ADAKVEO- crizanlizumab injection
ADAKVEO by
Drug Labeling and Warnings
ADAKVEO by is a Prescription medication manufactured, distributed, or labeled by Novartis Pharmaceuticals Corporation. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
-
HIGHLIGHTS OF PRESCRIBING INFORMATION
These highlights do not include all the information needed to use ADAKVEO safely and effectively. See full prescribing information for ADAKVEO.
ADAKVEO® (crizanlizumab-tmca) injection, for intravenous use
Initial U.S. Approval: 2019
INDICATIONS AND USAGE
ADAKVEO is a selectin blocker indicated to reduce the frequency of vasoocclusive crises in adults and pediatric patients aged 16 years and older with sickle cell disease. (1)
DOSAGE AND ADMINISTRATION
DOSAGE FORMS AND STRENGTHS
Injection: 100 mg/10 mL (10 mg/mL) solution in a single-dose vial. (3)
CONTRAINDICATIONS
None. (4)
WARNINGS AND PRECAUTIONS
ADVERSE REACTIONS
Most common adverse reactions (incidence > 10%) are nausea, arthralgia, back pain, and pyrexia. (6.1)
To report SUSPECTED ADVERSE REACTIONS, contact Novartis Pharmaceuticals Corporation at 1-888-669-6682 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.USE IN SPECIFIC POPULATIONS
Pregnancy: May cause fetal harm. (8.1)
See 17 for PATIENT COUNSELING INFORMATION and FDA-approved patient labeling.
Revised: 11/2019
-
Table of Contents
FULL PRESCRIBING INFORMATION: CONTENTS*
1 INDICATIONS AND USAGE
2 DOSAGE AND ADMINISTRATION
2.1 Recommended Dosage
2.2 Preparation and Administration
3 DOSAGE FORMS AND STRENGTHS
4 CONTRAINDICATIONS
5 WARNINGS AND PRECAUTIONS
5.1 Infusion-Related Reactions
5.2 Laboratory Test Interference
6 ADVERSE REACTIONS
6.1 Clinical Trials Experience
6.2 Immunogenicity
7 DRUG INTERACTIONS
7.1 Laboratory Test Interference
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
8.2 Lactation
8.4 Pediatric Use
8.5 Geriatric Use
11 DESCRIPTION
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
12.2 Pharmacodynamics
12.3 Pharmacokinetics
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
13.2 Animal Toxicology and/or Pharmacology
14 CLINICAL STUDIES
16 HOW SUPPLIED/STORAGE AND HANDLING
17 PATIENT COUNSELING INFORMATION
- * Sections or subsections omitted from the full prescribing information are not listed.
- 1 INDICATIONS AND USAGE
-
2 DOSAGE AND ADMINISTRATION
2.1 Recommended Dosage
Administer ADAKVEO 5 mg/kg by intravenous infusion over a period of 30 minutes at Week 0, Week 2, and every 4 weeks thereafter.
If a dose is missed, administer ADAKVEO as soon as possible.
If ADAKVEO is administered within 2 weeks after the missed dose, continue dosing according to the patient's original schedule.
If ADAKVEO is administered more than 2 weeks after the missed dose, continue dosing every 4 weeks thereafter.
ADAKVEO may be given with or without hydroxyurea.
2.2 Preparation and Administration
ADAKVEO should be prepared and administered by a healthcare professional.
Preparation
- Use aseptic technique to prepare the solution for infusion.
- Calculate the dose (mg) and the total volume (mL) of ADAKVEO solution required, and the number of ADAKVEO vials needed based on the patient’s actual body weight.
- Prepare 5 mg of ADAKVEO per kg of actual body weight.
- Calculate the volume of ADAKVEO to be used according to the following equation:
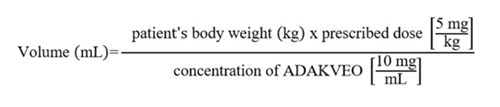
Dilution
Dilute ADAKVEO in 0.9% Sodium Chloride Injection, USP or 5% Dextrose Injection, USP to a total volume of 100 mL for intravenous infusion as follows:
- Obtain the number of vials required. One vial is needed for every 10 mL of ADAKVEO.
- Bring vials to room temperature for a maximum of 4 hours prior to the start of preparation (piercing the first vial).
- Visually inspect the vials.
- Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit.
- ADAKVEO is clear to opalescent, colorless or may have a slightly brownish-yellow tint.
- Do not use if particles are present in the solution.
- Obtain a 100 mL 0.9% Sodium Chloride Injection or 5% Dextrose Injection infusion bag/container
- Infusion bags/containers must be made of either polyvinyl chloride (PVC), polyethylene (PE), or polypropylene (PP).
- Remove a volume of 0.9% Sodium Chloride Injection or 5% Dextrose Injection from the infusion bag/container that is equal to the required volume of ADAKVEO solution.
- Withdraw the necessary amount of ADAKVEO solution and dilute by adding to the infusion bag/container containing 0.9% Sodium Chloride Injection or 5% Dextrose Injection.
- The volume of ADAKVEO added to the infusion bag/container should not exceed 96 mL.
- Gently invert the infusion bag to mix the diluted solution. DO NOT SHAKE.
- Single-dose vials. Discard unused portion.
Storage Conditions of the Diluted Solution
Administer ADAKVEO diluted solution as soon as possible. If not administered immediately, store the prepared solution either:
- At room temperature up to 25°C (77°F) for no more than 4.5 hours from the start of the preparation (piercing the first vial) to the completion of infusion.
- Under refrigeration at 2°C to 8°C (36°F to 46°F) for no more than 24 hours, from the start of the time of the preparation (piercing the first vial) to the completion of infusion. This includes the storage of the diluted solution and the time to warm up to room temperature. Protect the diluted solution from light during storage under refrigeration.
Administration
- Administer ADAKVEO diluted solution by intravenous infusion over a period of 30 minutes through an intravenous line, which must contain a sterile, nonpyrogenic 0.2 micron inline filter.
- No incompatibilities have been observed between ADAKVEO and infusion sets composed of PVC, polyethylene (PE-lined PVC), polyurethane (PU), and in-line filter membranes composed of polyethersulfone (PES, neutral and positively charged), positively charged polyamide (PA), and polysulphone (PSU).
- Do not mix or coadminister with other drugs through the same intravenous line.
- After administration of ADAKVEO, flush the line with at least 25 mL of 0.9% Sodium Chloride or 5% Dextrose Injection.
- Dispose of any unused product or waste material in accordance with local requirements.
- 3 DOSAGE FORMS AND STRENGTHS
- 4 CONTRAINDICATIONS
-
5 WARNINGS AND PRECAUTIONS
5.1 Infusion-Related Reactions
In the SUSTAIN clinical trial, infusion-related reactions (defined as occurring within 24 hours of infusion) were observed in 2 (3%) patients treated with ADAKVEO 5 mg/kg. Monitor patients for signs and symptoms of infusion-related reactions, which may include fever, chills, nausea, vomiting, fatigue, dizziness, pruritus, urticaria, sweating, shortness of breath or wheezing. Discontinue ADAKVEO infusion for severe reactions and institute appropriate medical care.
5.2 Laboratory Test Interference
Interference with automated platelet counts (platelet clumping) has been observed following administration of ADAKVEO, in particular, when blood samples were collected in tubes containing ethylenediaminetetraacetic acid (EDTA). Mitigation strategies are recommended [see Drug Interactions (7.1)].
-
6 ADVERSE REACTIONS
The following clinically significant adverse reactions are described elsewhere in the labeling:
- Infusion-related reactions [see Warnings and Precautions (5.1)]
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Sickle Cell Disease
The safety of ADAKVEO was evaluated in the SUSTAIN trial [see Clinical Studies (14.1)]. Eligible patients were diagnosed with sickle cell disease (any genotype including HbSS, HbSC, HbS beta0-thalassemia, HbSbeta+thalassemia, and others). Patients received ADAKVEO 5 mg/kg (N = 66) or 2.5 mg/kg (N = 64) or placebo (N = 62) administered by intravenous infusion on Week 0, Week 2, and every 4 weeks thereafter. The safety evaluation below is limited to the patients who received the recommended dose of 5 mg/kg.
Among the 66 patients that received the recommended dose (5 mg/kg), 83% were exposed for 6 months or longer and 61% were exposed for approximately one year; forty-two (64%) patients were treated with ADAKVEO in combination with hydroxyurea.
Serious adverse reactions were reported in 2 patients (3%) treated with ADAKVEO 5 mg/kg; both reactions were pyrexia.
Two deaths (3%) occurred in the ADAKVEO 5 mg/kg treatment group. None of the deaths were considered to be related to ADAKVEO.
The most common adverse reactions (≥ 10%) were nausea, arthralgia, back pain, and pyrexia.
Table 1 summarizes the adverse reactions in the SUSTAIN trial.
Table 1: Adverse Reactions (≥ 10%) in Patients Receiving ADAKVEO With a Difference Between Arms of > 3% Compared to Placebo in SUSTAIN ADAKVEO 5 mg/kg
N = 66
n (%)Placebo
N = 62
n (%)Adverse Reactions All Grades
(%)Grade ≥ 3
(%)All Grades
(%)Grade ≥ 3
(%)Gastrointestinal Disorders Nausea 12 (18) 0 7 (11) 1 (2) Musculoskeletal and Connective Tissue Disorders Arthralgia 12 (18) 1 (2) 5 (8) 1 (2) Back pain 10 (15) 0 7 (11) 0 General Disorders and Administration Site Conditions Pyrexia 7 (11) 1 (2) 4 (7) 0 Clinically relevant adverse reactions (all Grades) that were reported in less than < 10% of patients treated with ADAKVEO included: oropharyngeal pain, abdominal pain (abdominal pain, upper abdominal pain, lower abdominal pain, abdominal discomfort, and abdominal tenderness), diarrhea, vomiting, pruritus (pruritus and vulvovaginal pruritus), musculoskeletal chest pain, myalgia, infusion-site reaction (infusion-site extravasation, infusion-site pain, and infusion-site swelling), and infusion-related reaction.
6.2 Immunogenicity
As with all therapeutic proteins, there is potential for immunogenicity. The detection of antibody formation is highly dependent on the sensitivity and specificity of the assay. Additionally, the observed incidence of antibody (including neutralizing antibody) positivity in an assay may be influenced by several factors including assay methodology, sample handling, timing of sample collection, concomitant medications, and underlying disease. For these reasons, comparison of the incidence of antibodies in the studies described below with the incidence of antibodies in other studies or to other crizanlizumab products may be misleading.
The immunogenicity of ADAKVEO was evaluated using a validated bridging immunoassay for the detection of binding anti-crizanlizumab-tmca antibodies. In a single arm, open label multiple dose study, 0 of the 45 patients with sickle cell disease treated with ADAKVEO 5 mg/kg tested positive for treatment-induced anti-crizanlizumab-tmca antibodies. In a single-dose study of healthy subjects, 1 of the 61 (1.6%) evaluable subjects tested positive for a treatment-induced anti-crizanlizumab-tmca antibodies.
-
7 DRUG INTERACTIONS
7.1 Laboratory Test Interference
Platelet Tests
ADAKVEO interferes with automated platelet counts (platelet clumping) in particular when blood samples are collected in tubes containing EDTA, which may lead to unevaluable or falsely decreased platelet counts. Run blood samples within 4 hours of blood collection or collect blood samples in tubes containing citrate. When needed, estimate platelet count via peripheral blood smear.
-
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Risk Summary
Based on data from animal studies, ADAKVEO has the potential to cause fetal harm when administered to a pregnant woman. In an animal reproduction study, intravenous administration of crizanlizumab-tmca to pregnant cynomolgus monkeys from the onset of organogenesis through delivery resulted in a non-dose related increased fetal loss (abortions/stillbirths) at doses approximately 2.8 times the exposure at the recommended clinical dose at 5 mg/kg/dose once every 4 weeks (see Data).
There are insufficient human data on ADAKVEO use in pregnant women to evaluate for a drug-associated risk of major birth defects, miscarriage, or adverse maternal or fetal outcomes. Advise pregnant women of the potential risk to a fetus. ADAKVEO should only be used during pregnancy if the expected benefit to the patient justifies the potential risk to the fetus.
The estimated background risk of major birth defects and miscarriage for the indicated population is approximately 14% and up to 43%, respectively. All pregnancies have a background risk of birth defect, loss, or other adverse outcomes.
Clinical Considerations
Disease-Associated Maternal and/or Embryo/Fetal Risk
Women with sickle cell disease have an increased risk of adverse pregnancy outcomes for the mother and the fetus. Pregnant women are at greater risk for VOCs, pre-eclampsia, eclampsia, and maternal mortality. For the fetus, there is an increased risk for intrauterine growth restriction, preterm delivery, low birth weight, and perinatal mortality.
Data
Animal Data
In an enhanced pre- and postnatal development study in cynomolgus monkeys, pregnant animals received intravenous doses of crizanlizumab-tmca at 10 and 50 mg/kg once every 2 weeks during the period of onset of organogenesis through delivery. No maternal toxicity was observed. Maternal exposures at doses of 10 and 50 mg/kg were between 2.8 and 16 times, respectively, the human clinical exposure based on area under the curve (AUC) in patients with sickle cell disease at 5 mg/kg/dose once every 4 weeks. There was an increase in fetal loss (abortions or still births) at both crizanlizumab-tmca doses which was higher in the third trimester.
There were no effects on infant growth and development through 6-months postpartum that were attributable to crizanlizumab-tmca.
Measurable crizanlizumab-tmca serum concentrations were observed in the infant monkeys at postnatal Day 28, confirming that crizanlizumab crosses the placental barrier.
8.2 Lactation
Risk Summary
There is no data on the presence of crizanlizumab-tmca in human or animal milk, the effects on the breastfed child, or the effects on milk production. Maternal IgG is known to be present in human milk. The effects of local gastrointestinal exposure and limited systemic exposure in the breastfed child to crizanlizumab-tmca are unknown.
The developmental and health benefits of breast-feeding should be considered along with the mother’s clinical need for ADAKVEO and any potential adverse effects on the breastfed child from ADAKVEO or from the underlying maternal condition.
8.4 Pediatric Use
The safety and effectiveness of ADAKVEO for sickle cell disease have been established in pediatric patients aged 16 years and older. Use of ADAKVEO for sickle cell disease is supported by evidence from adequate and well-controlled studies in adults and pediatric patients (SUSTAIN Trial). The SUSTAIN trial enrolled one pediatric patient treated with ADAKVEO 5 mg/kg aged 16 years old [see Adverse Reactions (6.1), Clinical Pharmacology (12.3), Clinical Studies (14)].
The safety and efficacy of ADAKVEO in pediatric patients below the age of 16 years have not been established.
-
11 DESCRIPTION
Crizanlizumab-tmca is a selectin blocker humanized IgG2 kappa monoclonal antibody that binds to P-selectin. Crizanlizumab-tmca is produced using recombinant DNA technology in Chinese hamster ovary (CHO) cells. It is composed of 2 heavy chains, each containing 448 amino acids, and 2 light chains each containing 218 amino acids, with a theoretical molecular weight of approximately 146 kDa.
ADAKVEO (crizanlizumab-tmca) injection is supplied as a sterile, preservative-free, clear to opalescent, colorless to slightly brownish-yellow solution for dilution and subsequent administration by intravenous infusion. Each 10 mL vial contains 100 mg crizanlizumab-tmca, citric acid (5.4 mg), polysorbate 80 (2 mg), sodium citrate (50.5 mg), sucrose (753.3 mg) and water for injection with a pH of 6.
-
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Crizanlizumab-tmca is a humanized IgG2 kappa monoclonal antibody that binds to P-selectin and blocks interactions with its ligands including P-selectin glycoprotein ligand 1.
Binding P-selectin on the surface of the activated endothelium and platelets blocks interactions between endothelial cells, platelets, red blood cells, and leukocytes.
12.2 Pharmacodynamics
ADAKVEO resulted in a dose-dependent P-selectin inhibition (measured ex vivo) in patients with sickle cell disease and healthy volunteers.
12.3 Pharmacokinetics
The pharmacokinetics of crizanlizumab-tmca were evaluated in healthy volunteers and patients with sickle cell disease. The mean crizanlizumab-tmca Cmax, AUClast, or AUCinf increased disproportionally over the dose range of 0.2 to 8 mg/kg (0.04 to 1.6 times the approved recommended dosage) in healthy volunteers. In healthy volunteers administered the 5 mg/kg dose, the mean [coefficient of variation (CV%)] crizanlizumab-tmca Cmax, AUClast, or AUCinf were 0.16 (15.3%) mg/mL, 33.6 (12.6%) mg*hr/mL and 34.6 (13.1%) mg*hr/mL, respectively.
Distribution
The mean (% CV) volume of distribution was 4.26 (25.1%) L after a single crizanlizumab-tmca 5 mg/kg intravenous infusion in healthy volunteers.
Elimination
The mean (% CV) terminal elimination half-life (t1/2) of crizanlizumab-tmca was 10.6 (20.5%) days and the mean clearance was 11.7 (16.2%) mL/hr at 5 mg/kg doses in healthy volunteers. The mean (% CV) elimination t1/2 of crizanlizumab-tmca was 7.6 (28.5%) days during dosing interval in patients with sickle cell disease.
Metabolism
Crizanlizumab-tmca is expected to be metabolized into small peptides by catabolic pathways.
Specific Populations
The effect of renal or hepatic impairment on the pharmacokinetics of crizanlizumab-tmca is unknown.
Drug Interaction Studies
Hydroxyurea had no clinically meaningful effect on crizanlizumab-tmca pharmacokinetics in patients in clinical studies.
-
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
No carcinogenicity or genotoxicity studies have been conducted with crizanlizumab-tmca.
In the 26-week repeat-dose toxicity study, cynomolgus monkeys were administered crizanlizumab-tmca once every 4 weeks at doses up to 50 mg/kg (at least 13.5 times the human clinical exposure based on AUC in patients with sickle cell disease at 5 mg/kg once every 4 weeks). There were no adverse effects of crizanlizumab-tmca on male or female reproductive organs.
-
14 CLINICAL STUDIES
The efficacy of ADAKVEO was evaluated in patients with sickle cell disease in SUSTAIN [NCT01895361], a 52-week, randomized, multicenter, placebo-controlled, double-blind study. A total of 198 patients with sickle cell disease, any genotype (HbSS, HbSC, HbS/beta0-thalassemia, HbS/beta+-thalassemia, and others), and a history of 2-10 VOCs in the previous 12 months were eligible for inclusion. Patients were randomized 1:1:1 to ADAKVEO 5 mg/kg (N = 67), ADAKVEO 2.5 mg/kg (N = 66), or placebo (N = 65) administered over a period of 30 minutes by intravenous infusion on Week 0, Week 2, and every 4 weeks thereafter for a treatment duration of 52 weeks. Randomization was stratified by patients already receiving hydroxyurea (Y/N) and by the number of VOCs in the previous 12 months (2 to 4, 5 to 10).
Patients received ADAKVEO (with or without hydroxyurea) and were allowed to receive occasional transfusions and pain medications [i.e., acetaminophen, non-steroidal anti-inflammatory drugs (NSAIDs), and opioids] on an as needed basis.
Patients recruited in the study had complications associated with sickle cell disease and other comorbidities including a history of acute chest syndrome (18%); pulmonary hypertension (8%); priapism (7%); psychiatric manifestations (25%) including depression and anxiety; hypertension (17%); cholelithiasis (17%). Demographic and other baseline characteristics were similar among the treatment groups (see Table 2).
Table 2: Demographics and Baseline Characteristics in SUSTAIN Study Abbreviation: VOCs, vasoocclusive crises. ADAKVEO 5 mg/kg
(N = 67)Placebo
(N = 65)Age (years) Median 29 26 Range 16, 63 16, 56 Gender, n (%) Male 32 (48%) 27 (42%) Female 35 (52%) 38 (59%) Ethnicity, n (%) Hispanic or Latino 20 (30%) 11 (17%) Not Hispanic or Latino 45 (67%) 53 (82%) Unknown 2 (3%) 1 (2%) Race black or African American 60 (90%) 60 (92%) white 4 (6%) 3 (5%) Other 3 (5%) 2 (3%) Sickle cell disease genotype, n (%) HbSS 47 (70%) 47 (72%) HbSC 9 (13%) 8 (12%) HbS/beta0 - thalassemia 3 (5%) 7 (11%) HbS/beta+ - thalassemia 7 (10%) 1 (2%) Other 1 (2%) 2 (3%) Hydroxyurea use, n (%) Yes 42 (63%) 40 (62%) No 25 (37%) 25 (39%) Number of VOCs in previous 12 months, n (%) 2 to 4 42 (63%) 41 (63%) 5 to 10 25 (37%) 24 (37%) Efficacy was evaluated in the SUSTAIN study by the annual rate of VOCs leading to a healthcare visit. A VOC leading to a healthcare visit was defined as an acute episode of pain with no cause other than a vaso-occlusive event that required a medical facility visit and treatment with oral or parenteral opioids, or parenteral NSAIDs. Acute chest syndrome, hepatic sequestration, splenic sequestration, and priapism (requiring a visit to a medical facility) were also considered VOCs.
Patients with sickle cell disease who received ADAKVEO 5 mg/kg had a lower median annual rate of VOC compared to patients who received placebo (1.63 vs. 2.98) which was statistically significant (p = 0.010). Reductions in the frequency of VOCs were observed among patients regardless of sickle cell disease genotype and/or hydroxyurea use.
Thirty-six percent (36%) of patients treated with ADAKVEO 5 mg/kg did not experience a VOC compared to 17% of placebo-treated patients. The median time to first VOC from randomization was 4.1 months in the ADAKVEO 5mg/kg arm compared to 1.4 months in the placebo.
The main efficacy results of the pivotal study, SUSTAIN, are summarized in Table 3.
Table 3: Efficacy Results from SUSTAIN Trial in Sickle Cell Diseasea Abbreviations: HL, hodges-lehmann; VOC, vasoocclusive crises.
aVOCs were as assessed by an independent review committee.
bStandard median.
cHL median difference [95% confidence interval (CI)].Event ADAKVEO, 5 mg/kgb
(n = 67)Placebob
(n = 65)Treatment Difference Estimatec Annual rate of VOCa 1.63 2.98 HL = -1.01, (-2.00, 0.00) Annual rate of days hospitalized 4 6.87 -
16 HOW SUPPLIED/STORAGE AND HANDLING
How Supplied
ADAKVEO (crizanlizumab-tmca) injection is a sterile, clear to opalescent, colorless to slightly brownish-yellow solution for intravenous infusion supplied as:
Carton containing one 100 mg/10 mL (10 mg/mL) single-dose vial NDC: 0078-0883-61
The single-dose vial has a rubber stopper and an aluminum cap with a plastic flip-off disk. Each 10 mL vial is made of Type 1 glass.
Storage and Handling
- Store and transport refrigerated at 2°C to 8°C (36°F to 46°F) in the original carton to protect from light.
- Do not shake. Do not freeze.
-
17 PATIENT COUNSELING INFORMATION
Advise the patient to read the FDA-approved patient labeling (Patient Information).
Infusion-Related Reactions
Advise patients to contact their healthcare provider immediately for signs or symptoms of infusion-related reactions [see Warnings and Precautions (5.1)].
Interference With Automated Platelet Counts
Advise patients to inform their healthcare provider that they are receiving ADAKVEO prior to any blood tests due to the potential interference with laboratory tests used to measure platelet counts [see Warnings and Precautions (5.2)].
Manufactured by:
Novartis Pharmaceuticals Corporation
One Health Plaza
East Hanover, New Jersey 07936US License No. 1244
© Novartis
T2019-119
-
PATIENT PACKAGE INSERT
This Patient Information has been approved by the U.S. Food and Drug Administration. Issued: November 2019 PATIENT INFORMATION ADAKVEO® (ah dak vee oh)
(crizanlizumab-tmca)
injection, for intravenous useWhat is the most important information I should know about ADAKVEO?
ADAKVEO may cause serious side effects, including:
Infusion reactions. Infusion reactions may happen within 24 hours of receiving an infusion of ADAKVEO. Tell your healthcare provider right away if you get any of the following signs and symptoms of an infusion reaction:- fever
- chills or shivering
- nausea
- vomiting
- tiredness
- dizziness
- sweating
- hives
- itching
- shortness of breath or wheezing
Your healthcare provider may monitor you for signs and symptoms of infusion reactions.
ADAKVEO may interfere with a certain blood test.
Tell your healthcare providers that you are receiving ADAKVEO before having any blood tests. ADAKVEO may interfere with a laboratory test to measure your platelet counts.
See "What are possible side effects of ADAKVEO?" for more information about side effects.What is ADAKVEO?
ADAKVEO is used:- in people 16 years of age and older who have sickle cell disease
- to help reduce how often certain episodes (crises) happen.
Before receiving ADAKVEO, tell your healthcare provider about all of your medical conditions, including if you: - are pregnant or plan to become pregnant. It is not known if ADAKVEO may harm your unborn baby.
- are breastfeeding or plan to breastfeed. It is not known if ADAKVEO passes into your breast milk. You and your healthcare provider should decide the best way to feed your baby during treatment with ADAKVEO.
How will I receive ADAKVEO? - Your healthcare provider will give you ADAKVEO as an infusion into your vein through an intravenous (IV) line over 30 minutes.
- You will receive your first infusion, and then a second infusion 2 weeks later. After that, you will receive an infusion every 4 weeks.
- Your healthcare provider may also prescribe other treatments for you to take during treatment with ADAKVEO.
- Do not stop receiving ADAKVEO unless your healthcare provider tells you to.
- If you miss an appointment for infusion, call your healthcare provider as soon as possible to reschedule.
What are the possible side effects of ADAKVEO?
ADAKVEO may cause serious side effects. See "What is the most important information I should know about ADAKVEO?"
The most common side effects of ADAKVEO include:- nausea
- back pain
- joint pain
- fever
These are not all of the possible side effects of ADAKVEO. For more information, ask your healthcare provider or pharmacist.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.General information about the safe and effective use of ADAKVEO. Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. You can ask your healthcare provider or pharmacist for more information about ADAKVEO. What are the ingredients in ADAKVEO? Active ingredient: crizanlizumab-tmca
Inactive ingredients: citric acid, polysorbate 80, sodium citrate, and water for injectionManufactured by: Novartis Pharmaceuticals Corporation, One Health Plaza, East Hanover, New Jersey 07936
U.S. License No. 1244
© Novartis
T2019-120
For more information, go to www.adakveo.com or call 1-877-ADAKVE-0 (1-877-232-5830).
-
PRINCIPAL DISPLAY PANEL
NDC: 0078-0883-61
Rx Only
ADAKVEO®
(crizanlizumab-tmca)
Injection100 mg/10 mL
(10 mg/mL)For intravenous infusion after dilution.
1 Single-Dose Vial.
Discard Unused Portion.NOVARTIS

-
INGREDIENTS AND APPEARANCE
ADAKVEO
crizanlizumab injectionProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 0078-0883 Route of Administration INTRAVENOUS Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength CRIZANLIZUMAB (UNII: L7451S9126) (CRIZANLIZUMAB - UNII:L7451S9126) CRIZANLIZUMAB 10 mg in 1 mL Inactive Ingredients Ingredient Name Strength SUCROSE (UNII: C151H8M554) 75.33 mg in 1 mL SODIUM CITRATE (UNII: 1Q73Q2JULR) 5.053 mg in 1 mL CITRIC ACID MONOHYDRATE (UNII: 2968PHW8QP) 0.54 mg in 1 mL POLYSORBATE 80 (UNII: 6OZP39ZG8H) 0.200 mg in 1 mL WATER (UNII: 059QF0KO0R) Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 0078-0883-61 10 mL in 1 VIAL, GLASS; Type 0: Not a Combination Product 11/15/2019 Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date BLA BLA761128 11/15/2019 Labeler - Novartis Pharmaceuticals Corporation (002147023)
Trademark Results [ADAKVEO]
Mark Image Registration | Serial | Company Trademark Application Date |
|---|---|
 ADAKVEO 79236498 5609269 Live/Registered |
Novartis AG 2018-05-12 |
 ADAKVEO 79100532 4152348 Dead/Cancelled |
Novartis AG 2011-07-08 |
© 2026 FDA.report
This site is not affiliated with or endorsed by the FDA.