JANUVIA- sitagliptin tablet, film coated
JANUVIA by
Drug Labeling and Warnings
JANUVIA by is a Prescription medication manufactured, distributed, or labeled by Merck Sharp & Dohme LLC. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
-
HIGHLIGHTS OF PRESCRIBING INFORMATION
These highlights do not include all the information needed to use JANUVIA safely and effectively. See full prescribing information for JANUVIA.
JANUVIA® (sitagliptin) tablets, for oral use
Initial U.S. Approval: 2006INDICATIONS AND USAGE
JANUVIA is a dipeptidyl peptidase-4 (DPP-4) inhibitor indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus. (1)
Limitations of Use:DOSAGE AND ADMINISTRATION
The recommended dose of JANUVIA is 100 mg once daily. JANUVIA can be taken with or without food. (2.1)
Dosage adjustment is recommended for patients with eGFR less than 45 mL/min/1.73 m2. (2.2)Dosage Adjustment in Patients with Renal Impairment (2.2) eGFR greater than or equal to 30 mL/min/1.73 m2 to less than 45 mL/min/1.73 m2 eGFR less than 30 mL/min/1.73 m2 (including patients with end stage renal disease [ESRD] on dialysis) 50 mg once daily 25 mg once daily DOSAGE FORMS AND STRENGTHS
Tablets: 100 mg, 50 mg, and 25 mg (3)
CONTRAINDICATIONS
WARNINGS AND PRECAUTIONS
- There have been postmarketing reports of acute pancreatitis, including fatal and non-fatal hemorrhagic or necrotizing pancreatitis. If pancreatitis is suspected, promptly discontinue JANUVIA. (5.1)
- Heart failure has been observed with two other members of the DPP-4 inhibitor class. Consider risks and benefits of JANUVIA in patients who have known risk factors for heart failure. Monitor patients for signs and symptoms. (5.2)
- There have been postmarketing reports of acute renal failure, sometimes requiring dialysis. Dosage adjustment is recommended in patients with moderate or severe renal impairment and in patients with ESRD. Assessment of renal function is recommended prior to initiating JANUVIA and periodically thereafter. (2.2, 5.3, 6.2)
- There is an increased risk of hypoglycemia when JANUVIA is added to an insulin secretagogue (e.g., sulfonylurea) or insulin therapy. Consider lowering the dose of the sulfonylurea or insulin to reduce the risk of hypoglycemia. (5.4, 7.2)
- There have been postmarketing reports of serious allergic and hypersensitivity reactions in patients treated with JANUVIA such as anaphylaxis, angioedema, and exfoliative skin conditions including Stevens-Johnson syndrome. In such cases, promptly stop JANUVIA, assess for other potential causes, institute appropriate monitoring and treatment, and initiate alternative treatment for diabetes. (5.5, 6.2)
- Severe and disabling arthralgia has been reported in patients taking DPP-4 inhibitors. Consider as a possible cause for severe joint pain and discontinue drug if appropriate. (5.6)
- There have been postmarketing reports of bullous pemphigoid requiring hospitalization in patients taking DPP-4 inhibitors. Tell patients to report development of blisters or erosions. If bullous pemphigoid is suspected, discontinue JANUVIA. (5.7)
- There have been no clinical studies establishing conclusive evidence of macrovascular risk reduction with JANUVIA. (5.8)
ADVERSE REACTIONS
Adverse reactions reported in ≥5% of patients treated with JANUVIA and more commonly than in patients treated with placebo are: upper respiratory tract infection, nasopharyngitis and headache. In the add-on to sulfonylurea and add-on to insulin studies, hypoglycemia was also more commonly reported in patients treated with JANUVIA compared to placebo. (6.1)
To report SUSPECTED ADVERSE REACTIONS, contact Merck Sharp & Dohme Corp., a subsidiary of Merck & Co., Inc., at 1-877-888-4231 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.USE IN SPECIFIC POPULATIONS
- There are no adequate and well-controlled studies in pregnant women. To report drug exposure during pregnancy call 1-800-986-8999. (8.1)
See 17 for PATIENT COUNSELING INFORMATION and Medication Guide.
Revised: 8/2019
-
Table of Contents
FULL PRESCRIBING INFORMATION: CONTENTS*
1 INDICATIONS AND USAGE
2 DOSAGE AND ADMINISTRATION
2.1 Recommended Dosing
2.2 Recommendations for Use in Renal Impairment
3 DOSAGE FORMS AND STRENGTHS
4 CONTRAINDICATIONS
5 WARNINGS AND PRECAUTIONS
5.1 Pancreatitis
5.2 Heart Failure
5.3 Assessment of Renal Function
5.4 Use with Medications Known to Cause Hypoglycemia
5.5 Hypersensitivity Reactions
5.6 Severe and Disabling Arthralgia
5.7 Bullous Pemphigoid
5.8 Macrovascular Outcomes
6 ADVERSE REACTIONS
6.1 Clinical Trials Experience
6.2 Postmarketing Experience
7 DRUG INTERACTIONS
7.1 Digoxin
7.2 Insulin Secretagogues or Insulin
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
8.2 Lactation
8.4 Pediatric Use
8.5 Geriatric Use
8.6 Renal Impairment
10 OVERDOSAGE
11 DESCRIPTION
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
12.2 Pharmacodynamics
12.3 Pharmacokinetics
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
14 CLINICAL STUDIES
14.1 Monotherapy
14.2 Combination Therapy
16 HOW SUPPLIED/STORAGE AND HANDLING
17 PATIENT COUNSELING INFORMATION
- * Sections or subsections omitted from the full prescribing information are not listed.
-
1 INDICATIONS AND USAGE
JANUVIA® is indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus.
Limitations of Use
JANUVIA should not be used in patients with type 1 diabetes or for the treatment of diabetic ketoacidosis, as it would not be effective in these settings.
JANUVIA has not been studied in patients with a history of pancreatitis. It is unknown whether patients with a history of pancreatitis are at increased risk for the development of pancreatitis while using JANUVIA. [See Warnings and Precautions (5.1).]
-
2 DOSAGE AND ADMINISTRATION
2.1 Recommended Dosing
The recommended dose of JANUVIA is 100 mg once daily. JANUVIA can be taken with or without food.
2.2 Recommendations for Use in Renal Impairment
For patients with an estimated glomerular filtration rate [eGFR] greater than or equal to 45 mL/min/1.73 m2 to less than 90 mL/min/1.73 m2, no dosage adjustment for JANUVIA is required.
For patients with moderate renal impairment (eGFR greater than or equal to 30 mL/min/1.73 m2 to less than 45 mL/min/1.73 m2), the dose of JANUVIA is 50 mg once daily.
For patients with severe renal impairment (eGFR less than 30 mL/min/1.73 m2) or with end-stage renal disease (ESRD) requiring hemodialysis or peritoneal dialysis, the dose of JANUVIA is 25 mg once daily. JANUVIA may be administered without regard to the timing of dialysis.
Because there is a need for dosage adjustment based upon renal function, assessment of renal function is recommended prior to initiation of JANUVIA and periodically thereafter. There have been postmarketing reports of worsening renal function in patients with renal impairment, some of whom were prescribed inappropriate doses of sitagliptin.
- 3 DOSAGE FORMS AND STRENGTHS
-
4 CONTRAINDICATIONS
History of a serious hypersensitivity reaction to sitagliptin, such as anaphylaxis or angioedema. [See Warnings and Precautions (5.5); Adverse Reactions (6.2).]
-
5 WARNINGS AND PRECAUTIONS
5.1 Pancreatitis
There have been postmarketing reports of acute pancreatitis, including fatal and non-fatal hemorrhagic or necrotizing pancreatitis, in patients taking JANUVIA. After initiation of JANUVIA, patients should be observed carefully for signs and symptoms of pancreatitis. If pancreatitis is suspected, JANUVIA should promptly be discontinued and appropriate management should be initiated. It is unknown whether patients with a history of pancreatitis are at increased risk for the development of pancreatitis while using JANUVIA.
5.2 Heart Failure
An association between dipeptidyl peptidase-4 (DPP-4) inhibitor treatment and heart failure has been observed in cardiovascular outcomes trials for two other members of the DPP-4 inhibitor class. These trials evaluated patients with type 2 diabetes mellitus and atherosclerotic cardiovascular disease.
Consider the risks and benefits of JANUVIA prior to initiating treatment in patients at risk for heart failure, such as those with a prior history of heart failure and a history of renal impairment, and observe these patients for signs and symptoms of heart failure during therapy. Advise patients of the characteristic symptoms of heart failure and to immediately report such symptoms. If heart failure develops, evaluate and manage according to current standards of care and consider discontinuation of JANUVIA.
5.3 Assessment of Renal Function
Assessment of renal function is recommended prior to initiating JANUVIA and periodically thereafter. A dosage adjustment is recommended in patients with moderate or severe renal impairment and in patients with ESRD requiring hemodialysis or peritoneal dialysis. [See Dosage and Administration (2.2); Clinical Pharmacology (12.3).] Caution should be used to ensure that the correct dose of JANUVIA is prescribed for patients with moderate (eGFR ≥30 mL/min/1.73 m2 to <45 mL/min/1.73 m2) or severe (eGFR <30 mL/min/1.73 m2) renal impairment.
There have been postmarketing reports of worsening renal function, including acute renal failure, sometimes requiring dialysis. A subset of these reports involved patients with renal impairment, some of whom were prescribed inappropriate doses of sitagliptin. A return to baseline levels of renal impairment has been observed with supportive treatment and discontinuation of potentially causative agents. Consideration can be given to cautiously reinitiating JANUVIA if another etiology is deemed likely to have precipitated the acute worsening of renal function.
JANUVIA has not been found to be nephrotoxic in preclinical studies at clinically relevant doses, or in clinical trials.
5.4 Use with Medications Known to Cause Hypoglycemia
When JANUVIA was used in combination with a sulfonylurea or with insulin, medications known to cause hypoglycemia, the incidence of hypoglycemia was increased over that of placebo used in combination with a sulfonylurea or with insulin. [See Adverse Reactions (6.1).] Therefore, a lower dose of sulfonylurea or insulin may be required to reduce the risk of hypoglycemia. [See Drug Interactions (7.2).]
5.5 Hypersensitivity Reactions
There have been postmarketing reports of serious hypersensitivity reactions in patients treated with JANUVIA. These reactions include anaphylaxis, angioedema, and exfoliative skin conditions including Stevens-Johnson syndrome. Onset of these reactions occurred within the first 3 months after initiation of treatment with JANUVIA, with some reports occurring after the first dose. If a hypersensitivity reaction is suspected, discontinue JANUVIA, assess for other potential causes for the event, and institute alternative treatment for diabetes. [See Adverse Reactions (6.2).]
Angioedema has also been reported with other DPP-4 inhibitors. Use caution in a patient with a history of angioedema with another DPP-4 inhibitor because it is unknown whether such patients will be predisposed to angioedema with JANUVIA.
5.6 Severe and Disabling Arthralgia
There have been postmarketing reports of severe and disabling arthralgia in patients taking DPP-4 inhibitors. The time to onset of symptoms following initiation of drug therapy varied from one day to years. Patients experienced relief of symptoms upon discontinuation of the medication. A subset of patients experienced a recurrence of symptoms when restarting the same drug or a different DPP-4 inhibitor. Consider DPP-4 inhibitors as a possible cause for severe joint pain and discontinue drug if appropriate.
5.7 Bullous Pemphigoid
Postmarketing cases of bullous pemphigoid requiring hospitalization have been reported with DPP-4 inhibitor use. In reported cases, patients typically recovered with topical or systemic immunosuppressive treatment and discontinuation of the DPP-4 inhibitor. Tell patients to report development of blisters or erosions while receiving JANUVIA. If bullous pemphigoid is suspected, JANUVIA should be discontinued and referral to a dermatologist should be considered for diagnosis and appropriate treatment.
-
6 ADVERSE REACTIONS
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
In controlled clinical studies as both monotherapy and combination therapy with metformin, pioglitazone, or rosiglitazone and metformin, the overall incidence of adverse reactions, hypoglycemia, and discontinuation of therapy due to clinical adverse reactions with JANUVIA were similar to placebo. In combination with glimepiride, with or without metformin, the overall incidence of clinical adverse reactions with JANUVIA was higher than with placebo, in part related to a higher incidence of hypoglycemia (see Table 3); the incidence of discontinuation due to clinical adverse reactions was similar to placebo.
Two placebo-controlled monotherapy studies, one of 18- and one of 24-week duration, included patients treated with JANUVIA 100 mg daily, JANUVIA 200 mg daily, and placebo. Five placebo-controlled add-on combination therapy studies were also conducted: one with metformin; one with pioglitazone; one with metformin and rosiglitazone; one with glimepiride (with or without metformin); and one with insulin (with or without metformin). In these trials, patients with inadequate glycemic control on a stable dose of the background therapy were randomized to add-on therapy with JANUVIA 100 mg daily or placebo. The adverse reactions, excluding hypoglycemia, reported regardless of investigator assessment of causality in ≥5% of patients treated with JANUVIA 100 mg daily and more commonly than in patients treated with placebo, are shown in Table 1 for the clinical trials of at least 18 weeks duration. Incidences of hypoglycemia are shown in Table 3.
Table 1: Placebo-Controlled Clinical Studies of JANUVIA Monotherapy or Add-on Combination Therapy with Pioglitazone, Metformin + Rosiglitazone, or Glimepiride +/- Metformin: Adverse Reactions (Excluding Hypoglycemia) Reported in ≥5% of Patients and More Commonly than in Patients Given Placebo, Regardless of Investigator Assessment of Causality* Number of Patients (%) - * Intent-to-treat population
Monotherapy (18 or 24 weeks) JANUVIA 100 mg Placebo N = 443 N = 363 Nasopharyngitis 23 (5.2) 12 (3.3) Combination with Pioglitazone
(24 weeks)JANUVIA 100 mg +
PioglitazonePlacebo +
PioglitazoneN = 175 N = 178 Upper Respiratory Tract Infection 11 (6.3) 6 (3.4) Headache 9 (5.1) 7 (3.9) Combination with Metformin +
Rosiglitazone (18 weeks)JANUVIA 100 mg +
Metformin + RosiglitazonePlacebo +
Metformin + RosiglitazoneN = 181 N = 97 Upper Respiratory Tract Infection 10 (5.5) 5 (5.2) Nasopharyngitis 11 (6.1) 4 (4.1) Combination with Glimepiride
(+/- Metformin) (24 weeks)JANUVIA 100 mg
+ Glimepiride
(+/- Metformin)
Placebo
+ Glimepiride
(+/- Metformin)
N = 222 N = 219 Nasopharyngitis 14 (6.3) 10 (4.6) Headache 13 (5.9) 5 (2.3) In the 24-week study of patients receiving JANUVIA as add-on combination therapy with metformin, there were no adverse reactions reported regardless of investigator assessment of causality in ≥5% of patients and more commonly than in patients given placebo.
In the 24-week study of patients receiving JANUVIA as add-on therapy to insulin (with or without metformin), there were no adverse reactions reported regardless of investigator assessment of causality in ≥5% of patients and more commonly than in patients given placebo, except for hypoglycemia (see Table 3).
In the study of JANUVIA as add-on combination therapy with metformin and rosiglitazone (Table 1), through Week 54 the adverse reactions reported regardless of investigator assessment of causality in ≥5% of patients treated with JANUVIA and more commonly than in patients treated with placebo were: upper respiratory tract infection (JANUVIA, 15.5%; placebo, 6.2%), nasopharyngitis (11.0%, 9.3%), peripheral edema (8.3%, 5.2%), and headache (5.5%, 4.1%).
In a pooled analysis of the two monotherapy studies, the add-on to metformin study, and the add-on to pioglitazone study, the incidence of selected gastrointestinal adverse reactions in patients treated with JANUVIA was as follows: abdominal pain (JANUVIA 100 mg, 2.3%; placebo, 2.1%), nausea (1.4%, 0.6%), and diarrhea (3.0%, 2.3%).
In an additional, 24-week, placebo-controlled factorial study of initial therapy with sitagliptin in combination with metformin, the adverse reactions reported (regardless of investigator assessment of causality) in ≥5% of patients are shown in Table 2.
Table 2: Initial Therapy with Combination of Sitagliptin and Metformin: Adverse Reactions Reported (Regardless of Investigator Assessment of Causality) in ≥5% of Patients Receiving Combination Therapy (and Greater than in Patients Receiving Metformin alone, Sitagliptin alone, and Placebo)* Number of Patients (%) - * Intent-to-treat population.
- † Data pooled for the patients given the lower and higher doses of metformin.
Placebo
Sitagliptin
(JANUVIA)
100 mg QDMetformin
500 or 1000 mg bid†
Sitagliptin
50 mg bid +
Metformin
500 or 1000 mg bid†
N = 176 N = 179 N = 364† N = 372† Upper Respiratory Infection 9 (5.1) 8 (4.5) 19 (5.2) 23 (6.2) Headache 5 (2.8) 2 (1.1) 14 (3.8) 22 (5.9) In a 24-week study of initial therapy with JANUVIA in combination with pioglitazone, there were no adverse reactions reported (regardless of investigator assessment of causality) in ≥5% of patients and more commonly than in patients given pioglitazone alone.
No clinically meaningful changes in vital signs or in ECG (including in QTc interval) were observed in patients treated with JANUVIA.
In a pooled analysis of 19 double-blind clinical trials that included data from 10,246 patients randomized to receive sitagliptin 100 mg/day (N=5429) or corresponding (active or placebo) control (N=4817), the incidence of acute pancreatitis was 0.1 per 100 patient-years in each group (4 patients with an event in 4708 patient-years for sitagliptin and 4 patients with an event in 3942 patient-years for control). [See Warnings and Precautions (5.1).]
Hypoglycemia
In the above studies (N=9), adverse reactions of hypoglycemia were based on all reports of symptomatic hypoglycemia. A concurrent blood glucose measurement was not required although most (74%) reports of hypoglycemia were accompanied by a blood glucose measurement ≤70 mg/dL. When JANUVIA was coadministered with a sulfonylurea or with insulin, the percentage of patients with at least one adverse reaction of hypoglycemia was higher than in the corresponding placebo group (Table 3).
Table 3: Incidence and Rate of Hypoglycemia* in Placebo-Controlled Clinical Studies when JANUVIA was used as Add-On Therapy to Glimepiride (with or without Metformin) or Insulin (with or without Metformin), Regardless of Investigator Assessment of Causality Add-On to Glimepiride
(+/- Metformin) (24 weeks)JANUVIA 100 mg
+ Glimepiride
(+/- Metformin)Placebo
+ Glimepiride
(+/- Metformin)- * Adverse reactions of hypoglycemia were based on all reports of symptomatic hypoglycemia; a concurrent glucose measurement was not required; intent-to-treat population.
- † Based on total number of events (i.e., a single patient may have had multiple events).
- ‡ Severe events of hypoglycemia were defined as those events requiring medical assistance or exhibiting depressed level/loss of consciousness or seizure.
N = 222 N = 219 Overall (%) 27 (12.2) 4 (1.8) Rate (episodes/patient-year)† 0.59 0.24 Severe (%)‡ 0 (0.0) 0 (0.0) Add-On to Insulin
(+/- Metformin) (24 weeks)JANUVIA 100 mg
+ Insulin
(+/- Metformin)Placebo
+ Insulin
(+/- Metformin)N = 322 N = 319 Overall (%) 50 (15.5) 25 (7.8) Rate (episodes/patient-year)† 1.06 0.51 Severe (%)‡ 2 (0.6) 1 (0.3) In a pooled analysis of the two monotherapy studies, the add-on to metformin study, and the add-on to pioglitazone study, the overall incidence of adverse reactions of hypoglycemia was 1.2% in patients treated with JANUVIA 100 mg and 0.9% in patients treated with placebo.
In the study of JANUVIA as add-on combination therapy with metformin and rosiglitazone, the overall incidence of hypoglycemia was 2.2% in patients given add-on JANUVIA and 0.0% in patients given add-on placebo through Week 18. Through Week 54, the overall incidence of hypoglycemia was 3.9% in patients given add-on JANUVIA and 1.0% in patients given add-on placebo.
In the 24-week, placebo-controlled factorial study of initial therapy with JANUVIA in combination with metformin, the incidence of hypoglycemia was 0.6% in patients given placebo, 0.6% in patients given JANUVIA alone, 0.8% in patients given metformin alone, and 1.6% in patients given JANUVIA in combination with metformin.
In the study of JANUVIA as initial therapy with pioglitazone, one patient taking JANUVIA experienced a severe episode of hypoglycemia. There were no severe hypoglycemia episodes reported in other studies except in the study involving coadministration with insulin.
In an additional, 30-week placebo-controlled, study of patients with type 2 diabetes inadequately controlled with metformin comparing the maintenance of sitagliptin 100 mg versus withdrawal of sitagliptin when initiating basal insulin therapy, the event rate and incidence of documented symptomatic hypoglycemia (blood glucose measurement ≤70 mg/dL) did not differ between the sitagliptin and placebo groups.
Laboratory Tests
Across clinical studies, the incidence of laboratory adverse reactions was similar in patients treated with JANUVIA 100 mg compared to patients treated with placebo. A small increase in white blood cell count (WBC) was observed due to an increase in neutrophils. This increase in WBC (of approximately 200 cells/microL vs placebo, in four pooled placebo-controlled clinical studies, with a mean baseline WBC count of approximately 6600 cells/microL) is not considered to be clinically relevant. In a 12-week study of 91 patients with chronic renal insufficiency, 37 patients with moderate renal insufficiency were randomized to JANUVIA 50 mg daily, while 14 patients with the same magnitude of renal impairment were randomized to placebo. Mean (SE) increases in serum creatinine were observed in patients treated with JANUVIA [0.12 mg/dL (0.04)] and in patients treated with placebo [0.07 mg/dL (0.07)]. The clinical significance of this added increase in serum creatinine relative to placebo is not known.
6.2 Postmarketing Experience
Additional adverse reactions have been identified during postapproval use of JANUVIA as monotherapy and/or in combination with other antihyperglycemic agents. Because these reactions are reported voluntarily from a population of uncertain size, it is generally not possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Hypersensitivity reactions including anaphylaxis, angioedema, rash, urticaria, cutaneous vasculitis, and exfoliative skin conditions including Stevens-Johnson syndrome [see Warnings and Precautions (5.5)]; hepatic enzyme elevations; acute pancreatitis, including fatal and non-fatal hemorrhagic and necrotizing pancreatitis [see Indications and Usage (1.2); Warnings and Precautions (5.1)]; worsening renal function, including acute renal failure (sometimes requiring dialysis) [see Warnings and Precautions (5.3)]; severe and disabling arthralgia [see Warnings and Precautions (5.6)]; bullous pemphigoid [see Warnings and Precautions (5.7)]; constipation; vomiting; headache; myalgia; pain in extremity; back pain; pruritus; mouth ulceration; stomatitis; rhabdomyolysis.
-
7 DRUG INTERACTIONS
7.1 Digoxin
There was a slight increase in the area under the curve (AUC, 11%) and mean peak drug concentration (Cmax, 18%) of digoxin with the coadministration of 100 mg sitagliptin for 10 days. Patients receiving digoxin should be monitored appropriately. No dosage adjustment of digoxin or JANUVIA is recommended.
7.2 Insulin Secretagogues or Insulin
Coadministration of JANUVIA with an insulin secretagogue (e.g., sulfonylurea) or insulin may require lower doses of the insulin secretagogue or insulin to reduce the risk of hypoglycemia. [See Warnings and Precautions (5.4).]
-
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Pregnancy Exposure Registry
There is a pregnancy exposure registry that monitors pregnancy outcomes in women exposed to JANUVIA during pregnancy. Health care providers are encouraged to report any prenatal exposure to JANUVIA by calling the Pregnancy Registry at 1-800-986-8999.
Risk Summary
The limited available data with JANUVIA in pregnant women are not sufficient to inform a drug-associated risk for major birth defects and miscarriage. There are risks to the mother and fetus associated with poorly controlled diabetes in pregnancy [see Clinical Considerations]. No adverse developmental effects were observed when sitagliptin was administered to pregnant rats and rabbits during organogenesis at oral doses up to 30-times and 20-times, respectively, the 100 mg clinical dose, based on AUC [see Data].
The estimated background risk of major birth defects is 6-10% in women with pre-gestational diabetes with a Hemoglobin A1c >7% and has been reported to be as high as 20-25% in women with a Hemoglobin A1c >10%. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2-4% and 15-20%, respectively.
Clinical Considerations
Disease-Associated Maternal and/or Embryo/Fetal Risk
Poorly controlled diabetes in pregnancy increases the maternal risk for diabetic ketoacidosis, pre-eclampsia, spontaneous abortions, preterm delivery, and delivery complications. Poorly controlled diabetes increases the fetal risk for major birth defects, still birth, and macrosomia related morbidity.
Data
Animal Data
In embryo-fetal development studies, sitagliptin administered to pregnant rats and rabbits during organogenesis (gestation day 6 to 20) did not adversely affect developmental outcomes at oral doses up to 250 mg/kg (30-times the 100 mg clinical dose) and 125 mg/kg (20-times the 100 mg clinical dose), respectively, based on AUC. Higher doses in rats associated with maternal toxicity increased the incidence of rib malformations in offspring at 1000 mg/kg, or approximately 100-times the clinical dose, based on AUC. Placental transfer of sitagliptin was observed in pregnant rats and rabbits.
Sitagliptin administered to female rats from gestation day 6 to lactation day 21 caused no functional or behavioral toxicity in offspring of rats at doses up to 1000 mg/kg.
8.2 Lactation
Risk Summary
There is no information regarding the presence of JANUVIA in human milk, the effects on the breastfed infant, or the effects on milk production. Sitagliptin is present in rat milk and therefore possibly present in human milk [see Data]. The developmental and health benefits of breastfeeding should be considered along with the mother's clinical need for JANUVIA and any potential adverse effects on the breastfed infant from JANUVIA or from the underlying maternal condition.
8.4 Pediatric Use
Safety and effectiveness of JANUVIA in pediatric patients under 18 years of age have not been established.
8.5 Geriatric Use
Of the total number of subjects (N=3884) in pre-approval clinical safety and efficacy studies of JANUVIA, 725 patients were 65 years and over, while 61 patients were 75 years and over. No overall differences in safety or effectiveness were observed between subjects 65 years and over and younger subjects. While this and other reported clinical experience have not identified differences in responses between the elderly and younger patients, greater sensitivity of some older individuals cannot be ruled out.
Because sitagliptin is substantially excreted by the kidney, and because aging can be associated with reduced renal function, renal function should be assessed more frequently in elderly patients [see Warnings and Precautions (5.3); Clinical Pharmacology (12.3)].
8.6 Renal Impairment
Sitagliptin is excreted by the kidney, and sitagliptin exposure is increased in patients with renal impairment. Lower dosages are recommended in patients with eGFR less than 45 mL/min/1.73 m2 (moderate and severe renal impairment, as well as in ESRD patients requiring dialysis). [See Dosage and Administration (2.2); Clinical Pharmacology (12.3).]
-
10 OVERDOSAGE
In the event of an overdose with JANUVIA, contact the Poison Control Center.
In the event of an overdose, it is reasonable to employ supportive measures, e.g., remove unabsorbed material from the gastrointestinal tract, employ clinical monitoring (including obtaining an electrocardiogram), and institute supportive therapy as dictated by the patient's clinical status.
Sitagliptin is modestly dialyzable. In clinical studies, approximately 13.5% of the dose was removed over a 3- to 4-hour hemodialysis session. Prolonged hemodialysis may be considered if clinically appropriate. It is not known if sitagliptin is dialyzable by peritoneal dialysis.
-
11 DESCRIPTION
JANUVIA Tablets contain sitagliptin phosphate, an orally-active inhibitor of the dipeptidyl peptidase-4 (DPP-4) enzyme.
Sitagliptin phosphate monohydrate is described chemically as 7-[(3R)-3-amino-1-oxo-4-(2,4,5-trifluorophenyl)butyl]-5,6,7,8-tetrahydro-3-(trifluoromethyl)-1,2,4-triazolo[4,3-a]pyrazine phosphate (1:1) monohydrate.
The empirical formula is C16H15F6N5OH3PO4H2O and the molecular weight is 523.32. The structural formula is:
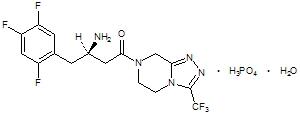
Sitagliptin phosphate monohydrate is a white to off-white, crystalline, non-hygroscopic powder. It is soluble in water and N,N-dimethyl formamide; slightly soluble in methanol; very slightly soluble in ethanol, acetone, and acetonitrile; and insoluble in isopropanol and isopropyl acetate.
Each film-coated tablet of JANUVIA contains 32.13, 64.25, or 128.5 mg of sitagliptin phosphate monohydrate, which is equivalent to 25, 50, or 100 mg, respectively, of free base and the following inactive ingredients: microcrystalline cellulose, anhydrous dibasic calcium phosphate, croscarmellose sodium, magnesium stearate, and sodium stearyl fumarate. In addition, the film coating contains the following inactive ingredients: polyvinyl alcohol, polyethylene glycol, talc, titanium dioxide, red iron oxide, and yellow iron oxide.
-
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Sitagliptin is a DPP-4 inhibitor, which is believed to exert its actions in patients with type 2 diabetes mellitus by slowing the inactivation of incretin hormones. Concentrations of the active intact hormones are increased by sitagliptin, thereby increasing and prolonging the action of these hormones. Incretin hormones, including glucagon-like peptide-1 (GLP-1) and glucose-dependent insulinotropic polypeptide (GIP), are released by the intestine throughout the day, and levels are increased in response to a meal. These hormones are rapidly inactivated by the enzyme, DPP-4. The incretins are part of an endogenous system involved in the physiologic regulation of glucose homeostasis. When blood glucose concentrations are normal or elevated, GLP-1 and GIP increase insulin synthesis and release from pancreatic beta cells by intracellular signaling pathways involving cyclic AMP. GLP-1 also lowers glucagon secretion from pancreatic alpha cells, leading to reduced hepatic glucose production. By increasing and prolonging active incretin levels, sitagliptin increases insulin release and decreases glucagon levels in the circulation in a glucose-dependent manner. Sitagliptin demonstrates selectivity for DPP-4 and does not inhibit DPP-8 or DPP-9 activity in vitro at concentrations approximating those from therapeutic doses.
12.2 Pharmacodynamics
General
In patients with type 2 diabetes mellitus, administration of sitagliptin led to inhibition of DPP-4 enzyme activity for a 24-hour period. After an oral glucose load or a meal, this DPP-4 inhibition resulted in a 2- to 3-fold increase in circulating levels of active GLP-1 and GIP, decreased glucagon concentrations, and increased responsiveness of insulin release to glucose, resulting in higher C-peptide and insulin concentrations. The rise in insulin with the decrease in glucagon was associated with lower fasting glucose concentrations and reduced glucose excursion following an oral glucose load or a meal.
In studies with healthy subjects, sitagliptin did not lower blood glucose or cause hypoglycemia.
Sitagliptin and Metformin hydrochloride Coadministration
In a two-day study in healthy subjects, sitagliptin alone increased active GLP-1 concentrations, whereas metformin alone increased active and total GLP-1 concentrations to similar extents. Coadministration of sitagliptin and metformin had an additive effect on active GLP-1 concentrations. Sitagliptin, but not metformin, increased active GIP concentrations. It is unclear how these findings relate to changes in glycemic control in patients with type 2 diabetes mellitus.
Cardiac Electrophysiology
In a randomized, placebo-controlled crossover study, 79 healthy subjects were administered a single oral dose of sitagliptin 100 mg, sitagliptin 800 mg (8 times the recommended dose), and placebo. At the recommended dose of 100 mg, there was no effect on the QTc interval obtained at the peak plasma concentration, or at any other time during the study. Following the 800 mg dose, the maximum increase in the placebo-corrected mean change in QTc from baseline was observed at 3 hours postdose and was 8.0 msec. This increase is not considered to be clinically significant. At the 800 mg dose, peak sitagliptin plasma concentrations were approximately 11 times higher than the peak concentrations following a 100-mg dose.
In patients with type 2 diabetes mellitus administered sitagliptin 100 mg (N=81) or sitagliptin 200 mg (N=63) daily, there were no meaningful changes in QTc interval based on ECG data obtained at the time of expected peak plasma concentration.
12.3 Pharmacokinetics
The pharmacokinetics of sitagliptin have been extensively characterized in healthy subjects and patients with type 2 diabetes mellitus. Following a single oral 100-mg dose to healthy volunteers, mean plasma AUC of sitagliptin was 8.52 μMhr, Cmax was 950 nM, and apparent terminal half-life (t1/2) was 12.4 hours. Plasma AUC of sitagliptin increased in a dose-proportional manner and increased approximately 14% following 100 mg doses at steady-state compared to the first dose. The intra-subject and inter-subject coefficients of variation for sitagliptin AUC were small (5.8% and 15.1%). The pharmacokinetics of sitagliptin was generally similar in healthy subjects and in patients with type 2 diabetes mellitus.
Absorption
After oral administration of a 100 mg dose to healthy subjects, sitagliptin was rapidly absorbed with peak plasma concentrations (median Tmax) occurring 1 to 4 hours postdose. The absolute bioavailability of sitagliptin is approximately 87%.
Effect of Food
Coadministration of a high-fat meal with sitagliptin had no effect on the pharmacokinetics of sitagliptin.
Distribution
The mean volume of distribution at steady state following a single 100-mg intravenous dose of sitagliptin to healthy subjects is approximately 198 liters. The fraction of sitagliptin reversibly bound to plasma proteins is low (38%).
Elimination
Approximately 79% of sitagliptin is excreted unchanged in the urine with metabolism being a minor pathway of elimination. The apparent terminal t1/2 following a 100 mg oral dose of sitagliptin was approximately 12.4 hours and renal clearance was approximately 350 mL/min.
Metabolism
Following a [14C]sitagliptin oral dose, approximately 16% of the radioactivity was excreted as metabolites of sitagliptin. Six metabolites were detected at trace levels and are not expected to contribute to the plasma DPP-4 inhibitory activity of sitagliptin. In vitro studies indicated that the primary enzyme responsible for the limited metabolism of sitagliptin was CYP3A4, with contribution from CYP2C8.
Excretion
Following administration of an oral [14C]sitagliptin dose to healthy subjects, approximately 100% of the administered radioactivity was eliminated in feces (13%) or urine (87%) within one week of dosing.
Elimination of sitagliptin occurs primarily via renal excretion and involves active tubular secretion. Sitagliptin is a substrate for human organic anion transporter-3 (hOAT-3), which may be involved in the renal elimination of sitagliptin. The clinical relevance of hOAT-3 in sitagliptin transport has not been established. Sitagliptin is also a substrate of P-glycoprotein (P-gp), which may also be involved in mediating the renal elimination of sitagliptin. However, cyclosporine, a P-gp inhibitor, did not reduce the renal clearance of sitagliptin.
Specific Populations
Patients with Renal Impairment
An approximately 2-fold increase in the plasma AUC of sitagliptin was observed in patients with moderate renal impairment with eGFR of 30 to less than 45 mL/min/1.73 m2, and an approximately 4-fold increase was observed in patients with severe renal impairment, including patients with ESRD on hemodialysis, as compared to normal healthy control subjects.
Patients with Hepatic Impairment
In patients with moderate hepatic impairment (Child-Pugh score 7 to 9), mean AUC and Cmax of sitagliptin increased approximately 21% and 13%, respectively, compared to healthy matched controls following administration of a single 100-mg dose of sitagliptin. These differences are not considered to be clinically meaningful.
There is no clinical experience in patients with severe hepatic impairment (Child-Pugh score >9).
Effects of Age, Body Mass Index (BMI), Gender, and Race
Based on a population pharmacokinetic analysis or a composite analysis of available pharmacokinetic data, BMI, gender, and race do not have a clinically meaningful effect on the pharmacokinetics of sitagliptin. When the effects of age on renal function are taken into account, age alone did not have a clinically meaningful impact on the pharmacokinetics of sitagliptin based on a population pharmacokinetic analysis. Elderly subjects (65 to 80 years) had approximately 19% higher plasma concentrations of sitagliptin compared to younger subjects.
Drug Interaction Studies
In Vitro Assessment of Drug Interactions
Sitagliptin is not an inhibitor of CYP isozymes CYP3A4, 2C8, 2C9, 2D6, 1A2, 2C19 or 2B6, and is not an inducer of CYP3A4. Sitagliptin is a P-gp substrate, but does not inhibit P-gp mediated transport of digoxin. Based on these results, sitagliptin is considered unlikely to cause interactions with other drugs that utilize these pathways.
Sitagliptin is not extensively bound to plasma proteins. Therefore, the propensity of sitagliptin to be involved in clinically meaningful drug-drug interactions mediated by plasma protein binding displacement is very low.
In Vivo Assessment of Drug Interactions
Effects of Sitagliptin on Other Drugs
In clinical studies, sitagliptin did not meaningfully alter the pharmacokinetics of metformin, glyburide, simvastatin, rosiglitazone, digoxin, warfarin, or an oral contraceptive (ethinyl estradiol and norethindrone) (Table 4), providing in vivo evidence of a low propensity for causing drug interactions with substrates of CYP3A4, CYP2C8, CYP2C9, P-gp, and organic cationic transporter (OCT).
Table 4: Effect of Sitagliptin on Systemic Exposure of Coadministered Drugs Coadministered Drug Dose of Coadministered Drug* Dose of Sitagliptin* Geometric Mean Ratio
(ratio with/without sitagliptin)
No Effect = 1.00AUC† Cmax - * All doses administered as single dose unless otherwise specified.
- † AUC is reported as AUC0-∞ unless otherwise specified.
- ‡ Multiple dose.
- § AUC0-24hr.
- ¶ AUC0-last.
- # AUC0-12hr.
Digoxin 0.25 mg‡ once daily for 10 days 100 mg‡ once daily for 10 days Digoxin 1.11§ 1.18 Glyburide 1.25 mg 200 mg‡ once daily for 6 days Glyburide 1.09 1.01 Simvastatin 20 mg 200 mg‡ once daily for 5 days Simvastatin 0.85¶ 0.80 Simvastatin Acid 1.12¶ 1.06 Rosiglitazone 4 mg 200 mg‡ once daily for 5 days Rosiglitazone 0.98 0.99 Warfarin 30 mg single dose on day 5 200 mg‡ once daily for 11 days S(-) Warfarin 0.95 0.89 R(+) Warfarin 0.99 0.89 Ethinyl estradiol and norethindrone 21 days once daily of 35 µg ethinyl estradiol with norethindrone 0.5 mg × 7 days, 0.75 mg × 7 days, 1.0 mg × 7 days 200 mg‡ once daily for 21 days Ethinyl estradiol 0.99 0.97 Norethindrone 1.03 0.98 Metformin 1000 mg‡ twice daily for 14 days 50 mg‡ twice daily for 7 days Metformin 1.02# 0.97 Effects of Other Drugs on Sitagliptin
Clinical data described below suggest that sitagliptin is not susceptible to clinically meaningful interactions by coadministered medications (Table 5).
Table 5: Effect of Coadministered Drugs on Systemic Exposure of Sitagliptin Coadministered Drug Dose of Coadministered Drug* Dose of Sitagliptin* Geometric Mean Ratio
(ratio with/without coadministered drug)
No Effect = 1.00AUC† Cmax - * All doses administered as single dose unless otherwise specified.
- † AUC is reported as AUC0-∞ unless otherwise specified.
- ‡ Multiple dose.
- § AUC0-12hr.
Cyclosporine 600 mg once daily 100 mg once daily Sitagliptin 1.29 1.68 Metformin 1000 mg‡ twice daily for 14 days 50 mg‡ twice daily for 7 days Sitagliptin 1.02§ 1.05 -
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
A two-year carcinogenicity study was conducted in male and female rats given oral doses of sitagliptin of 50, 150, and 500 mg/kg/day. There was an increased incidence of combined liver adenoma/carcinoma in males and females and of liver carcinoma in females at 500 mg/kg. This dose results in exposures approximately 60 times the human exposure at the maximum recommended daily adult human dose (MRHD) of 100 mg/day based on AUC comparisons. Liver tumors were not observed at 150 mg/kg, approximately 20 times the human exposure at the MRHD. A two-year carcinogenicity study was conducted in male and female mice given oral doses of sitagliptin of 50, 125, 250, and 500 mg/kg/day. There was no increase in the incidence of tumors in any organ up to 500 mg/kg, approximately 70 times human exposure at the MRHD. Sitagliptin was not mutagenic or clastogenic with or without metabolic activation in the Ames bacterial mutagenicity assay, a Chinese hamster ovary (CHO) chromosome aberration assay, an in vitro cytogenetics assay in CHO, an in vitro rat hepatocyte DNA alkaline elution assay, and an in vivo micronucleus assay.
In rat fertility studies with oral gavage doses of 125, 250, and 1000 mg/kg, males were treated for 4 weeks prior to mating, during mating, up to scheduled termination (approximately 8 weeks total) and females were treated 2 weeks prior to mating through gestation day 7. No adverse effect on fertility was observed at 125 mg/kg (approximately 12 times human exposure at the MRHD of 100 mg/day based on AUC comparisons). At higher doses, nondose-related increased resorptions in females were observed (approximately 25 and 100 times human exposure at the MRHD based on AUC comparison).
-
14 CLINICAL STUDIES
There were approximately 5200 patients with type 2 diabetes randomized in nine double-blind, placebo-controlled clinical safety and efficacy studies conducted to evaluate the effects of sitagliptin on glycemic control. In a pooled analysis of seven of these studies, the ethnic/racial distribution was approximately 59% white, 20% Hispanic, 10% Asian, 6% black, and 6% other groups. Patients had an overall mean age of approximately 55 years (range 18 to 87 years). In addition, an active (glipizide)-controlled study of 52-weeks duration was conducted in 1172 patients with type 2 diabetes who had inadequate glycemic control on metformin.
In patients with type 2 diabetes, treatment with JANUVIA produced clinically significant improvements in hemoglobin A1C, fasting plasma glucose (FPG) and 2-hour post-prandial glucose (PPG) compared to placebo.
14.1 Monotherapy
A total of 1262 patients with type 2 diabetes participated in two double-blind, placebo-controlled studies, one of 18-week and another of 24-week duration, to evaluate the efficacy and safety of JANUVIA monotherapy. In both monotherapy studies, patients currently on an antihyperglycemic agent discontinued the agent, and underwent a diet, exercise, and drug washout period of about 7 weeks. Patients with inadequate glycemic control (A1C 7% to 10%) after the washout period were randomized after completing a 2-week single-blind placebo run-in period; patients not currently on antihyperglycemic agents (off therapy for at least 8 weeks) with inadequate glycemic control (A1C 7% to 10%) were randomized after completing the 2-week single-blind placebo run-in period. In the 18-week study, 521 patients were randomized to placebo, JANUVIA 100 mg, or JANUVIA 200 mg, and in the 24-week study 741 patients were randomized to placebo, JANUVIA 100 mg, or JANUVIA 200 mg. Patients who failed to meet specific glycemic goals during the studies were treated with metformin rescue, added on to placebo or JANUVIA.
Treatment with JANUVIA at 100 mg daily provided significant improvements in A1C, FPG, and 2-hour PPG compared to placebo (Table 6). In the 18-week study, 9% of patients receiving JANUVIA 100 mg and 17% who received placebo required rescue therapy. In the 24-week study, 9% of patients receiving JANUVIA 100 mg and 21% of patients receiving placebo required rescue therapy. The improvement in A1C compared to placebo was not affected by gender, age, race, prior antihyperglycemic therapy, or baseline BMI. As is typical for trials of agents to treat type 2 diabetes, the mean reduction in A1C with JANUVIA appears to be related to the degree of A1C elevation at baseline. In these 18- and 24-week studies, among patients who were not on an antihyperglycemic agent at study entry, the reductions from baseline in A1C were -0.7% and -0.8%, respectively, for those given JANUVIA, and -0.1% and -0.2%, respectively, for those given placebo. Overall, the 200 mg daily dose did not provide greater glycemic efficacy than the 100 mg daily dose. The effect of JANUVIA on lipid endpoints was similar to placebo. Body weight did not increase from baseline with JANUVIA therapy in either study, compared to a small reduction in patients given placebo.
Table 6: Glycemic Parameters in 18- and 24-Week Placebo-Controlled Studies of JANUVIA in Patients with Type 2 Diabetes* 18-Week Study 24-Week Study JANUVIA 100 mg Placebo JANUVIA 100 mg Placebo - * Intent-to-treat population using last observation on study prior to metformin rescue therapy.
- † Least squares means adjusted for prior antihyperglycemic therapy status and baseline value.
- ‡ p<0.001 compared to placebo.
- § Data not available.
A1C (%) N = 193 N = 103 N = 229 N = 244 Baseline (mean) 8.0 8.1 8.0 8.0 Change from baseline (adjusted mean†) -0.5 0.1 -0.6 0.2 Difference from placebo (adjusted mean†)
(95% CI)-0.6‡
(-0.8, -0.4)-0.8‡
(-1.0, -0.6)Patients (%) achieving A1C <7% 69 (36%) 16 (16%) 93 (41%) 41 (17%) FPG (mg/dL) N = 201 N = 107 N = 234 N = 247 Baseline (mean) 180 184 170 176 Change from baseline (adjusted mean†) -13 7 -12 5 Difference from placebo (adjusted mean†)
(95% CI)-20‡
(‑31, -9)-17‡
(‑24, -10)2-hour PPG (mg/dL) § § N = 201 N = 204 Baseline (mean) 257 271 Change from baseline (adjusted mean†) -49 -2 Difference from placebo (adjusted mean†)
(95% CI)-47‡
(-59, -34)Additional Monotherapy Study
A multinational, randomized, double-blind, placebo-controlled study was also conducted to assess the safety and tolerability of JANUVIA in 91 patients with type 2 diabetes and chronic renal insufficiency (creatinine clearance <50 mL/min). Patients with moderate renal insufficiency received 50 mg daily of JANUVIA and those with severe renal insufficiency or with ESRD on hemodialysis or peritoneal dialysis received 25 mg daily. In this study, the safety and tolerability of JANUVIA were generally similar to placebo. A small increase in serum creatinine was reported in patients with moderate renal insufficiency treated with JANUVIA relative to those on placebo. In addition, the reductions in A1C and FPG with JANUVIA compared to placebo were generally similar to those observed in other monotherapy studies. [See Clinical Pharmacology (12.3).]
14.2 Combination Therapy
Add-on Combination Therapy with Metformin
A total of 701 patients with type 2 diabetes participated in a 24-week, randomized, double-blind, placebo-controlled study designed to assess the efficacy of JANUVIA in combination with metformin. Patients already on metformin (N=431) at a dose of at least 1500 mg per day were randomized after completing a 2-week single-blind placebo run-in period. Patients on metformin and another antihyperglycemic agent (N=229) and patients not on any antihyperglycemic agents (off therapy for at least 8 weeks, N=41) were randomized after a run-in period of approximately 10 weeks on metformin (at a dose of at least 1500 mg per day) in monotherapy. Patients with inadequate glycemic control (A1C 7% to 10%) were randomized to the addition of either 100 mg of JANUVIA or placebo, administered once daily. Patients who failed to meet specific glycemic goals during the studies were treated with pioglitazone rescue.
In combination with metformin, JANUVIA provided significant improvements in A1C, FPG, and 2-hour PPG compared to placebo with metformin (Table 7). Rescue glycemic therapy was used in 5% of patients treated with JANUVIA 100 mg and 14% of patients treated with placebo. A similar decrease in body weight was observed for both treatment groups.
Table 7: Glycemic Parameters at Final Visit (24-Week Study) for JANUVIA in Add-on Combination Therapy with Metformin* JANUVIA 100 mg + Metformin Placebo + Metformin - * Intent-to-treat population using last observation on study prior to pioglitazone rescue therapy.
- † Least squares means adjusted for prior antihyperglycemic therapy and baseline value.
- ‡ p<0.001 compared to placebo + metformin.
A1C (%) N = 453 N = 224 Baseline (mean) 8.0 8.0 Change from baseline (adjusted mean†) -0.7 -0.0 Difference from placebo + metformin (adjusted mean†)
(95% CI)-0.7‡
(-0.8, -0.5)Patients (%) achieving A1C <7% 213 (47%) 41 (18%) FPG (mg/dL) N = 454 N = 226 Baseline (mean) 170 174 Change from baseline (adjusted mean†) -17 9 Difference from placebo + metformin (adjusted mean†)
(95% CI)-25‡
(-31, -20)2-hour PPG (mg/dL) N = 387 N = 182 Baseline (mean) 275 272 Change from baseline (adjusted mean†) -62 -11 Difference from placebo + metformin (adjusted mean†)
(95% CI)-51‡
(-61, -41)Initial Combination Therapy with Metformin
A total of 1091 patients with type 2 diabetes and inadequate glycemic control on diet and exercise participated in a 24-week, randomized, double-blind, placebo-controlled factorial study designed to assess the efficacy of sitagliptin as initial therapy in combination with metformin. Patients on an antihyperglycemic agent (N=541) discontinued the agent, and underwent a diet, exercise, and drug washout period of up to 12 weeks duration. After the washout period, patients with inadequate glycemic control (A1C 7.5% to 11%) were randomized after completing a 2-week single-blind placebo run-in period. Patients not on antihyperglycemic agents at study entry (N=550) with inadequate glycemic control (A1C 7.5% to 11%) immediately entered the 2-week single-blind placebo run-in period and then were randomized. Approximately equal numbers of patients were randomized to receive initial therapy with placebo, 100 mg of JANUVIA once daily, 500 mg or 1000 mg of metformin twice daily, or 50 mg of sitagliptin twice daily in combination with 500 mg or 1000 mg of metformin twice daily. Patients who failed to meet specific glycemic goals during the study were treated with glyburide (glibenclamide) rescue.
Initial therapy with the combination of JANUVIA and metformin provided significant improvements in A1C, FPG, and 2-hour PPG compared to placebo, to metformin alone, and to JANUVIA alone (Table 8, Figure 1). Mean reductions from baseline in A1C were generally greater for patients with higher baseline A1C values. For patients not on an antihyperglycemic agent at study entry, mean reductions from baseline in A1C were: JANUVIA 100 mg once daily, -1.1%; metformin 500 mg bid, -1.1%; metformin 1000 mg bid, -1.2%; sitagliptin 50 mg bid with metformin 500 mg bid, -1.6%; sitagliptin 50 mg bid with metformin 1000 mg bid, -1.9%; and for patients receiving placebo, -0.2%. Lipid effects were generally neutral. The decrease in body weight in the groups given sitagliptin in combination with metformin was similar to that in the groups given metformin alone or placebo.
Table 8: Glycemic Parameters at Final Visit (24-Week Study) for Sitagliptin and Metformin, Alone and in Combination as Initial Therapy* Placebo
Sitagliptin
(JANUVIA)
100 mg QD
Metformin
500 mg bidMetformin
1000 mg bidSitagliptin
50 mg bid +
Metformin
500 mg bidSitagliptin
50 mg bid +
Metformin
1000 mg bid- * Intent-to-treat population using last observation on study prior to glyburide (glibenclamide) rescue therapy.
- † Least squares means adjusted for prior antihyperglycemic therapy status and baseline value.
- ‡ p<0.001 compared to placebo.
A1C (%) N = 165 N = 175 N = 178 N = 177 N = 183 N = 178 Baseline (mean) 8.7 8.9 8.9 8.7 8.8 8.8 Change from baseline (adjusted mean†) 0.2 -0.7 -0.8 -1.1 -1.4 -1.9 Difference from placebo (adjusted mean†) (95% CI) -0.8‡
(-1.1, -0.6)-1.0‡
(-1.2, -0.8)-1.3‡
(-1.5, -1.1)-1.6‡
(-1.8, -1.3)-2.1‡
(-2.3, -1.8)Patients (%) achieving A1C <7% 15 (9%) 35 (20%) 41 (23%) 68 (38%) 79 (43%) 118 (66%) % Patients receiving rescue medication 32 21 17 12 8 2 FPG (mg/dL) N = 169 N = 178 N = 179 N = 179 N = 183 N = 180 Baseline (mean) 196 201 205 197 204 197 Change from baseline (adjusted mean†) 6 -17 -27 -29 -47 -64 Difference from placebo (adjusted mean†) (95% CI) -23‡
(-33, -14)-33‡
(-43, -24)-35‡
(-45, -26)-53‡
(-62, -43)-70‡
(-79, -60)2-hour PPG (mg/dL) N = 129 N = 136 N = 141 N = 138 N = 147 N = 152 Baseline (mean) 277 285 293 283 292 287 Change from baseline (adjusted mean†) 0 -52 -53 -78 -93 -117 Difference from placebo (adjusted mean†) (95% CI) -52‡
(-67, -37)-54‡
(-69, -39)-78‡
(-93, -63)-93‡
(-107, -78)-117‡
(-131, -102)Figure 1: Mean Change from Baseline for A1C (%) over 24 Weeks with Sitagliptin and Metformin, Alone and in Combination as Initial Therapy in Patients with Type 2 Diabetes* - * All Patients Treated Population: least squares means adjusted for prior antihyperglycemic therapy and baseline value.
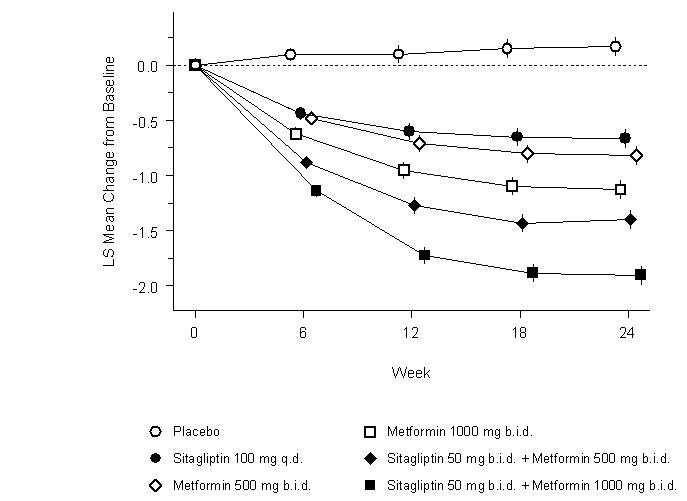
Initial combination therapy or maintenance of combination therapy may not be appropriate for all patients. These management options are left to the discretion of the health care provider.
Active-Controlled Study vs Glipizide in Combination with Metformin
The efficacy of JANUVIA was evaluated in a 52-week, double-blind, glipizide-controlled noninferiority trial in patients with type 2 diabetes. Patients not on treatment or on other antihyperglycemic agents entered a run-in treatment period of up to 12 weeks duration with metformin monotherapy (dose of ≥1500 mg per day) which included washout of medications other than metformin, if applicable. After the run-in period, those with inadequate glycemic control (A1C 6.5% to 10%) were randomized 1:1 to the addition of JANUVIA 100 mg once daily or glipizide for 52 weeks. Patients receiving glipizide were given an initial dosage of 5 mg/day and then electively titrated over the next 18 weeks to a maximum dosage of 20 mg/day as needed to optimize glycemic control. Thereafter, the glipizide dose was to be kept constant, except for down-titration to prevent hypoglycemia. The mean dose of glipizide after the titration period was 10 mg.
After 52 weeks, JANUVIA and glipizide had similar mean reductions from baseline in A1C in the intent-to-treat analysis (Table 9). These results were consistent with the per protocol analysis (Figure 2). A conclusion in favor of the non-inferiority of JANUVIA to glipizide may be limited to patients with baseline A1C comparable to those included in the study (over 70% of patients had baseline A1C <8% and over 90% had A1C <9%).
Table 9: Glycemic Parameters in a 52-Week Study Comparing JANUVIA to Glipizide as Add-On Therapy in Patients Inadequately Controlled on Metformin (Intent-to-Treat Population)* JANUVIA 100 mg Glipizide - * The intent-to-treat analysis used the patients' last observation in the study prior to discontinuation.
- † Least squares means adjusted for prior antihyperglycemic therapy status and baseline A1C value.
A1C (%) N = 576 N = 559 Baseline (mean) 7.7 7.6 Change from baseline (adjusted mean†) -0.5 -0.6 FPG (mg/dL) N = 583 N = 568 Baseline (mean) 166 164 Change from baseline (adjusted mean†) -8 -8 Figure 2: Mean Change from Baseline for A1C (%) Over 52 Weeks in a Study Comparing JANUVIA to Glipizide as Add-On Therapy in Patients Inadequately Controlled on Metformin (Per Protocol Population)* - * The per protocol population (mean baseline A1C of 7.5%) included patients without major protocol violations who had observations at baseline and at Week 52.
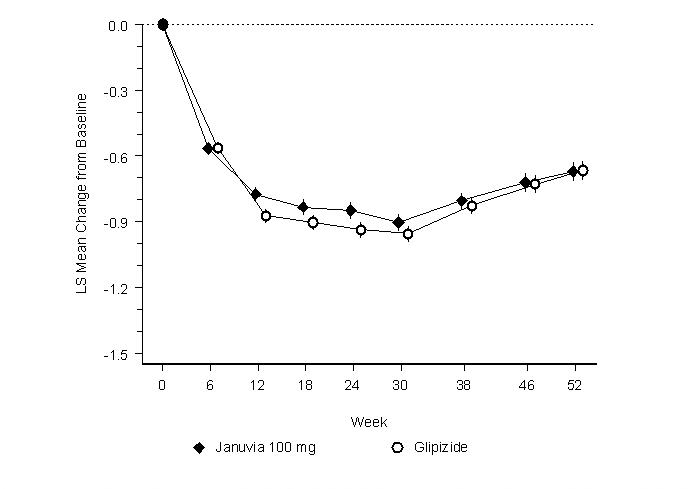
The incidence of hypoglycemia in the JANUVIA group (4.9%) was significantly (p<0.001) lower than that in the glipizide group (32.0%). Patients treated with JANUVIA exhibited a significant mean decrease from baseline in body weight compared to a significant weight gain in patients administered glipizide (-1.5 kg vs +1.1 kg).
Add-on Combination Therapy with Pioglitazone
A total of 353 patients with type 2 diabetes participated in a 24-week, randomized, double-blind, placebo-controlled study designed to assess the efficacy of JANUVIA in combination with pioglitazone. Patients on any oral antihyperglycemic agent in monotherapy (N=212) or on a PPARγ agent in combination therapy (N=106) or not on an antihyperglycemic agent (off therapy for at least 8 weeks, N=34) were switched to monotherapy with pioglitazone (at a dose of 30-45 mg per day), and completed a run-in period of approximately 12 weeks in duration. After the run-in period on pioglitazone monotherapy, patients with inadequate glycemic control (A1C 7% to 10%) were randomized to the addition of either 100 mg of JANUVIA or placebo, administered once daily. Patients who failed to meet specific glycemic goals during the studies were treated with metformin rescue. Glycemic endpoints measured were A1C and fasting glucose.
In combination with pioglitazone, JANUVIA provided significant improvements in A1C and FPG compared to placebo with pioglitazone (Table 10). Rescue therapy was used in 7% of patients treated with JANUVIA 100 mg and 14% of patients treated with placebo. There was no significant difference between JANUVIA and placebo in body weight change.
Table 10: Glycemic Parameters at Final Visit (24-Week Study) for JANUVIA in Add-on Combination Therapy with Pioglitazone* JANUVIA 100 mg + Pioglitazone Placebo + Pioglitazone - * Intent-to-treat population using last observation on study prior to metformin rescue therapy.
- † Least squares means adjusted for prior antihyperglycemic therapy status and baseline value.
- ‡ p<0.001 compared to placebo + pioglitazone.
A1C (%) N = 163 N = 174 Baseline (mean) 8.1 8.0 Change from baseline (adjusted mean†) -0.9 -0.2 Difference from placebo + pioglitazone (adjusted mean†)
(95% CI)-0.7‡
(-0.9, -0.5)Patients (%) achieving A1C <7% 74 (45%) 40 (23%) FPG (mg/dL) N = 163 N = 174 Baseline (mean) 168 166 Change from baseline (adjusted mean†) -17 1 Difference from placebo + pioglitazone (adjusted mean†)
(95% CI)-18‡
(-24, -11)Initial Combination Therapy with Pioglitazone
A total of 520 patients with type 2 diabetes and inadequate glycemic control on diet and exercise participated in a 24-week, randomized, double-blind study designed to assess the efficacy of JANUVIA as initial therapy in combination with pioglitazone. Patients not on antihyperglycemic agents at study entry (<4 weeks cumulative therapy over the past 2 years, and with no treatment over the prior 4 months) with inadequate glycemic control (A1C 8% to 12%) immediately entered the 2-week single-blind placebo run-in period and then were randomized. Approximately equal numbers of patients were randomized to receive initial therapy with 100 mg of JANUVIA in combination with 30 mg of pioglitazone once daily or 30 mg of pioglitazone once daily as monotherapy. There was no glycemic rescue therapy in this study.
Initial therapy with the combination of JANUVIA and pioglitazone provided significant improvements in A1C, FPG, and 2-hour PPG compared to pioglitazone monotherapy (Table 11). The improvement in A1C was generally consistent across subgroups defined by gender, age, race, baseline BMI, baseline A1C, or duration of disease. In this study, patients treated with JANUVIA in combination with pioglitazone had a mean increase in body weight of 1.1 kg compared to pioglitazone alone (3.0 kg vs. 1.9 kg). Lipid effects were generally neutral.
Table 11: Glycemic Parameters at Final Visit (24-Week Study) for JANUVIA in Combination with Pioglitazone as Initial Therapy* JANUVIA 100 mg + Pioglitazone Pioglitazone - * Intent-to-treat population using last observation on study.
- † Least squares means adjusted for baseline value.
- ‡ p<0.001 compared to placebo + pioglitazone.
A1C (%) N = 251 N = 246 Baseline (mean) 9.5 9.4 Change from baseline (adjusted mean†) -2.4 -1.5 Difference from pioglitazone (adjusted mean†) (95% CI) -0.9‡
(-1.1, -0.7)Patients (%) achieving A1C <7% 151 (60%) 68 (28%) FPG (mg/dL) N = 256 N = 253 Baseline (mean) 203 201 Change from baseline (adjusted mean†) -63 -40 Difference from pioglitazone (adjusted mean†) (95% CI) -23‡
(-30, -15)2-hour PPG (mg/dL) N = 216 N = 211 Baseline (mean) 283 284 Change from baseline (adjusted mean†) -114 -69 Difference from pioglitazone (adjusted mean†) (95% CI) -45‡
(-57, -32)Add-on Combination Therapy with Metformin and Rosiglitazone
A total of 278 patients with type 2 diabetes participated in a 54-week, randomized, double-blind, placebo-controlled study designed to assess the efficacy of JANUVIA in combination with metformin and rosiglitazone. Patients on dual therapy with metformin ≥1500 mg/day and rosiglitazone ≥4 mg/day or with metformin ≥1500 mg/day and pioglitazone ≥30 mg/day (switched to rosiglitazone ≥4 mg/day) entered a dose-stable run-in period of 6 weeks. Patients on other dual therapy were switched to metformin ≥1500 mg/day and rosiglitazone ≥4 mg/day in a dose titration/stabilization run-in period of up to 20 weeks in duration. After the run-in period, patients with inadequate glycemic control (A1C 7.5% to 11%) were randomized 2:1 to the addition of either 100 mg of JANUVIA or placebo, administered once daily. Patients who failed to meet specific glycemic goals during the study were treated with glipizide (or other sulfonylurea) rescue. The primary time point for evaluation of glycemic parameters was Week 18.
In combination with metformin and rosiglitazone, JANUVIA provided significant improvements in A1C, FPG, and 2-hour PPG compared to placebo with metformin and rosiglitazone (Table 12) at Week 18. At Week 54, mean reduction in A1C was -1.0% for patients treated with JANUVIA and -0.3% for patients treated with placebo in an analysis based on the intent-to-treat population. Rescue therapy was used in 18% of patients treated with JANUVIA 100 mg and 40% of patients treated with placebo. There was no significant difference between JANUVIA and placebo in body weight change.
Table 12: Glycemic Parameters at Week 18 for JANUVIA in Add-on Combination Therapy with Metformin and Rosiglitazone* JANUVIA 100 mg + Metformin + Rosiglitazone Placebo +
Metformin + Rosiglitazone- * Intent-to-treat population using last observation on study prior to glipizide (or other sulfonylurea) rescue therapy.
- † Least squares means adjusted for prior antihyperglycemic therapy status and baseline value.
- ‡ p<0.001 compared to placebo + metformin + rosiglitazone.
A1C (%) N = 176 N = 93 Baseline (mean) 8.8 8.7 Change from baseline (adjusted mean†) -1.0 -0.4 Difference from placebo + rosiglitazone + metformin (adjusted mean†) (95% CI) -0.7‡
(-0.9, -0.4)Patients (%) achieving A1C <7% 39 (22%) 9 (10%) FPG (mg/dL) N = 179 N = 94 Baseline (mean) 181 182 Change from baseline (adjusted mean†) -30 -11 Difference from placebo + rosiglitazone + metformin (adjusted mean†) (95% CI) -18‡
(-26, -10)2-hour PPG (mg/dL) N = 152 N = 80 Baseline (mean) 256 248 Change from baseline (adjusted mean†) -59 -21 Difference from placebo + rosiglitazone + metformin (adjusted mean†) (95% CI) -39‡
(-51, -26)Add-on Combination Therapy with Glimepiride, with or without Metformin
A total of 441 patients with type 2 diabetes participated in a 24-week, randomized, double-blind, placebo-controlled study designed to assess the efficacy of JANUVIA in combination with glimepiride, with or without metformin. Patients entered a run-in treatment period on glimepiride (≥4 mg per day) alone or glimepiride in combination with metformin (≥1500 mg per day). After a dose-titration and dose-stable run-in period of up to 16 weeks and a 2-week placebo run-in period, patients with inadequate glycemic control (A1C 7.5% to 10.5%) were randomized to the addition of either 100 mg of JANUVIA or placebo, administered once daily. Patients who failed to meet specific glycemic goals during the studies were treated with pioglitazone rescue.
In combination with glimepiride, with or without metformin, JANUVIA provided significant improvements in A1C and FPG compared to placebo (Table 13). In the entire study population (patients on JANUVIA in combination with glimepiride and patients on JANUVIA in combination with glimepiride and metformin), a mean reduction from baseline relative to placebo in A1C of -0.7% and in FPG of -20 mg/dL was seen. Rescue therapy was used in 12% of patients treated with JANUVIA 100 mg and 27% of patients treated with placebo. In this study, patients treated with JANUVIA had a mean increase in body weight of 1.1 kg vs. placebo (+0.8 kg vs. -0.4 kg). In addition, there was an increased rate of hypoglycemia. [See Warnings and Precautions (5.4); Adverse Reactions (6.1).]
Table 13: Glycemic Parameters at Final Visit (24-Week Study) for JANUVIA as Add-On Combination Therapy with Glimepiride, with or without Metformin* JANUVIA 100 mg
+ GlimepiridePlacebo +
GlimepirideJANUVIA 100 mg
+ Glimepiride
+ MetforminPlacebo
+ Glimepiride
+ Metformin- * Intent-to-treat population using last observation on study prior to pioglitazone rescue therapy.
- † Least squares means adjusted for prior antihyperglycemic therapy status and baseline value.
- ‡ p<0.001 compared to placebo.
- § p<0.01 compared to placebo.
A1C (%) N = 102 N = 103 N = 115 N = 105 Baseline (mean) 8.4 8.5 8.3 8.3 Change from baseline (adjusted mean†) -0.3 0.3 -0.6 0.3 Difference from placebo (adjusted mean†)
(95% CI)-0.6‡
(-0.8, -0.3)-0.9‡
(-1.1, -0.7)Patients (%) achieving A1C <7% 11 (11%) 9 (9%) 26 (23%) 1 (1%) FPG (mg/dL) N = 104 N = 104 N = 115 N = 109 Baseline (mean) 183 185 179 179 Change from baseline (adjusted mean†) -1 18 -8 13 Difference from placebo (adjusted mean†)
(95% CI)-19§
(-32, -7)-21‡
(-32, -10)Add-on Combination Therapy with Insulin (with or without Metformin)
A total of 641 patients with type 2 diabetes participated in a 24-week, randomized, double-blind, placebo-controlled study designed to assess the efficacy of JANUVIA as add-on to insulin therapy (with or without metformin). The racial distribution in this study was approximately 70% white, 18% Asian, 7% black, and 5% other groups. Approximately 14% of the patients in this study were Hispanic. Patients entered a 2-week, single-blind run-in treatment period on pre-mixed, long-acting, or intermediate-acting insulin, with or without metformin (≥1500 mg per day). Patients using short-acting insulins were excluded unless the short-acting insulin was administered as part of a pre-mixed insulin. After the run-in period, patients with inadequate glycemic control (A1C 7.5% to 11%) were randomized to the addition of either 100 mg of JANUVIA or placebo, administered once daily. Patients were on a stable dose of insulin prior to enrollment with no changes in insulin dose permitted during the run-in period. Patients who failed to meet specific glycemic goals during the double-blind treatment period were to have uptitration of the background insulin dose as rescue therapy.
The median daily insulin dose at baseline was 42 units in the patients treated with JANUVIA and 45 units in the placebo-treated patients. The median change from baseline in daily dose of insulin was zero for both groups at the end of the study. In combination with insulin (with or without metformin), JANUVIA provided significant improvements in A1C, FPG, and 2-hour PPG compared to placebo (Table 14). Both treatment groups had an adjusted mean increase in body weight of 0.1 kg from baseline to Week 24. There was an increased rate of hypoglycemia in patients treated with JANUVIA. [See Warnings and Precautions (5.4); Adverse Reactions (6.1).]
Table 14: Glycemic Parameters at Final Visit (24-Week Study) for JANUVIA as Add-on Combination Therapy with Insulin* JANUVIA 100 mg
+ Insulin
(+/- Metformin)Placebo +
Insulin
(+/- Metformin)- * Intent-to-treat population using last observation on study prior to rescue therapy.
- † Least squares means adjusted for metformin use at the screening visit (yes/no), type of insulin used at the screening visit (pre-mixed vs. non-pre-mixed [intermediate- or long-acting]), and baseline value.
- ‡ Treatment by stratum interaction was not significant (p>0.10) for metformin stratum and for insulin stratum.
- § p<0.001 compared to placebo.
A1C (%) N = 305 N = 312 Baseline (mean) 8.7 8.6 Change from baseline (adjusted mean†) -0.6 -0.1 Difference from placebo (adjusted mean†,‡) (95% CI) -0.6§
(-0.7, -0.4)Patients (%) achieving A1C <7% 39 (12.8%) 16 (5.1%) FPG (mg/dL) N = 310 N = 313 Baseline (mean) 176 179 Change from baseline (adjusted mean†) -18 -4 Difference from placebo (adjusted mean†) (95% CI) -15§
(-23, -7)2-hour PPG (mg/dL) N = 240 N = 257 Baseline (mean) 291 292 Change from baseline (adjusted mean†) -31 5 Difference from placebo (adjusted mean†) (95% CI) -36§
(-47, -25)Maintenance of JANUVIA During Initiation and Titration of Insulin Glargine
A total of 746 patients with type 2 diabetes (mean baseline HbA1C 8.8%, disease duration 10.8 years) participated in a 30-week, randomized, double-blind, placebo-controlled study to assess the efficacy and safety of continuing JANUVIA during the initiation and uptitration of insulin glargine. Patients who were on a stable dose of metformin (≥1500 mg/day) in combination with a DPP-4 inhibitor and/or sulfonylurea but with inadequate glycemic control (A1C 7.5% to 11%) were enrolled in the study. Those on metformin and JANUVIA (100 mg/day) directly entered the double-blind treatment period; those on another DPP-4 inhibitor and/or on a sulfonylurea entered a 4-8 week run-in period in which they were maintained on metformin and switched to JANUVIA (100 mg); other DPP-4 inhibitors and sulfonylureas were discontinued. At randomization patients were randomized either to continue JANUVIA or to discontinue JANUVIA and switch to a matching placebo. On the day of randomization, insulin glargine was initiated at a dose of 10 units subcutaneously in the evening. Patients were instructed to uptitrate their insulin dose in the evening based on fasting blood glucose measurements to achieve a target of 72-100 mg/dL.
At 30 weeks, the mean reduction in A1C was greater in the sitagliptin group than in the placebo group (Table 15). At the end of the trial, 27.3% of patients in the sitagliptin group and 27.3% in the placebo group had a fasting plasma glucose (FPG) in the target range; there was no significant difference in insulin dose between arms.
Table 15: Change from Baseline in A1C and FPG at Week 30 in the Maintenance of JANUVIA During Initiation and Titration of Insulin Glargine Study Sitagliptin 100 mg
+Metformin
+ Insulin GlarginePlacebo
+Metformin
+ Insulin Glargine- * N is the number of randomized and treated patients.
- † Analysis of Covariance including all post-baseline data regardless of rescue or treatment discontinuation. Model estimates calculated using multiple imputation to model washout of the treatment effect using placebo data for all subjects having missing Week 30 data.
- ‡ p<0.001 compared to placebo.
A1C (%) N = 373* N = 370* Baseline (mean) 8.8 8.8 Week 30 (mean) 6.9 7.3 Change from baseline (adjusted mean)† -1.9 -1.4 Difference from placebo (adjusted mean) (95% CI)† -0.4 (-0.6, -0.3)‡ Patients (%) with A1C <7% 202 (54.2%) 131 (35.4%) FPG (mg/dL) N = 373* N = 370* Baseline (mean) 199 201 Week 30 (mean) 118 123 Change from baseline (adjusted mean)† -81 -76 -
16 HOW SUPPLIED/STORAGE AND HANDLING
Tablets: JANUVIA, 25 mg, are pink, round, film-coated tablets with "221" on one side. They are supplied as follows:
NDC 0006-0221-31 unit-of-use bottles of 30
NDC 0006-0221-54 unit-of-use bottles of 90
NDC 0006-0221-28 unit dose blister packages of 100.
Tablets: JANUVIA, 50 mg, are light beige, round, film-coated tablets with "112" on one side. They are supplied as follows:
NDC 0006-0112-31 unit-of-use bottles of 30
NDC 0006-0112-54 unit-of-use bottles of 90
NDC 0006-0112-28 unit dose blister packages of 100.
Tablets: JANUVIA, 100 mg, are beige, round, film-coated tablets with "277" on one side. They are supplied as follows:
NDC 0006-0277-31 unit-of-use bottles of 30
NDC 0006-0277-54 unit-of-use bottles of 90
NDC: 0006-0277-02 unit-of-use blister calendar package of 30
NDC: 0006-0277-33 unit-of-use blister calendar package of 30
NDC 0006-0277-28 unit dose blister packages of 100
NDC 0006-0277-82 bottles of 1000.
-
17 PATIENT COUNSELING INFORMATION
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
Pancreatitis
Inform patients that acute pancreatitis has been reported during postmarketing use of JANUVIA. Inform patients that persistent severe abdominal pain, sometimes radiating to the back, which may or may not be accompanied by vomiting, is the hallmark symptom of acute pancreatitis. Instruct patients to promptly discontinue JANUVIA and contact their physician if persistent severe abdominal pain occurs [see Warnings and Precautions (5.1)].
Heart Failure
Inform patients of the signs and symptoms of heart failure. Before initiating JANUVIA, ask patients about a history of heart failure or other risk factors for heart failure including moderate to severe renal impairment. Instruct patients to contact their health care provider as soon as possible if they experience symptoms of heart failure, including increasing shortness of breath, rapid increase in weight or swelling of the feet [see Warnings and Precautions (5.2)].
Hypoglycemia
Inform patients that the incidence of hypoglycemia is increased when JANUVIA is added to a sulfonylurea or insulin and that a lower dose of the sulfonylurea or insulin may be required to reduce the risk of hypoglycemia.
Hypersensitivity Reactions
Inform patients that allergic reactions have been reported during postmarketing use of JANUVIA. If symptoms of allergic reactions (including rash, hives, and swelling of the face, lips, tongue, and throat that may cause difficulty in breathing or swallowing) occur, patients must stop taking JANUVIA and seek medical advice promptly.
Severe and Disabling Arthralgia
Inform patients that severe and disabling joint pain may occur with this class of drugs. The time to onset of symptoms can range from one day to years. Instruct patients to seek medical advice if severe joint pain occurs [see Warnings and Precautions (5.6)].
Bullous Pemphigoid
Inform patients that bullous pemphigoid may occur with this class of drugs. Instruct patients to seek medical advice if blisters or erosions occur [see Warnings and Precautions (5.7)].
-
SPL UNCLASSIFIED SECTION
Distributed by: Merck Sharp & Dohme Corp., a subsidiary of
MERCK & CO., INC., Whitehouse Station, NJ 08889, USAFor patent information: www.merck.com/product/patent/home.html
Copyright © 2006-2019 Merck Sharp & Dohme Corp., a subsidiary of Merck & Co., Inc.
All rights reserved.uspi-mk0431-t-1908r024
-
MEDICATION GUIDE
Medication Guide
JANUVIA® (jah-NEW-vee-ah)
(sitagliptin)
TabletsThis Medication Guide has been approved by the U.S. Food and Drug Administration. Revised: 08/2017 Read this Medication Guide carefully before you start taking JANUVIA and each time you get a refill. There may be new information. This information does not take the place of talking with your doctor about your medical condition or your treatment. If you have any questions about JANUVIA, ask your doctor or pharmacist. What is the most important information I should know about JANUVIA?
Serious side effects can happen in people taking JANUVIA, including:-
Inflammation of the pancreas (pancreatitis) which may be severe and lead to death. Certain medical problems make you more likely to get pancreatitis.
Before you start taking JANUVIA, tell your doctor if you have ever had:
- pancreatitis
- high blood triglyceride levels
- stones in your gallbladder (gallstones)
- kidney problems
- a history of alcoholism
Stop taking JANUVIA and call your doctor right away if you have pain in your stomach area (abdomen) that is severe and will not go away. The pain may be felt going from your abdomen through to your back. The pain may happen with or without vomiting. These may be symptoms of pancreatitis. -
Heart failure. Heart failure means your heart does not pump blood well enough.
Before you start taking JANUVIA, tell your doctor if you have ever had heart failure or have problems with your kidneys. Contact your doctor right away if you have any of the following symptoms:
- increasing shortness of breath or trouble breathing, especially when you lie down
- swelling or fluid retention, especially in the feet, ankles or legs
- an unusually fast increase in weight
- unusual tiredness
What is JANUVIA? - JANUVIA is a prescription medicine used along with diet and exercise to lower blood sugar in adults with type 2 diabetes.
- JANUVIA is not for people with type 1 diabetes.
- JANUVIA is not for people with diabetic ketoacidosis (increased ketones in your blood or urine).
- If you have had pancreatitis (inflammation of the pancreas) in the past, it is not known if you have a higher chance of getting pancreatitis while you take JANUVIA.
- It is not known if JANUVIA is safe and effective when used in children under 18 years of age.
Who should not take JANUVIA?
Do not take JANUVIA if:- you are allergic to any of the ingredients in JANUVIA. See the end of this Medication Guide for a complete list of ingredients in JANUVIA.
What should I tell my doctor before taking JANUVIA?
Before you take JANUVIA, tell your doctor if you:- have or have had inflammation of your pancreas (pancreatitis).
- have kidney problems.
- have any other medical conditions.
- are pregnant or plan to become pregnant. It is not known if JANUVIA will harm your unborn baby. If you are pregnant, talk with your doctor about the best way to control your blood sugar while you are pregnant.
Pregnancy Registry: If you take JANUVIA at any time during your pregnancy, talk with your doctor about how you can join the JANUVIA pregnancy registry. The purpose of this registry is to collect information about the health of you and your baby. You can enroll in this registry by calling 1-800-986-8999. - are breast-feeding or plan to breast-feed. It is not known if JANUVIA will pass into your breast milk. Talk with your doctor about the best way to feed your baby if you are taking JANUVIA.
Know the medicines you take. Keep a list of your medicines and show it to your doctor and pharmacist when you get a new medicine.How should I take JANUVIA? - Take JANUVIA 1 time each day exactly as your doctor tells you.
- You can take JANUVIA with or without food.
- Your doctor may do blood tests from time to time to see how well your kidneys are working. Your doctor may change your dose of JANUVIA based on the results of your blood tests.
- Your doctor may tell you to take JANUVIA along with other diabetes medicines. Low blood sugar can happen more often when JANUVIA is taken with certain other diabetes medicines. See "What are the possible side effects of JANUVIA?".
- If you miss a dose, take it as soon as you remember. If you do not remember until it is time for your next dose, skip the missed dose and go back to your regular schedule. Do not take two doses of JANUVIA at the same time.
- If you take too much JANUVIA, call your doctor or local Poison Control Center right away.
- When your body is under some types of stress, such as fever, trauma (such as a car accident), infection or surgery, the amount of diabetes medicine that you need may change. Tell your doctor right away if you have any of these conditions and follow your doctor's instructions.
- Check your blood sugar as your doctor tells you to.
- Stay on your prescribed diet and exercise program while taking JANUVIA.
- Talk to your doctor about how to prevent, recognize and manage low blood sugar (hypoglycemia), high blood sugar (hyperglycemia), and problems you have because of your diabetes.
- Your doctor will check your diabetes with regular blood tests, including your blood sugar levels and your hemoglobin A1C.
What are the possible side effects of JANUVIA?
Serious side effects have happened in people taking JANUVIA.- See "What is the most important information I should know about JANUVIA?".
- Low blood sugar (hypoglycemia). If you take JANUVIA with another medicine that can cause low blood sugar, such as a sulfonylurea or insulin, your risk of getting low blood sugar is higher. The dose of your sulfonylurea medicine or insulin may need to be lowered while you use JANUVIA. Signs and symptoms of low blood sugar may include:
- headache
- drowsiness
- irritability
- hunger
- dizziness
- confusion
- sweating
- feeling jittery
- weakness
- fast heart beat
- Serious allergic reactions. If you have any symptoms of a serious allergic reaction, stop taking JANUVIA and call your doctor right away. See "Who should not take JANUVIA?". Your doctor may give you a medicine for your allergic reaction and prescribe a different medicine for your diabetes.
- Kidney problems, sometimes requiring dialysis
- Joint pain. Some people who take medicines called DPP-4 inhibitors like JANUVIA, may develop joint pain that can be severe. Call your doctor if you have severe joint pain.
- Skin reaction. Some people who take medicines called DPP-4 inhibitors like JANUVIA may develop a skin reaction called bullous pemphigoid that can require treatment in a hospital. Tell your doctor right away if you develop blisters or the breakdown of the outer layer of your skin (erosion). Your doctor may tell you to stop taking JANUVIA.
JANUVIA may have other side effects, including stomach upset and diarrhea, swelling of the hands or legs, when JANUVIA is used with rosiglitazone (Avandia®). Rosiglitazone is another type of diabetes medicine.
These are not all the possible side effects of JANUVIA. For more information, ask your doctor or pharmacist.
Tell your doctor if you have any side effect that bothers you, is unusual or does not go away.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.How should I store JANUVIA?
Store JANUVIA at 68°F to 77°F (20°C to 25°C).
Keep JANUVIA and all medicines out of the reach of children.General information about the use of JANUVIA
Medicines are sometimes prescribed for purposes that are not listed in Medication Guides. Do not use JANUVIA for a condition for which it was not prescribed. Do not give JANUVIA to other people, even if they have the same symptoms you have. It may harm them.
This Medication Guide summarizes the most important information about JANUVIA. If you would like to know more information, talk with your doctor. You can ask your doctor or pharmacist for additional information about JANUVIA that is written for health professionals. For more information, go to www.JANUVIA.com or call 1-800-622-4477.What are the ingredients in JANUVIA?
Active ingredient: sitagliptin
Inactive ingredients: microcrystalline cellulose, anhydrous dibasic calcium phosphate, croscarmellose sodium, magnesium stearate, and sodium stearyl fumarate. The tablet film coating contains the following inactive ingredients: polyvinyl alcohol, polyethylene glycol, talc, titanium dioxide, red iron oxide, and yellow iron oxide.What is type 2 diabetes?
Type 2 diabetes is a condition in which your body does not make enough insulin, and the insulin that your body produces does not work as well as it should. Your body can also make too much sugar. When this happens, sugar (glucose) builds up in the blood. This can lead to serious medical problems.
High blood sugar can be lowered by diet and exercise, and by certain medicines when necessary.Distributed by: Merck Sharp & Dohme Corp., a subsidiary of
MERCK & CO., INC., Whitehouse Station, NJ 08889, USA
For patent information: www.merck.com/product/patent/home.html. The trademarks depicted herein are owned by their respective companies. Copyright © 2010-2017 Merck Sharp & Dohme Corp., a subsidiary of Merck & Co., Inc.
All rights reserved. usmg-mk0431-t-1708r016 -
Inflammation of the pancreas (pancreatitis) which may be severe and lead to death. Certain medical problems make you more likely to get pancreatitis.
-
PRINCIPAL DISPLAY PANEL - 25 mg Tablet Bottle Label
NDC: 0006-0221-31
Januvia®
(sitagliptin) tablets25 mg
Dispense the accompanying Medication
Guide to each patient.Each tablet contains 32.13 mg sitagliptin
phosphate, equivalent to 25 mg sitagliptin.Rx only
30 Tablets
-
PRINCIPAL DISPLAY PANEL - 50 mg Tablet Bottle Label
NDC: 0006-0112-31
Januvia®
(sitagliptin) tablets50 mg
Dispense the accompanying Medication
Guide to each patient.Each tablet contains 64.25 mg sitagliptin
phosphate, equivalent to 50 mg sitagliptin.Rx only
30 Tablets
-
PRINCIPAL DISPLAY PANEL - 100 mg Tablet Bottle Label
NDC: 0006-0277-31
Januvia®
(sitagliptin) tablets100 mg
Dispense the accompanying Medication
Guide to each patient.Each tablet contains 128.5 mg
sitagliptin phosphate, equivalent
to 100 mg sitagliptin.Rx only
30 Tablets
-
INGREDIENTS AND APPEARANCE
JANUVIA
sitagliptin tablet, film coatedProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 0006-0221 Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength SITAGLIPTIN PHOSPHATE (UNII: TS63EW8X6F) (SITAGLIPTIN - UNII:QFP0P1DV7Z) SITAGLIPTIN 25 mg Inactive Ingredients Ingredient Name Strength ANHYDROUS DIBASIC CALCIUM PHOSPHATE (UNII: L11K75P92J) CROSCARMELLOSE SODIUM (UNII: M28OL1HH48) MAGNESIUM STEARATE (UNII: 70097M6I30) MICROCRYSTALLINE CELLULOSE (UNII: OP1R32D61U) POLYETHYLENE GLYCOL, UNSPECIFIED (UNII: 3WJQ0SDW1A) POLYVINYL ALCOHOL, UNSPECIFIED (UNII: 532B59J990) FERRIC OXIDE RED (UNII: 1K09F3G675) SODIUM STEARYL FUMARATE (UNII: 7CV7WJK4UI) talc (UNII: 7SEV7J4R1U) titanium dioxide (UNII: 15FIX9V2JP) FERRIC OXIDE YELLOW (UNII: EX438O2MRT) Product Characteristics Color PINK (pink) Score no score Shape ROUND (round) Size 6mm Flavor Imprint Code 221 Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 0006-0221-28 100 in 1 CARTON 10/16/2006 1 NDC: 0006-0221-01 1 in 1 BLISTER PACK; Type 0: Not a Combination Product 2 NDC: 0006-0221-31 30 in 1 BOTTLE; Type 0: Not a Combination Product 10/16/2006 3 NDC: 0006-0221-54 90 in 1 BOTTLE; Type 0: Not a Combination Product 10/16/2006 Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date NDA NDA021995 10/16/2006 JANUVIA
sitagliptin tablet, film coatedProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 0006-0112 Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength SITAGLIPTIN PHOSPHATE (UNII: TS63EW8X6F) (SITAGLIPTIN - UNII:QFP0P1DV7Z) SITAGLIPTIN 50 mg Inactive Ingredients Ingredient Name Strength ANHYDROUS DIBASIC CALCIUM PHOSPHATE (UNII: L11K75P92J) CROSCARMELLOSE SODIUM (UNII: M28OL1HH48) magnesium stearate (UNII: 70097M6I30) MICROCRYSTALLINE CELLULOSE (UNII: OP1R32D61U) POLYETHYLENE GLYCOL, UNSPECIFIED (UNII: 3WJQ0SDW1A) POLYVINYL ALCOHOL, UNSPECIFIED (UNII: 532B59J990) FERRIC OXIDE RED (UNII: 1K09F3G675) SODIUM STEARYL FUMARATE (UNII: 7CV7WJK4UI) talc (UNII: 7SEV7J4R1U) titanium dioxide (UNII: 15FIX9V2JP) FERRIC OXIDE YELLOW (UNII: EX438O2MRT) Product Characteristics Color BROWN (light beige) Score no score Shape ROUND (round) Size 8mm Flavor Imprint Code 112 Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 0006-0112-28 100 in 1 CARTON 10/16/2006 1 NDC: 0006-0112-01 1 in 1 BLISTER PACK; Type 0: Not a Combination Product 2 NDC: 0006-0112-31 30 in 1 BOTTLE; Type 0: Not a Combination Product 10/16/2006 3 NDC: 0006-0112-54 90 in 1 BOTTLE; Type 0: Not a Combination Product 10/16/2006 Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date NDA NDA021995 10/16/2006 JANUVIA
sitagliptin tablet, film coatedProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 0006-0277 Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength SITAGLIPTIN PHOSPHATE (UNII: TS63EW8X6F) (SITAGLIPTIN - UNII:QFP0P1DV7Z) SITAGLIPTIN 100 mg Inactive Ingredients Ingredient Name Strength ANHYDROUS DIBASIC CALCIUM PHOSPHATE (UNII: L11K75P92J) croscarmellose sodium (UNII: M28OL1HH48) magnesium stearate (UNII: 70097M6I30) MICROCRYSTALLINE CELLULOSE (UNII: OP1R32D61U) POLYETHYLENE GLYCOL, UNSPECIFIED (UNII: 3WJQ0SDW1A) POLYVINYL ALCOHOL, UNSPECIFIED (UNII: 532B59J990) FERRIC OXIDE RED (UNII: 1K09F3G675) SODIUM STEARYL FUMARATE (UNII: 7CV7WJK4UI) talc (UNII: 7SEV7J4R1U) titanium dioxide (UNII: 15FIX9V2JP) FERRIC OXIDE YELLOW (UNII: EX438O2MRT) Product Characteristics Color BROWN (beige) Score no score Shape ROUND (round) Size 10mm Flavor Imprint Code 277 Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 0006-0277-28 100 in 1 CARTON 10/16/2006 1 NDC: 0006-0277-01 1 in 1 BLISTER PACK; Type 0: Not a Combination Product 2 NDC: 0006-0277-31 30 in 1 BOTTLE; Type 0: Not a Combination Product 10/16/2006 3 NDC: 0006-0277-54 90 in 1 BOTTLE; Type 0: Not a Combination Product 10/16/2006 4 NDC: 0006-0277-02 30 in 1 DOSE PACK; Type 0: Not a Combination Product 10/16/2006 5 NDC: 0006-0277-33 30 in 1 DOSE PACK; Type 0: Not a Combination Product 10/16/2006 6 NDC: 0006-0277-82 1000 in 1 BOTTLE; Type 0: Not a Combination Product 10/16/2006 7 NDC: 0006-0277-14 2 in 1 CARTON 10/12/2012 7 7 in 1 BLISTER PACK; Type 0: Not a Combination Product 8 NDC: 0006-0277-27 4 in 1 CARTON 10/16/2006 09/30/2015 8 7 in 1 BLISTER PACK; Type 0: Not a Combination Product 9 NDC: 0006-0277-30 30 in 1 BOTTLE; Type 0: Not a Combination Product 10/16/2006 02/29/2016 Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date NDA NDA021995 10/16/2006 Labeler - Merck Sharp & Dohme Corp. (001317601)
Trademark Results [JANUVIA]
Mark Image Registration | Serial | Company Trademark Application Date |
|---|---|
 JANUVIA 78833412 3621009 Live/Registered |
MERCK SHARP & DOHME CORP. 2006-03-09 |
 JANUVIA 76635570 3261637 Live/Registered |
MERCK SHARP & DOHME CORP. 2005-04-07 |
© 2026 FDA.report
This site is not affiliated with or endorsed by the FDA.