PHENYLEPHRINE HYDROCHLORIDE injection
Phenylephrine Hydrochloride by
Drug Labeling and Warnings
Phenylephrine Hydrochloride by is a Prescription medication manufactured, distributed, or labeled by General Injectables and Vaccines, Inc.. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
-
HIGHLIGHTS OF PRESCRIBING INFORMATION
Phenylephrine Hydrochloride
These highlights do not include all the information needed to use PHENYLEPHRINE HYDROCHLORIDE INJECTION safely and effectively. See full prescribing information for PHENYLEPHRINE HYDROCHLORIDE INJECTION.
PHENYLEPHRINE HYDROCHLORIDE injection for intravenouse use
Initial U.S. Approval: 1954INDICATIONS AND USAGE
Phenylephrine hydrochloride injection is an alpha-1 adrenergic receptor agonist indicated for the treatment of clinically important hypotension resulting primarily from vasodilation in the setting of anesthesia. (1) (1)
DOSAGE AND ADMINISTRATION
Phenylephrine hydrochloride injection, 10 mg/mL, is injected intravenously either as a bolus or in a dilute solution as a continuous infusion. (2)
Dilute before administration. (2) (2)
Dosing for treatment of hypotension during anesthesia (2)
- Bolus intravenous injection: 40 mcg to 100 mcg every 1 to 2 minutes as needed, not to exceed 200 mcg. (2)
- Intravenous infusion: 10 mcg/min to 35 mcg/min, titrating to effect, not to exceed 200 mcg/min. (2)
The dose should be adjusted according to the pressor response (i.e. titrate to effect). (2) (2)
DOSAGE FORMS AND STRENGTHS
- Injection. (3)
- 1 mL single-dose vials containing 10 mg phenylephrine hydrochloride (10 mg/mL). (3)
CONTRAINDICATIONS
None. (4) (4)
WARNINGS AND PRECAUTIONS
- Extravasation during intravenous administration may cause necrosis or sloughing of tissue. (5.3)
- Severe bradycardia and decreased cardiac output. (5.4)
- Allergic-type reactions: Sulfite. (5.5)
- Concomitant use with oxytocic drugs: Pressor effect of sympathomimetic pressor amines is potentiated. (5.8)
ADVERSE REACTIONS
DRUG INTERACTIONS
- Agonistic effects with monoamine oxidase inhibitors (MAOI), oxytocin and oxytocic drugs, tricyclic antidepressants, angiotensin and aldosterone, atropine, steroids, norepinephrine transporter inhibitors, ergot alkaloids. (7.1)
- Antagonistic effects with α-adrenergic antagonists, phosphodiesterase Type 5 inhibitors, mixed α- and β-receptor antagonists, calcium channel blockers, benzodiazepines and ACE inhibitors, centrally acting sympatholytic agents. (7.2)
USE IN SPECIFIC POPULATIONS
Revised: 1/2020
-
Table of Contents
FULL PRESCRIBING INFORMATION: CONTENTS*
1 INDICATIONS AND USAGE
2 DOSAGE AND ADMINISTRATION
3 DOSAGE FORMS AND STRENGTHS
4 CONTRAINDICATIONS
5 WARNINGS AND PRECAUTIONS
6 ADVERSE REACTIONS
7 DRUG INTERACTIONS
8 USE IN SPECIFIC POPULATIONS
10 OVERDOSAGE
11 DESCRIPTION
12 CLINICAL PHARMACOLOGY
13 NONCLINICAL TOXICOLOGY
14 CLINICAL STUDIES
16 HOW SUPPLIED/STORAGE AND HANDLING
- * Sections or subsections omitted from the full prescribing information are not listed.
- 1 INDICATIONS AND USAGE
-
2 DOSAGE AND ADMINISTRATION
2.1 General Dosage and Administration Instructions
Phenylephrine hydrochloride injection, 10 mg/mL must be diluted before administration as an intravenous bolus or continuous intravenous infusion to achieve the desired concentration:
- Bolus: Dilute with normal saline or 5% dextrose in water.
- Continuous infusion: Dilute with normal saline or 5% dextrose in water.
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration. Do not use if the solution is colored or cloudy, or if it contains particulate matter. The diluted solution should not be held for more than 4 hours at room temperature or for more than 24 hours under refrigerated conditions. Discard any unused portion.
During phenylephrine hydrochloride injection administration:
- Correct intravascular volume depletion.
- Correct acidosis. Acidosis may reduce the effectiveness of phenylephrine.
2.2 Dosing for Treatment of Hypotension during Anesthesia
The following are the recommended dosages for the treatment of hypotension during anesthesia.
- The recommended initial dose is 40 to 100 mcg administered by intravenous bolus. May administer additional boluses every 1 to 2 minutes as needed; not to exceed a total dosage of 200 mcg.
- If blood pressure is below the target goal, start a continuous intravenous infusion with an infusion rate of 10 to 35 mcg/minute; not to exceed 200 mcg/minute.
- Adjust dosage according to the blood pressure goal.
2.3 Prepare a 100 mcg/mL Solution for Bolus Intravenous Administration
For bolus intravenous administration, prepare a solution containing a final concentration of 100 mcg/mL of phenylephrine hydrochloride injection:
- Withdraw 10 mg (1 mL of 10 mg/mL) of phenylephrine hydrochloride and dilute with 99 mL of 5% Dextrose Injection, USP or 0.9% Sodium Chloride Injection, USP.
- Withdraw an appropriate dose from the 100 mcg/mL solution prior to bolus intravenous administration.
2.4 Prepare a Solution for Continuous Intravenous Administration
For continuous intravenous infusion, prepare a solution containing a final concentration of 20 mcg/mL of phenylephrine hydrochloride in 5% Dextrose Injection, USP or 0.9% Sodium Chloride Injection, USP:
- Withdraw 10 mg (1 mL of 10 mg/mL) of phenylephrine hydrochloride and dilute with 500 mL of 5% Dextrose Injection, USP or 0.9% Sodium Chloride Injection, USP.
- 3 DOSAGE FORMS AND STRENGTHS
- 4 CONTRAINDICATIONS
-
5 WARNINGS AND PRECAUTIONS
5.1 Exacerbation of Angina, Heart Failure, or Pulmonary Arterial Hypertension
Because of its increasing blood pressure effects, phenylephrine hydrochloride can precipitate angina in patients with severe arteriosclerosis or history of angina, exacerbate underlying heart failure, and increase pulmonary arterial pressure.
5.2 Peripheral and Visceral Ischemia
Phenylephrine hydrochloride can cause excessive peripheral and visceral vasoconstriction and ischemia to vital organs, particularly in patients with extensive peripheral vascular disease.
5.3 Skin and Subcutaneous Necrosis
Extravasation of phenylephrine hydrochloride can cause necrosis or sloughing of tissue. The infusion site should be checked for free flow. Care should be taken to avoid extravasation of phenylephrine hydrochloride.
5.4 Bradycardia
Phenylephrine hydrochloride can cause severe bradycardia and decreased cardiac output.
5.5 Allergic Reactions
Phenylephrine hydrochloride contains sodium metabisulfite, a sulfite that may cause allergic-type reactions, including anaphylactic symptoms and life-threatening or less severe asthmatic episodes in certain susceptible people. The overall prevalence of sulfite sensitivity in the general population is unknown and probably low. Sulfite sensitivity is seen more frequently in asthmatic than in nonasthmatic people.
5.6 Renal Toxicity
Phenylephrine hydrochloride can increase the need for renal replacement therapy in patients with septic shock. Monitor renal function.
5.7 Risk of Augmented Pressor Affect in Patients with Autonomic Dysfunction
The increasing blood pressure response to adrenergic drugs, including phenylephrine hydrochloride, can be increased in patients with autonomic dysfunction, as may occur with spinal cord injuries.
5.8 Pressor Effect with Concomitant Oxytocic Drugs
Oxytocic drugs potentiate the increasing blood pressure effect of sympathomimetic pressor amines including phenylephrine hydrochloride [see DRUG INTERACTIONS (7.1)], with the potential for hemorrhagic stroke.
-
6 ADVERSE REACTIONS
Adverse reactions to phenylephrine hydrochloride are primarily attributable to excessive pharmacologic activity. Adverse reactions reported in published clinical studies, observational trials, and case reports of phenylephrine hydrochloride are listed below by body system. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to estimate their frequency reliably or to establish a causal relationship to drug exposure.
Cardiac disorders: Reflex bradycardia, lowered cardiac output, ischemia, hypertension, arrhythmias
Gastrointestinal disorders: Epigastric pain, vomiting, nausea
Nervous system disorders: Headache, blurred vision, neck pain, tremors
Vascular disorders: Hypertensive crisis
Respiratory, Thoracic and Mediastinal Disorders: Dyspnea
Skin and subcutaneous tissue disorders: Pruritis
-
7 DRUG INTERACTIONS
7.1 Interactions that Augment Pressor Effect
The increasing blood pressure effect of phenylephrine hydrochloride is increased in patients receiving:
- Monoamine oxidase inhibitors (MAOI)
- Oxytocin and oxytocic drugs
- Tricyclic antidepressants
- Angiotensin, aldosterone
- Atropine
- Steroids, such as hydrocortisone
- Norepinephrine transporter inhibitors, such as atomoxetine
- Ergot alkaloids, such as methylergonovine maleate
7.2 Interactions that Antagonize the Pressor Effect
The increasing blood pressure effect of phenylephrine hydrochloride is decreased in patients receiving:
- α-adrenergic antagonists
- Phosphodiesterase Type 5 inhibitors
- Mixed α- and β-receptor antagonists
- Calcium channel blockers, such as nifedipine
- Benzodiazepines
- ACE inhibitors
- Centrally acting sympatholytic agents, such as reserpine, guanfacine.
-
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Pregnancy Category C
Risk Summary
There are no adequate or well-controlled studies with phenylephrine hydrochloride injection in pregnant women, nor have animal reproduction studies been conducted. Published studies in normotensive pregnant rabbits report early onset labor, increased fetal lethality, and adverse placental effects with subcutaneous phenylephrine administration during gestation at doses approximately 1.9-times the total daily human dose. Published studies in normotensive pregnant sheep report decreased uterine blood flow and decreased PaO2 in the fetus with intravenous phenylephrine administration during late gestation at doses less than and similar to the human dose. It is not known whether phenylephrine hydrochloride, can cause fetal harm when administered to a pregnant woman. Phenylephrine hydrochloride, should be given to a pregnant woman only if the potential benefit justifies the potential risk to the fetus.
Clinical Considerations
Labor and Delivery
The most common maternal adverse reactions reported in published studies of phenylephrine use during neuraxial anesthesia during Cesarean delivery include nausea and vomiting, bradycardia, reactive hypertension, and transient arrhythmias. Phenylephrine, when administered during labor or delivery, does not appear to alter either neonatal Apgar scores or umbilical artery blood-gas status.
Data
Animal Data
Studies in the published literature evaluating subcutaneously administered phenylephrine (0.33 mg/kg, TID) in normotensive pregnant rabbits reported fetal deaths, adverse histopathology findings in the placenta (necrosis, calcification and thickened vascular walls with narrowed lumen) and possible teratogenic effects (one incidence of clubbed feet, partial development of the intestine) when treatment was initiated during the first trimester or later; and premature labor when treatment was initiated at the second trimester or later. The doses administered were 1.9- times the total daily human dose of 10 mg/day based on a body surface area comparison. Published studies in pregnant normotensive sheep demonstrate that intravenous phenylephrine (4 mcg/kg/min for 30 minutes, equivalent to 3.6 to 4.1 mcg/kg/min human equivalent dose based on body surface area) administered during the third trimester of pregnancy decreased uterine blood flow by 42%. This dose is 1.1- to 1.2-times the human bolus dose of 200 mcg/60 kg person based on body surface area. Mean fetal blood pressure and heart rate fluctuated above and below controls by about 7% during the infusion. Fetal PaO2 was significantly decreased by approximately 26% of control during the infusion. Likewise, PaCO2 was increased and pH was decreased. The clinical significance of these findings is not clear; however, the results suggest the potential for cardiovascular effects on the fetus when phenylephrine is used during pregnancy.
8.3 Nursing Mothers
It is not known whether phenylephrine is present in human milk. The developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for phenylephrine hydrochloride and any potential adverse effects on the breastfed child from the drug or from the underlying maternal condition. Exercise caution when phenylephrine hydrochloride injection is administered to a nursing woman.
8.4 Pediatric Use
Safety and effectiveness in pediatric patients have not been established.
8.5 Geriatric Use
Clinical studies of phenylephrine did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy.
8.6 Hepatic Impairment
In patients with liver cirrhosis [Child Pugh Class B and Class C], dose-response data indicate decreased responsiveness to phenylephrine. Start dosing in the recommended dose range but consider that you may need to give more phenylephrine in this population.
8.7 Renal Impairment
In patients with end stage renal disease (ESRD), dose-response data indicate increased responsiveness to phenylephrine. Consider starting at the lower end of the recommended dose range, and adjusting dose based on the target blood pressure goal.
-
10 OVERDOSAGE
Overdose of phenylephrine hydrochloride can cause a rapid rise in blood pressure. Symptoms of overdose include headache, vomiting, hypertension, reflex bradycardia, a sensation of fullness in the head, tingling of the extremities, and cardiac arrhythmias including ventricular extrasystoles and ventricular tachycardia.
-
11 DESCRIPTION
Phenylephrine is an alpha-1 adrenergic receptor agonist. Phenylephrine hydrochloride injection USP, 10 mg/mL is a sterile, nonpyrogenic solution for intravenous use. It must be diluted before administration as an intravenous bolus or continuous intravenous infusion. The chemical name of phenylephrine hydrochloride is (-)-m-hydroxy-α-[(methylamino)methyl]benzyl alcohol hydrochloride, and its structural formula is depicted below:
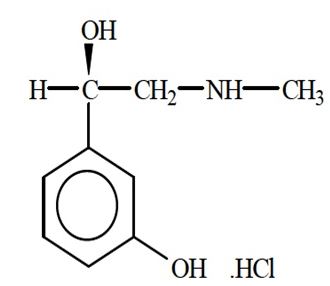
Phenylephrine hydrochloride, USP is a white or practically white crystals with a molecular formula of C9H13NO2 HCl and a molecular weight of 203.67. It is freely soluble in water and in alcohol.
Phenylephrine hydrochloride injection USP, 10 mg/mL is sensitive to light.
Each mL contains: phenylephrine hydrochloride, USP 10 mg, sodium chloride 3.5 mg, trisodium citrate dihydrate 4 mg, citric acid monohydrate 1 mg, and sodium metabisulfite 2 mg in water for injection. The pH is adjusted with sodium hydroxide and/or hydrochloric acid if necessary. The pH range is 3.5 to 5.5.
-
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Phenylephrine hydrochloride is an α-1 adrenergic receptor agonist.
12.2 Pharmacodynamics
Interaction of phenylephrine with α1-adrenergic receptors on vascular smooth muscle cells causes activation of the cells and results in vasoconstriction. Following phenylephrine hydrochloride intravenous administration, increases in systolic and diastolic blood pressures, mean arterial blood pressure, and total peripheral vascular resistance are observed. The onset of blood pressure increase following an intravenous bolus phenylephrine hydrochloride administration is rapid, typically within minutes. As blood pressure increases following intravenous administration, vagal activity also increases, resulting in reflex bradycardia. Phenylephrine has activity on most vascular beds, including renal, pulmonary, and splanchnic arteries.
12.3 Pharmacokinetics
Following an intravenous infusion of phenylephrine hydrochloride, the observed effective half-life was approximately 5 minutes. The steady-state volume of distribution of approximately 340 L suggests a high distribution into organs and peripheral tissues. The average total serum clearance is approximately 2100 mL/min. The observed phenylephrine plasma terminal elimination half-life was 2.5 hours.
Phenylephrine is metabolized primarily by monoamine oxidase and sulfotransferase. After intravenous administration of radiolabeled phenylephrine, approximately 80% of the total dose was eliminated within first 12 hours; and approximately 86% of the total dose was recovered in the urine within 48 hours. The excreted unchanged parent drug was 16% of the total dose in the urine at 48 hours post intravenous administration. There are two major metabolites, with approximately 57 and 8% of the total dose excreted as m-hydroxymandelic acid and sulfate conjugates, respectively. The metabolites are considered not pharmacologically active.
-
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis: Long-term animal studies that evaluated the carcinogenic potential of orally administered phenylephrine hydrochloride in F344/N rats and B6C3F, mice were completed by the National Toxicology Program using the dietary route of administration. There was no evidence of carcinogenicity in mice administered approximately 270 mg/kg/day (131-times the maximum recommended daily dose of < 10 mg/day) or rats administered approximately 50 mg/kg/day (48-times the maximum recommended daily dose of < 10 mg/day) based on body surface area comparisons.
Mutagenesis: Phenylephrine hydrochloride tested negative in the in vitro bacterial reverse mutation assay (S.typhimurium strains TA98, TA100, TA1535 and TA1537), the in vitro chromosomal aberrations assay, the in vitro sister chromatid exchange assay, and the in vivo rat micronucleus assay. Positive results were reported in only one of two replicates of the in vitro mouse lymphoma assay.
Impairment of Fertility: Studies to evaluate the effect of phenylephrine on fertility have not been conducted.
-
14 CLINICAL STUDIES
The evidence for the efficacy of phenylephrine hydrochloride is derived from studies of phenylephrine hydrochloride in the published literature. The literature support includes 16 studies evaluating the use of intravenous phenylephrine to treat hypotension during anesthesia. The 16 studies include 9 studies where phenylephrine was used in low-risk (ASA 1 and 2) pregnant women undergoing neuraxial anesthesia during Cesarean delivery, 6 studies in non-obstetric surgery under general anesthesia, and 1 study in non-obstetric surgery under combined general and neuraxial anesthesia. Phenylephrine has been shown to raise systolic and mean blood pressure when administered either as a bolus dose or by continuous infusion following the development of hypotension during anesthesia.
-
16 HOW SUPPLIED/STORAGE AND HANDLING
Phenylephrine Hydrochloride Injection, USP is a sterile, clear, colorless solution and supplied in 1 mL single-dose glass vials. Each mL contains phenylephrine hydrochloride USP, 10 mg.
10 mg/mL (1 mL)
1 mL Single-dose Vial: NDC: 70121-1577-1
25 Vials in a Carton: NDC: 70121-1577-5
Store phenylephrine hydrochloride injection USP, 10 mg/mL at 20° to 25°C (68° to 77°F); excursions permitted between 15° to 30°C (59° to 86°F) [see USP Controlled Room Temperature].
Protect from light. Store in carton until time of use. Vial stoppers are not manufactured with natural rubber latex.
The diluted solution should not be held for more than 4 hours at room temperature or for more than 24 hours under refrigerated conditions. Discard any unused portion.
-
17 PATIENT COUNSELING INFORMATION
If applicable, inform patients, family member, or caregiver that certain medication conditions and mediations might influence how phenylephrine hydrochloride injection works.
Manufactured by:
Amneal Pharmaceuticals Pvt. Ltd.
Parenteral Unit
Ahmedabad 382213, INDIA
Distributed by:
Amneal Biosciences LLC
Bridgewater, NJ 08807
Rev. 07-2018-01
- SAMPLE PACKAGE LABEL
-
INGREDIENTS AND APPEARANCE
PHENYLEPHRINE HYDROCHLORIDE
phenylephrine hydrochloride injectionProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 52584-577(NDC:70121-1577) Route of Administration INTRAVENOUS Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength PHENYLEPHRINE HYDROCHLORIDE (UNII: 04JA59TNSJ) (PHENYLEPHRINE - UNII:1WS297W6MV) PHENYLEPHRINE HYDROCHLORIDE 10 mg in 1 mL Inactive Ingredients Ingredient Name Strength CITRIC ACID MONOHYDRATE (UNII: 2968PHW8QP) 1 mg in 1 mL HYDROCHLORIC ACID (UNII: QTT17582CB) SODIUM CHLORIDE (UNII: 451W47IQ8X) 3.5 mg in 1 mL SODIUM HYDROXIDE (UNII: 55X04QC32I) SODIUM METABISULFITE (UNII: 4VON5FNS3C) 2 mg in 1 mL TRISODIUM CITRATE DIHYDRATE (UNII: B22547B95K) 4 mg in 1 mL WATER (UNII: 059QF0KO0R) Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 52584-577-01 1 in 1 BAG 07/23/2019 1 1 mL in 1 VIAL, SINGLE-DOSE; Type 0: Not a Combination Product Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA211079 07/23/2019 Labeler - General Injectables and Vaccines, Inc. (108250663)
© 2026 FDA.report
This site is not affiliated with or endorsed by the FDA.
