DEXTROSE- dextrose monohydrate injection
Dextrose by
Drug Labeling and Warnings
Dextrose by is a Prescription medication manufactured, distributed, or labeled by Baxter Healthcare Company, Baxter Healthcare Corporation, SITEC LABS LIMITED. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
-
HIGHLIGHTS OF PRESCRIBING INFORMATION
These highlights do not include all the information needed to use DEXTROSE INJECTION safely and effectively. See full prescribing information for DEXTROSE INJECTION.
Initial U.S. Approval: 1940RECENT MAJOR CHANGES
INDICATIONS AND USAGE
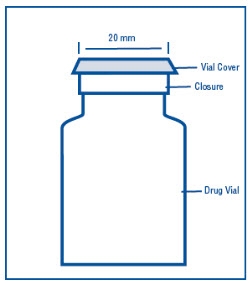
Dextrose Injection is indicated as a source of calories and water and may also be used as diluent for reconstitution of a powdered or liquid (up to 10 mL) drug product packaged in a vial with a 20 mm closure. (1)
DOSAGE AND ADMINISTRATION
DOSAGE FORMS AND STRENGTHS
Injection: 5% (0.05 grams/mL), 5 grams of dextrose hydrous per 100 mL in 50 mL and 100 mL single-dose, partial-fill flexible containers: (3)
WARNINGS AND PRECAUTIONS
- Hyperglycemia or Hyperosmolar Hyperglycemic State: Monitor blood glucose and administer insulin as needed. (5.1)
- Hypersensitivity Reactions: Monitor for signs and symptoms and discontinue infusion if reactions occur. (5.2)
- Vein Damage and Thrombosis: Consider central vein when administering more than 5% dextrose or with an osmolarity of ≥ 900 mOsm/L or when there is peripheral vein irritation, phlebitis, and/or associated pain. (2.2, 5.3)
- Hyponatremia: Avoid in patients with or at risk for hyponatremia. If use cannot be avoided, monitor serum sodium concentrations (5.4)
- Electrolyte Imbalance and Fluid Overload: Avoid in patients with or at risk for fluid and/or solute overloading. If use cannot be avoided, monitor daily fluid balance, electrolyte concentrations, and acid-base balance, as needed and especially during prolonged use (5.5)
- Refeeding Syndrome: Monitor severely undernourished patients and slowly increase nutrient intake. (5.6)
ADVERSE REACTIONS
The most common adverse reactions are, hyperglycemia, hypersensitivity reactions, hyponatremia, infection both systemic and at the injection site, vein thrombosis or phlebitis, and electrolyte imbalance. (6)
To report SUSPECTED ADVERSE REACTIONS, contact Baxter Healthcare at 1-866-888-2472 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
USE IN SPECIFIC POPULATIONS
Pediatric Use: Increased risk of hypoglycemia/hyperglycemia; monitor serum glucose concentrations. (8.4)
See 17 for PATIENT COUNSELING INFORMATION.
Revised: 2/2020
-
Table of Contents
FULL PRESCRIBING INFORMATION: CONTENTS*
1 INDICATIONS AND USAGE
2 DOSAGE AND ADMINISTRATION
2.1 Important Administration Instructions
2.2 Recommended Dosage
2.3 Instructions for Use
3 DOSAGE FORMS AND STRENGTHS
4 CONTRAINDICATIONS
5 WARNINGS AND PRECAUTIONS
5.1 Hyperglycemia and Hyperosmolar Hyperglycemic State
5.2 Hypersensitivity Reactions
5.3 Vein Damage and Thrombosis
5.4 Hyponatremia
5.5 Electrolyte Imbalance and Fluid Overload
5.6 Refeeding Syndrome
6 ADVERSE REACTIONS
7 DRUG INTERACTIONS
7.1 Other Products that Affect Glycemic Control or Fluid and/or Electrolyte Balance
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
8.2 Lactation
8.4 Pediatric Use
8.5 Geriatric Use
10 OVERDOSAGE
11 DESCRIPTION
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
16 HOW SUPPLIED/STORAGE AND HANDLING
17 PATIENT COUNSELING INFORMATION
- * Sections or subsections omitted from the full prescribing information are not listed.
- 1 INDICATIONS AND USAGE
-
2 DOSAGE AND ADMINISTRATION
2.1 Important Administration Instructions
- Dextrose Injection is intended for intravenous use.
- Peripheral administration of 5% dextrose is generally acceptable, however, consider central vein when administering more than 5% dextrose or with an osmolarity of at least 900 mOsm/L or when there is peripheral vein irritation, phlebitis, and/or associated pain [see Warnings and Precautions (5.3)].
- Do not administer Dextrose Injection simultaneously with blood products through the same administration set because of the possibility of pseudoagglutination or hemolysis.
- To prevent air embolism, use a non-vented infusion set or close the vent on a vented set, avoid multiple connections, do not connect flexible containers in series, fully evacuate residual gas in the container prior to administration, do not pressurize the flexible container to increase flow rates, and if administration is controlled by a pumping device, turn off pump before the container runs dry.
- Prior to infusion, visually inspect the diluted dextrose solution for particulate matter. The solution should be clear and there should be no precipitates. Do not administer unless solution is clear and container is undamaged.
- Use of a final filter is recommended during administration of parenteral solutions, where possible.
2.2 Recommended Dosage
The choice of dextrose concentration, rate and volume depends on the age, weight, clinical and metabolic conditions of the patient and concomitant therapy. Electrolyte supplementation may be indicated according to the clinical needs of the patient.
The administration rate should be governed, especially for premature infants with low birth weight, during the first few days of therapy, by the patient’s tolerance to dextrose.
Increase the infusion rate gradually as indicated by frequent monitoring of blood glucose concentrations [see Warnings and Precautions (5.1), Use in Specific Populations (8.4)].
2.3 Instructions for Use
To Open
- Do not remove from overpouch until ready to use.
- Tear overwrap sharply down from the slit and remove solution container. Small amounts of moisture may be found on the solution container from water permeating from inside the container. The amount of permeated water is insufficient to affect the solution significantly. If larger amounts of water are found, the container should be checked for tears or leaks.
-
Visually inspect the container. Some opacity of the plastic due to moisture absorption during the sterilization process may be observed. This is normal and does not affect the solution quality or safety. The opacity will diminish gradually. Evaluate the following:
- If the outlet port protector is damaged, detached, or not present, discard container.
- Check to ensure the solution is clear and there are no precipitates. Discard if there is a color change and/or the appearance of precipitates, insoluble complexes or crystals.
- Check for minute leaks by separately squeezing the inner bag firmly. If leaks are found, discard container.
- Check that the vial adaptor cover is intact. If the vial adaptor cover is not intact, discard product.
Preparation for Administration
- Instructions for Assembly and Reconstitution: (Steps 1-3 for Assembly and steps 4-6 for Reconstitution)
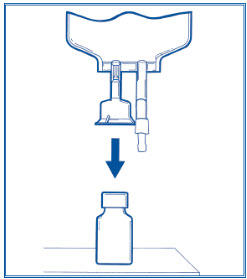
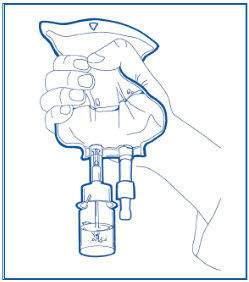
- Step 1: Remove vial cover and disinfect stopper.
Step 2: Peel off foil cover. Inspect adaptor for moisture. Discard if moisture is found.
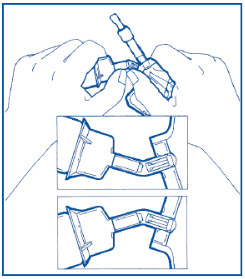
Step 3: Place vial upright and hold firmly. Push adaptor down until vial snaps in place. DO NOT TWIST. Pull vial to ensure fully seated.
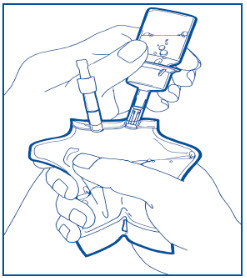
Step 4: Squeeze the bag and check vial. Use only if vial is fully seated and dry. Bend up then down to break the seal.
Step 5: Hold bag with vial down. Squeeze solution into vial until half full. Shake to suspend drug in solution.
Step 6: Hold bag with vial upside down. Squeeze bag to force air into vial. Release to drain suspended drug from vial. Repeat steps 5 and 6 until vial is empty of drug and solution is thoroughly mixed. Ensure drug is completely dissolved. Do Not Remove Drug Vial.
- Inspect the container to ensure precipitates have not formed during the mixing or addition of additives and that the solution has not changed color. Discard the admixture if either are observed.
- Insert transfer set into prepared solution container to be transferred. Follow directions accompanying transfer set.
- Remove port protector and attached administration set per its directions.
- Transfer solution by gravity. Ensure that vial is empty of drug and solution. Repeat step 6 if drug and solution remain in vial.
- Check for leaks.
To Add Medication
- Additives may be incompatible. Complete information is not available. Do not use additives known or determined to be incompatible.
- Consult with pharmacist, if available. If, in the informed judgment of the healthcare provider, it is deemed advisable to introduce additives, use aseptic technique.
- When introducing additives, consult the instructions for use of the medication to be added and other relevant literature.
- Before adding a substance or medication, verify that it is soluble and/or stable in Dextrose Injection and that the pH range of Dextrose Injection is appropriate.
Storage
- Use promptly after admixing or dilution; do not store solutions containing additives.
- Single-dose container.
- Discard unused portion.
- 3 DOSAGE FORMS AND STRENGTHS
-
4 CONTRAINDICATIONS
The use of Dextrose Injection is contraindicated in patients with:
- Clinically significant hyperglycemia [see Warnings and Precautions (5.1)].
- Known hypersensitivity to dextrose [see Warnings and Precautions (5.2)]
-
5 WARNINGS AND PRECAUTIONS
5.1 Hyperglycemia and Hyperosmolar Hyperglycemic State
The use of dextrose infusions in patients with impaired glucose tolerance may worsen hyperglycemia. Administration of dextrose at a rate exceeding the patient’s utilization rate may lead to hyperglycemia, coma, and death.
Hyperglycemia is associated with an increase in serum osmolality, resulting in osmotic diuresis, dehydration and electrolyte losses [see Warnings and Precautions (5.5)]. Patients with underlying CNS disease and renal impairment who receive dextrose infusions, may be at greater risk of developing hyperosmolar hyperglycemic state.
Monitor blood glucose levels and treat hyperglycemia to maintain levels within normal limits while administering Dextrose Injection. Insulin may be administered or adjusted to maintain optimal blood glucose levels during Dextrose Injection administration.
5.2 Hypersensitivity Reactions
Hypersensitivity and infusion reactions including anaphylaxis, have been reported with Dextrose Injection [see Adverse Reactions (6)]. Stop infusion immediately and treat patient accordingly if signs or symptoms of a hypersensitivity reaction develop. Appropriate therapeutic countermeasures must be instituted as clinically indicated.
5.3 Vein Damage and Thrombosis
Peripheral administration of 5% Dextrose Injection is generally acceptable, however, consider central vein when administering more than 5% dextrose or with an osmolarity of ≥ 900 mOsm/L or when there is peripheral vein irritation, phlebitis, and/or associated pain [see Dosage and Administration (2.1)]. The infusion of hypertonic solutions into a peripheral vein may result in vein irritation, vein damage, and/or thrombosis. The primary complication of peripheral access is venous thrombophlebitis, which manifests as pain, erythema, tenderness or a palpable cord. Remove the catheter as soon as possible, if thrombophlebitis develops.
5.4 Hyponatremia
5% Dextrose Injection is an isotonic solution [see Description, Table 1 (11)]. In the body, however, glucose containing fluids can become extremely physiologically hypotonic due to rapid glucose metabolization. Monitoring of serum sodium is particularly important for hypotonic fluids.
Depending on the tonicity of the solution, the volume and rate of infusion, and depending on a patient’s underlying clinical condition and capability to metabolize glucose, intravenous administration of glucose can cause electrolyte disturbances, most importantly hypo- or hyperosmotic hyponatremia. Monitor serum sodium to minimize the risk of hyponatremia.
The risk for hyponatremia is increased in pediatric patients, elderly patients, postoperative patients, those with psychogenic polydipsia, and in patients treated with medications that increase the risk of hyponatremia (such as diuretics, certain antiepileptic and psychotropic medications). Close clinical monitoring may be warranted.
Acute hyponatremia can lead to acute hyponatremic encephalopathy characterized by headache, nausea, seizures, lethargy and vomiting. Patients with brain edema are at particular risk of severe, irreversible and life-threatening brain injury. Patients at increased risk for developing complications of hyponatremia, such as hyponatremic encephalopathy include pediatric patients; women, in particular, premenopausal women; patients with hypoxemia; and in patients with underlying central nervous system disease [see Use in Specific Populations (8.4, 8.5)].
Avoid Dextrose Injection in patients with or at risk for hyponatremia. If use cannot be avoided, monitor serum sodium concentrations.
Rapid correction of hyponatremia is potentially dangerous with risk of serious neurologic complications. Brain adaptations reducing risk of cerebral edema make the brain vulnerable to injury when chronic hyponatremia is too rapidly corrected, which is known as osmotic demyelination syndrome (ODS). To avoid complications, monitor serum sodium and chloride concentrations, fluid status, acid-base balance, and signs of neurologic complications.
High volume infusion must be used with close monitoring in patients with cardiac or pulmonary failure, and in patients with non-osmotic vasopressin release (including SIADH), due to the risk of hospital-acquired hyponatremia.
5.5 Electrolyte Imbalance and Fluid Overload
Electrolyte deficits, particularly in serum potassium and phosphate, may occur during prolonged use of concentrated dextrose solutions.
Depending on the volume and rate of infusion, the intravenous administration of dextrose solutions can cause fluid and/or solute overloading resulting in dilution of serum electrolyte concentrations (including hypoosmotic hyponatremia, overhydration, congested states or pulmonary edema. The risk of dilutional states is inversely proportional to the electrolyte concentrations in the administered solution. The risk of solute overload causing congested states with peripheral and pulmonary edema is directly proportional to the electrolyte concentrations in the solution.
Avoid Dextrose Injection in patients with or at risk for fluid and/or solute overloading. If use cannot be avoided, monitor fluid balance, blood electrolyte levels, concentration of glucose, acid-base balance, correct fluid and electrolyte imbalances during prolonged parenteral therapy or whenever the condition of the patient or the rate of administration warrants such evaluation. Additional monitoring is recommended for patients with water and electrolyte disturbances that could be aggravated by increased glucose, insulin administration and/or free water load.
Patients at increased risk for developing hyponatremic encephalopathy include pediatric patients; elderly patients, women, in particular premenopausal women; patients with hypoxemia; and patients with underlying CNS disease [see Use in Specific Populations (8.4, 8.5)].
5.6 Refeeding Syndrome
Refeeding severely undernourished patients may result in refeeding syndrome, characterized by the intracellular shift of potassium, phosphorus, and magnesium as the patient becomes anabolic. Thiamine deficiency and fluid retention may also develop. To prevent these complications, monitor severely undernourished patients and slowly increase nutrient intakes.
-
6 ADVERSE REACTIONS
The following adverse reactions associated with the use of dextrose injection were identified in clinical trials or postmarketing reports. Because these reactions were reported voluntarily from a population of uncertain size, it is not always possible to estimate their frequency, reliably, or to establish a causal relationship to drug exposure.
The following clinically significant adverse reactions are described elsewhere in the labeling:
- Hyperglycemia and hyperosmolar hyperglycemic state [see Warnings and Precautions (5.1)]
- Hypersensitivity reactions: anaphylaxis, pruritis, bronchospasm, cyanosis, angioedema, hypotension, pyrexia, chills, and rash [see Warnings and Precautions (5.2)]
- Infusion Site Reactions: infusion site phlebitis, infusion site erythema, vein damage and thrombosis [see Warnings and Precautions (5.3)]
- Hyponatremia and hyponatremic encephalopathy [see Warnings and Precautions (5.4)]
- Refeeding syndrome [see Warnings and Precautions (5.6)]
- Electrolyte imbalance, fluid overload and hypervolemia [see Warnings and Precautions (5.5)]
-
7 DRUG INTERACTIONS
7.1 Other Products that Affect Glycemic Control or Fluid and/or Electrolyte Balance
Dextrose Injection can affect glycemic control, vasopressin and fluid and/or electrolyte balance [see Warnings and Precautions (5.1, 5.4, 5.5)]. Monitor blood glucose concentrations, fluid balance, serum electrolyte concentrations and acid-base balance when using Dextrose Injection in patients treated with other substances that affect glycemic control, vasopressin or fluid and/or electrolyte balance.
-
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Risk Summary
Appropriate administration of Dextrose Injection during pregnancy is not expected to cause adverse developmental outcomes, including congenital malformations. Animal reproduction studies have not been conducted with injectable dextrose solutions.
The estimated background risk of major birth defects and miscarriage for the indicated population is unknown. All pregnancies have a background risk of birth defect, loss, or other adverse outcomes. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2 to 4% and 15 to 20%, respectively.
8.2 Lactation
Risk Summary
There are no data on the presence of dextrose in human milk, the effects on a breastfed infant, or the effects on milk production. The lack of clinical data during lactation precludes a clear determination of the risk of Dextrose Injection to an infant during lactation; therefore, the developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for Dextrose Injection and any potential adverse effects on the breastfed infant from Dextrose Injection or from the underlying maternal condition.
8.4 Pediatric Use
The safety profile of Dextrose Injection in pediatric patients is similar to adults.
Neonates, especially premature infants with low birth weight, are at increased risk of developing hypo- or hyperglycemia and therefore need close monitoring during treatment with intravenous glucose infusions to ensure adequate glycemic control in order to avoid potential long-term adverse effects.
Closely monitor plasma electrolyte concentrations in pediatric patients who may have impaired ability to regulate fluids and electrolytes. In very low birth weight infants, excessive or rapid administration of Dextrose Injection may result in increased serum osmolality and risk of intracerebral hemorrhage.
Children (including neonates and older children) are at increased risk of developing hyponatremia as well as for developing hyponatremic encephalopathy [see Warnings and Precautions (5.4)].
8.5 Geriatric Use
Clinical studies of Dextrose Injection did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Elderly patients are at increased risk of developing hyponatremia as well as for developing hyponatremic encephalopathy [see Warnings and Precautions (5.4)]. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy.
Dextrose is known to be substantially excreted by the kidney, and the risk of toxic reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and it may be useful to monitor renal function.
-
10 OVERDOSAGE
An increased infusion rate of Dextrose Injection or administration of dextrose solutions can cause hyperglycemia, hyperosmolality, and adverse effects on water and electrolyte balance [see Warnings and Precautions (5.1, 5.5)].
Severe hyperglycemia and severe dilutional hyponatremia, and their complications, can be fatal. Discontinue infusion, reduce dose and institute appropriate corrective measures such as administration of exogenous insulin.
Discontinue infusion and institute appropriate corrective measures in the event of overhydration or solute overload during therapy, with particular attention to CNS, respiratory and cardiovascular systems.
If over-exposure occurs, call your Poison Control Center at 1-800-222-1222 for current information on the management of poisoning or overdosage.
-
11 DESCRIPTION
Dextrose Injection, 5% USP is a clear, sterile, non-pyrogenicsolutions of Dextrose, USP in Water for Injection in a polyvinylchloride flexible plastic container for intravenous administration after admixture with a single dose powdered or liquid (up to 10 mL) drug vial [see Dosage and Administration (2.1)].
Partial-fill containers, designed to facilitate admixture, are available in 50 mL, and 100 mL sizes. See Table 1 for the content and characteristics of this solution.
The solution contains no bacteriostatic, antimicrobial agent or added buffer and is intended only for use as a single-dose injection. The pH range is 4.0 (3.2 to 6.5).
Water can permeate from inside the container into the overwrap but not in amounts sufficient to affect the solution significantly.
Table 1. Contents and Characteristics of Dextrose Injection 5%, USP Strength Fill Volume Amount of Dextrose Hydrous per Container kcal* per Container mOsmol per liter - * Caloric value calculated on the basis of 3.4 kcal/g of dextrose, hydrous
Dextrose Injection 5%, USP
(0.05 grams/mL)50 mL
2.5 grams
8.5
252
100 mL
5 grams
17
252
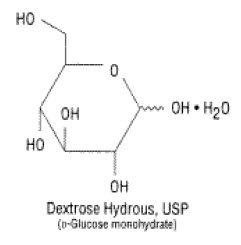
Dextrose, USP is chemically designated D-glucose, monohydrate (C6H12O6 H2O), a hexose sugar freely soluble in water. The molecular weight of dextrose (D-glucose) monohydrate is 198.17. It has the following structural formula:
Water for Injection, USP is chemically designated H2O.
Dextrose is derived from corn.
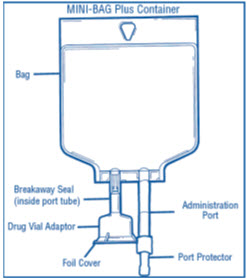
The MINI-BAG Plus Container is a standard diluent container with an integral drug vial adaptor. It allows for drug admixture after connection to a single dose powdered or liquid (up to 10 mL) drug vial having a 20 mm closure. A breakaway seal in the tube between the vial adaptor and the container is broken to allow transfer of the diluent into the vial and reconstitution of the drug. The MiniBag Plus product mechanically prohibits the transfer of contaminants into and out of the system during and after docking, minimizing environmental and personal exposure. The reconstituted drug is then transferred from the vial into the container diluent and mixed to result in an admixture for delivery to the patient.
The VIAFLEX Plus plastic container is fabricated from a specially formulated polyvinyl chloride (PL 146 Plastic). VIAFLEX Plus on the container indicates the presence of a drug additive in a drug vehicle. The VIAFLEX Plus plastic container system utilizes the same container as the VIAFLEX plastic container system. The amount of water that can permeate from inside the container into the overwrap is insufficient to affect the solution significantly. Solutions in contact with the plastic container can leach out certain of its chemical components in very small amounts within the expiration period, e.g., di-2-ethylhexyl phthalate (DEHP), up to 5 parts per million. However, the safety of the plastic has been confirmed in tests in animals according to USP biological tests for plastic containers as well as by tissue culture toxicity studies.
- 12 CLINICAL PHARMACOLOGY
-
16 HOW SUPPLIED/STORAGE AND HANDLING
Dextrose Injection 5%, USP is a clear, sterile solutions of dextrose supplied in single-dose, partial-fill flexible containers.
Product Description
Size
Code
NDC
Dextrose Injection 5%, USP
(0.05 grams/mL)50 mL
2B0040
0338-0551-11
100 mL
2B0041
0338-0551-18
Do not remove container from the overwrap until intended for use.
Use the product immediately after mixing and the introduction of additives.
Store between 20ºC to 25°C (68º F to 77°F). [See USP controlled room temperature.]
Do not freeze.
-
17 PATIENT COUNSELING INFORMATION
Inform patients, caregivers, or home healthcare providers of the following risks of Dextrose Injection:
- Hyperglycemia and hyperosmolar hyperglycemic state [see Warnings and Precautions (5.1)]
- Hypersensitivity reactions [see Warnings and Precautions (5.2)]
- Vein damage and thrombosis [see Warnings and Precautions (5.3)]
- Hyponatremia [see Warnings and Precautions (5.4)]
- Electrolyte imbalance and fluid overload [see Warnings and Precautions (5.5)]
- Refeeding syndrome [see Warnings and Precautions (5.6)]
- SPL UNCLASSIFIED SECTION
-
PACKAGE/LABEL PRINCIPAL DISPLAY PANEL
LOT EXP
-
5% Dextrose
Injection USP
2B0040
NDC: 0338-0551-11MINI-BAG Plus Container
50mL EACH 50 mL CONTAINS 2.5 g DEXTROSE HYDROUS
USP pH 4.0 (3.2 TO 6.5) OSMOLARITY 252
mOsmol/L (CALC) STERILE NONPYROGENIC READ PACKAGE
INSERT FOR FULL INFORMATION ADDITIVES MAY BE INCOMPATIBLE
DOSAGE INTRAVENOUSLY AS DIRECTED BY A PHYSICIAN CAUTIONS
MUST NOT BE USED IN SERIES CONNECTIONS DO NOT ADMINISTER
SIMULTANEOUSLY WITH BLOOD DO NOT USE UNLESS SOLUTION IS
CLEAR RX ONLYBaxter Logo
BAXTER HEALTHCARE CORPORATION
DEERFIELD IL 60015 USA
MADE IN USAVIAFLEX SINGLE DOSE CONTAINER
PL 146 PLASTIC
BAXTER VIAFLEX MINI-BAG
AND PL 146 ARE TRADEMARKS OF
BAXTER INTERNATIONAL INCBREAK SEAL AND MIX BEFORE USE
Lot:PXX Exp:XX XX
QTY:80-50mL
Code: 2B0040
NDC: 0338-0551-11
5% DEXTROSE INJECTION, USP
IN MINI-BAG PLUS CONTAINER
(17) XXXX00 (10) PXX
(01) 50303380551113
-
5% Dextrose
-
INGREDIENTS AND APPEARANCE
DEXTROSE
dextrose monohydrate injectionProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 0338-0551 Route of Administration INTRAVENOUS Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength DEXTROSE MONOHYDRATE (UNII: LX22YL083G) (ANHYDROUS DEXTROSE - UNII:5SL0G7R0OK) DEXTROSE MONOHYDRATE 5 g in 100 mL Inactive Ingredients Ingredient Name Strength WATER (UNII: 059QF0KO0R) Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 0338-0551-11 50 mL in 1 BAG; Type 0: Not a Combination Product 12/07/1992 2 NDC: 0338-0551-18 100 mL in 1 BAG; Type 0: Not a Combination Product 12/07/1992 Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date NDA NDA020179 12/07/1992 Labeler - Baxter Healthcare Corporation (005083209) Establishment Name Address ID/FEI Business Operations Baxter Healthcare Corporation 189326168 ANALYSIS(0338-0551) , LABEL(0338-0551) , MANUFACTURE(0338-0551) , PACK(0338-0551) , STERILIZE(0338-0551) Establishment Name Address ID/FEI Business Operations Baxter Healthcare Corporation 194684502 ANALYSIS(0338-0551) Establishment Name Address ID/FEI Business Operations Baxter Healthcare Corporation 059140764 ANALYSIS(0338-0551) Establishment Name Address ID/FEI Business Operations Baxter Healthcare Corporation 091171389 ANALYSIS(0338-0551) , LABEL(0338-0551) , MANUFACTURE(0338-0551) , PACK(0338-0551) , STERILIZE(0338-0551)
© 2026 FDA.report
This site is not affiliated with or endorsed by the FDA.