CLOBETASOL PROPIONATE cream
Clobetasol Propionate by
Drug Labeling and Warnings
Clobetasol Propionate by is a Prescription medication manufactured, distributed, or labeled by Zydus Lifesciences Limited. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
- SPL UNCLASSIFIED SECTION
-
DESCRIPTION
Clobetasol propionate cream USP, 0.05% contain the active compound clobetasol propionate, a synthetic corticosteroid, for topical dermatologic use. Clobetasol, an analog of prednisolone, has a high degree of glucocorticoid activity and a slight degree of mineralocorticoid activity.
Chemically, clobetasol propionate is (11ß,16ß)-21-chloro-9-fluoro-11-hydroxy-16-methyl-17-(1-oxopropoxy)-pregna-1,4-diene-3,20-dione, and it has the following structural formula:
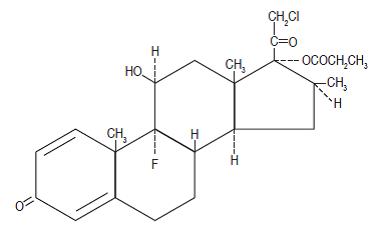
Clobetasol propionate has the molecular formula C25H32ClFO5 and a molecular weight of 467. It is a white to cream crystalline powder and soluble in acetone, in dimethyl sulfoxide, in chloroform, in methanol, and in dioxane; sparingly soluble in ethanol; slightly soluble in benzene and diethyl ether and practically insoluble in water.
Clobetasol propionate cream USP, 0.05% contains clobetasol propionate, USP 0.5 mg/g in a cream base of propylene glycol, cetyl alcohol, stearyl alcohol, citric acid monohydrate, sodium citrate anhydrous, methylparaben, propylparaben, ethylene glycol stearate, PEG-400 monostearate, polysorbate 60, lanolin oil, white petrolatum, and purified water.
-
CLINICAL PHARMACOLOGY
Like other topical corticosteroids, clobetasol propionate has anti-inflammatory, antipruritic, and vasoconstrictive properties. The mechanism of the anti-inflammatory activity of the topical steroids, in general, is unclear. However, corticosteroids are thought to act by the induction of phospholipase A2 inhibitory proteins, collectively called lipocortins. It is postulated that these proteins control the biosynthesis of potent mediators of inflammation such as prostaglandins and leukotrienes by inhibiting the release of their common precursor, arachidonic acid. Arachidonic acid is released from membrane phospholipids by phospholipase A2.
Pharmacokinetics
The extent of percutaneous absorption of topical corticosteroids is determined by many factors, including the vehicle and the integrity of the epidermal barrier. Occlusive dressing with hydrocortisone for up to 24 hours has not been demonstrated to increase penetration; however, occlusion of hydrocortisone for 96 hours markedly enhances penetration. Topical corticosteroids can be absorbed from normal intact skin. Inflammation and/or other disease processes in the skin may increase percutaneous absorption.
Studies performed with clobetasol propionate cream indicate that they are in the super-high range of potency as compared with other topical corticosteroids.
-
INDICATIONS AND USAGE
Clobetasol propionate cream is super-high potency corticosteroid formulations indicated for the relief of the inflammatory and pruritic manifestations of corticosteroid-responsive dermatoses. Treatment beyond 2 consecutive weeks is not recommended, and the total dosage should not exceed 50 g/week because of the potential for the drug to suppress the hypothalamic-pituitary-adrenal (HPA) axis. Use in pediatric patients under 12 years of age is not recommended.
As with other highly active corticosteroids, therapy should be discontinued when control has been achieved. If no improvement is seen within 2 weeks, reassessment of the diagnosis may be necessary.
- CONTRAINDICATIONS
-
PRECAUTIONS
General
Clobetasol propionate cream should not be used in the treatment of rosacea or perioral dermatitis, and should not be used on the face, groin, or axillae.
Systemic absorption of topical corticosteroids can produce reversible HPA axis suppression with the potential for glucocorticosteroid insufficiency after withdrawal from treatment. Manifestations of Cushing syndrome, hyperglycemia, and glucosuria can also be produced in some patients by systemic absorption of topical corticosteroids while on therapy.
Patients applying a topical steroid to a large surface area or to areas under occlusion should be evaluated periodically for evidence of HPA axis suppression. This may be done by using the ACTH stimulation, A.M. plasma cortisol, and urinary free cortisol tests. Patients receiving super-potent corticosteroids should not be treated for more than 2 weeks at a time, and only small areas should be treated at any one time due to the increased risk of HPA suppression.
Clobetasol propionate cream produced HPA axis suppression when used at doses as low as 2 g/day for 1 week in patients with eczema.
If HPA axis suppression is noted, an attempt should be made to withdraw the drug, to reduce the frequency of application, or to substitute a less potent corticosteroid. Recovery of HPA axis function is generally prompt upon discontinuation of topical corticosteroids. Infrequently, signs and symptoms of glucocorticosteroid insufficiency may occur that require supplemental systemic corticosteroids. For information on systemic supplementation, see prescribing information for those products.
Pediatric patients may be more susceptible to systemic toxicity from equivalent doses due to their larger skin surface to body mass ratios (see PRECAUTIONS: Pediatric Use).
If irritation develops, clobetasol propionate cream should be discontinued and appropriate therapy instituted. Allergic contact dermatitis with corticosteroids is usually diagnosed by observing a failure to heal rather than noting a clinical exacerbation as with most topical products not containing corticosteroids. Such an observation should be corroborated with appropriate diagnostic patch testing.
If concomitant skin infections are present or develop, an appropriate antifungal or antibacterial agent should be used. If a favorable response does not occur promptly, use of clobetasol propionate cream should be discontinued until the infection has been adequately controlled.
Information for Patients
Patients using topical corticosteroids should receive the following information and instructions:
1. This medication is to be used as directed by the physician. It is for external use only. Avoid contact with the eyes.
2. This medication should not be used for any disorder other than that for which it was prescribed.
3. The treated skin area should not be bandaged, otherwise covered, or wrapped so as to be occlusive unless directed by the physician.
4. Patients should report any signs of local adverse reactions to the physician.
Laboratory Tests
The following tests may be helpful in evaluating patients for HPA axis suppression:
ACTH stimulation test
A.M. plasma cortisol test
Urinary free cortisol test
Carcinogenesis, Mutagenesis, Impairment of Fertility
Long-term animal studies have not been performed to evaluate the carcinogenic potential of clobetasol propionate.
Studies in the rat following subcutaneous administration at dosage levels up to 50 mcg/kg/day revealed that the females exhibited an increase in the number of resorbed embryos and a decrease in the number of living fetuses at the highest dose.
Clobetasol propionate was nonmutagenic in 3 different test systems: the Ames test, the Saccharomyces cerevisiaegene conversion assay, and the E. coli B WP2 fluctuation test.
Pregnancy
Pregnancy Category C.
Corticosteroids have been shown to be teratogenic in laboratory animals when administered systemically at relatively low dosage levels. Some corticosteroids have been shown to be teratogenic after dermal application to laboratory animals.
Clobetasol propionate has not been tested for teratogenicity when applied topically; however, it is absorbed percutaneously, and when administered subcutaneously it was a significant teratogen in both the rabbit and mouse. Clobetasol propionate has greater teratogenic potential than steroids that are less potent.
Teratogenicity studies in mice using the subcutaneous route resulted in fetotoxicity at the highest dose tested (1 mg/kg) and teratogenicity at all dose levels tested down to 0.03 mg/kg. These doses are approximately 1.4 and 0.04 times, respectively, the human topical dose of clobetasol propionate cream. Abnormalities seen included cleft palate and skeletal abnormalities.
In rabbits, clobetasol propionate was teratogenic at doses of 3 and 10 mcg/kg. These doses are approximately 0.02 and 0.05 times, respectively, the human topical dose of clobetasol propionate cream. Abnormalities seen included cleft palate, cranioschisis, and other skeletal abnormalities.
There are no adequate and well-controlled studies of the teratogenic potential of clobetasol propionate in pregnant women. Clobetasol propionate cream should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
Nursing Mothers
Systemically administered corticosteroids appear in human milk and could suppress growth, interfere with endogenous corticosteroid production, or cause other untoward effects. It is not known whether topical administration of corticosteroids could result in sufficient systemic absorption to produce detectable quantities in human milk. Because many drugs are excreted in human milk, caution should be exercised when clobetasol propionate cream is administered to a nursing woman.
Pediatric Use
Safety and effectiveness of clobetasol propionate cream in pediatric patients have not been established. Use in pediatric patients under 12 years of age is not recommended. Because of a higher ratio of skin surface area to body mass, pediatric patients are at a greater risk than adults of HPA axis suppression and Cushing syndrome when they are treated with topical corticosteroids. They are therefore also at greater risk of adrenal insufficiency during or after withdrawal of treatment. Adverse effects including striae have been reported with inappropriate use of topical corticosteroids in infants and children.
HPA axis suppression, Cushing syndrome, linear growth retardation, delayed weight gain, and intracranial hypertension have been reported in children receiving topical corticosteroids. Manifestations of adrenal suppression in children include low plasma cortisol levels and an absence of response to ACTH stimulation. Manifestations of intracranial hypertension include bulging fontanelles, headaches, and bilateral papilledema.
Geriatric Use
A limited number of patients at or above 65 years of age have been treated with clobetasol propionate cream (n=231) and with clobetasol propionate ointment (n=101) in US and non-US clinical trials. While the number of patients is too small to permit separate analysis of efficacy and safety, the adverse reactions reported in this population were similar to those reported by younger patients. Based on available data, no adjustment of dosage of clobetasol propionate cream in geriatric patients is warranted.
-
ADVERSE REACTIONS
In controlled clinical trials, the most frequent adverse reactions reported for clobetasol propionate cream were burning and stinging sensation in 1% of treated patients. Less frequent adverse reactions were itching , skin atrophy, and cracking and fissuring of the skin. In controlled clinical trials, the most frequent adverse events reported for clobetasol propionate ointment were burning sensation, irritation, and itching in 0.5% of treated patients. Less frequent adverse reactions were stinging, cracking , erythema, folliculitis, numbness of fingers, skin atrophy, and telangiectasia.
Cushing syndrome has been reported in infants and adults as a result of prolonged use of topical clobetasol propionate formulations.
The following additional local adverse reactions have been reported with topical corticosteroids, and they may occur more frequently with the use of occlusive dressings and higher potency corticosteroids. These reactions are listed in an approximately decreasing order of occurrence: dryness, acneiform eruptions, hypopigmentation, perioral dermatitis, allergic contact dermatitis, secondary infection, irritation, striae, and miliaria.
-
OVERDOSAGE
Topically applied clobetasol propionate cream can be absorbed in sufficient amounts to produce systemic effects (see PRECAUTIONS).
-
DOSAGE AND ADMINISTRATION
Apply a thin layer of clobetasol propionate cream to the affected skin areas twice daily and rub in gently and completely (see INDICATIONS AND USAGE).
Clobetasol propionate cream is super-high potency topical corticosteroids; therefore, treatment should be limited to 2 consecutive weeks and amounts greater than 50 g/week should not be used.
As with other highly active corticosteroids, therapy should be discontinued when control has been achieved. If no improvement is seen within 2 weeks, reassessment of diagnosis may be necessary.
Clobetasol propionate cream should not be used with occlusive dressings.
Geriatric Use
In studies where geriatric patients (65 years of age or older, see PRECAUTIONS) have been treated with clobetasol propionate cream, safety did not differ from that in younger patients; therefore, no dosage adjustment is recommended.
-
HOW SUPPLIED
Clobetasol Propionate Cream USP, 0.05% is white to off-white cream supplied in:
NDC: 70771-1442-1 in tube of 15 g
NDC: 70771-1442-2 in tube of 30 g
NDC: 70771-1442-4 in tube of 45 g
NDC: 70771-1442-3 in tube of 60 g
- SPL UNCLASSIFIED SECTION
- SPL UNCLASSIFIED SECTION
- PACKAGE LABEL.PRINCIPAL DISPLAY PANEL
-
INGREDIENTS AND APPEARANCE
CLOBETASOL PROPIONATE
clobetasol propionate creamProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 70771-1442 Route of Administration TOPICAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength CLOBETASOL PROPIONATE (UNII: 779619577M) (CLOBETASOL - UNII:ADN79D536H) CLOBETASOL PROPIONATE 0.5 mg in 1 g Inactive Ingredients Ingredient Name Strength PROPYLENE GLYCOL (UNII: 6DC9Q167V3) CETYL ALCOHOL (UNII: 936JST6JCN) STEARYL ALCOHOL (UNII: 2KR89I4H1Y) CITRIC ACID MONOHYDRATE (UNII: 2968PHW8QP) ANHYDROUS TRISODIUM CITRATE (UNII: RS7A450LGA) METHYLPARABEN (UNII: A2I8C7HI9T) PROPYLPARABEN (UNII: Z8IX2SC1OH) POLYSORBATE 60 (UNII: CAL22UVI4M) LANOLIN OIL (UNII: OVV5IIJ58F) PETROLATUM (UNII: 4T6H12BN9U) WATER (UNII: 059QF0KO0R) GLYCOL STEARATE (UNII: 0324G66D0E) PEG-8 STEARATE (UNII: 2P9L47VI5E) Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 70771-1442-1 1 in 1 CARTON 01/09/2019 1 15 g in 1 TUBE; Type 0: Not a Combination Product 2 NDC: 70771-1442-2 1 in 1 CARTON 01/09/2019 2 30 g in 1 TUBE; Type 0: Not a Combination Product 3 NDC: 70771-1442-4 1 in 1 CARTON 01/09/2019 3 45 g in 1 TUBE; Type 0: Not a Combination Product 4 NDC: 70771-1442-3 1 in 1 CARTON 01/09/2019 4 60 g in 1 TUBE; Type 0: Not a Combination Product Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA211074 01/09/2019 Labeler - Cadila Healthcare Limited (918596198) Registrant - Cadila Healthcare Limited (650650802) Establishment Name Address ID/FEI Business Operations Cadila Healthcare Limited 650650802 ANALYSIS(70771-1442) , MANUFACTURE(70771-1442)
© 2026 FDA.report
This site is not affiliated with or endorsed by the FDA.

