestinal Disorders: abdominal pain upper, dysphagia, fecaloma, abdominal discomfort, fecal incontinence, lip swelling, cheilitis, aptyalism
General Disorders: thirst, feeling abnormal, gait disturbance, pitting edema, edema, chills, discomfort, generalized edema, drug withdrawal syndrome, peripheral coldness
Immune System Disorders: drug hypersensitivity
Infections and Infestations: tonsillitis, eye infection, cellulitis, otitis media, onychomycosis, acarodermatitis, bronchopneumonia, respiratory tract infection, tracheobronchitis, otitis media chronic
Investigations: body temperature increased, heart rate increased, eosinophil count increased, WBC count decreased, hemoglobin decreased, blood creatine phosphokinase increased, hematocrit decreased, body temperature decreased, blood pressure decreased, transaminases increased
Metabolism and Nutrition Disorders: polydipsia
Musculoskeletal, Connective Tissue, and Bone Disorders: joint swelling, joint stiffness, rhabdomyolysis, torticollis
Nervous System Disorders: hypertonia, balance disorder, dysarthria, unresponsive to stimuli, depressed level of consciousness, movement disorder, hypokinesia, parkinsonian rest tremor, transient ischemic attack, cerebrovascular accident, masked facies, speech disorder, loss of consciousness, muscle contractions involuntary, akinesia, cerebral ischemia, cerebrovascular disorder, neuroleptic malignant syndrome (NMS), diabetic coma, head titubation
Psychiatric Disorders: blunted affect, confusional state, middle insomnia, listlessness, anorgasmia
Renal and Urinary Disorders: enuresis, dysuria, pollakiuria
Reproductive System and Breast Disorders: vaginal discharge, retrograde ejaculation, ejaculation disorder, ejaculation failure, breast enlargement
Respiratory, Thoracic, and Mediastinal Disorders: epistaxis, wheezing, pneumonia aspiration, dysphonia, productive cough, pulmonary congestion, respiratory tract congestion, rales, respiratory disorder, hyperventilation, nasal edema
Skin and Subcutaneous Tissue Disorders: erythema, skin discoloration, skin lesion, skin disorder, rash erythematous, rash papular, hyperkeratosis, dandruff, seborrheic dermatitis, rash generalized, rash maculopapular
Vascular Disorders: flushing
Discontinuations Due to Adverse Reactions
Schizophrenia
Approximately 11% (22/202) of risperidone long-acting (intramuscular)-treated patients in the 12-week double-blind, placebo-controlled schizophrenia trial discontinued treatment due to an adverse reaction, compared with 13% (13/98) who received placebo. The adverse reactions associated with discontinuation in two or more risperidone long-acting injection (intramuscular)-treated patients were agitation (3%), depression (2%), anxiety (1%), and akathisia (1%).
Bipolar Disorder
In the 24-month double-blind, placebo-controlled treatment period of the trial assessing the efficacy and safety of risperidone long-acting injection (intramuscular) monotherapy for maintenance treatment in patients with bipolar I disorder, 1 (0.6%) of 154 risperidone long-acting injection (intramuscular)-treated patients discontinued due to an adverse reaction (hyperglycemia).
In the 52-week double-blind phase of the placebo-controlled trial in which risperidone long-acting injection (intramuscular) was administered as adjunctive therapy to patients with bipolar disorder in addition to continuing with their usual treatment, approximately 4% (3/72) of risperidone long-acting injection (intramuscular)-treated patients discontinued treatment due to an adverse event, compared with 1.5% (1/67) of placebo-treated patients. Adverse reactions associated with discontinuation in risperidone long-acting injection(intramuscular)-treated patients were hypokinesia (one patient) and tardive dyskinesia (one patient).
Dose Dependency of Adverse Reactions in Clinical Trials
Extrapyramidal Symptoms (EPS)
Two methods were used to measure EPS in the 12-week double-blind, placebo-controlled trial comparing three doses of risperidone long-acting injection (intramuscular) (25 mg, 50 mg, and 75 mg) with placebo in patients with schizophrenia: (1) the incidence of spontaneous reports of EPS symptoms; and (2) the change from baseline to endpoint on the total score (sum of the subscale scores for parkinsonism, dystonia, and dyskinesia) of the Extrapyramidal Symptom Rating Scale (ESRS).
The overall incidence of EPS-related adverse reactions (akathisia, dystonia, parkinsonism, and tremor) in patients treated with 25 mg risperidone long-acting injection (intramuscular)was comparable to that of patients treated with placebo; the incidence of EPS-related adverse reactions was higher in patients treated with 50 mg risperidone long-acting injection (intramuscular) (Table 4).
The median change from baseline to endpoint in total ESRS score showed no worsening in patients treated with risperidone long-acting injection (intramuscular) compared with patients treated with placebo: 0 (placebo group); -1 (25-mg group, significantly less than the placebo group); and 0 (50-mg group).
Dystonia
Symptoms of dystonia, prolonged abnormal contractions of muscle groups, may occur in susceptible individuals during the first few days of treatment. Dystonic symptoms include neck muscle spasms, sometimes progressing to tightness of the throat, swallowing difficulty, difficulty breathing, and/or protrusion of the tongue. While these symptoms can occur at low doses, they occur more frequently and with greater severity with high potency and at higher doses of first-generation antipsychotic drugs. An elevated risk of acute dystonia is observed in males and younger age groups.
Changes in ECG
The ECGs of 202 patients with schizophrenia treated with 25 mg or 50 mg risperidone long-acting injection (intramuscular) and 98 schizophrenic patients treated with placebo in the 12-week double-blind, placebo-controlled trial were evaluated. There were no statistically significant differences in QTc intervals (using Fridericia's and linear correction factors) during treatment with either risperidone long-acting injection (intramuscular)or placebo.
The ECGs of 227 patients with Bipolar I Disorder were evaluated in the 24-month double-blind, placebo-controlled period. There were no clinically relevant differences in QTc intervals (using Fridericia's and linear correction factors) during treatment with risperidone long-acting injection (intramuscular) compared to placebo.
The ECGs of 85 patients with bipolar disorder were evaluated in the 52-week double-blind, placebo-controlled trial. There were no statistically significant differences in QTc intervals (using Fridericia's and linear correction factors) during adjunctive treatment with either risperidone long-acting injection (intramuscular) (25 mg, 37.5 mg, or 50 mg) or placebo in addition to treatment as usual.
Pain Assessment and Local Injection Site Reactions
The mean intensity of injection pain reported by patients with schizophrenia using a visual analog scale (0 = no pain to 100 = unbearably painful) decreased in all treatment groups from the first to the last dose of risperidone long-acting injection (intramuscular) (placebo: 16.7 to 12.6; 25 mg: 12.0 to 9.0; 50 mg: 18.2 to 11.8). After the sixth injection (Week 10), investigator ratings indicated that 1% of patients treated with 25 mg or 50 mg risperidone long-acting injection (intramuscular) experienced redness, swelling, or induration at the injection site.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of risperidone. Because these reactions are reported voluntarily from a population of uncertain size, it is not possible to reliably estimate their frequency or establish causal relationship to a drug exposure. These adverse reactions include: agranulocytosis, alopecia, anaphylactic reaction, angioedema, atrial fibrillation, blood cholesterol increased, blood triglycerides increased, catatonia, diabetes mellitus, diabetic ketoacidosis in patients with impaired glucose metabolism, drug withdrawal syndrome neonatal, dysgeusia, hypoglycemia, hypothermia, ileus, inappropriate antidiuretic hormone secretion, intestinal obstruction, jaundice, mania, pancreatitis, priapism, QT prolongation, sleep apnea syndrome, somnambulism, Stevens-Johnson syndrome and toxic epidermal necrolysis (SJS/TEN), thrombocytopenia, thrombotic thrombocytopenic purpura, urinary retention, and water intoxication. In addition, the following adverse reactions have been observed during post-approval use of risperidone long-acting injection (intramuscular): cerebrovascular disorders, including cerebrovascular accidents, and diabetes mellitus aggravated.
Retinal artery occlusion after use of risperidone long-acting injection (intramuscular) has been reported during postmarketing surveillance. This was reported in the presence of abnormal arteriovenous anastomosis.
Serious injection site reactions including abscess, cellulitis, cyst, hematoma, necrosis, nodule, and ulcer have been reported with risperidone long-acting injection (intramuscular) during postmarketing surveillance. Isolated cases required surgical intervention.
Very rarely, cases of anaphylactic reaction after administration of risperidone long-acting injection (intramuscular) have been reported during postmarketing experience in patients who previously tolerated oral risperidone.
Postmarketing cases of extrapyramidal symptoms (dystonia and dyskinesia) have been reported in patients concomitantly taking methylphenidate and risperidone when there was an increase or decrease in dosage, initiation, or discontinuation of either or both medications.
-
7 DRUG INTERACTIONS
7.1 Drugs Having Clinically Significant Interactions with RYKINDO
The interactions of RYKINDO with co-administration of other drugs have not been studied. The drug interaction data provided in this section is based on studies with oral risperidone.
Clinically significant drug interactions with RYKINDO are included in Table 7.
Table 7. Clinically Significant Drug Interactions with RYKINDO Strong CYP2D6 Inhibitors Clinical Impact Concomitant use of RYKINDO with strong CYP2D6 inhibitors may increase the plasma concentration of risperidone and lower the concentration of 9-hydroxyrisperidone, a major active metabolite of risperidone [see Clinical Pharmacology (12.3)]. Intervention When initiation of strong CYP2D6 inhibitors is considered, patients may be placed on a lower dose of RYKINDO between 2 to 4 weeks before the planned start of strong CYP2D6 inhibitors to adjust for the expected increase in plasma concentrations of risperidone. When a strong CYP2D6 inhibitor is initiated in patients receiving the recommended dose of 25 mg RYKINDO, it is recommended to continue treatment with the 25 mg dose unless clinical judgment necessitates either lowering the dose to 12.5 mg, in which case a different risperidone long-acting injection intramuscular formulation should be used, or interruption of RYKINDO treatment. The effects of discontinuation of strong CYP2D6 inhibitors on the pharmacokinetics of risperidone and 9-hydroxyrisperidone have not been studied [see Dosage and Administration (2.7) ]. Strong CYP3A4 Inducers Clinical Impact Co-administration of a strong CYP3A4 inducer with RYKINDO may cause decreases in the combined plasma concentrations of risperidone and 9-hydroxyrisperidone, which could lead to decreased efficacy of RYKINDO® treatment [see Clinical Pharmacology (12.3)]. Intervention When initiating therapy with a strong CYP3A4 inducer, patients should be closely monitored during the first 4 to 8 weeks because the dose of RYKINDO may need to be adjusted. A dose increase or additional oral risperidone may need to be considered. When discontinuing a strong CYP3A4 inducer, the dosage of RYKINDO should be re-evaluated and decreased, if necessary. Patients may be placed on a lower dose of RYKINDO between 2 to 4 weeks before the planned discontinuation of CYP3A4 inducers to adjust for the expected increase in plasma concentrations of risperidone plus 9-hydroxyrisperidone. For patients treated with the recommended dose of 25 mg RYKINDO and discontinuing from a CYP3A4 enzyme inducer, it is recommended to continue treatment with the 25-mg dose unless clinical judgment necessitates either lowering the RYKINDO dose to 12.5 mg, in which case a different risperidone long-acting injection intramuscular formulation should be used, or interruption of RYKINDO treatment. [see Dosage and Administration (2.7)]. Centrally-Acting Drugs and Alcohol Clinical Impact Nervous system disorders may be exacerbated due to additive pharmacological effects associated with the concomitant use of centrally-acting drugs, including alcohol. Intervention Use caution when RYKINDO is administered in combination with other centrally-acting drugs or alcohol. Hypotensive Agents Clinical Impact Because of its potential for inducing hypotension, RYKINDO may enhance the hypotensive effects of other therapeutic agents with this potential. Intervention Use caution when RYKINDO is administered in combination with other therapeutic agents with hypotensive effects. Dopamine Agonists Clinical Impact RYKINDO may antagonize the effects of levodopa and dopamine agonists. Intervention Caution should be used when RYKINDO is administered in combination with levodopa and dopamine agonists. Methylphenidate Clinical Impact: Concomitant use with methylphenidate, when there is change in dosage of either medication, may increase the risk of extrapyramidal symptoms (EPS) [see Adverse Reactions (6.2)]. Intervention: Monitor for symptoms of EPS with concomitant use of RYKINDO and methylphenidate. 7.2 Drugs Having No Clinically Important Interactions with RYKINDO
Based on pharmacokinetic studies with oral risperidone, no dosage adjustment of RYKINDO® is required when administered concomitantly with amitriptyline, cimetidine, ranitidine, clozapine, topiramate and moderate CYP3A4 inhibitors (erythromycin). Additionally, no dosage adjustment is necessary for lithium, valproate, topiramate, digoxin and CYP2D6 substrates (donepezil and galantamine) when co-administered with RYKINDO [see Clinical Pharmacology (12.3)].
-
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Pregnancy Exposure Registry
There is a pregnancy exposure registry that monitors pregnancy outcomes in women exposed to atypical antipsychotics, including RYKINDO, during pregnancy. Healthcare providers are encouraged to register patients by contacting the National Pregnancy Registry for Atypical Antipsychotics at 1-866-961-2388 or online at http://womensmentalhealth.org/clinicaland-research-programs/pregnancyregistry/.
Risk Summary
Neonates exposed to antipsychotic drugs during the third trimester of pregnancy are at risk for extrapyramidal and/or withdrawal symptoms following delivery (see Clinical Considerations). Overall, available data from published epidemiologic studies of pregnant women exposed to risperidone have not established a drug-associated risk of major birth defects, miscarriage, or adverse maternal or fetal outcomes (see Data). There are risks to the mother associated with untreated schizophrenia or bipolar I disorder and with exposure to antipsychotics, including RYKINDO, during pregnancy (see Clinical Considerations). Risperidone has been detected in plasma in adult subjects up to 6 weeks after a single-dose of RYKINDO [see Clinical Pharmacology (12.3)]. The clinical significance of RYKINDO administered before or during pregnancy is unknown.
Oral administration of risperidone to pregnant mice caused cleft palate at doses 3 to 4 times the maximum recommended human dose (MRHD) with maternal toxicity observed at 4 times the MRHD based on mg/m2 body surface area. Risperidone was not teratogenic in rats or rabbits at doses up to 6 times the MRHD based on mg/m2 body surface area. Increased incidence of stillbirths and decreased birth weight occurred after oral risperidone administration to pregnant rats at 1.5 times the MRHD based on mg/m2 body surface area. Learning was impaired in the offspring of dams dosed at 0.6-times the MRHD and offspring mortality increased at maternal doses 0.1 to 3 times the MRHD based on mg/m2 body surface area.
The estimated background risk of major birth defects and miscarriage for the indicated population is unknown. All pregnancies have a background risk of birth defect, loss, or other adverse outcomes. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2% to 4% and 15% to 20%, respectively.
Clinical Considerations
Disease-associated maternal and/or embryo/fetal risk
There is a risk to the mother from untreated schizophrenia or bipolar I disorder, including increased risk of relapse, hospitalization, and suicide. Schizophrenia and bipolar I disorder are associated with increased adverse perinatal outcomes, including preterm birth. It is not known if this is a direct result of the illness or other comorbid factors.
Fetal/Neonatal Adverse Reactions
Extrapyramidal and/or withdrawal symptoms (including agitation, hypertonia, hypotonia, tremor, somnolence, respiratory distress, and feeding disorder) have been reported in neonates who were exposed to antipsychotic drugs, including risperidone, during the third trimester of pregnancy. These symptoms varied in severity. Monitor neonates for extrapyramidal and/or withdrawal symptoms and manage symptoms appropriately. Some neonates recovered within hours or days without specific treatment; others required prolonged hospitalization.
Data
Human Data
Published data from observational studies, birth registries, and case reports on the use of atypical antipsychotics during pregnancy do not show a clear association between antipsychotics and major birth defects. A prospective observational study including 6 women treated with risperidone demonstrated placental passage of risperidone. A retrospective cohort study from a Medicaid database of 9258 women exposed to antipsychotics during pregnancy did not indicate an overall increased risk for major birth defects. There was a small increase in the risk of major birth defects (RR=1.26, 95% CI: 1.02-1.56) and of cardiac malformations (RR=1.26, 95% CI: 0.88-1.81) in a subgroup of 1566 women exposed to risperidone during the first trimester of pregnancy; however, there is no mechanism of action to explain the difference in malformation rates.
Animal Data
Oral administration of risperidone to pregnant mice during organogenesis caused cleft palate at 10 mg/kg/day or 3 times the MRHD of 16 mg/day based on mg/m2 body surface area; maternal toxicity occurred at 4 times the MRHD. Risperidone was not teratogenic when administered orally to rats at 0.6 to 10 mg/kg/day and rabbits at 0.3 to 5 mg/kg/day which are up to 6 times the MRHD of 16 mg/day risperidone based on mg/m2 body surface area. Learning was impaired in the offspring of rats dosed orally throughout pregnancy at 1 mg/kg/day which is 0.6 times the MRHD and neuronal cell death increased in fetal brains of rats dosed during pregnancy at 1 and 2 mg/kg/day which are 0.6 and 1.2 times the MRHD; postnatal development and growth of the offspring were also delayed.
Rat offspring mortality increased during the first 4 days of lactation when pregnant rats were dosed throughout gestation at 0.16 to 5 mg/kg/day which are 0.1 to 3 times the MRHD of 16 mg/day risperidone based on mg/m2 body surface area. It is not known whether these deaths were due to a direct effect on the fetuses or pups or to effects on the dams; a no-effect dose could not be determined. The rate of stillbirths was increased at 2.5 mg/kg or 1.5 times the MRHD.
In a rat cross-fostering study, the number of live offspring was decreased, the number of stillbirths was increased, and the offspring birth weight was decreased in offspring of drug-treated pregnant rats. In addition, the number of deaths increased by Day 1 among offspring of drug-treated pregnant rats, regardless of whether or not the offspring were cross-fostered. Risperidone also appeared to impair maternal behavior in that offspring body weight gain and survival (from Day 1 to 4 of lactation) were reduced for offspring born to control but reared by drug-treated dams. All of these effects occurred at 5 mg/kg which is 3 times the MRHD and the only dose tested in the study.
8.2 Lactation
Risk Summary
Limited data from published literature reports the presence of risperidone and its metabolite, 9-hydroxyrisperidone, in human breast milk at relative infant doses ranging between 2.3% and 4.7% of the maternal weight-adjusted dose. There are reports of sedation, failure to thrive, jitteriness, and EPS (tremors and abnormal muscle movements) in breastfed infants exposed to risperidone (see Clinical Considerations). Risperidone has been detected in the plasma in adult subjects up to 6 weeks after a single-dose of RYKINDO [see Clinical Pharmacology (12.3)], and the clinical significance on the breastfed infant is not known. There is no information on the effects of risperidone on milk production. The developmental and health benefits of breastfeeding should be considered along with the mother's clinical need for RYKINDO and any potential adverse effects on the breastfed child from RYKINDO or from the mother's underlying condition.
8.3 Females and Males of Reproductive Potential
Infertility
Females
Based on the pharmacologic action of risperidone (D2 receptor antagonism), treatment with RYKINDO may result in an increase in serum prolactin levels, which may lead to a reversible reduction in fertility in females of reproductive potential [see Warnings and Precautions (5.6) and Nonclinical Toxicology (13.1)].
8.4 Pediatric Use
Safety and effectiveness of RYKINDO have not been established in pediatric patients.
Juvenile Animal Toxicity Studies
Juvenile dogs were treated with oral risperidone from weeks 10 to 50 of age (equivalent to childhood through adolescence in humans) at doses of 0.31, 1.25, or 5 mg/kg/day (1.2, 3.4, or 13.5 times the MRHD of 6 mg/day for children, based on mg/m2 body surface area). Bone length and density were decreased with a no-effect dose of 0.31 mg/kg/day; this dose produced plasma AUCs of risperidone and 9-hydroxyrisperidone combined that were similar to those in children and adolescents receiving the MRHD of 6 mg/day. In addition, sexual maturation was delayed at all doses in both males and females. The above effects showed little or no reversibility in females after a 12-week drug-free recovery period.
Juvenile rats treated with oral risperidone from days 12 to 50 of age (equivalent to the period of infancy through adolescence in humans) showed impaired learning and memory performance (reversible only in females) with a no-effect dose of 0.63 mg/kg/day (0.5 times the MRHD of 6 mg/day for children). This dose produced plasma AUCs of risperidone and 9-hydroxyrisperidone combined that were approximately half the AUCs observed in humans at the MRHD. No other consistent effects on neurobehavioral or reproductive development were seen in juvenile rats given up to the highest tested dose of 1.25 mg/kg/day which is 1 time the MRHD and produced plasma AUCs of risperidone plus paliperidone that were about two thirds of those observed in humans at the MRHD of 6mg/day of children.
8.5 Geriatric Use
In an open-label study, 57 clinically stable, geriatric patients (≥ 65 years old) with schizophrenia or schizoaffective disorder received risperidone long-acting injection (intramuscular) every 2 weeks for up to 12 months. In general, no differences in the tolerability of risperidone long-acting injection (intramuscular) were observed between otherwise healthy geriatric and younger patients.
Because geriatric patients exhibit a greater tendency for orthostatic hypotension than nonelderly patients, geriatric patients should be instructed in nonpharmacologic interventions that help to reduce the occurrence of orthostatic hypotension (e.g., sitting on the edge of the bed for several minutes before attempting to stand in the morning and slowly rising from a seated position). In addition, monitoring of orthostatic vital signs should be considered in geriatric patients for whom orthostatic hypotension is a concern [see Warnings and Precautions (5.7)].
Elderly patients with dementia-related psychosis treated with RYKINDO are at an increased risk of death compared to placebo. RYKINDO is not approved for the treatment of patients with dementia related psychosis [see Boxed Warning and Warnings and Precautions (5.1, 5.2)].
8.6 Renal Impairment
In patients with renal impairment, titrate with oral risperidone (up to at least 2 mg) prior to initiating treatment with RYKINDO [see Dosage and Administration (2.6)].
Although patients with renal impairment were not studied with RYKINDO, they may have reduced risperidone elimination compared to patients with normal renal function [see Clinical Pharmacology (12.3)].
8.7 Hepatic Impairment
In patients with hepatic impairment, titrate with oral risperidone (up to at least 2 mg) prior to initiating treatment with RYKINDO [see Dosage and Administration (2.6)].
Although patients with hepatic impairment were not studied in RYKINDO clinical trials, they may have a clinically significant increase in the free fraction of risperidone, possibly resulting in an enhanced effect [see Clinical Pharmacology (12.3)].
8.8 Patients with Parkinson's Disease or Dementia with Lewy Bodies
Patients with Parkinson's disease or dementia with Lewy bodies can experience increased sensitivity to RYKINDO. Manifestations can include confusion, obtundation, postural instability with frequent falls, extrapyramidal symptoms, and clinical features consistent with neuroleptic malignant syndrome.
-
10 OVERDOSAGE
Human Experience
In premarketing experience with oral risperidone, there were eight reports of acute risperidone overdosage with estimated doses ranging from 20 to 300 mg and no fatalities. In general, reported signs and symptoms were those resulting from an exaggeration of the drug's known pharmacological effects, i.e., drowsiness and sedation, tachycardia and hypotension, and EPS. In one case, hyponatremia, hypokalemia, prolonged QT, and widened QRS were observed after a patient took an estimated 240 mg of oral risperidone. In another case, a patient had a seizure after taking an estimated 36 mg of oral risperidone.
Postmarketing experience with oral risperidone included reports of acute overdose with estimated doses up to 360 mg. In general, the most frequently reported signs and symptoms were those resulting from an exaggeration of the drug's known pharmacological effects, i.e., drowsiness, sedation, tachycardia, hypotension, and EPS. Other postmarketing adverse reactions related to oral risperidone overdose included prolonged QT interval and convulsions. Torsade de pointes was reported in association with combined overdose of oral risperidone and paroxetine.
Management of Overdosage
In case of acute overdosage, establish and maintain an airway and ensure adequate oxygenation and ventilation. Cardiovascular monitoring should commence immediately and include continuous electrocardiographic monitoring to detect possible arrhythmias. If antiarrhythmic therapy is administered, disopyramide, procainamide, and quinidine carry a theoretical hazard of QT prolonging effects that might be additive to those of risperidone. Similarly, it is reasonable to expect that the alpha-blocking properties of bretylium might be additive to those of risperidone, resulting in problematic hypotension.
There is no specific antidote to risperidone. Therefore, appropriate supportive measures should be implemented. The possibility of multiple drug involvement should be considered. Hypotension and circulatory collapse should be treated with appropriate measures, such as intravenous fluids and/or sympathomimetic agents (epinephrine and dopamine should not be used, since beta stimulation may worsen hypotension in the setting of risperidone-induced alpha blockade). In cases of severe EPS, anticholinergic medication should be administered. Close medical supervision and monitoring should continue until the patient recovers.
Consider contacting the Poison Help line (1-800-222-1222) or medical toxicologist for additional overdosage management recommendations.
-
11 DESCRIPTION
RYKINDO contains risperidone, an atypical antipsychotic belonging to the chemical class of benzisoxazole derivatives. The chemical designation is 3-[2-[4-(6-fluoro-1,2-benzisoxazol-3-yl)piperidin-1-yl] ethyl]-2-methyl-6,7,8,9-tetrahydro-4H-pyrido[1,2-a]pyrimidin-4-one. Its molecular formula is C23H27FN4O2 and its molecular weight is 410.5 g/mol. The structural formula is:
Risperidone is practically insoluble in water, freely soluble in methylene chloride, and soluble in methanol and 0.1 N HCl. RYKINDO is provided as a single-dose kit consisting of: a vial containing a white to almost white powder, a pre-filled syringe containing 2 mL of a colorless, clear diluent, a vial adapter, and a needle (a 20 gauge 2-inch needle with needle protection device).
The vial contains a white to almost white sterile powder containing risperidone. The powder consists of risperidone, mannitol (5.38 mg/100 mg risperidone), polylactide-co-glycolide (PLGA) 5050 (24.2 mg/100 mg risperidone) and polylactide-co-glycolide (PLGA) 7525 (96.7 mg/100 mg risperidone).
The diluent is a sterile, clear, colorless, 2 mL solution. The diluent contains: 1.10 mg/mL citric acid monohydrate, 1.02 mg/mL dibasic sodium phosphate anhydrous, 1 mg/mL polysorbate 80, 9 mg/mL sodium carboxymethyl cellulose, 7.5 mg/mL sodium chloride, 0.54 mg/mL sodium hydroxide, and water.
RYKINDO (risperidone) for extended-release injectable suspension, for intramuscular use is, when fully mixed, a white suspension, available in strengths of 25 mg, 37.5 mg, or 50 mg.
-
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
The mechanism of action of risperidone in schizophrenia is unclear. The drug's therapeutic activity could be mediated through a combination of dopamine Type 2 (D2) and serotonin Type 2 (5HT2) receptor antagonism. The clinical effect from risperidone results from the combined concentrations of risperidone and its major active metabolite, 9-hydroxyrisperidone (paliperidone) [see Clinical Pharmacology (12.3)]. Antagonism at receptors other than D2 and 5HT2 may explain some of the other effects of risperidone.
12.2 Pharmacodynamics
Risperidone is a monoaminergic antagonist with high affinity (Ki of 0.12 to 7.3 nM) for the serotonin Type 2 (5HT2), dopamine Type 2 (D2), α1 and α2 adrenergic, and H1 histaminergic receptors. Risperidone shows low to moderate affinity (Ki of 47 to 253 nM) for the serotonin 5HT1C, 5HT1D, and 5HT1A receptors; weak affinity (Ki of 620 to 800 nM) for the dopamine D1 and haloperidol-sensitive sigma site; and no affinity (when tested at concentrations >10-5 M) for cholinergic muscarinic or β1 and β2 adrenergic receptors.
12.3 Pharmacokinetics
Absorption
After a single intramuscular injection of RYKINDO, the release profile consists of an initial release of risperidone followed by a stable release phase of 2 to 4 weeks. The median time to peak concentration (Tmax) of risperidone and 9-hydroxyrisperidone combined are 14 and 17 days after administration of 25 mg and 50 mg of RYKINDO, respectively. Systemic exposures (AUC0-t and Cmax) of the active moiety increase in a dose proportional manner across the dosing range from 25 mg to 50 mg.
The combination of the release profile and the dosage regimen (intramuscular injections every 2 weeks) of RYKINDO results in sustained concentrations within the dosing interval (every 2 weeks). Steady-state plasma concentration levels are reached after 2 injections and can be maintained for 2 to 3 weeks after the last injection. Following multiple IM injections (25 mg every two weeks for five consecutive injections) in patients, the geometric mean ratios [RYKINDO to risperidone long-acting injection (intramuscular)] of risperidone and 9-hydroxyrisperidone combined were 102.33% for the Css-max and 94.08% for the AUCss-tau, and the 90% CIs of the ratios were within the 80% to 125% range.
Distribution
The volume of distribution of risperidone is 1-2 L/kg. In plasma, risperidone is bound to albumin and α1-acid glycoprotein. The plasma protein binding of risperidone is approximately 90%, and that of its major metabolite, 9-hydroxyrisperidone, is 77%. Neither risperidone nor 9-hydroxyrisperidone displaces the other from plasma binding sites. High therapeutic concentrations of sulfamethazine (100 mcg/mL), warfarin (10 mcg/mL), and carbamazepine (10 mcg/mL) caused only a slight increase in the free fraction of risperidone at 10 ng/mL and of 9-hydroxyrisperidone at 50 ng/mL, changes of unknown clinical significance.
Elimination
Metabolism
Risperidone is extensively metabolized in the liver. The main metabolic pathway is through hydroxylation of risperidone to 9-hydroxyrisperidone by the enzyme CYP2D6. A minor metabolic pathway is through N-dealkylation. The main metabolite, 9-hydroxyrisperidone, has similar pharmacological activity as risperidone. Consequently, the clinical effect of the drug results from the combined concentrations of risperidone plus 9-hydroxyrisperidone.
CYP2D6, also called debrisoquin hydroxylase, is responsible for metabolism of many neuroleptics, antidepressants, antiarrhythmics, and other drugs. CYP2D6 is subject to genetic polymorphism (about 6% to 8% of Caucasians, and a very low percentage of Asians, have little or no activity and are "poor metabolizers") and to inhibition by a variety of substrates and some non-substrates, notably quinidine. Extensive CYP2D6 metabolizers convert risperidone rapidly into 9-hydroxyrisperidone, whereas poor CYP2D6 metabolizers convert it much more slowly. Although extensive metabolizers have lower risperidone and higher 9-hydroxyrisperidone concentrations than poor metabolizers, the pharmacokinetics of risperidone and 9-hydroxyrisperidone combined, after single and multiple doses, are similar in extensive and poor metabolizers.
Excretion
Risperidone and its metabolites are eliminated via the urine and, to a much lesser extent, via the feces. In a mass balance study of a single 1 mg oral dose of 14C-risperidone administered in solution to three healthy male volunteers, total recovery of radioactivity at 1 week was 84%, including 70% in the urine and 14% in the feces.
The apparent half-life (t½) of active moiety following RYKINDO administration is 3 to 6 days and associated with a monoexponential decline in plasma concentrations after a single dose. This t½ is related to the erosion of the sterile powder and subsequent absorption of risperidone after RYKINDO intramuscular administration.
The clearance of risperidone and risperidone plus 9-hydroxyrisperidone was 13.7 L/h and 5.0 L/h in extensive CYP2D6 metabolizers, and 3.3 L/h and 3.2 L/h in poor CYP 2D6 metabolizers, respectively. The elimination phase is completed approximately 6 weeks after the last injection.
Specific Populations
Patients with Renal Impairment
Clearance of the sum of risperidone and 9-hydroxyrisperidone decreased by 60% in patients with moderate to severe renal disease compared with young healthy subjects treated with oral risperidone. [see Dosage and Administration (2.6)].
Patients with Hepatic Impairment
While the pharmacokinetics of oral risperidone in subjects with liver disease were comparable to those in young healthy subjects, the mean free fraction of risperidone in plasma was increased by about 35% because of the diminished concentration of both albumin and α1-acid glycoprotein. Although patients with hepatic impairment were not studied in RYKINDO clinical trials, it is recommended that patients with hepatic impairment be carefully titrated on oral risperidone before treatment with RYKINDO [see Dosage and Administration (2.6)].
Geriatric Patients
In an open-label trial, steady-state concentrations of risperidone plus 9-hydroxyrisperidone in otherwise healthy elderly patients (≥ 65 years old) treated with risperidone long-acting injection (intramuscular) for up to 12 months fell within the range of values observed in otherwise healthy nonelderly patients. Dosing recommendations are the same for otherwise healthy elderly patients and nonelderly patients.
Racial or Ethnic Groups and Male and Female Patients
No specific pharmacokinetic study was conducted to investigate race and gender effects, but a population pharmacokinetic analysis with risperidone long-acting injection (intramuscular) did not identify important differences in the disposition of risperidone due to gender (whether or not corrected for body weight) or race.
Drug Interaction Studies
Clinical Studies
The interactions of RYKINDO with co-administration of other drugs have not been systematically evaluated in humans. The drug interaction data provided in this section is based primarily on studies with oral risperidone. Effects of other drugs on the exposures of risperidone, 9-hydroxyrisperidone and total active moiety as well as the effects of risperidone on the exposures of other drugs are summarized below.
Effects of Other Drugs on Risperidone, 9-hydroxyrisperidone and Total Active Moiety Pharmacokinetics
Strong CYP2D6 Inhibitors (Fluoxetine and Paroxetine)
Fluoxetine (20 mg once daily) and paroxetine (20 mg once daily), potent CYP2D6 inhibitors, have been shown to increase the plasma concentration of risperidone by 2.5- to 2.8-fold and 3- to 9-fold, respectively. Fluoxetine did not affect the plasma concentration of 9-hydroxyrisperidone. Paroxetine lowered the concentration of 9-hydroxyrisperidone by about 10%. The effects of discontinuation of concomitant fluoxetine or paroxetine therapy on the pharmacokinetics of risperidone and 9-hydroxyrisperidone have not been studied [see Dosage and Administration (2.8) and Drug Interactions (7.1)].
Moderate CYP3A4 Inhibitor (Erythromycin)
There was no significant interaction between oral risperidone and erythromycin, a moderate CYP3A4 inhibitor.
Strong CYP3A4 Inducer (Carbamazepine)
Carbamazepine co-administration with oral risperidone decreased the steady-state plasma concentrations of risperidone and 9-hydroxyrisperidone by about 50%. Plasma concentrations of carbamazepine were not affected. Co-administration of other known CYP3A4 enzyme inducers (e.g., phenytoin, rifampin, and phenobarbital) with risperidone may cause similar decreases in the combined plasma concentrations of risperidone and 9-hydroxyrisperidone, which could lead to decreased efficacy of RYKINDO treatment [see Dosage and Administration (2.8) and Drug Interactions (7.1)].
Amitriptyline, Cimetidine, Ranitidine, Clozapine
Clinically meaningful pharmacokinetic interaction between RYKINDO and other drugs, such as amitriptyline, cimetidine, ranitidine and clozapine, is not expected.
Amitriptyline did not affect the pharmacokinetics of risperidone or of risperidone and 9- hydroxyrisperidone combined following concomitant administration with oral risperidone. Cimetidine and ranitidine increased the bioavailability of oral risperidone by 64% and 26%, respectively. However, cimetidine did not affect the AUC of risperidone and 9- hydroxyrisperidone combined, whereas ranitidine increased the AUC of risperidone and 9-hydroxyrisperidone combined by 20%. Chronic administration of clozapine with risperidone may decrease the clearance of risperidone.
Effects of Oral Risperidone on Pharmacokinetics of Other Drugs
Lithium
Repeated doses of oral risperidone (3 mg twice daily) did not affect the exposure (AUC) or peak plasma concentrations (Cmax) of lithium (n = 13).
Valproate
Repeated doses of oral risperidone (4 mg once daily) did not affect the pre-dose or average plasma concentrations and exposure (AUC) of valproate (1000 mg/day in three divided doses) compared to placebo (n = 21). However, there was a 20% increase in valproate peak plasma concentration (Cmax) after concomitant administration of oral risperidone.
Topiramate
Oral risperidone administered at doses from 1 to 6 mg/day concomitantly with topiramate 400 mg/day resulted in a 23% decrease in risperidone Cmax and a 33% decrease in risperidone AUC0-12 hour at steady state. Minimal reductions in the exposure to risperidone and 9-hydroxyrisperidone combined, and no change for 9-hydroxyrisperidone were observed. This interaction is unlikely to be of clinical significance. There was no clinically relevant effect of oral risperidone on the pharmacokinetics of topiramate.
Digoxin
Oral risperidone (0.25 mg twice daily) did not show a clinically relevant effect on the pharmacokinetics of digoxin.
Drugs Metabolized by CYP2D6
In vitro studies indicate that risperidone is a relatively weak inhibitor of CYP2D6. Therefore, RYKINDO® is not expected to substantially inhibit the clearance of drugs that are metabolized by this enzymatic pathway. In drug interaction studies, oral risperidone did not significantly affect the pharmacokinetics of donepezil and galantamine, which are metabolized by CYP2D6.
-
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis - Oral
Risperidone was administered in the diet at doses of 0.63, 2.5, and 10 mg/kg for 18 months to mice and for 25 months to rats. These doses are equivalent to approximately 0.2, 0.75, and 3 times (mice) and 0.4, 1.5, and 6 times (rats) the MRHD of 16 mg/day, based on mg/m2 body surface area. A maximum tolerated dose was not achieved in male mice. There was a significant increase in pituitary gland adenomas, endocrine pancreatic adenomas, and mammary gland adenocarcinomas. Table 8 summarizes the multiples of the human dose on a mg/m2 (mg/kg) basis at which these tumors occurred.
Table 8. Summary of Tumor Occurrence at Multiples of the MRHD* with Oral Risperidone Dosing in Mice and Rats Tumor Type Species Sex Multiples of the MRHD in mg/m2 (mg/kg) Lowest Effect Level Highest No-Effect Level - * MRHD = maximum recommended human dose on a mg/ m2 (mg/kg) basis
Pituitary adenomas Mouse Female 0.75 (9.4) 0.2 (2.4) Endocrine pancreas adenomas Rat Male 1.5 (9.4) 0.4 (2.4) Mammary gland adenocarcinomas Mouse Female 0.2 (2.4) None Rat Female 0.4 (2.4) None Rat Male 6.0 (37.5) 1.5 (9.4) Mammary gland neoplasm (total) Rat Male 1.5 (9.4) 0.4 (2.4) Antipsychotic drugs chronically elevate prolactin levels in rodents. Serum prolactin levels were not measured during the risperidone carcinogenicity studies; however, measurements during subchronic toxicity studies showed that risperidone elevated serum prolactin levels by 5- to 6- fold in mice and rats at the same doses used in the carcinogenicity studies. An increase in mammary, pituitary, and endocrine pancreas neoplasms were found in rodents after chronic administration of other antipsychotic drugs. These neoplasms were considered to be prolactin-mediated. The clinical relevance of the findings of prolactin-mediated endocrine tumors in rodents is unclear [see Warnings and Precautions (5.6)].
Carcinogenesis - Intramuscular
Risperidone was evaluated in a 24-month carcinogenicity study in which SPF Wistar rats were treated every 2 weeks with intramuscular (IM) injections of either 5 mg/kg or 40 mg/kg of risperidone. These doses are 1 and 8 times the MRHD (50 mg) on a mg/m2 basis. A control group received injections of 0.9% NaCl, and a vehicle control group was injected with placebo. There was a significant increase in pituitary gland adenomas, endocrine pancreas adenomas, and adrenomedullary pheochromocytomas at 8 times the IM MRHD on a mg/m2 basis. The incidence of mammary gland adenocarcinomas was significantly increased in female rats at both doses (1 and 8 times the IM MRHD on a mg/m2 basis). A significant increase in renal tubular tumors (adenoma, adenocarcinomas) was observed in male rats at 8 times the IM MRHD on a mg/m2 basis. Plasma exposures (AUC) in rats were 0.3 and 2 times (at 5 and 40 mg/kg, respectively) the expected plasma exposure (AUC) at the IM MRHD.
Dopamine D2 receptor antagonists have been shown to chronically elevate prolactin levels in rodents. Serum prolactin levels were not measured during the carcinogenicity studies of oral risperidone; however, measurements taken during subchronic toxicity studies showed that oral risperidone elevated serum prolactin levels by 5- to 6-fold in mice and rats at the same doses used in the oral carcinogenicity studies. Serum prolactin levels increased in a dose-dependent manner up to 6- and 1.5-fold in male and female rats, respectively, at the end of the 24-month treatment with risperidone every 2 weeks IM. Increases in the incidence of pituitary gland, endocrine pancreas, and mammary gland neoplasms have been found in rodents after chronic administration of other antipsychotic drugs and may be prolactin-mediated.
The relevance for human risk of the findings of prolactin-mediated endocrine tumors in rodents is unknown [see Warnings and Precautions (5.6)].
Mutagenesis
No evidence of mutagenic or clastogenic potential for risperidone was found in the in vitro tests of Ames gene mutation, the mouse lymphoma assay, rat hepatocyte DNA-repair assay, the chromosomal aberration test in human lymphocytes, Chinese hamster ovary cells, or in the in vivo micronucleus test in mice, and the sex-linked recessive lethal test in Drosophila.
In addition, no evidence of mutagenic potential was found in the in vitro Ames reverse mutation test for risperidone long-acting injection (intramuscular).
Impairment of Fertility
Oral risperidone (0.16 to 5 mg/kg) impaired mating, but not fertility, in rat reproductive studies at doses between 0.1 and 3 times the oral maximum recommended human dose (MRHD of 16 mg/day) based on a mg/m2 body surface area. The effect appeared to be in females since impaired mating behavior was not noted in the male fertility study. In a subchronic study in Beagle dogs in which oral risperidone was administered at doses of 0.31 to 5 mg/kg, sperm motility and concentration were decreased at doses between 0.6 and 10 times the oral MRHD on a mg/m2 basis. Dose-related decreases were also noted in serum testosterone at the same doses. Serum testosterone and sperm values partially recovered but remained decreased after treatment discontinuation. A no-effect dose could not be determined in either rat or dog.
-
14 CLINICAL STUDIES
14.1 Schizophrenia
The effectiveness of RYKINDO in the treatment of schizophrenia is based on an adequate and well-controlled study with risperidone long-acting injection (intramuscular). The effectiveness of risperidone long-acting injection (intramuscular) was established, in part, on the basis of the established effectiveness of the oral formulation of risperidone as well as in a 12-week, placebo-controlled trial in adult inpatients and outpatients who met the DSM-IV criteria for schizophrenia. The results of the adequate and well-controlled study are presented below.
Efficacy data were obtained from 400 patients with schizophrenia who were randomized to receive injections of 25 mg, 50 mg, or 75 mg risperidone long-acting injection (intramuscular) or placebo every 2 weeks. During a 1-week run-in period, patients were discontinued from other antipsychotics and were titrated to a dose of 4 mg oral risperidone. Patients who received risperidone long-acting injection (intramuscular) were given doses of oral risperidone (2 mg for patients in the 25-mg group, 4 mg for patients in the 50-mg group, and 6 mg for patients in the 75-mg group) for 3 weeks after the first injection to provide therapeutic plasma concentrations until the main release phase of risperidone from the injection site had begun. Patients who received placebo injections were given placebo tablets.
Efficacy was evaluated using the Positive and Negative Syndrome Scale (PANSS), a validated, multi-item inventory, composed of five subscales to evaluate positive symptoms, negative symptoms, disorganized thoughts, uncontrolled hostility/excitement, and anxiety/depression.
The primary efficacy variable in this trial was change from baseline to endpoint in the total PANSS score. The mean total PANSS score at baseline for schizophrenic patients in this study was 81.5.
Total PANSS scores showed significant improvement in the change from baseline to endpoint in schizophrenic patients treated with each dose of risperidone long-acting injection (intramuscular) (25 mg, 50 mg, or 75 mg) compared with patients treated with placebo. While there were no statistically significant differences between the treatment effects for the three dose groups, the effect size for the 75 mg dose group was actually numerically less than that observed for the 50 mg dose group.
Subgroup analyses did not indicate any differences in treatment outcome as a function of age, race, or gender.
14.2 Bipolar Disorder - Monotherapy
The effectiveness of RYKINDO for the maintenance treatment of bipolar I disorder is based on an adequate and well-controlled study with risperidone long-acting injection (intramuscular). The efficacy of risperidone long-acting injection (intramuscular) was established in a multicenter, double-blind, placebo-controlled study of adult patients who met DSM-IV criteria for Bipolar Disorder Type I, who were stable on medications or experiencing an acute manic or mixed episode. The results of the adequate and well-controlled study are presented below.
A total of 501 patients were treated during a 26-week open-label period with the risperidone long-acting injection (intramuscular) (starting dose of 25 mg, and titrated, if deemed clinically desirable, to 37.5 mg or 50 mg; in patients not tolerating the 25 mg dose, the dose could be reduced to 12.5 mg). In the open-label phase, 303 (60%) patients were judged to be stable and were randomized to double-blind treatment with either the same dose of risperidone long-acting injection (intramuscular) or placebo and monitored for relapse. The primary endpoint was time to relapse to any mood episode (depression, mania, hypomania, or mixed).
Time to relapse was delayed in patients receiving risperidone long-acting injection (intramuscular) monotherapy compared with patients receiving placebo. The majority of relapses were due to manic rather than depressive symptoms. Based on their bipolar disorder history, subjects entering this study had, on average, more manic episodes than depressive episodes.
14.3 Bipolar Disorder - Adjunctive Therapy
The effectiveness of RYKINDO as an adjunct to treatment with lithium or valproate for the maintenance treatment of bipolar I disorder is based on an adequate and well-controlled study of risperidone long-acting injection (intramuscular). The results of the adequate and well-controlled study are presented below.
The efficacy of risperidone long-acting injection (intramuscular) was established in a multi-center, randomized, double-blind, placebo-controlled study of adult patients who met DSM-IV criteria for Bipolar Disorder Type I and who experienced at least 4 episodes of mood disorder requiring psychiatric/clinical intervention in the previous 12 months, including at least 2 episodes in the 6 months prior to the start of the study.
A total of 240 patients were treated during a 16-week open-label period with risperidone long-acting injection (intramuscular) (starting dose of 25 mg, and titrated, if deemed clinically desirable, to 37.5 mg or 50 mg), as adjunctive therapy in addition to continuing their usual treatment for bipolar disorder, which consisted of mood stabilizers (primarily lithium and valproate), antidepressants, and/or anxiolytics. All oral antipsychotics were discontinued after the first three weeks after the initial injection of risperidone long-acting injection (intramuscular). In the open-label phase, 124 (51.7%) were judged to be stable for at least the last 4 weeks and were randomized to double-blind treatment with either the same dose of risperidone long-acting injection (intramuscular) or placebo in addition to continuing their usual treatment and monitored for relapse during a 52-week period. The primary endpoint was time to relapse to any new mood episode (depression, mania, hypomania, or mixed).
Time to relapse was delayed in patients receiving adjunctive therapy with risperidone long-acting injection (intramuscular) compared with patients receiving adjunctive therapy with placebo. The relapse types were about half depressive and half manic or mixed episodes.
-
16 HOW SUPPLIED/STORAGE AND HANDLING
How Supplied
RYKINDO (risperidone) for extended-release injectable suspension, for intramuscular use is, when fully mixed, a white suspension, available in strengths of 25 mg, 37.5 mg, or 50 mg. It is provided as a single-dose kit, consisting of: a vial containing a white to almost white powder, a pre-filled syringe containing 2 mL of a colorless, clear diluent, a vial adapter, and a needle (a 20 gauge 2-inch needle with needle protection device).
RYKINDO: 25-mg kit (NDC: 72526-102-11): A white to almost white powder provided in a vial with a green flip-off cap (NDC: 72526-202-01); a pre-filled syringe containing 2 mL of a colorless, clear diluent (NDC: 72526-801-01); a needle; and a vial adapter.
RYKINDO: 37.5-mg kit: (NDC: 72526-103-11): A white to almost white powder provided in a vial with a purple flip-off cap (NDC: 72526-203-01); a pre-filled syringe containing 2 mL of a colorless, clear diluent (NDC: 72526-801-01); a needle; and a vial adapter.
RYKINDO 50-mg kit: (NDC: 72526-104-11): A white to almost white powder provided in a vial with a blue flip-off cap (NDC: 72526-204-01); a pre-filled syringe containing 2 mL of a colorless, clear diluent (NDC: 72526-801-01); a needle; and a vial adapter.
Storage and Handling
Store kit in refrigerator at 2° to 8°C (36° to 46°F). Protect from light.
If refrigeration is unavailable, RYKINDO can be stored in its unopened original packaging at temperatures not exceeding 77°F (25°C) for no more than 7 days prior to administration.
After removal from the refrigerator, use RYKINDO within 7 days or discard.
-
17 PATIENT COUNSELING INFORMATION
Neuroleptic Malignant Syndrome (NMS)
Counsel patients about a potentially fatal adverse reaction, Neuroleptic Malignant Syndrome (NMS), that has been reported in association with administration of antipsychotic drugs. Advise patients, family members, or caregivers to contact the healthcare provider or report to the emergency room if they experience signs and symptoms of NMS [see Warnings and Precautions (5.3)].
Tardive Dyskinesia
Counsel patients on the signs and symptoms of tardive dyskinesia and to contact their healthcare provider if these abnormal movements occur [see Warnings and Precautions (5.4)].
Metabolic Changes
Educate patients about the risk of metabolic changes, how to recognize symptoms of hyperglycemia and diabetes mellitus and the need for specific monitoring, including blood glucose, lipids, and weight [see Warnings and Precautions (5.5)].
Hyperprolactinemia
Counsel patients on signs and symptoms of hyperprolactinemia that may be associated with chronic use of RYKINDO. Advise them to seek medical attention if they experience any of the following: amenorrhea or galactorrhea in females, erectile dysfunction or gynecomastia in males [see Warnings and Precautions (5.6)].
Orthostatic Hypotension and Syncope
Educate patients about the risk of orthostatic hypotension and syncope, particularly at the time of initiating treatment, re-initiating treatment, or increasing the dose [see Warnings and Precautions (5.7)].
Leukopenia/Neutropenia
Advise patients with a pre-existing low WBC or a history of drug induced leukopenia/neutropenia that they should have their CBC monitored while being treated with RYKINDO [see Warnings and Precautions (5.9)].
Potential for Cognitive and Motor Impairment
Inform patients that RYKINDO has the potential to impair judgment, thinking, or motor skills. Caution patients about performing activities requiring mental alertness, such as operating hazardous machinery or operating a motor vehicle, until they are reasonably certain that treatment with RYKINDO does not affect them adversely [see Warnings and Precautions (5.10)].
Priapism
Advise patients of the possibility of painful or prolonged penile erections (priapism). Instruct the patient to seek immediate medical attention in the event of priapism [see Warnings and Precautions (5.13)].
Heat Exposure and Dehydration
Educate patients regarding appropriate care in avoiding overheating and dehydration [see Warnings and Precautions (5.14)].
Concomitant Medication
Advise patients to inform their healthcare providers if they are taking, or plan to take, any prescription or over-the-counter drugs, since there is a potential for interactions [see Drug Interactions (7)].
Alcohol
Advise patients to avoid alcohol during treatment with RYKINDO [see Drug Interactions (7.1)].
Pregnancy
Advise patients to notify their healthcare provider if they become pregnant or intend to become pregnant during treatment with RYKINDO. Advise patients that RYKINDO may cause extrapyramidal and/or withdrawal symptoms (agitation, hypertonia, hypotonia, tremor, somnolence, respiratory distress, and feeding disorder) in a neonate. Advise patients that there is a pregnancy registry that monitors pregnancy outcomes in women exposed to RYKINDO during pregnancy [see Use in Specific Populations (8.1)].
Lactation
Advise breastfeeding women using RYKINDO to monitor infants for somnolence, failure to thrive, jitteriness, and EPS (tremors and abnormal muscle movements) and to seek medical care if they notice these signs [see Use in Specific Populations (8.2)].
Infertility
Advise females of reproductive potential that RYKINDO may impair fertility due to an increase in serum prolactin levels. The effects on fertility are reversible [see Use in Specific Populations (8.3)].
- SPL UNCLASSIFIED SECTION
-
INSTRUCTIONS FOR USE
RYKINDO® [ray-KIN-do]
(risperidone)
injection, for gluteal intramuscular useThis Instruction for Use contains information on how to inject RYKINDO®
Important Information You Need to Know Before Injecting RYKINDO®
For gluteal intramuscular injection use only
For gluteal intramuscular injection only. Do not inject by any other route. Alternate injections between the two buttocks.
Wait 30 minutes
Remove dose pack from the refrigerator and allow to sit at room temperature for at least 30 minutes prior to preparation. Do not warm any other way. Prepare medication when you are ready to administer the dose.
Use components provided
The components in this dose pack are specifically designed for use with RYKINDO. RYKINDO must be reconstituted only in the diluent supplied in the dose pack. Do not substitute ANY components of the dose pack.
Do not store suspension after reconstitution.
Administer dose as soon as possible after reconstitution to avoid settling.
Proper dosing
The entire contents of the vial must be administered to ensure the intended dose of RYKINDO is delivered.
Do not reuse.
RYKINDO® is for one-time use only. Do not reuse RYKINDO.
The components of the single-dose kit are shown in Figure 1.
Figure1: Single-dose Kit Components
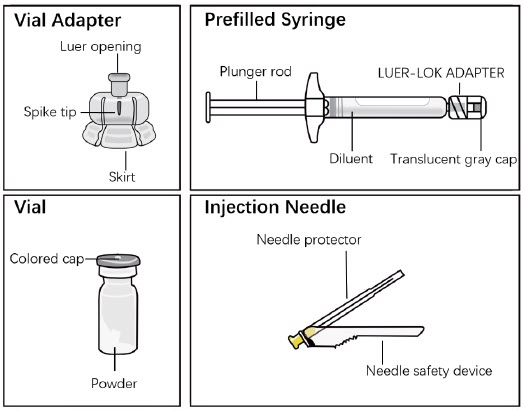
Preparing to Inject RYKINDO®
Step 1. Take out kit and connect vial adapter to vial
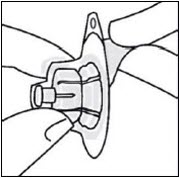
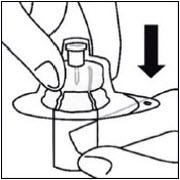
Wait 30 minutes
Remove dose pack from the refrigerator and allow to sit at room temperature for at least 30 minutes before reconstituting.
Do not warm any other way.Remove cap from vial
Flip off colored cap from vial.
Wipe top of the gray stopper with an alcohol swab. Allow to air dry.
Do not remove gray rubber stopper.Prepare vial adapter
Hold sterile blister as shown. Peel back and remove paper backing.
Do not remove vial adapter from blister.
Do not touch spike tip at any time. This will result in contamination.Connect vial adapter to vial
Place vial on a hard surface and hold by the base. Center vial adapter over the gray rubber stopper. Push vial adapter straight down onto vial top until it snaps securely into place.
Do not place vial adapter on at an angle or diluent may leak upon transfer to the vial.
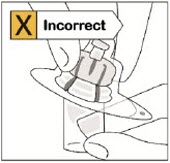
Step 2. Connect prefilled syringe to vial adapter
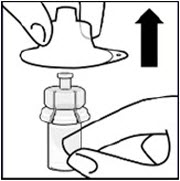
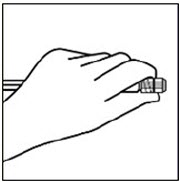
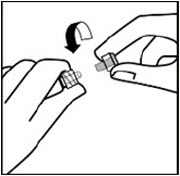
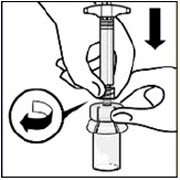
Remove sterile blister

Keep vial vertical to prevent leakage. Hold base of vial and pull up on the sterile blister to remove.
Do not shake.
Do not touch exposed luer opening on vial adapter.
This will result in contamination.Use proper grip
Hold by the LUER-LOK ADAPTER at the tip of the syringe.
Do not hold syringe by the glass barrel during assembly.
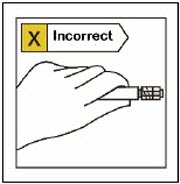
Remove cap
Holding the transparent LUER-LOK ADAPTER, unscrew the translucent gray cap.
Do not snap or cut off the translucent gray cap.
Do not touch syringe tip. This will result in contamination.
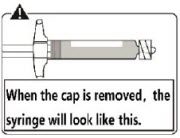
The unscrewed cap can be discarded.Connect syringe to vial adapter
Hold vial adapter by skirt to keep stationary.
Hold syringe by the LUER-LOK ADAPTER then turn it to connect with the luer opening of the vial adapter.
Do not hold the glass syringe barrel. This may cause the LUER-LOK ADAPTER to loosen or detach.
Attach the syringe to the vial adapter with a firm clockwise twisting motion until it feels snug.
Do not over-tighten. Over-tightening may cause the syringe tip to break.Step 3. Reconstitute powder
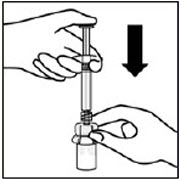
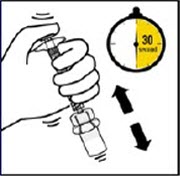
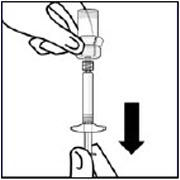
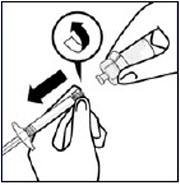
Inject diluent
Inject entire amount of diluent from syringe into the vial.

Suspend powder in diluent
Continuing to hold down the plunger rod, shake vigorously for at least 30 seconds, as shown.
Check the suspension. When properly mixed, the suspension appears uniform, thick and milky in color.
Immediately proceed to the next step so suspension does not settle.Transfer suspension to syringe
Invert vial completely. Slowly pull plunger rod down to withdraw entire contents from the vial into the syringe.Remove vial adapter
Hold the LUER-LOK ADAPTER on the syringe and unscrew from vial adapter.
Tear section of the vial label at the perforation. Apply detached label to the syringe for identification purposes.
Discard both vial and vial adapter appropriately.Step 4. Attach needle
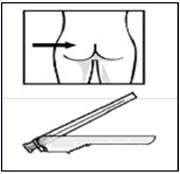
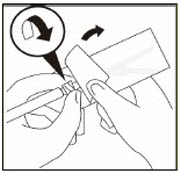
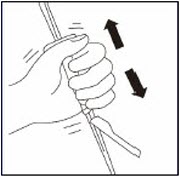
Take out needle
Take out needle for gluteal injection.Attach needle
Peel blister pouch open part way and use to grasp the base of the needle, as shown.
Holding the LUER-LOK ADAPTER on the syringe, attach syringe to needle luer connection with a firm clockwise twisting motion until snug.
Do not touch needle luer opening. This will result in contamination.Resuspend powder
Fully remove the blister pouch.
Just before injection, shake syringe vigorously for 20 to 30 seconds until there is no deposition of powder, as some settling will have occurred.Step 5. Inject RYKINDO®
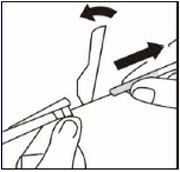
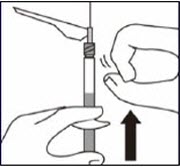
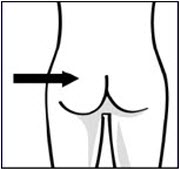
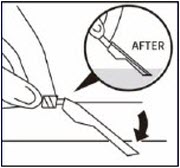
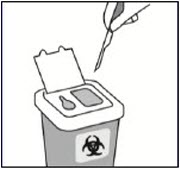
Remove transparent needle protector
Move the needle safety device back towards the syringe, as shown. Then hold the LUER-LOK ADAPTER on syringe and carefully pull the transparent needle protector straight off.
Do not twist transparent needle protector, as the luer connection may loosen.Remove air bubbles
Hold syringe upright and tap gently to make any air bubbles rise to the top.
Slowly and carefully press plunger rod upward to remove air.Inject
Immediately inject entire contents of syringe intramuscularly into the upper outer quadrant of the gluteal muscle of the patient. Do not administer by any other route.Secure needle in safety device
Using one hand, place needle safety device at a 45-degree angle on a hard, flat surface. Press down with a firm, quick motion until needle is fully engaged in safety device.
Avoid needle stick injury:
Do not use two hands.
Do not intentionally disengage or mishandle the needle safety device.
Do not attempt to straighten the needle or engage the safety device if the needle is bent or damaged.Properly dispose of syringes
Check to confirm needle safety device is fully engaged.
Discard in an approved sharps container.Storing RYKINDO®
Store kit in refrigerator at 2° to 8°C (36° to 46°F). Protect from light.
If refrigeration is unavailable, RYKINDO can be stored in its unopened original packaging at temperatures not exceeding 77°F (25°C) for no more than 7 days prior to administration. After removal from the refrigerator, use RYKINDO within 7 days or discard.
For product or service related questions, call 1-800-548-9765 or visit www.rykindo.com.
Shandong Luye Pharmaceutical Co., Ltd.
No.15 Chuangye Road, High-tech Zone,
Yantai, Shandong, 264003
ChinaThis Instruction for Use has been approved by the U.S. Food and Drug Administration.
Issued: 05/2023 -
PRINCIPAL DISPLAY PANEL - 25 mg Kit Carton
25 mg
KitRykindo®
(risperiDONE) for extended-release
injectable suspensionKIT CONTENTS:
- One 25 mg vial of risperiDONE for extended-release injectable suspension
- One pre-filled syringe containing 2 mL of diluent
- One Vial Adapter
- One 20-gauge 2-inch safety needle for gluteal intramuscular injection only
Do not substitute any components of the kit.
For gluteal intramuscular injection only.
Each injection should be administered by a healthcare professional.Rx only
Single doseStore Kit in Refrigerator
(see bottom panel for storage conditions)PLEASE READ COMPLETE
INSTRUCTIONS PRIOR TO USE.NDC: 72526-102-11

-
PRINCIPAL DISPLAY PANEL - 37.5 mg Kit Carton
37.5 mg
KitRykindo®
(risperiDONE) for extended-release
injectable suspensionKIT CONTENTS:
- One 37.5 mg vial of risperiDONE for extended-release injectable suspension
- One pre-filled syringe containing 2 mL of diluent
- One Vial Adapter
- One 20-gauge 2-inch safety needle for gluteal intramuscular injection only
Do not substitute any components of the kit.
For gluteal intramuscular injection only.
Each injection should be administered by a healthcare professional.Rx only
Single doseStore Kit in Refrigerator
(see bottom panel for storage conditions)PLEASE READ COMPLETE
INSTRUCTIONS PRIOR TO USE.NDC: 72526-103-11

-
PRINCIPAL DISPLAY PANEL - 50 mg Kit Carton
50 mg
KitRykindo®
(risperiDONE) for extended-release
injectable suspensionKIT CONTENTS:
- One 50 mg vial of risperiDONE for extended-release injectable suspension
- One pre-filled syringe containing 2 mL of diluent
- One Vial Adapter
- One 20-gauge 2-inch safety needle for gluteal intramuscular injection only
Do not substitute any components of the kit.
For gluteal intramuscular injection only.
Each injection should be administered by a healthcare professional.Rx only
Single doseStore Kit in Refrigerator
(see bottom panel for storage conditions)PLEASE READ COMPLETE
INSTRUCTIONS PRIOR TO USE.NDC: 72526-104-11

-
INGREDIENTS AND APPEARANCE
RYKINDO EXTENDED-RELEASE MICROSPHERES
risperidone kitProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 72526-102 Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 72526-102-11 1 in 1 KIT 06/20/2023 Quantity of Parts Part # Package Quantity Total Product Quantity Part 1 1 VIAL, SINGLE-DOSE 2 mL Part 2 1 SYRINGE, GLASS 2 mL Part 1 of 2 RYKINDO EXTENDED-RELEASE MICROSPHERES
risperidone injection, powder, lyophilized, for suspension, extended releaseProduct Information Item Code (Source) NDC: 72526-202 Route of Administration INTRAMUSCULAR Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength Risperidone (UNII: L6UH7ZF8HC) (Risperidone - UNII:L6UH7ZF8HC) Risperidone 25 mg in 2 mL Inactive Ingredients Ingredient Name Strength DL-LACTIDE AND GLYCOLIDE (75:25) COPOLYMER 140000 ACID (UNII: 1SIA8062RS) DL-LACTIDE AND GLYCOLIDE (50:50) COPOLYMER 46000 ACID (UNII: LQ35R50VR1) MANNITOL (UNII: 3OWL53L36A) Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 72526-202-01 2 mL in 1 VIAL, SINGLE-DOSE; Type 1: Convenience Kit of Co-Package Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date NDA NDA212849 06/20/2023 Part 2 of 2 DILUENT
diluent injectionProduct Information Item Code (Source) NDC: 72526-801 Route of Administration INTRAMUSCULAR Inactive Ingredients Ingredient Name Strength CITRIC ACID MONOHYDRATE (UNII: 2968PHW8QP) SODIUM PHOSPHATE, DIBASIC, ANHYDROUS (UNII: 22ADO53M6F) POLYSORBATE 80 (UNII: 6OZP39ZG8H) CARBOXYMETHYLCELLULOSE SODIUM, UNSPECIFIED (UNII: K679OBS311) SODIUM CHLORIDE (UNII: 451W47IQ8X) SODIUM HYDROXIDE (UNII: 55X04QC32I) WATER (UNII: 059QF0KO0R) Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 72526-801-01 2 mL in 1 SYRINGE, GLASS; Type 1: Convenience Kit of Co-Package Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date NDA NDA212849 06/20/2023 Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date NDA NDA212849 06/20/2023 RYKINDO EXTENDED-RELEASE MICROSPHERES
risperidone kitProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 72526-103 Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 72526-103-11 1 in 1 KIT 06/20/2023 05/27/2026 Quantity of Parts Part # Package Quantity Total Product Quantity Part 1 1 VIAL, SINGLE-DOSE 2 mL Part 2 1 SYRINGE, GLASS 2 mL Part 1 of 2 RYKINDO EXTENDED-RELEASE MICROSPHERES
risperidone injection, powder, lyophilized, for suspension, extended releaseProduct Information Item Code (Source) NDC: 72526-203 Route of Administration INTRAMUSCULAR Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength Risperidone (UNII: L6UH7ZF8HC) (Risperidone - UNII:L6UH7ZF8HC) Risperidone 37.5 mg in 2 mL Inactive Ingredients Ingredient Name Strength DL-LACTIDE AND GLYCOLIDE (75:25) COPOLYMER 140000 ACID (UNII: 1SIA8062RS) DL-LACTIDE AND GLYCOLIDE (50:50) COPOLYMER 46000 ACID (UNII: LQ35R50VR1) MANNITOL (UNII: 3OWL53L36A) Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 72526-203-01 2 mL in 1 VIAL, SINGLE-DOSE; Type 1: Convenience Kit of Co-Package Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date NDA NDA212849 06/20/2023 05/27/2026 Part 2 of 2 DILUENT
diluent injectionProduct Information Item Code (Source) NDC: 72526-801 Route of Administration INTRAMUSCULAR Inactive Ingredients Ingredient Name Strength CITRIC ACID MONOHYDRATE (UNII: 2968PHW8QP) SODIUM PHOSPHATE, DIBASIC, ANHYDROUS (UNII: 22ADO53M6F) POLYSORBATE 80 (UNII: 6OZP39ZG8H) CARBOXYMETHYLCELLULOSE SODIUM, UNSPECIFIED (UNII: K679OBS311) SODIUM CHLORIDE (UNII: 451W47IQ8X) SODIUM HYDROXIDE (UNII: 55X04QC32I) WATER (UNII: 059QF0KO0R) Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 72526-801-01 2 mL in 1 SYRINGE, GLASS; Type 1: Convenience Kit of Co-Package Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date NDA NDA212849 06/20/2023 Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date NDA NDA212849 06/20/2023 RYKINDO EXTENDED-RELEASE MICROSPHERES
risperidone kitProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 72526-104 Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 72526-104-11 1 in 1 KIT 06/20/2023 05/27/2026 Quantity of Parts Part # Package Quantity Total Product Quantity Part 1 1 VIAL, SINGLE-DOSE 2 mL Part 2 1 SYRINGE, GLASS 2 mL Part 1 of 2 RYKINDO EXTENDED-RELEASE MICROSPHERES
risperidone injection, powder, lyophilized, for suspension, extended releaseProduct Information Item Code (Source) NDC: 72526-204 Route of Administration INTRAMUSCULAR Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength Risperidone (UNII: L6UH7ZF8HC) (Risperidone - UNII:L6UH7ZF8HC) Risperidone 50 mg in 2 mL Inactive Ingredients Ingredient Name Strength DL-LACTIDE AND GLYCOLIDE (75:25) COPOLYMER 140000 ACID (UNII: 1SIA8062RS) DL-LACTIDE AND GLYCOLIDE (50:50) COPOLYMER 46000 ACID (UNII: LQ35R50VR1) MANNITOL (UNII: 3OWL53L36A) Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 72526-204-01 2 mL in 1 VIAL, SINGLE-DOSE; Type 1: Convenience Kit of Co-Package Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date NDA NDA212849 06/20/2023 05/27/2026 Part 2 of 2 DILUENT
diluent injectionProduct Information Item Code (Source) NDC: 72526-801 Route of Administration INTRAMUSCULAR Inactive Ingredients Ingredient Name Strength CITRIC ACID MONOHYDRATE (UNII: 2968PHW8QP) SODIUM PHOSPHATE, DIBASIC, ANHYDROUS (UNII: 22ADO53M6F) POLYSORBATE 80 (UNII: 6OZP39ZG8H) CARBOXYMETHYLCELLULOSE SODIUM, UNSPECIFIED (UNII: K679OBS311) SODIUM CHLORIDE (UNII: 451W47IQ8X) SODIUM HYDROXIDE (UNII: 55X04QC32I) WATER (UNII: 059QF0KO0R) Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 72526-801-01 2 mL in 1 SYRINGE, GLASS; Type 1: Convenience Kit of Co-Package Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date NDA NDA212849 06/20/2023 Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date NDA NDA212849 06/20/2023 Labeler - Shandong Luye Pharmaceutical Co., Ltd. (544705452) Establishment Name Address ID/FEI Business Operations Shandong Luye Pharmaceutical Co., Ltd. 544705452 MANUFACTURE(72526-102, 72526-103, 72526-104) , ANALYSIS(72526-102, 72526-103, 72526-104) , PACK(72526-102, 72526-103, 72526-104) , LABEL(72526-102, 72526-103, 72526-104)
Trademark Results [Rykindo]
Mark Image Registration | Serial | Company Trademark Application Date |
|---|---|
 RYKINDO 87131948 5532685 Live/Registered |
Shandong Luye Pharmaceutical Co., Ltd. 2016-08-09 |
© 2026 FDA.report
This site is not affiliated with or endorsed by the FDA.