FENOPROFEN- fenoprofen calcium capsule
FENOPROFEN by
Drug Labeling and Warnings
FENOPROFEN by is a Prescription medication manufactured, distributed, or labeled by Belcher Pharmaceuticals,LLC. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
-
HIGHLIGHTS OF PRESCRIBING INFORMATION
These highlights do not include all the information needed to use Fenoprofen safely and effectively. See full prescribing information for Fenoprofen.
Fenoprofen (fenoprofen calcium, USP) capsules, for oral use
Initial U.S. Approval: 1982WARNING: RISK OF SERIOUS CARDIOVASCULAR AND GASTROINTESTINAL EVENTS
See full prescribing information for complete boxed warning
- Non-Steroidal Anti-Inflammatory drugs (NSAIDs) cause an increased risk of serious cardiovascular thrombotic events, including myocardial infarction and stroke, which can be fatal. This risk may occur early in treatment and may increase with duration of use. (5.1)
- Fenoprofen is contraindicated in the setting of coronary artery bypass graft (CABG) surgery (4, 5.1)
- NSAIDs cause an increased risk of serious gastrointestinal (GI) adverse events including bleeding, ulceration, and perforation of stomach or intestines, which can be fatal. These events can occur at any time during use and without warning symptoms. Elderly patients and patients with a prior history of peptic ulcer disease and/or GI bleeding are at greater risk for serious GI events (5.2)
RECENT MAJOR CHANGES
INDICATIONS AND USAGE
DOSAGE AND ADMINISTRATION
- Use the lowest effective dosage for shortest duration consistent with individual patient treatment goals (2.1)
- Analgesia: For the treatment of mild to moderate pain, the recommended dosage is 200 mg given orally every 4 to 6 hours, as needed (2.1)
- Rheumatoid Arthritis and Osteoarthritis: For the relief of signs and symptoms of rheumatoid arthritis or osteoarthritis the recommended dose is 400 to 600 mg given orally, 3 or 4 times a day. The dose should be tailored to the needs of the patient and may be increased or decreased depending on the severity of the symptoms. Dosage adjustments may be made after initiation of drug therapy or during exacerbations of the disease. Total daily dosage should not exceed 3,200 mg.
DOSAGE FORMS AND STRENGTHS
Fenoprofen calcium® (fenoprofen calcium, USP) capsules: 200 mg and 400 mg (3) (3)
CONTRAINDICATIONS
WARNINGS AND PRECAUTIONS
- Hepatotoxicity: Inform patients of warning signs and symptoms of hepatotoxicity. Discontinue if abnormal liver tests persist or worsen or if clinical signs and symptoms of liver disease develop (5.3)
- Hypertension: Patients taking some antihypertensive medications may have impaired response to these therapies when taking NSAIDs. Monitor blood pressure (5.4, 7)
- Heart Failure and Edema: Avoid use of Fenoprofen in patients with severe heart failure unless benefits are expected to outweigh risk of worsening heart failure (5.5)
- Renal Toxicity: Monitor renal function in patients with renal or hepatic impairment, heart failure, dehydration, or hypovolemia. Avoid use of Fenoprofen in patients with advanced renal disease unless benefits are expected to outweigh risk of worsening renal function (5.6)
- Anaphylactic Reactions: Seek emergency help if an anaphylactic reaction occurs (5.7)
- Exacerbation of Asthma Related to Aspirin Sensitivity: Fenoprofen is contraindicated in patients with aspirin-sensitive asthma. Monitor patients with preexisting asthma (without aspirin sensitivity) (5.8)
- Serious Skin Reactions: Discontinue Fenoprofen at first appearance of skin rash or other signs of hypersensitivity (5.9)
- Premature Closure of Fetal Ductus Arteriosus: Avoid use in pregnant women starting at 30 weeks gestation (5.10, 8.1)
- Hematologic Toxicity: Monitor hemoglobin or hematocrit in patients with any signs or symptoms of anemia (5.11, 7)
ADVERSE REACTIONS
Most common adverse reactions (incidence ≥ 5%) are Dyspepsia, headache, somnolence, nausea, dizziness, constipation, nervousness, asthenia, and peripheral edema.
To report SUSPECTED ADVERSE REACTIONS, contact Belcher Pharmaceuticals, LLC at (727) 471-0850 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch (6)
DRUG INTERACTIONS
- Drugs that Interfere with Hemostasis (e.g. warfarin, aspirin, SSRIs/SNRIs): Monitor patients for bleeding who are concomitantly taking Fenoprofen with drugs that interfere with hemostasis. Concomitant use of Fenoprofen and analgesic doses of aspirin is not generally recommended (7)
- ACE Inhibitors, Angiotensin Receptor Blockers (ARB), or Beta-Blockers: Concomitant use with Fenoprofen may diminish the antihypertensive effect of these drugs. Monitor blood pressure (7)
- ACE Inhibitors and ARBs: Concomitant use with Fenoprofen in elderly, volume depleted, or those with renal impairment may result in deterioration of renal function. In such high risk patients, monitor for signs of worsening renal function (7)
- Diuretics: NSAIDs can reduce natriuretic effect of furosemide and thiazide diuretics. Monitor patients to assure diuretic efficacy including antihypertensive effects (7)
- Digoxin: Concomitant use with Fenoprofen can increase serum concentration and prolong half-life of digoxin. Monitor serum digoxin levels (7)
USE IN SPECIFIC POPULATIONS
Pregnancy: Use of NSAIDs during the third trimester of pregnancy increases the risk of premature closure of the fetal ductus arteriosus. Avoid use of NSAIDs in pregnant women starting at 30 weeks gestation (5.10, 8.1)
Infertility: NSAIDs are associated with reversible infertility. Consider withdrawal of Fenoprofen in women who have difficulties conceiving (8.3)
See 17 for PATIENT COUNSELING INFORMATION and Medication Guide.
Revised: 4/2017
-
Table of Contents
FULL PRESCRIBING INFORMATION: CONTENTS*
WARNING: RISK OF SERIOUS CARDIOVASCULAR AND GASTROINTESTINAL EVENTS
1. INDICATIONS AND USAGE
2. DOSAGE AND ADMINISTRATION
2.1 General Dosing Instructions
2.2 Analgesia
2.3 Rheumatoid Arthritis and Osteoarthritis
3. DOSAGE FORMS AND STRENGTHS
4. CONTRAINDICATIONS
5. WARNINGS AND PRECAUTIONS
5.1 Cardiovascular Thrombotic Events
5.2 Gastrointestinal Bleeding, Ulceration, and Perforation
5.3 Hepatotoxicity
5.4 Hypertension
5.5 Heart Failure and Edema
5.6 Renal Toxicity and Hyperkalemia
5.7 Anaphylactic Reactions
5.8 Exacerbation of Asthma Related to Aspirin Sensitivity
5.9 Serious Skin Reactions
5.10 Premature Closure of Fetal Ductus Arteriosus
5.11 Hematologic Toxicity
5.12 Masking of Inflammation and Fever
5.13 Laboratory Monitoring
5.14 Ocular Effects
5.15 Central Nervous System Effects
5.16 Impact on Hearing
6. ADVERSE REACTIONS
6.1 Clinical Trials Experience
7. DRUG INTERACTIONS
8. USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
8.2 Lactation
8.3 Females and Males of Reproductive Potential
8.4 Pediatric Use
8.5 Geriatric Use
10. OVERDOSAGE
11. DESCRIPTION
12. CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
12.3 Pharmacokinetics
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, and Impairment of Fertility
14. CLINICAL STUDIES
16. HOW SUPPLIED/STORAGE AND HANDLING
17. PATIENT COUNSELING INFORMATION
- * Sections or subsections omitted from the full prescribing information are not listed.
-
BOXED WARNING
(What is this?)
WARNING: RISK OF SERIOUS CARDIOVASCULAR AND GASTROINTESTINAL EVENTS
Cardiovascular Thrombic Events
- Non-Steroidal Anti-Inflammatory drugs (NSAIDs) cause an increased risk of serious cardiovascular thrombotic events, including myocardial infarction and stroke, which can be fatal. This risk may occur early in treatment and may increase with duration of use. [ see Warnings and Precautions (5.1) ].
Gastrointestinal Bleeding, Ulceration, and Perforation
- NSAIDs cause an increased risk of serious gastrointestinal (GI) adverse events including bleeding, ulceration, and perforation of stomach or intestines, which can be fatal. These events can occur at any time during use and without warning symptoms. Elderly patients and patients with a prior history of peptic ulcer disease and/or GI bleeding are at greater risk for serious GI events [ see Warnings and Precautions (5.2) ].
- 1. INDICATIONS AND USAGE
-
2. DOSAGE AND ADMINISTRATION
2.1 General Dosing Instructions
Carefully consider the potential benefits and risks of Fenoprofen and other treatment options before deciding to use Fenoprofen. Use lowest effective dosage for the shortest duration consistent with individual patient treatment goals [ see Warnings and Precautions (5) ].
Fenoprofen may be administered with meals or with milk. Although the total amount absorbed is not affected, peak blood levels are delayed and diminished.
Patients with rheumatoid arthritis generally seem to require larger doses of Fenoprofen calcium than do those with osteoarthritis. The smallest dose that yields acceptable control should be employed.
Although improvement may be seen in a few days in many patients, an additional 2 to 3 weeks may be required to gauge the full benefits of therapy.2.2 Analgesia
For the treatment of mild to moderate pain, the recommended dosage is 200 mg given orally every 4 to 6 hours, as needed.
2.3 Rheumatoid Arthritis and Osteoarthritis
For the relief of signs and symptoms of rheumatoid arthritis or osteoarthritis the recommended dose is 400 to 600 mg given orally, 3 or 4 times a day. The dose should be tailored to the needs of the patient and may be increased or decreased depending on the severity of the symptoms. Dosage adjustments may be made after initiation of drug therapy or during exacerbations of the disease. Total daily dosage should not exceed 3,200 mg.
- 3. DOSAGE FORMS AND STRENGTHS
-
4. CONTRAINDICATIONS
Fenoprofen is contraindicated in the following patients:
- Known hypersensitivity (e.g., anaphylactic reactions and serious skin reactions) to fenoprofen or any components of the drug product [ see Warnings and Precautions (5.7, 5.9) ]
- History of asthma, urticaria, or other allergic-type reactions after taking aspirin or other NSAIDs. Severe, sometimes fatal, anaphylactic reactions to NSAIDs have been reported in such patients [ see Warnings and Precautions (5.7, 5.8) ]
- In the setting of coronary artery bypass graft (CABG) surgery [ see Warnings and Precautions (5.1) ]
-
5. WARNINGS AND PRECAUTIONS
5.1 Cardiovascular Thrombotic Events
Clinical trials of several COX-2 selective and nonselective NSAIDs of up to three years duration have shown an increased risk of serious cardiovascular (CV) thrombotic events, including myocardial infarction (MI) and stroke, which can be fatal. Based on available data, it is unclear that the risk for CV thrombotic events is similar for all NSAIDs. The relative increase in serious CV thrombotic events over baseline conferred by NSAID use appears to be similar in those with and without known CV disease or risk factors for CV disease. However, patients with known CV disease or risk factors had a higher absolute incidence of excess serious CV thrombotic events, due to their increased baseline rate. Some observational studies found that this increased risk of serious CV thrombotic events began as early as the first weeks of treatment. The increase in CV thrombotic risk has been observed most consistently at higher doses.
To minimize the potential risk for an adverse CV event in NSAID-treated patients, use the lowest effective dose for the shortest duration possible. Physicians and patients should remain alert for the development of such events, throughout the entire treatment course, even in the absence of previous CV symptoms. Patients should be informed about the symptoms of serious CV events and the steps to take if they occur.
There is no consistent evidence that concurrent use of aspirin mitigates the increased risk of serious CV thrombotic events associated with NSAID use. The concurrent use of aspirin and an NSAID, such as fenoprofen, increases the risk of serious gastrointestinal (GI) events [ see Warnings and Precautions (5.2) ].
Status Post Coronary Artery Bypass Graft (CABG) Surgery
Two large, controlled clinical trials of a COX-2 selective NSAID for the treatment of pain in the first 10–14 days following CABG surgery found an increased incidence of myocardial infarction and stroke. NSAIDs are contraindicated in the setting of CABG [ see Contraindications (4) ].Post-MI Patients
Observational studies conducted in the Danish National Registry have demonstrated that patients treated with NSAIDs in the post-MI period were at increased risk of reinfarction, CV-related death, and all-cause mortality beginning in the first week of treatment. In this same cohort, the incidence of death in the first year post-MI was 20 per 100 person years in NSAID-treated patients compared to 12 per 100 person years in non-NSAID exposed patients. Although the absolute rate of death declined somewhat after the first year post-MI, the increased relative risk of death in NSAID users persisted over at least the next four years of follow-up.Avoid the use of Fenoprofen in patients with a recent MI unless the benefits are expected to outweigh the risk of recurrent CV thrombotic events. If Fenoprofen is used in patients with a recent MI, monitor patients for signs of cardiac ischemia.
5.2 Gastrointestinal Bleeding, Ulceration, and Perforation
NSAIDs, including Fenoprofen, cause serious gastrointestinal (GI) adverse events including inflammation, bleeding, ulceration, and perforation of the esophagus, stomach, small intestine, or large intestine, which can be fatal. These serious adverse events can occur at any time, with or without warning symptoms, in patients treated with NSAIDS. Only one in five patients who develop a serious upper GI adverse event on NSAID therapy is symptomatic. Upper GI ulcers, gross bleeding, or perforation caused by NSAIDs occurred in approximately 1% of patients treated for 3-6 months, and in about 2%-4% of patients treated for one year. However, even short-term NSAID therapy is not without risk.
Risk Factors for GI Bleeding, Ulceration, and Perforation
Patients with a prior history of peptic ulcer disease and/or GI bleeding who used NSAIDs had a greater than 10-fold increased risk of developing a GI bleed compared to patients without these risk factors. Other factors that increase the risk for GI bleeding in patients treated with NSAIDs include longer duration of NSAID therapy; concomitant use of oral corticosteroids, aspirin, anticoagulants, or selective serotonin reuptake inhibitors (SSRIs); smoking; use of alcohol; older age; and poor general health status. Most postmarketing reports of fatal GI events occurred in elderly or debilitated patients. Additionally, patients with advanced liver disease and/or coagulopathy are at increased risk for GI bleeding.Strategies to Minimize the GI Risks in NSAID-treated Patients:
- Use the lowest effective dosage for the shortest possible duration.
- Avoid administration of more than one NSAID at a time.
- Avoid use in patients at higher risk unless benefits are expected to outweigh theincreased risk of bleeding. For such patients, as well as those with active GIbleeding, consider alternate therapies other than NSAIDs.
- Remain alert for signs and symptoms of GI ulceration and bleeding during NSAID therapy.
- If a serious GI adverse event is suspected, promptly initiate evaluation and treatment, and discontinue Fenoprofen until a serious GI adverse event is ruled out.
- In the setting of concomitant use of low-dose aspirin for cardiac prophylaxis, monitor patients more closely for evidence of GI bleeding [ see Drug Interactions (7) ].
5.3 Hepatotoxicity
Elevations of ALT or AST (three or more times the upper limit of normal [ULN]) have been reported in approximately 1% of NSAID-treated patients in clinical trials. In addition, rare, sometimes fatal, cases of severe hepatic injury, including fulminant hepatitis, liver necrosis, and hepatic failure have been reported.
Elevations of ALT or AST (less than three times ULN) may occur in up to 15% of patients treated with NSAIDs including fenoprofen.
Inform patients of the warning signs and symptoms of hepatotoxicity (e.g., nausea, fatigue, lethargy, diarrhea, pruritus, jaundice, right upper quadrant tenderness, and "flu-like" symptoms). If clinical signs and symptoms consistent with liver disease develop, or if systemic manifestations occur (e.g., eosinophilia, rash, etc.), discontinue Fenoprofen immediately, and perform a clinical evaluation of the patient.
5.4 Hypertension
NSAIDs, including Fenoprofen, can lead to new onset of hypertension or worsening of pre-existing hypertension, either of which may contribute to the increased incidence of CV events. Patients taking angiotensin converting enzyme (ACE) inhibitors, thiazide diuretics, or loop diuretics may have impaired response to these therapies when taking NSAIDs [ see Drug Interactions (7) ].
Monitor blood pressure (BP) during the initiation of NSAID treatment and throughout the course of therapy.
5.5 Heart Failure and Edema
The Coxib and traditional NSAID Trialists’ Collaboration meta-analysis of randomized controlled trials demonstrated an approximately two-fold increase in hospitalizations for heart failure in COX-2 selective-treated patients and nonselective NSAID-treated patients compared to placebo-treated patients. In a Danish National Registry study of patients with heart failure, NSAID use increased the risk of MI, hospitalization for heart failure, and death.
Additionally, fluid retention and edema have been observed in some patients treated with NSAIDs. Use of fenoprofen may blunt the CV effects of several therapeutic agents used to treat these medical conditions (e.g., diuretics, ACE inhibitors, or angiotensin receptor blockers [ARBs]) [ see Drug Interactions (7) ].
Avoid the use of Fenoprofen in patients with severe heart failure unless the benefits are expected to outweigh the risk of worsening heart failure. If Fenoprofen is used in patients with severe heart failure, monitor patients for signs of worsening heart failure.
5.6 Renal Toxicity and Hyperkalemia
Renal Toxicity
Long-term administration of NSAIDs has resulted in renal papillary necrosis and other renal injury.Renal toxicity has also been seen in patients in whom renal prostaglandins have a compensatory role in the maintenance of renal perfusion. In these patients, administration of an NSAID may cause a dose-dependent reduction in prostaglandin formation and, secondarily, in renal blood flow, which may precipitate overt renal decompensation. Patients at greatest risk of this reaction are those with impaired renal function, dehydration, hypovolemia, heart failure, liver dysfunction, those taking diuretics and ACE inhibitors or ARBs, and the elderly. Discontinuation of NSAID therapy is usually followed by recovery to the pretreatment state.
No information is available from controlled clinical studies regarding the use of Fenoprofen in patients with advanced renal disease. The renal effects of Fenoprofen may hasten the progression of renal dysfunction in patients with pre-existing renal disease.
Correct volume status in dehydrated or hypovolemic patients prior to initiating Fenoprofen. Monitor renal function in patients with renal or hepatic impairment, heart failure, dehydration, or hypovolemia during use of Fenoprofen [ see Drug Interactions (7) ]. Avoid the use of Fenoprofen in patients with advanced renal disease unless the benefits are expected to outweigh the risk of worsening renal function. If Fenoprofen is used in patients with advanced renal disease, monitor patients for signs of worsening renal function.
Hyperkalemia
Increases in serum potassium concentration, including hyperkalemia, have been reported with use of NSAIDs, even in some patients without renal impairment. In patients with normal renal function, these effects have been attributed to a hyporeninemic-hypoaldosteronism state.5.7 Anaphylactic Reactions
Fenoprofen has been associated with anaphylactic reactions in patients with and without known hypersensitivity to fenoprofen and in patients with aspirin-sensitive asthma [ see Contraindications (4) and Warnings and Precautions (5.8) ].
Seek emergency help if an anaphylactic reaction occurs.
5.8 Exacerbation of Asthma Related to Aspirin Sensitivity
A subpopulation of patients with asthma may have aspirin-sensitive asthma which may include chronic rhinosinusitis complicated by nasal polyps; severe, potentially fatal bronchospasm; and/or intolerance to aspirin and other NSAIDs. Because cross-reactivity between aspirin and other NSAIDs has been reported in such aspirin-sensitive patients, Fenoprofen is contraindicated in patients with this form of aspirin sensitivity [ see Contraindications (4) ]. When Fenoprofen is used in patients with preexisting asthma (without known aspirin sensitivity), monitor patients for changes in the signs and symptoms of asthma.
5.9 Serious Skin Reactions
NSAIDs, including fenopropfen, can cause serious skin adverse reactions such as exfoliative dermatitis, Stevens-Johnson Syndrome (SJS), and toxic epidermal necrolysis (TEN), which can be fatal. These serious events may occur without warning. Inform patients about the signs and symptoms of serious skin reactions, and to discontinue the use of Fenoprofen at the first appearance of skin rash or any other sign of hypersensitivity.
Fenoprofen is contraindicated in patients with previous serious skin reactions to NSAIDs [ see Contraindications ( 4) ].
5.10 Premature Closure of Fetal Ductus Arteriosus
Fenoprofen may cause premature closure of the fetal ductus arteriosus. Avoid use of NSAIDs, including Fenoprofen, in pregnant women starting at 30 weeks of gestation (third trimester) [ see Use in Specific Populations (8.1) ].
5.11 Hematologic Toxicity
Anemia has occurred in NSAID-treated patients. This may be due to occult or gross blood loss, fluid retention, or an incompletely described effect on erythropoiesis. If a patient treated with Fenoprofen has any signs or symptoms of anemia, monitor hemoglobin or hematocrit.
NSAIDs, including Fenoprofen, may increase the risk of bleeding events. Co-morbid conditions such as coagulation disorders, concomitant use of warfarin, other anticoagulants, antiplatelet agents (e.g., aspirin), serotonin reuptake inhibitors (SSRIs) and serotonin norepinephrine reuptake inhibitors (SNRIs) may increase this risk. Monitor these patients for signs of bleeding [ see Drug Interactions (7) ].
5.12 Masking of Inflammation and Fever
The pharmacological activity of Fenoprofen in reducing inflammation, and possibly fever, may diminish the utility of diagnostic signs in detecting infections.
5.13 Laboratory Monitoring
Because serious GI bleeding, hepatotoxicity, and renal injury can occur without warning symptoms or signs, consider monitoring patients on long-term NSAID treatment with a CBC and a chemistry profile periodically [ see Warnings and Precautions (5.2, 5.3, 5.6) ].
5.14 Ocular Effects
Studies to date have not shown changes in the eyes attributable to the administration of Fenoprofen. However, adverse ocular effects have been observed with other anti-inflammatory drugs. Eye examinations, therefore, should be performed if visual disturbances occur in patients taking Fenoprofen.
-
6. ADVERSE REACTIONS
The following adverse reactions are discussed in greater detail in other sections of the labeling:
- Cardiovascular Thrombotic Events [ see Warnings and Precautions ( 5.1) ]
- GI Bleeding, Ulceration and Perforation [ see Warnings and Precautions ( 5.2) ]
- Hepatotoxicity [ see Warnings and Precautions ( 5.3) ]
- Hypertension [ see Warnings and Precautions ( 5.4) ]
- Heart Failure and Edema [ see Warnings and Precautions ( 5.5) ]
- Renal Toxicity and Hyperkalemia [ see Warnings and Precautions ( 5.6) ]
- Anaphylactic Reactions [ see Warnings and Precautions ( 5.7) ]
- Serious Skin Reactions [ see Warnings and Precautions ( 5.9) ]
- Hematologic Toxicity [ see Warnings and Precautions ( 5.11) ]
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
During clinical studies for rheumatoid arthritis, osteoarthritis, or mild to moderate pain and studies of pharmacokinetics, complaints were compiled from a checklist of potential adverse reactions, and the following data emerged. These encompass observations in 6,786 patients, including 188 observed for at least 52 weeks. For comparison, data are also presented from complaints received from the 266 patients who received placebo in these same trials. During short-term studies for analgesia, the incidence of adverse reactions was markedly lower than that seen in longer-term studies.
Adverse Drug Reactions Reported in >1% of Patients During Clinical Trials
Digestive System — During clinical trials with Fenoprofen Calcium, the most common adverse reactions were gastrointestinal in nature and occurred in 20.8% of patients receiving Fenoprofen Calcium as compared to 16.9% of patients receiving placebo. In descending order of frequency, these reactions included dyspepsia (10.3% Fenoprofen Calcium vs. 2.3% placebo), nausea (7.7% vs. 7.1%), constipation (7% vs. 1.5%), vomiting (2.6% vs. 1.9%), abdominal pain (2% vs. 1.1%), and diarrhea (1.8% vs. 4.1%). The drug was discontinued because of adverse gastrointestinal reactions in less than 2% of patients during premarketing studies.
Nervous System — The most frequent adverse neurologic reactions were headache (8.7% vs. 7.5%) and somnolence (8.5% vs. 6.4%). Dizziness (6.5% vs. 5.6%), tremor (2.2% vs. 0.4%), and confusion (1.4% vs. none) were noted less frequently. Fenoprofen Calcium was discontinued in less than 0.5% of patients because of these side effects during premarketing studies.
Skin and Appendages— Increased sweating (4.6% vs. 0.4%), pruritus (4.2% vs. 0.8%), and rash (3.7% vs. 0.4%) were reported. Fenoprofen Calcium was discontinued in about 1% of patients because of an adverse effect related to the skin during premarketing studies.
Special Senses — Tinnitus (4.5% vs. 0.4%), blurred vision (2.2% vs. none), and decreased hearing (1.6% vs. none) were reported. Fenoprofen Calcium was discontinued in less than 0.5% of patients because of adverse effects related to the special senses during premarketing studies.
Cardiovascular — Palpitations (2.5% vs. 0.4%). Fenoprofen Calcium was discontinued in about 0.5% of patients because of adverse cardiovascular reactions during premarketing studies.
Miscellaneous — Nervousness (5.7% vs. 1.5%), asthenia (5.4% vs. 0.4%), peripheral edema (5.0% vs. 0.4%), dyspnea (2.8% vs. none), fatigue (1.7% vs. 1.5%), upper respiratory infection (1.5% vs. 5.6%), and nasopharyngitis (1.2% vs. none).
Adverse Drug Reactions Reported in <1% of Patients During Clinical Trials
Digestive System—Gastritis, peptic ulcer with/without perforation, gastrointestinal hemorrhage, anorexia, flatulence, dry mouth, and blood in the stool. Increases in alkaline phosphatase, LDH, SGOT, jaundice, and cholestatic hepatitis, aphthous ulcerations of the buccal mucosa, metallic taste, and pancreatitis.
Cardiovascular—Atrial fibrillation, pulmonary edema, electrocardiographic changes, and supraventricular tachycardia.
Genitourinary Tract—Renal failure, dysuria, cystitis, hematuria, oliguria, azotemia, anuria, interstitial nephritis, nephrosis, and papillary necrosis.
Hypersensitivity—Angioedema (angioneurotic edema).
Hematologic—Purpura, bruising, hemorrhage, thrombocytopenia, hemolytic anemia, aplastic anemia, agranulocytosis, and pancytopenia.
Nervous System—Depression, disorientation, seizures, and trigeminal neuralgia.
Special Senses—Burning tongue, diplopia, and optic neuritis.
Skin and Appendages—Exfoliative dermatitis, toxic epidermal necrolysis, Stevens-Johnson syndrome, and alopecia.
Miscellaneous—Anaphylaxis, urticaria, malaise, insomnia, tachycardia, personality change, lymphadenopathy, mastodynia, and fever.
-
7. DRUG INTERACTIONS
See Table 1 for clinically significant drug interactions with fenoprophen.
Table 1: Clinically Significant Drug Interactions with Fenoprofen Drugs That Interfere with Hemostasis Clinical Impact: - Fenoprofen and anticoagulants such as warfarin have a synergistic effect on bleeding. The concomitant use of fenoprofen and anticoagulants have an increased risk of serious bleeding compared to the use of either drug alone.
- Serotonin release by platelets plays an important role in hemostasis. Case-control and cohort epidemiological studies showed that concomitant use of drugs that interfere with serotonin reuptake and an NSAID may potentiate the risk of bleeding more than an NSAID alone.
Intervention: Monitor patients with concomitant use of Fenoprofen with anticoagulants (e.g., warfarin), antiplatelet agents (e.g., aspirin), selective serotonin reuptake inhibitors (SSRIs), and serotonin norepinephrine reuptake inhibitors (SNRIs) for signs of bleeding [ see Warnings and Precautions (5.11) ]. Aspirin Clinical Impact: Controlled clinical studies showed that the concomitant use of NSAIDs and analgesic doses of aspirin does not produce any greater therapeutic effect than the use of NSAIDs alone. In a clinical study, the concomitant use of an NSAID and aspirin was associated with a significantly increased incidence of GI adverse reactions as compared to use of the NSAID alone [ see Warnings and Precautions (5.2) ]. Intervention: Concomitant use of Fenoprofen and analgesic doses of aspirin is not generally recommended because of the increased risk of bleeding [ see Warnings and Precautions (5.11) ].
Fenoprofen is not a substitute for low dose aspirin for cardiovascular protection.
ACE Inhibitors, Angiotensin Receptor Blockers, and Beta-Blockers Clinical Impact: - NSAIDs may diminish the antihypertensive effect of angiotensin converting enzyme (ACE) inhibitors, angiotensin receptor blockers (ARBs), or beta-blockers (including propranolol).
- In patients who are elderly, volume-depleted (including those on diuretic therapy), or have renal impairment, co-administration of an NSAID with ACE inhibitors or ARBs may result in deterioration of renal function, including possible acute renal failure. These effects are usually reversible.
Intervention: - During concomitant use of Fenoprofen and ACE-inhibitors, ARBs, or betablockers, monitor blood pressure to ensure that the desired blood pressure is obtained.
- During concomitant use of Fenoprofen ACE-inhibitors or ARBs in patients who are elderly, volume-depleted, or have impaired renal function, monitor for signs of worsening renal function [ see Warnings and Precautions (5.6) ].
- When these drugs are administered concomitantly, patients should be adequately hydrated. Assess renal function at the beginning of the concomitant treatment and periodically thereafter.
Diuretics Clinical Impact: Clinical studies, as well as post-marketing observations, showed that NSAIDs reduced the natriuretic effect of loop diuretics (e.g., furosemide) and thiazide diuretics in some patients. This effect has been attributed to the NSAID inhibition of renal prostaglandin synthesis. Intervention: During concomitant use of Fenoprofen with diuretics, observe patients for signs of worsening renal function, in addition to assuring diuretic efficacy including antihypertensive effects [ see Warnings and Precautions (5.6) ]. Digoxin Clinical Impact: The concomitant use of fenoprofen with digoxin has been reported to increase the serum concentration and prolong the half-life of digoxin. Intervention: During concomitant use of Fenoprofen and digoxin, monitor serum digoxin levels. Lithium Clinical Impact: NSAIDs have produced elevations in plasma lithium levels and reductions in renal lithium clearance. The mean minimum lithium concentration increased 15%, and the renal clearance decreased by approximately 20%. This effect has been attributed to NSAID inhibition of renal prostaglandin synthesis. Intervention: During concomitant use of Fenoprofen and lithium, monitor patients for signs of lithium toxicity. Methotrexate Clinical Impact: Concomitant use of NSAIDs and methotrexate may increase the risk for methotrexate toxicity (e.g., neutropenia, thrombocytopenia, renal dysfunction). Intervention: During concomitant use of Fenoprofen and methotrexate, monitor patients for methotrexate toxicity. Cyclosporine Clinical Impact: Concomitant use of Fenoprofen and cyclosporine may increase cyclosporine’s nephrotoxicity. Intervention: During concomitant use of Fenoprofen and cyclosporine, monitor patients for signs of worsening renal function. NSAIDs and Salicylates Clinical Impact: Concomitant use of fenoprofen with other NSAIDs or salicylates (e.g., diflunisal, salsalate) increases the risk of GI toxicity, with little or no increase in efficacy [ see Warnings and Precautions (5.2) ]. Intervention: The concomitant use of fenoprofen with other NSAIDs or salicylates is not recommended. Pemetrexed Clinical Impact: Concomitant use of Fenoprofen and pemetrexed may increase the risk of pemetrexed-associated myelosuppression, renal, and GI toxicity (see the pemetrexed prescribing information). Intervention: During concomitant use of Fenoprofen and pemetrexed, in patients with renal impairment whose creatinine clearance ranges from 45 to 79 mL/min, monitor for myelosuppression, renal and GI toxicity.
NSAIDs with short elimination half-lives (e.g., diclofenac, indomethacin) should be avoided for a period of two days before, the day of, and two days following administration of pemetrexed.
In the absence of data regarding potential interaction between pemetrexed and NSAIDs with longer half-lives (e.g., meloxicam, nabumetone), patients taking these NSAIDs should interrupt dosing for at least five days before, the day of, and two days following pemetrexed administration.
Phenobarbital Clinical Impact: Chronic administration of phenobarbital, a known enzyme inducer, may be associated with a decrease in the plasma half-life of fenoprofen. Intervention: When phenobarbital is added to or withdrawn from treatment, dosage adjustment of Fenoprofen may be required. Hydantoins, sulfonamides, or sulfonylureas Clinical Impact: In vitro studies have shown that fenoprofen, because of its affinity for albumin, may displace from their binding sites other drugs that are also albumin bound, and this may lead to drug interactions. Theoretically, fenoprofen could likewise be displaced. Intervention: Patients receiving hydantoins, sulfonamides, or sulfonylureas should be observed for increased activity of these drugs and, therefore, signs of toxicity from these drugs. Drug/Laboratory Test Interactions
Amerlex-M kit assay values of total and free triiodothyronine in patients receiving Fenoprofen Calcium have been reported as falsely elevated on the basis of a chemical cross-reaction that directly interferes with the assay. Thyroid-stimulating hormone, total thyroxine, and thyrotropin-releasing hormone response are not affected. Thus, results of the Amerlex-M kit assay should be interpreted with caution in these patients.
-
8. USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Risk Summary
Use of NSAIDs, including Fenoprofen, during the third trimester of pregnancy increases the risk of premature closure of the fetal ductus arteriosus. Avoid use of NSAIDs, including Fenoprofen, in pregnant women starting at 30 weeks of gestation (third trimester).There are no adequate and well-controlled studies of Fenoprofen in pregnant women. Data from observational studies regarding potential embryofetal risks of NSAID use in women in the first or second trimesters of pregnancy are inconclusive. In the general U.S. population, all clinically recognized pregnancies, regardless of drug exposure, have a background rate of 2-4% for major malformations, and 15-20% for pregnancy loss.
In animal reproduction studies, embryo-fetal lethality and skeletal abnormalities were noted in offspring of pregnant rabbits following oral administration of fenoprofen during organogenesis at 0.6 times the maximum human daily dose of 3200 mg/day. However, there were no major malformations noted following oral administration of fenoprofen calcium to pregnant rats and rabbits during organogenesis at exposures up to 0.3 and 0.6 times the maximum human daily dose of 3200 mg/day.
Based on animal data, prostaglandins have been shown to have an important role in endometrial vascular permeability, blastocyst implantation, and decidualization. In animal studies, administration of prostaglandin synthesis inhibitors such as fenoprofen, resulted in increased pre- and post-implantation loss.
Clinical Considerations
Labor or Delivery
There are no studies on the effects of Fenoprofen during labor or delivery. In animal studies, NSAIDS, including fenoprofen, inhibit prostaglandin synthesis, cause delayed parturition, and increase the incidence of stillbirth.Data
Human Data
There are no adequate and well-controlled studies of Fenoprofen in pregnant women. Data from observational studies regarding potential embryofetal risks of NSAID use in women in the first or second trimesters of pregnancy are inconclusive.Animal data
Pregnant rats were treated with fenoprofen using oral doses of 50 or 100 mg/kg (0.15 times and 0.3 times the maximum human daily dose (MHDD) of 3200 mg/day based on body surface area comparison) during the period of organogenesis. No major malformations were noted and there was no evidence of maternal toxicity at these doses, however, the exposures were below the exposures that will occur in humans.Pregnant rabbits were treated with fenoprofen using oral doses of 50 or 100 mg/kg (0.3 times and 0.6 times the MHDD of 3200 mg/day based on body surface area comparison) during the period of organogenesis. Maternal toxicity (mortality) was noted in the high dose animals. Although no major malformations were noted, there was an increased incidence of embryo-fetal lethality and skeletal abnormalities were present at 0.6 times the MHDD.
Pregnant rats were treated from Gestation Day 14 through Post-Natal Day 20 with oral doses of fenoprofen of 6.25, 12.5, 25, 50, or 100 mg/kg (0.02, 0.04, 0.08, 0.15, or 0.3 times the MDD of 3200 mg/day based on body surface area comparison). All doses produced significant toxicity, including vaginal bleeding, prolonged parturition, increased stillbirths, and maternal deaths.
Pregnant rats were treated from Gestation Day 6 through Gestation Day 19 and Post Partum Day 1 to 20 (excluding parturition) with an oral dose of fenoprofen of 100 mg/kg (0.3 times the MDD of 3200 mg/day based on body surface area comparison) demonstrated only a small increase in the incidence of impaired parturition despite the presence of maternal toxicity (gastrointestinal ulceration and renal toxicity).
8.2 Lactation
Risk Summary
In a published study, after a dose of 600 mg every 6 hours for 4 days in postpartum mothers, breastmilk fenoprofen levels were reportedly 1.6% of those in maternal plasma. The developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for FENOPROFEN CALCIUM and any potential adverse effects on the breastfed infant from the FENOPROFEN CALCIUM or from the underlying maternal condition.8.3 Females and Males of Reproductive Potential
Infertility
Females
Based on the mechanism of action, the use of prostaglandin-mediated NSAIDs, including FENOPROFEN CALCIUM, may delay or prevent rupture of ovarian follicles, which has been associated with reversible infertility in some women. Published animal studies have shown that administration of prostaglandin synthesis inhibitors has the potential to disrupt prostaglandinmediated follicular rupture required for ovulation. Small studies in women treated with NSAIDs have also shown a reversible delay in ovulation. Consider withdrawal of NSAIDs, including FENOPROFEN CALCIUM, in women who have difficulties conceiving or who are undergoing investigation of infertility.8.4 Pediatric Use
Safety and effectiveness in pediatric patients under the age of 18 have not been established.
8.5 Geriatric Use
Elderly patients, compared to younger patients, are at greater risk for NSAID-associated serious cardiovascular, gastrointestinal, and/or renal adverse reactions. If the anticipated benefit for the elderly patient outweighs these potential risks, start dosing at the low end of the dosing range, and monitor patients for adverse effects [ see Warnings and Precautions (5.1, 5.2, 5.3, 5.6, 5.13) ].
-
10. OVERDOSAGE
Symptoms following acute NSAID overdosages have been typically limited to lethargy, drowsiness, nausea, vomiting, and epigastric pain, which have been generally reversible with supportive care. Gastrointestinal bleeding has occurred. Hypertension, acute renal failure, respiratory depression, and coma have occurred, but were rare [ see Warnings and Precautions (5.1, 5.2, 5.4, 5.6) ].
Manage patients with symptomatic and supportive care following an NSAID overdosage. There are no specific antidotes. Consider emesis and/or activated charcoal (60 to 100 grams in adults, 1 to 2 grams per kg of body weight in pediatric patients) and/or osmotic cathartic in symptomatic patients seen within four hours of ingestion or in patients with a large overdosage (5 to 10 times the recommended dosage). Forced diuresis, alkalinization of urine, hemodialysis, or hemoperfusion may not be useful due to high protein binding.
For additional information about overdosage treatment contact a poison control center (1-800-222-1222).
-
11. DESCRIPTION
Fenoprofen (fenoprofen calcium, USP) capsules is a nonsteroidal, anti-inflammatory drug available in 200 mg and 400 mg capsule form for oral administration.
The 200 mg capsule is opaque yellow No. 97 cap and opaque white body, imprinted with “RX681” on the cap and body.
The 400 mg capsule is opaque green cap and opaque blue body, imprinted with “NALFON 400 mg" on the cap and “EP 123” on the body.
The chemical name is Benzenaecetic acid, α-methyl-3-phenoxy-, calcium salt dihydrate, (±)-. The molecular weight is 558.65. Its molecular formula is C30H26CaO62H2O, and it has the following chemical structure.
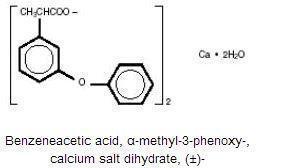
Fenoprofen Calcium is an arylacetic acid derivative. It is a white crystalline powder. At 25°C, it dissolves to a 15 mg/mL solution in alcohol (95%). It is slightly soluble in water and insoluble in benzene.The pKa of fenoprofen calcium is 4.5 at 25°C.
Fenoprofen capsules contain fenoprofen calcium as the dihydrate in an amount equivalent to 200 mg (0.826 mmol) or 400 mg (1.65 mmol) of fenoprofen.
Inactive ingredients in Fenoprofen capsules are crospovidone, magnesium stearate, sodium lauryl sulfate, and talc. In addition, the 200 mg capsules contain gelatin, titanium dioxide, yellow iron oxide, and red iron oxide, and the 400 mg capsules contain gelatin, D&C Yellow #10, FD&C Blue #1, FD&C Red #40, FD&C Yellow #6, and titanium dioxide.
-
12. CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Fernoprofen has analgesic, anti-inflammatory, and antipyretic properties.
The mechanism of action of Fenoprofen, like that of other NSAIDs, is not completely understood but involves inhibition of cyclooxygenase (COX-1 and COX-2).
Fenoprofen is a potent inhibitor of prostaglandin synthesis in vitro. Fenoprofen concentrations reached during therapy have produced in vivo effects. Prostaglandins sensitize afferent nerves and potentiate the action of bradykinin in inducing pain in animal models. Prostaglandins are mediators of inflammation. Because fenoprofen is an inhibitor of prostaglandin synthesis, its mode of action may be due to a decrease of prostaglandins in peripheral tissues.
12.3 Pharmacokinetics
Absorption
Under fasting conditions, fenoprofen is rapidly absorbed, and peak plasma levels of 50 mcg/L are achieved within 2 hours after oral administration of 600 mg doses. Good dose proportionality was observed between 200 and 600 mg doses in fasting male volunteers.Distribution
Fenoprofen is highly bound (99%) to albumin.Elimination
Metabolism
The plasma half-life is approximately 3 hours.Excretion
About 90% of a single oral dose is eliminated within 24 hours as fenoprofen glucuronide and 4'-hydroxyfenoprofen glucuronide, the major urinary metabolites of fenoprofen.Specific Populations
Gertatrics
Peak plasma levels of fenoprofen in normal elderly volunteers were similar to those observed in normal young volunteers. Elderly volunteers had a mean plasma clearance of 2.2 L/hour while plasma clearance of fenoprofen in normal young volunteers ranged from 3 to 3.5 L/hour. The overall elimination rate constant, plasma half-life and ratio of renal to nonrenal clearance of fenoprofen was the same in elderly and young volunteers. The 30 to 60% decrease in plasma clearance is due to a decrease in the volume of distribution in the body.Drug Interaction Studies
Aspirin: When NSAIDs were administered with aspirin, the protein binding of NSAIDs were reduced, although the clearance of free NSAID was not altered. The clinical significance of this interaction is not known. See Table 1 for clinically significant drug interactions of NSAIDs with aspirin [ see Drug Interactions (7) ].Antacid: The concomitant administration of antacid (containing both aluminum and magnesium hydroxide) does not interfere with absorption of fenoprofen.
-
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, and Impairment of Fertility
Carcinogenesis
Long-term studies in animals to evaluate the carcinogenic potential of fenoprofen have not been conducted.Mutagenesis
Studies to evaluate the genotoxic potential of fenoprofen have not been conducted.Impairment of Fertility
Female and Male rats were treated with 60 to 70 mg/kg/day or 120 to 150 mg/kg/day fenoprofen calcium via the diet (approximately 0.2 or 0.4 times the maximum human daily dose of 3200 mg/day based on body surface area comparison, respectively). Male rats were treated from 77 days prior to mating and during mating. Female rats were treated from 14 days prior to mating and through gestation. Pregnancy rates were slightly reduced in the low and high dose groups compared to controls. There was no adverse effect on implantations, resorptions, or live fetuses. -
14. CLINICAL STUDIES
Fenoprofen is a nonsteroidal, anti-inflammatory, antiarthritic drug that also possesses analgesic and antipyretic activities. Its exact mode of action is unknown, but it is thought that prostaglandin synthetase inhibition is involved.
Results in humans demonstrate that fenoprofen has both anti-inflammatory and analgesic actions. The emergence and degree of erythemic response were measured in adult male volunteers exposed to ultraviolet irradiation. The effects of Fenoprofen, aspirin, and indomethacin were each compared with those of a placebo. All 3 drugs demonstrated antierythemic activity.
In all patients with rheumatoid arthritis, the anti-inflammatory action of Fenoprofen has been evidenced by relief of pain, increase in grip strength, and reductions in joint swelling, duration of morning stiffness, and disease activity (as assessed by both the investigator and the patient). The anti-inflammatory action of Fenoprofen has also been evidenced by increased mobility (i.e., a decrease in the number of joints having limited motion).
The use of Fenoprofen in combination with gold salts or corticosteroids has been studied in patients with rheumatoid arthritis. The studies, however, were inadequate in demonstrating whether further improvement is obtained by adding Fenoprofen to maintenance therapy with gold salts or steroids. Whether or not Fenoprofen used in conjunction with partially effective doses of a corticosteroid has a “steroid-sparing” effect is unknown.
In patients with osteoarthritis, the anti-inflammatory and analgesic effects of Fenoprofen have been demonstrated by reduction in tenderness as a response to pressure and reductions in night pain, stiffness, swelling, and overall disease activity (as assessed by both the patient and the investigator). These effects have also been demonstrated by relief of pain with motion and at rest and increased range of motion in involved joints.
In patients with rheumatoid arthritis and osteoarthritis, clinical studies have shown Fenoprofen to be comparable to aspirin in controlling the aforementioned measures of disease activity, but mild gastrointestinal reactions (nausea, dyspepsia) and tinnitus occurred less frequently in patients treated with Fenoprofen than in aspirin-treated patients. It is not known whether Fenoprofen causes less peptic ulceration than does aspirin.
In patients with pain, the analgesic action of Fenoprofen calcium has produced a reduction in pain intensity, an increase in pain relief, improvement in total analgesia scores, and a sustained analgesic effect.
-
16. HOW SUPPLIED/STORAGE AND HANDLING
Fenoprofen® (fenoprofen calcium, USP) are available in capsule form for oral administration, and are supplied as following:
● The 200 mg capsule has an opaque yellow No. 97 cap and an opaque white body, imprinted with "RX681" on the cap and body. NDC NDC: 62250-691-02 Bottles of 100.
Storage:
Store at room temperature 20°C to 25°C (68°F to 77°F); excursions permitted between 15°C to 30°C (59°F to 86°F) [see USP Controlled Room Temperature].
Preserve in well-closed containers -
17. PATIENT COUNSELING INFORMATION
Advise the patient to read the FDA-approved patient labeling (Medication Guide) that accompanies each prescription dispensed. Inform patients, families, or their caregivers of the following information before initiating therapy with Fenoprofen and periodically during the course of ongoing therapy.
Cardiovascular Thrombotic Events
Advise patients to be alert for the symptoms of cardiovascular thrombotic events, including chest pain, shortness of breath, weakness, or slurring of speech, and to report any of these symptoms to their health care provider immediately [ see Warnings and Precautions (5.1) ].
Gastrointestinal Bleeding, Ulceration, and Perforation
Advise patients to report symptoms of ulcerations and bleeding, including epigastric pain, dyspepsia, melena, and hematemesis to their health care provider. In the setting of concomitant use of low-dose aspirin for cardiac prophylaxis, inform patients of the increased risk for and the signs and symptoms of GI bleeding [ see Warnings and Precautions ( 5.2) ].Hepatotoxicity
Inform patients of the warning signs and symptoms of hepatotoxicity (e.g., nausea, fatigue, lethargy, pruritus, diarrhea, jaundice, right upper quadrant tenderness, and “flu-like” symptoms). If these occur, instruct patients to stop Fenoprofen and seek immediate medical therapy [ see Warnings and Precautions (5.3) ].Heart Failure and Edema
Advise patients to be alert for the symptoms of congestive heart failure including shortness of breath, unexplained weight gain, or edema and to contact their healthcare provider if such symptoms occur [ see Warnings and Precautions (5.5) ].Anaphylactic Reactions
Inform patients of the signs of an anaphylactic reaction (e.g., difficulty breathing, swelling of the face or throat). Instruct patients to seek immediate emergency help if these occur [ see Contraindications (4) and Warnings and Precautions (5.7) ].Serious Skin Reactions
Advise patients to stop Fenoprofen immediately if they develop any type of rash and to contact their healthcare provider as soon as possible [ see Warnings and Precautions (5.9) ].Female Fertility
Advise females of reproductive potential who desire pregnancy that NSAIDs, including Fenoprofen, may be associated with a reversible delay in ovulation [ see Use in Specific Populations (8.3) ]Fetal Toxicity
Inform pregnant women to avoid use of Fenoprofen and other NSAIDs starting at 30 weeks gestation because of the risk of the premature closing of the fetal ductus arteriosus [ see Warnings and Precautions (5.10) and Use in Specific Populations (8.1) ].Avoid Concomitant Use of NSAIDs
Inform patients that the concomitant use of Fenoprofen with other NSAIDs or salicylates (e.g., diflunisal, salsalate) is not recommended due to the increased risk of gastrointestinal toxicity, and little or no increase in efficacy [ see Warnings and Precautions (5.2) and Drug Interactions (7) ]. Alert patients that NSAIDs may be present in “over the counter” medications for treatment of colds, fever, or insomnia.Use of NSAIDS and Low-Dose Aspirin
Inform patients not to use low-dose aspirin concomitantly with Fenoprofen until they talk to their healthcare provider [ see Drug Interactions (7) ]. -
Medication Guide for Non-Steroidal Anti-Inflammatory Drugs (NSAIDs)
What is the most important information I should know about medicines called Nonsteroidal Antiinflammatory Drugs (NSAIDs)?
NSAIDs can cause serious side effects, including:
-
Increased risk of a heart attack or stroke that can lead to death. This risk may happen early in treatment and may increase:
- with increasing doses of NSAIDs
- with longer use of NSAIDs
Do not take NSAIDs right before or after a heart surgery called a “coronary artery bypass graft (CABG)."
Avoid taking NSAIDs after a recent heart attack, unless your healthcare provider tells you to. You may have an increased risk of another heart attack if you take NSAIDs after a recent heart attack
-
Increased risk of bleeding, ulcers, and tears (perforation) of the esophagus (tube leading from the mouth to the stomach), stomach and intestines:
- anytime during use
- without warning symptoms
- that may cause death
The risk of getting an ulcer or bleeding increases with:
-
- past history of stomach ulcers, or stomach or intestinal bleeding with use of NSAIDs
- taking medicines called “corticosteroids”, “anticoagulants”, “SSRIs”, or “SNRIs”
- increasing doses of NSAIDs
- longer use of NSAIDs
- smoking
- drinking alcohol
- older age
- poor health
- advanced liver disease
- bleeding problems
NSAIDs should only be used:
-
- exactly as prescribed
- at the lowest dose possible for your treatment
- for the shortest time needed
What are NSAIDs?
NSAIDs are used to treat pain and redness, swelling, and heat (inflammation) from medical conditions such as different types of arthritis, menstrual cramps, and other types of short-term pain.
Who should not take NSAIDs?
Do not take NSAIDs:
- if you have had an asthma attack, hives, or other allergic reaction with aspirin or any other NSAIDs
- right before or after heart bypass surgery.
Before taking NSAIDS, tell your healthcare provider about all of your medical conditions, including if you:
- have liver or kidney problems
- have high blood pressure
- have asthma
- are pregnant or plan to become pregnant. Talk to your healthcare provivder if you are considering taking NSAIDs during pregnancy. You should not take NSAIDs after 29 weeks of pregnancy.
- are breastfeeding or plan to breast feed.
Tell your healthcare provider about all of the medicines you take, including prescription or over-the-counter medicines, vitamins or herbal supplements. NSAIDs and some other medicines can interact with each other and cause serious side effects. Do not start taking any new medicine without talking to your healthcare provider first.
What are the possible side effects of NSAIDs?
NSAIDs can cause serious side effects, including:
See “What is the most important information I should know about medicines called Nonsteroidal Anti-inflammatory Drugs (NSAIDs)?"
- new or worse high blood pressure
- heart failure
- liver problems including liver failure
- kidney problems including kidney failure
- low red blood cells (anemia)
- life-threatening skin reactions
- life-threatening allergic reactions
- Other side effects of NSAIDs include: stomach pain, constipation, diarrhea, gas, heartburn, nausea, vomiting, and dizziness
Get emergency help right away if you get any of the following symptoms:
- shortness of breath or trouble breathing
- chest pain
- weakness in one part or side of your body
- slurred speech
- swelling of the face or throat
Stop taking your NSAID and call your healthcare provider right away if you get any of the following symptoms:
- nausea
- more tired or weaker than usual
- diarrhea
- itching
- your skin or eyes look yellow
- indigestion or stomach pain
- flu-like symptoms
- vomit blood
- there is blood in your bowel movement or it is black and sticky like tar
- unusual weight gain
- skin rash or blisters with fever
- swelling of the arms, legs, hands and feet
If you take too much of your NSAID, call your healthcare provider or get medical help right away. These are not all the possible side effects of NSAIDs. For more information, ask your healthcare provider or pharmacist about NSAIDs.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
Other information about NSAIDs
- Aspirin is an NSAID but it does not increase the chance of a heart attack. Aspirin can cause bleeding in the brain, stomach, and intestines. Aspirin can also cause ulcers in the stomach and intestines.
- Some NSAIDs are sold in lower doses without a prescription (over-the counter). Talk to your healthcare provider before using over-the-counter NSAIDs for more than 10 days.
General information about the safe and effective use of NSAIDs
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use NSAIDs for a condition for which it was not prescribed. Do not give NSAIDs to other people, even if they have the same symptoms that you have. It may harm them.
If you would like more information about NSAIDs, talk with your healthcare provider. You can ask your pharmacist or healthcare provider for information about NSAIDs that is written for health professionals.
Manufactured for:
Belcher Pharmaceuticals, LLC
Largo, FL 33777
This Medication Guide has been approved by the U.S. Food and Drug Administration.
Issued: 04/ 2016 -
Increased risk of a heart attack or stroke that can lead to death. This risk may happen early in treatment and may increase:
-
PRINCIPAL DISPLAY PANEL
PRINCIPAL DISPLAY PANEL - 200 mg
NDC: 62250-691-02Fenoprofen® (fenoprofen calcium, USP)
200 mg

Manufactured for:
Belcher Pharmaceuticals, LLCLargo, FL 33777
100 capsules
-
INGREDIENTS AND APPEARANCE
FENOPROFEN
fenoprofen calcium capsuleProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 62250-691 Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength FENOPROFEN CALCIUM (UNII: 0X2CW1QABJ) (FENOPROFEN - UNII:RA33EAC7KY) FENOPROFEN 200 mg Inactive Ingredients Ingredient Name Strength CROSPOVIDONE (UNII: 2S7830E561) MAGNESIUM STEARATE (UNII: 70097M6I30) SODIUM LAURYL SULFATE (UNII: 368GB5141J) TALC (UNII: 7SEV7J4R1U) GELATIN (UNII: 2G86QN327L) TITANIUM DIOXIDE (UNII: 15FIX9V2JP) BROWN IRON OXIDE (UNII: 1N032N7MFO) Product Characteristics Color yellow (opaque) , white (opaque) Score no score Shape CAPSULE Size 23mm Flavor Imprint Code RX681 Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 62250-691-02 100 in 1 BOTTLE; Type 0: Not a Combination Product 04/19/2017 Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date NDA NDA017604 04/19/2017 Labeler - Belcher Pharmaceuticals,LLC (965082543)
© 2026 FDA.report
This site is not affiliated with or endorsed by the FDA.