BENDAMUSTINE HYDROCHLORIDE injection
BENDAMUSTINE HYDROCHLORIDE by
Drug Labeling and Warnings
BENDAMUSTINE HYDROCHLORIDE by is a Prescription medication manufactured, distributed, or labeled by Eagle Pharmaceuticals, Inc. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
-
HIGHLIGHTS OF PRESCRIBING INFORMATION
These highlights do not include all the information needed to use BENDAMUSTINE HYDROCHLORIDE INJECTION safely and effectively. See full prescribing information for BENDAMUSTINE HYDROCHLORIDE INJECTION.
BENDAMUSTINE HYDROCHLORIDE INJECTION, for intravenous use.
Initial U.S. Approval: 2008
INDICATIONS AND USAGE
Bendamustine Hydrochloride Injection is an alkylating drug indicated for treatment of patients with:
DOSAGE AND ADMINISTRATION
For CLL:
- 100 mg/m2 infused intravenously over 30 minutes on Days 1 and 2 of a 28-day cycle, up to 6 cycles. (2.1)
- Dose modifications for hematologic toxicity: for Grade 3 or greater toxicity, reduce dose to 50 mg/m2 on Days 1 and 2; if Grade 3 or greater toxicity recurs, reduce dose to 25 mg/m2 on Days 1 and 2. (2.1)
- Dose modifications for non-hematologic toxicity: for clinically significant Grade 3 or greater toxicity, reduce the dose to 50 mg/m2 on Days 1 and 2 of each cycle. (2.1)
- Dose re-escalation may be considered. (2.1)
For NHL:
- 120 mg/m2 infused intravenously over 60 minutes on Days 1 and 2 of a 21-day cycle, up to 8 cycles. (2.2)
- Dose modifications for hematologic toxicity: for Grade 4 toxicity, reduce the dose to 90 mg/m2 on Days 1 and 2 of each cycle; if Grade 4 toxicity recurs, reduce the dose to 60 mg/m2 on Days 1 and 2 of each cycle. (2.2)
- Dose modifications for non-hematologic toxicity: for Grade 3 or greater toxicity, reduce the dose to 90 mg/m2 on Days 1 and 2 of each cycle; if Grade 3 or greater toxicity recurs, reduce the dose to 60 mg/m2 on Days 1 and 2 of each cycle. (2.2)
General Dosing Considerations:
DOSAGE FORMS AND STRENGTHS
Injection: 100mg/4mL (25mg/mL) as a ready to dilute solution in a multiple-dose vial. (3)
CONTRAINDICATIONS
WARNINGS AND PRECAUTIONS
- Myelosuppression: Delay or reduce dose. Restart treatment based on ANC and platelet count recovery. (2.1) Complications of myelosuppression may lead to death. (5.1)
- Infections: Monitor for fever and other signs of infection or reactivation of infections and treat promptly. (5.2)
- Anaphylaxis and Infusion Reactions: Severe anaphylactic reactions have occurred. Monitor clinically and discontinue bendamustine hydrochloride . Pre-medicate in subsequent cycles for milder reactions. (5.3)
- Tumor Lysis Syndrome: Acute renal failure and death; anticipate and use supportive measures. (5.4)
- Skin Reactions: Discontinue for severe skin reactions. Cases of SJS, DRESS and TEN, some fatal, have been reported. (5.5)
- Hepatotoxicity: Monitor liver chemistry tests prior to and during treatment. (5.6)
- Other Malignancies: Pre-malignant and malignant diseases have been reported. (5.7)
- Extravasation Injury: Assure good venous access and monitor infusion site during and after administration. (5.8)
- Embryo-fetal toxicity: Fetal harm can occur when administered to a pregnant woman. Women should be advised to avoid becoming pregnant when receiving bendamustine hydrochloride. (5.9, 8.1)
ADVERSE REACTIONS
- Most common non-hematologic adverse reactions for CLL (frequency ≥15%) are pyrexia, nausea, and vomiting. (6.1)
- Most common non-hematologic adverse reactions for NHL (frequency ≥15%) are nausea, fatigue, vomiting, diarrhea, pyrexia, constipation, anorexia, cough, headache, weight decreased, dyspnea, rash, and stomatitis. (6.2)
- Most common hematologic abnormalities (frequency ≥15%) are lymphopenia, anemia, leukopenia, thrombocytopenia, and neutropenia. (6.1, 6.2)
To report SUSPECTED ADVERSE REACTIONS, contact Eagle Pharmaceuticals, Inc. at 1-855-318-2170 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
DRUG INTERACTIONS
Concomitant CYP1A2 inducers or inhibitors have the potential to affect the exposure of bendamustine. (7)
USE IN SPECIFIC POPULATIONS
See 17 for PATIENT COUNSELING INFORMATION.
Revised: 3/2018
-
Table of Contents
FULL PRESCRIBING INFORMATION: CONTENTS*
1 INDICATIONS AND USAGE
1.1 Chronic Lymphocytic Leukemia (CLL)
1.2 Non-Hodgkin Lymphoma (NHL)
2 DOSAGE AND ADMINISTRATION
2.1 Dosing Instructions for CLL
2.2 Dosing Instructions for NHL
2.3 Preparation for Intravenous Administration
2.4 Admixture Stability
2.5 Stability of Partially Used Vials (Needle Punched Vials)
3 DOSAGE FORMS AND STRENGTHS
4 CONTRAINDICATIONS
5 WARNINGS AND PRECAUTIONS
5.1 Myelosuppression
5.2 Infections
5.3 Anaphylaxis and Infusion Reactions
5.4 Tumor Lysis Syndrome
5.5 Skin Reactions
5.6 Hepatotoxicity
5.7 Other Malignancies
5.8 Extravasation Injury
5.9 Embryo-fetal Toxicity
6 ADVERSE REACTIONS
6.1 Clinical Trials Experience
6.2 Postmarketing Experience
7 DRUG INTERACTIONS
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
8.2 Nursing Mothers
8.4 Pediatric Use
8.5 Geriatric Use
8.6 Renal Impairment
8.7 Hepatic Impairment
8.8 Effect of Gender
10 OVERDOSAGE
11 DESCRIPTION
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
12.2 Pharmacodynamics
12.3 Pharmacokinetics
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
14 CLINICAL STUDIES
14.1 Chronic Lymphocytic Leukemia (CLL)
14.2 Non-Hodgkin Lymphoma (NHL)
15 REFERENCES
16 HOW SUPPLIED/STORAGE AND HANDLING
16.1 Safe Handling and Disposal
16.2 How Supplied
16.3 Storage
17 PATIENT COUNSELING INFORMATION
- * Sections or subsections omitted from the full prescribing information are not listed.
- 1 INDICATIONS AND USAGE
-
2 DOSAGE AND ADMINISTRATION
2.1 Dosing Instructions for CLL
Recommended Dosage:
The recommended dose is 100 mg/m2 administered intravenously over 30 minutes on Days 1 and 2 of a 28-day cycle, up to 6 cycles.Dose Delays, Dose Modifications and Reinitiation of Therapy for CLL:
Bendamustine Hydrochloride Injection 100 mg/4 mL (25 mg/mL) administration should be delayed in the event of Grade 4 hematologic toxicity or clinically significant Grade 2 or greater non-hematologic toxicity. Once non-hematologic toxicity has recovered to ≤ Grade 1 and/or the blood counts have improved [Absolute Neutrophil Count (ANC) ≥ 1 x 109/L, platelets ≥ 75 x 109/L], Bendamustine Hydrochloride Injection 100 mg/4 mL (25 mg/mL) can be reinitiated at the discretion of the treating physician. In addition, dose reduction may be warranted. [see Warnings and Precautions (5.1)]Dose modifications for hematologic toxicity: for Grade 3 or greater toxicity, reduce the dose to 50 mg/m2 on Days 1 and 2 of each cycle; if Grade 3 or greater toxicity recurs, reduce the dose to 25 mg/m2 on Days 1 and 2 of each cycle.
Dose modifications for non-hematologic toxicity: for clinically significant Grade 3 or greater toxicity, reduce the dose to 50 mg/m2 on Days 1 and 2 of each cycle.
Dose re-escalation in subsequent cycles may be considered at the discretion of the treating physician.
2.2 Dosing Instructions for NHL
Recommended Dosage:
The recommended dose is 120 mg/m2 administered intravenously over 60 minutes on Days 1 and 2 of a 21-day cycle, up to 8 cycles.
Dose Delays, Dose Modifications and Reinitiation of Therapy for NHL:
Bendamustine Hydrochloride Injection administration should be delayed in the event of a Grade 4 hematologic toxicity or clinically significant ≥ Grade 2 non-hematologic toxicity. Once non-hematologic toxicity has recovered to ≤ Grade 1 and/or the blood counts have improved [Absolute Neutrophil Count (ANC) ≥ 1 x 109/L, platelets ≥ 75 x 109/L], Bendamustine Hydrochloride Injection can be reinitiated at the discretion of the treating physician. In addition, dose reduction may be warranted. [see Warnings and Precautions (5.1)]
Dose modifications for hematologic toxicity: for Grade 4 toxicity, reduce the dose to 90 mg/m2 on Days 1 and 2 of each cycle; if Grade 4 toxicity recurs, reduce the dose to 60 mg/m2 on Days 1 and 2 of each cycle.
Dose modifications for non-hematologic toxicity: for Grade 3 or greater toxicity, reduce the dose to 90 mg/m2 on Days 1 and 2 of each cycle; if Grade 3 or greater toxicity recurs, reduce the dose to 60 mg/m2 on Days 1 and 2 of each cycle.
2.3 Preparation for Intravenous Administration
Bendamustine Hydrochloride Injection is a cytotoxic drug. Follow applicable special handling and disposal procedures.1
Bendamustine Hydrochloride Injection is a clear and colorless to yellow solution. Store Bendamustine Hydrochloride Injection at recommended refrigerated storage conditions (2° to 8°C or 36° to 46°F). When refrigerated the contents may partially freeze. Allow the vial to reach room temperature (15° to 30°C or 59° to 86°F) prior to use. Observe the contents of the vial for any visible solid or particulate matter. Do not use the product if solid or particulate matter is observed after reaching room temperature.
Intravenous Infusion
- Aseptically withdraw the volume needed for the required dose (based on 25 mg/mL concentration) as per Table A below and immediately transfer to a 500 mL infusion bag of 0.9% Sodium Chloride Injection, USP (normal saline). As an alternative to 0.9% Sodium Chloride Injection, USP (normal saline), a 500 mL infusion bag of 2.5% Dextrose/0.45% Sodium Chloride Injection, USP, may be considered. The resulting final concentration of bendamustine HCL in the infusion bag should be within 0.2 – 0.7 mg/mL. After transferring, thoroughly mix the contents of the infusion bag. The admixture should be a clear and colorless to slightly yellow solution.
Use either 0.9% Sodium Chloride Injection, USP, or 2.5% Dextrose/0.45% Sodium Chloride Injection, USP, for dilution, as outlined above. No other diluents have been shown to be compatible.
Table A: Volume (mL) of Bendamustine Hydrochloride Injection required for dilution into 500 mL of 0.9% Saline, or 0.45% Saline/2.5% Dextrose for a given dose (mg/m2) and Body Surface Area (m2)
Body Surface Area (m2) Volume of Bendamustine Hydrochloride Injection to withdraw (mL) 120 mg/m2 100 mg/m2 90 mg/m2 60 mg/m2 50 mg/m2 25 mg/m2 1 4.8 4 3.6 2.4 2 1 1.1 5.3 4.4 4 2.6 2.2 1.1 1.2 5.8 4.8 4.3 2.9 2.4 1.2 1.3 6.2 5.2 4.7 3.1 2.6 1.3 1.4 6.7 5.6 5 3.4 2.8 1.4 1.5 7.2 6 5.4 3.6 3 1.5 1.6 7.7 6.4 5.8 3.8 3.2 1.6 1.7 8.2 6.8 6.1 4.1 3.4 1.7 1.8 8.6 7.2 6.5 4.3 3.6 1.8 1.9 9.1 7.6 6.8 4.6 3.8 1.9 2 9.6 8 7.2 4.8 4 2 2.1 10.1 8.4 7.6 5 4.2 2.1 2.2 10.6 8.8 7.9 5.3 4.4 2.2 2.3 11 9.2 8.3 5.5 4.6 2.3 2.4 11.5 9.6 8.6 5.8 4.8 2.4 2.5 12 10 9 6 5 2.5 2.6 12.5 10.4 9.4 6.2 5.2 2.6 2.7 13 10.8 9.7 6.5 5.4 2.7 2.8 13.4 11.2 10.1 6.7 5.6 2.8 2.9 13.9 11.6 10.4 7 5.8 2.9 3 14.4 12 10.8 7.2 6 3 General Information
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration whenever solution and container permit. Any unused solution should be discarded according to institutional procedures for antineoplastics.
2.4 Admixture Stability
Bendamustine Hydrochloride Injection contains no antimicrobial preservative. The admixture should be prepared as close as possible to the time of patient administration.
Once diluted with 0.9% Sodium Chloride Injection, USP, or 2.5% Dextrose/0.45% Sodium Chloride Injection, USP, the final admixture is stable for 24 hours when stored under refrigerated (2° to 8°C or 36° to 46°F) or for 3 hours when stored at room temperature (15° to 30°C or 59° to 86°F) and room light. Administration of diluted Bendamustine Hydrochloride Injection must be completed within this period of time. Bendamustine Hydrochloride Injection is a multiple-dose vial. Retain the partially used vial in original package to protect from light and store refrigerated (2° to 8°C or 36° to 46°F) if additional dose withdrawal from the same vial is intended.
2.5 Stability of Partially Used Vials (Needle Punched Vials)
Bendamustine Hydrochloride Injection is a multiple-dose vial. Although it does not contain any antimicrobial preservative, Bendamustine Hydrochloride Injection is bacteriostatic and does not support bacterial growth. The partially used vials are stable for up to 28 days when stored in its original carton under refrigeration (2° to 8°C or 36° to 46°F). Each vial is not recommended for more than a total of six (6) dose withdrawals.
After first use, the partially used vial should be stored in original carton at 2° to 8°C (36° to 46°F), and then discarded after 28 days.
- 3 DOSAGE FORMS AND STRENGTHS
-
4 CONTRAINDICATIONS
Bendamustine Hydrochloride Injection is contraindicated in patients with a known hypersensitivity (e.g., anaphylactic and anaphylactoid reactions) to bendamustine, polyethylene glycol 400, propylene glycol, or monothioglycerol. [see Warnings and Precautions (5.3)]
-
5 WARNINGS AND PRECAUTIONS
5.1 Myelosuppression
Bendamustine hydrochloride caused severe myelosuppression (Grade 3-4) in 98% of patients in the two NHL studies (see Table 4). Three patients (2%) died from myelosuppression-related adverse reactions; one each from neutropenic sepsis, diffuse alveolar hemorrhage with Grade 3 thrombocytopenia, and pneumonia from an opportunistic infection (CMV).
In the event of treatment-related myelosuppression, monitor leukocytes, platelets, hemoglobin (Hgb), and neutrophils frequently. In the clinical trials, blood counts were monitored every week initially. Hematologic nadirs were observed predominantly in the third week of therapy. Myelosuppression may require dose delays and/or subsequent dose reductions if recovery to the recommended values has not occurred by the first day of the next scheduled cycle. Prior to the initiation of the next cycle of therapy, the ANC should be ≥ 1 x 109/L and the platelet count should be ≥ 75 x 109/L. [see Dosage and Administration (2.1) and (2.2)]
5.2 Infections
Infection, including pneumonia, sepsis, septic shock, hepatitis and death has occurred in adult and pediatric patients in clinical trials and in postmarketing reports for bendamustine hydrochloride. Patients with myelosuppression following treatment with bendamustine hydrochloride are more susceptible to infections. Advise patients with myelosuppression following bendamustine hydrochloride treatment to contact a physician immediately if they have symptoms or signs of infection.
Patients treated with bendamustine hydrochloride are at risk for reactivation of infections including (but not limited to) hepatitis B, cytomegalovirus, Mycobacterium tuberculosis, and herpes zoster. Patients should undergo appropriate measures (including clinical and laboratory monitoring, prophylaxis, and treatment) for infection and infection reactivation prior to administration.
5.3 Anaphylaxis and Infusion Reactions
Infusion reactions to bendamustine hydrochloride have occurred commonly in clinical trials. Symptoms include fever, chills, pruritus and rash. In rare instances severe anaphylactic and anaphylactoid reactions have occurred, particularly in the second and subsequent cycles of therapy. Monitor clinically and discontinue drug for severe reactions. Ask patients about symptoms suggestive of infusion reactions after their first cycle of therapy. Patients who experience Grade 3 or worse allergic-type reactions should not be rechallenged. Consider measures to prevent severe reactions, including antihistamines, antipyretics and corticosteroids in subsequent cycles in patients who have experienced Grade 1 or 2 infusion reactions. Discontinue bendamustine hydrochloride for patients with Grade 4 infusion reactions. Consider discontinuation for Grade 3 infusion reactions as clinically appropriate considering individual benefits, risks, and supportive care.
5.4 Tumor Lysis Syndrome
Tumor lysis syndrome associated with bendamustine hydrochloride has occurred in patients in clinical trials and in post-marketing reports. The onset tends to be within the first treatment cycle of bendamustine hydrochloride and, without intervention, may lead to acute renal failure and death. Preventive measures include vigorous hydration and close monitoring of blood chemistry, particularly potassium and uric acid levels. Allopurinol has also been used during the beginning of bendamustine hydrochloride therapy. However, there may be an increased risk of severe skin toxicity when bendamustine hydrochloride and allopurinol are administered concomitantly. [see Warnings and Precautions (5.5)]
5.5 Skin Reactions
Fatal and serious skin reactions have been reported with bendamustine hydrochloride treatment in clinical trials and postmarketing safety reports, including toxic skin reactions [Stevens-Johnson Syndrome (SJS), toxic epidermal necrolysis (TEN), and drug reaction with eosinophilia and systemic symptoms (DRESS), bullous exanthema, and rash. Events occurred when bendamustine hydrochloride was given as a single agent and in combination with other anticancer agents or allopurinol.
Where skin reactions occur, they may be progressive and increase in severity with further treatment. Monitor patients with skin reactions closely. If skin reactions are severe or progressive, withhold or discontinue bendamustine hydrochloride.
5.6 Hepatotoxicity
Fatal and serious cases of liver injury have been reported with bendamustine hydrochloride injection. Combination therapy, progressive disease or reactivation of hepatitis B were confounding factors in some patients. [see Warnings and Precautions (5.2)] Most cases were reported within the first three months of starting therapy. Monitor liver chemistry tests prior to and during bendamustine therapy.
5.7 Other Malignancies
There are reports of pre-malignant and malignant diseases that have developed in patients who have been treated with bendamustine hydrochloride, including myelodysplastic syndrome, myeloproliferative disorders, acute myeloid leukemia and bronchial carcinoma.
5.8 Extravasation Injury
Bendamustine hydrochloride extravasations have been reported in post marketing resulting in hospitalizations from erythema, marked swelling, and pain. Assure good venous access prior to starting bendamustine hydrochloride infusion and monitor the intravenous infusion site for redness, swelling, pain, infection, and necrosis during and after administration of bendamustine hydrochloride.
5.9 Embryo-fetal Toxicity
Bendamustine hydrochloride can cause fetal harm when administered to a pregnant woman. Single intraperitoneal doses of bendamustine in mice and rats administered during organogenesis caused an increase in resorptions, skeletal and visceral malformations, and decreased fetal body weights. [see Use in Specific Populations (8.1)]
-
6 ADVERSE REACTIONS
The following serious adverse reactions have been associated with bendamustine hydrochloride in clinical trials and are discussed in greater detail in other sections of the prescribing information.
- Myelosuppression [see Warnings and Precautions (5.1)]
- Infections [see Warnings and Precautions (5.2)]
- Anaphylaxis and Infusion Reactions [see Warnings and Precautions (5.3)]
- Tumor Lysis Syndrome [see Warnings and Precautions (5.4)]
- Skin Reactions [see Warnings and Precautions (5.5)]
- Hepatotoxicity [see Warnings and Precautions (5.6)]
- Other Malignancies [see Warnings and Precautions (5.7)]
- Extravasation Injury [see Warnings and Precautions (5.8)]
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Chronic Lymphocytic Leukemia
The data described below reflect exposure to bendamustine hydrochloride in 153 patients with CLL studied in an active-controlled, randomized trial. The population was 45-77 years of age, 63% male, 100% white, and were treatment naïve. All patients started the study at a dose of 100 mg/m2 intravenously over 30 minutes on Days 1 and 2 every 28 days.
Adverse reactions were reported according to NCI CTC v.2.0. Non-hematologic adverse reactions (any grade) in the bendamustine hydrochloride group that occurred with a frequency greater than 15% were pyrexia (24%), nausea (20%), and vomiting (16%).
Other adverse reactions seen frequently in one or more studies included asthenia, fatigue, malaise, and weakness; dry mouth; somnolence; cough; constipation; headache; mucosal inflammation and stomatitis.
Worsening hypertension was reported in 4 patients treated with bendamustine hydrochloride in the CLL trial and in none treated with chlorambucil. Three of these 4 adverse reactions were described as a hypertensive crisis and were managed with oral medications and resolved.
The most frequent adverse reactions leading to study withdrawal for patients receiving bendamustine hydrochloride were hypersensitivity (2%) and pyrexia (1%).
Table 1 contains the treatment emergent adverse reactions, regardless of attribution, that were reported in ≥ 5% of patients in either treatment group in the randomized CLL clinical study.
Table 1: Non-Hematologic Adverse Reactions Occurring in Randomized CLL Clinical Study in at Least 5% of Patients Number (%) of patients Bendamustine Hydrochloride
(N=153)Chlorambucil
(N=143)Body System
Adverse ReactionAll Grades Grade 3/4 All Grades Grade 3/4 Total number of patients with at least 1 adverse reaction 121 (79) 52 (34) 96 (67) 25 (17) Gastrointestinal disorders Nausea 31 (20) 1 (<1) 21 (15) 1 (<1) Vomiting 24 (16) 1 (<1) 9 (6) 0 Diarrhea 14 (9) 2 (1) 5 (3) 0 General disorders and administration site conditions Pyrexia 36 (24) 6 (4) 8 (6) 2 (1) Fatigue 14 (9) 2 (1) 8 (6) 0 Asthenia 13 (8) 0 6 (4) 0 Chills 9 (6) 0 1 (<1) 0 Immune system disorders Hypersensitivity 7 (5) 2 (1) 3 (2) 0 Infections and infestations Nasopharyngitis 10 (7) 0 12 (8) 0 Infection 9 (6) 3 (2) 1 (<1) 1 (<1) Herpes simplex 5 (3) 0 7 (5) 0 Investigations Weight decreased 11 (7) 0 5 (3) 0 Metabolism and nutrition disorders Hyperuricemia 11 (7) 3 (2) 2 (1) 0 Respiratory, thoracic and mediastinal disorders Cough 6 (4) 1 (<1) 7 (5) 1 (<1) Skin and subcutaneous tissue disorders Rash 12 (8) 4 (3) 7 (5) 3 (2) Pruritus 8 (5) 0 2 (1) 0 The Grade 3 and 4 hematology laboratory test values by treatment group in the randomized CLL clinical study are described in Table 2. These findings confirm the myelosuppressive effects seen in patients treated with bendamustine hydrochloride. Red blood cell transfusions were administered to 20% of patients receiving bendamustine hydrochloride compared with 6% of patients receiving chlorambucil.
Table 2: Incidence of Hematology Laboratory Abnormalities in Patients Who Received Bendamustine Hydrochloride or Chlorambucil in the Randomized CLL Clinical Study Laboratory Abnormality Bendamustine Hydrochloride N=150 Chlorambucil
N=141All Grades
n (%)Grade 3/4
n (%)All Grades
n (%)Grade 3/4
n (%)Hemoglobin
Decreased134 (89) 20 (13) 115 (82) 12 (9) Platelets
Decreased116 (77) 16 (11) 110 (78) 110 (78) Platelets
Decreased92 (61) 42 (28) 26 (18) 4 (3) Lymphocytes
Decreased102 (68) 70 (47) 27 (19) 6 (4) Neutrophil
Decreased113 (75) 65 (43) 86 (61) 30 (21) In the CLL trial, 34% of patients had bilirubin elevations, some without associated significant elevations in AST and ALT. Grade 3 or 4 increased bilirubin occurred in 3% of patients. Increases in AST and ALT of Grade 3 or 4 were limited to 1% and 3% of patients, respectively. Patients treated with bendamustine hydrochloride may also have changes in their creatinine levels. If abnormalities are detected, monitoring of these parameters should be continued to ensure that further deterioration does not occur.
Non-Hodgkin Lymphoma
The data described below reflect exposure to bendamustine hydrochloride in 176 patients with indolent B-cell NHL treated in two single-arm studies. The population was 31-84 years of age, 60% male, and 40% female. The race distribution was 89% White, 7% Black, 3% Hispanic, 1% other, and <1% Asian. These patients received bendamustine hydrochloride at a dose of 120 mg/m2 intravenously on Days 1 and 2 for up to eight 21-day cycles.The adverse reactions occurring in at least 5% of the NHL patients, regardless of severity, are shown in Table 3. The most common non-hematologic adverse reactions (≥30%) were nausea (75%), fatigue (57%), vomiting (40%), diarrhea (37%) and pyrexia (34%). The most common non-hematologic Grade 3 or 4 adverse reactions (≥5%) were fatigue (11%), febrile neutropenia (6%), and pneumonia, hypokalemia and dehydration, each reported in 5% of patients.
Table 3: Non-Hematologic Adverse Reactions Occurring in at Least 5% of NHL Patients Treated with Bendamustine Hydrochloride by System Organ Class and Preferred Term (N=176) *Patients may have reported more than 1 adverse reaction. Body System Number (%) of patients* Adverse Reaction All Grades Grade 3/4 Total number of patients with at
least 1 adverse reaction176 (100) 94 (53) Cardiac Disorders Tachycardia 13 (7) 0 Gastrointestinal disorders Nausea 132 (75) 7 (4) Vomiting 71 (40) 5 (3) Diarrhea 65 (37) 6 (3) Constipation 51 (29) 1 (<1) Stomatitis 27 (15) 1 (<1) Abdominal pain 22 (13) 2 (1) Dyspepsia 20 (11) 0 Gastroesophageal reflux disease 18 (10) 0 Dry mouth 15 (9) 1 (<1) Abdominal pain upper 8 (5) 0 Abdominal distension 8 (5) 0 General disorders and administration site conditions Fatigue 101 (57) 19 (11) Pyrexia 59 (34) 3 (2) Chills 24 (14) 0 Edema peripheral 23 (13) 1 (<1) Asthenia 19 (11) 4 (2) Chest pain 11 (6) 1 (<1) Infusion site pain 11 (6) 0 Pain 10 (6) 0 Catheter site pain 8 (5) 0 Infections and infestations Herpes zoster 18 (10) 5 (3) Upper respiratory tract infection 18 (10) 0 Urinary tract infection 17 (10) 4 (2) Sinusitis 15 (9) 0 Pneumonia 14 (8) 9 (5) Febrile neutropenia 11 (6) 11 (6) Oral candidiasis 11 (6) 2 (1) Nasopharyngitis 11 (6) 0 Investigations Weight decreased Weight decreased 3 (2) Metabolism and nutrition disorders Anorexia 40 (23) 3 (2) Dehydration 24 (14) 8 (5) Decreased appetite 22 (13) 1 (<1) Hypokalemia 15 (9) 9 (5) Musculoskeletal and connective tissue disorders Back pain 25 (14) 5 (3) Arthralgia 11 (6) 0 Pain in extremity 8 (5) 2 (1) Bone pain 8 (5) 0 Nervous system disorders Headache 36 (21) 0 Dizziness 25 (14) 0 Dysgeusia 13 (7) 0 Psychiatric disorder Insomnia 23 (13) 0 Anxiety 14 (8) 1 (<1) Depression 10 (6) 0 Respiratory, thoracic and mediastinal disorders Cough 38 (22) 1 (<1) Dyspnea 28 (16) 3 (2) Pharyngolaryngeal pain 14 (8) 1 (<1) Wheezing 8 (5) 0 Nasal congestion 8 (5) 0 Skin and subcutaneous tissue disorders Rash 28 (16) 1 (<1) Pruritus 11 (6) 0 Dry skin 9 (5) 0 Night sweats 9 (5) 0 Hyperhidrosis 8 (5) 0 Vascular disorders Hypotension 10 (6) 2 (1) NOTE: Patients counted only once in each preferred term category and once in each system organ class category
Hematologic toxicities, based on laboratory values and CTC grade, in NHL patients treated in both single arm studies combined are described in Table 4. Clinically important chemistry laboratory values that were new or worsened from baseline and occurred in >1% of patients at Grade 3 or 4, in NHL patients treated in both single arm studies combined were hyperglycemia (3%), elevated creatinine (2%), hyponatremia (2%), and hypocalcemia (2%).
Table 4: Incidence of Hematology Laboratory Abnormalities in Patients Who Received Bendamustine Hydrochloride in the NHL Studies Hematology Variable Percent of Patients All Grades Grade 3/4 Lymphocytes Decreased 99 94 Leukocytes Decreased 94 56 Hemoglobin Decreased 88 11 Neutrophils Decreased 86 60 Platelets Decreased 86 25 In both studies, serious adverse reactions, regardless of causality, were reported in 37% of patients receiving bendamustine hydrochloride. The most common serious adverse reactions occurring in ≥5% of patients were febrile neutropenia and pneumonia. Other important serious adverse reactions reported in clinical trials and/or post-marketing experience were acute renal failure, cardiac failure, hypersensitivity, skin reactions, pulmonary fibrosis, and myelodysplastic syndrome.
Serious drug-related adverse reactions reported in clinical trials included myelosuppression, infection, pneumonia, tumor lysis syndrome and infusion reactions. [see Warnings and Precautions (5)] Adverse reactions occurring less frequently but possibly related to bendamustine hydrochloride treatment were hemolysis, dysgeusia/taste disorder, atypical pneumonia, sepsis, herpes zoster, erythema, dermatitis, and skin necrosis.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of bendamustine hydrochloride. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Blood and lymphatic systems disorders: Pancytopenia
Cardiovascular disorders: Atrial fibrillation, congestive heart failure (some fatal), myocardial infarction (some fatal), palpitation
General disorders and administration site conditions: Injection site reactions (including phlebitis, pruritus, irritation, pain, swelling), infusion site reactions (including phlebitis, pruritus, irritation, pain, swelling)
Immune system disorders: Anaphylaxis
Infections and infestations: Pneumocystis jiroveci pneumonia
Respiratory, thoracic and mediastinal disorders: Pneumonitis
Skin and subcutaneous tissue disorders: Stevens-Johnson syndrome, Toxic epidermal necrolysis, DRESS (Drug reaction with eosinophilia and systemic symptoms). [see Warnings and Precautions (5.5)]
-
7 DRUG INTERACTIONS
No formal clinical assessments of pharmacokinetic drug-drug interactions between bendamustine hydrochloride and other drugs have been conducted.
Bendamustine's active metabolites, gamma-hydroxy bendamustine (M3) and N-desmethyl-bendamustine (M4), are formed via cytochrome P450 CYP1A2. Inhibitors of CYP1A2 (e.g., fluvoxamine, ciprofloxacin) have potential to increase plasma concentrations of bendamustine and decrease plasma concentrations of active metabolites. Inducers of CYP1A2 (e.g., omeprazole, smoking) have potential to decrease plasma concentrations of bendamustine and increase plasma concentrations of its active metabolites. Caution should be used, or alternative treatments considered if concomitant treatment with CYP1A2 inhibitors or inducers is needed.
The role of active transport systems in bendamustine distribution has not been fully evaluated. In vitro data suggest that P-glycoprotein, breast cancer resistance protein (BCRP), and/or other efflux transporters may have a role in bendamustine transport.
Based on in vitro data, bendamustine is not likely to inhibit metabolism via human CYP isoenzymes CYP1A2, 2C9/10, 2D6, 2E1, or 3A4/5, or to induce metabolism of substrates of cytochrome P450 enzymes.
-
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Pregnancy Category D [see Warnings and Precautions (5.9)]
Risk Summary
Bendamustine hydrochloride can cause fetal harm when administered to a pregnant woman. Bendamustine caused malformations in animals, when a single dose was administered to pregnant animals. Advise women to avoid becoming pregnant while receiving bendamustine hydrochloride and for 3 months after therapy has stopped. If this drug is used during pregnancy, or if the patient becomes pregnant while receiving this drug, the patient should be apprised of the potential hazard to a fetus. Advise men receiving bendamustine hydrochloride to use reliable contraception for the same time period.
Animal data
Single intraperitoneal doses of bendamustine from 210 mg/m2 (70 mg/kg) in mice administered during organogenesis caused an increase in resorptions, skeletal and visceral malformations (exencephaly, cleft palates, accessory rib, and spinal deformities) and decreased fetal body weights. This dose did not appear to be maternally toxic and lower doses were not evaluated. Repeat intraperitoneal dosing in mice on gestation days 7-11 resulted in an increase in resorptions from 75 mg/m2 (25 mg/kg) and an increase in abnormalities from 112.5 mg/m2 (37.5 mg/kg) similar to those seen after a single intraperitoneal administration. Single intraperitoneal doses of bendamustine from 120 mg/m2 (20 mg/kg) in rats administered on gestation days 4, 7, 9, 11, or 13 caused embryo and fetal lethality as indicated by increased resorptions and a decrease in live fetuses. A significant increase in external [effect on tail, head, and herniation of external organs (exomphalos)] and internal (hydronephrosis and hydrocephalus) malformations were seen in dosed rats. There are no adequate and well-controlled studies in pregnant women. If this drug is used during pregnancy, or if the patient becomes pregnant while taking this drug, the patient should be apprised of the potential hazard to the fetus.
8.2 Nursing Mothers
It is not known whether this drug is excreted in human milk. Because many drugs are excreted in human milk and because of the potential for serious adverse reactions in nursing infants and tumorigenicity shown for bendamustine in animal studies, a decision should be made whether to discontinue nursing or to discontinue the drug, taking into account the importance of the drug to the mother.
8.4 Pediatric Use
The effectiveness of bendamustine hydrochloride in pediatric patients has not been established. Bendamustine hydrochloride was evaluated in a single Phase 1/2 trial in pediatric patients with leukemia. The safety profile for bendamustine hydrochloride in pediatric patients was consistent with that seen in adults, and no new safety signals were identified.
The trial included pediatric patients from 1-19 years of age with relapsed or refractory acute leukemia, including 27 patients with acute lymphocytic leukemia (ALL) and 16 patients with acute myeloid leukemia (AML). Bendamustine hydrochloride was administered as an intravenous infusion over 60 minutes on Days 1 and 2 of each 21-day cycle. Doses of 90 and 120 mg/m2 were evaluated. The Phase 1 portion of the study determined that the recommended Phase 2 dose of bendamustine hydrochloride in pediatric patients was 120 mg/m2.
A total of 32 patients entered the Phase 2 portion of the study at the recommended dose and were evaluated for response. There was no treatment response (CR+ CRp) in any patient at this dose. However, there were 2 patients with ALL who achieved a CR at a dose of 90 mg/m2 in the Phase 1 portion of the study.
In the above-mentioned pediatric trial, the pharmacokinetics of bendamustine hydrochloride at 90 and 120 mg/m2 doses were evaluated in 5 and 38 patients, respectively, aged 1 to 19 years (median age of 10 years).
The geometric mean body surface adjusted clearance of bendamustine was 14.2 L/h/m2. The exposures (AUC0-24 and Cmax) to bendamustine in pediatric patients following a 120 mg/m2 intravenous infusion over 60 minutes were similar to those in adult patients following the same 120 mg/m2 dose.
8.5 Geriatric Use
In CLL and NHL studies, there were no clinically significant differences in the adverse reaction profile between geriatric (≥ 65 years of age) and younger patients.
Chronic Lymphocytic Leukemia
In the randomized CLL clinical study, 153 patients received bendamustine hydrochloride. The overall response rate for patients younger than 65 years of age was 70% (n=82) for bendamustine hydrochloride and 30% (n=69) for chlorambucil. The overall response rate for patients 65 years or older was 47% (n=71) for bendamustine hydrochloride and 22% (n=79) for chlorambucil. In patients younger than 65 years of age, the median progression-free survival was 19 months in the bendamustine hydrochloride group and 8 months in the chlorambucil group. In patients 65 years or older, the median progression-free survival was 12 months in the bendamustine hydrochloride group and 8 months in the chlorambucil group.Non-Hodgkin Lymphoma
Efficacy (Overall Response Rate and Duration of Response) was similar in patients < 65 years of age and patients ≥ 65 years. Irrespective of age, all of the 176 patients experienced at least one adverse reaction.8.6 Renal Impairment
No formal studies assessing the impact of renal impairment on the pharmacokinetics of bendamustine have been conducted. Bendamustine hydrochloride should not be used in patients with CrCL less than 30 mL/min. [see Clinical Pharmacology (12.3)]
8.7 Hepatic Impairment
No formal studies assessing the impact of hepatic impairment on the pharmacokinetics of bendamustine have been conducted. Bendamustine hydrochloride should not be used in patients with moderate (AST or ALT 2.5-10 X ULN and total bilirubin 1.5-3 X ULN) or severe (total bilirubin greater than 3 X ULN) hepatic impairment. [see Clinical Pharmacology (12.3)]
8.8 Effect of Gender
No clinically significant differences between genders were seen in the overall incidences of adverse reactions in CLL or NHL studies.
Chronic Lymphocytic Leukemia
In the randomized CLL clinical study, the overall response rate (ORR) for men (n=97) and women (n=56) in the bendamustine hydrochloride group was 60% and 57%, respectively. The ORR for men (n=90) and women (n=58) in the chlorambucil group was 24% and 28%, respectively. In this study, the median progression-free survival for men was 19 months in the bendamustine hydrochloride treatment group and 6 months in the chlorambucil treatment group. For women, the median progression-free survival was 13 months in the bendamustine hydrochloride treatment group and 8 months in the chlorambucil treatment group.Non-Hodgkin Lymphoma
The pharmacokinetics of bendamustine were similar in male and female patients with indolent NHL. No clinically-relevant differences between genders were seen in efficacy (Overall Response Rate and Duration of Response). -
10 OVERDOSAGE
The intravenous LD50 of bendamustine hydrochloride is 240 mg/m2 in the mouse and rat. Toxicities included sedation, tremor, ataxia, convulsions and respiratory distress.
Across all clinical experience, the reported maximum single dose received was 280 mg/m2. Three of four patients treated at this dose showed ECG changes considered dose-limiting at 7 and 21 days post-dosing. These changes included QT prolongation (one patient), sinus tachycardia (one patient), ST and T wave deviations (two patients) and left anterior fascicular block (one patient). Cardiac enzymes and ejection fractions remained normal in all patients.
No specific antidote for bendamustine hydrochloride overdose is known. Management of overdosage should include general supportive measures, including monitoring of hematologic parameters and ECGs. -
11 DESCRIPTION
The active ingredient, bendamustine hydrochloride is an alkylating agent. The chemical name of bendamustine hydrochloride is 1H-benzimidazole-2-butanoic acid, 5-[bis(2-chloroethyl)amino]-1 methyl-, monohydrochloride. Its empirical molecular formula is C16H21Cl2N3O2·HCl, and the molecular weight is 394.7. Bendamustine hydrochloride contains a mechlorethamine group and a benzimidazole heterocyclic ring with a butyric acid substituent, and has the following structural formula:
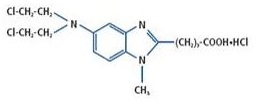
Bendamustine Hydrochloride Injection is intended for intravenous infusion only after dilution with either 0.9% Sodium Chloride Injection, USP, or 2.5% Dextrose/0.45% Sodium Chloride Injection, USP. It is supplied as a sterile multiple-dose, clear, colorless to yellow ready-to-dilute solution in a multiple-dose clear glass vial. Each milliliter of the injection contains 25 mg of bendamustine hydrochloride, 0.1 mL of propylene glycol, USP, 5 mg of monothioglycerol, NF and q.s. to 1 mL polyethylene glycol 400, NF.
-
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Bendamustine is a bifunctional mechlorethamine derivative containing a purine-like benzimidazole ring. Mechlorethamine and its derivatives form electrophilic alkyl groups. These groups form covalent bonds with electron-rich nucleophilic moieties, resulting in interstrand DNA crosslinks. The bifunctional covalent linkage can lead to cell death via several pathways. Bendamustine is active against both quiescent and dividing cells. The exact mechanism of action of bendamustine remains unknown.
12.2 Pharmacodynamics
Based on the pharmacokinetics/pharmacodynamics analyses of data from adult NHL patients, nausea increased with increasing bendamustine Cmax.
Cardiac Electrophysiology
The effect of bendamustine on the QTc interval was evaluated in 53 patients with indolent NHL and mantle cell lymphoma on Day 1 of Cycle 1 after administration of rituximab at 375 mg/m2 intravenous infusion followed by a 30-minute intravenous infusion of bendamustine at 90 mg/m2/day. No mean changes greater than 20 milliseconds were detected up to one hour post infusion. The potential for delayed effects on the QT interval after one hour was not evaluated.12.3 Pharmacokinetics
Absorption
Following a single IV dose of bendamustine hydrochloride Cmax typically occurred at the end of infusion. The dose proportionality of bendamustine has not been studied.Distribution
In vitro, the binding of bendamustine to human serum plasma proteins ranged from 94-96% and was concentration independent from 1-50 μg/mL. Data suggest that bendamustine is not likely to displace or to be displaced by highly protein-bound drugs. The blood to plasma concentration ratios in human blood ranged from 0.84 to 0.86 over a concentration range of 10 to 100 μg/mL indicating that bendamustine distributes freely in human red blood cells.In a mass balance study, plasma radioactivity levels were sustained for a greater period of time than plasma concentrations of bendamustine, γ hydroxybendamustine (M3), and N desmethylbendamustine (M4). This suggests that there are bendamustine derived materials (detected via the radiolabel), that are rapidly cleared and have a longer half-life than bendamustine and its active metabolites.
The mean steady-state volume of distribution (Vss) of bendamustine was approximately 20-25 L. Steady-state volume of distribution for total radioactivity was approximately 50 L, indicating that neither bendamustine nor total radioactivity are extensively distributed into the tissues.
Metabolism
In vitro data indicate that bendamustine is primarily metabolized via hydrolysis to monohydroxy (HP1) and dihydroxy-bendamustine (HP2) metabolites with low cytotoxic activity. In vitro, studies indicate that two active minor metabolites, M3 and M4, are primarily formed via CYP1A2. However, concentrations of these metabolites in plasma are 1/10th and 1/100th that of the parent compound, respectively, suggesting that the cytotoxic activity is primarily due to bendamustine.Results of a human mass balance study confirm that bendamustine is extensively metabolized via hydrolytic, oxidative, and conjugative pathways.
In vitro studies using human liver microsomes indicate that bendamustine does not inhibit CYP1A2, 2C9/10, 2D6, 2E1, or 3A4/5. Bendamustine did not induce metabolism of CYP1A2, CYP2A6, CYP2B6, CYP2C8, CYP2C9, CYP2C19, CYP2E1, or CYP3A4/5 enzymes in primary cultures of human hepatocytes.
Elimination
Mean recovery of total radioactivity in cancer patients following IV infusion of [14C] bendamustine hydrochloride was approximately 76% of the dose. Approximately 50% of the dose was recovered in the urine and approximately 25% of the dose was recovered in the feces. Urinary excretion was confirmed as a relatively minor pathway of elimination of bendamustine, with approximately 3.3% of the dose recovered in the urine as parent. Less than 1% of the dose was recovered in the urine as M3 and M4, and less than 5% of the dose was recovered in the urine as HP2.Bendamustine clearance in humans is approximately 700 mL/minute. After a single dose of 120 mg/m2 bendamustine IV over 1-hour the intermediate t½ of the parent compound is approximately 40 minutes. The mean apparent terminal elimination t½ of M3 and M4 are approximately 3 hours and 30 minutes respectively. Little or no accumulation in plasma is expected for bendamustine administered on Days 1 and 2 of a 28-day cycle.
Renal Impairment
In a population pharmacokinetic analysis of bendamustine in patients receiving 120 mg/m2 there was no meaningful effect of renal impairment (CrCL 30 - 80 mL/min, N=31) on the pharmacokinetics of bendamustine. Bendamustine has not been studied in patients with CrCL less than 30 mL/min and should not be used in these patients.Hepatic Impairment
In a population pharmacokinetic analysis of bendamustine in patients receiving 120 mg/m2 there was no meaningful effect of mild (total bilirubin ≤ ULN, AST ≥ ULN to 2.5 x ULN, and/or ALP ≥ ULN to 5 x ULN, N=26) hepatic impairment on the pharmacokinetics of bendamustine. Bendamustine has not been studied in patients with moderate or severe hepatic impairment.Bendamustine should not be used in patients with moderate (AST or ALT 2.5 – 10 x ULN and total bilirubin 1.5 – 3 x ULN) or severe (total bilirubin greater than 3 x ULN) hepatic impairment. [see Use in Specific Populations (8.7)]
Effect of Age
Bendamustine exposure (as measured by AUC and Cmax) has been studied in patients ages 31 through 84 years. The pharmacokinetics of bendamustine (AUC and Cmax) were not significantly different between patients less than or greater than/equal to 65 years of age. [see Use in Specific Populations (8.4, 8.5)]Effect of Gender
The pharmacokinetics of bendamustine were similar in male and female patients. [see Use in Specific Populations (8.8)]Effect of Race
The effect of race on the safety, and/or efficacy of bendamustine hydrochloride has not been established. Based on a cross-study comparison, Japanese subjects (n=6) had on average exposures that were 40% higher than non-Japanese subjects receiving the same dose. The significance of this difference on the safety and efficacy of bendamustine hydrochloride in Japanese subjects has not been established. -
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Bendamustine was carcinogenic in mice. After intraperitoneal injections at 37.5 mg/m2/day (12.5 mg/kg/day, the lowest dose tested) and 75 mg/m2/day (25 mg/kg/day) for four days, peritoneal sarcomas in female AB/jena mice were produced. Oral administration at 187.5 mg/m2/day (62.5 mg/kg/day, the only dose tested) for four days induced mammary carcinomas and pulmonary adenomas.
Bendamustine is a mutagen and clastogen. In a reverse bacterial mutation assay (Ames assay), bendamustine was shown to increase revertant frequency in the absence and presence of metabolic activation. Bendamustine was clastogenic in human lymphocytes in vitro, and in rat bone marrow cells in vivo (increase in micronucleated polychromatic erythrocytes) from 37.5 mg/m2, the lowest dose tested.
Impaired spermatogenesis, azoospermia, and total germinal aplasia have been reported in male patients treated with alkylating agents, especially in combination with other drugs. In some instances spermatogenesis may return in patients in remission, but this may occur only several years after intensive chemotherapy has been discontinued. Patients should be warned of the potential risk to their reproductive capacities.
-
14 CLINICAL STUDIES
14.1 Chronic Lymphocytic Leukemia (CLL)
The safety and efficacy of bendamustine hydrochloride were evaluated in an open-label, randomized, controlled multicenter trial comparing bendamustine hydrochloride to chlorambucil. The trial was conducted in 301 previously-untreated patients with Binet Stage B or C (Rai Stages I - IV) CLL requiring treatment. Need-to-treat criteria included hematopoietic insufficiency, B-symptoms, rapidly progressive disease or risk of complications from bulky lymphadenopathy. Patients with autoimmune hemolytic anemia or autoimmune thrombocytopenia, Richter’s syndrome, or transformation to prolymphocytic leukemia were excluded from the study.
The patient populations in the bendamustine hydrochloride and chlorambucil treatment groups were balanced with regard to the following baseline characteristics: age (median 63 vs. 66 years), gender (63% vs. 61% male), Binet stage (71% vs. 69% Binet B), lymphadenopathy (79% vs. 82%), enlarged spleen (76% vs. 80%), enlarged liver (48% vs. 46%), hypercellular bone marrow (79% vs. 73%), “B” symptoms (51% vs. 53%), lymphocyte count (mean 65.7x109/L vs. 65.1x109/L), and serum lactate dehydrogenase concentration (mean 370.2 vs. 388.4 U/L). Ninety percent of patients in both treatment groups had immuno-phenotypic confirmation of CLL (CD5, CD23 and either CD19 or CD20 or both).
Patients were randomly assigned to receive either bendamustine hydrochloride at 100 mg/m2, administered intravenously over a period of 30 minutes on Days 1 and 2 or chlorambucil at 0.8 mg/kg (Broca’s normal weight) administered orally on Days 1 and 15 of each 28-day cycle. Efficacy endpoints of objective response rate and progression-free survival were calculated using a pre-specified algorithm based on NCI working group criteria for CLL.
The results of this open-label randomized study demonstrated a higher rate of overall response and a longer progression-free survival for bendamustine hydrochloride compared to chlorambucil (see Table 5). Survival data are not mature.
Table 5: Efficacy Data for CLL CI = confidence interval
* CR was defined as peripheral lymphocyte count ≤ 4 x 109/L, neutrophils ≥ 1.5 x 109/L, platelets >100 x 109/L, hemoglobin > 110g/L, without transfusions, absence of palpable hepatosplenomegaly, lymph nodes ≤ 1.5 cm, < 30% lymphocytes without nodularity in at least a normocellular bone marrow and absence of “B” symptoms. The clinical and laboratory criteria were required to be maintained for a period of at least 56 days.
** nPR was defined as described for CR with the exception that the bone marrow biopsy shows persistent nodules.
† PR was defined as ≥50% decrease in peripheral lymphocyte count from the pretreatment baseline value, and either ≥50% reduction in lymphadenopathy, or ≥50% reduction in the size of spleen or liver, as well as one of the following hematologic improvements: neutrophils ≥ 1.5 x 109/L or 50% improvement over baseline, platelets >100 x 109/L or 50% improvement over baseline, hemoglobin >110g/L or 50% improvement over baseline without transfusions, for a period of at least 56 days.
†† PFS was defined as time from randomization to progression or death from any cause.Bendamustine Hydrochloride
(N=153)Chlorambucil
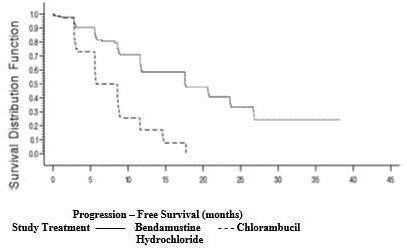
(N=148)p-value Response Rate n (%) Overall response rate 90 (59) 38 (26) <0.0001 (95% CI) (51, 66.6) (18.6, 32.7) Complete response (CR)* 13 (8) 1 (<1) Nodular partial response (nPR)** 4 (3) 0 Partial response (PR) † 73 (48) 37 (25) Progression-Free Survival †† Median, months (95% CI) 18 (11.7, 23.5) 6 (5.6, 8.6) Hazard ratio (95% CI) 0.27 (0.17, 0.43) <0.0001 Kaplan-Meier estimates of progression-free survival comparing bendamustine hydrochloride with chlorambucil are shown in Figure 1.
Figure 1. Progression-Free Survival
14.2 Non-Hodgkin Lymphoma (NHL)
The efficacy of bendamustine hydrochloride was evaluated in a single arm study of 100 patients with indolent B-cell NHL that had progressed during or within six months of treatment with rituximab or a rituximab-containing regimen. Patients were included if they relapsed within 6 months of either the first dose (monotherapy) or last dose (maintenance regimen or combination therapy) of rituximab. All patients received bendamustine hydrochloride intravenously at a dose of 120 mg/m2, on Days 1 and 2 of a 21-day treatment cycle. Patients were treated for up to 8 cycles.
The median age was 60 years, 65% were male, and 95% had a baseline WHO performance status of 0 or 1. Major tumor subtypes were follicular lymphoma (62%), diffuse small lymphocytic lymphoma (21%), and marginal zone lymphoma (16%). Ninety-nine percent of patients had received previous chemotherapy, 91% of patients had received previous alkylator therapy, and 97% of patients had relapsed within 6 months of either the first dose (monotherapy) or last dose (maintenance regimen or combination therapy) of rituximab.
Efficacy was based on the assessments by a blinded independent review committee (IRC) and included overall response rate (complete response + complete response unconfirmed + partial response) and duration of response (DR) as summarized in Table 6.
Table 6: Efficacy Data for NHL* CI = confidence interval
*IRC assessment was based on modified International Working Group response criteria (IWG-RC). Modifications to IWG-RC specified that a persistently positive bone marrow in patients who met all other criteria for CR would be scored as PR. Bone marrow sample lengths were not required to be ≥20 mmBendamustine Hydrochloride
(N=100)Response Rate (%) Overall response rate (CR+CRu+PR) 74 (95% CI) (64.3, 82.3) Complete response (CR) 13 Complete response unconfirmed (CRu) 4 Partial response (PR) 57 Duration of Response (DR) Median, months (95% CI) 9.2 months
(7.1, 10.8) -
15 REFERENCES
- OSHA Hazardous Drugs. OSHA. [Accessed on 02/16/16, from http://www.osha.gov/SLTC/hazardousdrugs/index.html]
-
16 HOW SUPPLIED/STORAGE AND HANDLING
16.1 Safe Handling and Disposal
Bendamustine Hydrochloride Injection is a cytotoxic drug. Follow applicable special handling and disposal procedures1. Care should be exercised in the handling and preparation of solutions prepared from Bendamustine Hydrochloride Injection. The use of gloves and safety glasses is recommended to avoid exposure in case of breakage of the vial or other accidental spillage. If gloves come in contact with Bendamustine Hydrochloride Injection prior to dilution, remove gloves and follow disposal procedures1. If a solution of Bendamustine Hydrochloride Injection contacts the skin, wash the skin immediately and thoroughly with soap and water. If Bendamustine Hydrochloride Injection contacts the mucous membranes, flush thoroughly with water.
16.2 How Supplied
Bendamustine Hydrochloride Injection is supplied in individual cartons of 5 mL clear multiple-dose vials containing 100 mg of bendamustine hydrochloride as a clear, colorless to yellow ready-to-dilute solution.
NDC: 42367-520-25, 100 mg/4 mL (25 mg/mL).
-
17 PATIENT COUNSELING INFORMATION
Allergic (Hypersensitivity) Reactions
Inform patients of the possibility of serious or mild allergic reactions and to immediately report rash, facial swelling, or difficulty breathing during or soon after infusion. [see Warnings and Precautions (5.3)]Myelosuppression
Inform patients of the likelihood that bendamustine hydrochloride will cause a decrease in white blood cells, platelets, and red blood cells and the need for frequent monitoring of blood counts. Advise patients to report shortness of breath, significant fatigue, bleeding, fever, or other signs of infection. [see Warnings and Precautions (5.1)]Hepatotoxicity
Inform patients of the possibility of developing liver function abnormalities and serious hepatic toxicity. Advise patients to immediately contact their health care provider if signs of liver failure occur, including jaundice, anorexia, bleeding or bruising. [see Warnings and Precautions (5.6)].Fatigue
Advise patients that bendamustine hydrochloride may cause tiredness and to avoid driving any vehicle or operating any dangerous tools or machinery if they experience this side effect. [see Adverse Reactions (6.1)]Nausea and Vomiting
Advise patients that bendamustine hydrochloride may cause nausea and/or vomiting. Patients should report nausea and vomiting so that symptomatic treatment may be provided. [see Adverse Reactions (6.1)]Diarrhea
Advise patients that bendamustine hydrochloride may cause diarrhea. Patients should report diarrhea to the physician so that symptomatic treatment may be provided. [see Adverse Reactions (6.1)]Rash
Advise patients that a rash or itching may occur during treatment with bendamustine hydrochloride. Advise patients to immediately report severe or worsening rash or itching. [see Adverse Reactions (5.5)]Pregnancy and Nursing
Bendamustine hydrochloride can cause fetal harm. Women should be advised to avoid becoming pregnant throughout treatment and for 3 months after bendamustine hydrochloride therapy has stopped. Men receiving bendamustine hydrochloride should use reliable contraception for the same time period. Advise patients to report pregnancy immediately. Advise patients to avoid nursing while receiving bendamustine hydrochloride. [see Use in Specific Populations (8.1)]
Marketed by
Eagle Pharmaceuticals, Inc.
Woodcliff Lake, NJAll rights reserved.
- PRINCIPAL DISPLAY PANEL - NDC: 42367-520-25 - Carton Label
- PRINCIPAL DISPLAY PANEL - NDC: 42367-520-25 - Vial Label (Front)
- PRINCIPAL DISPLAY PANEL - NDC: 42367-520-25 - Vial Label (Inside of Front Label)
- PRINCIPAL DISPLAY PANEL - NDC: 42367-520-25 - Vial Label (Base)
-
INGREDIENTS AND APPEARANCE
BENDAMUSTINE HYDROCHLORIDE
bendamustine hydrochloride injectionProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 42367-520 Route of Administration INTRAVENOUS Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength BENDAMUSTINE HYDROCHLORIDE (UNII: 981Y8SX18M) (BENDAMUSTINE - UNII:9266D9P3PQ) BENDAMUSTINE HYDROCHLORIDE 100 mg Inactive Ingredients Ingredient Name Strength PROPYLENE GLYCOL (UNII: 6DC9Q167V3) MONOTHIOGLYCEROL (UNII: AAO1P0WSXJ) POLYETHYLENE GLYCOL 400 (UNII: B697894SGQ) SODIUM HYDROXIDE (UNII: 55X04QC32I) Product Characteristics Color YELLOW (colorless to yellow) Score Shape Size Flavor Imprint Code Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 42367-520-25 1 in 1 CARTON 05/15/2018 09/30/2020 1 1 in 1 VIAL, MULTI-DOSE; Type 0: Not a Combination Product Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date NDA NDA205580 05/15/2018 09/30/2020 Labeler - Eagle Pharmaceuticals, Inc (849818161)
© 2026 FDA.report
This site is not affiliated with or endorsed by the FDA.