LAMOTRIGINE tablet, extended release
Lamotrigine by
Drug Labeling and Warnings
Lamotrigine by is a Prescription medication manufactured, distributed, or labeled by Wockhardt Limited. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
-
HIGHLIGHTS OF PRESCRIBING INFORMATION
These highlights do not include all the information needed to use lamotrigine extended-release tablets safely and effectively. See full prescribing information for lamotrigine extended-release tablets.
Lamotrigine Extended-Release Tablets
Initial U.S. Approval: 1994
WARNING: SERIOUS SKIN RASHES
See full prescribing information for complete boxed warning.
Cases of life-threatening serious rashes, including Stevens-Johnson syndrome and toxic epidermal necrolysis, and/or rash-related death have been caused by lamotrigine. The rate of serious rash is greater in pediatric patients than in adults. Additional factors that may increase the risk of rash include (5.1):
WARNING
Suicidality and Antidepressant Drugs
- coadministration with valproate
- exceeding recommended initial dose of lamotrigine extended-release tablets
- exceeding recommended dose escalation of lamotrigine extended-release tablets.
Benign rashes are also caused by lamotrigine; however, it is not possible to predict which rashes will prove to be serious or life threatening. Lamotrigine extended-release tablets should be discontinued at the first sign of rash, unless the rash is clearly not drug related. (5.1)
RECENT MAJOR CHANGES
Warnings and Precautions, Multiorgan
Hypersensitivity and Organ Failure (5.2) August 2011
INDICATIONS AND USAGE
Lamotrigine extended-release tablet is an antiepileptic drug (AED) indicated for:
- adjunctive therapy for partial onset seizures with or without secondary generalization in patients ≥13 years of age. (1.1)
- Limitation of use: Safety and effectiveness in patients less than 13 years of age have not been established. (1.3)
DOSAGE AND ADMINISTRATION
- Do not exceed the recommended initial dosage and subsequent dose escalation. (2.1)
- Initiation of adjunctive therapy requires slow titration dependent on concomitant AEDs; the prescriber must refer to the appropriate algorithm in Dosage and Administration (2.2)
● Adjunct therapy target therapeutic dose range is 200 to 600 mg daily and is dependent on concomitant AEDs. (2.2)
- Conversion from immediate-release lamotrigine to lamotrigine extended-release tablet: The initial dose of lamotrigine extended-release tablets should match the total daily dose of the immediate-release lamotrigine. Patients should be closely monitored for seizure control after conversion. (2.4)
- Do not restart lamotrigine extended-release tablets in patients who discontinued due to rash unless the potential benefits clearly outweigh the risks. (2.1, 5.1)
- Adjustments to maintenance doses are likely in patients starting or stopping estrogen-containing oral contraceptives. (2.1, 5.7)
- Discontinuation: Taper over a period of at least 2 weeks (approximately 50% dose reduction per week). (2.1, 5.8)
DOSAGE FORMS AND STRENGTHS
CONTRAINDICATIONS
Hypersensitivity to the drug or its ingredients. (Boxed Warning, 4)
WARNINGS AND PRECAUTIONS
- Life-threatening serious rash and/or rash-related death: Discontinue at the first sign of rash, unless the rash is clearly not drug related. (Boxed Warning, 5.1)
- Fatal or life-threatening hypersensitivity reaction: Multiorgan hypersensitivity reactions, also known as Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS), may be fatal or life threatening. Early signs may include rash, fever, and lymphadenopathy. These reactions may be associated with other organ involvement, such as hepatitis, hepatic failure, blood dyscrasias, or acute multiorgan failure. Lamotrigine extended-release tablets should be discontinued if alternate etiology for this reaction is not found. (5.2)
- Blood dyscrasias (e.g., neutropenia, thrombocytopenia, pancytopenia): May occur, either with or without an associated hypersensitivity syndrome. Monitor for signs of anemia, unexpected infection, or bleeding. (5.3)
- Suicidal behavior and ideation: Monitor for suicidal thoughts or behaviors. (5.4)
- Aseptic meningitis: Monitor for signs of meningitis. (5.5)
- Medication errors due to product name confusion: Strongly advise patients to visually inspect tablets to verify the received drug is correct. (3.2, 5.6, 16, 17.10)
ADVERSE REACTIONS
- Most common adverse reactions with use as adjunctive therapy (treatment difference between lamotrigine extended-release tablets and placebo ≥4%) are dizziness, tremor/intention tremor, vomiting, and diplopia. (6.1)
To report SUSPECTED ADVERSE REACTIONS, contact Wockhardt USA LLC. at 1-800-346-6854 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
DRUG INTERACTIONS
- Valproate increases lamotrigine concentrations more than 2-fold. (7, 12.3)
- Carbamazepine, phenytoin, phenobarbital, and primidone decrease lamotrigine concentrations by approximately 40%. (7, 12.3)
- Estrogen-containing oral contraceptives and rifampin also decrease lamotrigine concentrations by approximately 50%. (7, 12.3)
USE IN SPECIFIC POPULATIONS
- Pregnancy: Based on animal data may cause fetal harm. Pregnancy registry available. (8.1)
- Hepatic impairment: Dosage adjustments required in patients with moderate and severe liver impairment. (2.1, 8.6)
- Renal impairment: Reduced maintenance doses may be effective for patients with significant renal impairment. (2.1, 8.7)
See 17 for PATIENT COUNSELING INFORMATION and Medication Guide.
Revised: 11/2011
-
Table of Contents
FULL PRESCRIBING INFORMATION: CONTENTS*
WARNING: SERIOUS SKIN RASHES
1. INDICATIONS AND USAGE
1.1 Adjunctive Therapy
1.3 Limitation of Use
2. DOSAGE AND ADMINISTRATION
2.1 General Dosing Considerations
2.2 Adjunctive Therapy for Partial Onset Seizures
2.4 Conversion From Immediate-Release Lamotrigine Tablets to Lamotrigine Extended-Release Tablets
3. DOSAGE FORMS AND STRENGTHS
3.1 Extended-Release Tablets
3.2 Potential Medication Errors
4. CONTRAINDICATIONS
5. WARNINGS AND PRECAUTIONS
5.1 Serious Skin Rashes
5.2 Multiorgan Hypersensitivity Reactions and Organ Failure
5.3 Blood Dyscrasias
5.4 Suicidal Behavior and Ideation
5.5 Aseptic Meningitis
5.6 Potential Medication Errors
5.7 Concomitant Use With Oral Contraceptives
5.8 Withdrawal Seizures
5.9 Status Epilepticus
5.10 Sudden Unexplained Death in Epilepsy
5.11 Addition of Lamotrigine Extended-Release Tablets to a Multidrug Regimen That Includes Valproate
5.12 Binding in the Eye and Other Melanin-Containing Tissues
5.13 Laboratory Tests
6. ADVERSE REACTIONS
6.1 Clinical Trial Experience with lamotrigine extended-release tablets for Treatment of Partial Onset Seizures
6.2 Other Adverse Reactions Observed During the Clinical Development of the Immediate-Release Lamotrigine
6.3 Postmarketing Experience with the Immediate-Release Lamotrigine
7. DRUG INTERACTIONS
8. USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
8.2 Labor and Delivery
8.3 Nursing Mothers
8.4 Pediatric Use
8.5 Geriatric Use
8.6 Patients With Hepatic Impairment
8.7 Patients With Renal Impairment
10. OVERDOSAGE
10.1 Human Overdose Experience
10.2 Management of Overdose
11. DESCRIPTION
12. CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
12.2 Pharmacodynamics
12.3 Pharmacokinetics
13. NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment Of Fertility
14. CLINICAL STUDIES
14.2 Adjunctive Therapy for Partial Onset Seizures
15. REFERENCES
16. HOW SUPPLIED/STORAGE AND HANDLING
17. PATIENT COUNSELING INFORMATION
17.1 Rash
17.2 Multiorgan Hypersensitivity Reactions, Blood Dyscrasias and Organ Failure
17.3 Suicidal Thinking and Behavior
17.4 Worsening of Seizures
17.5 Central Nervous System Adverse Effects
17.6 Pregnancy and Nursing
17.7 Oral Contraceptive Use
17.8 Discontinuing lamotrigine extended-release tablets
17.9 Aseptic Meningitis
17.10 Potential Medication Errors
- * Sections or subsections omitted from the full prescribing information are not listed.
-
BOXED WARNING
(What is this?)
WARNING: SERIOUS SKIN RASHES
Lamotrigine extended-release tablets can cause serious rashes requiring hospitalization and discontinuation of treatment. The incidence of these rashes, which have included Stevens Johnson syndrome, is approximately 0.8% (8 per 1,000) in pediatric patients (aged 2 to 16 years) receiving immediate-release lamotrigine as adjunctive therapy for epilepsy and 0.3% (3 per 1,000) in adults on adjunctive therapy for epilepsy. In a prospectively followed cohort of 1,983 pediatric patients (aged 2 to 16 years) with epilepsy taking adjunctive immediate-release lamotrigine, there was 1 rash-related death. Lamotrigine extended-release tablet is not approved for patients less than 13 years of age. In worldwide postmarketing experience, rare cases of toxic epidermal necrolysis and/or rash-related death have been reported in adult and pediatric patients, but their numbers are too few to permit a precise estimate of the rate.
The risk of serious rash caused by treatment with lamotrigine extended-release tablet is not expected to differ from that with the immediate-release lamotrigine. However, the relatively limited treatment experience with lamotrigine extended-release tablets makes it difficult to characterize the frequency and risk of serious rashes caused by treatment with lamotrigine extended-release tablets.
Other than age, there are as yet no factors identified that are known to predict the risk of occurrence or the severity of rash caused by lamotrigine extended-release tablets. There are suggestions, yet to be proven, that the risk of rash may also be increased by (1) coadministration of lamotrigine extended-release tablets with valproate (includes valproic acid and divalproex sodium), (2) exceeding the recommended initial dose of lamotrigine extended-release tablets, or (3) exceeding the recommended dose escalation for lamotrigine extended-release tablets. However, cases have occurred in the absence of these factors.
Nearly all cases of life-threatening rashes caused by the immediate-release lamotrigine have occurred within 2 to 8 weeks of treatment initiation. However, isolated cases have occurred after prolonged treatment (e.g., 6 months). Accordingly, duration of therapy cannot be relied upon as means to predict the potential risk heralded by the first appearance of a rash.
Although benign rashes are also caused by lamotrigine extended-release tablets, it is not possible to predict reliably which rashes will prove to be serious or life-threatening. Accordingly, lamotrigine extended-release tablets should ordinarily be discontinued at the first sign of rash, unless the rash is clearly not drug-related. Discontinuation of treatment may not prevent a rash from becoming life threatening or permanently disabling or disfiguring [see Warnings and Precautions (5.1)].
- 1. INDICATIONS AND USAGE
-
2. DOSAGE AND ADMINISTRATION
Lamotrigine extended-release tablets are taken once daily, with or without food. Tablets must be swallowed whole and must not be chewed, crushed, or divided.
2.1 General Dosing Considerations
Rash: There are suggestions, yet to be proven, that the risk of severe, potentially life-threatening rash may be increased by (1) coadministration of lamotrigine extended-release tablets with valproate, (2) exceeding the recommended initial dose of lamotrigine extended-release tablets, or (3) exceeding the recommended dose escalation for lamotrigine extended-release tablets. However, cases have occurred in the absence of these factors [see Boxed Warning]. Therefore, it is important that the dosing recommendations be followed closely.
The risk of nonserious rash may be increased when the recommended initial dose and/or the rate of dose escalation for lamotrigine extended-release tablet is exceeded and in patients with a history of allergy or rash to other AEDs.
It is recommended that lamotrigine extended-release tablets not be restarted in patients who discontinued due to rash associated with prior treatment with lamotrigine, unless the potential benefits clearly outweigh the risks. If the decision is made to restart a patient who has discontinued lamotrigine extended-release tablets, the need to restart with the initial dosing recommendations should be assessed. The greater the interval of time since the previous dose, the greater consideration should be given to restarting with the initial dosing recommendations. If a patient has discontinued lamotrigine for a period of more than 5 half-lives, it is recommended that initial dosing recommendations and guidelines be followed. The half-life of lamotrigine is affected by other concomitant medications [see Clinical Pharmacology (12.3)].
Lamotrigine Extended-Release Tablets Added to Drugs Known to Induce or Inhibit Glucuronidation: Drugs other than those listed in the Clinical Pharmacology section [see Clinical Pharmacology (12.3)] have not been systematically evaluated in combination with lamotrigine. Because lamotrigine is metabolized predominantly by glucuronic acid conjugation, drugs that are known to induce or inhibit glucuronidation may affect the apparent clearance of lamotrigine and doses of lamotrigine extended-release tablets may require adjustment based on clinical response.
Target Plasma Levels: A therapeutic plasma concentration range has not been established for lamotrigine. Dosing of lamotrigine extended-release tablets should be based on therapeutic response [see Clinical Pharmacology (12.3)].
Women Taking Estrogen-Containing Oral Contraceptives: Starting Lamotrigine Extended-Release Tablets in Women Taking Estrogen-Containing Oral Contraceptives: Although estrogen-containing oral contraceptives have been shown to increase the clearance of lamotrigine [see Clinical Pharmacology (12.3)], no adjustments to the recommended dose-escalation guidelines for lamotrigine extended-release tablets should be necessary solely based on the use of estrogen-containing oral contraceptives. Therefore, dose escalation should follow the recommended guidelines for initiating adjunctive therapy with lamotrigine extended-release tablets based on the concomitant AED or other concomitant medications (see Table 1). See below for adjustments to maintenance doses of lamotrigine extended-release tablets in women taking estrogen-containing oral contraceptives.
Adjustments to the Maintenance Dose of Lamotrigine Extended-Release Tablets in Women Taking Estrogen-Containing Oral Contraceptives:
(1) Taking Estrogen-Containing Oral Contraceptives: For women not taking carbamazepine, phenytoin, phenobarbital, primidone, or other drugs such as rifampin that induce lamotrigine glucuronidation [see Drug Interactions, (7), Clinical Pharmacology (12.3)], the maintenance dose of lamotrigine extended-release tablets will in most cases need to be increased by as much as 2-fold over the recommended target maintenance dose in order to maintain a consistent lamotrigine plasma level [see Clinical Pharmacology (12.3)].
(2) Starting Estrogen-Containing Oral Contraceptives: In women taking a stable dose of lamotrigine extended-release tablets and not taking carbamazepine, phenytoin, phenobarbital, primidone, or other drugs such as rifampin that induce lamotrigine glucuronidation [see Drug Interactions (7), Clinical Pharmacology (12.3)], the maintenance dose will in most cases need to be increased by as much as 2-fold in order to maintain a consistent lamotrigine plasma level. The dose increases should begin at the same time that the oral contraceptive is introduced and continue, based on clinical response, no more rapidly than 50 to 100 mg/day every week. Dose increases should not exceed the recommended rate (see Table 1) unless lamotrigine plasma levels or clinical response support larger increases. Gradual transient increases in lamotrigine plasma levels may occur during the week of inactive hormonal preparation (pill-free week), and these increases will be greater if dose increases are made in the days before or during the week of inactive hormonal preparation. Increased lamotrigine plasma levels could result in additional adverse reactions, such as dizziness, ataxia, and diplopia. If adverse reactions attributable to lamotrigine extended-release tablets consistently occur during the pill-free week, dose adjustments to the overall maintenance dose may be necessary. Dose adjustments limited to the pill-free week are not recommended. For women taking lamotrigine extended-release tablets in addition to carbamazepine, phenytoin, phenobarbital, primidone, or other drugs such as rifampin that induce lamotrigine glucuronidation [see Drug Interactions (7), Clinical Pharmacology (12.3)], no adjustment to the dose of lamotrigine extended-release tablets should be necessary.
(3) Stopping Estrogen-Containing Oral Contraceptives: For women not taking carbamazepine, phenytoin, phenobarbital, primidone, or other drugs such as rifampin that induce lamotrigine glucuronidation [see Drug Interactions (7), Clinical Pharmacology (12.3)], the maintenance dose of lamotrigine extended-release tablets will in most cases need to be decreased by as much as 50% in order to maintain a consistent lamotrigine plasma level. The decrease in dose of lamotrigine extended-release tablets should not exceed 25% of the total daily dose per week over a 2-week period, unless clinical response or lamotrigine plasma levels indicate otherwise [see Clinical Pharmacology (12.3)]. For women taking lamotrigine extended-release tablets in addition to carbamazepine, phenytoin, phenobarbital, primidone, or other drugs such as rifampin that induce lamotrigine glucuronidation [see Drug Interactions (7), Clinical Pharmacology (12.3)], no adjustment to the dose of lamotrigine extended-release tablets should be necessary.
Women and Other Hormonal Contraceptive Preparations or Hormone Replacement Therapy: The effect of other hormonal contraceptive preparations or hormone replacement therapy on the pharmacokinetics of lamotrigine has not been systematically evaluated. It has been reported that ethinylestradiol, not progestogens, increased the clearance of lamotrigine up to 2-fold, and the progestin-only pills had no effect on lamotrigine plasma levels. Therefore, adjustments to the dosage of lamotrigine extended-release tablets in the presence of progestogens alone will likely not be needed.
Patients With Hepatic Impairment: Experience in patients with hepatic impairment is limited. Based on a clinical pharmacology study in 24 patients with mild, moderate, and severe liver impairment [see Use in Specific Populations (8.6), Clinical Pharmacology (12.3)], the following general recommendations can be made. No dosage adjustment is needed in patients with mild liver impairment. Initial, escalation, and maintenance doses should generally be reduced by approximately 25% in patients with moderate and severe liver impairment without ascites and 50% in patients with severe liver impairment with ascites. Escalation and maintenance doses may be adjusted according to clinical response.
Patients With Renal Impairment: Initial doses of lamotrigine extended-release tablets should be based on patients’ concomitant medications (see Table 1); reduced maintenance doses may be effective for patients with significant renal impairment [see Use in Specific Populations (8.7), Clinical Pharmacology (12.3)]. Few patients with severe renal impairment have been evaluated during chronic treatment with immediate-release lamotrigine. Because there is inadequate experience in this population, lamotrigine extended-release tablets should be used with caution in these patients.
Discontinuation Strategy: For patients receiving lamotrigine extended-release tablets in combination with other AEDs, a re-evaluation of all AEDs in the regimen should be considered if a change in seizure control or an appearance or worsening of adverse reactions is observed.
If a decision is made to discontinue therapy with lamotrigine extended-release tablets, a step-wise reduction of dose over at least 2 weeks (approximately 50% per week) is recommended unless safety concerns require a more rapid withdrawal [see Warnings and Precautions (5.8)].
Discontinuing carbamazepine, phenytoin, phenobarbital, primidone, or other drugs such as rifampin that induce lamotrigine glucuronidation should prolong the half-life of lamotrigine; discontinuing valproate should shorten the half-life of lamotrigine.
2.2 Adjunctive Therapy for Partial Onset Seizures
This section provides specific dosing recommendations for patients ≥13 years of age. Specific dosing recommendations are provided depending upon concomitant AED or other concomitant medications.
Table 1. Escalation Regimen for Lamotrigine Extended-Release Tablets in Patients ≥13 Years of Age a Valproate has been shown to inhibit glucuronidation and decrease the apparent
clearance of lamotrigine [see Drug Interactions (7), Clinical Pharmacology (12.3)].
b These drugs induce glucuronidation and increase clearance [see Drug Interactions (7),
Clinical Pharmacology (12.3)]. Other drugs which have similar effects include estrogen-
containing oral contraceptives [see Drug Interactions (7), Clinical Pharmacology (12.3)].
Dosing recommendations for oral contraceptives can be found in General Dosing
Considerations [see Dosage and Administration (2.1)]. Patients on rifampin, or other drugs
that induce lamotrigine glucuronidation and increase clearance, should follow the same
dosing titration/maintenance regimen as that used with anticonvulsants that have this
effect.
c Dose increases at week 8 or later should not exceed 100 mg daily at weekly intervals.
For Patients TAKING
Valproatea
For Patients NOT
TAKING Carbamazepine,
Phenytoin, Phenobarbital,
Primidoneb, or
Valproatea
For Patients TAKING
Carbamazepine,
Phenytoin,
Phenobarbital, or
Primidoneb and NOT
TAKING Valproatea
Weeks 1 and 2
25 mg every
other day
25 mg every day
50 mg every day
Weeks 3 and 4
25 mg every day
50 mg every day
100 mg every day
Week 5
50 mg every day
100 mg every day
200 mg every day
Week 6
100 mg every day
150 mg every day
300 mg every day
Week 7
150 mg every day
200 mg every day
400 mg every day
Maintenance range
(week 8 and
onward)
200 to 250 mg
every dayc
300 to 400 mg
every dayc
400 to 600 mg
every dayc
2.4 Conversion From Immediate-Release Lamotrigine Tablets to Lamotrigine Extended-Release Tablets
Patients may be converted directly from immediate-release lamotrigine to lamotrigine extended-release tablets. The initial dose of lamotrigine extended-release tablets should match the total daily dose of immediate-release lamotrigine. However, some subjects on concomitant enzyme-inducing agents may have lower plasma levels of lamotrigine on conversion and should be monitored [see Clinical Pharmacology (12.3)].
Following conversion to lamotrigine extended-release tablets, all patients (but especially those on drugs that induce lamotrigine glucuronidation) should be closely monitored for seizure control [see Drug Interactions (7)]. Depending on the therapeutic response after conversion, the total daily dose may need to be adjusted within the recommended dosing instructions (Table 1).
-
3. DOSAGE FORMS AND STRENGTHS
3.1 Extended-Release Tablets
25 mg, yellow, enteric-coated, circular shaped tablet, debossed with "W" on one side and "271" on the other side.
50 mg, pink, enteric-coated, circular shaped tablet, debossed with "W" on one side and "274" on the other side.
100 mg, light brown, enteric-coated, circular shaped tablet, debossed with "W" on one side and "273" on the other side.
200 mg, pink, enteric-coated, circular shaped tablet, debossed with "W" on one side and "272" on the other side.
300 mg, pink, enteric-coated, circular shaped tablet, debossed with "W" on one side and "275" on the other side.
3.2 Potential Medication Errors
Patients should be strongly advised to visually inspect their tablets to verify that they are receiving lamotrigine extended-release tablets, as opposed to other medications, and that they are receiving the correct formulation of lamotrigine each time they fill their prescription. Depictions of the lamotrigine extended-release tablets can be found in the Medication Guide.
-
4. CONTRAINDICATIONS
Lamotrigine extended-release tablet is contraindicated in patients who have demonstrated hypersensitivity (e.g., rash, angioedema, acute urticaria, extensive pruritus, mucosal ulceration) to the drug or its ingredients [see Boxed Warning, Warnings and Precautions (5.1, 5.2)].
-
5. WARNINGS AND PRECAUTIONS
5.1 Serious Skin Rashes
The risk of serious rash caused by treatment with lamotrigine extended-release tablet is not expected to differ from that with immediate-release lamotrigine [see Boxed Warning]. However, the relatively limited treatment experience with lamotrigine extended-release tablets makes it difficult to characterize the frequency and risk of serious rashes caused by treatment with lamotrigine extended-release tablets.
Pediatric Population: The incidence of serious rash associated with hospitalization and discontinuation of immediate-release lamotrigine in a prospectively followed cohort of pediatric patients (aged 2 to 16 years) with epilepsy receiving adjunctive therapy with immediate-release lamotrigine was approximately 0.8% (16 of 1,983). When 14 of these cases were reviewed by 3 expert dermatologists, there was considerable disagreement as to their proper classification. To illustrate, one dermatologist considered none of the cases to be Stevens-Johnson syndrome; another assigned 7 of the 14 to this diagnosis. There was 1 rash-related death in this 1,983-patient cohort. Additionally, there have been rare cases of toxic epidermal necrolysis with and without permanent sequelae and/or death in US and foreign postmarketing experience.
There is evidence that the inclusion of valproate in a multidrug regimen increases the risk of serious, potentially life-threatening rash in pediatric patients. In pediatric patients who used valproate concomitantly, 1.2% (6 of 482) experienced a serious rash compared with 0.6% (6 of 952) patients not taking valproate.
Lamotrigine extended-release tablet is not approved in patients less than 13 years of age.
Adult Population: Serious rash associated with hospitalization and discontinuation of immediate-release lamotrigine occurred in 0.3% (11 of 3,348) of adult patients who received immediate-release lamotrigine tablets in premarketing clinical trials of epilepsy. In worldwide postmarketing experience, rare cases of rash-related death have been reported, but their numbers are too few to permit a precise estimate of the rate.
Among the rashes leading to hospitalization were Stevens-Johnson syndrome, toxic epidermal necrolysis, angioedema, and those associated with multiorgan hypersensitivity [see Warnings and Precautions (5.2)].
There is evidence that the inclusion of valproate in a multidrug regimen increases the risk of serious, potentially life-threatening rash in adults. Specifically, of 584 patients administered immediate-release lamotrigine with valproate in epilepsy clinical trials, 6 (1%) were hospitalized in association with rash; in contrast, 4 (0.16%) of 2,398 clinical trial patients and volunteers administered immediate-release lamotrigine in the absence of valproate were hospitalized.
Patients With History of Allergy or Rash to Other Antiepileptic Drugs: The risk of nonserious rash may be increased when the recommended initial dose and/or the rate of dose escalation of lamotrigine extended-release tablets are exceeded and in patients with a history of allergy or rash to other AEDs.
5.2 Multiorgan Hypersensitivity Reactions and Organ Failure
Multiorgan hypersensitivity reactions, also known as Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS), have occurred with lamotrigine. Some have been fatal or life threatening. DRESS typically, although not exclusively, presents with fever, rash, and/or lymphadenopathy in association with other organ system involvement, such as hepatitis, nephritis, hematologic abnormalities, myocarditis, or myositis, sometimes resembling an acute viral infection. Eosinophilia is often present. This disorder is variable in its expression and other organ systems not noted here may be involved.
Fatalities associated with acute multiorgan failure and various degrees of hepatic failure have been reported in 2 of 3,796 adult patients and 4 of 2,435 pediatric patients who received lamotrigine in epilepsy clinical trials. Rare fatalities from multiorgan failure have also been reported in postmarketing use.
Isolated liver failure without rash or involvement of other organs has also been reported with lamotrigine.
It is important to note that early manifestations of hypersensitivity (e.g., fever, lymphadenopathy) may be present even though a rash is not evident. If such signs or symptoms are present, the patient should be evaluated immediately. Lamotrigine extended-release tablets should be discontinued if an alternative etiology for the signs or symptoms cannot be established.
Prior to initiation of treatment with lamotrigine extended-release tablets, the patient should be instructed that a rash or other signs or symptoms of hypersensitivity (e.g., fever, lymphadenopathy) may herald a serious medical event and that the patient should report any such occurrence to a physician immediately.
5.3 Blood Dyscrasias
There have been reports of blood dyscrasias with immediate-release lamotrigine that may or may not be associated with multiorgan hypersensitivity (also known as DRESS) [see Warnings and Precautions (5.2)]. These have included neutropenia, leukopenia, anemia, thrombocytopenia, pancytopenia, and, rarely, aplastic anemia and pure red cell aplasia.
5.4 Suicidal Behavior and Ideation
AEDs, including lamotrigine extended-release tablets, increase the risk of suicidal thoughts or behavior in patients taking these drugs for any indication. Patients treated with any AED for any indication should be monitored for the emergence or worsening of depression, suicidal thoughts or behavior, and/or any unusual changes in mood or behavior.
Pooled analyses of 199 placebo-controlled clinical trials (monotherapy and adjunctive therapy) of 11 different AEDs showed that patients randomized to one of the AEDs had approximately twice the risk (adjusted Relative Risk 1.8, 95% CI:1.2, 2.7) of suicidal thinking or behavior compared to patients randomized to placebo. In these trials, which had a median treatment duration of 12 weeks, the estimated incidence of suicidal behavior or ideation among 27,863 AED-treated patients was 0.43%, compared to 0.24% among 16,029 placebo-treated patients, representing an increase of approximately 1 case of suicidal thinking or behavior for every 530 patients treated. There were 4 suicides in drug-treated patients in the trials and none in placebo-treated patients, but the number of events is too small to allow any conclusion about drug effect on suicide.
The increased risk of suicidal thoughts or behavior with AEDs was observed as early as 1 week after starting treatment with AEDs and persisted for the duration of treatment assessed. Because most trials included in the analysis did not extend beyond 24 weeks, the risk of suicidal thoughts or behavior beyond 24 weeks could not be assessed.
The risk of suicidal thoughts or behavior was generally consistent among drugs in the data analyzed. The finding of increased risk with AEDs of varying mechanism of action and across a range of indications suggests that the risk applies to all AEDs used for any indication. The risk did not vary substantially by age (5 to 100 years) in the clinical trials analyzed.
Table 2 shows absolute and relative risk by indication for all evaluated AEDs.
Table 2. Risk by Indication for Antiepileptic Drugs in the Pooled Analysis Indication
Placebo Patients
With Events Per
1,000 Patients
Drug Patients
With Events Per
1,000 Patients
Relative Risk:
Incidence of Events
in Drug Patients/
Incidence in
Placebo Patients
Risk Difference:
Additional Drug
Patients With
Events Per
1,000 Patients
Epilepsy
1.0
3.4
3.5
2.4
Psychiatric
5.7
8.5
1.5
2.9
Other
1.0
1.8
1.9
0.9
Total
2.4
4.3
1.8
1.9
The relative risk for suicidal thoughts or behavior was higher in clinical trials for epilepsy than in clinical trials for psychiatric or other conditions, but the absolute risk differences were similar for the epilepsy and psychiatric indications.
Anyone considering prescribing lamotrigine extended-release tablets or any other AED must balance the risk of suicidal thoughts or behavior with the risk of untreated illness. Epilepsy and many other illnesses for which AEDs are prescribed are themselves associated with morbidity and mortality and an increased risk of suicidal thoughts and behavior. Should suicidal thoughts and behavior emerge during treatment, the prescriber needs to consider whether the emergence of these symptoms in any given patient may be related to the illness being treated.
Patients, their caregivers, and families should be informed that AEDs increase the risk of suicidal thoughts and behavior and should be advised of the need to be alert for the emergence or worsening of the signs and symptoms of depression; any unusual changes in mood or behavior; or the emergence of suicidal thoughts, behavior, or thoughts about self-harm. Behaviors of concern should be reported immediately to healthcare providers.
5.5 Aseptic Meningitis
Therapy with lamotrigine increases the risk of developing aseptic meningitis. Because of the potential for serious outcomes of untreated meningitis due to other causes, patients should also be evaluated for other causes of meningitis and treated as appropriate.
Postmarketing cases of aseptic meningitis have been reported in pediatric and adult patients taking lamotrigine for various indications. Symptoms upon presentation have included headache, fever, nausea, vomiting, and nuchal rigidity. Rash, photophobia, myalgia, chills, altered consciousness, and somnolence were also noted in some cases. Symptoms have been reported to occur within 1 day to one and a half months following the initiation of treatment. In most cases, symptoms were reported to resolve after discontinuation of lamotrigine. Re-exposure resulted in a rapid return of symptoms (from within 30 minutes to 1 day following re-initiation of treatment) that were frequently more severe. Some of the patients treated with lamotrigine who developed aseptic meningitis had underlying diagnoses of systemic lupus erythematosus or other autoimmune diseases.
Cerebrospinal fluid (CSF) analyzed at the time of clinical presentation in reported cases was characterized by a mild to moderate pleocytosis, normal glucose levels, and mild to moderate increase in protein. CSF white blood cell count differentials showed a predominance of neutrophils in a majority of the cases, although a predominance of lymphocytes was reported in approximately one third of the cases. Some patients also had new onset of signs and symptoms of involvement of other organs (predominantly hepatic and renal involvement), which may suggest that in these cases the aseptic meningitis observed was part of a hypersensitivity reaction [see Warnings and Precautions (5.2)].
5.6 Potential Medication Errors
Medication errors involving lamotrigine have occurred. In particular, the name lamotrigine can be confused with the names of other commonly used medications. Medication errors may also occur between the different formulations of lamotrigine. To reduce the potential of medication errors, write and say lamotrigine extended-release tablets clearly. Depictions of the lamotrigine extended-release tablets can be found in the Medication Guide. Each lamotrigine extended-release tablet has a distinct debossing and is debossed with "W" on one side and "271" on the other side for 25 mg, "W" on one side and "274" on the other side for 50 mg, "W" on one side and "273" on the other side for 100 mg, "W" on one side and "272" on the other side for 200 mg and "W" on one side and "275" on the other side for 300 mg. These distinctive features serve to identify the different presentations of the drug and thus may help reduce the risk of medication errors. Lamotrigine extended-release tablets are supplied in circular, unit-of-use bottles containing 30 tablets and 100 unit dose blister pack. Additionally, Lamotrigine extended-release tablets are also supplied as 500 count bottle pack. The label on the bottle includes a depiction of the tablets which further communicates to patients and pharmacists that the medication is lamotrigine extended-release tablets and the specific tablet strength included in the bottle. To avoid the medication error of using the wrong drug or formulation, patients should be strongly advised to visually inspect their tablets to verify that they are lamotrigine extended-release tablets each time they fill their prescription.
5.7 Concomitant Use With Oral Contraceptives
Some estrogen-containing oral contraceptives have been shown to decrease serum concentrations of lamotrigine [see Clinical Pharmacology (12.3)]. Dosage adjustments will be necessary in most patients who start or stop estrogen-containing oral contraceptives while taking lamotrigine extended-release tablets [see Dosage and Administration (2.1)]. During the week of inactive hormone preparation (pill-free week) of oral contraceptive therapy, plasma lamotrigine levels are expected to rise, as much as doubling at the end of the week. Adverse reactions consistent with elevated levels of lamotrigine, such as dizziness, ataxia, and diplopia, could occur.
5.8 Withdrawal Seizures
As with other AEDs, lamotrigine extended-release tablets should not be abruptly discontinued. In patients with epilepsy there is a possibility of increasing seizure frequency. Unless safety concerns require a more rapid withdrawal, the dose of lamotrigine extended-release tablets should be tapered over a period of at least 2 weeks (approximately 50% reduction per week) [see Dosage and Administration (2.1)].
5.9 Status Epilepticus
Valid estimates of the incidence of treatment-emergent status epilepticus among patients treated with immediate-release lamotrigine are difficult to obtain because reporters participating in clinical trials did not all employ identical rules for identifying cases. At a minimum, 7 of 2,343 adult patients had episodes that could unequivocally be described as status epilepticus. In addition, a number of reports of variably defined episodes of seizure exacerbation (e.g., seizure clusters, seizure flurries) were made.
5.10 Sudden Unexplained Death in Epilepsy
During the premarketing development of the immediate-release formulation of lamotrigine, 20 sudden and unexplained deaths were recorded among a cohort of 4,700 patients with epilepsy (5,747 patient-years of exposure).
Some of these could represent seizure-related deaths in which the seizure was not observed, e.g., at night. This represents an incidence of 0.0035 deaths per patient-year. Although this rate exceeds that expected in a healthy population matched for age and sex, it is within the range of estimates for the incidence of sudden unexplained deaths in patients with epilepsy not receiving lamotrigine (ranging from 0.0005 for the general population of patients with epilepsy, to 0.004 for a recently studied clinical trial population similar to that in the clinical development program for immediate-release lamotrigine, to 0.005 for patients with refractory epilepsy). Consequently, whether these figures are reassuring or suggest concern depends on the comparability of the populations reported upon to the cohort receiving immediate-release lamotrigine and the accuracy of the estimates provided. Probably most reassuring is the similarity of estimated sudden unexplained death in epilepsy (SUDEP) rates in patients receiving immediate-release lamotrigine and those receiving other AEDs, chemically unrelated to each other, that underwent clinical testing in similar populations. Importantly, that drug is chemically unrelated to lamotrigine. This evidence suggests, although it certainly does not prove, that the high SUDEP rates reflect population rates, not a drug effect.
5.11 Addition of Lamotrigine Extended-Release Tablets to a Multidrug Regimen That Includes Valproate
Because valproate reduces the clearance of lamotrigine, the dosage of lamotrigine in the presence of valproate is less than half of that required in its absence [see Dosage and Administration (2.1, 2.2), Drug Interactions (7)].
5.12 Binding in the Eye and Other Melanin-Containing Tissues
Because lamotrigine binds to melanin, it could accumulate in melanin-rich tissues over time. This raises the possibility that lamotrigine may cause toxicity in these tissues after extended use. Although ophthalmological testing was performed in one controlled clinical trial, the testing was inadequate to exclude subtle effects or injury occurring after long-term exposure. Moreover, the capacity of available tests to detect potentially adverse consequences, if any, of lamotrigine binding to melanin is unknown [see Clinical Pharmacology (12.2)].
Accordingly, although there are no specific recommendations for periodic ophthalmological monitoring, prescribers should be aware of the possibility of long-term ophthalmologic effects.
5.13 Laboratory Tests
Plasma Concentrations of Lamotrigine: The value of monitoring plasma concentrations of lamotrigine in patients treated with lamotrigine extended-release tablets has not been established. Because of the possible pharmacokinetic interactions between lamotrigine and other drugs, including AEDs (see Table 5), monitoring of the plasma levels of lamotrigine and concomitant drugs may be indicated, particularly during dosage adjustments. In general, clinical judgment should be exercised regarding monitoring of plasma levels of lamotrigine and other drugs and whether or not dosage adjustments are necessary.
Effect on Leukocytes: Treatment with lamotrigine extended-release tablets caused an increased incidence of subnormal (below the reference range) values in some hematology analytes (e.g., total white blood cells, monocytes). The treatment effect (Lamotrigine extended-release tablets % - Placebo %) incidence of subnormal counts was 3% for total white blood cells and 4% for monocytes.
-
6. ADVERSE REACTIONS
The following adverse reactions are described in more detail in the Warnings and Precautions section of the label:
- Serious skin rashes [see Warnings and Precautions (5.1)]
- Multiorgan hypersensitivity reactions and organ failure [see Warnings and Precautions (5.2)]
- Blood dyscrasias [see Warnings and Precautions (5.3)]
- Suicidal behavior and ideation [see Warnings and Precautions (5.4)]
- Aseptic meningitis [see Warnings and Precautions (5.5)]
- Withdrawal seizures [see Warnings and Precautions (5.8)]
- Status epilepticus [see Warnings and Precautions (5.9)]
- Sudden unexplained death in epilepsy [see Warnings and Precautions (5.10)]
6.1 Clinical Trial Experience with lamotrigine extended-release tablets for Treatment of Partial Onset Seizures
Most Common Adverse Reactions in Clinical Studies: Adjunctive Therapy in Patients With Epilepsy: Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared with rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Lamotrigine extended-release tablets have been evaluated for safety in patients ≥13 years of age with partial onset seizures. The most commonly observed adverse reactions in these 2 double-blind, placebo-controlled trial of adjunctive therapy with lamotrigine extended-release tablets were, in order of decreasing incidence (treatment difference between lamotrigine extended-release tablets and placebo ≥4%): dizziness, tremor/intention tremor, vomiting, and diplopia.
In these 2 trials, adverse reactions led to withdrawal of 4 (2%) patients in the group receiving placebo and 10 (5%) patients in the group receiving lamotrigine extended-release tablets. Dizziness was the most common reason for withdrawal in the group receiving lamotrigine extended-release tablets (5 patients [3%]). The next most common adverse reactions leading to withdrawal in 2 patients each (1%) were rash, headache, nausea, and nystagmus.
Table 3 displays the incidence of adverse reactions in these two 19-week, double-blind, placebo-controlled studies of patients with partial onset seizures.
Table 3. Adverse Reaction Incidence in Double-Blind, Placebo-Controlled Adjunctive Trials of Patients With Epilepsy (Adverse Reactions ≥2% of Patients Treated With Lamotrigine Extended-Release Tablets and Numerically More Frequent Than in the Placebo Group) Note: In these trials the incidence of nonserious rash was 2% for lamotrigine
extended-release tablets and 3% for placebo. In clinical trials evaluating the
immediate-release formulation of lamotrigine tablets, the rate of serious rash was
0.3% in adults on adjunctive therapy for epilepsy [see Boxed Warning].
Body System/Adverse Reaction
Lamotrigine
Extended-Release Tablets
(n = 190)
%
Placebo
(n = 195)
%
Ear and labyrinth disorders
Vertigo
3
<1
Eye disorders
Diplopia
5
<1
Vision blurred
3
2
Gastrointestinal disorders
Nausea
7
4
Vomiting
6
3
Diarrhea
5
3
Constipation
2
<1
Dry mouth
2
1
General disorders and administration
site conditions
Asthenia and fatigue
6
4
Infections and infestations
Sinusitis
2
1
Metabolic and nutritional disorders
Anorexia
3
2
Musculoskeletal and connective
tissue disorder
Myalgia
2
0
Nervous system
Dizziness
14
6
Tremor and intention tremor
6
1
Somnolence
5
3
Cerebellar coordination and
balance disorder
3
0
Nystagmus
2
<1
Psychiatric disorders
Depression
3
<1
Anxiety
3
0
Respiratory, thoracic, and
mediastinal disorders
Pharyngolaryngeal pain
3
2
Vascular disorder
Hot flush
2
0
Adverse reactions were also analyzed to assess the incidence of the onset of an event in the titration period, and in the maintenance period, and if adverse reactions occurring in the titration phase persisted in the maintenance phase.
The incidence for many adverse reactions caused by treatment with lamotrigine extended-release tablets treatment was increased relative to placebo (i.e., treatment difference between lamotrigine extended-release tablets and placebo ≥2%) in either the titration or maintenance phases of the study. During the titration phase, an increased incidence (shown in descending order of % treatment difference) was observed for diarrhea, nausea, vomiting, somnolence, vertigo, myalgia, hot flush, and anxiety. During the maintenance phase, an increased incidence was observed for dizziness, tremor, and diplopia. Some adverse reactions developing in the titration phase were notable for persisting (>7 days) into the maintenance phase. These "persistent" adverse reactions included somnolence and dizziness.
There were inadequate data to evaluate the effect of dose and/or concentration on the incidence of adverse reactions because, although patients were randomized to different target doses based upon concomitant AED, the plasma exposure was expected to be generally similar among all patients receiving different doses. However, in a randomized, parallel study comparing placebo and 300 and 500 mg/day of immediate-release formulation of lamotrigine, the incidence of the most common adverse reactions (>5%) such as ataxia, blurred vision, diplopia, and dizziness were dose related. Less common adverse reactions (<5%) were not assessed for dose-response relationships.
6.2 Other Adverse Reactions Observed During the Clinical Development of the Immediate-Release Lamotrigine
All reported reactions are included except those already listed in the previous tables or elsewhere in the labeling, those too general to be informative, and those not reasonably associated with the use of the drug.
Adjunctive Therapy in Adults With Epilepsy: In addition to the adverse reactions reported above from the development of lamotrigine extended-release tablets, the following adverse reactions with an uncertain relationship to lamotrigine were reported during the clinical development of immediate-release lamotrigine for treatment of epilepsy in adults. These reactions occurred in ≥2% of patients receiving immediate-release lamotrigine and more frequently than in the placebo group.
Body as a Whole: Headache, flu syndrome, fever, neck pain.
Musculoskeletal: Arthralgia.
Nervous: Insomnia, convulsion, irritability, speech disorder, concentration disturbance.
Respiratory: Pharyngitis, cough increased.
Skin and Appendages: Rash, pruritus.
Urogenital (female patients only): Vaginitis, amenorrhea, dysmenorrhea.
Other Clinical Trial Experience: Immediate-release lamotrigine has been administered to 6,694 individuals for whom complete adverse reaction data was captured during all clinical trials, only some of which were placebo controlled.
Adverse reactions are further classified within body system categories and enumerated in order of decreasing frequency using the following definitions: frequent adverse reactions are defined as those occurring in at least 1/100 patients; infrequent adverse reactions are those occurring in 1/100 to 1/1,000 patients; rare adverse reactions are those occurring in fewer than 1/1,000 patients.
Cardiovascular System: Infrequent: Hypertension, palpitations, postural hypotension, syncope, tachycardia, vasodilation.
Dermatological: Infrequent: Acne, alopecia, hirsutism, maculopapular rash, urticaria. Rare: Leukoderma, multiforme erythema, petechial rash, pustular rash.
Digestive System: Infrequent: Dysphagia, liver function tests abnormal, mouth ulceration. Rare: Gastrointestinal hemorrhage, hemorrhagic colitis, hepatitis, melena and stomach ulcer.
Endocrine System: Rare: Goiter, hypothyroidism.
Hematologic and Lymphatic System: Infrequent: Ecchymosis, leukopenia. Rare: Anemia, eosinophilia, fibrin decrease, fibrinogen decrease, iron deficiency anemia, leukocytosis, lymphocytosis, macrocytic anemia, petechia, thrombocytopenia.
Metabolic and Nutritional Disorders: Infrequent: Aspartate transaminase increased. Rare: Alcohol intolerance, alkaline phosphatase increase, alanine transaminase increase, bilirubinemia, gamma glutamyl transpeptidase increase, hyperglycemia.
Musculoskeletal System: Rare: Muscle atrophy, pathological fracture, tendinous contracture.
Nervous System: Frequent: Confusion. Infrequent: Akathisia, apathy, aphasia, depersonalization, dysarthria, dyskinesia, euphoria, hallucinations, hostility, hyperkinesia, hypertonia, libido decreased, memory decrease, mind racing, movement disorder, myoclonus, panic attack, paranoid reaction, personality disorder, psychosis, stupor. Rare: Choreoathetosis, delirium, delusions, dysphoria, dystonia, extrapyramidal syndrome, hemiplegia, hyperalgesia, hyperesthesia, hypokinesia, hypotonia, manic depression reaction, neuralgia, paralysis, peripheral neuritis.
Respiratory System: Rare: Hiccup, hyperventilation.
Special Senses: Frequent: Amblyopia. Infrequent: Abnormality of accommodation, conjunctivitis, dry eyes, ear pain, photophobia, taste perversion, tinnitus. Rare: Deafness, lacrimation disorder, oscillopsia, parosmia, ptosis, strabismus, taste loss, uveitis, visual field defect.
Urogenital System: Infrequent: Abnormal ejaculation, hematuria, impotence, menorrhagia, polyuria, urinary incontinence. Rare: Acute kidney failure, breast neoplasm, creatinine increase, female lactation, kidney failure, kidney pain, nocturia, urinary retention, urinary urgency.
6.3 Postmarketing Experience with the Immediate-Release Lamotrigine
The following adverse events (not listed above in clinical trials or other sections of the prescribing information) have been identified during postapproval use of immediate-release lamotrigine. Because these events are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Blood and Lymphatic: Agranulocytosis, hemolytic anemia, lymphadenopathy not associated with hypersensitivity disorder.
Gastrointestinal: Esophagitis.
Hepatobiliary Tract and Pancreas: Pancreatitis.
Immunologic: Lupus-like reaction, vasculitis.
Lower Respiratory: Apnea.
Musculoskeletal: Rhabdomyolysis has been observed in patients experiencing hypersensitivity reactions.
Neurology: Exacerbation of Parkinsonian symptoms in patients with pre-existing Parkinson’s disease, tics.
Non-site Specific: Progressive immunosuppression.
-
7. DRUG INTERACTIONS
Significant drug interactions with lamotrigine are summarized in Table 4. Additional details of these drug interaction studies, which were conducted using immediate-release lamotrigine, are provided in the Clinical Pharmacology section [see Clinical Pharmacology (12.3)].
Table 4. Established and Other Potentially Significant Drug Interactions ↓ = Decreased (induces lamotrigine glucuronidation).
↑ = Increased (inhibits lamotrigine glucuronidation).
? = Conflicting data.
Concomitant Drug
Effect on Concentration
of Lamotrigine or
Concomitant Drug
Clinical Comment
Estrogen-containing oral
contraceptive preparations
containing 30 mcg
ethinylestradiol and 150 mcg
levonorgestrel
↓ lamotrigine
↓ levonorgestrel
Decreased lamotrigine levels
approximately 50%.
Decrease in levonorgestrel
component by 19%.
Carbamazepine and
carbamazepine epoxide
↓ lamotrigine
? carbamazepine
epoxide
Addition of carbamazepine
decreases lamotrigine
concentration approximately 40%.
May increase carbamazepine
epoxide levels.
Phenobarbital/Primidone
↓ lamotrigine
Decreased lamotrigine
concentration approximately 40%.
Phenytoin
↓ lamotrigine
Decreased lamotrigine
concentration approximately 40%.
Rifampin
↓ lamotrigine
Decreased lamotrigine
AUC approximately 40%.
Valproate
↑ lamotrigine
? valproate
Increased lamotrigine
concentrations slightly more than
2-fold.
Decreased valproate concentrations
an average of 25% over a 3-week
period then stabilized in healthy
volunteers; no change in controlled
clinical trials in epilepsy patients.
-
8. USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
As with other AEDs, physiological changes during pregnancy may affect lamotrigine concentrations and/or therapeutic effect. There have been reports of decreased lamotrigine concentrations during pregnancy and restoration of pre-partum concentrations after delivery. Dosage adjustments may be necessary to maintain clinical response.
Pregnancy Category C.
There are no adequate and well-controlled studies in pregnant women. In animal studies, lamotrigine was developmentally toxic at doses lower than those administered clinically. Lamotrigine extended-release tablets should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
When lamotrigine was administered to pregnant mice, rats, or rabbits during the period of organogenesis (oral doses of up to 125, 25, and 30 mg/kg, respectively), reduced fetal body weight and increased incidences of fetal skeletal variations were seen in mice and rats at doses that were also maternally toxic. The no-effect doses for embryo-fetal developmental toxicity in mice, rats, and rabbits (75, 6.25, and 30 mg/kg, respectively) are similar to (mice and rabbits) or less than the human dose of 400 mg/day on a body surface area (mg/m2) basis.
In a study in which pregnant rats were administered lamotrigine (oral doses of 5 or 25 mg/kg) during the period of organogenesis and offspring were evaluated postnatally, behavioral abnormalities were observed in exposed offspring at both doses. The lowest effect dose for developmental neurotoxicity in rats is less than the human dose of 400 mg/day on a mg/m2 basis. Maternal toxicity was observed at the higher dose tested.
When pregnant rats were administered lamotrigine (oral doses of 5, 10, or 20 mg/kg) during the latter part of gestation, increased offspring mortality (including stillbirths) was seen at all doses. The lowest effect dose for peri/postnatal developmental toxicity in rats is less than the human dose of 400 mg/day on a mg/m2 basis. Maternal toxicity was observed at the two highest doses tested.
Lamotrigine decreases fetal folate concentrations in rat, an effect known to be associated with adverse pregnancy outcomes in animals and humans.
Pregnancy Registry: To provide information regarding the effects of in utero exposure to lamotrigine extended-release tablets, physicians are advised to recommend that pregnant patients taking lamotrigine extended-release tablets enroll in the North American Antiepileptic Drug (NAAED) Pregnancy Registry. This can be done by calling the toll-free number 1-888-233-2334, and must be done by patients themselves. Information on the registry can also be found at the website http://www.aedpregnancyregistry.org.
8.2 Labor and Delivery
The effect of lamotrigine extended-release tablets on labor and delivery in humans is unknown.
8.3 Nursing Mothers
Lamotrigine is present in milk from lactating women taking lamotrigine extended-release tablets. Data from multiple small studies indicate that lamotrigine plasma levels in human milk-fed infants have been reported to be as high as 50% of the maternal serum levels. Neonates and young infants are at risk for high serum levels because maternal serum and milk levels can rise to high levels postpartum if lamotrigine dosage has been increased during pregnancy but not later reduced to the pre-pregnancy dosage. Lamotrigine exposure is further increased due to the immaturity of the infant glucuronidation capacity needed for drug clearance. Events including apnea, drowsiness, and poor sucking have been reported in infants who have been human milk-fed by mothers using lamotrigine; whether or not these events were caused by lamotrigine is unknown. Human milk fed infants should be closely monitored for adverse events resulting from lamotrigine. Measurement of infant serum levels should be performed to rule out toxicity if concerns arise. Human milk-feeding should be discontinued in infants with lamotrigine toxicity. Caution should be exercised when lamotrigine extended-release tablet is administered to a nursing woman.
8.4 Pediatric Use
Lamotrigine extended-release tablet is indicated as adjunctive therapy for partial onset seizures with or without secondary generalization in patients ≥13 years of age. Safety and effectiveness of lamotrigine extended-release tablets for any use in patients less than 13 years of age have not been established.
Immediate-release lamotrigine is indicated for adjunctive therapy in patients ≥2 years of age for partial seizures, the generalized seizures of Lennox-Gastaut syndrome, and PGTC seizures.
Safety and efficacy of immediate-release lamotrigine, used as adjunctive treatment for partial seizures, were not demonstrated in a small, randomized, double-blind, placebo-controlled withdrawal study in very young pediatric patients (aged 1 to 24 months). Immediate-release lamotrigine was associated with an increased risk for infectious adverse reactions (lamotrigine 37%, placebo 5%), and respiratory adverse reactions (lamotrigine 26%, placebo 5%). Infectious adverse reactions included bronchiolitis, bronchitis, ear infection, eye infection, otitis externa, pharyngitis, urinary tract infection, and viral infection. Respiratory adverse reactions included nasal congestion, cough, and apnea.
In a juvenile animal study in which lamotrigine (oral doses of 5, 15, or 30 mg/kg) was administered to young rats (postnatal days 7-62), decreased viability and growth were seen at the highest dose tested and long-term behavioral abnormalities (decreased locomotor activity, increased reactivity, and learning deficits in animals tested as adults) were observed at the two highest doses. The no-effect dose for adverse effects on neurobehavioral development is less than the human dose of 400 mg/day on a mg/m2 basis.
8.5 Geriatric Use
Clinical studies of lamotrigine extended-release tablets for epilepsy did not include sufficient numbers of subjects aged 65 years and over to determine whether they respond differently from younger subjects or exhibit a different safety profile than that of younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function and of concomitant disease or other drug therapy.
8.6 Patients With Hepatic Impairment
Experience in patients with hepatic impairment is limited. Based on a clinical pharmacology study with immediate-release lamotrigine in 24 patients with mild, moderate, and severe liver impairment [see Clinical Pharmacology (12.3)], the following general recommendations can be made. No dosage adjustment is needed in patients with mild liver impairment. Initial, escalation, and maintenance doses should generally be reduced by approximately 25% in patients with moderate and severe liver impairment without ascites and 50% in patients with severe liver impairment with ascites. Escalation and maintenance doses may be adjusted according to clinical response [see Dosage and Administration (2.1)].
8.7 Patients With Renal Impairment
Lamotrigine is metabolized mainly by glucuronic acid conjugation, with the majority of the metabolites being recovered in the urine. In a small study comparing a single dose of immediate-release lamotrigine in patients with varying degrees of renal impairment with healthy volunteers, the plasma half-life of lamotrigine was approximately twice as long in the patients with significant renal impairment [see Clinical Pharmacology (12.3)].
Initial doses of lamotrigine extended-release tablets should be based on patients’ AED regimens; reduced maintenance doses may be effective for patients with significant renal impairment. Few patients with severe renal impairment have been evaluated during chronic treatment with lamotrigine. Because there is inadequate experience in this population, lamotrigine extended-release tablets should be used with caution in these patients [see Dosage and Administration (2.1)].
-
10. OVERDOSAGE
10.1 Human Overdose Experience
Overdoses involving quantities up to 15 g have been reported for immediate-release lamotrigine, some of which have been fatal. Overdose has resulted in ataxia, nystagmus, increased seizures, decreased level of consciousness, coma, and intraventricular conduction delay.
10.2 Management of Overdose
There are no specific antidotes for lamotrigine. Following a suspected overdose, hospitalization of the patient is advised. General supportive care is indicated, including frequent monitoring of vital signs and close observation of the patient. If indicated, emesis should be induced; usual precautions should be taken to protect the airway. It is uncertain whether hemodialysis is an effective means of removing lamotrigine from the blood. In 6 renal failure patients, about 20% of the amount of lamotrigine in the body was removed by hemodialysis during a 4-hour session. A Poison Control Center should be contacted for information on the management of overdosage of lamotrigine extended-release tablets.
-
11. DESCRIPTION
Lamotrigine, an AED of the phenyltriazine class, is chemically unrelated to existing AEDs. Its chemical name is 3,5-diamino-6-(2,3-dichlorophenyl)-as-triazine, its molecular formula is C9H7N5Cl2, and its molecular weight is 256.09. Lamotrigine is a white or almost white powder and has a pKa of 5.7. Lamotrigine is very slightly soluble in water and in 0.1M hydrochloric acid. The structural formula is:
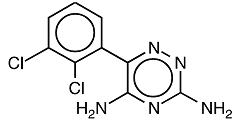
Lamotrigine Extended-Release Tablets are supplied for oral administration as 25 mg (yellow, enteric-coated, circular shaped tablet), 50 mg (pink, enteric-coated, circular shaped tablet), 100 mg (light brown, enteric-coated, circular shaped tablet), 200 mg (pink, enteric-coated, circular shaped tablet) and 300 mg (pink, enteric-coated, circular shaped tablet). Each tablet contains the labeled amount of lamotrigine and the following inactive ingredients: diethyl phthalate, hypromellose, lactose monohydrate, magnesium stearate, methacrylic acid copolymer, polyethylene glycol, talc, titanium dioxide, iron oxide yellow for (25 mg and 100 mg) and iron oxide red for (50 mg, 100 mg, 200 mg and 300 mg).
Lamotrigine extended-release tablets contain a modified-release eroding formulation as the core. The tablets are coated with enteric coat to enable a controlled release of drug in the acidic environment of the stomach. The combination of this and the modified-release core are designed to control the dissolution rate of lamotrigine over a period of approximately 12 to 15 hours, leading to a gradual increase in serum lamotrigine levels.
-
12. CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
The precise mechanism(s) by which lamotrigine exerts its anticonvulsant action are unknown. In animal models designed to detect anticonvulsant activity, lamotrigine was effective in preventing seizure spread in the maximum electroshock and pentylenetetrazol tests, and prevented seizures in the visually and electrically evoked after-discharge tests for antiepileptic activity. Lamotrigine also displayed inhibitory properties in the kindling model in rats both during kindling development and in the fully kindled state. The relevance of these models to human epilepsy, however, is not known.
One proposed mechanism of action of lamotrigine, the relevance of which remains to be established in humans, involves an effect on sodium channels. In vitro pharmacological studies suggest that lamotrigine inhibits voltage-sensitive sodium channels, thereby stabilizing neuronal membranes and consequently modulating presynaptic transmitter release of excitatory amino acids (e.g., glutamate and aspartate).
Effect of Lamotrigine on N-Methyl d-Aspartate-Receptor Mediated Activity: Lamotrigine did not inhibit N-methyl d-aspartate (NMDA)-induced depolarizations in rat cortical slices or NMDA-induced cyclic GMP formation in immature rat cerebellum, nor did lamotrigine displace compounds that are either competitive or noncompetitive ligands at this glutamate receptor complex (CNQX, CGS, TCHP). The IC50 for lamotrigine effects on NMDA-induced currents (in the presence of 3 μM of glycine) in cultured hippocampal neurons exceeded 100 μM.
12.2 Pharmacodynamics
Folate Metabolism: In vitro, lamotrigine inhibited dihydrofolate reductase, the enzyme that catalyzes the reduction of dihydrofolate to tetrahydrofolate. Inhibition of this enzyme may interfere with the biosynthesis of nucleic acids and proteins. When oral daily doses of lamotrigine were given to pregnant rats during organogenesis, fetal, placental, and maternal folate concentrations were reduced. Significantly reduced concentrations of folate are associated with teratogenesis [see Use in Specific Populations (8.1)]. Folate concentrations were also reduced in male rats given repeated oral doses of lamotrigine. Reduced concentrations were partially returned to normal when supplemented with folinic acid.
Cardiovascular: In dogs, lamotrigine is extensively metabolized to a 2-N-methyl metabolite. This metabolite causes dose-dependent prolongations of the PR interval, widening of the QRS complex, and, at higher doses, complete AV conduction block. Similar cardiovascular effects are not anticipated in humans because only trace amounts of the 2-N-methyl metabolite (<0.6% of lamotrigine dose) have been found in human urine [see Clinical Pharmacology (12.3)]. However, it is conceivable that plasma concentrations of this metabolite could be increased in patients with a reduced capacity to glucuronidate lamotrigine (e.g., in patients with liver disease, patients taking concomitant medications that inhibit glucuronidation).
12.3 Pharmacokinetics
In comparison to immediate-release lamotrigine, the plasma lamotrigine levels following administration of lamotrigine extended-release tablets are not associated with any significant changes in trough plasma concentrations, and are characterized by lower peaks, longer time to peaks, and lower peak-to-trough fluctuation, as described in detail below.
Absorption: Lamotrigine is absorbed after oral administration with negligible first-pass metabolism. The bioavailability of lamotrigine is not affected by food.
In an open-label, crossover study of 44 subjects with epilepsy receiving concomitant AEDs, the steady-state pharmacokinetics of lamotrigine were compared following administration of equivalent total doses of lamotrigine extended-release tablets given once daily with those of lamotrigine immediate-release given twice daily. In this study, the median time to peak concentration (Tmax) following administration of lamotrigine extended-release tablets was 4 to 6 hours in patients taking carbamazepine, phenytoin, phenobarbital, or primidone; 9 to 11 hours in patients taking valproate; and 6 to 10 hours in patients taking AEDs other than carbamazepine, phenytoin, phenobarbital, primidone, or valproate. In comparison, the median Tmax following administration of immediate-release lamotrigine was between 1 and 1.5 hours.
The steady-state trough concentrations for extended-release lamotrigine were similar to or higher than those of immediate-release lamotrigine depending on concomitant AED (Table 5). A mean reduction in the lamotrigine Cmax by 11% to 29% was observed for lamotrigine extended-release tablets compared to immediate-release lamotrigine, resulting in a decrease in the peak-to-trough fluctuation in serum lamotrigine concentrations. However, in some subjects receiving enzyme-inducing AEDs, a reduction in Cmax of 44% to 77% was observed. The degree of fluctuation was reduced by 17% in patients taking enzyme-inducing AEDs; 34% in patients taking valproate; and 37% in patients taking AEDs other than carbamazepine, phenytoin, phenobarbital, primidone, or valproate. Lamotrigine extended-release tablets and immediate-release lamotrigine regimens were similar with respect to area under the curve (AUC, a measure of the extent of bioavailability) for patients receiving AEDs other than those known to induce the metabolism of lamotrigine. The relative bioavailability of extended-release lamotrigine was approximately 21% lower than immediate-release lamotrigine in subjects receiving enzyme-inducing AEDs. However, a reduction in exposure of up to 70% was observed in some subjects in this group when they switched to lamotrigine extended-release tablets. Therefore, doses may need to be adjusted in some subjects based on therapeutic response.
Table 5. Steady-State Bioavailability of Lamotrigine Extended-Release Tablets Relative to Immediate-Release Lamotrigine at Equivalent Daily Doses (Ratio of Extended-Release to Immediate-Release 90% CI) a Enzyme-inducing antiepileptic drugs include carbamazepine, phenytoin, phenobarbital, and primidone.
Concomitant Antiepileptic Drug
AUC (0-24ss)
Cmax
Cmin
Enzyme-inducing antiepileptic drugsa
0.79 (0.69, 0.90)
0.71 (0.61, 0.82)
0.99 (0.89, 1.09)
Valproate
0.94 (0.81, 1.08)
0.88 (0.75, 1.03)
0.99 (0.88, 1.10)
Antiepileptic drugs other than enzyme-inducing antiepileptic drugsa or valproate
1.00 (0.88, 1.14)
0.89 (0.78, 1.03)
1.14 (1.03, 1.25)
Dose Proportionality: In healthy volunteers not receiving any other medications and given lamotrigine extended-release tablets once daily, the systemic exposure to lamotrigine increased in direct proportion to the dose administered over the range of 50 to 200 mg. At doses between 25 and 50 mg, the increase was less than dose proportional, with a 2-fold increase in dose resulting in an approximately 1.6-fold increase in systemic exposure.
Distribution: Estimates of the mean apparent volume of distribution (Vd/F) of lamotrigine following oral administration ranged from 0.9 to 1.3 L/kg. Vd/F is independent of dose and is similar following single and multiple doses in both patients with epilepsy and in healthy volunteers.
Protein Binding: Data from in vitro studies indicate that lamotrigine is approximately 55% bound to human plasma proteins at plasma lamotrigine concentrations from 1 to 10 mcg/mL (10 mcg/mL is 4 to 6 times the trough plasma concentration observed in the controlled efficacy trials). Because lamotrigine is not highly bound to plasma proteins, clinically significant interactions with other drugs through competition for protein binding sites are unlikely. The binding of lamotrigine to plasma proteins did not change in the presence of therapeutic concentrations of phenytoin, phenobarbital, or valproate. Lamotrigine did not displace other AEDs (carbamazepine, phenytoin, phenobarbital) from protein-binding sites.
Metabolism: Lamotrigine is metabolized predominantly by glucuronic acid conjugation; the major metabolite is an inactive 2-N-glucuronide conjugate. After oral administration of 240 mg of 14C-lamotrigine (15 μCi) to 6 healthy volunteers, 94% was recovered in the urine and 2% was recovered in the feces. The radioactivity in the urine consisted of unchanged lamotrigine (10%), the 2-N-glucuronide (76%), a 5-N-glucuronide (10%), a 2-N-methyl metabolite (0.14%), and other unidentified minor metabolites (4%).
Enzyme Induction: The effects of lamotrigine on the induction of specific families of mixed-function oxidase isozymes have not been systematically evaluated.
Following multiple administrations (150 mg twice daily) to normal volunteers taking no other medications, lamotrigine induced its own metabolism, resulting in a 25% decrease in t½ and a 37% increase in CL/F at steady state compared with values obtained in the same volunteers following a single dose. Evidence gathered from other sources suggests that self-induction by lamotrigine may not occur when lamotrigine is given as adjunctive therapy in patients receiving enzyme-inducing drugs such as carbamazepine, phenytoin, phenobarbital, primidone, or other drugs such as rifampin that induce lamotrigine glucuronidation [see Drug Interactions (7)].
Elimination: The elimination half-life and apparent clearance of lamotrigine following oral administration of immediate-release lamotrigine to adult patients with epilepsy and healthy volunteers is summarized in Table 6. Half-life and apparent clearance vary depending on concomitant AEDs.
Since the half-life of lamotrigine following administration of single doses of immediate-release lamotrigine is comparable to that observed following administration of lamotrigine extended-release tablets, similar changes in the half-life of lamotrigine would be expected for lamotrigine extended-release tablets.
Table 6. Meana Pharmacokinetic Parameters of Immediate-Release Lamotrigine in Healthy Volunteers and Adult Patients With Epilepsy a The majority of parameter means determined in each study had coefficients
of variation between 20% and 40% for half-life and CL/F and between 30%
and 70% for Tmax. The overall mean values were calculated from individual
study means that were weighted based on the number of volunteers/patients in
each study. The numbers in parentheses below each parameter mean represent
the range of individual volunteer/patient values across studies.
b Carbamazepine, phenobarbital, phenytoin, and primidone have been shown to
increase the apparent clearance of lamotrigine. Estrogen-containing oral
contraceptives and other drugs such as rifampin that induce lamotrigine
glucuronidation have also been shown to increase the apparent clearance of
lamotrigine [see Drug Interactions (7)].
Adult Study Population
Number of
Subjects
t½:
Elimination Half-life
(hr)
CL/F:
Apparent Plasma
Clearance
(mL/min/kg)
Healthy volunteers taking no other
medications:
Single-dose lamotrigine
179
32.8
0.44
(14.0-103.0)
(0.12-1.10)
Multiple-dose lamotrigine
36
25.4
0.58
(11.6-61.6)
(0.24-1.15)
Healthy volunteers taking valproate:
Single-dose lamotrigine
6
48.3
0.30
(31.5-88.6)
(0.14-0.42)
Multiple-dose lamotrigine
18
70.3
0.18
(41.9-113.5)
(0.12-0.33)
Patients with epilepsy taking
valproate only:
Single-dose lamotrigine
4
58.8
0.28
(30.5-88.8)
(0.16-0.40)
Patients with epilepsy taking
carbamazepine, phenytoin,
phenobarbital, or primidoneb plus
valproate:
Single-dose lamotrigine
25
27.2
0.53
(11.2-51.6)
(0.27-1.04)
Patients with epilepsy taking
carbamazepine, phenytoin,
phenobarbital, or primidone: b
Single-dose lamotrigine
24
14.4
1.10
(6.4-30.4)
(0.51-2.22)
Multiple-dose lamotrigine
17
12.6
1.21
(7.5-23.1)
(0.66-1.82)
Drug Interactions: The apparent clearance of lamotrigine is affected by the coadministration of certain medications [see Warnings and Precautions (5.7, 5.11), Drug Interactions (7)].
The net effects of drug interactions with lamotrigine are summarized in Table 7. Details of the drug interaction studies, which were done using immediate-release lamotrigine, are provided following Table 7.
Table 7. Summary of Drug Interactions With Lamotrigine a From adjunctive clinical trials and volunteer studies.
b Net effects were estimated by comparing the mean clearance values obtained in adjunctive clinical trials and volunteer studies.
c The effect of other hormonal contraceptive preparations or hormone replacement therapy on the pharmacokinetics of lamotrigine has not been systematically evaluated in clinical trials, although the effect may be similar to that seen with the ethinylestradiol/levonorgestrel combinations.
d Modest decrease in levonorgestrel.
e Not administered, but an active metabolite of carbamazepine.
f Slight decrease, not expected to be clinically relevant.
g Not administered, but an active metabolite of oxcarbazepine.
h Slight increase, not expected to be clinically relevant.
↔ = No significant effect.
? = Conflicting data.
Drug
Drug Plasma
Concentration With
Adjunctive
Lamotriginea
Lamotrigine Plasma
Concentration With
Adjunctive Drugsb
Oral contraceptives (e.g.,
ethinylestradiol/levonorgestrelc)
↔d
↓
Bupropion
Not assessed
↔
Carbamazepine
↔
↓
Carbamazepine epoxidee
?
Felbamate
Not assessed
↔
Gabapentin
Not assessed
↔
Levetiracetam
↔
↔
Lithium
↔
Not assessed
Olanzapine
↔
↔f
Oxcarbazepine
↔
↔
10-monohydroxy oxcarbazepine metaboliteg
↔
Phenobarbital/primidone
↔
↓
Phenytoin
↔
↓
Pregabalin
↔
↔
Rifampin
Not assessed
↓
Topiramate
↔h
↔
Valproate
↓
↑
Valproate + phenytoin and/or carbamazepine
Not assessed
↔
Zonisamide
Not assessed
↔
Estrogen-Containing Oral Contraceptives: In 16 female volunteers, an oral contraceptive preparation containing 30 mcg ethinylestradiol and 150 mcg levonorgestrel increased the apparent clearance of lamotrigine (300 mg/day) by approximately 2-fold with mean decreases in AUC of 52% and in Cmax of 39%. In this study, trough serum lamotrigine concentrations gradually increased and were approximately 2-fold higher on average at the end of the week of the inactive hormone preparation compared with trough lamotrigine concentrations at the end of the active hormone cycle.
Gradual transient increases in lamotrigine plasma levels (approximate 2-fold increase) occurred during the week of inactive hormone preparation (pill-free week) for women not also taking a drug that increased the clearance of lamotrigine (carbamazepine, phenytoin, phenobarbital, primidone, or other drugs that induce lamotrigine glucuronidation [see Drug Interactions (7)]. The increase in lamotrigine plasma levels will be greater if the dose of lamotrigine extended-release tablet is increased in the few days before or during the pill-free week. Increases in lamotrigine plasma levels could result in dose-dependent adverse reactions.
In the same study, coadministration of lamotrigine (300 mg/day) in 16 female volunteers did not affect the pharmacokinetics of the ethinylestradiol component of the oral contraceptive preparation. There were mean decreases in the AUC and Cmax of the levonorgestrel component of 19% and 12%, respectively. Measurement of serum progesterone indicated that there was no hormonal evidence of ovulation in any of the 16 volunteers, although measurement of serum FSH, LH, and estradiol indicated that there was some loss of suppression of the hypothalamic-pituitary-ovarian axis.
The effects of doses of lamotrigine other than 300 mg/day have not been systematically evaluated in controlled clinical trials.
The clinical significance of the observed hormonal changes on ovulatory activity is unknown. However, the possibility of decreased contraceptive efficacy in some patients cannot be excluded. Therefore, patients should be instructed to promptly report changes in their menstrual pattern (e.g., break-through bleeding).
Dosage adjustments may be necessary for women receiving estrogen-containing oral contraceptive preparations [see Dosage and Administration (2.1)].
Other Hormonal Contraceptives or Hormone Replacement Therapy: The effect of other hormonal contraceptive preparations or hormone replacement therapy on the pharmacokinetics of lamotrigine has not been systematically evaluated. It has been reported that ethinylestradiol, not progestogens, increased the clearance of lamotrigine up to 2-fold, and the progestin-only pills had no effect on lamotrigine plasma levels. Therefore, adjustments to the dosage of lamotrigine extended-release tablets in the presence of progestogens alone will likely not be needed.
Bupropion: The pharmacokinetics of a 100-mg single dose of lamotrigine in healthy volunteers (n = 12) were not changed by coadministration of bupropion sustained-release formulation (150 mg twice daily) starting 11 days before lamotrigine.
Carbamazepine: Lamotrigine has no appreciable effect on steady-state carbamazepine plasma concentration. Limited clinical data suggest there is a higher incidence of dizziness, diplopia, ataxia, and blurred vision in patients receiving carbamazepine with lamotrigine than in patients receiving other AEDs with lamotrigine [see Adverse Reactions (6.1)]. The mechanism of this interaction is unclear. The effect of lamotrigine on plasma concentrations of carbamazepine-epoxide is unclear. In a small subset of patients (n = 7) studied in a placebo-controlled trial, lamotrigine had no effect on carbamazepine-epoxide plasma concentrations, but in a small, uncontrolled study (n = 9), carbamazepine-epoxide levels increased.
The addition of carbamazepine decreases lamotrigine steady-state concentrations by approximately 40%.
Esomeprazole: In a study of 30 subjects, coadministration of lamotrigine extended-release tablets with esomeprazole resulted in no significant change in lamotrigine levels and a small decrease in Tmax. The levels of gastric pH were not altered compared with pre-lamotrigine dosing.
Felbamate: In a study of 21 healthy volunteers, coadministration of felbamate (1,200 mg twice daily) with lamotrigine (100 mg twice daily for 10 days) appeared to have no clinically relevant effects on the pharmacokinetics of lamotrigine.
Folate Inhibitors: Lamotrigine is a weak inhibitor of dihydrofolate reductase. Prescribers should be aware of this action when prescribing other medications that inhibit folate metabolism.
Gabapentin: Based on a retrospective analysis of plasma levels in 34 patients who received lamotrigine both with and without gabapentin, gabapentin does not appear to change the apparent clearance of lamotrigine.
Levetiracetam: Potential drug interactions between levetiracetam and lamotrigine were assessed by evaluating serum concentrations of both agents during placebo-controlled clinical trials. These data indicate that lamotrigine does not influence the pharmacokinetics of levetiracetam and that levetiracetam does not influence the pharmacokinetics of lamotrigine.
Lithium: The pharmacokinetics of lithium were not altered in healthy subjects (n = 20) by coadministration of lamotrigine (100 mg/day) for 6 days.
Olanzapine: The AUC and Cmax of olanzapine were similar following the addition of olanzapine (15 mg once daily) to lamotrigine (200 mg once daily) in healthy male volunteers (n = 16) compared with the AUC and Cmax in healthy male volunteers receiving olanzapine alone (n = 16).
In the same study, the AUC and Cmax of lamotrigine were reduced on average by 24% and 20%, respectively, following the addition of olanzapine to lamotrigine in healthy male volunteers compared with those receiving lamotrigine alone. This reduction in lamotrigine plasma concentrations is not expected to be clinically relevant.
Oxcarbazepine: The AUC and Cmax of oxcarbazepine and its active 10-monohydroxy oxcarbazepine metabolite were not significantly different following the addition of oxcarbazepine (600 mg twice daily) to lamotrigine (200 mg once daily) in healthy male volunteers (n = 13) compared with healthy male volunteers receiving oxcarbazepine alone (n = 13).
In the same study, the AUC and Cmax of lamotrigine were similar following the addition of oxcarbazepine (600 mg twice daily) to lamotrigine in healthy male volunteers compared with those receiving lamotrigine alone. Limited clinical data suggest a higher incidence of headache, dizziness, nausea, and somnolence with coadministration of lamotrigine and oxcarbazepine compared with lamotrigine alone or oxcarbazepine alone.
Phenobarbital, Primidone: The addition of phenobarbital or primidone decreases lamotrigine steady-state concentrations by approximately 40%.
Phenytoin: Lamotrigine has no appreciable effect on steady-state phenytoin plasma concentrations in patients with epilepsy. The addition of phenytoin decreases lamotrigine steady-state concentrations by approximately 40%.
Pregabalin: Steady-state trough plasma concentrations of lamotrigine were not affected by concomitant pregabalin (200 mg 3 times daily) administration. There are no pharmacokinetic interactions between lamotrigine and pregabalin.
Rifampin: In 10 male volunteers, rifampin (600 mg/day for 5 days) significantly increased the apparent clearance of a single 25-mg dose of lamotrigine by approximately 2-fold (AUC decreased by approximately 40%).
Topiramate: Topiramate resulted in no change in plasma concentrations of lamotrigine. Administration of lamotrigine resulted in a 15% increase in topiramate concentrations.
Valproate: When lamotrigine was administered to healthy volunteers (n = 18) receiving valproate, the trough steady-state valproate plasma concentrations decreased by an average of 25% over a 3-week period, and then stabilized. However, adding lamotrigine to the existing therapy did not cause a change in valproate plasma concentrations in either adult or pediatric patients in controlled clinical trials.
The addition of valproate increased lamotrigine steady-state concentrations in normal volunteers by slightly more than 2-fold. In one study, maximal inhibition of lamotrigine clearance was reached at valproate doses between 250 and 500 mg/day and did not increase as the valproate dose was further increased.
Zonisamide: In a study of 18 patients with epilepsy, coadministration of zonisamide (200 to 400 mg/day) with lamotrigine (150 to 500 mg/day for 35 days) had no significant effect on the pharmacokinetics of lamotrigine.
Known Inducers or Inhibitors of Glucuronidation: Drugs other than those listed above have not been systematically evaluated in combination with lamotrigine. Since lamotrigine is metabolized predominately by glucuronic acid conjugation, drugs that are known to induce or inhibit glucuronidation may affect the apparent clearance of lamotrigine, and doses of lamotrigine extended-release tablets may require adjustment based on clinical response.
Other: Results of in vitro experiments suggest that clearance of lamotrigine is unlikely to be reduced by concomitant administration of amitriptyline, clonazepam, clozapine, fluoxetine, haloperidol, lorazepam, phenelzine, risperidone, sertraline, or trazodone.
Results of in vitro experiments suggest that lamotrigine does not reduce the clearance of drugs eliminated predominantly by CYP2D6.
Special Populations: Patients With Renal Impairment: Twelve volunteers with chronic renal failure (mean creatinine clearance: 13 mL/min; range: 6 to 23) and another 6 individuals undergoing hemodialysis were each given a single 100-mg dose of immediate-release lamotrigine. The mean plasma half-lives determined in the study were 42.9 hours (chronic renal failure), 13.0 hours (during hemodialysis), and 57.4 hours (between hemodialysis) compared with 26.2 hours in healthy volunteers. On average, approximately 20% (range: 5.6 to 35.1) of the amount of lamotrigine present in the body was eliminated by hemodialysis during a 4-hour session [see Dosage and Administration (2.1)].
Hepatic Disease: The pharmacokinetics of lamotrigine following a single 100-mg dose of immediate-release lamotrigine were evaluated in 24 subjects with mild, moderate, and severe hepatic impairment (Child-Pugh Classification system) and compared with 12 subjects without hepatic impairment. The patients with severe hepatic impairment were without ascites (n = 2) or with ascites (n = 5). The mean apparent clearances of lamotrigine in patients with mild (n = 12), moderate (n = 5), severe without ascites (n = 2), and severe with ascites (n = 5) liver impairment were 0.30 ± 0.09, 0.24 ± 0.1, 0.21 ± 0.04, and 0.15 ± 0.09 mL/min/kg, respectively, as compared with 0.37 ± 0.1 mL/min/kg in the healthy controls. Mean half-lives of lamotrigine in patients with mild, moderate, severe without ascites, and severe with ascites hepatic impairment were 46 ± 20, 72 ± 44, 67 ± 11, and 100 ± 48 hours, respectively, as compared with 33 ± 7 hours in healthy controls [see Dosage and Administration (2.1)].
Elderly: The pharmacokinetics of lamotrigine following a single 150-mg dose of immediate-release lamotrigine were evaluated in 12 elderly volunteers between the ages of 65 and 76 years (mean creatinine clearance: 61 mL/min, range: 33 to 108 mL/min). The mean half-life of lamotrigine in these subjects was 31.2 hours (range: 24.5 to 43.4 hours), and the mean clearance was 0.40 mL/min/kg (range: 0.26 to 0.48 mL/min/kg).
Gender: The clearance of lamotrigine is not affected by gender. However, during dose escalation of immediate-release lamotrigine in one clinical trial in patients with epilepsy on a stable dose of valproate (n = 77), mean trough lamotrigine concentrations, unadjusted for weight, were 24% to 45% higher (0.3 to 1.7 mcg/mL) in females than in males.
Race: The apparent oral clearance of lamotrigine was 25% lower in non-Caucasians than Caucasians.
Pediatric Patients: Safety and effectiveness of lamotrigine extended-release tablets for use in patients less than 13 years of age have not been established.
-
13. NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment Of Fertility
No evidence of carcinogenicity was seen in mouse or rat following oral administration of lamotrigine for up to 2 years at doses up to 30 mg/kg/day and 10 to 15 mg/kg/day in mouse and rat, respectively. The highest doses tested are less than the human dose of 400 mg/day on a body surface area (mg/m2) basis.
Lamotrigine was negative in in vitro gene mutation (Ames and mouse lymphoma tk) assays and in clastogenicity (in vitro human lymphocyte and in vivo rat bone marrow) assays.
No evidence of impaired fertility was detected in rats given oral doses of lamotrigine up to 20 mg/kg/day. The highest dose tested is less than the human dose of 400 mg/day on a mg/m2 basis.
-
14. CLINICAL STUDIES
14.2 Adjunctive Therapy for Partial Onset Seizures
The effectiveness of immediate-release lamotrigine as adjunctive therapy was initially established in 3 pivotal multicenter, placebo-controlled, double-blind clinical trials in 355 adults with refractory partial onset seizures.
The effectiveness of lamotrigine extended-release tablets as adjunctive therapy in partial onset seizures, with or without secondary generalization, was established in a 19-week, multicenter, double-blind, placebo-controlled trial in 236 patients, 13 years of age and older (approximately 93% of patients were aged 16 to 65 years). Approximately 36% were from the U.S. and approximately 64% were from other countries including Argentina, Brazil, Chile, Germany, India, Korea, Russian Federation, and Ukraine. Patients with at least 8 partial onset seizures during an 8-week prospective baseline phase (or 4-week prospective baseline coupled with a 4-week historical baseline documented with seizure diary data) were randomized to treatment with lamotrigine extended-release tablets (n = 116) or placebo (n = 120) added to their current regimen of 1 or 2 AEDs. Approximately half of the patients were taking 2 concomitant AEDs at baseline. Target doses ranged from 200 to 500 mg/day of lamotrigine extended-release tablets based on concomitant AED (target dose = 200 mg for valproate, 300 mg for AEDs not altering plasma lamotrigine, and 500 mg for enzyme-inducing AEDs). The median partial seizure frequency per week at baseline was 2.3 for lamotrigine extended-release tablets and 2.1 for placebo.
The primary endpoint was the median percent change from baseline in partial onset seizure frequency during the entire double-blind treatment phase. The median percent reductions in weekly partial onset seizures were 47% in patients treated with lamotrigine extended-release tablets and 25% on placebo, a difference that was statistically significant, defined as a 2-sided P value <0.05.
Figure 1 presents the percentage of patients (X-axis) with a percent reduction in partial seizure frequency (responder rate) from baseline through the entire treatment period at least as great as that represented on the Y-axis. The proportion of patients achieving any particular level of reduction in partial seizure frequency was consistently higher for the group treated with lamotrigine extended-release tablets compared with the placebo group. For example, 44% of patients randomized to lamotrigine extended-release tablets experienced a 50% or greater reduction in partial seizure frequency, compared with 21% of patients randomized to placebo.
Figure 1. Proportion of Patients by Responder Rate for Lamotrigine Extended-Release Tablets and Placebo Group (Partial Onset Seizure Study)
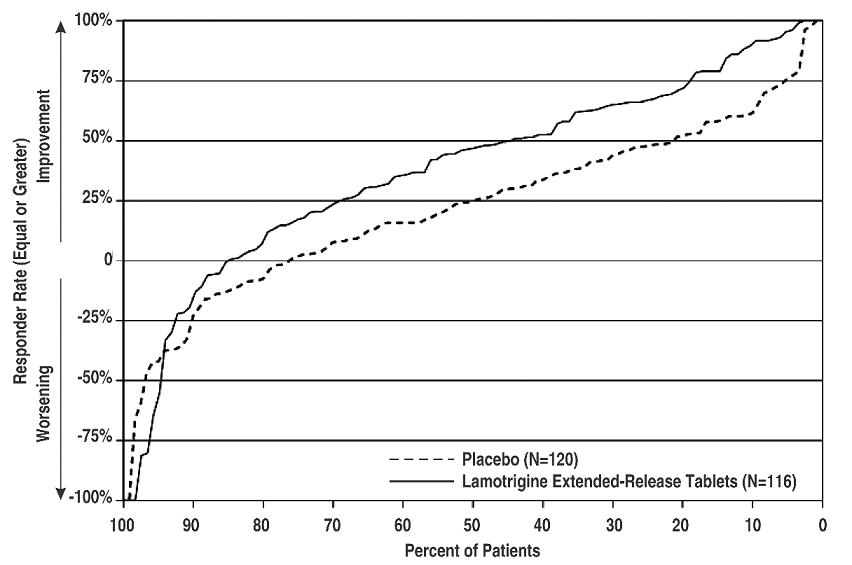
- 15. REFERENCES
-
16. HOW SUPPLIED/STORAGE AND HANDLING
Lamotrigine extended-release tablets
25 mg are available as yellow, enteric-coated, circular shaped tablets, debossed with "W" on one side and "271" on the other side.
NDC: 64679-271-01, bottle of 30 tablets
NDC: 64679-271-02, bottle of 500 tablets
NDC: 64679-271-04, unit dose of 100 tablets
50 mg are available as pink, enteric-coated, circular shaped tablets, debossed with "W" on one side and "274" on the other side.
NDC: 64679-274-01, bottle of 30 tablets
NDC: 64679-274-02, bottle of 500 tablets
NDC: 64679-274-03, unit dose of 100 tablets
100 mg are available as light brown, enteric-coated, circular shaped tablets, debossed with "W" on one side and "273" on the other side.
NDC: 64679-273-01, bottle of 30 tablets
NDC: 64679-273-02, bottle of 500 tablets
NDC: 64679-273-04, unit dose of 100 tablets
200 mg are available as pink, enteric-coated, circular shaped tablets, debossed with "W" on one side and "272" on the other side.
NDC: 64679-272-01, bottle of 30 tablets
NDC: 64679-272-02, bottle of 500 tablets
NDC: 64679-272-04, unit dose of 100 tablets
300 mg are available as pink, enteric-coated, circular shaped tablets, debossed with "W" on one side and "275" on the other side.
NDC: 64679-275-01, bottle of 30 tablets
NDC: 64679-275-02, bottle of 500 tablets
NDC: 64679-275-04, unit dose of 100 tablets
Storage: Store at 20°-25°C (68°-77°F); [see USP Controlled Room Temperature].
-
17. PATIENT COUNSELING INFORMATION
See FDA-approved patient labeling (Medication Guide).
17.1 Rash
Prior to initiation of treatment with lamotrigine extended-release tablets, the patient should be instructed that a rash or other signs or symptoms of hypersensitivity (e.g., fever, lymphadenopathy) may herald a serious medical event and that the patient should report any such occurrence to a physician immediately.
17.2 Multiorgan Hypersensitivity Reactions, Blood Dyscrasias and Organ Failure
Patients should be instructed that multiorgan hypersensitivity reactions and acute multiorgan failure may occur with lamotrigine. Isolated organ failure or isolated blood dyscrasias without evidence of multiorgan hypersensitivity may also occur. Patients should contact their physician immediately if they experience any signs or symptoms of these conditions [see Warnings and Precautions (5.2, 5.3)].
17.3 Suicidal Thinking and Behavior
Patients, their caregivers, and families should be counseled that AEDs, including lamotrigine extended-release tablets, may increase the risk of suicidal thoughts and behavior and should be advised of the need to be alert for the emergence or worsening of symptoms of depression; any unusual changes in mood or behavior, or the emergence of suicidal thoughts, behavior; or thoughts about self-harm. Behaviors of concern should be reported immediately to healthcare providers.
17.4 Worsening of Seizures
Patients should be advised to notify their physician if worsening of seizure control occurs.
17.5 Central Nervous System Adverse Effects
Patients should be advised that lamotrigine extended-release tablets may cause dizziness, somnolence, and other symptoms and signs of central nervous system depression. Accordingly, they should be advised neither to drive a car nor to operate other complex machinery until they have gained sufficient experience on lamotrigine extended-release tablets to gauge whether or not it adversely affects their mental and/or motor performance.
17.6 Pregnancy and Nursing
Patients should be advised to notify their physicians if they become pregnant or intend to become pregnant during therapy. Patients should be advised to notify their physicians if they intend to breastfeed or are breastfeeding an infant.
Patients should also be encouraged to enroll in the NAAED Pregnancy Registry if they become pregnant. This registry is collecting information about the safety of antiepileptic drugs during pregnancy. To enroll, patients can call the toll-free number 1-888-233-2334 [see Use in Specific Populations (8.1)].
Patients who intend to breastfeed should be informed that lamotrigine extended-release tablet is present in breast milk and that they should monitor their child for potential adverse effects of this drug. Benefits and risks of continuing breastfeeding should be discussed with the patient.
17.7 Oral Contraceptive Use
Women should be advised to notify their physician if they plan to start or stop use of oral contraceptives or other female hormonal preparations. Starting estrogen-containing oral contraceptives may significantly decrease lamotrigine plasma levels and stopping estrogen-containing oral contraceptives (including the pill-free week) may significantly increase lamotrigine plasma levels [see Warnings and Precautions (5.7), Clinical Pharmacology (12.3)]. Women should also be advised to promptly notify their physician if they experience adverse reactions or changes in menstrual pattern (e.g., break-through bleeding) while receiving lamotrigine extended-release tablets in combination with these medications.
17.8 Discontinuing lamotrigine extended-release tablets
Patients should be advised to notify their physician if they stop taking lamotrigine extended-release tablets for any reason and not to resume lamotrigine extended-release tablets without consulting their physician.
17.9 Aseptic Meningitis
Patients should be advised that lamotrigine extended-release tablets may cause aseptic meningitis. Patients should be advised to notify their physician immediately if they develop signs and symptoms of meningitis such as headache, fever, nausea, vomiting, stiff neck, rash, abnormal sensitivity to light, myalgia, chills, confusion, or drowsiness while taking lamotrigine extended-release tablets.
17.10 Potential Medication Errors
Medication errors involving lamotrigine have occurred. In particular, the name lamotrigine can be confused with the names of other commonly used medications. Medication errors may also occur between the different formulations of lamotrigine. To reduce the potential of medication errors, write and say lamotrigine extended-release tablets clearly. Depictions of the lamotrigine extended-release tablets can be found in the Medication Guide. Each lamotrigine extended-release tablet has a distinct debossing and is debossed with "W" on one side and "271" on the other side for 25 mg; "W" on one side and "274" on the other side for 50 mg; "W" on one side and "273" on the other side for 100 mg; "W" on one side and "272" on the other side for 200 mg and "W" on one side and "275" on the other side for 300 mg. These distinctive features serve to identify the different presentations of the drug and thus may help reduce the risk of medication errors. Lamotrigine extended-release tablets are supplied in circular, unit-of-use bottles containing 30 tablets and 100 unit dose blister pack. Additionally, lamotrigine extended-release tablets are also supplied as 500 count bottle pack. The label on the bottle includes a depiction of the tablets which further communicates to patients and pharmacists that the medication is lamotrigine extended-release tablets and the specific tablet strength included in the bottle. To avoid the medication error of using the wrong drug or formulation, patients should be strongly advised to visually inspect their tablets to verify that they are lamotrigine extended-release tablets each time they fill their prescription and to immediately talk to their doctor/pharmacist if they receive a lamotrigine extended-release tablets without debossed on the tablet as they may have received the wrong medication [see Dosage Forms and Strengths (3), How Supplied/Storage and Handling (16)].
-
MEDICATION GUIDE
Lamotrigine Extended-Release Tablets
Read this Medication Guide before you start taking lamotrigine extended-release tablets and each time you get a refill. There may be new information. This information does not take the place of talking with your healthcare provider about your medical condition or treatment. If you have questions about lamotrigine extended-release tablets, ask your healthcare provider or pharmacist.
What is the most important information I should know about lamotrigine extended-release tablets?
1. Lamotrigine extended-release tablets may cause a serious skin rash that may cause you to be hospitalized or to stop lamotrigine extended-release tablets; it may rarely cause death.
There is no way to tell if a mild rash will develop into a more serious reaction. These serious skin reactions are more likely to happen when you begin taking lamotrigine extended-release tablets, within the first 2 to 8 weeks of treatment. But it can happen in people who have taken lamotrigine extended-release tablets for any period of time. Children between 2 to 16 years of age have a higher chance of getting this serious skin reaction while taking lamotrigine. Lamotrigine extended-release tablet is not approved for use in children less than 13 years of age.
The risk of getting a rash is higher if you:
- take lamotrigine extended-release tablets while taking valproate [DEPAKENE® (valproic acid) or DEPAKOTE® (divalproex sodium)].
- take a higher starting dose of lamotrigine extended-release tablets than your healthcare provider prescribed.
- increase your dose of lamotrigine extended-release tablets faster than prescribed.
Lamotrigine extended-release tablets can also cause other types of allergic reactions or serious problems that may affect organs and other parts of your body like the liver or blood cells. You may or may not have a rash with these types of reactions.
Call your healthcare provider right away if you have any of the following:
- a skin rash
- hives
- fever
- swollen lymph glands
- painful sores in the mouth or around your eyes
- swelling of your lips or tongue
- yellowing of your skin or eyes
- unusual bruising or bleeding
- severe fatigue or weakness
- severe muscle pain
- frequent infections
These symptoms may be the first signs of a serious skin reaction. A healthcare provider should examine you to decide if you should continue taking lamotrigine extended-release tablets.
2. Like other antiepileptic drugs, lamotrigine extended-release tablets may cause suicidal thoughts or actions in a very small number of people, about 1 in 500.
Call a healthcare provider right away if you have any of these symptoms, especially if they are new, worse, or worry you:
- thoughts about suicide or dying
- attempt to commit suicide
- new or worse depression
- new or worse anxiety
- feeling agitated or restless
- panic attacks
- trouble sleeping (insomnia)
- new or worse irritability
- acting aggressive, being angry, or violent
- acting on dangerous impulses
- an extreme increase in activity and talking (mania)
- other unusual changes in behavior or mood
Do not stop lamotrigine extended-release tablets without first talking to a healthcare provider.
- Stopping lamotrigine extended-release tablets suddenly can cause serious problems.
- Suicidal thoughts or actions can be caused by things other than medicines. If you have suicidal thoughts or actions, your healthcare provider may check for other causes.
How can I watch for early symptoms of suicidal thoughts and actions?
- Pay attention to any changes, especially sudden changes, in mood, behaviors, thoughts, or feelings.
- Keep all follow-up visits with your healthcare provider as scheduled.
- Call your healthcare provider between visits as needed, especially if you are worried about symptoms.
3. Lamotrigine extended-release tablets may rarely cause aseptic meningitis, a serious inflammation of the protective membrane that covers the brain and spinal cord.
Call your healthcare provider right away if you have any of the following symptoms:
- Headache
- Fever
- Nausea
- Vomiting
- Stiff neck
- Rash
- Unusual sensitivity to light
- Muscle pains
- Chills
- Confusion
- Drowsiness
Meningitis has many causes other than lamotrigine extended-release tablets, which your doctor would check for if you developed meningitis while taking lamotrigine extended-release tablets.
Lamotrigine extended-release tablets can have other serious side effects. For more information ask your healthcare provider or pharmacist. Tell your healthcare provider if you have any side effect that bothers you. Be sure to read the section below entitled "What are the possible side effects of lamotrigine extended-release tablets?"
4. Patients prescribed lamotrigine tablets have sometimes been given the wrong medicine because many medicines have names similar to lamotrigine tablets, so always check that you receive lamotrigine extended-release tablets.
Taking the wrong medication can cause serious health problems. When your healthcare provider gives you a prescription for lamotrigine extended-release tablets:
- Make sure you can read it clearly.
- Talk to your pharmacist to check that you are given the correct medicine.
- Each time you fill your prescription, check the tablets you receive against the pictures of the tablets below.
These pictures show the distinct wording, debossing, and sizes of the tablets that help to identify the right strength of lamotrigine extended-release tablets. Immediately call your pharmacist if you receive a lamotrigine extended-release tablet that does not look like one of the tablets shown below, as you may have received the wrong medication.
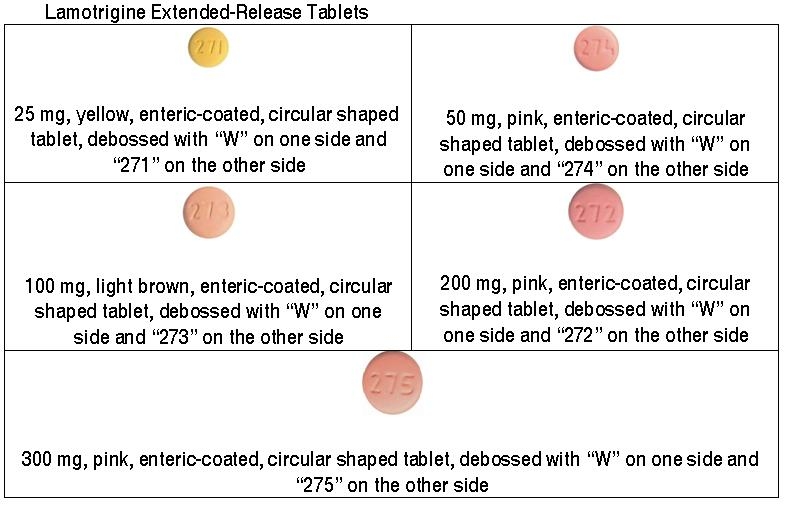

What is lamotrigine extended-release tablet?
Lamotrigine extended-release tablet is a prescription medicine used:
- together with other medicines to treat partial onset seizures in people 13 years of age and older.
It is not known if lamotrigine extended-release tablet is safe or effective in children less than 13 years of age. Other forms of lamotrigine can be used in children 2 to 12 years.
Who should not take lamotrigine extended-release tablets?
You should not take lamotrigine extended-release tablets if you have had an allergic reaction to lamotrigine or to any of the inactive ingredients in lamotrigine extended-release tablets. See the end of this leaflet for a complete list of ingredients in lamotrigine extended-release tablets.
What should I tell my healthcare provider before taking lamotrigine extended-release tablets?
Before taking lamotrigine extended-release tablets, tell your healthcare provider about all of your medical conditions, including if you:
- have had a rash or allergic reaction to another antiseizure medicine.
- have or have had depression, mood problems or suicidal thoughts or behavior.
- are taking oral contraceptives (birth control pills) or other female hormonal medicines. Do not start or stop taking birth control pills or other female hormonal medicine until you have talked with your healthcare provider. Tell your healthcare provider if you have any changes in your menstrual pattern such as breakthrough bleeding. Stopping these medicines may cause side effects (such as dizziness, lack of coordination, or double vision). Starting these medicines may lessen how well lamotrigine extended-release tablet works.
- are pregnant or plan to become pregnant. It is not known if lamotrigine extended-release tablets will harm your unborn baby. If you become pregnant while taking lamotrigine extended-release tablets, talk to your healthcare provider about registering with the North American Antiepileptic Drug Pregnancy Registry. You can enroll in this registry by calling 1-888-233-2334. The purpose of this registry is to collect information about the safety of antiepileptic drugs during pregnancy.
- are breastfeeding. Lamotrigine extended-release tablet passes into breast milk and may cause side effects in a breastfed baby. If you breastfeed while taking lamotrigine extended-release tablets, watch your baby closely for trouble breathing, episodes of temporarily stopping breathing, sleepiness, or poor sucking. Call your baby’s healthcare provider right away if you see any of these problems. Talk to your healthcare provider about the best way to feed your baby if you take lamotrigine extended-release tablets.
Tell your healthcare provider about all the medicines you take or if you are planning to take a new medicine, including prescription and non-prescription medicines, vitamins, and herbal supplements. Using lamotrigine extended-release tablets with certain other medicines can affect each other, causing side effects.
How should I take lamotrigine extended-release tablets?
- Take lamotrigine extended-release tablets exactly as prescribed.
- Your healthcare provider may change your dose. Do not change your dose without talking to your healthcare provider.
- Do not stop taking lamotrigine extended-release tablets without talking to your healthcare provider. Stopping lamotrigine extended-release tablets suddenly may cause serious problems. For example, if you have epilepsy and you stop taking lamotrigine extended-release tablets suddenly, you may get seizures that do not stop. Talk with your healthcare provider about how to stop lamotrigine extended-release tablets slowly.
- If you miss a dose of lamotrigine extended-release tablets, take it as soon as you remember. If it is almost time for your next dose, just skip the missed dose. Take the next dose at your regular time. Do not take 2 doses at the same time.
- You may not feel the full effect of lamotrigine extended-release tablets for several weeks.
- If you have epilepsy, tell your healthcare provider if your seizures get worse or if you have any new types of seizures.
- Lamotrigine extended-release tablets can be taken with or without food.
- Do not chew, crush, or divide lamotrigine extended-release tablets.
- Swallow lamotrigine extended-release tablets whole.
- If you have trouble swallowing lamotrigine extended-release tablets, tell your healthcare provider because there may be another form of lamotrigine you can take.
- If you receive lamotrigine extended-release tablets in a blisterpack, examine the blisterpack before use. Do not use if blisters are torn, broken, or missing.
What should I avoid while taking lamotrigine extended-release tablets?
Do not drive a car or operate complex, hazardous machinery until you know how lamotrigine extended-release tablet affects you.
What are possible side effects of lamotrigine extended-release tablets?
- See "What is the most important information I should know about lamotrigine extended-release tablets?"
Common side effects of lamotrigine extended-release tablets include:
- Dizziness
- Tremor
- Double vision
- Nausea
- Vomiting
- Trouble with balance and coordination
- Anxiety
Other common side effects that have been reported with another form of lamotrigine include headache, sleepiness, blurred vision, runny nose, and rash.
Tell your healthcare provider about any side effect that bothers you or that does not go away. These are not all the possible side effects of lamotrigine extended-release tablets. For more information, ask your healthcare provider or pharmacist.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
How should I store lamotrigine extended-release tablets?
- Store lamotrigine extended-release tablets at room temperature between 20°-25°C (68°-77°F).
- Keep lamotrigine extended-release tablets and all medicines out of the reach of children.
General information about lamotrigine extended-release tablets
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use lamotrigine extended-release tablets for a condition for which it was not prescribed. Do not give lamotrigine extended-release tablets to other people, even if they have the same symptoms you have. It may harm them.
This Medication Guide summarizes the most important information about lamotrigine extended-release tablets. If you would like more information, talk with your healthcare provider. You can ask your healthcare provider or pharmacist for information about lamotrigine extended-release tablets that is written for healthcare professionals.
For more information, call 1-800-346-6854.
What are the ingredients in lamotrigine extended-release tablets?
Active ingredient: Lamotrigine.
Inactive ingredients: diethyl phthalate, hypromellose, lactose monohydrate, magnesium stearate, methacrylic acid copolymer, polyethylene glycol, talc, titanium dioxide, iron oxide yellow for (25 mg and 100 mg) and iron oxide red for (50 mg, 100 mg, 200 mg and 300 mg).
This Medication Guide has been approved by the U.S. Food and Drug Administration.
DEPAKENE® and DEPAKOTE® are registered trademarks of Abbott Laboratories.
Wockhardt Limited,
Mumbai, India.
Distributed by:
Wockhardt USA LLC.
20 Waterview Blvd.
Parsippany, NJ 07054
USA.
Iss.240812
- PRINCIPAL DISPLAY PANEL
-
INGREDIENTS AND APPEARANCE
LAMOTRIGINE
lamotrigine tablet, extended releaseProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 55648-271 Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength LAMOTRIGINE (UNII: U3H27498KS) (LAMOTRIGINE - UNII:U3H27498KS) LAMOTRIGINE 25 mg Inactive Ingredients Ingredient Name Strength DIETHYL PHTHALATE (UNII: UF064M00AF) FERRIC OXIDE YELLOW (UNII: EX438O2MRT) HYPROMELLOSES (UNII: 3NXW29V3WO) LACTOSE MONOHYDRATE (UNII: EWQ57Q8I5X) MAGNESIUM STEARATE (UNII: 70097M6I30) METHACRYLIC ACID - ETHYL ACRYLATE COPOLYMER (1:1) TYPE A (UNII: NX76LV5T8J) POLYETHYLENE GLYCOLS (UNII: 3WJQ0SDW1A) TALC (UNII: 7SEV7J4R1U) TITANIUM DIOXIDE (UNII: 15FIX9V2JP) Product Characteristics Color YELLOW (yellow, coated) Score no score Shape ROUND (circular shaped tablets) Size 10mm Flavor Imprint Code W;271 Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 55648-271-01 30 in 1 BOTTLE 2 NDC: 55648-271-02 500 in 1 BOTTLE 3 NDC: 55648-271-04 10 in 1 CARTON 3 10 in 1 BLISTER PACK Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA202498 11/29/2012 LAMOTRIGINE
lamotrigine tablet, extended releaseProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 55648-274 Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength LAMOTRIGINE (UNII: U3H27498KS) (LAMOTRIGINE - UNII:U3H27498KS) LAMOTRIGINE 50 mg Inactive Ingredients Ingredient Name Strength DIETHYL PHTHALATE (UNII: UF064M00AF) FERRIC OXIDE RED (UNII: 1K09F3G675) HYPROMELLOSES (UNII: 3NXW29V3WO) LACTOSE MONOHYDRATE (UNII: EWQ57Q8I5X) MAGNESIUM STEARATE (UNII: 70097M6I30) METHACRYLIC ACID - ETHYL ACRYLATE COPOLYMER (1:1) TYPE A (UNII: NX76LV5T8J) POLYETHYLENE GLYCOLS (UNII: 3WJQ0SDW1A) TALC (UNII: 7SEV7J4R1U) TITANIUM DIOXIDE (UNII: 15FIX9V2JP) Product Characteristics Color PINK (pink, coated) Score no score Shape ROUND (circular shaped tablets) Size 10mm Flavor Imprint Code W;274 Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 55648-274-01 30 in 1 BOTTLE 2 NDC: 55648-274-02 500 in 1 BOTTLE 3 NDC: 55648-274-03 10 in 1 CARTON 3 10 in 1 BLISTER PACK Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA202498 11/29/2012 LAMOTRIGINE
lamotrigine tablet, extended releaseProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 55648-273 Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength LAMOTRIGINE (UNII: U3H27498KS) (LAMOTRIGINE - UNII:U3H27498KS) LAMOTRIGINE 100 mg Inactive Ingredients Ingredient Name Strength DIETHYL PHTHALATE (UNII: UF064M00AF) FERRIC OXIDE RED (UNII: 1K09F3G675) FERRIC OXIDE YELLOW (UNII: EX438O2MRT) HYPROMELLOSES (UNII: 3NXW29V3WO) LACTOSE MONOHYDRATE (UNII: EWQ57Q8I5X) MAGNESIUM STEARATE (UNII: 70097M6I30) METHACRYLIC ACID - ETHYL ACRYLATE COPOLYMER (1:1) TYPE A (UNII: NX76LV5T8J) POLYETHYLENE GLYCOLS (UNII: 3WJQ0SDW1A) TALC (UNII: 7SEV7J4R1U) TITANIUM DIOXIDE (UNII: 15FIX9V2JP) Product Characteristics Color BROWN (light brown, coated) Score no score Shape ROUND (circular shaped tablets) Size 10mm Flavor Imprint Code W;273 Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 55648-273-01 30 in 1 BOTTLE 2 NDC: 55648-273-02 500 in 1 BOTTLE 3 NDC: 55648-273-04 10 in 1 CARTON 3 10 in 1 BLISTER PACK Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA202498 11/29/2012 LAMOTRIGINE
lamotrigine tablet, extended releaseProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 55648-272 Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength LAMOTRIGINE (UNII: U3H27498KS) (LAMOTRIGINE - UNII:U3H27498KS) LAMOTRIGINE 200 mg Inactive Ingredients Ingredient Name Strength DIETHYL PHTHALATE (UNII: UF064M00AF) FERRIC OXIDE RED (UNII: 1K09F3G675) HYPROMELLOSES (UNII: 3NXW29V3WO) LACTOSE MONOHYDRATE (UNII: EWQ57Q8I5X) MAGNESIUM STEARATE (UNII: 70097M6I30) METHACRYLIC ACID - ETHYL ACRYLATE COPOLYMER (1:1) TYPE A (UNII: NX76LV5T8J) POLYETHYLENE GLYCOLS (UNII: 3WJQ0SDW1A) TALC (UNII: 7SEV7J4R1U) TITANIUM DIOXIDE (UNII: 15FIX9V2JP) Product Characteristics Color PINK (Pink, coated) Score no score Shape ROUND (circular shaped tablets) Size 10mm Flavor Imprint Code W;272 Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 55648-272-01 30 in 1 BOTTLE 2 NDC: 55648-272-02 500 in 1 BOTTLE 3 NDC: 55648-272-04 10 in 1 CARTON 3 10 in 1 BLISTER PACK Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA202498 11/29/2012 LAMOTRIGINE
lamotrigine tablet, extended releaseProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 55648-275 Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength LAMOTRIGINE (UNII: U3H27498KS) (LAMOTRIGINE - UNII:U3H27498KS) LAMOTRIGINE 300 mg Inactive Ingredients Ingredient Name Strength DIETHYL PHTHALATE (UNII: UF064M00AF) FERRIC OXIDE RED (UNII: 1K09F3G675) HYPROMELLOSES (UNII: 3NXW29V3WO) LACTOSE MONOHYDRATE (UNII: EWQ57Q8I5X) MAGNESIUM STEARATE (UNII: 70097M6I30) METHACRYLIC ACID - ETHYL ACRYLATE COPOLYMER (1:1) TYPE A (UNII: NX76LV5T8J) POLYETHYLENE GLYCOLS (UNII: 3WJQ0SDW1A) TALC (UNII: 7SEV7J4R1U) TITANIUM DIOXIDE (UNII: 15FIX9V2JP) Product Characteristics Color PINK (Pink, coated) Score no score Shape ROUND (circular shaped tablets) Size 11mm Flavor Imprint Code W;275 Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 55648-275-01 30 in 1 BOTTLE 2 NDC: 55648-275-02 500 in 1 BOTTLE 3 NDC: 55648-275-04 10 in 1 CARTON 3 10 in 1 BLISTER PACK Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA202498 11/29/2012 Labeler - Wockhardt Limited (650069115) Registrant - Wockhardt Limited (650069115) Establishment Name Address ID/FEI Business Operations Wockhardt Limited 676257570 ANALYSIS(55648-271, 55648-274, 55648-273, 55648-272, 55648-275) , MANUFACTURE(55648-271, 55648-274, 55648-273, 55648-272, 55648-275) , PACK(55648-271, 55648-274, 55648-273, 55648-272, 55648-275) , LABEL(55648-271, 55648-274, 55648-273, 55648-272, 55648-275)
© 2026 FDA.report
This site is not affiliated with or endorsed by the FDA.

