TRELEGY ELLIPTA- fluticasone furoate, umeclidinium bromide and vilanterol trifenatate powder
Trelegy Ellipta by
Drug Labeling and Warnings
Trelegy Ellipta by is a Prescription medication manufactured, distributed, or labeled by GlaxoSmithKline LLC. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
-
HIGHLIGHTS OF PRESCRIBING INFORMATION
These highlights do not include all the information needed to use TRELEGY ELLIPTA safely and effectively. See full prescribing information for TRELEGY ELLIPTA.
TRELEGY ELLIPTA (fluticasone furoate, umeclidinium, and vilanterol inhalation powder), for oral inhalation use
Initial U.S. Approval: 2017RECENT MAJOR CHANGES
INDICATIONS AND USAGE
TRELEGY ELLIPTA is a combination of fluticasone furoate, an inhaled corticosteroid (ICS); umeclidinium, an anticholinergic; and vilanterol, a long‑acting beta2-adrenergic agonist (LABA), indicated for the maintenance treatment of patients with chronic obstructive pulmonary disease (COPD). (1)
Important limitations of use: Not indicated for relief of acute bronchospasm or the treatment of asthma. (1, 5.2)
DOSAGE AND ADMINISTRATION
DOSAGE FORMS AND STRENGTHS
Inhalation powder: Inhaler containing 2 foil blister strips of powder formulation for oral inhalation. One strip contains fluticasone furoate 100 mcg per blister and the other contains umeclidinium/vilanterol 62.5 mcg/25 mcg per blister. (3)
CONTRAINDICATIONS
Severe hypersensitivity to milk proteins or any ingredients. (4)
WARNINGS AND PRECAUTIONS
- LABA monotherapy increases the risk of serious asthma-related events. (5.1)
- Do not initiate in acutely deteriorating COPD. Do not use to treat acute symptoms. (5.2)
- Do not use in combination with an additional medicine containing a LABA because of risk of overdose. (5.3)
- Candida albicans infection of the mouth and pharynx may occur. Monitor patients periodically. Advise the patient to rinse his/her mouth with water without swallowing after inhalation to help reduce the risk. (5.4)
- Increased risk of pneumonia in patients with COPD. Monitor patients for signs and symptoms of pneumonia. (5.5)
- Potential worsening of infections (e.g., existing tuberculosis; fungal, bacterial, viral, or parasitic infections; ocular herpes simplex). Use with caution in patients with these infections. More serious or even fatal course of chickenpox or measles can occur in susceptible patients. (5.6)
- Risk of impaired adrenal function when transferring from systemic corticosteroids. Taper patients slowly from systemic corticosteroids if transferring to TRELEGY ELLIPTA. (5.7)
- Hypercorticism and adrenal suppression may occur with very high dosages or at the regular dosage in susceptible individuals. If such changes occur, consider appropriate therapy. (5.8)
- If paradoxical bronchospasm occurs, discontinue TRELEGY ELLIPTA and institute alternative therapy. (5.10)
- Use with caution in patients with cardiovascular disorders because of beta-adrenergic stimulation. (5.12)
- Assess for decrease in bone mineral density initially and periodically thereafter. (5.13)
- Glaucoma and cataracts may occur with long-term use of ICS. Worsening of narrow-angle glaucoma may occur. Use with caution in patients with narrow-angle glaucoma and instruct patients to contact a healthcare provider immediately if symptoms occur. Consider referral to an ophthalmologist in patients who develop ocular symptoms or use TRELEGY ELLIPTA long term. (5.14)
- Worsening of urinary retention may occur. Use with caution in patients with prostatic hyperplasia or bladder-neck obstruction and instruct patients to contact a healthcare provider immediately if symptoms occur. (5.15)
- Use with caution in patients with convulsive disorders, thyrotoxicosis, diabetes mellitus, and ketoacidosis. (5.16)
- Be alert to hypokalemia and hyperglycemia. (5.17)
ADVERSE REACTIONS
Most common adverse reactions (incidence ≥1%) are upper respiratory tract infection, pneumonia, bronchitis, oral candidiasis, headache, back pain, arthralgia, influenza, sinusitis, pharyngitis, rhinitis, dysgeusia, constipation, urinary tract infection, diarrhea, gastroenteritis, oropharyngeal pain, cough, and dysphonia. (6.1)
To report SUSPECTED ADVERSE REACTIONS, contact GlaxoSmithKline at 1-888-825-5249 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
DRUG INTERACTIONS
- Strong cytochrome P450 3A4 inhibitors (e.g., ketoconazole): Use with caution. May cause systemic corticosteroid and cardiovascular effects. (7.1)
- Monoamine oxidase inhibitors and tricyclic antidepressants: Use with extreme caution. May potentiate effect of vilanterol on vascular system. (7.2)
- Beta-blockers: Use with caution. May block bronchodilatory effects of beta-agonists and produce severe bronchospasm. (7.3)
- Diuretics: Use with caution. Electrocardiographic changes and/or hypokalemia associated with non–potassium-sparing diuretics may worsen with concomitant beta-agonists. (7.4)
- Anticholinergics: May interact additively with concomitantly used anticholinergic medications. Avoid administration of TRELEGY ELLIPTA with other anticholinergic-containing drugs. (7.5)
USE IN SPECIFIC POPULATIONS
See 17 for PATIENT COUNSELING INFORMATION and FDA-approved patient labeling.
Revised: 5/2019
-
Table of Contents
FULL PRESCRIBING INFORMATION: CONTENTS*
1 INDICATIONS AND USAGE
2 DOSAGE AND ADMINISTRATION
3 DOSAGE FORMS AND STRENGTHS
4 CONTRAINDICATIONS
5 WARNINGS AND PRECAUTIONS
5.1 Serious Asthma-Related Events – Hospitalizations, Intubations, Death
5.2 Deterioration of Disease and Acute Episodes
5.3 Excessive Use of TRELEGY ELLIPTA and Use with Other Long-acting Beta2-agonists
5.4 Local Effects of Inhaled Corticosteroids
5.5 Pneumonia
5.6 Immunosuppression
5.7 Transferring Patients from Systemic Corticosteroid Therapy
5.8 Hypercorticism and Adrenal Suppression
5.9 Drug Interactions with Strong Cytochrome P450 3A4 Inhibitors
5.10 Paradoxical Bronchospasm
5.11 Hypersensitivity Reactions, including Anaphylaxis
5.12 Cardiovascular Effects
5.13 Reduction in Bone Mineral Density
5.14 Glaucoma and Cataracts, Worsening of Narrow-Angle Glaucoma
5.15 Worsening of Urinary Retention
5.16 Coexisting Conditions
5.17 Hypokalemia and Hyperglycemia
6 ADVERSE REACTIONS
6.1 Clinical Trials Experience
7 DRUG INTERACTIONS
7.1 Inhibitors of Cytochrome P450 3A4
7.2 Monoamine Oxidase Inhibitors and Tricyclic Antidepressants
7.3 Beta-adrenergic Receptor Blocking Agents
7.4 Non–Potassium-Sparing Diuretics
7.5 Anticholinergics
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
8.2 Lactation
8.4 Pediatric Use
8.5 Geriatric Use
8.6 Hepatic Impairment
8.7 Renal Impairment
10 OVERDOSAGE
10.1 Fluticasone Furoate
10.2 Umeclidinium
10.3 Vilanterol
11 DESCRIPTION
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
12.2 Pharmacodynamics
12.3 Pharmacokinetics
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
14 CLINICAL STUDIES
16 HOW SUPPLIED/STORAGE AND HANDLING
17 PATIENT COUNSELING INFORMATION
- * Sections or subsections omitted from the full prescribing information are not listed.
- 1 INDICATIONS AND USAGE
-
2 DOSAGE AND ADMINISTRATION
TRELEGY ELLIPTA should be administered as 1 inhalation once daily by the orally inhaled route only.
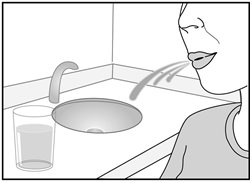
After inhalation, the patient should rinse his/her mouth with water without swallowing to help reduce the risk of oropharyngeal candidiasis.
TRELEGY ELLIPTA should be used at the same time every day.
Do not use TRELEGY ELLIPTA more than 1 time every 24 hours.
No dosage adjustment is required for geriatric patients, patients with renal impairment, or patients with moderate hepatic impairment [see Clinical Pharmacology (12.3)].
-
3 DOSAGE FORMS AND STRENGTHS
Inhalation powder: Disposable light grey and beige plastic inhaler containing 2 foil blister strips of powder intended for oral inhalation only. One strip contains fluticasone furoate (100 mcg per blister) and the other strip contains a blend of umeclidinium and vilanterol (62.5 mcg and 25 mcg per blister, respectively).
- 4 CONTRAINDICATIONS
-
5 WARNINGS AND PRECAUTIONS
5.1 Serious Asthma-Related Events – Hospitalizations, Intubations, Death
The safety and efficacy of TRELEGY ELLIPTA in patients with asthma have not been established. TRELEGY ELLIPTA is not indicated for the treatment of asthma.
Use of long-acting beta2-adrenergic agonists (LABA) as monotherapy [without inhaled corticosteroid (ICS)] for asthma is associated with an increased risk of asthma-related death. Available data from controlled clinical trials also suggest that use of LABA as monotherapy increases the risk of asthma-related hospitalization in pediatric and adolescent patients. These findings are considered a class effect of LABA monotherapy. When LABA are used in fixed‑dose combination with ICS, data from large clinical trials do not show a significant increase in the risk of serious asthma-related events (hospitalizations, intubations, death) compared with ICS alone.
Available data from clinical trials in subjects with COPD do not suggest an increased risk of death with use of LABA in patients with COPD.
5.2 Deterioration of Disease and Acute Episodes
TRELEGY ELLIPTA should not be initiated in patients during rapidly deteriorating or potentially life-threatening episodes of COPD. TRELEGY ELLIPTA has not been studied in subjects with acutely deteriorating COPD. The initiation of TRELEGY ELLIPTA in this setting is not appropriate.
TRELEGY ELLIPTA should not be used for the relief of acute symptoms, i.e., as rescue therapy for the treatment of acute episodes of bronchospasm. TRELEGY ELLIPTA has not been studied in the relief of acute symptoms and extra doses should not be used for that purpose. Acute symptoms should be treated with an inhaled, short-acting beta2-agonist.
When beginning treatment with TRELEGY ELLIPTA, patients who have been taking oral or inhaled, short-acting beta2-agonists on a regular basis (e.g., 4 times a day) should be instructed to discontinue the regular use of these drugs and to use them only for symptomatic relief of acute respiratory symptoms.
COPD may deteriorate acutely over a period of hours or chronically over several days or longer. If TRELEGY ELLIPTA no longer controls symptoms of bronchoconstriction; the patient’s inhaled, short-acting beta2-agonist becomes less effective; or the patient needs more short-acting beta2-agonist than usual, these may be markers of deterioration of disease. In this setting a reevaluation of the patient and the COPD treatment regimen should be undertaken at once. Increasing the daily dose of TRELEGY ELLIPTA beyond the recommended dose is not appropriate in this situation.
5.3 Excessive Use of TRELEGY ELLIPTA and Use with Other Long-acting Beta2-agonists
TRELEGY ELLIPTA should not be used more often than recommended, at higher doses than recommended, or in conjunction with other medicines containing LABA, as an overdose may result. Clinically significant cardiovascular effects and fatalities have been reported in association with excessive use of inhaled sympathomimetic drugs. Patients using TRELEGY ELLIPTA should not use another medicine containing a LABA (e.g., salmeterol, formoterol fumarate, arformoterol tartrate, indacaterol) for any reason.
5.4 Local Effects of Inhaled Corticosteroids
TRELEGY ELLIPTA contains fluticasone furoate, an ICS. Localized infections of the mouth and pharynx with Candida albicans have occurred in subjects treated with orally inhaled drug products containing fluticasone furoate. When such an infection develops, it should be treated with appropriate local or systemic (i.e., oral) antifungal therapy while treatment with TRELEGY ELLIPTA continues, but at times therapy with TRELEGY ELLIPTA may need to be interrupted. Advise the patient to rinse his/her mouth with water without swallowing following inhalation to help reduce the risk of oropharyngeal candidiasis.
5.5 Pneumonia
Physicians should remain vigilant for the possible development of pneumonia in patients with COPD as clinical features of pneumonia and exacerbations frequently overlap. Lower respiratory tract infections, including pneumonia, have been reported following the inhaled administration of corticosteroids.
In two 12-week trials of subjects with COPD (N = 824), the incidence of pneumonia was <1% for both treatment arms: umeclidinium 62.5 mcg + fluticasone furoate/vilanterol 100 mcg/25 mcg or placebo + fluticasone furoate/vilanterol 100 mcg/25 mcg. Fatal pneumonia occurred in 1 subject receiving placebo + fluticasone furoate/vilanterol 100 mcg/25 mcg.
In a 52-week trial of subjects with COPD (N = 10,355), the incidence of pneumonia was 8% for TRELEGY ELLIPTA (n = 4,151), 7% for fluticasone furoate/vilanterol 100 mcg/25 mcg (n = 4,134), and 5% for umeclidinium/vilanterol 62.5 mcg/25 mcg (n = 2,070). Fatal pneumonia occurred in 12 of 4,151 patients (0.35 per 100 patient-years) receiving TRELEGY ELLIPTA, 5 of 4,134 patients (0.17 per 100 patient-years) receiving fluticasone furoate/vilanterol, and 5 of 2,070 patients (0.29 per 100 patient-years) receiving umeclidinium/vilanterol.
In a mortality trial with fluticasone furoate/vilanterol with a median treatment duration of 1.5 years in 16,568 subjects with moderate COPD and cardiovascular disease, the annualized incidence rate of pneumonia was 3.4 per 100 patient-years for fluticasone furoate/vilanterol 100 mcg/25 mcg, 3.2 for placebo, 3.3 for fluticasone furoate 100 mcg, and 2.3 for vilanterol 25 mcg. Adjudicated, on‑treatment deaths due to pneumonia occurred in 13 subjects receiving fluticasone furoate/vilanterol 100 mcg/25 mcg, 9 subjects receiving placebo, 10 subjects receiving fluticasone furoate 100 mcg, and 6 subjects receiving vilanterol 25 mcg (<0.2 per 100 patient-years for each treatment group).
5.6 Immunosuppression
Persons who are using drugs that suppress the immune system are more susceptible to infections than healthy individuals. Chickenpox and measles, for example, can have a more serious or even fatal course in susceptible children or adults using corticosteroids. In such children or adults who have not had these diseases or been properly immunized, particular care should be taken to avoid exposure. How the dose, route, and duration of corticosteroid administration affect the risk of developing a disseminated infection is not known. The contribution of the underlying disease and/or prior corticosteroid treatment to the risk is also not known. If a patient is exposed to chickenpox, prophylaxis with varicella zoster immune globulin (VZIG) may be indicated. If a patient is exposed to measles, prophylaxis with pooled intramuscular immunoglobulin (IG) may be indicated. (See the respective package inserts for complete VZIG and IG prescribing information.) If chickenpox develops, treatment with antiviral agents may be considered.
ICS should be used with caution, if at all, in patients with active or quiescent tuberculosis infections of the respiratory tract; systemic fungal, bacterial, viral, or parasitic infections; or ocular herpes simplex.
5.7 Transferring Patients from Systemic Corticosteroid Therapy
Particular care is needed for patients who have been transferred from systemically active corticosteroids to ICS because deaths due to adrenal insufficiency have occurred in patients with asthma during and after transfer from systemic corticosteroids to less systemically available ICS. After withdrawal from systemic corticosteroids, a number of months are required for recovery of hypothalamic-pituitary-adrenal (HPA) function.
Patients who have been previously maintained on 20 mg or more of prednisone (or its equivalent) may be most susceptible, particularly when their systemic corticosteroids have been almost completely withdrawn. During this period of HPA suppression, patients may exhibit signs and symptoms of adrenal insufficiency when exposed to trauma, surgery, or infection (particularly gastroenteritis) or other conditions associated with severe electrolyte loss. Although TRELEGY ELLIPTA may control COPD symptoms during these episodes, in recommended doses it supplies less than normal physiological amounts of glucocorticoid systemically and does NOT provide the mineralocorticoid activity that is necessary for coping with these emergencies.
During periods of stress or a severe COPD exacerbation, patients who have been withdrawn from systemic corticosteroids should be instructed to resume oral corticosteroids (in large doses) immediately and to contact their physicians for further instruction. These patients should also be instructed to carry a warning card indicating that they may need supplementary systemic corticosteroids during periods of stress or a severe COPD exacerbation.
Patients requiring oral corticosteroids should be weaned slowly from systemic corticosteroid use after transferring to TRELEGY ELLIPTA. Prednisone reduction can be accomplished by reducing the daily prednisone dose by 2.5 mg on a weekly basis during therapy with TRELEGY ELLIPTA. Lung function (forced expiratory volume in 1 second [FEV1]), beta-agonist use, and COPD symptoms should be carefully monitored during withdrawal of oral corticosteroids. In addition, patients should be observed for signs and symptoms of adrenal insufficiency, such as fatigue, lassitude, weakness, nausea and vomiting, and hypotension.
Transfer of patients from systemic corticosteroid therapy to TRELEGY ELLIPTA may unmask allergic conditions previously suppressed by the systemic corticosteroid therapy (e.g., rhinitis, conjunctivitis, eczema, arthritis, eosinophilic conditions).
During withdrawal from oral corticosteroids, some patients may experience symptoms of systemically active corticosteroid withdrawal (e.g., joint and/or muscular pain, lassitude, depression) despite maintenance or even improvement of respiratory function.
5.8 Hypercorticism and Adrenal Suppression
Inhaled fluticasone furoate is absorbed into the circulation and can be systemically active. Effects of fluticasone furoate on the HPA axis are not observed with the therapeutic doses of fluticasone furoate in TRELEGY ELLIPTA. However, exceeding the recommended dosage or coadministration with a strong cytochrome P450 3A4 (CYP3A4) inhibitor may result in HPA dysfunction [see Warnings and Precautions (5.9), Drug Interactions (7.1)].
Because of the possibility of significant systemic absorption of ICS in sensitive patients, patients treated with TRELEGY ELLIPTA should be observed carefully for any evidence of systemic corticosteroid effects. Particular care should be taken in observing patients postoperatively or during periods of stress for evidence of inadequate adrenal response.
It is possible that systemic corticosteroid effects such as hypercorticism and adrenal suppression (including adrenal crisis) may appear in a small number of patients who are sensitive to these effects. If such effects occur, appropriate therapy should be considered.
5.9 Drug Interactions with Strong Cytochrome P450 3A4 Inhibitors
Caution should be exercised when considering the coadministration of TRELEGY ELLIPTA with ketoconazole and other known strong CYP3A4 inhibitors (e.g., ritonavir, clarithromycin, conivaptan, indinavir, itraconazole, lopinavir, nefazodone, nelfinavir, saquinavir, telithromycin, troleandomycin, voriconazole) because increased systemic corticosteroid and increased cardiovascular adverse effects may occur [see Drug Interactions (7.1), Clinical Pharmacology (12.3)].
5.10 Paradoxical Bronchospasm
As with other inhaled medicines, TRELEGY ELLIPTA can produce paradoxical bronchospasm, which may be life threatening. If paradoxical bronchospasm occurs following dosing with TRELEGY ELLIPTA, it should be treated immediately with an inhaled, short-acting bronchodilator; TRELEGY ELLIPTA should be discontinued immediately; and alternative therapy should be instituted.
5.11 Hypersensitivity Reactions, including Anaphylaxis
Hypersensitivity reactions such as anaphylaxis, angioedema, rash, and urticaria may occur after administration of TRELEGY ELLIPTA. Discontinue TRELEGY ELLIPTA if such reactions occur. There have been reports of anaphylactic reactions in patients with severe milk protein allergy after inhalation of other powder medications containing lactose; therefore, patients with severe milk protein allergy should not use TRELEGY ELLIPTA [see Contraindications (4)].
5.12 Cardiovascular Effects
Vilanterol, like other beta2-agonists, can produce a clinically significant cardiovascular effect in some patients as measured by increases in pulse rate, systolic or diastolic blood pressure, and also cardiac arrhythmias, such as supraventricular tachycardia and extrasystoles. If such effects occur, TRELEGY ELLIPTA may need to be discontinued. In addition, beta-agonists have been reported to produce electrocardiographic changes, such as flattening of the T wave, prolongation of the QTc interval, and ST segment depression, although the clinical significance of these findings is unknown [see Clinical Pharmacology (12.2)]. Fatalities have been reported in association with excessive use of inhaled sympathomimetic drugs.
TRELEGY ELLIPTA, like other sympathomimetic amines, should be used with caution in patients with cardiovascular disorders, especially coronary insufficiency, cardiac arrhythmias, and hypertension.
In a 52-week trial of subjects with COPD, the exposure-adjusted rates for any on-treatment major adverse cardiac event, including non-fatal central nervous system hemorrhages and cerebrovascular conditions, non-fatal myocardial infarction (MI), non-fatal acute MI, and adjudicated on-treatment death due to cardiovascular events, was 2.2 per 100 patient-years for TRELEGY ELLIPTA (n = 4,151), 1.9 per 100 patient-years for fluticasone furoate/vilanterol 100 mcg/25 mcg (n = 4,134), and 2.2 per 100 patient-years for umeclidinium/vilanterol 62.5 mcg/25 mcg (n = 2,070). Adjudicated on-treatment deaths due to cardiovascular events occurred in 20 of 4,151 patients (0.54 per 100 patient-years) receiving TRELEGY ELLIPTA, 27 of 4,134 patients (0.78 per 100 patient-years) receiving fluticasone furoate/vilanterol, and 16 of 2,070 patients (0.94 per 100 patient-years) receiving umeclidinium/vilanterol.
In a mortality trial with fluticasone furoate/vilanterol with a median treatment duration of 1.5 years in 16,568 subjects with moderate COPD and cardiovascular disease, the annualized incidence rate of adjudicated cardiovascular events (composite of myocardial infarction, stroke, unstable angina, transient ischemic attack, or on-treatment death due to cardiovascular events) was 2.5 per 100 patient-years for fluticasone furoate/vilanterol 100 mcg/25 mcg, 2.7 for placebo, 2.4 for fluticasone furoate 100 mcg, and 2.6 for vilanterol 25 mcg. Adjudicated, on-treatment deaths due to cardiovascular events occurred in 82 subjects receiving fluticasone furoate/vilanterol 100 mcg/25 mcg, 86 subjects receiving placebo, 80 subjects receiving fluticasone furoate 100 mcg, and 90 subjects receiving vilanterol 25 mcg (annualized incidence rate ranged from 1.2 to 1.3 per 100 patient-years for the treatment groups).
5.13 Reduction in Bone Mineral Density
Decreases in bone mineral density (BMD) have been observed with long-term administration of products containing ICS. The clinical significance of small changes in BMD with regard to long‑term consequences such as fracture is unknown. Patients with major risk factors for decreased bone mineral content, such as prolonged immobilization, family history of osteoporosis, postmenopausal status, tobacco use, advanced age, poor nutrition, or chronic use of drugs that can reduce bone mass (e.g., anticonvulsants, oral corticosteroids) should be monitored and treated with established standards of care. Since patients with COPD often have multiple risk factors for reduced BMD, assessment of BMD is recommended prior to initiating TRELEGY ELLIPTA and periodically thereafter. If significant reductions in BMD are seen and TRELEGY ELLIPTA is still considered medically important for that patient’s COPD therapy, use of medicine to treat or prevent osteoporosis should be strongly considered.
5.14 Glaucoma and Cataracts, Worsening of Narrow-Angle Glaucoma
Glaucoma, increased intraocular pressure, and cataracts have been reported in patients with COPD following the long-term administration of ICS or with use of inhaled anticholinergics. TRELEGY ELLIPTA should be used with caution in patients with narrow-angle glaucoma. Prescribers and patients should also be alert for signs and symptoms of acute narrow-angle glaucoma (e.g., eye pain or discomfort, blurred vision, visual halos or colored images in association with red eyes from conjunctival congestion and corneal edema). Instruct patients to consult a healthcare provider immediately if any of these signs or symptoms develop. Consider referral to an ophthalmologist in patients who develop ocular symptoms or use TRELEGY ELLIPTA long term.
5.15 Worsening of Urinary Retention
TRELEGY ELLIPTA, like all medicines containing an anticholinergic, should be used with caution in patients with urinary retention. Prescribers and patients should be alert for signs and symptoms of urinary retention (e.g., difficulty passing urine, painful urination), especially in patients with prostatic hyperplasia or bladder-neck obstruction. Instruct patients to consult a healthcare provider immediately if any of these signs or symptoms develop.
5.16 Coexisting Conditions
TRELEGY ELLIPTA, like all medicines containing sympathomimetic amines, should be used with caution in patients with convulsive disorders or thyrotoxicosis and in those who are unusually responsive to sympathomimetic amines. Doses of the related beta2-adrenoceptor agonist albuterol, when administered intravenously, have been reported to aggravate preexisting diabetes mellitus and ketoacidosis.
5.17 Hypokalemia and Hyperglycemia
Beta-adrenergic agonist medicines may produce significant hypokalemia in some patients, possibly through intracellular shunting, which has the potential to produce adverse cardiovascular effects. The decrease in serum potassium is usually transient, not requiring supplementation. Beta-agonist medications may produce transient hyperglycemia in some patients.
-
6 ADVERSE REACTIONS
The following adverse reactions are described in greater detail in other sections:
- Serious asthma-related events – hospitalizations, intubations, death [see Warnings and Precautions (5.1)]
- Candida albicans infection [see Warnings and Precautions (5.4)]
- Increased risk of pneumonia in COPD [see Warnings and Precautions (5.5)]
- Immunosuppression [see Warnings and Precautions (5.6)]
- Hypercorticism and adrenal suppression [see Warnings and Precautions (5.8)]
- Paradoxical bronchospasm [see Warnings and Precautions (5.10)]
- Cardiovascular effects [see Warnings and Precautions (5.12)]
- Reduction in bone mineral density [see Warnings and Precautions (5.13)]
- Worsening of narrow-angle glaucoma [see Warnings and Precautions (5.14)]
- Worsening of urinary retention [see Warnings and Precautions (5.15)]
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared with rates in the clinical trials of another drug and may not reflect the rates observed in practice.
The safety of TRELEGY ELLIPTA is based on the safety data from two 12-week treatment trials with coadministration of umeclidinium and the fixed-dose combination of fluticasone furoate/vilanterol and a 52-week long-term trial of TRELEGY ELLIPTA compared with the fixed-dose combinations of fluticasone furoate/vilanterol and umeclidinium/vilanterol [see Clinical Studies (14)].
Trials 1 and 2
Two 12-week treatment trials (Trial 1 and Trial 2) evaluated the coadministration of umeclidinium + fluticasone furoate/vilanterol, the components of TRELEGY ELLIPTA, compared with placebo + fluticasone furoate/vilanterol. A total of 824 subjects with COPD across two 12-week, randomized, double-blind clinical trials received at least 1 dose of umeclidinium 62.5 mcg + fluticasone furoate/vilanterol 100 mcg/25 mcg or placebo + fluticasone furoate/vilanterol 100 mcg/25 mcg administered once daily (mean age: 64 years, 92% white, 66% male across all treatments) [see Clinical Studies (14)]. The incidence of adverse reactions associated with the use of umeclidinium 62.5 mcg + fluticasone furoate/vilanterol 100 mcg/25 mcg presented in Table 1 is based on the two 12-week trials.
Table 1. Adverse Reactions with Umeclidinium + Fluticasone Furoate/Vilanterol with ≥1% Incidence and More Common than Placebo + Fluticasone Furoate/Vilanterol (Trials 1 and 2) Adverse Reaction
Umeclidinium +
Fluticasone Furoate/
Vilanterol(n = 412)
%
Placebo +
Fluticasone Furoate/
Vilanterol(n = 412)
%
Nervous system disorders
Headache
4
3
Dysgeusia
2
<1
Musculoskeletal and connective tissue disorders
Back pain
4
2
Respiratory, thoracic, and mediastinal disorders
Cough
1
<1
Oropharyngeal pain
1
0
Gastrointestinal disorders
Diarrhea
2
<1
Infections and infestations
Gastroenteritis
1
0
Trial 3 - Long-term Safety Data
A 52-week trial (Trial 3) evaluated the long-term safety of TRELEGY ELLIPTA compared with the fixed-dose combinations of fluticasone furoate/vilanterol 100 mcg/25 mcg and umeclidinium/vilanterol 62.5 mcg/25 mcg. A total of 10,355 subjects with COPD with a history of moderate or severe exacerbations within the prior 12 months were randomized (2:2:1) to receive TRELEGY ELLIPTA, fluticasone furoate/vilanterol, or umeclidinium/vilanterol administered once daily in a double-blind clinical trial (mean age: 65 years, 77% white, 66% male across all treatments) [see Clinical Studies (14)].
The incidence of adverse reactions in the long-term trial were consistent with those in Trials 1 and 2. However, in addition to the adverse reactions shown in Table 1, adverse reactions occurring in ≥1% of the subjects treated with TRELEGY ELLIPTA (n = 4,151) for up to 52 weeks also included upper respiratory tract infection, pneumonia [see Warnings and Precautions (5.5)], bronchitis, oral candidiasis [see Warnings and Precautions (5.4)], arthralgia, influenza, sinusitis, pharyngitis, rhinitis, constipation, urinary tract infection, and dysphonia.
-
7 DRUG INTERACTIONS
7.1 Inhibitors of Cytochrome P450 3A4
Fluticasone furoate and vilanterol are substrates of CYP3A4. Concomitant administration of the strong CYP3A4 inhibitor ketoconazole increases the systemic exposure to fluticasone furoate and vilanterol. Caution should be exercised when considering the coadministration of TRELEGY ELLIPTA with ketoconazole and other known strong CYP3A4 inhibitors (e.g., ritonavir, clarithromycin, conivaptan, indinavir, itraconazole, lopinavir, nefazodone, nelfinavir, saquinavir, telithromycin, troleandomycin, voriconazole) [see Warnings and Precautions (5.9), Clinical Pharmacology (12.3)].
7.2 Monoamine Oxidase Inhibitors and Tricyclic Antidepressants
Vilanterol, like other beta2-agonists, should be administered with extreme caution to patients being treated with monoamine oxidase inhibitors, tricyclic antidepressants, or drugs known to prolong the QTc interval or within 2 weeks of discontinuation of such agents, because the effect of adrenergic agonists on the cardiovascular system may be potentiated by these agents. Drugs that are known to prolong the QTc interval have an increased risk of ventricular arrhythmias.
7.3 Beta-adrenergic Receptor Blocking Agents
Beta-blockers not only block the pulmonary effect of beta-agonists, such as vilanterol, but may also produce severe bronchospasm in patients with COPD. Therefore, patients with COPD should not normally be treated with beta-blockers. However, under certain circumstances, there may be no acceptable alternatives to the use of beta-adrenergic blocking agents for these patients; cardioselective beta-blockers could be considered, although they should be administered with caution.
7.4 Non–Potassium-Sparing Diuretics
The electrocardiographic changes and/or hypokalemia that may result from the administration of non–potassium-sparing diuretics (such as loop or thiazide diuretics) can be acutely worsened by beta-agonists, especially when the recommended dose of the beta-agonist is exceeded. Although the clinical significance of these effects is not known, caution is advised in the coadministration of beta-agonists with non–potassium-sparing diuretics.
7.5 Anticholinergics
There is potential for an additive interaction with concomitantly used anticholinergic medicines. Therefore, avoid coadministration of TRELEGY ELLIPTA with other anticholinergic-containing drugs as this may lead to an increase in anticholinergic adverse effects [see Warnings and Precautions (5.14, 5.15)].
-
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Risk Summary
There are insufficient data on the use of TRELEGY ELLIPTA or its individual components, fluticasone furoate, umeclidinium, and vilanterol, in pregnant women to inform a drug‑associated risk. (See Clinical Considerations.) In an animal reproduction study, fluticasone furoate and vilanterol administered by inhalation alone or in combination to pregnant rats during the period of organogenesis produced no fetal structural abnormalities. The highest fluticasone furoate and vilanterol doses in this study were approximately 9 and 40 times the maximum recommended human daily inhalation doses (MRHDID) of 100 and 25 mcg in adults, respectively. (See Data.) Umeclidinium administered via inhalation or subcutaneously to pregnant rats and rabbits was not associated with adverse effect on embryofetal development at exposures approximately 40 and 150 times, respectively, the human exposure at the MRHDID.
The estimated risk of major birth defects and miscarriage for the indicated populations is unknown. In the U.S. general population, the estimated risk of major birth defects and miscarriage in clinically recognized pregnancies is 2% to 4% and 15% to 20%, respectively.
Clinical Considerations
Labor and Delivery: TRELEGY ELLIPTA should be used during late gestation and labor only if the potential benefit justifies the potential for risks related to beta-agonists interfering with uterine contractility.
Data
Animal Data: The combination of fluticasone furoate, umeclidinium, and vilanterol has not been studied in pregnant animals. Studies in pregnant animals have been conducted with fluticasone furoate and vilanterol in combination and individually with fluticasone furoate, umeclidinium, or vilanterol.
Fluticasone Furoate and Vilanterol: In an embryofetal developmental study, pregnant rats received fluticasone furoate and vilanterol during the period of organogenesis at doses up to approximately 9 and 40 times the MRHDID, respectively, alone or in combination (on a mcg/m2 basis at inhalation doses up to approximately 95 mcg/kg/day). No evidence of structural abnormalities was observed.
Fluticasone Furoate: In 2 separate embryofetal developmental studies, pregnant rats and rabbits received fluticasone furoate during the period of organogenesis at doses up to approximately 9 and 2 times the MRHDID, respectively (on a mcg/m2 basis at maternal inhalation doses up to 91 and 8 mcg/kg/day). No evidence of structural abnormalities in fetuses was observed in either species. In a perinatal and postnatal developmental study in rats, dams received fluticasone furoate during late gestation and lactation periods at doses up to approximately 3 times the MRHDID (on a mcg/m2 basis at maternal inhalation doses up to 27 mcg/kg/day). No evidence of effects on offspring development was observed.
Umeclidinium: In 2 separate embryofetal developmental studies, pregnant rats and rabbits received umeclidinium during the period of organogenesis at doses up to approximately 40 and 150 times the MRHDID, respectively (on an AUC basis at maternal inhalation doses up to 278 mcg/kg/day in rats and at maternal subcutaneous doses up to 180 mcg/kg/day in rabbits). No evidence of teratogenic effects was observed in either species. In a perinatal and postnatal developmental study in rats, dams received umeclidinium during late gestation and lactation periods at doses up to approximately 20 times the MRHDID (on an AUC basis at maternal subcutaneous doses up to 60 mcg/kg/day). No evidence of effects on offspring development was observed.
Vilanterol: In 2 separate embryofetal developmental studies, pregnant rats and rabbits received vilanterol during the period of organogenesis at doses up to approximately 13,000 and 760 times, respectively, the MRHDID (on a mcg/m2 basis at maternal inhalation doses up to 33,700 mcg/kg/day in rats and on an AUC basis at maternal inhaled doses up to 5,740 mcg/kg/day in rabbits). No evidence of structural abnormalities was observed at any dose in rats or in rabbits up to approximately 120 times the MRHDID (on an AUC basis at maternal doses up to 591 mcg/kg/day). However, fetal skeletal variations were observed in rabbits at approximately 760 or 840 times the MRHDID (on an AUC basis at maternal inhaled or subcutaneous doses of 5,740 or 300 mcg/kg/day, respectively). The skeletal variations included decreased or absent ossification in cervical vertebral centrum and metacarpals. In a perinatal and postnatal developmental study in rats, dams received vilanterol during late gestation and the lactation periods at doses up to approximately 3,900 times the MRHDID (on a mcg/m2 basis at maternal oral doses up to 10,000 mcg/kg/day). No evidence of effects in offspring development was observed.
8.2 Lactation
Risk Summary
There is no information available on the presence of fluticasone furoate, umeclidinium, or vilanterol in human milk; the effects on the breastfed child; or the effects on milk production. Umeclidinium is present in rat milk (see Data). The developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for TRELEGY ELLIPTA and any potential adverse effects on the breastfed child from fluticasone furoate, umeclidinium, or vilanterol or from the underlying maternal condition.
Data
Animal Data: Subcutaneous administration of umeclidinium to lactating rats at approximately 20 times the MRHDID resulted in a quantifiable level of umeclidinium in 2 of 54 pups, which may indicate transfer of umeclidinium in rat milk.
8.4 Pediatric Use
TRELEGY ELLIPTA is not indicated for use in children. The safety and efficacy in pediatric patients have not been established.
8.5 Geriatric Use
Based on available data, no adjustment of the dosage of TRELEGY ELLIPTA in geriatric patients is necessary, but greater sensitivity in some older individuals cannot be ruled out.
In Trials 1 and 2 (coadministration trials), 189 subjects aged 65 years and older, of which 39 subjects were aged 75 years and older, were administered umeclidinium 62.5 mcg + fluticasone furoate/vilanterol 100 mcg/25 mcg. In Trial 3, 2,265 subjects aged 65 years and older, of which 565 subjects were aged 75 years and older, were administered TRELEGY ELLIPTA. No overall differences in safety or effectiveness were observed between these subjects and younger subjects, and other reported clinical experience has not identified differences in responses between the elderly and younger subjects.
8.6 Hepatic Impairment
TRELEGY ELLIPTA has not been studied in subjects with hepatic impairment. Information on the individual components is provided below.
Fluticasone Furoate/Vilanterol
Fluticasone furoate systemic exposure increased by up to 3-fold in subjects with hepatic impairment compared with healthy subjects. Hepatic impairment had no effect on vilanterol systemic exposure. Monitor patients for corticosteroid-related side effects [see Clinical Pharmacology (12.3)].
Umeclidinium
Patients with moderate hepatic impairment (Child-Pugh score of 7-9) showed no relevant increases in Cmax or AUC, nor did protein binding differ between subjects with moderate hepatic impairment and their healthy controls. Studies in subjects with severe hepatic impairment have not been performed [see Clinical Pharmacology (12.3)].
8.7 Renal Impairment
TRELEGY ELLIPTA has not been studied in subjects with renal impairment. Information on the individual components is provided below.
Fluticasone Furoate/Vilanterol
There were no significant increases in either fluticasone furoate or vilanterol exposure in subjects with severe renal impairment (CrCl <30 mL/min) compared with healthy subjects. No dosage adjustment is required in patients with renal impairment [see Clinical Pharmacology (12.3)].
Umeclidinium
Patients with severe renal impairment (CrCl <30 mL/min) showed no relevant increases in Cmax or AUC, nor did protein binding differ between subjects with severe renal impairment and their healthy controls. No dosage adjustment is required in patients with renal impairment [see Clinical Pharmacology (12.3)].
-
10 OVERDOSAGE
No human overdosage data has been reported for TRELEGY ELLIPTA.
TRELEGY ELLIPTA contains fluticasone furoate, umeclidinium, and vilanterol; therefore, the risks associated with overdosage for the individual components described below apply to TRELEGY ELLIPTA. Treatment of overdosage consists of discontinuation of TRELEGY ELLIPTA together with institution of appropriate symptomatic and/or supportive therapy. The judicious use of a cardioselective beta-receptor blocker may be considered, bearing in mind that such medicine can produce bronchospasm. Cardiac monitoring is recommended in cases of overdosage.
10.1 Fluticasone Furoate
Because of low systemic bioavailability (15.2%) and an absence of acute drug-related systemic findings in clinical trials, overdosage of fluticasone furoate is unlikely to require any treatment other than observation. If used at excessive doses for prolonged periods, systemic effects such as hypercorticism may occur [see Warnings and Precautions (5.8)].
Single- and repeat-dose trials of fluticasone furoate at doses of 50 to 4,000 mcg have been studied in human subjects. Decreases in mean serum cortisol were observed at dosages of 500 mcg or higher given once daily for 14 days.
10.2 Umeclidinium
High doses of umeclidinium may lead to anticholinergic signs and symptoms. However, there were no systemic anticholinergic adverse effects following a once-daily inhaled dose of up to 1,000 mcg of umeclidinium (16 times the maximum recommended daily dose) for 14 days in subjects with COPD.
10.3 Vilanterol
The expected signs and symptoms with overdosage of vilanterol are those of excessive beta‑adrenergic stimulation and/or occurrence or exaggeration of any of the signs and symptoms of beta-adrenergic stimulation (e.g., seizures, angina, hypertension or hypotension, tachycardia with rates up to 200 beats/min, arrhythmias, nervousness, headache, tremor, muscle cramps, dry mouth, palpitation, nausea, dizziness, fatigue, malaise, insomnia, hyperglycemia, hypokalemia, metabolic acidosis). As with all inhaled sympathomimetic medicines, cardiac arrest and even death may be associated with an overdose of vilanterol.
-
11 DESCRIPTION
TRELEGY ELLIPTA is an inhalation powder drug product for delivery of a combination of fluticasone furoate (an ICS), umeclidinium (an anticholinergic), and vilanterol (a LABA) to patients by oral inhalation.
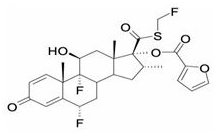
Fluticasone furoate, a synthetic trifluorinated corticosteroid, has the chemical name (6α,11β,16α,17α)-6,9-difluoro-17-{[(fluoro-methyl)thio]carbonyl}-11-hydroxy-16-methyl-3-oxoandrosta-1,4-dien-17-yl 2-furancarboxylate and the following chemical structure:
Fluticasone furoate is a white powder with a molecular weight of 538.6, and the empirical formula is C27H29F3O6S. It is practically insoluble in water.
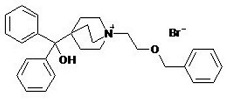
Umeclidinium bromide has the chemical name 1-[2-(benzyloxy)ethyl]-4-(hydroxydiphenylmethyl)-1-azoniabicyclo[2.2.2]octane bromide and the following chemical structure:
Umeclidinium bromide is a white powder with a molecular weight of 508.5, and the empirical formula is C29H34NO2Br (as a quaternary ammonium bromide compound). It is slightly soluble in water.
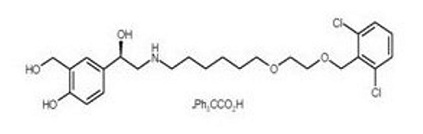
Vilanterol trifenatate has the chemical name triphenylacetic acid-4-{(1R)-2-[(6-{2-[2,6-dicholorobenzyl)oxy]ethoxy}hexyl)amino]-1-hydroxyethyl}-2-(hydroxymethyl)phenol (1:1) and the following chemical structure:
Vilanterol trifenatate is a white powder with a molecular weight of 774.8, and the empirical formula is C24H33Cl2NO5C20H16O2. It is practically insoluble in water.
TRELEGY ELLIPTA is a light grey and beige plastic inhaler containing 2 foil blister strips. Each blister on one strip contains a white powder mix of micronized fluticasone furoate (100 mcg) and lactose monohydrate (12.3 mg) and each blister on the other strip contains a white powder blend of micronized umeclidinium bromide (74.2 mcg equivalent to 62.5 mcg of umeclidinium), micronized vilanterol trifenatate (40 mcg equivalent to 25 mcg of vilanterol), magnesium stearate (75 mcg), and lactose monohydrate (12.3 mg). The lactose monohydrate contains milk proteins. After the inhaler is activated, the powder within both blisters is exposed and ready for dispersion into the airstream created by the patient inhaling through the mouthpiece.
Comparative in vitro data for drug delivery and aerodynamic particle size distribution of the delivered drugs fluticasone furoate, umeclidinium, and vilanterol demonstrated that there were no pharmaceutical interactions and each drug was delivered in a comparable manner whether administered via a single ELLIPTA inhaler or from separate inhalers.
Under standardized in vitro test conditions, TRELEGY ELLIPTA delivers 92, 55, and 22 mcg of fluticasone furoate, umeclidinium, and vilanterol, respectively, per dose when tested at a flow rate of 60 L/min for 4 seconds.
In adult subjects with very severe COPD (FEV1/FVC [forced vital capacity] <70% and FEV1 <30% predicted), mean peak inspiratory flow through the ELLIPTA inhaler was 65.8 L/min (range: 43.5 to 94.1 L/min). The actual amount of drug delivered to the lung will depend on patient factors, such as inspiratory flow profile.
-
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
TRELEGY ELLIPTA
TRELEGY ELLIPTA contains fluticasone furoate, umeclidinium, and vilanterol. The mechanisms of action described below for the individual components apply to TRELEGY ELLIPTA. These drugs represent 3 different classes of medications (an ICS, an anticholinergic, and a LABA), each having different effects on clinical and physiological indices.
Fluticasone Furoate
Fluticasone furoate is a synthetic trifluorinated corticosteroid with anti-inflammatory activity. Fluticasone furoate has been shown in vitro to exhibit a binding affinity for the human glucocorticoid receptor that is approximately 29.9 times that of dexamethasone and 1.7 times that of fluticasone propionate. The clinical relevance of these findings is unknown.
The precise mechanism through which fluticasone furoate affects COPD symptoms is not known. Inflammation is an important component in the pathogenesis of COPD. Corticosteroids have been shown to have a wide range of actions on multiple cell types (e.g., mast cells, eosinophils, neutrophils, macrophages, lymphocytes) and mediators (e.g., histamine, eicosanoids, leukotrienes, cytokines) involved in inflammation. Specific effects of fluticasone furoate demonstrated in in vitro and in vivo models included activation of the glucocorticoid response element, inhibition of pro-inflammatory transcription factors such as NFkB, and inhibition of antigen-induced lung eosinophilia in sensitized rats. These anti-inflammatory actions of corticosteroids may contribute to their efficacy.
Umeclidinium
Umeclidinium is a long-acting muscarinic antagonist, which is often referred to as an anticholinergic. It has similar affinity to the subtypes of muscarinic receptors M1 to M5. In the airways, it exhibits pharmacological effects through inhibition of M3 receptor at the smooth muscle leading to bronchodilation. The competitive and reversible nature of antagonism was shown with human and animal origin receptors and isolated organ preparations. In preclinical in vitro as well as in vivo studies, prevention of methacholine- and acetylcholine-induced bronchoconstrictive effects was dose-dependent and lasted longer than 24 hours. The clinical relevance of these findings is unknown. The bronchodilation following inhalation of umeclidinium is predominantly a site-specific effect.
Vilanterol
Vilanterol is a LABA. In vitro tests have shown the functional selectivity of vilanterol was similar to salmeterol. The clinical relevance of this in vitro finding is unknown.
Although beta2-receptors are the predominant adrenergic receptors in bronchial smooth muscle and beta1-receptors are the predominant receptors in the heart, there are also beta2-receptors in the human heart comprising 10% to 50% of the total beta-adrenergic receptors. The precise function of these receptors has not been established, but they raise the possibility that even highly selective beta2-agonists may have cardiac effects.
The pharmacologic effects of beta2-adrenergic agonist drugs, including vilanterol, are at least in part attributable to stimulation of intracellular adenyl cyclase, the enzyme that catalyzes the conversion of adenosine triphosphate (ATP) to cyclic-3ʹ,5ʹ-adenosine monophosphate (cyclic AMP). Increased cyclic AMP levels cause relaxation of bronchial smooth muscle and inhibition of release of mediators of immediate hypersensitivity from cells, especially from mast cells.
12.2 Pharmacodynamics
Cardiovascular Effects
The effect of umeclidinium/vilanterol on cardiac rhythm in subjects diagnosed with COPD was assessed using 24-hour Holter monitoring in 6- and 12-month trials: 53 subjects received umeclidinium/vilanterol 62.5 mcg/25 mcg, 281 subjects received umeclidinium/vilanterol 125 mcg/25 mcg, and 182 subjects received placebo. No clinically meaningful effects on cardiac rhythm were observed.
The cardiovascular effects from dual combinations of fluticasone furoate/vilanterol and umeclidinium/vilanterol in healthy subjects are presented below.
Fluticasone Furoate/Vilanterol Combination
Healthy Subjects: QTc interval prolongation was studied in a double-blind, multiple-dose, placebo- and positive-controlled crossover study in 85 healthy volunteers. The maximum mean (95% upper confidence bound) difference in QTcF from placebo after baseline correction was 4.9 (7.5) milliseconds and 9.6 (12.2) milliseconds seen 30 minutes after dosing for fluticasone furoate/vilanterol 200 mcg/25 mcg and fluticasone furoate/vilanterol 800 mcg/100 mcg, respectively.
A dose-dependent increase in heart rate was also observed. The maximum mean (95% upper confidence bound) difference in heart rate from placebo after baseline correction was 7.8 (9.4) beats/min and 17.1 (18.7) beats/min seen 10 minutes after dosing for fluticasone furoate/vilanterol 200 mcg/25 mcg and fluticasone furoate/vilanterol 800 mcg/100 mcg (8/4 times the recommended dosage), respectively.
Umeclidinium/Vilanterol Combination
Healthy Subjects: QTc interval prolongation was studied in a double-blind, multiple-dose, placebo- and positive-controlled crossover trial in 86 healthy subjects. The maximum mean (95% upper confidence bound) difference in QTcF from placebo after baseline correction was 4.6 (7.1) milliseconds and 8.2 (10.7) milliseconds for umeclidinium/vilanterol 125 mcg/25 mcg and umeclidinium/vilanterol 500 mcg/100 mcg (8/4 times the recommended dosage), respectively.
A dose-dependent increase in heart rate was also observed. The maximum mean (95% upper confidence bound) difference in heart rate from placebo after baseline correction was 8.8 (10.5) beats/min and 20.5 (22.3) beats/min seen 10 minutes after dosing for umeclidinium/vilanterol 125 mcg/25 mcg and umeclidinium/vilanterol 500 mcg/100 mcg, respectively.
HPA Axis Effects
Healthy Subjects: Inhaled fluticasone furoate at repeat doses up to 400 mcg was not associated with statistically significant decreases in serum or urinary cortisol in healthy subjects. Decreases in serum and urine cortisol levels were observed at fluticasone furoate exposures several-fold higher than exposures observed at the therapeutic dose.
Subjects with Chronic Obstructive Pulmonary Disease: In a trial with subjects with COPD, treatment with fluticasone furoate (50, 100, or 200 mcg)/vilanterol 25 mcg, vilanterol 25 mcg, or fluticasone furoate (100 or 200 mcg) for 6 months did not affect 24-hour urinary cortisol excretion. A separate trial with subjects with COPD demonstrated no effects on serum cortisol after 28 days of treatment with fluticasone furoate (50, 100, or 200 mcg)/vilanterol 25 mcg.
12.3 Pharmacokinetics
Linear pharmacokinetics was observed for fluticasone furoate (200 to 800 mcg), umeclidinium (62.5 to 500 mcg), and vilanterol (25 to 100 mcg). The pharmacokinetics of fluticasone furoate, umeclidinium, and vilanterol from TRELEGY ELLIPTA are comparable to the pharmacokinetics of fluticasone furoate, umeclidinium, and vilanterol when administered as fluticasone furoate/vilanterol or umeclidinium/vilanterol. Additionally, the systemic drug levels (steady-state Cmax and AUC) of fluticasone furoate, umeclidinium, and vilanterol following administration of TRELEGY ELLIPTA based on a combined pharmacokinetic dataset from 3 studies in subjects with COPD (N = 821) were within the range of those observed following administration of fluticasone furoate/vilanterol plus umeclidinium administered via 2 inhalers, fluticasone furoate/vilanterol and umeclidinium/vilanterol as the dual combinations, and after administration of fluticasone furoate, umeclidinium, and vilanterol as monotherapy. The pharmacokinetics of the individual components of TRELEGY ELLIPTA are presented below (Figures 1, 2, and 3). Plasma levels of fluticasone furoate, umeclidinium, and vilanterol may not predict therapeutic effect.
Absorption
Fluticasone Furoate: Following inhaled administration of fluticasone furoate, Cmax occurred within 0.5 to 1 hour. Absolute bioavailability of fluticasone furoate when administered by inhalation was 15.2%, primarily due to absorption of the inhaled portion of the dose delivered to the lung. Oral bioavailability from the swallowed portion of the dose is low (approximately 1.3%) due to extensive first-pass metabolism. Following repeat dosing of inhaled fluticasone furoate, steady state was achieved within 6 days with up to 2.6-fold accumulation.
Umeclidinium: Following inhaled administration of umeclidinium in healthy subjects, Cmax occurred at 5 to 15 minutes. Umeclidinium is mostly absorbed from the lung after inhaled doses with minimum contribution from oral absorption. Following repeat dosing of inhaled umeclidinium, steady state was achieved within 14 days with up to 1.8-fold accumulation.
Vilanterol: Following inhaled administration of vilanterol in healthy subjects, Cmax occurred at 5 to 15 minutes. Vilanterol is mostly absorbed from the lung after inhaled doses with negligible contribution from oral absorption. Following repeat dosing of inhaled vilanterol, steady state was achieved within 14 days with up to 1.7-fold accumulation.
Distribution
Fluticasone Furoate: Following intravenous administration to healthy subjects, the mean volume of distribution at steady state was 661 L. Binding of fluticasone furoate to human plasma proteins was high (>99%).
Umeclidinium: Following intravenous administration to healthy subjects, the mean volume of distribution was 86 L. In vitro plasma protein binding in human plasma was on average 89%.
Vilanterol: Following intravenous administration to healthy subjects, the mean volume of distribution at steady state was 165 L. In vitro plasma protein binding in human plasma was on average 94%.
Metabolism
Fluticasone Furoate: Fluticasone furoate is cleared from systemic circulation principally by hepatic metabolism via CYP3A4 to metabolites with significantly reduced corticosteroid activity. There was no in vivo evidence for cleavage of the furoate moiety resulting in the formation of fluticasone.
Umeclidinium: In vitro data showed that umeclidinium is primarily metabolized by the enzyme cytochrome P450 2D6 (CYP2D6) and is a substrate for the P-glycoprotein (P-gp) transporter. The primary metabolic routes for umeclidinium are oxidative (hydroxylation, O-dealkylation) followed by conjugation (e.g., glucuronidation), resulting in a range of metabolites with either reduced pharmacological activity or for which the pharmacological activity has not been established. Systemic exposure to the metabolites is low.
Vilanterol: In vitro data showed that vilanterol is metabolized principally by CYP3A4 and is a substrate for the P-gp transporter. Vilanterol is metabolized to a range of metabolites with significantly reduced β1- and β2-agonist activity.
Elimination
Fluticasone Furoate: The plasma elimination half-life following repeat-dose inhaled administration averaged 24 hours. Following intravenous dosing with radiolabeled fluticasone furoate, mass balance showed 90% of the radiolabel in the feces and 2% in the urine. Following oral dosing, radiolabel recovered in feces was 101% of the total dose and that in urine was approximately 1% of the total dose.
Umeclidinium: The effective half-life after once-daily oral dosing is 11 hours. Following intravenous dosing with radiolabeled umeclidinium, mass balance showed 58% of the radiolabel in the feces and 22% in the urine. The excretion of the drug-related material in the feces following intravenous dosing indicated elimination in the bile. Following oral dosing to healthy male subjects, radiolabel recovered in feces was 92% of the total dose and that in urine was <1% of the total dose, suggesting negligible oral absorption.
Vilanterol: The effective half-life for vilanterol, as determined from inhalation administration of multiple doses, is 11 hours. Following oral administration of radiolabeled vilanterol, mass balance showed 70% of the radiolabel in the urine and 30% in the feces.
Specific Populations
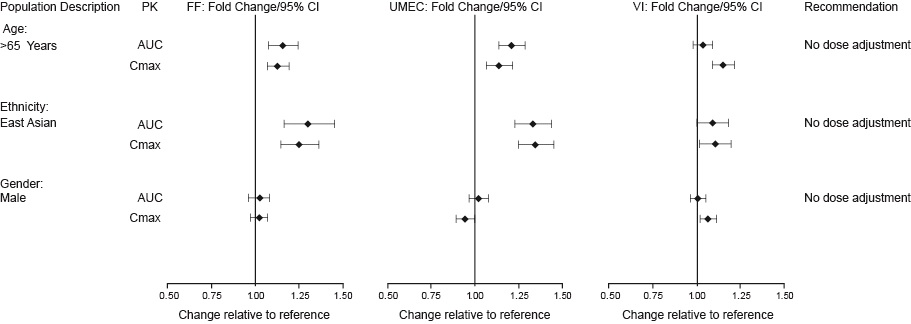
The effects of intrinsic and extrinsic factors on the pharmacokinetics of fluticasone furoate, umeclidinium, and vilanterol are shown in Figures 1, 2, and 3. Based on population pharmacokinetic analyses, none of the covariates assessed (i.e., age, race, gender) had a clinically relevant effect on fluticasone furoate, umeclidinium, or vilanterol pharmacokinetics when administered as TRELEGY ELLIPTA.
Figure 1. Impact of Intrinsic Factors on the Pharmacokinetics (PK) of Fluticasone Furoate (FF), Umeclidinium (UMEC), and Vilanterol (VI) Following Coadministration
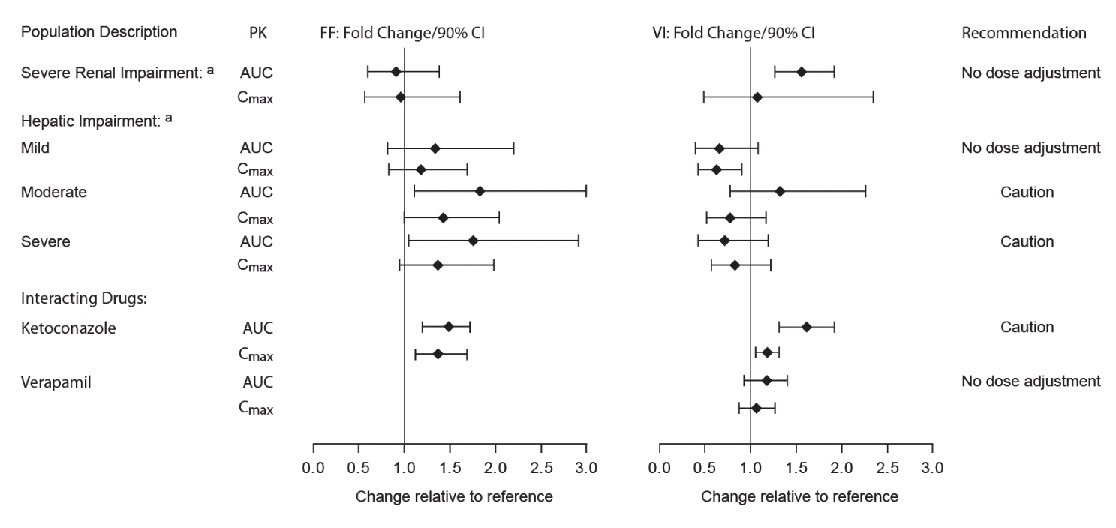
Figure 2. Impact of Intrinsic Factorsa and Coadministered Drugsb on the Pharmacokinetics (PK) of Fluticasone Furoate (FF) and Vilanterol (VI) Following Administration as Fluticasone Furoate/Vilanterol Combination or Following Vilanterol Coadministered with Umeclidinium
a Renal groups (fluticasone furoate/vilanterol 200 mcg/25 mcg) and hepatic groups (fluticasone furoate/vilanterol 200 mcg/25 mcg or fluticasone furoate/vilanterol 100 mcg/12.5 mcg).
b Compared with placebo group.
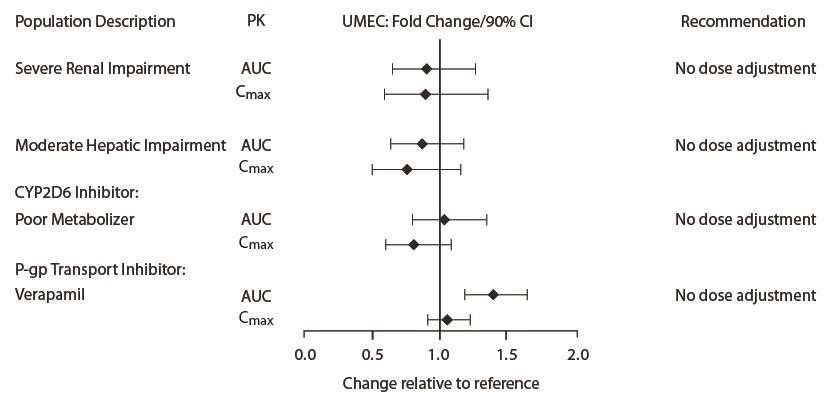
Figure 3. Impact of Intrinsic Factors and Coadministered Drugs on the Systemic Exposure of Umeclidinium
Racial or Ethnic Groups: Systemic exposure (AUCss) to inhaled fluticasone furoate was approximately 30% higher in subjects with COPD of East Asian heritage (n = 113) compared with white subjects (Figure 1). However, this higher exposure to fluticasone furoate is not expected to have clinically relevant effects on serum or urine cortisol or on efficacy in these racial groups.
There was no effect of race on the pharmacokinetics of umeclidinium or vilanterol in subjects with COPD (Figure 1).
Patients with Hepatic Impairment: Fluticasone Furoate: Following repeat dosing of fluticasone furoate/vilanterol 200 mcg/25 mcg (100 mcg/12.5 mcg in the severe impairment group) for 7 days, there was an increase of 34%, 83%, and 75% in fluticasone furoate systemic exposure (AUC) in subjects with mild, moderate, and severe hepatic impairment, respectively, compared with healthy subjects (Figure 2).
In subjects with moderate hepatic impairment receiving fluticasone furoate/vilanterol 200 mcg/25 mcg, mean serum cortisol (0 to 24 hours) was reduced by 34% (90% CI: 11%, 51%) compared with healthy subjects. In subjects with severe hepatic impairment receiving fluticasone furoate/vilanterol 100 mcg/12.5 mcg, mean serum cortisol (0 to 24 hours) was increased by 14% (90% CI: -16%, 55%) compared with healthy subjects. Patients with moderate to severe hepatic disease should be closely monitored.
Umeclidinium: The impact of hepatic impairment on the pharmacokinetics of umeclidinium has been evaluated in subjects with moderate hepatic impairment (Child-Pugh score of 7-9). There was no evidence of an increase in systemic exposure to umeclidinium (Cmax and AUC) (Figure 3). There was no evidence of altered protein binding in subjects with moderate hepatic impairment compared with healthy subjects. TRELEGY ELLIPTA has not been evaluated in subjects with severe hepatic impairment.
Vilanterol: Hepatic impairment had no effect on vilanterol systemic exposure (Cmax and AUCss on Day 7) following repeat-dose administration of fluticasone furoate/vilanterol 200 mcg/25 mcg (100 mcg/12.5 mcg in the severe impairment group) for 7 days (Figure 2).
There were no additional clinically relevant effects of the fluticasone furoate/vilanterol combinations on heart rate or serum potassium in subjects with mild or moderate hepatic impairment (vilanterol 25 mcg combination) or with severe hepatic impairment (vilanterol 12.5 mcg combination) compared with healthy subjects.
Patients with Renal Impairment: Fluticasone Furoate: Systemic exposure was not increased in subjects with severe renal impairment compared with healthy subjects (Figure 2). There was no evidence of greater corticosteroid class-related systemic effects (assessed by serum cortisol) in subjects with severe renal impairment compared with healthy subjects.
Umeclidinium: The pharmacokinetics of umeclidinium has been evaluated in subjects with severe renal impairment (creatinine clearance <30 mL/min). There was no evidence of an increase in systemic exposure to umeclidinium (Cmax and AUC) (Figure 3). There was no evidence of altered protein binding in subjects with severe renal impairment compared with healthy subjects.
Vilanterol: Systemic exposure (AUCss) was 56% higher in subjects with severe renal impairment compared with healthy subjects (Figure 2). There was no evidence of greater beta‑agonist class-related systemic effects (assessed by heart rate and serum potassium) in subjects with severe renal impairment compared with healthy subjects.
Drug Interaction Studies
No drug-drug interaction studies have been conducted with TRELEGY ELLIPTA. The information below is from drug-drug interaction studies conducted with umeclidinium, fluticasone furoate/vilanterol, or umeclidinium/vilanterol. The potential for fluticasone furoate, umeclidinium, and vilanterol to inhibit or induce metabolic enzymes and transporter systems is negligible at low inhalation doses.
Inhibitors of Cytochrome P450 3A4: The exposure (AUC) of fluticasone furoate and vilanterol were 36% and 65% higher, respectively, when coadministered with ketoconazole 400 mg compared with placebo (Figure 2). The increase in fluticasone furoate exposure was associated with a 27% reduction in weighted mean serum cortisol (0 to 24 hours). The increase in vilanterol exposure was not associated with an increase in beta-agonist–related systemic effects on heart rate or blood potassium.
Cytochrome P450 2D6: In vitro metabolism of umeclidinium is mediated primarily by CYP2D6. However, no clinically meaningful difference in systemic exposure to umeclidinium (500 mcg) (8 times the approved dose) was observed following repeat daily inhaled dosing to normal (ultra‑rapid, extensive, and intermediate metabolizers) and CYP2D6 poor metabolizer subjects.
Inhibitors of P-glycoprotein: Fluticasone furoate, umeclidinium, and vilanterol are substrates of P‑gp. Coadministration of repeat-dose (240 mg once daily) verapamil (a moderate CYP3A4 inhibitor and a P-gp inhibitor) did not affect the vilanterol Cmax or AUC in healthy subjects (Figure 2). Drug interaction trials with a specific P-gp inhibitor and fluticasone furoate have not been conducted. The effect of the moderate P-gp transporter inhibitor verapamil (240 mg once daily) on the steady-state pharmacokinetics of umeclidinium was assessed in healthy subjects. No effect on umeclidinium Cmax was observed; however, an approximately 1.4-fold increase in umeclidinium AUC was observed (Figure 3).
-
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
TRELEGY ELLIPTA
No studies of carcinogenicity, mutagenicity, or impairment of fertility were conducted with TRELEGY ELLIPTA; however, studies are available for the individual components, fluticasone furoate, umeclidinium, and vilanterol, as described below.
Fluticasone Furoate
Fluticasone furoate produced no treatment-related increases in the incidence of tumors in 2-year inhalation studies in rats and mice at inhaled doses up to 9 and 19 mcg/kg/day, respectively (both approximately equal to the MRHDID for adults on a mcg/m2 basis).
Fluticasone furoate did not induce gene mutation in bacteria or chromosomal damage in a mammalian cell mutation test in mouse lymphoma L5178Y cells in vitro. There was also no evidence of genotoxicity in the in vivo micronucleus test in rats.
No evidence of impairment of fertility was observed in male and female rats at inhaled fluticasone furoate doses up to 29 and 91 mcg/kg/day, respectively (approximately 7 and 17 times, respectively, the MRHDID for adults on an AUC basis).
Umeclidinium
Umeclidinium produced no treatment-related increases in the incidence of tumors in 2-year inhalation studies in rats and mice at inhaled doses up to 137 and 295/200 mcg/kg/day (male/female), respectively (approximately 17 and 20/20 times the MRHDID for adults on an AUC basis, respectively).
Umeclidinium tested negative in the following genotoxicity assays: the in vitro Ames assay, in vitro mouse lymphoma assay, and in vivo rat bone marrow micronucleus assay.
No evidence of impairment of fertility was observed in male and female rats at subcutaneous doses up to 180 mcg/kg/day and at inhaled doses up to 294 mcg/kg/day, respectively (approximately 60 and 40 times, respectively, the MRHDID for adults on an AUC basis).
Vilanterol
In a 2-year carcinogenicity study in mice, vilanterol caused a statistically significant increase in ovarian tubulostromal adenomas in females at an inhaled dose of 29,500 mcg/kg/day (approximately 9,920 times the MRHDID for adults on an AUC basis). No increase in tumors was seen at an inhaled dose of 615 mcg/kg/day (approximately 370 times the MRHDID for adults on an AUC basis).
In a 2-year carcinogenicity study in rats, vilanterol caused statistically significant increases in mesovarian leiomyomas in females and shortening of the latency of pituitary tumors at inhaled doses greater than or equal to 84.4 mcg/kg/day (greater than or equal to approximately 25 times the MRHDID for adults on an AUC basis). No tumors were seen at an inhalation dose of 10.5 mcg/kg/day (approximately equal to the MRHDID for adults on an AUC basis).
These tumor findings in rodents are similar to those reported previously for other beta-adrenergic agonist drugs. The relevance of these findings to human use is unknown.
Vilanterol tested negative in the following genotoxicity assays: the in vitro Ames assay, in vivo rat bone marrow micronucleus assay, in vivo rat unscheduled DNA synthesis (UDS) assay, and in vitro Syrian hamster embryo (SHE) cell assay. Vilanterol tested equivocal in the in vitro mouse lymphoma assay.
No evidence of impairment of fertility was observed in male and female rats at inhaled vilanterol doses up to 31,500 and 37,100 mcg/kg/day, respectively (both approximately 4,090 times the MRHDID based on AUC).
-
14 CLINICAL STUDIES
The clinical efficacy of TRELEGY ELLIPTA has been evaluated in 3 clinical trials in subjects with COPD, including chronic bronchitis and/or emphysema: Trial 1 (NCT #01957163), Trial 2 (NCT #02119286), and Trial 3 (NCT #02164513).
Trials 1 and 2 were multicenter, randomized, double-blind, parallel-group, 12-week treatment trials. Across both trials, a total of 412 subjects received coadministration of umeclidinium 62.5 mcg + fluticasone furoate/vilanterol 100 mcg/25 mcg, the components of TRELEGY ELLIPTA. Comparative in vitro data provide support for reliance on coadministration studies with umeclidinium 62.5 mcg + fluticasone furoate/vilanterol 100 mcg/25 mcg [see Description (11)].
The population demographics for Trials 1 and 2 were: mean age of 64 years, 92% white, 66% male, and an average smoking history of 48 pack-years, with 50% identified as current smokers. At screening, the mean postbronchodilator percent predicted FEV1 was 46% (range: 14% to 76%), the mean postbronchodilator FEV1/FVC ratio was 0.48 (range: 0.21 to 0.70), and the mean percent reversibility was 13% (range: -24% to 86%).
Trial 3 was a randomized, multicenter, double-blind, parallel-group, 52-week treatment trial comparing the clinical efficacy of TRELEGY ELLIPTA with the fixed-dose combinations of fluticasone furoate/vilanterol 100 mcg/25 mcg and umeclidinium/vilanterol 62.5 mcg/25 mcg. A total of 10,355 subjects with COPD with a history of 1 or more moderate or severe exacerbations in the prior 12 months were randomized (2:2:1) to receive TRELEGY ELLIPTA, fluticasone furoate/vilanterol, or umeclidinium/vilanterol administered once daily.
The population demographics across all treatments were: mean age of 65 years, 77% white, 66% male, and an average smoking history of 46.6 pack-years, with 35% identified as current smokers. At study entry, the most common COPD medications were ICS + anticholinergic + LABA (34%), ICS + LABA (26%), anticholinergic + LABA (8%), and anticholinergic (7%); the mean postbronchodilator percent predicted FEV1 was 46% (SD: 15%), the mean postbronchodilator FEV1/FVC ratio was 0.47 (SD: 0.12), and the mean percent reversibility was 10% (range: -59% to 125%).
Lung Function: In Trials 1 and 2, the primary endpoint was change from baseline in trough (predose) FEV1 at Day 85 (defined as the mean of the FEV1 values obtained at 23 and 24 hours after the previous dose on Day 84). For both trials, umeclidinium + fluticasone furoate/vilanterol demonstrated a statistically significant increase relative to placebo + fluticasone furoate/vilanterol (Table 2); similar results were demonstrated for the secondary endpoint of the weighted mean FEV1 (0 to 6 hours postdose) on Day 84 (Table 2).
Table 2. Least Squares (LS) Mean Change from Baseline in Trough FEV1 and Weighted Mean FEV1 (0-6 h) at Week 12 (Days 84/85) FEV1 = Forced Expiratory Volume in 1 Second; FF/VI = Fluticasone Furoate/Vilanterol 100 mcg/25 mcg; UMEC = Umeclidinium 62.5 mcg.
a At Day 85.
b At Day 84.
c For Placebo + FF/VI: Trial 1, n = 206; Trial 2, n = 206.Treatment
n
Trough FEV1 (mL)a
Weighted Mean FEV1 (0-6 h) (mL)b
Difference from
Placebo + FF/VIc
(95% CI)
Difference from
Placebo + FF/VIc
(95% CI)
Trial 1
UMEC + FF/VI
206
124
(93, 154)
153
(118, 187)
Trial 2
UMEC + FF/VI
206
122
(91, 152)
147
(114, 179)
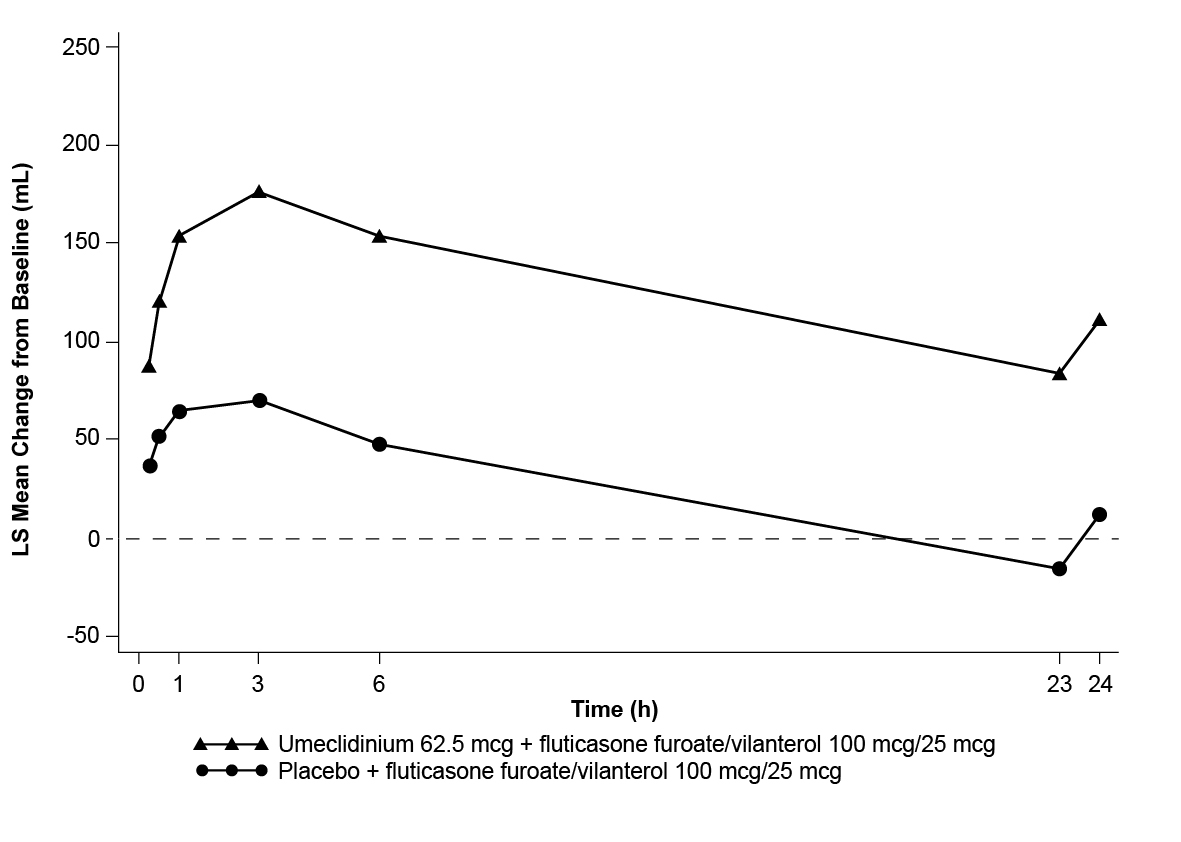
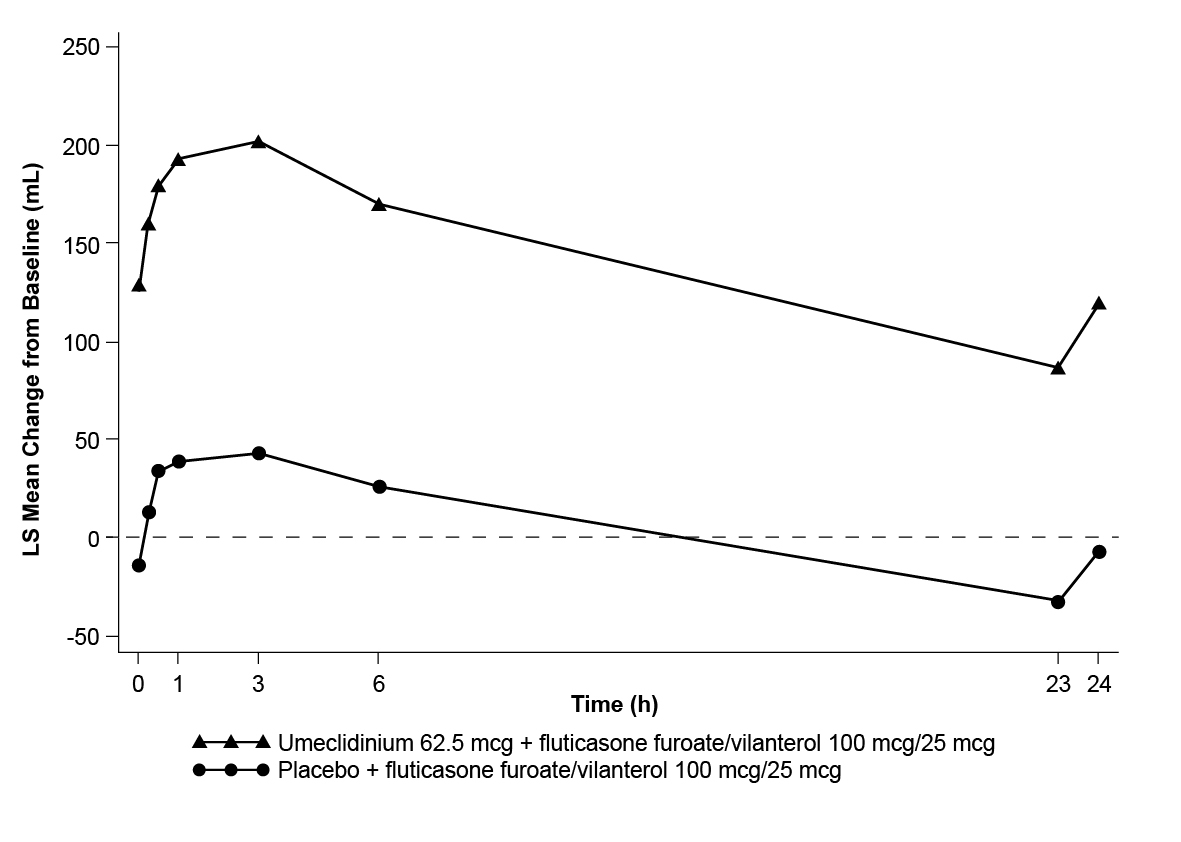
Greater LS mean changes from baseline in FEV1 over time were demonstrated for the umeclidinium + fluticasone furoate/vilanterol treatment group compared with the placebo + fluticasone furoate/vilanterol treatment group starting at 15 minutes postdose on Day 1. For Trial 1, LS mean changes in FEV1 over time relative to baseline are displayed for Day 1 and Day 84 in Figures 4 and 5, respectively. Similar results were seen in Trial 2.
Figure 4. Least Squares (LS) Mean Change from Baseline in Postdose Serial FEV1 (mL) on Day 1
Figure 5. Least Squares (LS) Mean Change from Baseline in Postdose Serial FEV1 (mL) on Day 84
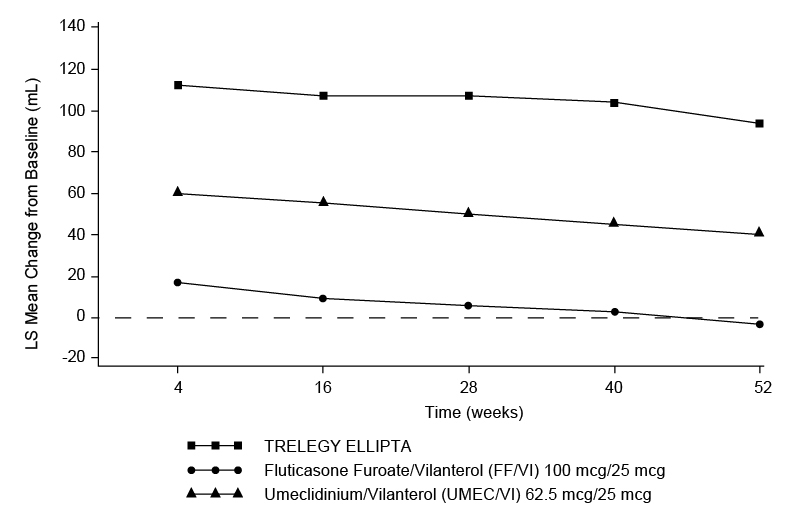
In Trial 3, treatment with TRELEGY ELLIPTA demonstrated a statistically significant improvement in lung function (mean change from baseline trough FEV1 at Week 52) compared with fluticasone furoate/vilanterol and umeclidinium/vilanterol. The mean change from baseline in trough (predose) FEV1 at Week 52 was 97 mL for TRELEGY ELLIPTA compared with fluticasone furoate/vilanterol (95% CI: 85, 109; P<0.001) and 54 mL for TRELEGY ELLIPTA compared with umeclidinium/vilanterol (95% CI: 39, 69; P<0.001). The effects on lung function (mean change from baseline trough FEV1) of TRELEGY ELLIPTA compared with fluticasone furoate/vilanterol and umeclidinium/vilanterol were observed at all timepoints over the course of the 52-week study (Figure 6).
Figure 6. Least Squares (LS) Mean Change from Baseline in Trough FEV1 (mL)
Exacerbations: In Trial 3, the primary endpoint was annual rate of on-treatment moderate and severe exacerbations in subjects treated with TRELEGY ELLIPTA compared with fluticasone furoate/vilanterol and umeclidinium/vilanterol. Exacerbations were defined as worsening of 2 or more major symptoms (dyspnea, sputum volume, and sputum purulence) or worsening of any 1 major symptom together with any 1 of the following minor symptoms: sore throat, colds (nasal discharge and/or nasal congestion), fever without other cause, and increased cough or wheeze for at least 2 consecutive days. Exacerbations were considered to be moderate severity if treatment with systemic corticosteroids and/or antibiotics was required and were considered to be severe if resulted in hospitalization or death.
Treatment with TRELEGY ELLIPTA statistically significantly reduced the on-treatment annual rate of moderate/severe exacerbations by 15% compared with fluticasone furoate/vilanterol and by 25% compared with umeclidinium/vilanterol (Table 3).
Table 3. Moderate and Severe Chronic Obstructive Pulmonary Disease Exacerbations (Trial 3)a FF/VI = Fluticasone Furoate/Vilanterol 100 mcg/25 mcg; UMEC/VI = Umeclidinium/Vilanterol 62.5 mcg/25 mcg.
a On-treatment analyses excluded exacerbation data collected after discontinuation of study treatment.Treatment
n
Mean Annual Rate
(exacerbations/year)
Rate Ratio vs. Comparator
(95% CI)
% Reduction in Exacerbation Rate
(95% CI)
P Value
TRELEGY ELLIPTA
4,145
0.91
FF/VI
4,133
1.07
0.85
(0.80, 0.90)
15
(10, 20)
P<0.001
UMEC/VI
2,069
1.21
0.75
(0.70, 0.81)
25
(19, 30)
P<0.001
Treatment with TRELEGY ELLIPTA statistically significantly decreased the risk of a moderate/severe exacerbation as measured by time to first exacerbation when compared with fluticasone furoate/vilanterol (14.8%; 95% CI: 9.3, 19.9; P<0.001) and umeclidinium/vilanterol (16.0%; 95% CI: 9.4, 22.1; P<0.001).
Treatment with TRELEGY ELLIPTA reduced the on-treatment annual rate of severe exacerbations (i.e., requiring hospitalization or resulting in death) by 13% compared with fluticasone furoate/vilanterol (95% CI: -1, 24; P = 0.064) which was not statistically significant. Treatment with TRELEGY ELLIPTA statistically significantly reduced the on-treatment annual rate of severe exacerbations by 34% compared with umeclidinium/vilanterol (95% CI: 22, 44; P<0.001).
Health-Related Quality of Life: In all 3 trials, health-related quality of life was assessed using the St. George’s Respiratory Questionnaire for COPD patients (SGRQ-C), a disease-specific shorter version derived from the original St. George’s Respiratory Questionnaire (SGRQ). Results were transformed to the SGRQ for reporting purposes. In Trial 1, the on‑treatment responder rate at Week 12 (response defined as a decrease in score from baseline of 4 or more) was 40% for umeclidinium +fluticasone furoate/vilanterol vs. 35% for placebo + fluticasone furoate/vilanterol (odds ratio 1.2; 95% CI: 0.8, 1.8). In Trial 2, the on‑treatment responder rate at Week 12 was 35% for umeclidinium + fluticasone furoate/vilanterol vs. 21% for placebo + fluticasone furoate/vilanterol (odds ratio 2.0; 95% CI: 1.3, 3.1). In Trial 3, the on-treatment responder rate at Week 52 was statistically significantly greater for subjects treated with TRELEGY ELLIPTA (42%) compared with fluticasone furoate/vilanterol (34%; odds ratio 1.41; 95% CI: 1.29, 1.55; P<0.001) and compared with umeclidinium/vilanterol (34%; odds ratio 1.41; 95% CI: 1.26, 1.57; P<0.001).
Other Endpoints: In Trials 1 and 2, subjects treated with umeclidinium + fluticasone furoate/vilanterol on average used less rescue medication compared with subjects treated with placebo + fluticasone furoate/vilanterol over Weeks 1 to 12. In Trial 3, subjects treated with TRELEGY ELLIPTA on average used less rescue medication (mean number of uses per day and percentage of rescue-free 24-hour periods) compared with subjects treated with fluticasone furoate/vilanterol or umeclidinium/vilanterol over the course of the 52-week study.
-
16 HOW SUPPLIED/STORAGE AND HANDLING
TRELEGY ELLIPTA is supplied as a disposable light grey and beige plastic inhaler containing 2 foil strips, each with 30 blisters (or 14 blisters for the institutional pack). One strip contains fluticasone furoate (100 mcg per blister), and the other strip contains a blend of umeclidinium and vilanterol (62.5 mcg and 25 mcg per blister, respectively). A blister from each strip is used to create 1 dose. The inhaler is packaged within a moisture-protective foil tray with a desiccant and a peelable lid in the following packs:
NDC: 0173-0887-10 TRELEGY ELLIPTA 30 inhalations (60 blisters)
NDC: 0173-0887-14 TRELEGY ELLIPTA 14 inhalations (28 blisters), institutional pack
Store at room temperature between 68°F and 77°F (20°C and 25°C); excursions permitted from 59°F to 86°F (15°C to 30°C) [See USP Controlled Room Temperature]. Store in a dry place away from direct heat or sunlight. Keep out of reach of children.
TRELEGY ELLIPTA should be stored inside the unopened moisture-protective foil tray and only removed from the tray immediately before initial use. Discard TRELEGY ELLIPTA 6 weeks after opening the foil tray or when the counter reads “0” (after all blisters have been used), whichever comes first. The inhaler is not reusable. Do not attempt to take the inhaler apart.
-
17 PATIENT COUNSELING INFORMATION
Advise the patient to read the FDA-approved patient labeling (Patient Information and Instructions for Use).
Not for Acute Symptoms
Inform patients that TRELEGY ELLIPTA is not meant to relieve acute symptoms of COPD and extra doses should not be used for that purpose. Advise patients to treat acute symptoms with an inhaled, short-acting beta2-agonist such as albuterol. Provide patients with such medication and instruct them in how it should be used.
Instruct patients to seek medical attention immediately if they experience any of the following:
- Decreasing effectiveness of inhaled, short-acting beta2-agonists
- Need for more inhalations than usual of inhaled, short-acting beta2-agonists
- Significant decrease in lung function as outlined by the physician
Tell patients they should not stop therapy with TRELEGY ELLIPTA without physician/provider guidance since symptoms may recur after discontinuation.
Do Not Use Additional Long-acting Beta2-agonists
Instruct patients not to use other LABA.
Local Effects
Inform patients that localized infections with Candida albicans occurred in the mouth and pharynx in some patients. If oropharyngeal candidiasis develops, treat it with appropriate local or systemic (i.e., oral) antifungal therapy while still continuing therapy with TRELEGY ELLIPTA, but at times therapy with TRELEGY ELLIPTA may need to be temporarily interrupted under close medical supervision. Advise patients to rinse the mouth with water without swallowing after inhalation to help reduce the risk of thrush.
Pneumonia
Patients with COPD have a higher risk of pneumonia; instruct them to contact their healthcare providers if they develop symptoms of pneumonia.
Immunosuppression
Warn patients who are on immunosuppressant doses of corticosteroids to avoid exposure to chickenpox or measles and, if exposed, to consult their physicians without delay. Inform patients of potential worsening of existing tuberculosis; fungal, bacterial, viral, or parasitic infections; or ocular herpes simplex.
Hypercorticism and Adrenal Suppression
Advise patients that TRELEGY ELLIPTA may cause systemic corticosteroid effects of hypercorticism and adrenal suppression. Additionally, inform patients that deaths due to adrenal insufficiency have occurred during and after transfer from systemic corticosteroids. Patients should taper slowly from systemic corticosteroids if transferring to TRELEGY ELLIPTA.
Paradoxical Bronchospasm
As with other inhaled medicines, TRELEGY ELLIPTA can cause paradoxical bronchospasm. If paradoxical bronchospasm occurs, instruct patients to discontinue TRELEGY ELLIPTA and contact their healthcare provider right away.
Hypersensitivity Reactions, including Anaphylaxis
Advise patients that hypersensitivity reactions (e.g., anaphylaxis, angioedema, rash, urticaria) may occur after administration of TRELEGY ELLIPTA. Instruct patients to discontinue TRELEGY ELLIPTA if such reactions occur. There have been reports of anaphylactic reactions in patients with severe milk protein allergy after inhalation of other powder medications containing lactose; therefore, patients with severe milk protein allergy should not use TRELEGY ELLIPTA.
Reduction in Bone Mineral Density
Advise patients who are at an increased risk for decreased BMD that the use of corticosteroids may pose an additional risk.
Glaucoma and Cataracts
Advise patients that long-term use of ICS may increase the risk of some eye problems (cataracts or glaucoma); consider regular eye examinations.
Instruct patients to be alert for signs and symptoms of acute narrow-angle glaucoma (e.g., eye pain or discomfort, blurred vision, visual halos or colored images in association with red eyes from conjunctival congestion and corneal edema). Instruct patients to consult a physician immediately if any of these signs or symptoms develop.
Worsening of Urinary Retention
Instruct patients to be alert for signs and symptoms of urinary retention (e.g., difficulty passing urine, painful urination). Instruct patients to consult a physician immediately if any of these signs or symptoms develop.
Risks Associated with Beta-agonist Therapy
Inform patients of adverse effects associated with beta2-agonists, such as palpitations, chest pain, rapid heart rate, tremor, or nervousness.
Trademarks are owned by or licensed to the GSK group of companies.
TRELEGY ELLIPTA was developed in collaboration with Innoviva.
GlaxoSmithKline
Research Triangle Park, NC 27709
©2019 GSK group of companies or its licensor.
TRL:5PI
-
PATIENT PACKAGE INSERT
PATIENT INFORMATION
TRELEGY ELLIPTA (TREL-e-gee e-LIP-ta)
(fluticasone furoate, umeclidinium, and vilanterol inhalation powder)
for oral inhalation use
What is TRELEGY ELLIPTA?
- TRELEGY ELLIPTA combines 3 medicines in one inhaler, an inhaled corticosteroid (ICS) medicine (fluticasone furoate), an anticholinergic medicine (umeclidinium), and a long-acting beta2-adrenergic agonist (LABA) medicine (vilanterol).
- ICS medicines such as fluticasone furoate help to decrease inflammation in the lungs. Inflammation in the lungs can lead to breathing problems.
- Anticholinergic medicines such as umeclidinium and LABA medicines such as vilanterol help the muscles around the airways in your lungs stay relaxed to prevent symptoms such as wheezing, cough, chest tightness, and shortness of breath. These symptoms can happen when the muscles around the airways tighten. This makes it hard to breathe.
- TRELEGY ELLIPTA is a prescription medicine used long term (chronic) to treat people with chronic obstructive pulmonary disease (COPD). COPD is a chronic lung disease that includes chronic bronchitis, emphysema, or both.
- TRELEGY ELLIPTA is used as 1 inhalation 1 time each day to improve symptoms of COPD for better breathing and to reduce the number of flare-ups (the worsening of your COPD symptoms for several days).
- TRELEGY ELLIPTA is not approved for the treatment of asthma. TRELEGY ELLIPTA contains vilanterol. LABA medicines such as vilanterol when used alone increase the risk of hospitalizations and death from asthma problems. TRELEGY ELLIPTA contains an ICS, an anticholinergic, and a LABA. When an ICS and LABA are used together, there is not a significant increased risk in hospitalizations and death from asthma problems.
- TRELEGY ELLIPTA is not used to relieve sudden breathing problems and will not replace a rescue inhaler. Always have a rescue inhaler (an inhaled, short-acting bronchodilator) with you to treat sudden breathing problems. If you do not have a rescue inhaler, contact your healthcare provider to have one prescribed for you.
- TRELEGY ELLIPTA should not be used in children. It is not known if TRELEGY ELLIPTA is safe and effective in children.
Do not use TRELEGY ELLIPTA if you:
- have a severe allergy to milk proteins. Ask your healthcare provider if you are not sure.
- are allergic to fluticasone furoate, umeclidinium, vilanterol, or any of the ingredients in TRELEGY ELLIPTA. See the end of this Patient Information for a complete list of ingredients in TRELEGY ELLIPTA.
Before using TRELEGY ELLIPTA, tell your healthcare provider about all of your medical conditions, including if you:
- have heart problems.
- have high blood pressure.
- have seizures.
- have thyroid problems.
- have diabetes.
- have liver problems.
- have weak bones (osteoporosis).
- have an immune system problem.
- have eye problems such as glaucoma, increased pressure in your eye, cataracts, blurred vision, or other changes in vision. TRELEGY ELLIPTA may make your glaucoma worse.
- are allergic to milk proteins.
- have prostate or bladder problems, or problems passing urine. TRELEGY ELLIPTA may make these problems worse.
- have any type of viral, bacterial, parasitic, or fungal infection.
- are exposed to chickenpox or measles.
- are pregnant or plan to become pregnant. It is not known if TRELEGY ELLIPTA may harm your unborn baby.
- are breastfeeding. It is not known if the medicines in TRELEGY ELLIPTA pass into your milk and if they can harm your baby.
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. TRELEGY ELLIPTA and certain other medicines may interact with each other. This may cause serious side effects.
Especially tell your healthcare provider if you take:
- anticholinergics (including tiotropium, ipratropium, aclidinium)
- atropine
- other LABA (including salmeterol, formoterol, arformoterol, olodaterol, and indacaterol)
- antifungal or anti-HIV medicines.
Know the medicines you take. Keep a list of them to show your healthcare provider and pharmacist when you get a new medicine.
How should I use TRELEGY ELLIPTA?
Read the step-by-step instructions for using TRELEGY ELLIPTA at the end of this Patient Information.
- Do not use TRELEGY ELLIPTA unless your healthcare provider has taught you how to use the inhaler and you understand how to use it correctly.
- Use TRELEGY ELLIPTA exactly as your healthcare provider tells you to use it. Do not use TRELEGY ELLIPTA more often than prescribed.
- Use 1 inhalation of TRELEGY ELLIPTA 1 time each day. Use TRELEGY ELLIPTA at the same time each day.
- If you miss a dose of TRELEGY ELLIPTA, take it as soon as you remember. Do not take more than 1 inhalation per day. Take your next dose at your usual time. Do not take 2 doses at 1 time.
- If you take too much TRELEGY ELLIPTA, call your healthcare provider or go to the nearest hospital emergency room right away if you have any unusual symptoms, such as worsening shortness of breath, chest pain, increased heart rate, or shakiness.
- Do not use other medicines that contain a LABA or an anticholinergic for any reason. Ask your healthcare provider or pharmacist if any of your other medicines are LABA or anticholinergic medicines.
- Do not stop using TRELEGY ELLIPTA unless told to do so by your healthcare provider because your symptoms might get worse. Your healthcare provider will change your medicines as needed.
- TRELEGY ELLIPTA does not relieve sudden symptoms of COPD and you should not take extra doses of TRELEGY ELLIPTA to relieve these sudden symptoms. Always have a rescue inhaler with you to treat sudden symptoms. If you do not have a rescue inhaler, call your healthcare provider to have one prescribed for you.
-
Call your healthcare provider or get medical care right away if:
- your breathing problems get worse.
- you need to use your rescue inhaler more often than usual.
- your rescue inhaler does not work as well to relieve your symptoms.
What are the possible side effects of TRELEGY ELLIPTA?
TRELEGY ELLIPTA can cause serious side effects, including:
- fungal infection in your mouth or throat (thrush). Rinse your mouth with water without swallowing after using TRELEGY ELLIPTA to help reduce your chance of getting thrush.
- pneumonia. People with COPD have a higher chance of getting pneumonia. TRELEGY ELLIPTA may increase the chance of getting pneumonia. Call your healthcare provider if you notice any of the following symptoms:
- increase in mucus (sputum) production
- change in mucus color
- fever
- chills
- increased cough
- increased breathing problems
- weakened immune system and increased chance of getting infections (immunosuppression).
- reduced adrenal function (adrenal insufficiency). Adrenal insufficiency is a condition where the adrenal glands do not make enough steroid hormones. This can happen when you stop taking oral corticosteroid medicines (such as prednisone) and start taking a medicine containing an ICS (such as TRELEGY ELLIPTA). During this transition period, when your body is under stress from fever, trauma (such as a car accident), infection, surgery, or worse COPD symptoms, adrenal insufficiency can get worse and may cause death.
- Symptoms of adrenal insufficiency include:
- feeling tired
- lack of energy
- weakness
- nausea and vomiting
- low blood pressure (hypotension)
- sudden breathing problems immediately after inhaling your medicine. If you have sudden breathing problems immediately after inhaling your medicine, stop taking TRELEGY ELLIPTA and call your healthcare provider right away.
- serious allergic reactions. Call your healthcare provider or get emergency medical care if you get any of the following symptoms of a serious allergic reaction:
- rash
- hives
- swelling of your face, mouth, and tongue
- breathing problems
- effects on heart.
- increased blood pressure
- a fast or irregular heartbeat, awareness of heartbeat
- chest pain
- effects on nervous system.
- tremor
- nervousness
- bone thinning or weakness (osteoporosis).
- eye problems including glaucoma, increased pressure in your eye, cataracts, blurred vision, worsening of narrow-angle glaucoma, or other changes in vision. You should have regular eye exams while using TRELEGY ELLIPTA.
- Acute narrow-angle glaucoma can cause permanent loss of vision if not treated. Symptoms of acute narrow-angle glaucoma may include:
- eye pain or discomfort
- nausea or vomiting
- blurred vision
- seeing halos or bright colors around lights
- red eyes
- If you have these symptoms, call your healthcare provider right away before taking another dose.
- 1. urinary retention. People who take TRELEGY ELLIPTA may develop new or worse urinary retention. Symptoms of urinary retention may include:
- difficulty urinating
- painful urination
- urinating frequently
- urination in a weak stream or drips
- If you have these symptoms of urinary retention, stop taking TRELEGY ELLIPTA, and call your healthcare provider right away before taking another dose.
- 1. changes in laboratory blood values, including high levels of blood sugar (hyperglycemia) and low levels of potassium (hypokalemia).
Common side effects of TRELEGY ELLIPTA include:
- upper respiratory tract infection
- pneumonia
- bronchitis
- thrush in your mouth and throat. Rinse your mouth with water without swallowing after use to help prevent this.
- headache
- back pain
- joint pain
- flu
- inflammation of the sinuses
- runny nose and sore throat
- taste disturbance
- constipation
- painful and frequent urination
- (signs of a urinary tract infection)
- nausea, vomiting, and diarrhea
- mouth and throat pain
- cough
- hoarseness
These are not all the possible side effects of TRELEGY ELLIPTA.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
How should I store TRELEGY ELLIPTA?
- Store TRELEGY ELLIPTA at room temperature between 68°F and 77°F (20°C and 25°C). Keep in a dry place away from heat and sunlight.
- Store TRELEGY ELLIPTA in the unopened tray and only open when ready for use.
- Safely throw away TRELEGY ELLIPTA in the trash 6 weeks after you open the tray or when the counter reads “0”, whichever comes first. Write the date you open the tray on the label on the inhaler.
Keep TRELEGY ELLIPTA and all medicines out of the reach of children.
General information about the safe and effective use of TRELEGY ELLIPTA.
Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. Do not use TRELEGY ELLIPTA for a condition for which it was not prescribed. Do not give TRELEGY ELLIPTA to other people, even if they have the same symptoms that you have. It may harm them.
You can ask your healthcare provider or pharmacist for information about TRELEGY ELLIPTA that is written for health professionals.
What are the ingredients in TRELEGY ELLIPTA?
Active ingredients: fluticasone furoate, umeclidinium, vilanterol
Inactive ingredients: lactose monohydrate (contains milk proteins), magnesium stearate
For more information about TRELEGY ELLIPTA, call 1-888-825-5249 or visit our website at www.trelegy.com.
Trademarks are owned by or licensed to the GSK group of companies.
TRELEGY ELLIPTA was developed in collaboration with Innoviva.
GlaxoSmithKline, Research Triangle Park, NC 27709
©2019 GSK group of companies or its licensor.
TRL:4PIL
- This Patient Information has been approved by the U.S. Food and Drug Administration Revised: May 2019
This Instructions for Use has been approved by the U.S. Food and Drug Administration Revised: April 2018
-
PRINCIPAL DISPLAY PANEL
PRINCIPAL DISPLAY PANEL
NDC: 0173-0887-10
Trelegy ELLIPTA
(fluticasone furoate, umeclidinium, and vilanterol inhalation powder)
100 mcg/62.5 mcg/25 mcg
Rx Only
FOR ORAL INHALATION ONLY
TRELEGY ELLIPTA contains 2 foils strips of 30 blisters each. Each blister on one strip contains 100 mcg of fluticasone furoate and lactose monohydrate. Each blister on the other strip contains 62.5 mcg of umeclidinium, 25 mcg of vilanterol, magnesium stearate, and lactose monohydrate.
1 ELLIPTA Inhaler containing 30 doses (60 blisters total)
Made in UK
©2018 GSK group of companies or its licensor.
10000000149452
Rev. 7/18
-
INGREDIENTS AND APPEARANCE
TRELEGY ELLIPTA
fluticasone furoate, umeclidinium bromide and vilanterol trifenatate powderProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 0173-0887 Route of Administration RESPIRATORY (INHALATION) Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength FLUTICASONE FUROATE (UNII: JS86977WNV) (FLUTICASONE - UNII:CUT2W21N7U) FLUTICASONE FUROATE 100 ug UMECLIDINIUM BROMIDE (UNII: 7AN603V4JV) (UMECLIDINIUM - UNII:GE2T1418SV) UMECLIDINIUM 62.5 ug VILANTEROL TRIFENATATE (UNII: 40AHO2C6DG) (VILANTEROL - UNII:028LZY775B) VILANTEROL 25 ug Inactive Ingredients Ingredient Name Strength MAGNESIUM STEARATE (UNII: 70097M6I30) LACTOSE MONOHYDRATE (UNII: EWQ57Q8I5X) Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 0173-0887-10 1 in 1 CARTON 09/18/2017 1 1 in 1 TRAY 1 30 in 1 INHALER; Type 2: Prefilled Drug Delivery Device/System (syringe, patch, etc.) 2 NDC: 0173-0887-14 1 in 1 CARTON 09/18/2017 2 1 in 1 TRAY 2 14 in 1 INHALER; Type 2: Prefilled Drug Delivery Device/System (syringe, patch, etc.) 3 NDC: 0173-0887-61 1 in 1 CARTON 09/18/2017 3 1 in 1 TRAY 3 14 in 1 INHALER; Type 0: Not a Combination Product Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date NDA NDA209482 09/18/2017 Labeler - GlaxoSmithKline LLC (167380711)
Trademark Results [Trelegy Ellipta]
Mark Image Registration | Serial | Company Trademark Application Date |
|---|---|
 TRELEGY ELLIPTA 88196660 not registered Live/Pending |
Glaxo Group Limited 2018-11-16 |
© 2026 FDA.report
This site is not affiliated with or endorsed by the FDA.