GADAVIST- gadobutrol injection
Gadavist by
Drug Labeling and Warnings
Gadavist by is a Prescription medication manufactured, distributed, or labeled by Bayer HealthCare Pharmaceuticals Inc., Bayer AG. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
-
HIGHLIGHTS OF PRESCRIBING INFORMATION
These highlights do not include all the information needed to use GADAVIST safely and effectively. See full prescribing information for GADAVIST.
GADAVIST (gadobutrol) injection, for intravenous use
Initial U.S. Approval: 2011WARNING: RISK ASSOCIATED WITH INTRATHECAL USE and NEPHROGENIC SYSTEMIC FIBROSIS
See full prescribing information for complete boxed warning.
- Intrathecal administration of gadolinium-based contrast agents (GBCAs) can cause serious adverse reactions including death, coma, encephalopathy, and seizures. GADAVIST is not approved for intrathecal use. (5.1)
-
GBCAs increase the risk for nephrogenic systemic fibrosis (NSF) among patients with impaired elimination of the drugs. Avoid use of GADAVIST in these patients unless the diagnostic information is essential and not available with non-contrasted MRI or other modalities.
The risk for NSF appears highest among patients with:- Chronic, severe kidney disease (GFR < 30 mL/min/1.73m2), or
- Acute kidney injury.
RECENT MAJOR CHANGES
Warnings and Precautions, Acute Respiratory Distress Syndrome (5.4) 3/2025 INDICATIONS AND USAGE
GADAVIST is a gadolinium-based contrast agent indicated for use with magnetic resonance imaging (MRI):
- To detect and visualize areas with disrupted blood brain barrier and/or abnormal vascularity of the central nervous system in adult and pediatric patients including term neonates
- To assess the presence and extent of malignant breast disease in adult patients
- To evaluate known or suspected supra-aortic or renal artery disease in adult and pediatric patients including term neonates
- To assess myocardial perfusion (stress, rest) and late gadolinium enhancement in adult patients with known or suspected coronary artery disease (CAD) (1)
DOSAGE AND ADMINISTRATION
DOSAGE FORMS AND STRENGTHS
Injection: 1 mmol/mL of gadobutrol available in single-dose vial, single-dose prefilled syringe, and imaging bulk package (3)
CONTRAINDICATIONS
History of severe hypersensitivity reaction to GADAVIST (4)
WARNINGS AND PRECAUTIONS
- Hypersensitivity Reactions: Anaphylactic and other hypersensitivity reactions with cardiovascular, respiratory or cutaneous manifestations, ranging from mild to severe, including death, have occurred. Monitor patients closely during and after administration of GADAVIST. (5.3)
- Acute Respiratory Distress Syndrome: For patients demonstrating respiratory distress after administration, assess oxygen requirement and monitor for worsening respiratory function. (5.4)
- Gadolinium Retention: Gadolinium is retained for months or years in brain, bone, and other organs. (5.5)
ADVERSE REACTIONS
Most common adverse reactions (incidence ≥ 0.5%) are headache, nausea, and dizziness. (6.1)
To report SUSPECTED ADVERSE REACTIONS, contact Bayer HealthCare Pharmaceuticals Inc. at 1-888-842-2937 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch
USE IN SPECIFIC POPULATIONS
Pregnancy: Use only if imaging is essential during pregnancy and cannot be delayed. (8.1)
See 17 for PATIENT COUNSELING INFORMATION and Medication Guide.
Revised: 2/2026
-
Table of Contents
FULL PRESCRIBING INFORMATION: CONTENTS*
WARNING: RISK ASSOCIATED WITH INTRATHECAL USE and NEPHROGENIC SYSTEMIC FIBROSIS
1 INDICATIONS AND USAGE
2 DOSAGE AND ADMINISTRATION
2.1 Recommended Dose
2.2 Administration and Imaging Instructions
2.3 Directions for Use of Single-Dose Containers
2.4 Directions for Use of Imaging Bulk Package
3 DOSAGE FORMS AND STRENGTHS
4 CONTRAINDICATIONS
5 WARNINGS AND PRECAUTIONS
5.1 Risk Associated with Intrathecal Use
5.2 Nephrogenic Systemic Fibrosis
5.3 Hypersensitivity Reactions
5.4 Acute Respiratory Distress Syndrome
5.5 Gadolinium Retention
5.6 Acute Kidney Injury
5.7 Extravasation and Injection Site Reactions
5.8 Overestimation of Extent of Malignant Disease in MRI of the Breast
5.9 Low Sensitivity for Significant Arterial Stenosis
6 ADVERSE REACTIONS
6.1 Clinical Trials Experience
6.2 Postmarketing Experience
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
8.2 Lactation
8.4 Pediatric Use
8.5 Geriatric Use
8.6 Renal Impairment
10 OVERDOSAGE
11 DESCRIPTION
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
12.2 Pharmacodynamics
12.3 Pharmacokinetics
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
13.2 Animal Toxicology and/or Pharmacology
14 CLINICAL STUDIES
14.1 MRI of the CNS
14.2 MRI of the Breast
14.3 MRA
14.4 Cardiac MRI
16 HOW SUPPLIED/STORAGE AND HANDLING
17 PATIENT COUNSELING INFORMATION
- * Sections or subsections omitted from the full prescribing information are not listed.
-
BOXED WARNING
(What is this?)
WARNING: RISK ASSOCIATED WITH INTRATHECAL USE and NEPHROGENIC SYSTEMIC FIBROSIS
Risk Associated with Intrathecal Use
Intrathecal administration of gadolinium-based contrast agents (GBCAs) can cause serious adverse reactions including death, coma, encephalopathy, and seizures. GADAVIST is not approved for intrathecal use [see Warnings and Precautions (5.1)].
Nephrogenic Systemic Fibrosis
GBCAs increase the risk for nephrogenic systemic fibrosis (NSF) among patients with impaired elimination of the drugs. Avoid use of GADAVIST in these patients unless the diagnostic information is essential and not available with non-contrasted MRI or other modalities. NSF may result in fatal or debilitating fibrosis affecting the skin, muscle and internal organs.
The risk for NSF appears highest among patients with:
- Chronic, severe kidney disease (GFR < 30 mL/min/1.73m2), or
- Acute kidney injury.
Screen patients for acute kidney injury and other conditions that may reduce renal function. For patients at risk for chronically reduced renal function (for example, age > 60 years, hypertension or diabetes), estimate the glomerular filtration rate (GFR) through laboratory testing.
For patients at highest risk for NSF, do not exceed the recommended GADAVIST dose and allow a sufficient period of time for elimination of the drug from the body prior to any re-administration [see Warnings and Precautions (5.2)].
-
1 INDICATIONS AND USAGE
GADAVIST is indicated for:
- Magnetic resonance imaging (MRI) of the central nervous system (CNS) to detect and visualize areas with disrupted blood brain barrier and/or abnormal vascularity in adult and pediatric patients including term neonates
- MRI of the breast to assess the presence and extent of malignant breast disease in adult patients
- Magnetic resonance angiography (MRA) to evaluate known or suspected supra-aortic or renal artery disease in adult and pediatric patients including term neonates
- Cardiac MRI (CMRI) to assess myocardial perfusion (stress, rest) and late gadolinium enhancement in adult patients with known or suspected coronary artery disease (CAD)
-
2 DOSAGE AND ADMINISTRATION
2.1 Recommended Dose
The recommended dose of GADAVIST for adult and pediatric patients, including term neonates, is 0.1 mmol/kg actual body weight (equivalent to 0.1 mL/kg) administered intravenously.
For CMRI, the dose is divided into two separate, equal injections [see Dosage and Administration (2.2)].
Refer to Table 1 for volumes to be administered for example body weights.
Table 1: Volume of GADAVIST for Example Body Weights Body Weight (kg) Volume to be Administered (mL) 2.5 0.25 5 0.5 10 1 15 1.5 20 2 25 2.5 30 3 35 3.5 40 4 45 4.5 50 5 60 6 70 7 80 8 90 9 100 10 110 11 120 12 130 13 140 14 2.2 Administration and Imaging Instructions
General
- GADAVIST is formulated at a higher concentration (1 mmol/mL) compared to certain other gadolinium-based contrast agents, resulting in a lower volume of administration [see Dosage and Administration (2.1)].
- GADAVIST is for intravenous use only and must not be administered intrathecally [see Warnings and Precautions (5.1)].
- Use aseptic technique when preparing and administering GADAVIST.
- Visually inspect GADAVIST for particulate matter and discoloration prior to administration. Do not use the solution if it is discolored, if particulate matter is present, or if the container appears damaged.
- If solidification occurs due to cold exposure, bring GADAVIST to room temperature before use and inspect to ensure that the solution is clear and colorless to pale yellow.
- Do not mix GADAVIST with other medications and do not administer GADAVIST in the same intravenous line simultaneously with other medications.
MRI of the CNS in Adult and Pediatric Patients Including Term Neonates
- Administer GADAVIST as an intravenous injection, manually or by power injector, at a flow rate of approximately 2 mL/sec.
- Follow GADAVIST injection with a flush of 0.9% Sodium Chloride Injection to ensure complete administration of the contrast.
- Post contrast MRI can commence immediately following contrast administration.
MRI of the Breast in Adults
- Administer GADAVIST as an intravenous bolus by power injector, followed by a flush of 0.9% Sodium Chloride Injection to ensure complete administration of the contrast.
- Start image acquisition following GADAVIST administration and then repeat sequentially to determine peak intensity and wash-out.
MR Angiography in Adult and Pediatric Patients Including Term Neonates
- Image acquisition should coincide with peak arterial concentration, which varies among patients.
- For adults, administer GADAVIST as an intravenous injection by power injector, at a flow rate of approximately 1.5 mL/sec, followed by a 30 mL flush of 0.9% Sodium Chloride Injection at the same rate to ensure complete administration of the contrast.
- For pediatric patients including term neonates, administer GADAVIST as an intravenous injection by power injector or manually, followed by a flush of 0.9% Sodium Chloride Injection to ensure complete administration of the contrast.
Cardiac MRI in Adults
- Administer GADAVIST through a separate intravenous line in the contralateral arm if concomitantly providing a continuous infusion of a pharmacologic stress agent.
- Administer GADAVIST as two separate bolus injections: 0.05 mmol/kg actual body weight (equivalent to 0.05 mL/kg) at peak pharmacologic stress followed by 0.05 mmol/kg (equivalent to 0.05 mL/kg) at rest.
- Administer GADAVIST via a power injector at a flow rate of approximately 4 mL/sec and follow each injection with a 20 mL flush of 0.9% Sodium Chloride Injection at the same flow rate.
2.3 Directions for Use of Single-Dose Containers
Single-Dose Vials
- Draw GADAVIST into the syringe immediately before use.
- Pierce the rubber stopper only once.
- Discard any unused vial contents.
Single-Dose Prefilled Syringes
- Remove the tip cap from the prefilled syringe immediately before use.
- Discard any unused syringe contents.
2.4 Directions for Use of Imaging Bulk Package
- GADAVIST Imaging Bulk Package (IBP) contains many single doses for use only with an automated contrast injection system, contrast management system, or contrast media transfer set approved or cleared for use with this contrast agent in this IBP.
- See drug and device labeling for information on devices indicated for use with this IBP and techniques to help assure safe use.
- The IBP is to be used only in a room designated for radiological procedures that involve intravascular administration of a contrast agent.
- Utilize aseptic technique for penetrating the container closure of the IBP and transferring GADAVIST.
- Penetrate the container closure only one time with a suitable sterile component of the automated contrast injection system, contrast management system, or contrast media transfer set (e.g., transfer spike) approved or cleared for use with this contrast agent in this IBP.
- Once the IBP is punctured, do not remove it from the work area during the entire period of use. Storage temperature of GADAVIST IBP after the closure has been entered is 20°C to 25°C (68°F to 77°F).
- Maximum use time from puncture is 24 hours. Discard any unused portion 24 hours after puncture of the IBP.
- After the container closure is punctured, if the integrity of the IBP and the delivery system cannot be assured through direct continuous supervision, the IBP and all associated disposable components for the automated contrast injection system, contrast management system, or contrast media transfer set (e.g., transfer spike) should be discarded.
-
3 DOSAGE FORMS AND STRENGTHS
Injection: 1 mmol/mL of gadobutrol as a clear and colorless to pale yellow solution available in the following strengths:
Strength Package Type - 2 mmol/2 mL (1 mmol/mL)
- 7.5 mmol/7.5 mL (1 mmol/mL)
- 10 mmol/10 mL (1 mmol/mL)
- 15 mmol/15 mL (1 mmol/mL)
Single-Dose Vial - 7.5 mmol/7.5 mL (1 mmol/mL)
- 10 mmol/10 mL (1 mmol/mL)
- 15 mmol/15 mL (1 mmol/mL)
Single-Dose Prefilled Syringe - 30 mmol/30 mL (1 mmol/mL)
- 65 mmol/65 mL (1 mmol/mL)
Imaging Bulk Package -
4 CONTRAINDICATIONS
GADAVIST is contraindicated in patients with history of severe hypersensitivity reactions to GADAVIST [see Warnings and Precautions (5.3)].
-
5 WARNINGS AND PRECAUTIONS
5.1 Risk Associated with Intrathecal Use
Intrathecal administration of GBCAs can cause serious adverse reactions including death, coma, encephalopathy, and seizures. The safety and effectiveness of GADAVIST have not been established with intrathecal use. GADAVIST is not approved for intrathecal use [see Dosage and Administration (2.2)].
5.2 Nephrogenic Systemic Fibrosis
GBCAs increase the risk for nephrogenic systemic fibrosis (NSF) among patients with impaired elimination of the drugs. Avoid use of GADAVIST among these patients unless the diagnostic information is essential and not available with non-contrast MRI or other modalities. The GBCA-associated NSF risk appears highest for patients with chronic, severe kidney disease (GFR < 30 mL/min/1.73m2) as well as patients with acute kidney injury. The risk appears lower for patients with chronic, moderate kidney disease (GFR 30 to 59 mL/min/1.73m2) and little, if any, for patients with chronic, mild kidney disease (GFR 60 to 89 mL/min/1.73m2). NSF may result in fatal or debilitating fibrosis affecting the skin, muscle and internal organs. Report any diagnosis of NSF following GADAVIST administration to Bayer Healthcare (1-888-842-2937) or FDA (1-800-FDA-1088 or www.fda.gov/medwatch).
Screen patients for acute kidney injury and other conditions that may reduce renal function. Features of acute kidney injury consist of rapid (over hours to days) and usually reversible decrease in kidney function, commonly in the setting of surgery, severe infection, injury or drug-induced kidney toxicity. Serum creatinine levels and estimated GFR may not reliably assess renal function in the setting of acute kidney injury. For patients at risk for chronically reduced renal function (for example, age > 60 years, diabetes mellitus or chronic hypertension), estimate the GFR through laboratory testing.
Among the factors that may increase the risk for NSF are repeated or higher than recommended doses of a GBCA and degree of renal impairment at the time of exposure. Record the specific GBCA and the dose administered to a patient. For patients at highest risk for NSF, do not exceed the recommended GADAVIST dose and allow a sufficient period of time for elimination of the drug prior to re-administration. For patients receiving hemodialysis, consider the prompt initiation of hemodialysis following the administration of a GBCA in order to enhance the contrast agent's elimination [see Use in Specific Populations (8.6) and Clinical Pharmacology (12.3)]. The usefulness of hemodialysis in the prevention of NSF is unknown.
5.3 Hypersensitivity Reactions
Anaphylactic and other hypersensitivity reactions with cardiovascular, respiratory or cutaneous manifestations, ranging from mild to severe, have occurred following GADAVIST administration [see Adverse Reactions (6.1, 6.2)]. There have been reports of life-threatening and fatal outcomes from these adverse reactions. Most hypersensitivity reactions to GADAVIST have occurred within half an hour after administration. Delayed reactions can occur up to several days after administration.
- Before GADAVIST administration, assess all patients for any history of a reaction to contrast media, bronchial asthma and/or allergic disorders. These patients may have an increased risk for a hypersensitivity reaction to GADAVIST.
- GADAVIST is contraindicated in patients with history of hypersensitivity reactions to GADAVIST [see Contraindications (4)].
- Administer GADAVIST only in situations where trained personnel and therapies are promptly available for the treatment of hypersensitivity reactions, including personnel trained in resuscitation.
- Observe patients for signs and symptoms of hypersensitivity reactions during and following GADAVIST administration.
5.4 Acute Respiratory Distress Syndrome
Acute respiratory distress syndrome (ARDS) has been reported in patients administered GADAVIST and may be characterized by severe hypoxemia requiring oxygen support and mechanical ventilation. These manifestations may resemble an immediate hypersensitivity reaction with onset of respiratory distress within <30 minutes to 24 hours after GADAVIST administration. For patients demonstrating respiratory distress after GADAVIST administration, assess oxygen requirement and monitor for worsening respiratory function.
5.5 Gadolinium Retention
Gadolinium is retained for months or years in several organs. The highest concentrations (nanomoles per gram of tissue) have been identified in the bone, followed by other organs (for example, brain, skin, kidney, liver, and spleen). The duration of retention also varies by tissue and is longest in bone. Linear GBCAs cause more retention than macrocyclic GBCAs. At equivalent doses, gadolinium retention varies among the linear agents with gadodiamide causing greater retention than other linear agents such as gadoxetate disodium and gadobenate dimeglumine. Retention is lowest and similar among the macrocyclic GBCAs such as gadoterate meglumine, gadobutrol, gadoteridol, and gadopiclenol.
Consequences of gadolinium retention in the brain have not been established. Pathologic and clinical consequences of GBCA administration and retention in skin and other organs have been established in patients with impaired renal function [see Warnings and Precautions (5.2)]. There are rare reports of pathologic skin changes in patients with normal renal function. Adverse events involving multiple organ systems have been reported in patients with normal renal function without an established causal link to gadolinium retention [see Adverse Reactions (6.2)].
While clinical consequences of gadolinium retention have not been established in patients with normal renal function, certain patients might be at higher risk. These include patients requiring multiple lifetime doses, pregnant and pediatric patients, and patients with inflammatory conditions. Consider the retention characteristics of the agent when choosing a GBCA for these patients. Minimize repetitive GBCA imaging studies particularly closely spaced studies, when possible.
5.6 Acute Kidney Injury
In patients with chronic renal impairment, acute kidney injury sometimes requiring dialysis has been observed with the use of some GBCAs. Do not exceed the recommended dose; the risk of acute kidney injury may increase with higher than recommended doses.
5.7 Extravasation and Injection Site Reactions
Injection site reactions have been reported in clinical studies with GADAVIST [see Adverse Reactions (6.1)]. Extravasation into tissues during GADAVIST administration may result in moderate irritation [see Nonclinical Toxicology (13.2)]. Ensure catheter and venous patency before the injection of GADAVIST.
5.8 Overestimation of Extent of Malignant Disease in MRI of the Breast
GADAVIST MRI of the breast overestimated the histologically confirmed extent of malignancy in the diseased breast in up to 50% of the patients [see Clinical Studies (14.2)].
5.9 Low Sensitivity for Significant Arterial Stenosis
The performance of GADAVIST MRA for detecting arterial segments with significant stenosis (>50% renal, >70% supra-aortic) has not been shown to exceed 55%. Therefore, a negative MRA study alone should not be used to rule out significant stenosis [see Clinical Studies (14.3)].
-
6 ADVERSE REACTIONS
The following clinically significant adverse reactions are discussed elsewhere in labeling:
- Nephrogenic Systemic Fibrosis [see Warnings and Precautions (5.2)]
- Hypersensitivity Reactions [see Contraindications (4) and Warnings and Precautions (5.3)]
- Acute Respiratory Distress Syndrome [see Warnings and Precautions (5.4)]
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
The safety of GADAVIST was evaluated in 7,713 subjects (including 184 pediatric population, ages 0 to 17 years) who received GADAVIST in clinical trials. Approximately 52% of the subjects were male and the racial and ethnic distribution was 62% White, 28% Asian, 5% Hispanic or Latino, 2.5% Black or African American, and 2.5% other ethnic groups. The average age was 56 years (range from 1 week to 93 years).
Table 2 lists adverse reactions that occurred in ≥ 0.1% subjects who received GADAVIST.
Table 2: Adverse Reactions Reported in ≥0.1% Subjects who Received GADAVIST in Clinical Trials Adverse Reaction GADAVIST
n=7,713
Rate (%)Headache 1.7 Nausea 1.2 Dizziness 0.5 Dysgeusia 0.4 Feeling Hot 0.4 Injection site reactions 0.4 Vomiting 0.4 Rash (includes generalized, macular, papular, pruritic) 0.3 Erythema 0.2 Paresthesia 0.2 Pruritus (includes generalized) 0.2 Dyspnea 0.1 Urticaria 0.1 Adverse reactions that occurred with a frequency of < 0.1% in subjects who received GADAVIST include: hypersensitivity/anaphylactic reaction, loss of consciousness, convulsion, parosmia, tachycardia, palpitation, dry mouth, malaise and feeling cold.
Adverse Reactions in Pediatric Patients
The frequency, type, and severity of adverse reactions observed in pediatric patients from the clinical studies were similar to adverse reactions in adults [see Use in Specific Populations (8.4)].
6.2 Postmarketing Experience
The following additional adverse reactions have been identified during postmarketing use of GADAVIST or other GBCAs. Because these reactions are reported voluntarily from a population of uncertain size, it is not possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Cardiac Disorders: Cardiac arrest
Gastrointestinal Disorders: Acute pancreatitis with onset within 48 hours after GBCA administration
General Disorders and Administration Site Conditions: Fatigue, asthenia, pain syndromes, and heterogeneous clusters of symptoms in the neurological, cutaneous, and musculoskeletal systems with variable onset and duration after GBCA administration [see Warnings and Precautions (5.5)]
Immune System Disorders: Hypersensitivity reactions (anaphylactic shock, circulatory collapse, respiratory arrest, bronchospasm, cyanosis, oropharyngeal swelling, laryngeal edema, blood pressure increased, chest pain, angioedema, conjunctivitis, hyperhidrosis, cough, sneezing, burning sensation, and pallor)
Renal Disorders: Nephrogenic systemic fibrosis
Respiratory, Thoracic, and Mediastinal Disorders: Acute respiratory distress syndrome, pulmonary edema
Skin Disorders: Gadolinium associated plaques
-
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Risk Summary
GBCAs cross the placenta and result in fetal exposure. In human placental imaging studies, contrast was visualized in the placenta and fetal tissues after maternal GBCA administration. Based on animal studies, use of GBCAs during pregnancy may result in fetal gadolinium retention.
Published epidemiological studies on the association between GBCAs and adverse fetal outcomes have reported inconsistent findings and have important methodological limitations (see Data).
In animal reproduction studies, although teratogenicity was not observed, embryolethality was observed in monkeys, rabbits and rats receiving intravenous gadobutrol during organogenesis at doses 8 times and above the recommended human dose. Retardation of embryonal development was observed in rabbits and rats receiving intravenous gadobutrol during organogenesis at doses 8 and 12 times, respectively, the recommended human dose (see Data). Because of the potential risks of gadolinium to the fetus, use GADAVIST only if imaging is essential during pregnancy and cannot be delayed.
The background risk of major birth defects and miscarriage for the indicated population is unknown. All pregnancies have a background risk of birth defect, loss, or other adverse outcomes. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2% to 4% and is 15% to 20%, respectively.
Human Data
Available data regarding exposure to GBCAs during pregnancy from published epidemiological studies are not sufficient to assess the risk of adverse fetal and neonatal effects that may be associated with GBCAs. A retrospective cohort study of over 1.4 million pregnancies in Ontario, Canada, comparing pregnant women who had a GBCA MRI to pregnant women who did not have an MRI, reported a higher occurrence of stillbirths and neonatal deaths in the group receiving GBCA MRI. Limitations of this study include a lack of comparison with non-contrast MRI and lack of information about the maternal indication for MRI. Another retrospective cohort study of over 11 million pregnancies in the Medicaid database found no increased risk of fetal or neonatal death or Neonatal Intensive Care Unit admission when comparing pregnancies exposed to GBCA MRI versus non-contrast MRI. These two retrospective observational studies assessed a limited number of potential pregnancy outcomes and did not evaluate the full spectrum of potential fetal risk.
Animal Data
Gadolinium Retention
GBCAs administered to pregnant non-human primates (0.1 mmol/kg on gestational days 85 and 135) result in measurable gadolinium concentration in the offspring in bone, brain, skin, liver, kidney, and spleen for at least 7 months. GBCAs administered to pregnant mice (2 mmol/kg daily on gestational days 16 through 19) result in measurable gadolinium concentrations in the pups in bone, brain, kidney, liver, blood, muscle, and spleen at one month postnatal age.
Reproductive Toxicology
Embryolethality was observed when gadobutrol was administered intravenously to monkeys during organogenesis at doses 8 times the recommended single human dose (based on body surface area); gadobutrol was not maternally toxic or teratogenic at this dose. Embryolethality and retardation of embryonal development also occurred in pregnant rats receiving maternally toxic doses of gadobutrol (≥ 7.5 mmol/kg body weight; equivalent to 12 times the human dose based on body surface area) and in pregnant rabbits (≥ 2.5 mmol/kg body weight; equivalent to 8 times the recommended human dose based on body surface area). In rabbits, this finding occurred without evidence of pronounced maternal toxicity and with minimal placental transfer (0.01% of the administered dose detected in the fetuses). Because pregnant animals received repeated daily doses of GADAVIST, their overall exposure was significantly higher than that achieved with the standard single dose administered to humans.
8.2 Lactation
Risk Summary
There are no data on the presence of gadobutrol in human milk, the effects on the breastfed infant, or the effects on milk production. However, published lactation data on other GBCAs indicate that 0.01 to 0.04% of the maternal gadolinium dose is present in breast milk and there is limited GBCA gastrointestinal absorption in the breast-fed infant. Gadobutrol is present in rat milk (see Data). The developmental and health benefits of breastfeeding should be considered along with the mother's clinical need for GADAVIST and any potential adverse effects on the breastfed infant from GADAVIST or from the underlying maternal condition.
In lactating rats receiving 0.5 mmol/kg of intravenous [153Gd]-gadobutrol, 0.01% of the total administered radioactivity was transferred to the pup via maternal milk within 3 hours after administration, and the gastrointestinal absorption is poor (approximately 5% of the dose orally administered was excreted in the urine).
8.4 Pediatric Use
The safety and effectiveness of GADAVIST have been established in pediatric patients, including term neonates, for use with MRI to detect and visualize areas with disrupted blood brain barrier and/or abnormal vascularity of the CNS and for use in MRA to evaluate known or suspected supra-aortic or renal artery disease. Use of GADAVIST for these indications is supported by adequate and well-controlled studies in adults and by additional imaging, pharmacokinetic, and safety data from two studies (i.e., Trials 1 and 2) in a total of 182 pediatric patients aged less than 18 years, including term neonates, with CNS and non-CNS lesions. Trial 1 included 138 patients aged 2 to less than 18 years and Trial 2 included 44 patients aged less than 2 years [see Adverse Reactions (6.1), Clinical Pharmacology (12.3), and Clinical Studies (14.1, 14.3)].
The safety and effectiveness of GADAVIST have not been established in preterm neonates for any indication or in pediatric patients of any age for use with MRI to assess the presence and extent of malignant breast disease, or for use in CMRI to assess myocardial perfusion (stress, rest) and late gadolinium enhancement in patients with known or suspected coronary artery disease (CAD).
8.5 Geriatric Use
In clinical studies of GADAVIST, 1,377 patients were 65 years of age and over, while 104 patients were 80 years of age and over. No overall differences in safety or effectiveness were observed between these subjects and younger subjects, and other reported clinical experience has not identified differences between the elderly and younger patients.
This drug is known to be excreted by the kidney, and the risk of adverse reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, it may be useful to monitor renal function [see Warnings and Precautions (5.2) and Use in Specific Populations (8.6)].
8.6 Renal Impairment
In patients with renal impairment, the exposure of gadobutrol is increased compared to patients with normal renal function. This may increase the risk of adverse reactions such as NSF. Prior to administration of GADAVIST, screen all patients for renal dysfunction by obtaining a history and/or laboratory tests. For patients receiving hemodialysis, consider the prompt initiation of hemodialysis following the administration of GADAVIST in order to enhance elimination of gadobutrol [see Warnings and Precautions (5.2) and Clinical Pharmacology (12.3)].
-
10 OVERDOSAGE
In the event of an overdose with GADAVIST, the substance can be removed by hemodialysis [see Clinical Pharmacology (12.3)].
For additional overdose management recommendations, consider contacting the Poison Help line at 1-800-222-1222 or consulting a medical toxicologist.
-
11 DESCRIPTION
GADAVIST (gadobutrol) injection is a paramagnetic macrocyclic gadolinium-based contrast agent for intravenous use.
The chemical name for gadobutrol is 10–[(1SR,2RS)–2,3–dihydroxy–1–hydroxymethylpropyl]–1,4,7,10–tetraazacyclododecane–1,4,7–triacetic acid, gadolinium complex. Gadobutrol is a water-soluble, hydrophilic compound with a partition coefficient between n-butanol and buffer at pH 7.6 of 0.006, and has a molecular formula of C18H31GdN4O9 and a molecular weight of 604.72. The structural formula of gadobutrol is:
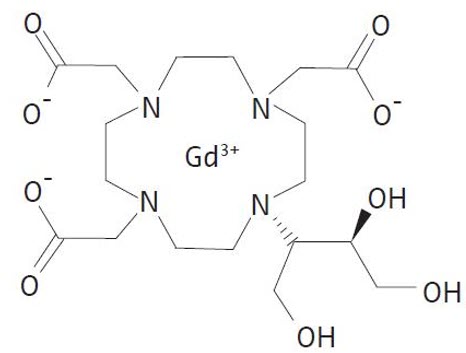
GADAVIST is a sterile, clear, colorless to pale yellow solution. Each mL contains 604.72 mg (1 mmol) of gadobutrol (containing 1 mmol of gadolinium) and the following inactive ingredients: 0.513 mg of calcobutrol sodium, 1.211 mg of trometamol, hydrochloric acid (for pH adjustment), and water for injection. GADAVIST contains no preservatives.
The main physicochemical properties of GADAVIST are listed in Table 3.
Table 3: Physicochemical Properties of GADAVIST Parameter Value Density (g/mL at 37°C) 1.3 Osmolarity at 37°C (mOsm/L solution) 1117 Osmolality at 37°C (mOsm/kg H2O) 1603 Viscosity at 37°C (mPa∙s) 4.96 pH 6.6 to 8 The thermodynamic stability constants for gadobutrol (log Ktherm and log Kcond at pH 7.4) are 21.8 and 15.3, respectively.
-
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Gadobutrol is a paramagnetic molecule (macrocyclic non-ionic complex of gadolinium) that develops a magnetic moment when placed in a magnetic field. The magnetic moment alters the relaxation rates of water protons in its vicinity in the body, leading to an increase in signal intensity (brightness) of tissues.
12.2 Pharmacodynamics
In MRI, visualization of normal and pathological tissue depends in part on variations in the radiofrequency signal intensity that occurs with:
- Differences in proton density
- Differences of the spin-lattice or longitudinal relaxation times (T1)
- Differences in the spin-spin or transverse relaxation time (T2)
When placed in a magnetic field, gadobutrol shortens the T1 and T2 relaxation times in targeted tissues. The extent to which a contrast agent can affect the relaxation rate of tissue water (1/T1 or 1/T2) is termed relaxivity (r1 or r2). The relaxivity of GBCAs is presented in Table 4.
Table 4: Relaxivity (r1) of GBCAs in Human Plasma at 1.5 T and 37°C Gadolinium-Chelate r1 (L∙mmol -1 ∙s-1) Gadobenate 6.3 Gadobutrol 5.2 Gadodiamide 4.3 Gadopiclenol 12.8 Gadoterate 3.6 Gadoteridol 4.1 Gadoxetate 6.9 Compared to 0.5 molar gadolinium-based contrast agents, the higher concentration of GADAVIST results in half the volume of administration and a more compact contrast bolus injection. At the site of imaging, the relative height and width of the time intensity curve for GADAVIST varies as a function of imaging location and multiple patient, injection, and device-specific factors.
12.3 Pharmacokinetics
After intravenous administration of 0.1 mmol/kg GADAVIST, average plasma levels of gadobutrol are 0.59 mmol/L at 2 minutes after injection and 0.3 mmol/L at 60 minutes after injection, with an AUC of 1,072 µmol∙h/L. Values for further PK parameters are given in Table 5 below.
Distribution
After intravenous administration, gadobutrol is distributed in the extracellular space. Gadobutrol does not display any particular protein binding. Following GBCA administration, gadolinium is present for months or years in brain, bone, skin, and other organs [see Warnings and Precautions (5.5)].
Elimination
The average elimination half-life (t1/2) of gadobutrol is 1.8 hours.
Metabolism
Gadobutrol is not metabolized.
Excretion
Gadobutrol is excreted in an unchanged form through the kidneys by glomerular filtration. In healthy subjects, renal clearance of gadobutrol is 1.1 to 1.7 mL/(min∙kg) and thus comparable to the renal clearance of inulin.
Within 2 hours after intravenous administration more than 50% and within 12 hours more than 90% of the given dose is eliminated via the urine. Extra-renal elimination is negligible.
Specific Populations
Geriatric Patients
A single intravenous dose of 0.1 mmol/kg GADAVIST was administered to 15 elderly and 16 non-elderly subjects. AUC was slightly higher (43%) and clearance slightly lower (31%) in elderly subjects as compared to non-elderly subjects [see Use in Specific Populations (8.5)].
Pediatric Patients
The pharmacokinetics of gadobutrol were evaluated in a total of 173 pediatric patients aged less than 18 years (including term neonates) who received a single intravenous dose of 0.1 mmol/kg of GADAVIST. Table 5 shows the pharmacokinetic parameters of gadobutrol by age group. The pharmacokinetic profile of gadobutrol in pediatric patients is similar to that in adults, resulting in similar values for AUC, body weight normalized plasma clearance, as well as elimination half-life. Approximately 99% (median value) of the dose was recovered in urine within 6 hours (this information was derived from the 2 to less than 18 year-old age group).
Table 5: Pharmacokinetics by Age Group (Median [Range]) 0 to < 2 years
N=432 to 6 years
N=457 to 11 years
N=3912 to < 18 years
N=46Adults
N=93AUC (µmol∙h/L) 781
[513, 1891]846
[412, 1331]1025
[623, 2285]1237
[946, 2211]1072
[667, 1992]CL (L/h/kg) 0.128
[0.053, 0.195]0.119
[0.080, 0.215]0.099
[0.043, 0.165]0.081
[0.046, 0.103]0.094
[0.051, 0.150]t1/2 (h) 2.91
[1.60, 12.4]1.91
[1.04, 2.70]1.66
[0.91, 2.71]1.68
[1.31, 2.48]1.80
[1.20, 6.55]C20 (µmol/L) 367
[280, 427]421
[369, 673]462
[392, 760]511
[387, 1077]441
[281, 829]Male and Female Patients
Gender has no clinically relevant effect on the pharmacokinetics of gadobutrol.
Patients with Renal Impairment
In patients with renal impairment, the serum half-life of gadobutrol is prolonged and correlated with the reduction in creatinine clearance.
After intravenous injection of GADAVIST 0.1 mmol/kg, the elimination half-life was 5.8 ± 2.4 hours in patients with mild to moderate renal impairment (80 > CLCR > 30 mL/min) and 17.6 ± 6.2 hours in patients with severe renal impairment not on dialysis (CLCR < 30 mL/min). The average AUC of gadobutrol in patients with normal renal function was 1.1 ± 0.1 mmol∙h/L, compared to 4.0 ± 1.8 mmol∙h/L in patients with mild to moderate renal impairment and 11.5 ± 4.3 mmol∙h/L in patients with severe renal impairment.
Complete recovery in the urine was seen in patients with mild or moderate renal impairment within 72 hours. In patients with severely impaired renal function about 80% of the administered dose was recovered in the urine within 5 days.
For patients receiving hemodialysis, 68% of gadobutrol is removed from the body after the first dialysis, 94% after the second dialysis, and 98% after the third dialysis session [see Warnings and Precautions (5.2) and Use in Specific Populations (8.6)].
-
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis
No carcinogenicity studies of gadobutrol have been conducted.
Mutagenesis
Gadobutrol was not mutagenic in in vitro reverse mutation tests in bacteria, in the HGPRT (hypoxanthine-guanine phosphoribosyl transferase) test using cultured Chinese hamster V79 cells, or in chromosome aberration tests in human peripheral blood lymphocytes, and was negative in an in vivo micronucleus test in mice after intravenous injection of 0.5 mmol/kg.
Impairment of Fertility
Gadobutrol had no effect on fertility and general reproductive performance of male and female rats when given in doses 12.2 times the human equivalent dose (based on body surface area).
13.2 Animal Toxicology and/or Pharmacology
Local intolerance reactions, including moderate irritation associated with infiltration of inflammatory cells was observed after paravenous administration to rabbits, suggesting the possibility of occurrence of local irritation if the contrast medium leaks around veins in a clinical setting [see Warnings and Precautions (5.7)].
-
14 CLINICAL STUDIES
14.1 MRI of the CNS
The effectiveness of GADAVIST for the visualization of lesions was evaluated in two clinical trials (i.e., Studies 1 and 2) in patients who were referred for MRI of the CNS with contrast. In both studies, patients underwent a baseline, pre-contrast MRI prior to administration of GADAVIST at a dose of 0.1 mmol/kg, followed by a post-contrast MRI. In Study 1, patients also underwent an MRI before and after the administration of gadoteridol. The studies were designed to demonstrate superiority of GADAVIST MRI to non-contrast MRI for lesion visualization. For both studies, pre-contrast and pre-plus-post contrast images (paired images) were independently evaluated by three readers for contrast enhancement and border delineation using a scale of 1 to 4, and for internal morphology using a scale of 1 to 3 (Table 6). Lesion counting was also performed to demonstrate non-inferiority of paired GADAVIST image sets to pre-contrast MRI. Readers were blinded to clinical information.
Table 6: Primary Endpoint Visualization Scoring System Score Visualization Characteristics Contrast Enhancement Border Delineation Internal Morphology 1 None None Poorly visible 2 Weak Moderate Moderately visible 3 Clear Clear but incomplete Sufficiently visible 4 Clear and bright Clear and complete N/A A total of 657 patients were evaluated. The average age was 49 years (range 18 to 85 years) and 42% were male. The racial and ethnic representations were 39% White, 4% Black or African American, 16% Hispanic or Latino, 38% Asian, and 3% of other ethnic groups.
Table 7 shows a comparison of visualization results between paired images and pre-contrast images. GADAVIST provided a statistically significant improvement for each of the three lesion visualization parameters when averaged across three independent readers for each study.
Table 7: Visualization Endpoint Results of Central Nervous System Adult MRI Studies with 0.1 mmol/kg GADAVIST Endpoint Study 1
N=336Study 2
N=321Pre-contrast Paired Difference* Pre-contrast Paired Difference - * Difference of means = (paired mean) – (pre-contrast mean)
- † p<0.001
- ‡ Did not meet noninferiority margin of -0.35
- § Met noninferiority margin of -0.35
Contrast Enhancement 0.97 2.26 1.29† 0.93 2.86 1.94† Border Delineation 1.98 2.58 0.60† 1.92 2.94 1.02† Internal Morphology 1.32 1.93 0.60† 1.57 2.35 0.78† Average # Lesions Detected 8.08 8.25 0.17‡ 2.65 2.97 0.32§ Performances of GADAVIST and gadoteridol for visualization parameters were similar. Regarding the number of lesions detected, Study 2 met the prespecified noninferiority margin of -0.35 for paired read versus pre-contrast read while in Study 1, GADAVIST and gadoteridol did not.
For the visualization endpoints contrast enhancement, border delineation, and internal morphology, the percentage of patients scoring higher for paired images compared to pre-contrast images ranged from 93% to 99% for Study 1, and 95% to 97% for Study 2. For both studies, the mean number of lesions detected on paired images exceeded that of the pre-contrast images; 37% for Study 1 and 24% for Study 2. There were 29% and 11% of patients in which the pre-contrast images detected more lesions for Study 1 and Study 2, respectively.
The percentage of patients whose average reader mean score changed by ≤ 0, up to 1, up to 2, and ≥ 2 scoring categories presented in Table 6 is shown in Table 8. The categorical improvement of (≤ 0) represents higher (< 0) or identical (= 0) scores for the pre-contrast read, the categories with scores > 0 represent the magnitude of improvement seen for the paired read.
Table 8: Primary Endpoint Visualization Categorical Improvement for Average Reader Study 1
N=336Study 2
N=321Endpoint Categorical Improvement
(Paired – Pre-Contrast) %Categorical Improvement
(Paired – Pre-Contrast) %≤ 0 > 0 – < 1 1 – < 2 ≥ 2 ≤ 0 > 0 – < 1 1 – < 2 ≥ 2 Contrast Enhancement 1 30 55 13 3 6 34 57 Border Delineation 7 73 18 1 5 38 51 5 Internal Morphology 4 79 17 0 5 61 33 1 For both studies, the improvement of visualization endpoints in paired GADAVIST images compared to pre-contrast images resulted in improved assessment of normal and abnormal CNS anatomy.
14.2 MRI of the Breast
The effectiveness of GADAVIST for the ability to assess the presence and extent of malignant breast disease was evaluated in two identical clinical trials (i.e., Studies 3 and 4) in patients with recently diagnosed breast cancer prior to surgery. Patients underwent non-contrast breast MRI (BMR) prior to GADAVIST (0.1 mmol/kg) breast MRI. BMR images and GADAVIST BMR (combined contrast plus non-contrast) images were independently evaluated in each study by three readers blinded to clinical information. In separate reading sessions the BMR images and GADAVIST BMR images were also interpreted together with X-ray mammography images (XRM).
A total of 787 patients were evaluated: Study 3 enrolled 390 female patients with an average age of 56 years and racial distribution of 74% White, 25% Asian, 0.5% Black or African American, and 0.5% other; Study 4 enrolled 396 female patients and 1 male patient with an average age of 57 years and racial distribution of 71% White, 24% Asian, 3% Black or African American, and 2% other.
The readers assessed 5 regions per breast for the presence of malignancy using each reading modality. The readings were compared to an independent standard of truth (SoT) consisting of histopathology for all regions where excisions were made and tissue evaluated. XRM plus ultrasound was used for all other regions.
The assessment of malignant disease was performed using a region based within-subject sensitivity. Sensitivity for each reading modality was defined as the mean of the percentage of malignant breast regions correctly interpreted for each subject. The within-subject sensitivity of GADAVIST BMR was superior to that of BMR. The lower bound of the 95% Confidence Interval (CI) for the difference in within-subject sensitivity ranged from 19% to 42% for Study 3 and from 12% to 27% for Study 4. The within-subject sensitivity for GADAVIST BMR and BMR as well as for GADAVIST BMR plus XRM and BMR plus XRM is presented in Table 9.
Table 9: Sensitivity of GADAVIST BMR for Detection of Malignant Breast Disease Study 3 Study 4 Sensitivity (%)
N=388 PatientsSensitivity (%)
N=390 PatientsReader BMR BMR
+
XRMGADAVIST
BMRGADAVIST
BMR
+XRMReader BMR BMR
+
XRMGADAVIST
BMRGADAVIST
BMR
+XRM1 37 71 83 84 4 73 83 87 90 2 49 76 80 83 5 57 81 89 90 3 63 75 87 87 6 55 80 86 88 Specificity was defined as the percentage of non-malignant breasts correctly identified as non-malignant. The lower limit of the 95% confidence interval for specificity of GADAVIST BMR was greater than 80% for 5 of 6 readers. (Table 10)
Table 10: Specificity of GADAVIST BMR in Non-Malignant Breasts Study 3 Study 4 Specificity (%)
N=372 PatientsSpecificity (%)
N=367 PatientsReader GADAVIST
BMRLower Limit
95% CIReader GADAVIST
BMRLower Limit
95% CI1 86 82 4 92 89 2 95 93 5 84 80 3 89 85 6 83 79 Three additional readers in each study read XRM alone. For these readers over both studies, sensitivity ranged from 68% to 73% and specificity in non-malignant breasts ranged from 86% to 94%.
In breasts with malignancy, a false positive detection rate was calculated as the percentage of subjects for which the readers assessed a region as malignant which could not be verified by SoT. The false positive detection rates for GADAVIST BMR ranged from 39% to 53% (95% CI Upper Bounds ranged from 44% to 58%).
14.3 MRA
The effectiveness of GADAVIST for the ability to evaluate known or suspected supra-aortic or renal artery disease was evaluated in two clinical trials (i.e., Studies 5 and 6). Study 5 enrolled patients with known or suspected disease of the supra-aortic arteries (for evaluation up to but excluding the basilar artery), and Study 6 enrolled patients with known or suspected disease of the renal arteries. In both studies, non-contrast, 2D time-of-flight (ToF) magnetic resonance angiography (MRA) was performed prior to GADAVIST MRA using a single intravenous injection of 0.1 mmol/kg. The injection rate of 1.5 mL/second was selected to extend the injection duration to at least half of the imaging duration. Imaging was performed with parallel-channel, 1.5T MRI devices and an automatic bolus tracking technique to trigger the image acquisition following GADAVIST administration using elliptically encoded, T1-weighted, 3D gradient-echo image acquisition and single breath hold. Three central readers blinded to clinical information interpreted the ToF and GADAVIST MRA images. Three additional central readers interpreted separately acquired computed tomographic angiography (CTA) images, which were used as the standard of reference (SoR) in each study.
A total of 749 patients were evaluated. The 457 patients in Study 5 had an average age of 68 years (range 25 to 93 years) and were 64% male with a racial distribution of 80% White, 28% Black or African American, and 16% Asian. The 292 patients in Study 6 had an average age of 55 years (range 18 to 88 years) and were 54% male with a racial distribution of 68% White, 7% Black or African American, and 22% Asian.
Efficacy was evaluated based on anatomical visualization and performance for distinguishing between normal and abnormal anatomy. The visualization metric depended on whether readers selected, "Yes, it can be visualized along its entire length..." when responding to the question, "Is this segment assessable?" Twenty-one segments in Study 5 and six segments in Study 6 were presented per subject to each reader. The performance metrics, sensitivity and specificity, depended on digital caliper-based quantitation of arterial narrowing in visualized, non-occluded, abnormal-appearing segments. Significant stenosis was defined as at least 70% in Study 5 and 50% in Study 6. Performance of GADAVIST MRA compared to ToF MRA was calculated using an imputation method for non-visualized segments by assigning them as a 50% match with SoR and a 50% mismatch. Performance of GADAVIST MRA compared to a pre-specified threshold of 50% was calculated after excluding non-visualized segments. Measurement variability and visualization of accessory renal arteries was also evaluated.
Results were analyzed for each of the three central readers.
Table 11: Visualization, Sensitivity, Specificity STUDY 5: SUPRA-AORTIC ARTERIES (457 patients)
Performance at the segment level
9597* segments of which 158* were positive for stenosis by SoR†VISUALIZATION (%) SENSITIVITY (%) SPECIFICITY (%) READER GAD
MRAToF
MRAGAD − ToF
(CI‡)GAD
MRAToF
MRAGAD − ToF
(CI§)GAD
MRAToF
MRAGAD − ToF
(CI§)- * Number of segments varied between readers; number for majority-reader shown.
- † Standard of Reference based on aggregate interpretation of three central CTA readers.
- ‡ 95.1/95% (Study 5/6) confidence interval for two-sided comparison.
- § 90.1/90% (Study 5/6) confidence interval for one-sided comparison against non-inferiority margin of -7.5.
1 88 24 64
(61, 67)60 54 6
(-4, 14)92 62 30
(29, 32)2 95 75 20
(18, 21)60 54 6
(-3, 14)95 85 10
(9, 11)3 97 82 15
(13, 17)58 55 3
(-4, 11)97 89 8
(7, 9)STUDY 6: RENAL ARTERIES (292 patients)
Performance at the segment level
1752* segments of which 133* were positive for stenosis by SoR†4 98 82 16
(13, 20)52 51 1
(-9, 11)94 83 11
(9, 14)5 96 72 24
(21, 28)54 39 15
(6, 24)95 85 10
(8, 12)6 96 78 17
(14, 21)53 50 3
(-6, 12)94 81 13
(11, 16)GAD MRA = Post-contrast GADAVIST Magnetic Resonance Angiography, ToF = Non-contrast 2D-Time of Flight.
For all three supra-aortic artery readers in Study 5, the lower bound of confidence for the sensitivity of GADAVIST MRA did not exceed 54%. For all three renal artery readers in Study 6, the lower bound of confidence for the sensitivity of GADAVIST MRA did not exceed 46%.
Measurement Variability
For both MRA and CTA, readers varied in the quantity of narrowing they assigned to the same arterial segments. Table 12 shows the percentage of patients in whom the measurement range was 30% or greater for the left or right internal carotid and proximal renal artery segments. There were approximately four measurements per patient segment, one from the site and three central readers. Measurement variability was high for both CTA and MRA, but numerically lower for GADAVIST compared to non-contrast ToF MRA.
Table 12: Percent of Patients with Range ≥ 30%, ≥ 50%, ≥ 70% for Measurement of Stenoses and Normal Vessel Diameters Internal Carotid Proximal Main Renal N ≥ 30% ≥ 50% ≥ 70% N ≥ 30% ≥ 50% ≥ 70% CTA 456 40 11 4 292 59 33 9 ToF MRA 443 55 22 9 270 44 22 9 GADAVIST MRA 454 47 13 4 286 34 14 4 Visualization of Accessory Renal Arteries for Surgical Planning and Renal Donor Evaluation (Study 6 only)
Of 1,752 main arteries visualized by the central CTA readers, 266 (15%) were also associated with positive visualization of at least one accessory (duplicate) artery. With the central MRA readers, the comparable rates were 232 of 1752 (13%) for GADAVIST MRA compared to 53 of 1,752 (3%) for ToF MRA.
14.4 Cardiac MRI
The effectiveness of GADAVIST for detection of coronary artery disease (CAD) was evaluated in two multi-center, open-label clinical trials (i.e., Studies 7 and 8) in adult patients with known or suspected CAD. Patients were excluded from study if they had a history of coronary artery bypass grafting, or if it was known in advance that they were unable to hold their breath, or had atrial fibrillation or other arrhythmia likely to prevent electrocardiogram-gated CMRI.
A total of 764 patients were evaluated. The 376 patients in Study 7 had an average age of 59 years (range 20 to 84 years) and were 69% male with a racial distribution of 74% White, 1% Black or African American, and 25% Asian. The 388 patients in Study 8 had an average age of 59 years (range 23 to 82 years) and were 61% male with a racial distribution of 67% White, 17% Black or African American, and 12% Asian.
All subjects underwent dynamic first-pass GADAVIST imaging during vasodilator stress, followed ~10 minutes later by dynamic first-pass GADAVIST imaging at rest, followed ~5 minutes later with imaging during a period of gradual GADAVIST washout from the myocardium (late gadolinium enhancement, LGE). Imaging was performed on 1.5 T or 3.0 T MRI devices equipped with multichannel surface coils to support accelerated acquisitions with parallel imaging, T1-weighted, 2D gradient-echo, dynamic acquisition of perfusion with at least 3 slices per heartbeat. GADAVIST was administered intravenously at a rate of ~4 mL/second as two separate bolus injections (0.05 mmol/kg each), the first at peak pharmacologic stress (~3 minutes after start of ongoing adenosine infusion, or immediately after completion of regadenoson administration, at approved doses). No additional GADAVIST was administered for LGE imaging.
Images were read by three independent readers blinded to clinical information. Reader detection of CAD depended on visually detecting defective perfusion or scar on GADAVIST CMRI (stress, rest, LGE) imaging. Quantitative coronary angiography (QCA) was used to measure intraluminal narrowing and served as the standard of reference (SoR). Computed tomographic angiography (CTA) was used as the SoR if disease could be unequivocally excluded, and no coronary angiography (CA) was available. The left ventricular myocardium was divided into six regions. Readers provided per-region (CMRI, CTA) and per-artery (QCA) interpretations for each subject. Subject-level endpoints reflected each subject's most abnormal localized finding.
The sensitivity results for GADAVIST CMRI to detect CAD defined as either maximum stenosis ≥ 50% or ≥ 70% by QCA are presented in Table 13. For each reader, sensitivity of GADAVIST CMRI larger than 60% can be concluded if the lower 95% confidence limit of the sensitivity estimate exceeds the pre-specified threshold of 60%.
Table 13: Sensitivity (%) of GADAVIST-CMRI for Detection of CAD in Patients with Maximum Stenosis* of ≥ 50% and ≥ 70% Study 7 Study 8 ≥ 50%
N=141≥ 70%
N=108≥ 50%
N=150≥ 70%
N=105- * Stenosis determined by Quantitative Coronary Angiography (QCA)
- † CMRI images were assessed by six independent blinded readers, three in each study.
- ‡ The bolded value represents the lower limit of the 95% confidence interval, which is compared to a pre-specified threshold of 60% for evaluation of sensitivity.
Reader 1† 77 (69, 83)‡ 90 (83, 95) 65 (57, 72) 77 (68, 85) Reader 2† 65 (57, 73) 80 (71, 87) 56 (48, 64) 71 (62, 80) Reader 3† 65 (56, 72) 79 (70, 86) 61 (53, 69) 76 (67, 84) The specificity results for GADAVIST CMRI to detect CAD defined as either maximum stenosis ≥ 50% or ≥ 70% by QCA are presented in Table 14. For each reader, specificity of GADAVIST CMRI larger than 55% can be concluded if the lower 95% confidence limit of the specificity estimate exceeds the pre-specified threshold of 55%.
Table 14: Specificity (%) of GADAVIST CMRI for Exclusion of CAD in Patients with Maximum Stenosis* of ≥ 50% and ≥ 70% Study 7 Study 8 ≥ 50%
N=235≥ 70%
N=268≥ 50%
N=239≥ 70%
N=283- * Stenosis determined by Quantitative Coronary Angiography (QCA)
- † CMRI images were assessed by six independent blinded readers, three in each study.
- ‡ The bolded value represents the lower limit of the 95% confidence interval, which is compared to a pre-specified threshold of 55% for evaluation of specificity.
Reader 1† 85 (80, 89)‡ 83 (78, 87) 85 (80, 90) 82 (77, 86) Reader 2† 92 (88, 95) 91 (87, 94) 89 (84, 92) 87 (83, 91) Reader 3† 92 (88, 95) 91 (87, 94) 90 (85, 93) 87 (82, 91) In Study 7, among the 33 patients with maximum stenosis by QCA between 50% and <70%, the proportion of GADAVIST-CMRI positive detections of CAD ranged from 15% to 33%. In Study 8, among the 45 patients with maximum stenosis by QCA between 50% and < 70%, the proportion of GADAVIST-CMRI positive detections of CAD ranged from 20% to 35%. The results of GADAVIST-CMRI reads to detect CAD in patients with maximum stenosis between 50% and < 70% are summarized in Table 15.
Table 15: GADAVIST-CMRI Detection of CAD in Patients with Maximum Stenosis* between 50% and < 70% Study 7 (n=33) Study 8 (n=45) GADAVIST-CMRI positive GADAVIST-CMRI positive - * Stenosis determined by Quantitative Coronary Angiography (QCA).
- † CMRI images were assessed by six independent blinded readers, three in each study.
Reader 1† 11 (33%) 16 (35%) Reader 2† 5 (15%) 9 (20%) Reader 3† 6 (18%) 12 (26%) Left Mainstem Stenosis
The studies did not include sufficient numbers of subjects to characterize the performance of GADAVIST CMRI for detection of left mainstem stenosis (LMS), a subgroup at high risk from false negative reads. In Studies 7 and 8, only three subjects had isolated LMS stenosis >50%. In two of the three cases, the CMRI was interpreted as normal by at least two of the three readers (false negative). Sixteen subjects had LMS stenosis >50% (including subjects with isolated LMS stenosis and subjects with LMS stenosis in addition to stenoses elsewhere). In five of these sixteen cases, the CMR was interpreted as normal by at least two of the three readers (false negative).
-
16 HOW SUPPLIED/STORAGE AND HANDLING
How Supplied
GADAVIST (gadobutrol) injection is supplied at a concentration of 1 mmol/mL of gadobutrol as a clear and colorless to pale yellow solution available in the following strengths:
Strength Package Type Sale Unit NDC 2 mmol/2 mL
(1 mmol/mL)Single-Dose Vial Boxes of 5 cartons containing 3 vials each (15 total) 50419-325-37 7.5 mmol/7.5 mL
(1 mmol/mL)Single-Dose Vial Boxes of 2 cartons containing 10 vials each (20 total) 50419-325-11 10 mmol/10 mL
(1 mmol/mL)Single-Dose Vial Boxes of 2 cartons containing 10 vials each (20 total) 50419-325-12 15 mmol/15 mL
(1 mmol/mL)Single-Dose Vial Boxes of 2 cartons containing 10 vials each (20 total) 50419-325-13 7.5 mmol/7.5 mL
(1 mmol/mL)Single-Dose Prefilled Syringe Boxes of 5 syringes 50419-325-27 10 mmol/10 mL
(1 mmol/mL)Single-Dose Prefilled Syringe Boxes of 5 syringes 50419-325-28 15 mmol/15 mL
(1 mmol/mL)Single-Dose Prefilled Syringe Boxes of 5 syringes 50419-325-29 30 mmol/30 mL
(1 mmol/mL)Imaging Bulk Package Boxes of 2 cartons containing 5 bottles each (10 total) 50419-325-18 65 mmol/65 mL
(1 mmol/mL)Imaging Bulk Package Boxes of 10 bottles 50419-325-19 Storage and Handling
Store at 25°C (77°F); excursions permitted to 15°C to 30°C (59°F to 86°F) [see USP Controlled Room Temperature].
If solidification occurs due to cold exposure, bring GADAVIST to room temperature before use and inspect to ensure that the solution is clear and colorless to pale yellow.
-
17 PATIENT COUNSELING INFORMATION
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
Nephrogenic Systemic Fibrosis
Inform the patient that GADAVIST may increase the risk of NSF among patients with impaired elimination of the drug and that NSF may result in fatal or debilitating fibrosis affecting the skin, muscle, and internal organs.
Instruct the patients to contact their physician if they develop signs or symptoms of NSF following GADAVIST administration, such as burning, itching, swelling, scaling, hardening and tightening of the skin; red or dark patches on the skin; stiffness in joints with trouble moving, bending or straightening the arms, hands, legs or feet; pain in the hip bones or ribs; or muscle weakness [see Warnings and Precautions (5.2)].
Acute Respiratory Distress Syndrome
Advise patients that acute respiratory distress syndrome (ARDS) has occurred with GADAVIST. Inform patients on the symptoms of the observed ARDS cases, and instruct patients to inform their healthcare provider if they experience these symptoms [see Warnings and Precautions (5.4)].
Gadolinium Retention
Advise patients that gadolinium is retained for months or years in brain, bone, skin, and other organs following GADAVIST administration even in patients with normal renal function. The clinical consequences of retention are unknown. Retention depends on multiple factors and is greater following administration of linear GBCAs than following administration of macrocyclic GBCAs [see Warnings and Precautions (5.5)].
Pregnancy
Advise pregnant women of the potential risk of fetal exposure to GADAVIST [see Use in Specific Populations (8.1)].
- SPL UNCLASSIFIED SECTION
-
MEDICATION GUIDE
MEDICATION GUIDE
GADAVIST (gad-a-vist)
(gadobutrol)
Injection, for intravenous useThis Medication Guide has been approved by the U.S. Food and Drug Administration. Revised: 2/2026 What is the most important information I should know about GADAVIST? - GBCAs like GADAVIST may cause serious side effects including death, coma, encephalopathy, and seizures when it is given intrathecally (injection given into the spinal canal). It is not known if GADAVIST is safe and effective with intrathecal use. GADAVIST is not approved for this use.
- GADAVIST contains a metal called gadolinium. Small amounts of gadolinium can stay in your body including the brain, bones, skin and other parts of your body for a long time (several months to years).
- It is not known how gadolinium may affect you, but so far, studies have not found harmful effects in patients with normal kidneys.
- Rarely, patients have reported pains, tiredness, and skin, muscle or bone ailments for a long time, but these symptoms have not been directly linked to gadolinium.
- There are different GBCAs that can be used for your MRI exam. The amount of gadolinium that stays in the body is different for different gadolinium medicines. Gadolinium stays in the body more after gadodiamide than after gadoxetate disodium or gadobenate dimeglumine. Gadolinium stays in the body the least after gadoterate meglumine, gadobutrol, gadoteridol, and gadopiclenol.
- People who get many doses of gadolinium medicines, women who are pregnant and young children may be at increased risk from gadolinium staying in the body.
- Some people with kidney problems who get gadolinium medicines can develop a condition with severe thickening of the skin, muscles and other organs in the body (nephrogenic systemic fibrosis). Your healthcare provider should screen you to see how well your kidneys are working before you receive GADAVIST.
What is GADAVIST? - GADAVIST is a prescription medicine called a gadolinium-based contrast agent (GBCA). GADAVIST, like other GBCAs, is injected into your vein and used with a magnetic resonance imaging (MRI) scanner.
- An MRI exam with a GBCA, including GADAVIST, helps your doctor to see problems better than an MRI exam without a GBCA.
- Your doctor has reviewed your medical records and has determined that you would benefit from using a GBCA with your MRI exam.
Do not receive GADAVIST if you have had a severe allergic reaction to GADAVIST. Before receiving GADAVIST, tell your healthcare provider about all your medical conditions, including if you: - have had any MRI procedures in the past where you received a GBCA. Your healthcare provider may ask you for more information including the dates of these MRI procedures.
- are pregnant or plan to become pregnant. It is not known if GADAVIST can harm your unborn baby. Talk to your healthcare provider about the possible risks to an unborn baby if a GBCA such as GADAVIST is received during pregnancy.
- have kidney problems, diabetes, or high blood pressure.
- have had an allergic reaction to dyes (contrast agents) including GBCAs.
What are the possible side effects of GADAVIST? - See "What is the most important information I should know about GADAVIST?"
- Allergic reactions. GADAVIST can cause allergic reactions that can sometimes be serious. Your healthcare provider will monitor you closely for symptoms of an allergic reaction.
- A serious lung problem called acute respiratory distress syndrome (ARDS). Call your healthcare provider right away if you have shortness of breath with or without a fever, trouble breathing, or a fast rate of breathing after receiving GADAVIST.
These are not all the possible side effects of GADAVIST.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.General information about the safe and effective use of GADAVIST.
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. You can ask your healthcare provider for information about GADAVIST that is written for health professionals.What are the ingredients in GADAVIST?
Active ingredient: gadobutrol
Inactive ingredients: calcobutrol sodium, trometamol, hydrochloric acid (for pH adjustment) and water for injection
Manufactured for Bayer HealthCare Pharmaceuticals Inc.
Manufactured in Germany © 2011
Bayer HealthCare Pharmaceuticals Inc. All rights reserved.
For more information, go to www.gadavist.com or call 1-888-842-2937. -
PACKAGE/LABEL PRINCIPAL DISPLAY PANEL
Gadavist Imaging Bulk Pack 65 mL Label
Dose: 0.1 mL/kg
NDC: 50419-325-09
65 mLRx only
sterile solution
Gadavist
sterile solution
Gadavist
(gadobutrol) injection
1 mmol/mLFor Intravenous Administration.
Multiple-Dose container.Discard unused portion 24 hours after initial puncture.
-
INGREDIENTS AND APPEARANCE
GADAVIST
gadobutrol injectionProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 50419-325 Route of Administration INTRAVENOUS Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength GADOBUTROL (UNII: 1BJ477IO2L) (GADOLINIUM CATION (3+) - UNII:AZV954TZ9N) GADOBUTROL 604.72 mg in 1 mL Inactive Ingredients Ingredient Name Strength TROMETHAMINE (UNII: 023C2WHX2V) HYDROCHLORIC ACID (UNII: QTT17582CB) WATER (UNII: 059QF0KO0R) Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 50419-325-18 2 in 1 BOX 03/15/2011 1 5 in 1 CARTON 1 30 mL in 1 BOTTLE, GLASS; Type 0: Not a Combination Product 2 NDC: 50419-325-19 10 in 1 BOX 03/15/2011 2 65 mL in 1 BOTTLE, GLASS; Type 0: Not a Combination Product 3 NDC: 50419-325-73 30 mL in 1 BOTTLE, GLASS; Type 0: Not a Combination Product 02/11/2021 4 NDC: 50419-325-74 65 mL in 1 BOTTLE, GLASS; Type 0: Not a Combination Product 02/11/2021 Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date NDA NDA201277 03/14/2011 Labeler - Bayer HealthCare Pharmaceuticals Inc. (005436809) Establishment Name Address ID/FEI Business Operations Bayer AG 315097875 ANALYSIS(50419-325) , MANUFACTURE(50419-325) , API MANUFACTURE(50419-325) , STERILIZE(50419-325) , PACK(50419-325) , LABEL(50419-325)
Trademark Results [Gadavist]
Mark Image Registration | Serial | Company Trademark Application Date |
|---|---|
 GADAVIST 85239263 4132896 Live/Registered |
BAYER INTELLECTUAL PROPERTY GMBH 2011-02-10 |
© 2026 FDA.report
This site is not affiliated with or endorsed by the FDA.
