STEGLATRO- ertugliflozin tablet, film coated
STEGLATRO by
Drug Labeling and Warnings
STEGLATRO by is a Prescription medication manufactured, distributed, or labeled by Merck Sharp & Dohme Corp.. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
-
HIGHLIGHTS OF PRESCRIBING INFORMATION
These highlights do not include all the information needed to use STEGLATRO safely and effectively. See full prescribing information for STEGLATRO.
STEGLATRO™ (ertugliflozin) tablets, for oral use
Initial U.S. Approval: 2017RECENT MAJOR CHANGES
Warnings and Precautions Ketoacidosis (5.2) 01/2020 INDICATIONS AND USAGE
DOSAGE AND ADMINISTRATION
- Recommended starting dose is 5 mg once daily, taken in the morning, with or without food. (2.1)
- Increase dose to 15 mg once daily in those tolerating STEGLATRO and needing additional glycemic control. (2.1)
- Assess renal function before initiating STEGLATRO and periodically thereafter (2.2):
- Do not use in patients with an estimated glomerular filtration rate (eGFR) below 30 mL/minute/1.73 m2.
- Initiation is not recommended in patients with an eGFR of 30 to less than 60 mL/minute/1.73 m2.
- Continued use is not recommended in patients with an eGFR persistently between 30 and less than 60 mL/min/1.73 m2.
DOSAGE FORMS AND STRENGTHS
Tablets: 5 mg and 15 mg (3)
CONTRAINDICATIONS
WARNINGS AND PRECAUTIONS
- Hypotension: May occur particularly in patients with renal impairment, the elderly, or patients on diuretics. Before initiating, assess and correct volume status. Monitor for signs and symptoms during therapy. (5.1)
- Ketoacidosis: Assess patients who present with signs and symptoms of metabolic acidosis for ketoacidosis, regardless of blood glucose level. If suspected, discontinue, evaluate, and treat promptly. Before initiating, consider risk factors for ketoacidosis. Patients may require monitoring and temporary discontinuation of therapy in clinical situations known to predispose to ketoacidosis. (5.2)
- Acute Kidney Injury and Impairment in Renal Function: Consider temporarily discontinuing in settings of reduced oral intake or fluid losses. If acute kidney injury occurs, discontinue and promptly treat. Monitor renal function. (5.3)
- Urosepsis and Pyelonephritis: Evaluate patients for signs and symptoms of urinary tract infections and treat promptly, if indicated. (5.4)
- Lower Limb Amputation: Before initiating, consider factors that may increase risk of amputation. Monitor patients for infections or ulcers of lower limbs, and discontinue if these occur. (5.5)
- Hypoglycemia: Consider a lower dose of insulin or insulin secretagogue to reduce risk of hypoglycemia when used in combination. (5.6)
- Necrotizing Fasciitis of the Perineum (Fournier's gangrene): Serious, life-threatening cases have occurred in both females and males. Assess patients presenting with pain or tenderness, erythema, or swelling in the genital or perineal area, along with fever or malaise. If suspected, institute prompt treatment. (5.7)
- Genital Mycotic Infections: Monitor and treat if indicated. (5.8)
- Increased LDL-C: Monitor and treat as appropriate. (5.9)
ADVERSE REACTIONS
- The most common adverse reactions associated with STEGLATRO (incidence ≥ 5%) were female genital mycotic infections. (6.1)
To report SUSPECTED ADVERSE REACTIONS, contact Merck Sharp & Dohme Corp., a subsidiary of Merck & Co., Inc., at 1-877-888-4231 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
USE IN SPECIFIC POPULATIONS
- Pregnancy: Advise females of the potential risk to a fetus especially during the second and third trimesters. (8.1)
- Lactation: Breastfeeding not recommended. (8.2)
- Geriatrics: Higher incidence of adverse reactions related to reduced intravascular volume. (5.1, 8.5)
- Renal Impairment: Higher incidence of adverse reactions related to reduced intravascular volume and renal function. (5.1, 5.3, 8.6)
See 17 for PATIENT COUNSELING INFORMATION and Medication Guide.
Revised: 1/2020
-
Table of Contents
FULL PRESCRIBING INFORMATION: CONTENTS*
1 INDICATIONS AND USAGE
2 DOSAGE AND ADMINISTRATION
2.1 Recommended Dosage
2.2 Patients with Renal Impairment
3 DOSAGE FORMS AND STRENGTHS
4 CONTRAINDICATIONS
5 WARNINGS AND PRECAUTIONS
5.1 Hypotension
5.2 Ketoacidosis
5.3 Acute Kidney Injury and Impairment in Renal Function
5.4 Urosepsis and Pyelonephritis
5.5 Lower Limb Amputation
5.6 Hypoglycemia with Concomitant Use with Insulin and Insulin Secretagogues
5.7 Necrotizing Fasciitis of the Perineum (Fournier's Gangrene)
5.8 Genital Mycotic Infections
5.9 Increases in Low-Density Lipoprotein Cholesterol (LDL-C)
5.10 Macrovascular Outcomes
6 ADVERSE REACTIONS
6.1 Clinical Trials Experience
6.2 Postmarketing Experience
7 DRUG INTERACTIONS
7.1 Concomitant Use with Insulin and Insulin Secretagogues
7.2 Positive Urine Glucose Test
7.3 Interference with 1,5-anhydroglucitol (1,5-AG) Assay
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
8.2 Lactation
8.4 Pediatric Use
8.5 Geriatric Use
8.6 Renal Impairment
8.7 Hepatic Impairment
10 OVERDOSAGE
11 DESCRIPTION
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
12.2 Pharmacodynamics
12.3 Pharmacokinetics
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
14 CLINICAL STUDIES
14.1 Overview of Clinical Studies in Patients with Type 2 Diabetes Mellitus
14.2 Clinical Study of Monotherapy Use of STEGLATRO in Patients with Type 2 Diabetes Mellitus
14.3 Clinical Studies of Combination Therapy Use of STEGLATRO in Patients with Type 2 Diabetes Mellitus
14.4 Clinical Study of STEGLATRO in Patients with Moderate Renal Impairment and Type 2 Diabetes Mellitus
16 HOW SUPPLIED/STORAGE AND HANDLING
17 PATIENT COUNSELING INFORMATION
- * Sections or subsections omitted from the full prescribing information are not listed.
- 1 INDICATIONS AND USAGE
-
2 DOSAGE AND ADMINISTRATION
2.1 Recommended Dosage
- The recommended starting dose of STEGLATRO is 5 mg once daily, taken in the morning, with or without food. In patients tolerating STEGLATRO 5 mg once daily, the dose may be increased to a maximum recommended dose of 15 mg once daily if additional glycemic control is needed.
- In patients with volume depletion, correct this condition prior to initiation of STEGLATRO [see Warnings and Precautions (5.1)].
2.2 Patients with Renal Impairment
- Assess renal function prior to initiation of STEGLATRO and periodically thereafter [see Warnings and Precautions (5.3)].
- Use of STEGLATRO is contraindicated in patients with an eGFR less than 30 mL/minute/1.73 m2 [see Contraindications (4)].
- Initiation of STEGLATRO is not recommended in patients with an eGFR of 30 mL/minute/1.73 m2 to less than 60 mL/minute/1.73 m2 [see Warnings and Precautions (5.3) and Use in Specific Populations (8.6)].
- Continued use of STEGLATRO is not recommended when eGFR is persistently between 30 and less than 60 mL/minute/1.73 m2.
No dose adjustment is needed in patients with mild renal impairment.
- 3 DOSAGE FORMS AND STRENGTHS
-
4 CONTRAINDICATIONS
- Severe renal impairment, end-stage renal disease (ESRD), or dialysis [see Warnings and Precautions (5.3) and Use in Specific Populations (8.6)].
- History of a serious hypersensitivity reaction to STEGLATRO.
-
5 WARNINGS AND PRECAUTIONS
5.1 Hypotension
STEGLATRO causes intravascular volume contraction. Therefore, symptomatic hypotension may occur after initiating STEGLATRO [see Adverse Reactions (6.1)] particularly in patients with impaired renal function (eGFR less than 60 mL/min/1.73 m2) [see Use in Specific Populations (8.6)], elderly patients (≥65 years), in patients with low systolic blood pressure, and in patients on diuretics. Before initiating STEGLATRO, volume status should be assessed and corrected if indicated. Monitor for signs and symptoms of hypotension after initiating therapy.
5.2 Ketoacidosis
Reports of ketoacidosis, a serious life-threatening condition requiring urgent hospitalization, have been identified in clinical trials and postmarketing surveillance in patients with type 1 and type 2 diabetes mellitus receiving sodium glucose co-transporter-2 (SGLT2) inhibitors and cases have been reported in STEGLATRO-treated patients in clinical trials. Across the clinical program, ketoacidosis was identified in 3 of 3,409 (0.1%) of STEGLATRO-treated patients and 0% of comparator-treated patients. Fatal cases of ketoacidosis have been reported in patients taking SGLT2 inhibitors. STEGLATRO is not indicated for the treatment of patients with type 1 diabetes mellitus [see Indications and Usage (1)].
Patients treated with STEGLATRO who present with signs and symptoms consistent with severe metabolic acidosis should be assessed for ketoacidosis regardless of presenting blood glucose levels, as ketoacidosis associated with STEGLATRO may be present even if blood glucose levels are less than 250 mg/dL. If ketoacidosis is suspected, STEGLATRO should be discontinued, patient should be evaluated, and prompt treatment should be instituted. Treatment of ketoacidosis may require insulin, fluid and carbohydrate replacement.
In many of the reported cases, and particularly in patients with type 1 diabetes, the presence of ketoacidosis was not immediately recognized and institution of treatment was delayed because presenting blood glucose levels were below those typically expected for diabetic ketoacidosis (often less than 250 mg/dL). Signs and symptoms at presentation were consistent with dehydration and severe metabolic acidosis and included nausea, vomiting, abdominal pain, generalized malaise, and shortness of breath. In some but not all cases, factors predisposing to ketoacidosis such as insulin dose reduction, acute febrile illness, reduced caloric intake, surgery, pancreatic disorders suggesting insulin deficiency (e.g., type 1 diabetes, history of pancreatitis or pancreatic surgery), and alcohol abuse were identified.
Before initiating STEGLATRO, consider factors in the patient history that may predispose to ketoacidosis, including pancreatic insulin deficiency from any cause, caloric restriction, and alcohol abuse.
For patients who undergo scheduled surgery, consider temporarily discontinuing STEGLATRO for at least 4 days prior to surgery [see Clinical Pharmacology (12.2, 12.3)].
Consider monitoring for ketoacidosis and temporarily discontinuing STEGLATRO in other clinical situations known to predispose to ketoacidosis (e.g., prolonged fasting due to acute illness or post-surgery). Ensure risk factors for ketoacidosis are resolved prior to restarting STEGLATRO.
Educate patients on the signs and symptoms of ketoacidosis and instruct patients to discontinue STEGLATRO and seek medical attention immediately if signs and symptoms occur.
5.3 Acute Kidney Injury and Impairment in Renal Function
STEGLATRO causes intravascular volume contraction and can cause renal impairment [see Adverse Reactions (6.1)]. There have been postmarketing reports of acute kidney injury some requiring hospitalization and dialysis in patients receiving SGLT2 inhibitors.
Before initiating STEGLATRO, consider factors that may predispose patients to acute kidney injury including hypovolemia, chronic renal insufficiency, congestive heart failure and concomitant medications (diuretics, ACE inhibitors, ARBs, NSAIDs). Consider temporarily discontinuing STEGLATRO in any setting of reduced oral intake (such as acute illness or fasting) or fluid losses (such as gastrointestinal illness or excessive heat exposure); monitor patients for signs and symptoms of acute kidney injury. If acute kidney injury occurs, discontinue STEGLATRO promptly and institute treatment.
STEGLATRO increases serum creatinine and decreases eGFR. Patients with moderate renal impairment (eGFR 30 to less than 60 mL/min/1.73 m2) may be more susceptible to these changes. Renal function abnormalities can occur after initiating STEGLATRO [see Adverse Reactions (6.1)]. Renal function should be evaluated prior to initiating STEGLATRO and periodically thereafter. Use of STEGLATRO is not recommended when eGFR is persistently between 30 and less than 60 mL/min/1.73 m2 and is contraindicated in patients with an eGFR less than 30 mL/min/1.73 m2 [see Dosage and Administration (2.2), Contraindications (4), and Use in Specific Populations (8.6)].
5.4 Urosepsis and Pyelonephritis
There have been postmarketing reports of serious urinary tract infections, including urosepsis and pyelonephritis, requiring hospitalization in patients receiving SGLT2 inhibitors. Cases of pyelonephritis also have been reported in STEGLATRO-treated patients in clinical trials. Treatment with SGLT2 inhibitors increases the risk for urinary tract infections. Evaluate patients for signs and symptoms of urinary tract infections and treat promptly, if indicated [see Adverse Reactions (6.1)].
5.5 Lower Limb Amputation
An increased risk for lower limb amputation (primarily of the toe) has been observed in clinical studies with another SGLT2 inhibitor. Across seven Phase 3 clinical trials in the STEGLATRO development program, non-traumatic lower limb amputations were reported in 1 (0.1%) patient in the comparator group, 3 (0.2%) patients in the STEGLATRO 5 mg group, and 8 (0.5%) patients in the STEGLATRO 15 mg group. A causal association between STEGLATRO and lower limb amputation has not been definitively established.
Before initiating STEGLATRO, consider factors in the patient history that may predispose them to the need for amputations, such as a history of prior amputation, peripheral vascular disease, neuropathy and diabetic foot ulcers. Counsel patients about the importance of routine preventative foot care. Monitor patients receiving STEGLATRO for signs and symptoms of infection (including osteomyelitis), new pain or tenderness, sores or ulcers involving the lower limbs, and discontinue STEGLATRO if these complications occur.
5.6 Hypoglycemia with Concomitant Use with Insulin and Insulin Secretagogues
Insulin and insulin secretagogues (e.g., sulfonylurea) are known to cause hypoglycemia. STEGLATRO may increase the risk of hypoglycemia when used in combination with insulin and/or an insulin secretagogue [see Adverse Reactions (6.1)]. Therefore, a lower dose of insulin or insulin secretagogue may be required to minimize the risk of hypoglycemia when used in combination with STEGLATRO.
5.7 Necrotizing Fasciitis of the Perineum (Fournier's Gangrene)
Reports of necrotizing fasciitis of the perineum (Fournier's gangrene), a rare but serious and life-threatening necrotizing infection requiring urgent surgical intervention, have been identified in postmarketing surveillance in patients with diabetes mellitus receiving SGLT2 inhibitors. Cases have been reported in females and males. Serious outcomes have included hospitalization, multiple surgeries, and death.
Patients treated with STEGLATRO presenting with pain or tenderness, erythema, or swelling in the genital or perineal area, along with fever or malaise, should be assessed for necrotizing fasciitis. If suspected, start treatment immediately with broad-spectrum antibiotics and, if necessary, surgical debridement. Discontinue STEGLATRO, closely monitor blood glucose levels, and provide appropriate alternative therapy for glycemic control.
5.8 Genital Mycotic Infections
STEGLATRO increases the risk of genital mycotic infections. Patients who have a history of genital mycotic infections or who are uncircumcised are more likely to develop genital mycotic infections [see Adverse Reactions (6.1)]. Monitor and treat appropriately.
5.9 Increases in Low-Density Lipoprotein Cholesterol (LDL-C)
Dose-related increases in LDL-C can occur with STEGLATRO [see Adverse Reactions (6.1)]. Monitor and treat as appropriate.
-
6 ADVERSE REACTIONS
The following important adverse reactions are described elsewhere in the labeling:
- Hypotension [see Warnings and Precautions (5.1)]
- Ketoacidosis [see Warnings and Precautions (5.2)]
- Acute Kidney Injury and Impairment in Renal Function [see Warnings and Precautions (5.3)]
- Urosepsis and Pyelonephritis [see Warnings and Precautions (5.4)]
- Lower Limb Amputation [see Warnings and Precautions (5.5)]
- Hypoglycemia with Concomitant Use with Insulin and Insulin Secretagogues [see Warnings and Precautions (5.6)]
- Necrotizing Fasciitis of the Perineum (Fournier's gangrene) [see Warnings and Precautions (5.7)]
- Genital Mycotic Infections [see Warnings and Precautions (5.8)]
- Increases in Low-Density Lipoprotein Cholesterol (LDL-C) [see Warnings and Precautions (5.9)]
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Pool of Placebo-Controlled Trials Evaluating STEGLATRO 5 and 15 mg
The data in Table 1 are derived from a pool of three 26-week, placebo-controlled trials. STEGLATRO was used as monotherapy in one trial and as add-on therapy in two trials [see Clinical Studies (14)]. These data reflect exposure of 1,029 patients to STEGLATRO with a mean exposure duration of approximately 25 weeks. Patients received STEGLATRO 5 mg (N=519), STEGLATRO 15 mg (N=510), or placebo (N=515) once daily. The mean age of the population was 57 years and 2% were older than 75 years of age. Fifty-three percent (53%) of the population was male and 73% were Caucasian, 15% were Asian, and 7% were Black or African American. At baseline the population had diabetes for an average of 7.5 years, had a mean HbA1c of 8.1%, and 19.4% had established microvascular complications of diabetes. Baseline renal function (mean eGFR 88.9 mL/min/1.73 m2) was normal or mildly impaired in 97% of patients and moderately impaired in 3% of patients.
Table 1 shows common adverse reactions associated with the use of STEGLATRO. These adverse reactions were not present at baseline, occurred more commonly on STEGLATRO than on placebo, and occurred in at least 2% of patients treated with either STEGLATRO 5 mg or STEGLATRO 15 mg.
Table 1: Adverse Reactions Reported in ≥2% of Patients with Type 2 Diabetes Mellitus Treated with STEGLATRO* and Greater than Placebo in Pooled Placebo-Controlled Clinical Studies of STEGLATRO Monotherapy or Combination Therapy Number (%) of Patients Placebo
N = 515STEGLATRO 5 mg
N = 519STEGLATRO 15 mg
N = 510- * The three placebo controlled studies included one monotherapy trial and two add-on combination trials with metformin or with metformin and sitagliptin.
- † Includes: genital candidiasis, genital infection fungal, vaginal infection, vulvitis, vulvovaginal candidiasis, vulvovaginal mycotic infection, and vulvovaginitis. Percentages calculated with the number of female patients in each group as denominator: placebo (N=235), STEGLATRO 5 mg (N=252), STEGLATRO 15 mg (N=245).
- ‡ Includes: balanitis candida, balanoposthitis, genital infection, and genital infection fungal. Percentages calculated with the number of male patients in each group as denominator: placebo (N=280), STEGLATRO 5 mg (N=267), STEGLATRO 15 mg (N=265).
- § Includes: cystitis, dysuria, streptococcal urinary tract infection, urethritis, urinary tract infection.
- ¶ Includes: vulvovaginal pruritus and pruritus genital. Percentages calculated with the number of female patients in each group as denominator: placebo (N=235), ertugliflozin 5 mg (N=252), ertugliflozin 15 mg (N=245).
- # Includes: pollakiuria, micturition urgency, polyuria, urine output increased, and nocturia.
- Þ Includes: thirst, dry mouth, polydipsia, and dry throat.
Female genital mycotic infections† 3.0% 9.1% 12.2% Male genital mycotic infections‡ 0.4% 3.7% 4.2% Urinary tract infections§ 3.9% 4.0% 4.1% Headache 2.3% 3.5% 2.9% Vaginal pruritus¶ 0.4% 2.8% 2.4% Increased urination# 1.0% 2.7% 2.4% Nasopharyngitis 2.3% 2.5% 2.0% Back pain 2.3% 1.7% 2.5% Weight decreased 1.0% 1.2% 2.4% ThirstÞ 0.6% 2.7% 1.4% Volume Depletion
STEGLATRO causes an osmotic diuresis, which may lead to intravascular volume contraction and adverse reactions related to volume depletion, particularly in patients with impaired renal function (eGFR less than 60 mL/min/1.73 m2). In patients with moderate renal impairment, adverse reactions related to volume depletion (e.g., dehydration, dizziness postural, presyncope, syncope, hypotension, and orthostatic hypotension) were reported in 0%, 4.4%, and 1.9% of patients treated with placebo, STEGLATRO 5 mg, and STEGLATRO 15 mg, respectively. STEGLATRO may also increase the risk of hypotension in other patients at risk for volume contraction [see Use in Specific Populations (8.5, 8.6)].
Ketoacidosis
Across the clinical program, ketoacidosis was identified in 3 of 3,409 (0.1%) ertugliflozin-treated patients and 0.0% of comparator-treated patients [see Warnings and Precautions (5.2)].
Impairment in Renal Function
Treatment with STEGLATRO was associated with increases in serum creatinine and decreases in eGFR (see Table 2). Patients with moderate renal impairment at baseline had larger mean changes. In a study in patients with moderate renal impairment, these abnormal laboratory findings were observed to reverse after treatment discontinuation [see Use in Specific Populations (8.5, 8.6)].
Table 2: Changes from Baseline in Serum Creatinine and eGFR in the Pool of Three 26-Week Placebo-Controlled Studies, and a 26-Week Moderate Renal Impairment Study in Patients with Type 2 Diabetes Mellitus Pool of 26-Week Placebo-Controlled Studies Placebo
N=515STEGLATRO 5 mg
N=519STEGLATRO 15 mg
N=510Baseline Mean Creatinine (mg/dL) 0.83 0.82 0.82 eGFR (mL/min/1.73 m2) 89.5 88.2 89.0 Week 6 Change Creatinine (mg/dL) 0.00 0.03 0.03 eGFR (mL/min/1.73 m2) -0.3 -2.7 -3.1 Week 26 Change Creatinine (mg/dL) -0.01 0.00 0.01 eGFR (mL/min/1.73 m2) 0.7 0.5 -0.6 Moderate Renal Impairment Study Placebo
N=154STEGLATRO 5 mg
N=158STEGLATRO 15 mg
N=155Baseline Creatinine (mg/dL) 1.39 1.38 1.37 eGFR (mL/min/1.73 m2) 46.0 46.8 46.9 Week 6 Change Creatinine (mg/dL) -0.02 0.11 0.12 eGFR (mL/min/1.73 m2) 0.6 -3.2 -4.1 Week 26 Change Creatinine (mg/dL) 0.02 0.08 0.10 eGFR (mL/min/1.73 m2) 0.0 -2.7 -2.6 Renal-related adverse reactions (e.g., acute kidney injury, renal impairment, acute prerenal failure) may occur in patients treated with STEGLATRO, particularly in patients with moderate renal impairment where the incidence of renal-related adverse reactions was 0.6%, 2.5%, and 1.3% in patients treated with placebo, STEGLATRO 5 mg, and STEGLATRO 15 mg, respectively.
Lower Limb Amputation
Across seven Phase 3 clinical trials in which STEGLATRO was studied as monotherapy and in combination with other antihyperglycemic agents, non-traumatic lower limb amputations occurred in 1 of 1,450 (0.1%) in the non-STEGLATRO group, 3 of 1,716 (0.2%) in the STEGLATRO 5 mg group, and 8 of 1,693 (0.5%) in the STEGLATRO 15 mg group.
Hypoglycemia
The incidence of hypoglycemia by study is shown in Table 3.
Table 3: Incidence of Overall* and Severe† Hypoglycemia in Placebo-Controlled Clinical Studies in Patients with Type 2 Diabetes Mellitus - * Overall hypoglycemic events: plasma or capillary glucose of less than or equal to 70 mg/dL.
- † Severe hypoglycemic events: required assistance, lost consciousness, or experienced a seizure regardless of blood glucose.
Monotherapy (26 weeks) Placebo
(N = 153)STEGLATRO
5 mg
(N =156)STEGLATRO
15 mg
(N = 152)Overall [N (%)] 1 (0.7) 4 (2.6) 4 (2.6) Severe [N (%)] 0 (0.0) 0 (0.0) 2 (1.3) Add-on Combination Therapy with Metformin (26 weeks) Placebo
(N = 209)STEGLATRO
5 mg
(N = 207)STEGLATRO
15 mg
(N = 205)Overall [N (%)] 9 (4.3) 15 (7.2) 16 (7.8) Severe [N (%)] 1 (0.5) 1 (0.5) 0 (0.0) Add-on Combination Therapy with Metformin and Sitagliptin (26 weeks) Placebo
(N = 153)STEGLATRO
5 mg
(N = 156)STEGLATRO
15 mg
(N = 153)Overall [N (%)] 5 (3.3) 7 (4.5) 3 (2.0) Severe [N (%)] 1 (0.7) 1 (0.6) 0 (0.0) In Combination with Insulin and/or an Insulin Secretagogue in Patients with Moderate Renal Impairment Placebo
(N = 133)STEGLATRO
5 mg
(N = 148)STEGLATRO
15 mg
(N = 143)Overall [N (%)] 48 (36.1) 53 (35.8) 39 (27.3) Severe [N (%)] 3 (2.3) 5 (3.4) 3 (2.1) Genital Mycotic Infections
In the pool of three placebo-controlled clinical trials, the incidence of female genital mycotic infections (e.g., genital candidiasis, genital infection fungal, vaginal infection, vulvitis, vulvovaginal candidiasis, vulvovaginal mycotic infection, vulvovaginitis) occurred in 3%, 9.1%, and 12.2% of females treated with placebo, STEGLATRO 5 mg, and STEGLATRO 15 mg, respectively (see Table 1). In females, discontinuation due to genital mycotic infections occurred in 0% and 0.6% of patients treated with placebo and STEGLATRO, respectively.
In the same pool, male genital mycotic infections (e.g., balanitis candida, balanoposthitis, genital infection, genital infection fungal) occurred in 0.4%, 3.7%, and 4.2% of males treated with placebo, STEGLATRO 5 mg, and STEGLATRO 15 mg, respectively (see Table 1). Male genital mycotic infections occurred more commonly in uncircumcised males. In males, discontinuations due to genital mycotic infections occurred in 0% and 0.2% of patients treated with placebo and STEGLATRO, respectively. Phimosis was reported in 8 of 1729 (0.5%) male ertugliflozin-treated patients, of which four required circumcision.
Laboratory Tests
Increases in Low-Density Lipoprotein Cholesterol (LDL-C)
In the pool of three placebo-controlled trials, dose-related increases in LDL-C were observed in patients treated with STEGLATRO. Mean percent changes from baseline to Week 26 in LDL-C relative to placebo were 2.6% and 5.4% with STEGLATRO 5 mg and STEGLATRO 15 mg, respectively. The range of mean baseline LDL-C was 96.6 to 97.7 mg/dL across treatment groups [see Warnings and Precautions (5.9)].
Increases in Hemoglobin
In the pool of three placebo-controlled trials, mean changes (percent changes) from baseline to Week 26 in hemoglobin were -0.21 g/dL (-1.4%) with placebo, 0.46 g/dL (3.5%) with STEGLATRO 5 mg, and 0.48 g/dL (3.5%) with STEGLATRO 15 mg. The range of mean baseline hemoglobin was 13.90 to 14.00 g/dL across treatment groups. At the end of treatment, 0.0%, 0.2%, and 0.4% of patients treated with placebo, STEGLATRO 5 mg, and STEGLATRO 15 mg, respectively, had a hemoglobin increase greater than 2 g/dL and above the upper limit of normal.
Increases in Serum Phosphate
In the pool of three placebo-controlled trials, mean changes (percent changes) from baseline in serum phosphate were 0.04 mg/dL (1.9%) with placebo, 0.21 mg/dL (6.8%) with STEGLATRO 5 mg, and 0.26 mg/dL (8.5%) with STEGLATRO 15 mg. The range of mean baseline serum phosphate was 3.53 to 3.54 mg/dL across treatment groups. In a clinical trial of patients with moderate renal impairment, mean changes (percent changes) from baseline at Week 26 in serum phosphate were -0.01 mg/dL (0.8%) with placebo, 0.29 mg/dL (9.7%) with STEGLATRO 5 mg, and 0.24 mg/dL (7.8%) with STEGLATRO 15 mg.
6.2 Postmarketing Experience
Additional adverse reactions have been identified during postapproval use. Because these reactions are reported voluntarily from a population of uncertain size, it is generally not possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- Cases of necrotizing fasciitis of the perineum (Fournier's gangrene) have been seen with SGLT2 inhibitors [see Warnings and Precautions (5.7)]
-
7 DRUG INTERACTIONS
7.1 Concomitant Use with Insulin and Insulin Secretagogues
STEGLATRO may increase the risk of hypoglycemia when used in combination with insulin and/or an insulin secretagogue [see Adverse Reactions (6.1)]. Therefore, a lower dose of insulin or insulin secretagogue may be required to minimize the risk of hypoglycemia when used in combination with STEGLATRO [see Warnings and Precautions (5.6)].
-
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Risk Summary
Based on animal data showing adverse renal effects, STEGLATRO is not recommended during the second and third trimesters of pregnancy.
The limited available data with STEGLATRO in pregnant women are not sufficient to determine a drug-associated risk of adverse developmental outcomes. There are risks to the mother and fetus associated with poorly controlled diabetes in pregnancy (see Clinical Considerations).
In animal studies, adverse renal changes were observed in rats when ertugliflozin was administered during a period of renal development corresponding to the late second and third trimesters of human pregnancy. Doses approximately 13 times the maximum clinical dose caused renal pelvic and tubule dilatations and renal mineralization that were not fully reversible. There was no evidence of fetal harm in rats or rabbits at exposures of ertugliflozin approximately 300 times higher than the maximal clinical dose of 15 mg/day when administered during organogenesis (see Data).
The estimated background risk of major birth defects is 6-10% in women with pre-gestational diabetes with a HbA1c >7 and has been reported to be as high as 20-25% in women with HbA1c >10. The estimated background risk of miscarriage for the indicated population is unknown. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2-4% and 15-20%, respectively.
Clinical Considerations
Disease-Associated Maternal and/or Embryo/Fetal Risk
Poorly-controlled diabetes in pregnancy increases the maternal risk for diabetic ketoacidosis, pre-eclampsia, spontaneous abortions, preterm delivery, stillbirth, and delivery complications. Poorly controlled diabetes increases the fetal risk for major birth defects, stillbirth, and macrosomia related morbidity.
Data
Animal Data
When ertugliflozin was orally administered to juvenile rats from PND 21 to PND 90, increased kidney weight, renal tubule and renal pelvis dilatation, and renal mineralization occurred at doses greater than or equal to 5 mg/kg (13-fold human exposures, based on AUC). These effects occurred with drug exposure during periods of renal development in rats that correspond to the late second and third trimester of human renal development, and did not fully reverse within a 1-month recovery period.
In embryo-fetal development studies, ertugliflozin (50, 100 and 250 mg/kg/day) was administered orally to rats on gestation days 6 to 17 and to rabbits on gestation days 7 to 19. Ertugliflozin did not adversely affect developmental outcomes in rats and rabbits at maternal exposures that were approximately 300 times the human exposure at the maximum clinical dose of 15 mg/day, based on AUC. A maternally toxic dose (250 mg/kg/day) in rats (707 times the clinical dose), was associated with reduced fetal viability, and a higher incidence of a visceral malformation (membranous ventricular septal defect). In the pre- and post-natal development study in pregnant rats, ertugliflozin was administered to the dams from gestation day 6 through lactation day 21 (weaning). Decreased post-natal growth (weight gain) was observed at maternal doses ≥100 mg/kg/day (greater than or equal to 331 times the human exposure at the maximum clinical dose of 15 mg/day, based on AUC).
8.2 Lactation
Risk Summary
There is no information regarding the presence of STEGLATRO in human milk, the effects on the breastfed infant, or the effects on milk production. Ertugliflozin is present in the milk of lactating rats (see Data). Since human kidney maturation occurs in utero and during the first 2 years of life when lactational exposure may occur, there may be risk to the developing human kidney. Because of the potential for serious adverse reactions in a breastfed infant, advise women that the use of STEGLATRO is not recommended while breastfeeding.
Data
Animal Data
The lacteal excretion of radiolabeled ertugliflozin in lactating rats was evaluated 10 to 12 days after parturition. Ertugliflozin derived radioactivity exposure in milk and plasma were similar, with a milk/plasma ratio of 1.07, based on AUC. Juvenile rats directly exposed to STEGLATRO during a developmental period corresponding to human kidney maturation were associated with a risk to the developing kidney (persistent increased organ weight, renal mineralization, and renal pelvic and tubular dilatations).
8.4 Pediatric Use
Safety and effectiveness of STEGLATRO in pediatric patients under 18 years of age have not been established.
8.5 Geriatric Use
No dosage adjustment of STEGLATRO is recommended based on age. Across the clinical program, a total of 876 (25.7%) patients treated with STEGLATRO were 65 years and older, and 152 (4.5%) patients treated with STEGLATRO were 75 years and older. Patients 65 years and older had a higher incidence of adverse reactions related to volume depletion compared to younger patients; events were reported in 1.1%, 2.2%, and 2.6% of patients treated with comparator, STEGLATRO 5 mg, and STEGLATRO 15 mg, respectively [see Warnings and Precautions (5.1) and Adverse Reactions (6.1)]. STEGLATRO is expected to have diminished efficacy in elderly patients with renal impairment [see Use in Specific Populations (8.6)].
8.6 Renal Impairment
The safety and efficacy of STEGLATRO have not been established in patients with type 2 diabetes mellitus and moderate renal impairment [see Clinical Studies (14.4)]. Compared to placebo-treated patients, patients with moderate renal impairment treated with STEGLATRO did not have improvement in glycemic control [see Clinical Studies (14.4)], and had increased risks for renal impairment, renal-related adverse reactions and volume depletion adverse reactions [see Dosage and Administration (2.2), Warnings and Precautions (5.3) and Adverse Reactions (6.1)]. Therefore, STEGLATRO is not recommended in this population.
STEGLATRO is contraindicated in patients with severe renal impairment, ESRD, or receiving dialysis. STEGLATRO is not expected to be effective in these patient populations [see Contraindications (4)].
No dosage adjustment or increased monitoring is needed in patients with mild renal impairment.
8.7 Hepatic Impairment
No dosage adjustment of STEGLATRO is necessary in patients with mild or moderate hepatic impairment. Ertugliflozin has not been studied in patients with severe hepatic impairment and is not recommended for use in this patient population [see Clinical Pharmacology (12.3)].
- 10 OVERDOSAGE
-
11 DESCRIPTION
STEGLATRO (ertugliflozin) tablets for oral use contain ertugliflozin L-pyroglutamic acid, a SGLT2 inhibitor.
The chemical name of ertugliflozin L-pyroglutamic acid is (1S,2S,3S,4R,5S)-5-(4-chloro-3-(4-ethoxybenzyl)phenyl)-1-(hydroxymethyl)-6,8-dioxabicyclo[3.2.1]octane-2,3,4-triol, compound with (2S)-5-oxopyrrolidine-2-carboxylic acid. The molecular formula is C27H32ClNO10 and the molecular weight is 566.00.
The chemical structure is:
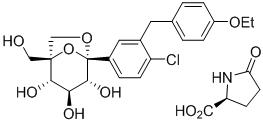
Ertugliflozin L-pyroglutamic acid is a white to off-white powder that is soluble in ethyl alcohol and acetone, slightly soluble in ethyl acetate and acetonitrile and very slightly soluble in water.
STEGLATRO is supplied as film-coated tablets, containing 6.48 or 19.43 mg of ertugliflozin L-pyroglutamic acid, which is equivalent to 5 and 15 mg of ertugliflozin.
Inactive ingredients are microcrystalline cellulose, lactose monohydrate, sodium starch glycolate, and magnesium stearate.
The film coating contains: hypromellose, lactose monohydrate, macrogol, triacetin, titanium dioxide and iron oxide red.
-
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
SGLT2 is the predominant transporter responsible for reabsorption of glucose from the glomerular filtrate back into the circulation. Ertugliflozin is an inhibitor of SGLT2. By inhibiting SGLT2, ertugliflozin reduces renal reabsorption of filtered glucose and lowers the renal threshold for glucose, and thereby increases urinary glucose excretion.
12.2 Pharmacodynamics
Urinary Glucose Excretion and Urinary Volume
Dose-dependent increases in the amount of glucose excreted in urine were observed in healthy subjects and in patients with type 2 diabetes mellitus following single- and multiple-dose administration of ertugliflozin. Dose-response modeling indicates that ertugliflozin 5 mg and 15 mg result in near maximal urinary glucose excretion (UGE). Enhanced UGE is maintained after multiple-dose administration. UGE with ertugliflozin also results in increases in urinary volume.
Cardiac Electrophysiology
The effect of STEGLATRO on QTc interval was evaluated in a Phase 1 randomized, placebo- and positive-controlled 3-period crossover study in 42 healthy subjects. At 6.7 times the therapeutic exposures with maximum recommended dose, STEGLATRO does not prolong QTc to any clinically relevant extent.
12.3 Pharmacokinetics
The pharmacokinetics of ertugliflozin are similar in healthy subjects and patients with type 2 diabetes mellitus. The steady state mean plasma AUC and Cmax were 398 ng∙hr/mL and 81.3 ng/mL, respectively, with 5 mg ertugliflozin once-daily treatment, and 1,193 ng∙hr/mL and 268 ng/mL, respectively, with 15 mg ertugliflozin once-daily treatment. Steady-state is reached after 4 to 6 days of once-daily dosing with ertugliflozin. Ertugliflozin does not exhibit time-dependent pharmacokinetics and accumulates in plasma up to 10-40% following multiple dosing.
Absorption
Following single-dose oral administration of 5 mg and 15 mg of ertugliflozin, peak plasma concentrations (median Tmax) of ertugliflozin occur at 1 hour postdose under fasted conditions. Plasma Cmax and AUC of ertugliflozin increase in a dose-proportional manner following single doses from 0.5 mg (0.1 times the lowest recommended dose) to 300 mg (20 times the highest recommended dose) and following multiple doses from 1 mg (0.2 times the lowest recommended dose) to 100 mg (6.7 times the highest recommended dose). The absolute oral bioavailability of ertugliflozin following administration of a 15 mg dose is approximately 100%.
Effect of Food
Administration of STEGLATRO with a high-fat and high-calorie meal decreases ertugliflozin Cmax by 29% and prolongs Tmax by 1 hour, but does not alter AUC as compared with the fasted state. The observed effect of food on ertugliflozin pharmacokinetics is not considered clinically relevant, and ertugliflozin may be administered with or without food. In Phase 3 clinical trials, STEGLATRO was administered without regard to meals.
Distribution
The mean steady-state volume of distribution of ertugliflozin following an intravenous dose is 85.5 L. Plasma protein binding of ertugliflozin is 93.6% and is independent of ertugliflozin plasma concentrations. Plasma protein binding is not meaningfully altered in patients with renal or hepatic impairment. The blood-to-plasma concentration ratio of ertugliflozin is 0.66.
Elimination
Metabolism
Metabolism is the primary clearance mechanism for ertugliflozin. The major metabolic pathway for ertugliflozin is UGT1A9 and UGT2B7-mediated O-glucuronidation to two glucuronides that are pharmacologically inactive at clinically relevant concentrations. CYP-mediated (oxidative) metabolism of ertugliflozin is minimal (12%).
Excretion
The mean systemic plasma clearance following an intravenous 100 µg dose was 11.2 L/hr. The mean elimination half-life in type 2 diabetic patients with normal renal function was estimated to be 16.6 hours based on the population pharmacokinetic analysis. Following administration of an oral [14C]-ertugliflozin solution to healthy subjects, approximately 40.9% and 50.2% of the drug-related radioactivity was eliminated in feces and urine, respectively. Only 1.5% of the administered dose was excreted as unchanged ertugliflozin in urine and 33.8% as unchanged ertugliflozin in feces, which is likely due to biliary excretion of glucuronide metabolites and subsequent hydrolysis to parent.
Specific Populations
Patients with Renal Impairment
In a Phase 1 clinical pharmacology study in patients with type 2 diabetes mellitus and mild, moderate, or severe renal impairment (as determined by eGFR), following a single-dose administration of 15 mg STEGLATRO, the mean increases in AUC of ertugliflozin were 1.6-, 1.7-, and 1.6-fold, respectively, for mild, moderate and severe renally impaired patients, compared to subjects with normal renal function. These increases in ertugliflozin AUC are not considered clinically meaningful. The 24-hour urinary glucose excretion declined with increasing severity of renal impairment [see Warnings and Precautions (5.3) and Use in Specific Populations (8.6)]. The plasma protein binding of ertugliflozin was unaffected in patients with renal impairment.
Patients with Hepatic Impairment
Moderate hepatic impairment (based on the Child-Pugh classification) did not result in an increase in exposure of ertugliflozin. The AUC of ertugliflozin decreased by approximately 13%, and Cmax decreased by approximately 21% compared to subjects with normal hepatic function. This decrease in ertugliflozin exposure is not considered clinically meaningful. There is no clinical experience in patients with Child-Pugh class C (severe) hepatic impairment. The plasma protein binding of ertugliflozin was unaffected in patients with moderate hepatic impairment [see Use in Specific Populations (8.7)].
Drug Interaction Studies
In Vitro Assessment of Drug Interactions
In in vitro studies, ertugliflozin and ertugliflozin glucuronides did not inhibit CYP450 isoenzymes (CYPs) 1A2, 2C9, 2C19, 2C8, 2B6, 2D6, or 3A4, and did not induce CYPs 1A2, 2B6, or 3A4. Ertugliflozin was not a time-dependent inhibitor of CYP3A in vitro. Ertugliflozin did not inhibit UGT1A6, 1A9, or 2B7 in vitro and was a weak inhibitor (IC50 >39 µM) of UGT1A1 and 1A4. Ertugliflozin glucuronides did not inhibit UGT1A1, 1A4, 1A6, 1A9, or 2B7 in vitro. Overall, ertugliflozin is unlikely to affect the pharmacokinetics of drugs eliminated by these enzymes. Ertugliflozin is a substrate of P-glycoprotein (P-gp) and breast cancer resistance protein (BCRP) transporters and is not a substrate of organic anion transporters (OAT1, OAT3), organic cation transporters (OCT1, OCT2), or organic anion transporting polypeptides (OATP1B1, OATP1B3). Ertugliflozin or ertugliflozin glucuronides do not meaningfully inhibit P-gp, OCT2, OAT1, or OAT3 transporters, or transporting polypeptides OATP1B1 and OATP1B3, at clinically relevant concentrations. Overall, ertugliflozin is unlikely to affect the pharmacokinetics of concurrently administered medications that are substrates of these transporters.
In Vivo Assessment of Drug Interactions
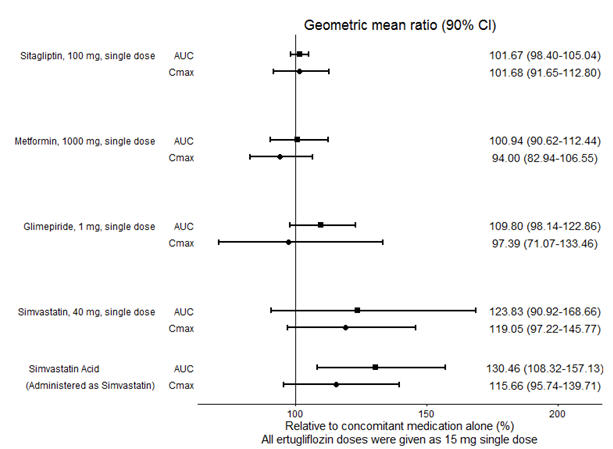
No dose adjustment of STEGLATRO is recommended when coadministered with commonly prescribed medicinal products. Ertugliflozin pharmacokinetics were similar with and without coadministration of metformin, glimepiride, sitagliptin, and simvastatin in healthy subjects (see Figure 1). Coadministration of ertugliflozin with multiple doses of 600 mg once-daily rifampin (an inducer of UGT and CYP enzymes) resulted in approximately 39% and 15% mean reductions in ertugliflozin AUC and Cmax, respectively, relative to ertugliflozin administered alone. These changes in exposure are not considered clinically relevant. Ertugliflozin had no clinically relevant effect on the pharmacokinetics of metformin, glimepiride, sitagliptin, and simvastatin when coadministered in healthy subjects (see Figure 2). Physiologically-based PK (PBPK) modeling suggests that coadministration of mefenamic acid (UGT inhibitor) may increase the AUC and Cmax of ertugliflozin by 1.51- and 1.19-fold, respectively. These predicted changes in exposure are not considered clinically relevant.
Figure 1: Effects of Other Drugs on the Pharmacokinetics of Ertugliflozin
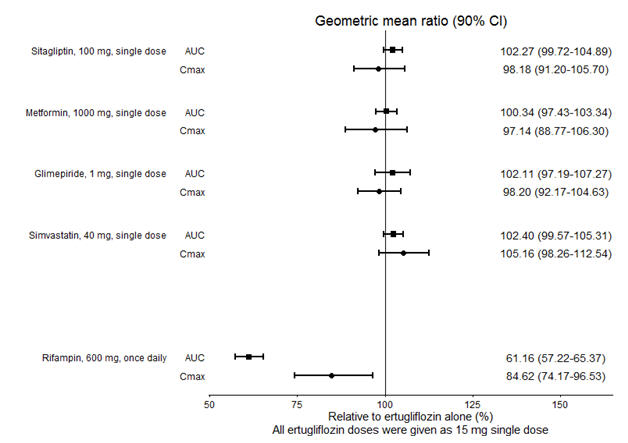
Figure 2: Effects of Ertugliflozin on the Pharmacokinetics of Other Drugs
-
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis
Carcinogenicity was evaluated in CD-1 mice and Sprague-Dawley rats. In the mouse study, ertugliflozin was administered by oral gavage at doses of 5, 15, and 40 mg/kg/day for up to 97 weeks in males and 102 weeks in females. There were no ertugliflozin-related neoplastic findings at doses up to 40 mg/kg/day (approximately 50 times human exposure at the maximum recommended human dose [MRHD] of 15 mg/day based on AUC). In the rat study, ertugliflozin was administered by oral gavage at doses of 1.5, 5, and 15 mg/kg/day for up to 92 weeks in females and 104 weeks in males. Ertugliflozin-related neoplastic findings included an increased incidence of adrenal medullary pheochromocytoma (PCC) in male rats at 15 mg/kg/day. Although the molecular mechanism remains unknown, this finding may be related to carbohydrate malabsorption leading to altered calcium homeostasis, which has been associated with PCC development in rats and has unclear relevancy to human risk. The no-observed-effect level (NOEL) for neoplasia was 5 mg/kg/day (approximately 16 times human exposure at the MRHD of 15 mg/day, based on AUC).
Mutagenesis
Ertugliflozin was not mutagenic or clastogenic with or without metabolic activation in the microbial reverse mutation, in vitro cytogenetic (human lymphocytes), and in vivo rat micronucleus assays.
Impairment of Fertility
In the rat fertility and embryonic development study, male and female rats were administered ertugliflozin at 5, 25, and 250 mg/kg/day. No effects on fertility were observed at 250 mg/kg/day (approximately 480 and 570 times male and female human exposures, respectively, at the MRHD of 15 mg/day based on AUC comparison).
-
14 CLINICAL STUDIES
14.1 Overview of Clinical Studies in Patients with Type 2 Diabetes Mellitus
The efficacy and safety of STEGLATRO have been studied in 7 multicenter, randomized, double-blind, placebo- or active comparator-controlled, clinical studies involving 4,863 patients with type 2 diabetes mellitus. These studies included White, Hispanic, Black, Asian, and other racial and ethnic groups, and patients with an average age of approximately 57.8 years.
STEGLATRO has been studied as monotherapy and in combination with metformin and/or a dipeptidyl peptidase 4 (DPP-4) inhibitor. STEGLATRO has also been studied in combination with antidiabetic medications, including insulin and a sulfonylurea, in patients with type 2 diabetes mellitus with moderate renal impairment.
In patients with type 2 diabetes mellitus treatment with STEGLATRO reduced hemoglobin A1c (HbA1c) compared to placebo.
In patients with type 2 diabetes mellitus treated with STEGLATRO, the reduction in HbA1c was generally similar across subgroups defined by age, sex, race, geographic region, baseline body mass index (BMI), and duration of type 2 diabetes mellitus. In patients with type 2 diabetes mellitus and moderate renal impairment, treatment with STEGLATRO did not result in a reduction in HbA1c compared to placebo.
14.2 Clinical Study of Monotherapy Use of STEGLATRO in Patients with Type 2 Diabetes Mellitus
A total of 461 patients with type 2 diabetes mellitus inadequately controlled (HbA1c between 7% and 10.5%) on diet and exercise participated in a randomized, double-blind, multi-center, 26-week, placebo-controlled study (NCT01958671) to evaluate the efficacy and safety of STEGLATRO monotherapy. These patients, who were either treatment naïve or not receiving any background antihyperglycemic treatment ≥8 weeks, entered a 2-week, single-blind, placebo run-in period and were randomized to placebo, STEGLATRO 5 mg, or STEGLATRO 15 mg, administered once daily.
At Week 26, treatment with STEGLATRO at 5 mg or 15 mg daily provided statistically significant reductions in HbA1c compared to placebo. STEGLATRO also resulted in a greater proportion of patients achieving an HbA1c <7% compared with placebo (see Table 4 and Figure 3).
Table 4: Results at Week 26 from a Placebo-Controlled Monotherapy Study of STEGLATRO in Patients with Type 2 Diabetes Mellitus* Placebo STEGLATRO 5 mg STEGLATRO 15 mg - * N includes all randomized and treated patients with a baseline measurement of the outcome variable. At Week 26, the primary HbA1c endpoint was missing for 23%, 11%, and 16% of patients, and during the trial, rescue medication was initiated by 25%, 2%, and 3% of patients randomized to placebo, STEGLATRO 5 mg, and STEGLATRO 15 mg, respectively. Missing Week 26 measurements were imputed using multiple imputation with a mean equal to the baseline value of the patient. Results include measurements collected after initiation of rescue medication. For those patients who did not receive rescue medication and had values measured at 26 weeks, the mean changes from baseline for HbA1c were -0.1%, -0.8%, and -1.0% for placebo, STEGLATRO 5 mg, and STEGLATRO 15 mg, respectively.
- † Intent-to-treat analysis using ANCOVA adjusted for baseline value, prior antihyperglycemic medication, and baseline eGFR.
- ‡ p<0.001 compared to placebo.
HbA1c (%) N = 153 N = 155 N = 151 Baseline (mean) 8.1 8.2 8.4 Change from baseline (LS mean†) -0.2 -0.7 -0.8 Difference from placebo (LS mean†, 95% CI) -0.6‡ (-0.8, -0.4) -0.7‡ (-0.9, -0.4) Patients [N (%)] with HbA1c <7% 26 (16.9) 47 (30.1) 59 (38.8) FPG (mg/dL) N = 150 N = 151 N = 149 Baseline (mean) 180.2 180.9 179.1 Change from baseline (LS mean†) -11.6 -31.0 -36.4 Difference from placebo (LS mean†, 95% CI) -19.4‡ (-27.6, -11.2) -24.8‡ (-33.2, -16.4) The mean baseline body weight was 94.2 kg, 94.0 kg, and 90.6 kg in the placebo, STEGLATRO 5 mg, and STEGLATRO 15 mg groups, respectively. The mean changes from baseline to Week 26 were -1.0 kg, -3.0 kg, and -3.1 kg in the placebo, STEGLATRO 5 mg, and STEGLATRO 15 mg groups, respectively. The difference from placebo (95% CI) for STEGLATRO 5 mg was -2.0 kg (-2.8, -1.2) and for STEGLATRO 15 mg was -2.1 kg (-2.9, -1.3).
- * Data to the left of the vertical line are observed means (non-model-based) excluding values occurring post glycemic rescue. Data to the right of the vertical line represent the final Week 26 data, including all values regardless of use of glycemic rescue medication and use of study drug, with missing Week 26 values imputed using multiple imputation (26-MI) with a mean equal to the baseline value of the patient (see Table 4).
Figure 3: HbA1c (%) Change Over Time in a 26-Week Placebo-Controlled Monotherapy Study of STEGLATRO in Patients with Type 2 Diabetes Mellitus* 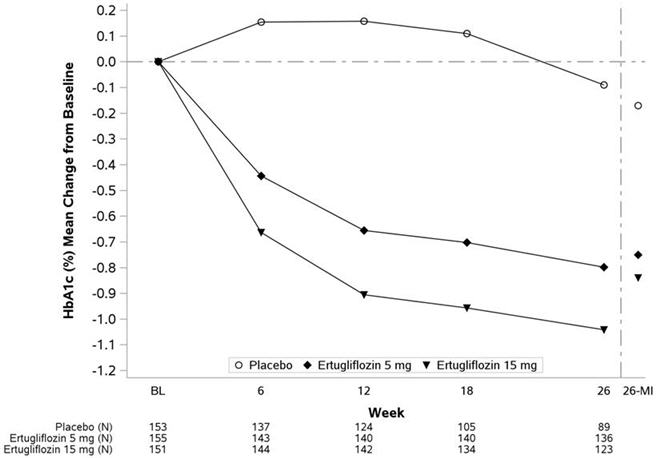
14.3 Clinical Studies of Combination Therapy Use of STEGLATRO in Patients with Type 2 Diabetes Mellitus
Add-on Combination Therapy with Metformin
A total of 621 patients with type 2 diabetes mellitus inadequately controlled (HbA1c between 7% and 10.5%) on metformin monotherapy (≥1,500 mg/day for ≥8 weeks) participated in a randomized, double-blind, multi-center, 26-week, placebo-controlled study (NCT02033889) to evaluate the efficacy and safety of STEGLATRO in combination with metformin. Patients entered a 2-week, single-blind, placebo run-in, and were randomized to placebo, STEGLATRO 5 mg, or STEGLATRO 15 mg administered once daily in addition to continuation of background metformin therapy.
At Week 26, treatment with STEGLATRO at 5 mg or 15 mg daily provided statistically significant reductions in HbA1c compared to placebo. STEGLATRO also resulted in a greater proportion of patients achieving an HbA1c <7% compared to placebo (see Table 5).
Table 5: Results at Week 26 from a Placebo-Controlled Study for STEGLATRO Used in Combination with Metformin in Patients with Type 2 Diabetes Mellitus* Placebo STEGLATRO 5 mg STEGLATRO 15 mg - * N includes all randomized and treated patients with a baseline measurement of the outcome variable. At Week 26, the primary HbA1c endpoint was missing for 12%, 6%, and 9% of patients, and during the trial, rescue medication was initiated by 18%, 3%, and 1% of patients randomized to placebo, STEGLATRO 5 mg, and STEGLATRO 15 mg, respectively. Missing Week 26 measurements were imputed using multiple imputation with a mean equal to the baseline value of the patient. Results include measurements collected after initiation of rescue medication. For those patients who did not receive rescue medication and had values measured at 26 weeks, the mean changes from baseline for HbA1c were -0.2%, -0.7%, and -1.0% for placebo, STEGLATRO 5 mg, and STEGLATRO 15 mg, respectively.
- † Intent-to-treat analysis using ANCOVA adjusted for baseline value, prior antihyperglycemic medication, menopausal status and baseline eGFR.
- ‡ p<0.001 compared to placebo.
HbA1c (%) N = 207 N = 205 N = 201 Baseline (mean) 8.2 8.1 8.1 Change from baseline (LS mean†) -0.2 -0.7 -0.9 Difference from placebo (LS mean†, 95% CI) -0.5‡ (-0.7, -0.4) -0.7‡ (-0.9, -0.5) Patients [N (%)] with HbA1c <7% 38 (18.4) 74 (36.3) 87 (43.3) FPG (mg/dL) N = 202 N = 199 N = 201 Baseline (mean) 169.1 168.1 167.9 Change from baseline (LS mean†) -8.7 -30.3 -40.9 Difference from placebo (LS mean†, 95% CI) -21.6‡ (-27.8, -15.5) -32.3‡ (-38.5, -26.0) The mean baseline body weight was 84.5 kg, 84.9 kg, and 85.3 kg in the placebo, STEGLATRO 5 mg, and STEGLATRO 15 mg groups, respectively. The mean changes from baseline to Week 26 were -1.4 kg, -3.2 kg, and -3.0 kg in the placebo, STEGLATRO 5 mg, and STEGLATRO 15 mg groups, respectively. The difference from placebo (95% CI) for STEGLATRO 5 mg was -1.8 kg (-2.4, -1.2) and for STEGLATRO 15 mg was -1.7 kg (-2.2, -1.1).
The mean baseline systolic blood pressure was 129.3 mmHg, 130.5 mmHg, and 130.2 mmHg in the placebo, STEGLATRO 5 mg, and STEGLATRO 15 mg groups, respectively. The mean changes from baseline to Week 26 were -1.8 mmHg, -5.1 mmHg, and -5.7 mmHg in the placebo, STEGLATRO 5 mg, and STEGLATRO 15 mg groups, respectively. The difference from placebo (95% CI) for STEGLATRO 5 mg was -3.3 mmHg (-5.6, -1.1) and for STEGLATRO 15 mg was -3.8 mmHg (-6.1, -1.5).
Active Controlled Study versus Glimepiride as Add-on Combination Therapy with Metformin
A total of 1,326 patients with type 2 diabetes mellitus inadequately controlled (HbA1c between 7% and 9%) on metformin monotherapy participated in a randomized, double-blind, multi-center, 52-week, active comparator controlled study (NCT01999218) to evaluate the efficacy and safety of STEGLATRO in combination with metformin. These patients, who were receiving metformin monotherapy (≥1,500 mg/day for ≥8 weeks), entered a 2-week, single-blind, placebo run-in period and were randomized to glimepiride, STEGLATRO 5 mg, or STEGLATRO 15 mg administered once daily in addition to continuation of background metformin therapy. Glimepiride was initiated at 1 mg/day and titrated up to a maximum dose of 6 or 8 mg/day (depending on maximum approved dose in each country) or a maximum tolerated dose or down-titrated to avoid or manage hypoglycemia. The mean daily dose of glimepiride was 3.0 mg.
STEGLATRO 15 mg was non-inferior to glimepiride after 52 weeks of treatment. (See Table 6.)
Table 6: Results at Week 52 from an Active-Controlled Study Comparing STEGLATRO to Glimepiride as Add-on Therapy in Patients with Type 2 Diabetes Mellitus Inadequately Controlled on Metformin* Glimepiride STEGLATRO 5 mg STEGLATRO 15 mg - * N includes all randomized and treated patients with a baseline measurement of the outcome variable. At Week 52, the primary HbA1c endpoint was missing for 15%, 20%, and 16% of patients and during the trial, rescue medication was initiated by 3%, 6%, and 4% of patients randomized to glimepiride, STEGLATRO 5 mg, and STEGLATRO 15 mg, respectively. Missing Week 52 measurements were imputed using multiple imputation with a mean equal to the baseline value of the patient. Results include measurements collected after initiation of rescue medication. For those patients who did not receive rescue medication and had values measured at 52 weeks, the mean changes from baseline for HbA1c were -0.8%, -0.6%, and -0.7% for glimepiride, STEGLATRO 5 mg, and STEGLATRO 15 mg, respectively.
- † Intent-to-treat analysis using ANCOVA adjusted for baseline value, prior antihyperglycemic medication and baseline eGFR.
- ‡ Non-inferiority is declared when the upper bound of the two-sided 95% confidence interval (CI) for the mean difference is less than 0.3%.
HbA1c (%) N = 437 N = 447 N = 440 Baseline (mean) 7.8 7.8 7.8 Change from baseline (LS mean†) -0.6 -0.5 -0.5 Difference from glimepiride (LS mean†, 95% CI) 0.2‡ (0.0, 0.3) 0.1‡ (-0.0, 0.2) Patients [N (%)] with HbA1c <7% 208 (47.7) 177 (39.5) 186 (42.2) The mean baseline body weight was 86.8 kg, 87.9 kg, and 85.6 kg in the glimepiride, STEGLATRO 5 mg, and STEGLATRO 15 mg groups, respectively. The mean changes from baseline to Week 52 were 0.6 kg, -2.6 kg, and -3.0 kg in the glimepiride, STEGLATRO 5 mg, and STEGLATRO 15 mg groups, respectively. The difference from glimepiride (95% CI) for STEGLATRO 5 mg was -3.2 kg (-3.7, -2.7) and for STEGLATRO 15 mg was -3.6 kg (-4.1, -3.1).
In Combination with Sitagliptin versus STEGLATRO Alone and Sitagliptin Alone, as Add-on to Metformin
A total of 1,233 patients with type 2 diabetes mellitus with inadequate glycemic control (HbA1c between 7.5% and 11%) on metformin monotherapy (≥1,500 mg/day for ≥8 weeks) participated in a randomized, double-blind, 26-week, active controlled study (NCT02099110) to evaluate the efficacy and safety of STEGLATRO 5 mg or 15 mg in combination with sitagliptin 100 mg compared to the individual components. Patients were randomized to one of five treatment arms: STEGLATRO 5 mg, STEGLATRO 15 mg, sitagliptin 100 mg, STEGLATRO 5 mg + sitagliptin 100 mg, or STEGLATRO 15 mg + sitagliptin 100 mg.
At Week 26, STEGLATRO 5 mg or 15 mg + sitagliptin 100 mg provided statistically significantly greater reductions in HbA1c compared to STEGLATRO (5 mg or 15 mg) alone or sitagliptin 100 mg alone. The mean change from baseline in HbA1c was -1.4% for STEGLATRO 5 mg or 15 mg + sitagliptin 100 mg versus -1.0%, for STEGLATRO 5 mg, STEGLATRO 15 mg, or sitagliptin 100 mg, respectively. More patients receiving STEGLATRO 5 mg or 15 mg + sitagliptin 100 mg achieved an HbA1c <7% (53.3% and 50.9%, for STEGLATRO 5 mg or 15 mg, respectively, + sitagliptin 100 mg) compared to the individual components (29.3%, 33.7%, and 38.5% for STEGLATRO 5 mg, STEGLATRO 15 mg, or sitagliptin 100 mg, respectively).
Add-on Combination Therapy with Metformin and Sitagliptin
A total of 463 patients with type 2 diabetes mellitus inadequately controlled (HbA1c between 7% and 10.5%) on metformin (≥1,500 mg/day for ≥8 weeks) and sitagliptin 100 mg once daily participated in a randomized, double-blind, multi-center, 26-week, placebo-controlled study (NCT02036515) to evaluate the efficacy and safety of STEGLATRO. Patients entered a 2-week, single-blind, placebo run-in period and were randomized to placebo, STEGLATRO 5 mg, or STEGLATRO 15 mg.
At Week 26, treatment with STEGLATRO at 5 mg or 15 mg daily provided statistically significant reductions in HbA1c. STEGLATRO also resulted in a higher proportion of patients achieving an HbA1c <7% compared to placebo (see Table 7).
Table 7: Results at Week 26 from an Add-on Study of STEGLATRO in Combination with Metformin and Sitagliptin in Patients with Type 2 Diabetes Mellitus* Placebo STEGLATRO 5 mg STEGLATRO 15 mg - * N includes all randomized and treated patients with a baseline measurement of the outcome variable. At Week 26, the primary HbA1c endpoint was missing for 10%, 11%, and 7% of patients and during the trial, rescue medication was initiated by 16%, 1%, and 2% of patients randomized to placebo, STEGLATRO 5 mg, and STEGLATRO 15 mg, respectively. Missing Week 26 measurements were imputed using multiple imputation with a mean equal to the baseline value of the patient. Results include measurements collected after initiation of rescue medication. For those patients who did not receive rescue medication and had values measured at 26 weeks, the mean changes from baseline for HbA1c were -0.2%, -0.8%, and -0.9% for placebo, STEGLATRO 5 mg, and STEGLATRO 15 mg, respectively.
- † Intent-to-treat analysis using ANCOVA adjusted for baseline value, prior antihyperglycemic medication and baseline eGFR.
- ‡ p<0.001 compared to placebo.
HbA1c (%) N = 152 N = 155 N = 152 Baseline (mean) 8.0 8.1 8.0 Change from baseline (LS mean†) -0.2 -0.7 -0.8 Difference from placebo (LS mean†, 95% CI) -0.5‡ (-0.7, -0.3) -0.6‡ (-0.8, -0.4) Patients [N (%)] with HbA1c <7% 31 (20.2) 54 (34.6) 64 (42.3) FPG (mg/dL) N = 152 N = 156 N = 152 Baseline (mean) 169.6 167.7 171.7 Change from baseline (LS mean†) -6.5 -25.7 -32.1 Difference from placebo (LS mean†, 95% CI) -19.2‡ (-26.8, -11.6) -25.6‡ (-33.2, -18.0) The mean baseline body weight was 86.5 kg, 87.6 kg, and 86.6 kg in the placebo, STEGLATRO 5 mg, and STEGLATRO 15 mg groups, respectively. The mean changes from baseline to Week 26 were -1.0 kg, -3.0 kg, and -2.8 kg in the placebo, STEGLATRO 5 mg, and STEGLATRO 15 mg groups, respectively. The difference from placebo (95% CI) for STEGLATRO 5 mg was -1.9 kg (-2.6, -1.3) and for STEGLATRO 15 mg was -1.8 kg (-2.4, -1.2).
The mean baseline systolic blood pressure was 130.2 mmHg, 132.1 mmHg, and 131.6 mmHg in the placebo, STEGLATRO 5 mg, and STEGLATRO 15 mg groups, respectively. The mean changes from baseline to Week 26 were -0.2 mmHg, -3.8 mmHg, and -4.5 mmHg in the placebo, STEGLATRO 5 mg, and STEGLATRO 15 mg groups, respectively. The difference from placebo (95% CI) for STEGLATRO 5 mg was -3.7 mmHg (-6.1, -1.2) and for STEGLATRO 15 mg was -4.3 mmHg (-6.7, -1.9).
Initial Combination Therapy with Sitagliptin
A total of 291 patients with type 2 diabetes mellitus inadequately controlled (HbA1c between 8% and 10.5%) on diet and exercise participated in a randomized, double-blind, multi-center, placebo-controlled 26-week study (NCT02226003) to evaluate the efficacy and safety of STEGLATRO in combination with sitagliptin. These patients, who were not receiving any background antihyperglycemic treatment for ≥8 weeks, entered a 2-week, single-blind, placebo run-in period and were randomized to placebo, STEGLATRO 5 mg or STEGLATRO 15 mg in combination with sitagliptin (100 mg) once daily.
At Week 26, treatment with STEGLATRO 5 mg and 15 mg in combination with sitagliptin at 100 mg daily provided statistically significant reductions in HbA1c compared to placebo. STEGLATRO 5 mg and 15 mg in combination with sitagliptin at 100 mg daily also resulted in a higher proportion of patients achieving an HbA1c <7% and greater reductions in FPG compared with placebo.
14.4 Clinical Study of STEGLATRO in Patients with Moderate Renal Impairment and Type 2 Diabetes Mellitus
The efficacy of STEGLATRO was assessed in a multicenter, randomized, double-blind, placebo-controlled study (NCT01986855) of patients with type 2 diabetes mellitus and moderate renal impairment (468 patients with eGFR ≥30 to <60 mL/min/1.73 m2). In this study, 202 patients exposed to STEGLATRO (5 mg or 15 mg) had an eGFR between 45 and 60 mL/min/1.73 m2 and 111 patients exposed to STEGLATRO (5 mg or 15 mg) had an eGFR between 30 and 45 mL/min/1.73 m2. The mean duration of diabetes for the study population was approximately 14 years, and the majority of patients were receiving background insulin (55.9%) and/or sulfonylurea (40.3%) therapy. Approximately 50% had a history of cardiovascular disease or heart failure.
STEGLATRO did not show efficacy in this study. The HbA1c reductions from baseline to Week 26 were not significantly different between placebo and STEGLATRO 5 mg or 15 mg [see Use in Specific Populations (8.6)].
-
16 HOW SUPPLIED/STORAGE AND HANDLING
STEGLATRO (ertugliflozin) tablets are available in the strengths listed below:
5 mg tablets, are pink, triangular-shaped, biconvex, with "701" debossed on one side and plain on the other side. They are supplied as follows:
NDC: 0006-5363-03 unit-of-use bottles of 30
NDC: 0006-5363-06 unit-of-use bottles of 90
NDC: 0006-5363-07 bulk bottles of 500
15 mg tablets, are red, triangular-shaped, biconvex, with "702" debossed on one side and plain on the other side. They are supplied as follows:
NDC: 0006-5364-03 unit-of-use bottles of 30
NDC: 0006-5364-06 unit-of-use bottles of 90
NDC: 0006-5364-07 bulk bottles of 500
-
17 PATIENT COUNSELING INFORMATION
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
Instructions
Instruct patients to read the Medication Guide before starting STEGLATRO (ertugliflozin) and to reread it each time the prescription is renewed.
Inform patients of the potential risks and benefits of STEGLATRO and of alternative modes of therapy. Also inform patients about the importance of adherence to dietary instructions, regular physical activity, periodic blood glucose monitoring and HbA1c testing, recognition and management of hypoglycemia and hyperglycemia, and assessment for diabetes complications. Advise patients to seek medical advice promptly during periods of stress such as fever, trauma, infection, or surgery, as medication requirements may change.
Instruct patients to take STEGLATRO only as prescribed. If a dose is missed, advise patients to take it as soon as it is remembered unless it is almost time for the next dose, in which case patients should skip the missed dose and take the medicine at the next regularly scheduled time. Advise patients not to take two doses of STEGLATRO at the same time.
Hypoglycemia with Concomitant Use of Insulin and/or Insulin Secretagogue
Inform patients that the incidence of hypoglycemia may increase when STEGLATRO is added to insulin and/or an insulin secretagogue and that a lower dose of insulin or insulin secretagogue may be required to reduce the risk of hypoglycemia [see Warnings and Precautions (5.6)].
Hypotension
Inform patients that symptomatic hypotension may occur with STEGLATRO and advise them to contact their doctor if they experience such symptoms [see Warnings and Precautions (5.1)]. Inform patients that dehydration may increase the risk for hypotension, and to have adequate fluid intake.
Ketoacidosis
Inform patients that ketoacidosis is a serious life-threatening condition and that cases of ketoacidosis have been reported during use of STEGLATRO, sometimes associated with illness or surgery among other risk factors. Instruct patients to check ketones (when possible) if symptoms consistent with ketoacidosis occur even if blood glucose is not elevated. If symptoms of ketoacidosis (including nausea, vomiting, abdominal pain, tiredness, and labored breathing) occur, instruct patients to discontinue STEGLATRO and seek medical attention immediately [see Warnings and Precautions (5.2)].
Acute Kidney Injury
Inform patients that acute kidney injury has been reported during use of STEGLATRO. Advise patients to seek medical advice immediately if they have reduced oral intake (due to acute illness or fasting) or increased fluid losses (due to vomiting, diarrhea, or excessive heat exposure), as it may be appropriate to temporarily discontinue STEGLATRO use in those settings [see Warnings and Precautions (5.3)].
Monitoring of Renal Function
Inform patients about the importance of regular testing of renal function when receiving treatment with STEGLATRO [see Warnings and Precautions (5.3)].
Serious Urinary Tract Infections
Inform patients of the potential for urinary tract infections, which may be serious. Provide them with information on the symptoms of urinary tract infections. Advise them to seek medical advice if such symptoms occur [see Warnings and Precautions (5.4)].
Amputation
Inform patients of the potential for an increased risk of amputations. Counsel patients about the importance of routine preventative foot care. Instruct patients to monitor for new pain or tenderness, sores or ulcers, or infections involving the leg or foot and to seek medical advice immediately if such signs or symptoms develop [see Warnings and Precautions (5.5)].
Necrotizing Fasciitis of the Perineum (Fournier's Gangrene)
Inform patients that necrotizing infections of the perineum (Fournier's gangrene) have occurred with SGLT2 inhibitors. Counsel patients to promptly seek medical attention if they develop pain or tenderness, redness, or swelling of the genitals or the area from the genitals back to the rectum, along with a fever above 100.4°F or malaise [see Warnings and Precautions (5.7)].
Genital Mycotic Infections in Females (e.g., Vulvovaginitis)
Inform female patients that vaginal yeast infections may occur and provide them with information on the signs and symptoms of vaginal yeast infection. Advise them of treatment options and when to seek medical advice [see Warnings and Precautions (5.8)].
Genital Mycotic Infections in Males (e.g., Balanitis or Balanoposthitis)
Inform male patients that yeast infections of the penis (e.g., balanitis or balanoposthitis) may occur, especially in uncircumcised males. Provide them with information on the signs and symptoms of balanitis and balanoposthitis (rash or redness of the glans or foreskin of the penis). Advise them of treatment options and when to seek medical advice [see Warnings and Precautions (5.8)].
Fetal Toxicity
Advise pregnant patients of the potential risk to a fetus with treatment with STEGLATRO. Instruct patients to immediately inform their healthcare provider if pregnant or planning to become pregnant [see Use in Specific Populations (8.1)].
Lactation
Advise patients that use of STEGLATRO is not recommended while breastfeeding [see Use in Specific Populations (8.2)].
-
SPL UNCLASSIFIED SECTION
Manufactured for: Merck Sharp & Dohme Corp., a subsidiary of
MERCK & CO., INC., Whitehouse Station, NJ 08889, USAFor patent information: www.merck.com/product/patent/home.html
Copyright © 2017-2020 Merck Sharp & Dohme Corp., a subsidiary of Merck & Co., Inc.
All rights reserved.uspi-mk8835-t-2001r003
-
MEDICATION GUIDE
Medication Guide
STEGLATRO™ (steh-GLA-troh)
(ertugliflozin)
tablets, for oral useThis Medication Guide has been approved by the U.S. Food and Drug Administration. Revised: 01/2020 Read this Medication Guide carefully before you start taking STEGLATRO and each time you get a refill. There may be new information. This information does not take the place of talking with your doctor about your medical condition or your treatment. What is the most important information I should know about STEGLATRO?
STEGLATRO may cause serious side effects, including:- Dehydration. STEGLATRO can cause some people to become dehydrated (the loss of body water and salt). Dehydration may cause you to feel dizzy, faint, lightheaded, or weak, especially when you stand up (orthostatic hypotension).
- have low blood pressure
- take medicines to lower your blood pressure, including water pills (diuretics)
- have kidney problems
- are on a low sodium (salt) diet
- are 65 years of age or older
-
Vaginal yeast infection. Women who take STEGLATRO may get vaginal yeast infections. Symptoms of a vaginal yeast infection include:
- vaginal odor
- white or yellowish vaginal discharge (discharge may be lumpy or look like cottage cheese)
- vaginal itching
- Yeast infection of the penis (balanitis or balanoposthitis). Men who take STEGLATRO may get a yeast infection of the skin around the penis. Certain men who are not circumcised may have swelling of the penis that makes it difficult to pull back the skin around the tip of your penis. Other symptoms of yeast infection of the penis include:
- redness, itching, or swelling of the penis
- foul smelling discharge from the penis
- rash of the penis
- pain in the skin around your penis
Talk to your doctor about what to do if you get symptoms of a yeast infection of the vagina or penis. Your doctor may suggest you use an over-the-counter antifungal medicine. Talk to your doctor right away if you use an over-the-counter antifungal medicine and your symptoms do not go away. What is STEGLATRO? - STEGLATRO is a prescription medicine used along with diet and exercise to lower blood sugar in adults with type 2 diabetes.
- STEGLATRO is not for people with type 1 diabetes.
- STEGLATRO is not for people with diabetic ketoacidosis (increased ketones in your blood or urine).
- It is not known if STEGLATRO is safe and effective in children under 18 years of age.
Do not take STEGLATRO if you: - have severe kidney problems or are on dialysis.
- are allergic to ertugliflozin or any of the ingredients in STEGLATRO. See the end of this Medication Guide for a list of ingredients in STEGLATRO. Symptoms of a serious allergic reaction to STEGLATRO may include skin rash, raised red patches on your skin (hives), swelling of the face, lips, tongue, and throat that may cause difficulty in breathing or swallowing.
Before you take STEGLATRO, tell your doctor about all of your medical conditions, including if you: - have type 1 diabetes or have had diabetic ketoacidosis.
- have kidney problems.
- have liver problems.
- have or have had problems with your pancreas, including pancreatitis or surgery on your pancreas.
- have a history of urinary tract infections or problems with urination.
- have a history of amputation.
- have had blocked or narrowed blood vessels, usually in the leg.
- have damage to the nerves (neuropathy) in your leg.
- have had diabetic foot ulcers or sores.
- are going to have surgery. Your doctor may stop your STEGLATRO before you have surgery. Talk to your doctor if you are having surgery about when to stop taking STEGLATRO and when to start it again.
- are eating less or there is a change in your diet.
- drink alcohol very often, or drink a lot of alcohol in the short term ("binge" drinking).
- are pregnant or plan to become pregnant. STEGLATRO may harm your unborn baby. If you become pregnant while taking STEGLATRO, your doctor may switch you to a different medicine to control your blood sugar. Talk to your doctor about the best way to control your blood sugar if you plan to become pregnant or while you are pregnant.
- are breastfeeding or plan to breastfeed. It is not known if STEGLATRO passes into your breast milk. You should not breastfeed if you take STEGLATRO.
How should I take STEGLATRO? - Take STEGLATRO exactly as your doctor tells you to take it.
- Take STEGLATRO by mouth 1 time in the morning each day, with or without food.
- Your doctor may change your dose if needed.
- If you miss a dose, take it as soon as you remember. If it is almost time for your next dose, skip the missed dose and take the medicine at the next regularly scheduled time. Do not take 2 doses of STEGLATRO at the same time.
- Your doctor may tell you to take STEGLATRO along with other diabetes medicines. Low blood sugar can happen more often when STEGLATRO is taken with certain other diabetes medicines. See "What are the possible side effects of STEGLATRO?".
- Stay on your prescribed diet and exercise program while taking STEGLATRO.
- Check your blood sugar as your doctor tells you to.
- Your doctor will check your diabetes with regular blood tests, including your blood sugar levels and your HbA1c.
- Talk to your doctor about how to prevent, recognize and manage low blood sugar (hypoglycemia), high blood sugar (hyperglycemia), complications of diabetes.
- Your doctor will do blood tests to check how well your kidneys are working before and during your treatment with STEGLATRO.
- When your body is under some types of stress, such as fever, trauma (such as a car accident), infection, or surgery, the amount of diabetes medicine you need may change. Tell your doctor right away if you have any of these conditions and follow your doctor's instructions.
- When taking STEGLATRO, you may have sugar in your urine, which will show up on a urine test.
- If you take too much STEGLATRO, call your doctor or go to the nearest hospital emergency room right away.
What are the possible side effects of STEGLATRO?
STEGLATRO may cause serious side effects, including:
See "What is the most important information I should know about STEGLATRO?"- ketoacidosis (increased ketones in your blood or urine). Ketoacidosis has happened in people who have type 1 diabetes or type 2 diabetes during treatment with STEGLATRO. Ketoacidosis has also happened in people with diabetes who were sick or who had surgery during treatment with STEGLATRO. Ketoacidosis is a serious condition, which may need to be treated in a hospital. Ketoacidosis may lead to death. Ketoacidosis can happen even if your blood sugar is less than 250 mg/dL. Stop taking STEGLATRO and call your doctor right away if you get any of the following symptoms:
- nausea
- vomiting
- stomach-area (abdominal) pain
- tiredness
- trouble breathing
If you get any of these symptoms during treatment with STEGLATRO, if possible check for ketones in your urine, even if your blood sugar is less than 250 mg/dL. -
kidney problems. Sudden kidney injury has happened to people treated with STEGLATRO. Talk to your doctor right away if you:
- reduce the amount of food or liquid you drink, for example, if you are sick or cannot eat or
- you start to lose liquids from your body, for example, from vomiting, diarrhea, or being in the sun too long
- serious urinary tract infections. Serious urinary tract infections that may lead to hospitalization have happened in people who are taking STEGLATRO. Tell your doctor if you have any signs or symptoms of a urinary tract infection such as a burning feeling when passing urine, a need to urinate often, the need to urinate right away, pain in the lower part of your stomach (pelvis), or blood in the urine. Sometimes people may also have a fever, back pain, nausea, or vomiting.
-
amputations. STEGLATRO may increase your risk of lower limb amputations. Amputations mainly involve removal of the toe.
You may be at a higher risk of lower limb amputation if you:- have a history of amputation
- have had blocked or narrowed blood vessels, usually in your leg
- have damage to the nerves (neuropathy) in your leg
- have had diabetic foot ulcers or sores
- low blood sugar (hypoglycemia). If you take STEGLATRO with another medicine that can cause low blood sugar such as a sulfonylurea or insulin, your risk of getting low blood sugar is higher. The dose of your sulfonylurea or insulin may need to be lowered while you take STEGLATRO. Signs and symptoms of low blood sugar may include:
- headache
- drowsiness
- hunger
- irritability
- dizziness
- confusion
- sweating
- feeling jittery or shaky
- weakness
- fast heartbeat
- a rare but serious bacterial infection that causes damage to the tissue under the skin (necrotizing fasciitis) in the area between and around the anus and genitals (perineum). Necrotizing fasciitis of the perineum has happened in women and men who take medicines that lower blood sugar in the same way as STEGLATRO. Necrotizing fasciitis of the perineum may lead to hospitalization, may require multiple surgeries, and may lead to death. Seek medical attention immediately if you have fever or you are feeling very weak, tired or uncomfortable (malaise) and you develop any of the following symptoms in the area between and around your anus and genitals:
- pain or tenderness
- swelling
- redness of skin (erythema)
- increased fats in your blood (bad cholesterol or LDL).
- vaginal yeast infections and yeast infections of the penis (See "What is the most important information I should know about STEGLATRO?")
- changes in urination, including urgent need to urinate more often, in larger amounts, or at night
Call your doctor for medical advice about side effects. You may report side effects to the FDA at 1-800-FDA-1088.How should I store STEGLATRO? - Store STEGLATRO at room temperature between 68°F to 77°F (20°C to 25°C).
- Keep STEGLATRO dry.
- Store blister packs of STEGLATRO in the original package.
General information about the safe and effective use of STEGLATRO.
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use STEGLATRO for a condition for which it was not prescribed. Do not give STEGLATRO to other people, even if they have the same symptoms that you have. It may harm them. You can ask your pharmacist or doctor for information about STEGLATRO that is written for health professionals.
For more information about STEGLATRO, go to www.steglatro.com or call 1-800-622-4477.What are the ingredients in STEGLATRO?
Active ingredient: ertugliflozin.
Inactive ingredients: microcrystalline cellulose, lactose monohydrate, sodium starch glycolate, and magnesium stearate. The tablet film coating contains the following inactive ingredients: hypromellose, lactose monohydrate, macrogol, triacetin, titanium dioxide, and iron oxide red.Manufactured for: Merck Sharp & Dohme Corp., a subsidiary of
MERCK & CO., INC., Whitehouse Station, NJ 08889, USA
For patent information, go to: www.merck.com/product/patent/home.html. Copyright © 2017-2020 Merck Sharp & Dohme Corp., a subsidiary of Merck & Co., Inc.
All rights reserved.
usmg-mk8835-t-2001r002 -
PRINCIPAL DISPLAY PANEL - 5 mg Tablet Bottle Label
NDC: 0006-5363-03
Steglatro™
(ertugliflozin) tablets5 mg
Dispense the accompanying Medication Guide
to each patient.Each tablet contains 6.48 mg ertugliflozin L-pyroglutamic
acid (equivalent to 5 mg ertugliflozin).Rx only
30 Tablets
-
PRINCIPAL DISPLAY PANEL - 15 mg Tablet Bottle Label
NDC: 0006-5364-03
Steglatro™
(ertugliflozin) tablets15 mg
Dispense the accompanying Medication Guide
to each patient.Each tablet contains 19.43 mg ertugliflozin L-pyroglutamic
acid (equivalent to 15 mg ertugliflozin).Rx only
30 Tablets
-
INGREDIENTS AND APPEARANCE
STEGLATRO
ertugliflozin tablet, film coatedProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 0006-5363 Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength ERTUGLIFLOZIN PIDOLATE (UNII: MLU731K321) (ERTUGLIFLOZIN - UNII:6C282481IP) ERTUGLIFLOZIN 5 mg Inactive Ingredients Ingredient Name Strength MICROCRYSTALLINE CELLULOSE (UNII: OP1R32D61U) LACTOSE MONOHYDRATE (UNII: EWQ57Q8I5X) SODIUM STARCH GLYCOLATE TYPE A POTATO (UNII: 5856J3G2A2) MAGNESIUM STEARATE (UNII: 70097M6I30) HYPROMELLOSE 2910 (6 MPA.S) (UNII: 0WZ8WG20P6) POLYETHYLENE GLYCOL 3350 (UNII: G2M7P15E5P) TRIACETIN (UNII: XHX3C3X673) TITANIUM DIOXIDE (UNII: 15FIX9V2JP) FERRIC OXIDE RED (UNII: 1K09F3G675) Product Characteristics Color PINK Score no score Shape TRIANGLE (Triangular, biconvex) Size 7mm Flavor Imprint Code 701 Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 0006-5363-03 30 in 1 BOTTLE; Type 0: Not a Combination Product 12/19/2017 2 NDC: 0006-5363-09 2 in 1 CARTON 12/19/2017 2 NDC: 0006-5363-08 7 in 1 BOTTLE; Type 0: Not a Combination Product 3 NDC: 0006-5363-06 90 in 1 BOTTLE; Type 0: Not a Combination Product 12/19/2017 4 NDC: 0006-5363-07 500 in 1 BOTTLE; Type 0: Not a Combination Product 12/19/2017 5 NDC: 0006-5363-10 30 in 1 BOTTLE; Type 0: Not a Combination Product 12/19/2017 Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date NDA NDA209803 12/19/2017 STEGLATRO
ertugliflozin tablet, film coatedProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 0006-5364 Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength ERTUGLIFLOZIN PIDOLATE (UNII: MLU731K321) (ERTUGLIFLOZIN - UNII:6C282481IP) ERTUGLIFLOZIN 15 mg Inactive Ingredients Ingredient Name Strength MICROCRYSTALLINE CELLULOSE (UNII: OP1R32D61U) LACTOSE MONOHYDRATE (UNII: EWQ57Q8I5X) SODIUM STARCH GLYCOLATE TYPE A POTATO (UNII: 5856J3G2A2) MAGNESIUM STEARATE (UNII: 70097M6I30) HYPROMELLOSE 2910 (6 MPA.S) (UNII: 0WZ8WG20P6) POLYETHYLENE GLYCOL 3350 (UNII: G2M7P15E5P) TRIACETIN (UNII: XHX3C3X673) TITANIUM DIOXIDE (UNII: 15FIX9V2JP) FERRIC OXIDE RED (UNII: 1K09F3G675) Product Characteristics Color RED Score no score Shape TRIANGLE (Triangular, biconvex) Size 9mm Flavor Imprint Code 702 Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 0006-5364-03 30 in 1 BOTTLE; Type 0: Not a Combination Product 12/19/2017 2 NDC: 0006-5364-09 2 in 1 CARTON 12/19/2017 2 NDC: 0006-5364-08 7 in 1 BOTTLE; Type 0: Not a Combination Product 3 NDC: 0006-5364-06 90 in 1 BOTTLE; Type 0: Not a Combination Product 12/19/2017 4 NDC: 0006-5364-07 500 in 1 BOTTLE; Type 0: Not a Combination Product 12/19/2017 Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date NDA NDA209803 12/19/2017 Labeler - Merck Sharp & Dohme Corp. (001317601)
Trademark Results [STEGLATRO]
Mark Image Registration | Serial | Company Trademark Application Date |
|---|---|
 STEGLATRO 86576333 5498114 Live/Registered |
Merck Sharp & Dohme Corp. 2015-03-25 |
© 2026 FDA.report
This site is not affiliated with or endorsed by the FDA.