Estradiol by Amneal Pharmaceuticals of New York LLC / Amneal Pharmaceuticals of New York, LLC ESTRADIOL insert
Estradiol by
Drug Labeling and Warnings
Estradiol by is a Prescription medication manufactured, distributed, or labeled by Amneal Pharmaceuticals of New York LLC, Amneal Pharmaceuticals of New York, LLC. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
-
HIGHLIGHTS OF PRESCRIBING INFORMATION
These highlights do not include all the information needed to use ESTRADIOL VAGINAL INSERTS safely and effectively. See full prescribing information for ESTRADIOL VAGINAL INSERTS.
ESTRADIOL vaginal inserts
Initial U.S. Approval: 1999WARNING: ENDOMETRIAL CANCER, CARDIOVASCULAR DISORDERS, BREAST CANCER and PROBABLE DEMENTIA
See full prescribing information for complete boxed warning
Estrogen-Alone Therapy
- There is an increased risk of endometrial cancer in a woman with a uterus who uses unopposed estrogens (5.3)
- Estrogen-alone therapy should not be used for the prevention of cardiovascular disease or dementia (5.2,5.4)
- The Women’s Health Initiative (WHI) estrogen-alone substudy reported increased risks of stroke and deep vein thrombosis (DVT) (5.2)
- The WHI Memory Study (WHIMS) estrogen-alone ancillary study of WHI reported an increased risk of probable dementia in postmenopausal women 65 years of age and older (5.4)
Estrogen Plus Progestin Therapy
- Estrogen plus progestin therapy should not be used for the prevention of cardiovascular disease or dementia (5.2,5.4)
- The WHI estrogen plus progestin substudy reported increased risks of stroke, DVT, pulmonary embolism (PE) and myocardial infarction (MI) (5.2)
- The WHI estrogen plus progestin substudy reported increased risks of invasive breast cancer (5.3)
- The WHIMS estrogen plus progestin ancillary study of WHI reported an increased risk of probable dementia in postmenopausal women 65 years of age and older (5.4)
INDICATIONS AND USAGE
- Estradiol vaginal inserts are an estrogen (estradiol) indicated for the treatment of atrophic vaginitis due to menopause (1.1)
DOSAGE AND ADMINISTRATION
Estradiol vaginal inserts should be administered intravaginally:
- 1 insert daily for 2 weeks, followed by 1 insert twice weekly (for example, Tuesday and Friday) (2.1)
DOSAGE FORMS AND STRENGTHS
- Estradiol vaginal inserts, USP: One vaginal insert contains 10.3 mcg of estradiol hemihydrate equivalent to 10 mcg of estradiol, USP (3)
CONTRAINDICATIONS
- Undiagnosed abnormal genital bleeding (4)
- Known, suspected, or history of breast cancer (4,5.3)
- Known or suspected estrogen-dependent neoplasia (4,5.3)
- Active DVT, PE, or history of these conditions (4,5.2)
- Active arterial thromboembolic disease (for example, stroke and MI), or a history of these conditions (4,5.2)
- Known anaphylactic reaction or angioedema to estradiol
- Known liver impairment or disease (4,5.11)
- Known protein C, protein S, or antithrombin deficient, or other known thrombophilic disorders (4)
- Known or suspected pregnancy (4,8.1)
WARNINGS AND PRECAUTIONS
- Estrogens increase the risk of gallbladder disease (5.5)
- Discontinue estrogen if severe hypercalcemia, loss of vision, severe hypertriglyceridemia or cholestatic jaundice occurs (5.6,5.7,5.10,5.11)
- The estradiol vaginal inserts applicator may cause vaginal abrasion (5.17)
- Monitor thyroid function in women on thyroid replacement therapy (5.12,5.19)
ADVERSE REACTIONS
In a prospective, randomized, placebo-controlled, double-blind study the most common adverse reactions (incidence ≥5 percent) were back pain, vulvovaginal pruritus, vulvovaginal mycotic infection and diarrhea. (6.1)
To report SUSPECTED ADVERSE REACTIONS, contact Amneal Pharmaceuticals at 1-877-835-5472 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
DRUG INTERACTIONS
- Inducers and inhibitors of CYP3A4 may affect estrogen drug metabolism (7.1)
USE IN SPECIFIC POPULATIONS
- Nursing Mothers: Estrogen administration to nursing women has been shown to decrease the quantity and quality of breast milk (8.3)
- Geriatric Use: An increased risk of probable dementia in women over 65 years of age was reported in the Women’s Health Initiative Memory ancillary studies of the Women’s Health Initiative (8.5)
See 17 for PATIENT COUNSELING INFORMATION and FDA-approved patient labeling.
Revised: 4/2019
-
Table of Contents
FULL PRESCRIBING INFORMATION: CONTENTS*
WARNING: ENDOMETRIAL CANCER, CARDIOVASCULAR DISORDERS, BREAST CANCER and PROBABLE DEMENTIA
1 INDICATIONS AND USAGE
1.1 Treatment of Atrophic Vaginitis due to Menopause
2 DOSAGE AND ADMINISTRATION
2.1 Treatment of Atrophic Vaginitis due to Menopause
3 DOSAGE FORMS AND STRENGTHS
4 CONTRAINDICATIONS
5 WARNINGS AND PRECAUTIONS
5.1 Risks from Systemic Absorption
5.2 Cardiovascular Disorders
5.3 Malignant Neoplasms
5.4 Probable Dementia
5.5 Gallbladder Disease
5.6 Hypercalcemia
5.7 Visual Abnormalities
5.8 Addition of a Progestin When a Woman Has Not Had a Hysterectomy
5.9 Elevated Blood Pressure
5.10 Hypertriglyceridemia
5.11 Hepatic Impairment and/or Past History of Cholestatic Jaundice
5.12 Hypothyroidism
5.13 Fluid Retention
5.14 Hypocalcemia
5.15 Exacerbation of Endometriosis
5.16 Hereditary Angioedema
5.17 Exacerbation of Other Conditions
5.18 Local Abrasion
5.19 Laboratory Tests
5.20 Drug-Laboratory Test Interactions
6 ADVERSE REACTIONS
6.1 Clinical Trials Experience
6.2 Postmarketing Experience
7 DRUG INTERACTIONS
7.1 Metabolic Interactions
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
8.3 Nursing Mothers
8.4 Pediatric Use
8.5 Geriatric Use
8.6 Renal Impairment
8.7 Hepatic Impairment
10 OVERDOSAGE
11 DESCRIPTION
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
12.2 Pharmacodynamics
12.3 Pharmacokinetics
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
14 CLINICAL STUDIES
14.1 Effects on Atrophic Vaginitis
14.2 Women’s Health Initiative Studies
14.3 Women’s Health Initiative Memory Study
15 REFERENCES
16 HOW SUPPLIED/STORAGE AND HANDLING
16.1 How Supplied
16.2 Storage and Handling
17 PATIENT COUNSELING INFORMATION
17.1 Vaginal Bleeding
17.2 Possible Serious Adverse Reactions with Estrogen-Alone Therapy
17.3 Possible Less Serious but Common Adverse Reactions with Estrogen-Alone Therapy
17.4 Instructions for Use of Applicator
- * Sections or subsections omitted from the full prescribing information are not listed.
-
BOXED WARNING
(What is this?)
WARNING: ENDOMETRIAL CANCER, CARDIOVASCULAR DISORDERS, BREAST CANCER and PROBABLE DEMENTIA
Estrogen-Alone Therapy
Endometrial Cancer
There is an increased risk of endometrial cancer in a woman with a uterus who uses unopposed estrogens. Adding a progestin to estrogen therapy has been shown to reduce the risk of endometrial hyperplasia, which may be a precursor to endometrial cancer. Adequate diagnostic measures, including directed or random endometrial sampling when indicated, should be undertaken to rule out malignancy in postmenopausal women with undiagnosed persistent or recurring abnormal genital bleeding [see Warnings and Precautions (5.3)].
Cardiovascular Disorders and Probable Dementia
Estrogen-alone therapy should not be used for the prevention of cardiovascular disease or dementia [see Warnings and Precautions (5.2,5.4) and Clinical Studies (14.2,14.3)].
The Women’s Health Initiative (WHI) estrogen-alone substudy reported increased risks of stroke and deep vein thrombosis (DVT) in postmenopausal women (50 to 79 years of age) during 7.1 years of treatment with daily oral conjugated estrogens (CE) [0.625 mg]-alone, relative to placebo [see Warnings and Precautions (5.2) and Clinical Studies (14.2)].
The WHI Memory Study (WHIMS) estrogen-alone ancillary study of WHI reported an increased risk of developing probable dementia in postmenopausal women 65 years of age or older during 5.2 years of treatment with daily CE (0.625 mg)-alone, relative to placebo. It is unknown whether this finding applies to younger postmenopausal women [see Warnings and Precautions (5.4), Use in Specific Populations (8.5) and Clinical Studies (14.3)].
In the absence of comparable data, these risks should be assumed to be similar for other doses of CE and other dosage forms of estrogens.
Estrogens with or without progestins should be prescribed at the lowest effective doses and for the shortest duration consistent with treatment goals and risks for the individual woman.
Estrogen Plus Progestin Therapy
Cardiovascular Disorders and Probable Dementia
Estrogen plus progestin therapy should not be used for the prevention of cardiovascular disease or dementia [see Warnings and Precautions (5.2,5.4) and Clinical Studies (14.2,14.3)].
The WHI estrogen plus progestin substudy reported increased risks of DVT, pulmonary embolism (PE), stroke and myocardial infarction (MI) in postmenopausal women (50 to 79 years of age) during 5.6 years of treatment with daily oral CE (0.625 mg) combined with medroxyprogesterone acetate (MPA) [2.5 mg], relative to placebo [see Warnings and Precautions (5.2) and Clinical Studies (14.2)].
The WHIMS estrogen plus progestin ancillary study of the WHI reported an increased risk of developing probable dementia in postmenopausal women 65 years of age or older during 4 years of treatment with daily CE (0.625 mg) combined with MPA (2.5 mg), relative to placebo. It is unknown whether this finding applies to younger postmenopausal women [see Warnings and Precautions (5.4), Use in Specific Populations (8.5) and Clinical Studies (14.3)].
Breast Cancer
The WHI estrogen plus progestin substudy also demonstrated an increased risk of invasive breast cancer [see Warnings and Precautions (5.3) and Clinical Studies (14.2)].
In the absence of comparable data, these risks should be assumed to be similar for other doses of CE and MPA, and other combinations and dosage forms of estrogens and progestins.
Estrogens with or without progestins should be prescribed at the lowest effective doses and for the shortest duration consistent with treatment goals and risks for the individual woman.
- 1 INDICATIONS AND USAGE
-
2 DOSAGE AND ADMINISTRATION
Generally, when estrogen is prescribed for a postmenopausal woman with a uterus, a progestin should also be considered to reduce the risk of endometrial cancer.
A woman without a uterus does not need a progestin. In some cases, however, hysterectomized women with a history of endometriosis may need a progestin [see Warnings and Precautions (5.3,5.15)].
Use of estrogen-alone, or in combination with a progestin, should be with the lowest effective dose and for the shortest duration consistent with treatment goals and risks for the individual woman. Postmenopausal women should be re-evaluated periodically as clinically appropriate to determine if treatment is still necessary.
- 3 DOSAGE FORMS AND STRENGTHS
-
4 CONTRAINDICATIONS
Estradiol should not be used in women with any of the following conditions:
- Undiagnosed abnormal genital bleeding
- Known, suspected, or history of breast cancer
- Known or suspected estrogen-dependent neoplasia
- Active DVT, PE, or history of these conditions
- Active arterial thromboembolic disease (for example, stroke and myocardial infarction), or a history of these conditions
- Known anaphylactic reaction or angioedema to estradiol
- Known liver impairment or disease
- Known protein C, protein S, or antithrombin deficiency, or other known thrombophilic disorders
- Known or suspected pregnancy
-
5 WARNINGS AND PRECAUTIONS
5.1 Risks from Systemic Absorption
Estradiol vaginal inserts are intended only for vaginal administration. Systemic absorption occurs with the use of estradiol vaginal inserts. The warnings, precautions and adverse reactions associated with the use of systemic estrogen-alone therapy should be taken into account.
5.2 Cardiovascular Disorders
An increased risk of stroke and DVT has been reported with estrogen-alone therapy. An increased risk of PE, DVT, stroke and MI has been reported with estrogen plus progestin therapy. Should any of these occur or be suspected, estrogen with or without progestin therapy should be discontinued immediately.
Risk factors for arterial vascular disease (for example, hypertension, diabetes mellitus, tobacco use, hypercholesterolemia and obesity) and/or venous thromboembolism (VTE) (for example, personal history or family history of VTE, obesity and systemic lupus erythematosus) should be managed appropriately.
Stroke
In the WHI estrogen-alone substudy, a statistically significant increased risk of stroke was reported in women 50 to 79 years of age receiving daily CE (0.625 mg)-alone compared to women in the same age group receiving placebo (45 versus 33 per 10,000 women-years). The increase in risk was demonstrated in year 1 and persisted [see Clinical Studies (14.2)]. Should a stroke occur or be suspected, estrogen-alone therapy should be discontinued immediately.
Subgroup analyses of women 50 to 59 years of age suggest no increased risk of stroke for those women receiving CE (0.625 mg)-alone versus those receiving placebo (18 versus 21 per 10,000 women-years).1
In the WHI estrogen plus progestin substudy, a statistically significant increased risk of stroke was reported in women 50 to 79 years of age receiving daily CE (0.625 mg) plus MPA (2.5 mg) compared to women in the same age group receiving placebo (33 versus 25 per 10,000 women-years) [see Clinical Studies (14.2)]. The increase in risk was demonstrated after the first year and persisted.1 Should a stroke occur or be suspected, estrogen plus progestin therapy should be discontinued immediately.
Coronary Heart Disease
In the WHI estrogen-alone substudy, no overall effect on coronary heart disease (CHD) events (defined as nonfatal MI, silent MI, or CHD death) was reported in women receiving estrogen-alone compared to placebo2[see Clinical Studies (14.2)].
Subgroup analysis of women 50 to 59 years of age suggests a statistically non-significant reduction in CHD events (CE [0.625 mg]-alone compared to placebo) in women with less than 10 years since menopause (8 versus 16 per 10,000 women-years).1
In the WHI estrogen plus progestin substudy, there was a statistically non-significant increased risk of CHD events reported in women receiving daily CE (0.625 mg) plus MPA (2.5 mg) compared to women receiving placebo (41 versus 34 per 10,000 women-years).1 An increase in relative risk was demonstrated in year 1, and a trend toward decreasing relative risk was reported in years 2 through 5 [see Clinical Studies (14.2)].
In postmenopausal women with documented heart disease (n=2,763), average 66.7 years of age, in a controlled clinical trial of secondary prevention of cardiovascular disease (Heart and Estrogen/Progestin Replacement Study [HERS]), treatment with daily CE (0.625 mg) plus MPA (2.5 mg) demonstrated no cardiovascular benefit. During an average follow-up of 4.1 years, treatment with CE plus MPA did not reduce the overall rate of CHD events in postmenopausal women with established coronary heart disease. There were more CHD events in the CE plus MPA-treated group than in the placebo group in year 1, but not during the subsequent years. Two thousand, three hundred and twenty-one (2,321) women from the original HERS trial agreed to participate in an open label extension of the original HERS, HERS II. Average follow-up in HERS II was an additional 2.7 years, for a total of 6.8 years overall. Rates of CHD events were comparable among women in the CE plus MPA group and the placebo group in HERS, HERS II, and overall.
Venous Thromboembolism
In the WHI estrogen-alone substudy, the risk of VTE (DVT and PE) was increased for women receiving daily CE (0.625 mg)-alone compared to placebo (30 versus 22 per 10,000 women-years), although only the increased risk of DVT reached statistical significance (23 versus 15 per 10,000 women-years). The increase in VTE risk was demonstrated during the first 2 years3[see Clinical Studies (14.2)]. Should a VTE occur or be suspected, estrogen-alone therapy should be discontinued immediately.
In the WHI estrogen plus progestin substudy, a statistically significant 2-fold greater rate of VTE was reported in women receiving daily CE (0.625 mg) plus MPA (2.5 mg) compared to women receiving placebo (35 versus 17 per 10,000 women-years). Statistically significant increases in risk for both DVT (26 versus 13 per 10,000 women-years) and PE (18 versus 8 per 10,000 women-years) were also demonstrated. The increase in VTE risk was demonstrated during the first year and persisted4[see Clinical Studies (14.2)]. Should a VTE occur or be suspected, estrogen plus progestin therapy should be discontinued immediately.
If feasible, estrogens should be discontinued at least 4 to 6 weeks before surgery of the type associated with an increased risk of thromboembolism, or during periods of prolonged immobilization.
5.3 Malignant Neoplasms
Endometrial Cancer
An increased risk of endometrial cancer has been reported with the use of unopposed estrogen therapy in a woman with a uterus. The reported endometrial cancer risk among unopposed estrogen users is about 2 to 12 times greater than in non-users, and appears dependent on duration of treatment and on estrogen dose. Most studies show no significant increased risk associated with use of estrogens for less than 1 year. The greatest risk appears associated with prolonged use, with an increased risk of 15- to 24-fold for 5 to 10 years or more and this risk has been shown to persist for at least 8 to 15 years after estrogen therapy is discontinued.
Clinical surveillance of all women using estrogen-alone or estrogen plus progestin therapy is important. Adequate diagnostic measures, including directed or random endometrial sampling when indicated, should be undertaken to rule out malignancy in postmenopausal women with undiagnosed persistent or recurring abnormal genital bleeding.
There is no evidence that the use of natural estrogens results in a different endometrial risk profile than synthetic estrogens of equivalent estrogen dose. Adding a progestin to estrogen therapy in postmenopausal women has been shown to reduce the risk of endometrial hyperplasia, which may be a precursor to endometrial cancer.
Breast Cancer
The most important randomized clinical trial providing information about breast cancer in estrogen-alone users is the WHI substudy of daily CE (0.625 mg)-alone. In the WHI estrogen-alone substudy, after an average follow-up of 7.1 years, daily CE-alone was not associated with an increased risk of invasive breast cancer [relative risk (RR) 0.80]5[see Clinical Studies (14.2)].
The most important randomized clinical trial providing information about breast cancer in estrogen plus progestin users is the WHI substudy of daily CE (0.625 mg) plus MPA (2.5 mg). After a mean follow-up of 5.6 years, the estrogen plus progestin substudy reported an increased risk of invasive breast cancer in women who took daily CE plus MPA. In this substudy, prior use of estrogen-alone or estrogen plus progestin therapy was reported by 26 percent of the women. The relative risk of invasive breast cancer was 1.24, and the absolute risk was 41 versus 33 cases per 10,000 women-years, for CE plus MPA compared with placebo. Among women who reported prior use of hormone therapy, the relative risk of invasive breast cancer was 1.86, and the absolute risk was 46 versus 25 cases per 10,000 women-years, for CE plus MPA compared with placebo. Among women who reported no prior use of hormone therapy, the relative risk of invasive breast cancer was 1.09, and the absolute risk was 40 versus 36 cases per 10,000 women-years for CE plus MPA compared with placebo. In the same substudy, invasive breast cancers were larger, were more likely to be node positive, and were diagnosed at a more advanced stage in the CE (0.625 mg) plus MPA (2.5 mg) group compared with the placebo group. Metastatic disease was rare, with no apparent difference between the two groups. Other prognostic factors, such as histologic subtype, grade and hormone receptor status did not differ between the groups6[see Clinical Studies (14.2)].
Consistent with the WHI clinical trial, observational studies have also reported an increased risk of breast cancer for estrogen plus progestin therapy, and a smaller increased risk for estrogen-alone therapy, after several years of use. The risk increased with duration of use, and appeared to return to baseline over about 5 years after stopping treatment (only the observational studies have substantial data on risk after stopping). Observational studies also suggest that the risk of breast cancer was greater, and became apparent earlier, with estrogen plus progestin therapy as compared to estrogen-alone therapy. However, these studies have not generally found significant variation in the risk of breast cancer among different estrogen plus progestin combinations, doses, or routes of administration.
The use of estrogen-alone and estrogen plus progestin therapy has been reported to result in an increase in abnormal mammograms requiring further evaluation.
All women should receive yearly breast examinations by a healthcare provider and perform monthly breast self-examinations. In addition, mammography examinations should be scheduled based on patient age, risk factors, and prior mammogram results.
Ovarian Cancer
The WHI estrogen plus progestin substudy reported a statistically non-significant increased risk of ovarian cancer. After an average follow-up of 5.6 years, the relative risk for ovarian cancer for CE plus MPA versus placebo was 1.58 (95 percent CI, 0.77 to 3.24). The absolute risk for CE plus MPA versus placebo was 4 versus 3 cases per 10,000 women-years.7
A meta-analysis of 17 prospective and 35 retrospective epidemiology studies found that women who used hormonal therapy for menopausal symptoms had an increased risk for ovarian cancer. The primary analysis, using case-control comparisons, included 12,110 cancer cases from the 17 prospective studies. The relative risks associated with current use of hormonal therapy was 1.41 (95% confidence interval [CI] 1.32 to 1.50); there was no difference in the risk estimates by duration of the exposure (less than 5 years [median of 3 years] vs. greater than 5 years [median of 10 years] of use before the cancer diagnosis). The relative risk associated with combined current and recent use (discontinued use within 5 years before cancer diagnosis) was 1.37 (95% CI 1.27 to 1.48), and the elevated risk was significant for both estrogen-alone and estrogen plus progestin products. The exact duration of hormone therapy use associated with an increased risk of ovarian cancer, however, is unknown.
5.4 Probable Dementia
In the WHIMS estrogen-alone ancillary study of WHI, a population of 2,947 hysterectomized women 65 to 79 years of age was randomized to daily CE (0.625 mg)-alone or placebo.
After an average follow-up of 5.2 years, 28 women in the estrogen-alone group and 19 women in the placebo group were diagnosed with probable dementia. The relative risk of probable dementia for CE-alone versus placebo was 1.49 (95 percent CI, 0.83 to 2.66). The absolute risk of probable dementia for CE-alone versus placebo was 37 versus 25 cases per 10,000 women-years8[see Use in Specific Populations (8.5) and Clinical Studies (14.3)].
In the WHIMS estrogen plus progestin ancillary study of WHI, a population of 4,532 postmenopausal women 65 to 79 years of age was randomized to daily CE (0.625 mg) plus MPA (2.5 mg) or placebo. After an average follow-up of 4 years, 40 women in the CE plus MPA group and 21 women in the placebo group were diagnosed with probable dementia. The relative risk of probable dementia for CE plus MPA versus placebo was 2.05 (95 percent CI, 1.21 to 3.48). The absolute risk of probable dementia for CE plus MPA versus placebo was 45 versus 22 cases per 10,000 women-years8[see Use in Specific Populations (8.5) and Clinical Studies (14.3)].
When data from the two populations in the WHIMS estrogen-alone and estrogen plus progestin ancillary studies were pooled as planned in the WHIMS protocol, the reported overall relative risk for probable dementia was 1.76 (95 percent CI, 1.19 to 2.60). Since both ancillary studies were conducted in women 65 to 79 years of age, it is unknown whether these findings apply to younger postmenopausal women8[see Use in Specific Populations (8.5) and Clinical Studies (14.3)].
5.5 Gallbladder Disease
A 2- to 4-fold increase in the risk of gallbladder disease requiring surgery in postmenopausal women receiving estrogens has been reported.
5.6 Hypercalcemia
Estrogen administration may lead to severe hypercalcemia in women with breast cancer and bone metastases. If hypercalcemia occurs, use of the drug should be stopped and appropriate measures taken to reduce the serum calcium level.
5.7 Visual Abnormalities
Retinal vascular thrombosis has been reported in women receiving estrogens. Discontinue medication pending examination if there is a sudden partial or complete loss of vision, or a sudden onset of proptosis, diplopia, or migraine. If examination reveals papilledema or retinal vascular lesions, estrogens should be permanently discontinued.
5.8 Addition of a Progestin When a Woman Has Not Had a Hysterectomy
Studies of the addition of a progestin for 10 or more days of a cycle of estrogen administration, or daily with estrogen in a continuous regimen, have reported a lowered incidence of endometrial hyperplasia than would be induced by estrogen treatment alone. Endometrial hyperplasia may be a precursor to endometrial cancer.
There are, however, possible risks that may be associated with the use of progestins with estrogens compared to estrogen-alone regimens. These include an increased risk of breast cancer.
5.9 Elevated Blood Pressure
In a small number of case reports, substantial increases in blood pressure have been attributed to idiosyncratic reactions to estrogens. In a large, randomized, placebo-controlled clinical trial, a generalized effect of estrogens on blood pressure was not seen.
5.10 Hypertriglyceridemia
In women with pre-existing hypertriglyceridemia, estrogen therapy may be associated with elevations of plasma triglycerides leading to pancreatitis. Consider discontinuation of treatment if pancreatitis occurs.
5.11 Hepatic Impairment and/or Past History of Cholestatic Jaundice
Estrogens may be poorly metabolized in women with impaired liver function. For women with a history of cholestatic jaundice associated with past estrogen use or with pregnancy, caution should be exercised, and in the case of recurrence, medication should be discontinued.
5.12 Hypothyroidism
Estrogen administration leads to increased thyroid-binding globulin (TBG) levels. Women with normal thyroid function can compensate for the increased TBG by making more thyroid hormone, thus maintaining free T4 and T3 serum concentrations in the normal range. Women dependent on thyroid hormone replacement therapy who are also receiving estrogens may require increased doses of their thyroid replacement therapy. These women should have their thyroid function monitored in order to maintain their free thyroid hormone levels in an acceptable range.
5.13 Fluid Retention
Estrogens may cause some degree of fluid retention. Women with conditions that might be influenced by this factor, such as a cardiac or renal dysfunction, warrant careful observation when estrogen-alone is prescribed.
5.14 Hypocalcemia
Estrogen therapy should be used with caution in women with hypoparathyroidism as estrogen-induced hypocalcemia may occur.
5.15 Exacerbation of Endometriosis
A few cases of malignant transformation of residual endometrial implants have been reported in women treated post-hysterectomy with estrogen-alone therapy. For women known to have residual endometriosis post-hysterectomy, the addition of progestin should be considered.
5.16 Hereditary Angioedema
Exogenous estrogens may exacerbate symptoms of angioedema in women with hereditary angioedema.
5.17 Exacerbation of Other Conditions
Estrogen therapy may cause an exacerbation of asthma, diabetes mellitus, epilepsy, migraine, porphyria, systemic lupus erythematosus and hepatic hemangiomas and should be used with caution in women with these conditions.
5.18 Local Abrasion
A few cases of local abrasion induced by the estradiol vaginal insert applicator have been reported, especially in women with severely atrophic vaginal mucosa.
5.19 Laboratory Tests
Serum follicle stimulating hormone (FSH) and estradiol levels have not been shown to be useful in the management of moderate to severe symptoms of vulvar and vaginal atrophy.
5.20 Drug-Laboratory Test Interactions
Accelerated prothrombin time, partial thromboplastin time and platelet aggregation time; increased platelet count; increased factors II, VII antigen, VIII antigen, VIII coagulant activity, IX, X, XII, VII-X complex, II-VII-X complex, and beta-thromboglobulin; decreased levels of antifactor Xa and antithrombin III, decreased antithrombin III activity; increased levels of fibrinogen and fibrinogen activity; increased plasminogen antigen and activity.
Increased thyroid-binding globulin (TBG) levels leading to increased circulating total thyroid hormone as measured by protein-bound iodine (PBI), T4 levels (by column or by radioimmunoassay) or T3 levels by radioimmunoassay. T3 resin uptake is decreased, reflecting the elevated TBG. Free T4 and free T3 concentrations are unaltered. Women on thyroid replacement therapy may require higher doses of thyroid hormone.
Other binding proteins may be elevated in serum, for example, corticosteroid binding globulin (CBG), sex hormone-binding globulin (SHBG), leading to increased total circulating corticosteroids and sex steroids, respectively. Free hormone concentrations, such as testosterone and estradiol, may be decreased. Other plasma proteins may be increased (angiotensinogen/renin substrate, alpha-1-antitrypsin, ceruloplasmin).
Increased plasma high-density lipoprotein (HDL) and HDL2 cholesterol subfraction concentrations, reduced low-density lipoprotein (LDL) cholesterol concentrations, increased triglyceride levels.
Impaired glucose tolerance.
-
6 ADVERSE REACTIONS
The following serious adverse reactions are discussed elsewhere in the labeling:
- Cardiovascular Disorders [see Boxed Warning, Warnings and Precautions (5.2)]
- Malignant Neoplasms [see Boxed Warning, Warnings and Precautions (5.3)]
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
In a 12-month randomized, double-blind, parallel group, placebo-controlled study, a total of 309 postmenopausal women were randomized to receive either placebo or estradiol 10 mcg vaginal inserts. Adverse reactions with an incidence of ≥5 percent in the estradiol 10 mcg group and greater than those reported in the placebo group are listed in Table 1.
Table 1: Treatment-Emergent Adverse Reactions Reported at a Frequency of ≥ 5 Percent in Women Receiving Estradiol 10 mcg Body System Treatment Adverse Reaction Number (%) of Women Placebo
N = 103
n (%)Estradiol
N = 205
n (%)N = Total number of women in study. n = Number of women who experienced adverse reactions. Body As A Whole Back Pain 2 (2) 14 (7) Digestive System Diarrhea 0 11 (5) Urogenital System Vulvovaginal Mycotic Infection 3 (3) 17 (8) Vulvovaginal Pruritus 2 (2) 16 (8) 6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of estradiol 10 mcg. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Gastrointestinal disorders
DiarrheaGeneral disorders and administration site conditions
Drug ineffectiveImmune system disorders
HypersensitivityInvestigations
Blood estrogen increased
Weight increasedMetabolism and nutrition disorders
Fluid retentionNeoplasms benign and malignant
Breast cancer
Endometrial cancerPsychiatric disorders
Depression
InsomniaCentral Nervous System
Aggravated migraineReproductive system and breast disorders
Endometrial hyperplasia
Vulvovaginal burning sensation
Vulvovaginal pain
Genital pruritus
Vulvovaginal rash
Vulvovaginal swelling
Vaginismus
Vaginal ulcerationSkin and subcutaneous tissue disorders
Rash
Rash erythematous
Rash pruritic
UrticariaVascular disorders
Deep vein thrombosisAdditional postmarketing adverse reactions have been reported in patients receiving other forms of hormone therapy.
-
7 DRUG INTERACTIONS
No drug-drug interaction studies have been conducted for estradiol.
7.1 Metabolic Interactions
In-vitro and in-vivo studies have shown that estrogens are metabolized partially by cytochrome P450 3A4 (CYP3A4). Therefore, inducers or inhibitors of CYP3A4 may affect estrogen drug metabolism. Inducers of CYP3A4, such as St. John’s wort (Hypericum perforatum) preparations, phenobarbital, carbamazepine and rifampin, may reduce plasma concentrations of estrogens, possibly resulting in a decrease in therapeutic effects and/or changes in the uterine bleeding profile. Inhibitors of CYP3A4 such as erythromycin, clarithromycin, ketoconazole, itraconazole, ritonavir and grapefruit juice may increase plasma concentrations of estrogens and may result in side effects.
-
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Estradiol should not be used during pregnancy [see Contraindications (4)]. There appears to be little or no increased risk of birth defects in children born to women who have used estrogens and progestins as an oral contraceptive inadvertently during early pregnancy.
8.3 Nursing Mothers
Estradiol should not be used during lactation. Estrogen administration to nursing women has been shown to decrease the quantity and quality of the breast milk. Detectable amounts of estrogens have been identified in the breast milk of women receiving estrogen therapy. Caution should be exercised when estradiol is administered to a nursing woman.
8.4 Pediatric Use
Estradiol is not indicated in children. Clinical studies have not been conducted in the pediatric population.
8.5 Geriatric Use
There have not been sufficient numbers of geriatric women involved in clinical studies utilizing estradiol to determine whether those over 65 years of age differ from younger subjects in their response to estradiol.
The Women’s Health Initiative Studies
In the WHI estrogen-alone substudy (daily CE [0.625 mg]-alone versus placebo), there was a higher relative risk of stroke in women greater than 65 years of age [see Clinical Studies (14.2)].
In the WHI estrogen plus progestin substudy (daily CE [0.625 mg] plus MPA [2.5 mg] versus placebo), there was a higher relative risk of nonfatal stroke and invasive breast cancer in women greater than 65 years of age [see Clinical Studies (14.2)].
The Women’s Health Initiative Memory Study
In the WHIMS ancillary studies of postmenopausal women 65 to 79 years of age, there was an increased risk of developing probable dementia in women receiving estrogen-alone or estrogen plus progestin when compared to placebo [see Warnings and Precautions (5.4) and Clinical Studies (14.3)].
Since both ancillary studies were conducted in women 65 to 79 years of age, it is unknown whether these findings apply to younger postmenopausal women8[see Warnings and Precautions (5.4) and Clinical Studies (14.3)].
- 10 OVERDOSAGE
-
11 DESCRIPTION
Estradiol vaginal inserts USP, 10 mcg, are small, white, film-coated inserts containing 10.3 mcg of estradiol hemihydrate equivalent to 10 mcg of estradiol, USP. Each insert of estradiol vaginal insert USP, 10 mcg contains the following excipients: corn starch, hypromellose, lactose monohydrate and magnesium stearate. The film coating contains hypromellose and polyethylene glycol. Each estradiol vaginal insert, USP is 6 mm in diameter and is placed in a disposable applicator. Each insert-filled applicator is packaged separately in a blister pack. Estradiol vaginal inserts, USP are used intravaginally. When the insert comes in contact with the vaginal mucosa, estradiol, USP is released into the vagina.
USP Dissolution Test is pending.
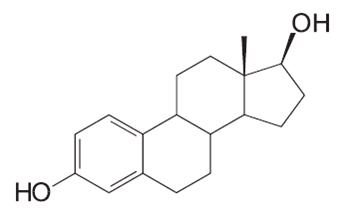
Estradiol hemihydrate is a white, almost white or colorless crystalline solid, chemically described as estra-1,3,5 (10)-triene-3,17β-diol. The chemical formula is C18H24O2 ½ H2O with a molecular weight of 281.4.
The structural formula is:
-
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Endogenous estrogens are largely responsible for the development and maintenance of the female reproductive system and secondary sexual characteristics. Although circulating estrogens exist in a dynamic equilibrium of metabolic interconversions, estradiol is the principal intracellular human estrogen and is substantially more potent than its metabolites, estrone and estriol, at the receptor level.
The primary source of estrogen in normally cycling adult women is the ovarian follicle, which secretes 70 to 500 mcg of estradiol daily, depending on the phase of the menstrual cycle. After menopause, most endogenous estrogen is produced by conversion of androstenedione, secreted by the adrenal cortex, to estrone in the peripheral tissues. Thus, estrone and the sulfate conjugated form, estrone sulfate, are the most abundant circulating estrogens in postmenopausal women.
Estrogens act through binding to nuclear receptors in estrogen-responsive tissues. To date, two estrogen receptors have been identified. These vary in proportion from tissue to tissue.
Circulating estrogens modulate the pituitary secretion of the gonadotropins, luteinizing hormone (LH), and FSH, through a negative feedback mechanism. Estrogens act to reduce the elevated levels of these hormones seen in postmenopausal women.
12.3 Pharmacokinetics
Absorption
Estrogen drug products are well absorbed through the skin, mucous membranes and the gastrointestinal tract. The vaginal delivery of estrogens circumvents first-pass metabolism.
In a single-center, randomized, open-label, multiple-dose study conducted in 29 patients, estradiol 10 mcg demonstrated a mean estradiol (E2) Cave at Day 83 of 5.5 pg/mL after 12 weeks of treatment (see Table 2).
Table 2: Arithmetic Means of Estradiol (E2), Estrone (E1) and Estrone Sulfate (E1S) PK Parameters Following Multiple Dosesa of Estradiol 10 mcg Uncorrected for baseline, N=29 E2 E1 E1S AUC0-24
(h.pg/mL)Cave (0-24)
(pg/mL)%CVb AUC0-24
(h.pg/mL)Cave (0-24)
(pg/mL)%CVb AUC0-24
(h.pg/mL)Cave (0-24)
(pg/mL)%CVb a Patients received vaginal inserts as a once daily intravaginal treatment for the first 2 weeks and a twice weekly intravaginal maintenance for the following 10 weeks. b CV: Coefficient of Variance for both AUC0-24 and Cave(0-24) Day 1 242.08 10.09 33.02 485.21 20.22 44.86 5158.32 214.93 53.57 Day 14 176.49 7.35 43.69 496.14 20.67 30.88 6323.41 263.48 50.07 Day 83 132.04 5.50 59.69 411.08 17.13 39.58 3804.65 158.53 49.76 Distribution
The distribution of exogenous estrogens is similar to that of endogenous estrogens. Estrogens are widely distributed in the body and are generally found in higher concentrations in the sex hormone target organs. Estrogens circulate in the blood largely bound to SHBG and albumin.
Metabolism
Exogenous estrogens are metabolized in the same manner as endogenous estrogens. Circulating estrogens exist in a dynamic equilibrium of metabolic interconversions. These transformations take place mainly in the liver. Estradiol is converted reversibly to estrone, and both can be converted to estriol, which is the major urinary metabolite. Estrogens also undergo enterohepatic recirculation via sulfate and glucuronide conjugation in the liver, biliary secretion of conjugates into the intestine, and hydrolysis in the gut followed by reabsorption. In postmenopausal women, a significant portion of the circulating estrogens exist as sulfate conjugates, especially estrone sulfate, which serves as a circulating reservoir for the formation of more active estrogens.
Excretion
Estradiol, estrone and estriol are excreted in the urine along with glucuronide and sulfate conjugates.
Use in Specific Populations
No pharmacokinetic studies were conducted in specific populations, including patients with renal or hepatic impairment.
- 13 NONCLINICAL TOXICOLOGY
-
14 CLINICAL STUDIES
14.1 Effects on Atrophic Vaginitis
A 12-month double-blind, randomized, parallel group, placebo-controlled multicenter study was conducted in the U.S. and Canada to evaluate the efficacy and safety of estradiol 10 mcg in the treatment of atrophic vaginitis in 309 postmenopausal women between 46 and 81 years of age (mean 57.6 years of age) who at baseline identified their most bothersome symptom of atrophic vaginitis from among six symptoms (vaginal dryness, vaginal and/or vulvar irritation/itching, vaginal soreness, dysuria, dyspareunia and vaginal bleeding associated with intercourse). Women inserted one insert intravaginally each day for 14 days, then one insert twice weekly for the remaining 50 weeks. The majority (92.9 percent) of the women were Caucasian (n=287), 3.2 percent were Black (n=10), 1.6 percent were Asian (n=5) and 2.2 percent were Other (n=7). All subjects were assessed for improvement in the mean change from baseline to Week 12 for co-primary efficacy variables of: a composite of most bothersome symptoms of atrophic vaginitis; percentage of vaginal superficial cells and percentage of vaginal parabasal cells on a vaginal smear; and vaginal pH.
Relief of Vaginal Symptoms
Estradiol 10 mcg was statistically superior to placebo in reducing the severity of a composite score of most bothersome symptoms associated with atrophic vaginitis at Week 12 (see Table 3).
Table 3: Mean Change from Baseline to Week 12 in a Composite Score of Most Bothersome Symptoms Compared to Placebo – ITT Populationa Placebo Estradiol 10 mcg ITT Populationa a All randomized subjects who received at least one dose of study drug and had at least one post-baseline evaluation. N 93 190 Baseline mean composite score 2.29 2.35 Change from baseline at Week 12 (LOCF) -0.84 -1.20 p-value versus Placebo --- 0.002 Also demonstrated for estradiol 10 mcg compared to placebo was a statistically significant increase in the percentage of superficial cells at Week 12 (13.2 percent compared to 3.8 percent for matching placebo, p<0.001), a statistically significant decrease in parabasal cells at Week 12 (-37 percent compared to -9.3 percent for matching placebo, p<0.001), and a statistically significant mean reduction between baseline and Week 12 in vaginal pH score (-1.3 compared to -0.4 for matching placebo, p<0.001).
Endometrial safety was assessed by endometrial biopsy at the screening and final study visit. Of the 172 subjects in the estradiol 10 mcg group who had a biopsy performed at end of study, 92 subjects had endometrial tissue that was atrophic or inactive and 73 subjects had no tissue or tissue insufficient for diagnosis. There was one case of adenocarcinoma grade 2 and one case of complex hyperplasia without atypia. Three subjects exhibited polyps (two atrophic polyps and one adenomyomatus type polyp) and two others had adenomyosis and an atypical epithelial proliferation.
Endometrial safety of estradiol 10 mcg was additionally evaluated in a second, 12 month, open-label, multicenter safety study. Of the 297 subjects who had a biopsy performed at end of study, 183 subjects had endometrial tissue that was atrophic or inactive and 111 subjects had no tissue or tissue insufficient for diagnosis. There was one case of complex hyperplasia without atypia. Two subjects exhibited polyps.
14.2 Women’s Health Initiative Studies
The WHI enrolled approximately 27,000 predominantly healthy postmenopausal women in two substudies to assess the risks and benefits of daily oral CE (0.625 mg)-alone or in combination with MPA (2.5 mg) compared to placebo in the prevention of certain chronic diseases. The primary endpoint was the incidence of CHD (defined as nonfatal MI, silent MI and CHD death), with invasive breast cancer as the primary adverse outcome. A “global index” included the earliest occurrence of CHD, invasive breast cancer, stroke, PE, endometrial cancer (only in the CE plus MPA substudy), colorectal cancer, hip fracture, or death due to other causes. These substudies did not evaluate the effects of CE-alone or CE plus MPA on menopausal symptoms.
WHI Estrogen-Alone Substudy
The WHI estrogen-alone substudy was stopped early because an increased risk of stroke was observed, and it was deemed that no further information would be obtained regarding the risks and benefits of estrogen-alone in predetermined primary endpoints.
Results of the estrogen-alone substudy, which included 10,739 women (average 63 years of age, range 50 to 79; 75.3 percent White, 15.1 percent Black, 6.1 percent Hispanic, 3.6 percent Other) after an average follow-up of 7.1 years, are presented in Table 4.
Table 4: Relative and Absolute Risk Seen in the Estrogen-Alone Substudy of WHIa Event Relative Risk
CE vs. Placebo
(95% nCIb)CE
n = 5,310Placebo
n = 5,429Absolute Risk per 10,000 Women-Years
aAdapted from numerous WHI publications. WHI publications can be viewed at www.nhlbi.nih.gov/whi. bNominal confidence intervals unadjusted for multiple looks and multiple comparisons. cResults are based on centrally adjudicated data for an average follow-up of 7.1 years. dNot included in “global index”. eResults are based on an average follow-up of 6.8 years. fAll deaths, except from breast or colorectal cancer, definite or probable CHD, PE or cerebrovascular disease. gA subset of the events was combined in a “global index”, defined as the earliest occurrence of CHD events, invasive breast cancer, stroke, pulmonary embolism, colorectal cancer, hip fracture, or death due to other causes. CHD eventsc 0.95 (0.78 to 1.16) 54 57 Non-fatal MIc 0.91 (0.73 to 1.14) 40 43 CHD deathc 1.01 (0.71 to 1.43) 16 16 All Strokesc 1.33 (1.05 to 1.68) 45 33 Ischemic strokec 1.55 (1.19 to 2.01) 38 25 Deep vein thrombosisc,d 1.47 (1.06 to 2.06) 23 15 Pulmonary embolismc 1.37 (0.90 to 2.07) 14 10 Invasive breast cancerc 0.80 (0.62 to 1.04) 28 34 Colorectal cancere 1.08 (0.75 to 1.55) 17 16 Hip fracturec 0.65 (0.45 to 0.94) 12 19 Vertebral fracturesc,d 0.64 (0.44 to 0.93) 11 18 Lower arm/wrist fracturesc,d 0.58 (0.47 to 0.72) 35 59 Total fracturesc,d 0.71 (0.64 to 0.80) 144 197 Death due to other causese,f 1.08 (0.88 to 1.32) 53 50 Overall mortalityc,d 1.04 (0.88 to 1.22) 79 75 Global Indexg 1.02 (0.92 to 1.13) 206 201 For those outcomes included in the WHI “global index” that reached statistical significance, the absolute excess risk per 10,000 women-years in the group treated with CE-alone was 12 more strokes while the absolute risk reduction per 10,000 women-years was 7 fewer hip fractures.9 The absolute excess risk of events included in the “global index” was a non-significant 5 events per 10,000 women-years. There was no difference between the groups in terms of all-cause mortality.
No overall difference for primary CHD events (nonfatal MI, silent MI and CHD death) and invasive breast cancer incidence in women receiving CE-alone compared with placebo was reported in final centrally adjudicated results from the estrogen-alone substudy, after an average follow up of 7.1 years.
Centrally adjudicated results for stroke events from the estrogen-alone substudy, after an average follow-up of 7.1 years, reported no significant difference in distribution of stroke subtype or severity, including fatal strokes, in women receiving CE-alone compared to placebo. Estrogen-alone increased the risk for ischemic stroke, and this excess risk was present in all subgroups of women examined.10
Timing of the initiation of estrogen-alone therapy relative to the start of menopause may affect the overall risk benefit profile. The WHI estrogen-alone substudy, stratified by age, showed in women 50 to 59 years of age a non-significant trend toward reduced risk for CHD [hazard ratio (HR) 0.63 (95 percent CI, 0.36 to 1.09)] and overall mortality [HR 0.71 (95 percent CI, 0.46 to 1.11)].
WHI Estrogen Plus Progestin Substudy
The WHI estrogen plus progestin substudy was stopped early. According to the predefined stopping rule, after an average follow-up of 5.6 years of treatment, the increased risk of invasive breast cancer and cardiovascular events exceeded the specified benefits included in the “global index.” The absolute excess risk of events included in the “global index” was 19 per 10,000 women-years.
For those outcomes included in the WHI “global index” that reached statistical significance after 5.6 years of follow-up, the absolute excess risks per 10,000 women-years in the group treated with CE plus MPA were 7 more CHD events, 8 more strokes, 10 more PEs, and 8 more invasive breast cancers, while the absolute risk reductions per 10,000 women-years were 6 fewer colorectal cancers and 5 fewer hip fractures.
Results of the CE plus MPA substudy, which included 16,608 women (average 63 years of age, range 50 to 79; 83.9 percent White, 6.8 percent Black, 5.4 percent Hispanic, 3.9 percent Other) are presented in Table 5. These results reflect centrally adjudicated data after an average follow-up of 5.6 years.
Table 5: Relative and Absolute Risk Seen in the Estrogen Plus Progestin Substudy of WHI at an Average of 5.6 Yearsa,b Event Relative Risk
CE/MPA vs Placebo
(95% nCI c)CE/MPA
n = 8,506Placebo
n = 8,102Absolute Risk per 10,000 Women-Years aAdapted from numerous WHI publications. WHI publications can be viewed at www.nhlbi.nih.gov/whi. bResults are based on centrally adjudicated data. cNominal confidence intervals unadjusted for multiple looks and multiple comparisons. dNot included in “global index”. eIncludes metastatic and non-metastatic breast cancer, with the exception of in situ cancer. fAll deaths, except from breast or colorectal cancer, definite or probable CHD, PE or cerebrovascular disease. gA subset of the events was combined in a “global index”, defined as the earliest occurrence of CHD events, invasive breast cancer, stroke, pulmonary embolism, colorectal cancer, hip fracture, or death due to other causes. CHD events 1.23 (0.99 to 1.53) 41 34 Non-fatal MI 1.28 (1 to 1.63) 31 25 CHD death 1.10 (0.70 to 1.75) 8 8 All Strokes 1.31 (1.03 to 1.68) 33 25 Ischemic stroke 1.44 (1.09 to 1.90) 26 18 Deep vein thrombosisd 1.95 (1.43 to 2.67) 26 13 Pulmonary embolism 2.13 (1.45 to 3.11) 18 8 Invasive breast cancere 1.24 (1.01 to 1.54) 41 33 Colorectal cancer 0.61 (0.42 to 0.87) 10 16 Endometrial cancerd 0.81 (0.48 to 1.36) 6 7 Cervical cancerd 1.44 (0.47 to 4.42) 2 1 Hip fracture 0.67 (0.47 to 0.96) 11 16 Vertebral fracturesd 0.65 (0.46 to 0.92) 11 17 Lower arm/wrist fracturesd 0.71 (0.59 to 0.85) 44 62 Total fracturesd 0.76 (0.69 to 0.83) 152 199 Overall Mortalityf 1 (0.83 to 1.19) 52 52 Global Indexg 1.13 (1.02 to 1.25) 184 165 Timing of the initiation of estrogen plus progestin therapy relative to the start of menopause may affect the overall risk benefit profile. The WHI estrogen plus progestin substudy stratified by age showed in women 50 to 59 years of age, a non-significant trend toward reduced risk for overall mortality [HR 0.69 (95 percent CI, 0.44 to 1.07)].
14.3 Women’s Health Initiative Memory Study
The WHIMS estrogen-alone ancillary study of WHI enrolled 2,947 predominately healthy hysterectomized postmenopausal women 65 to 79 years of age and older (45 percent were 65 to 69 years of age; 36 percent were 70 to 74 years of age; 19 percent were 75 years of age and older) to evaluate the effects of daily CE (0.625 mg)-alone on the incidence of probable dementia (primary outcome) compared to placebo.
After an average follow-up of 5.2 years, the relative risk of probable dementia for CE-alone versus placebo was 1.49 (95 percent CI, 0.83 to 2.66). The absolute risk of probable dementia for CE-alone versus placebo was 37 versus 25 cases per 10,000 women-years. Probable dementia as defined in this study included Alzheimer’s disease (AD), vascular dementia (VaD) and mixed types (having features of both AD and VaD). The most common classification of probable dementia in the treatment group and the placebo group was AD. Since the ancillary study was conducted in women 65 to 79 years of age, it is unknown whether these findings apply to younger postmenopausal women [see Warnings and Precautions (5.4) and Use in Specific Populations (8.5)].
The WHIMS estrogen plus progestin ancillary study of WHI enrolled 4,532 predominantly healthy postmenopausal women 65 years of age and older (47 percent were 65 to 69 years of age; 35 percent were 70 to 74 years; 18 percent were 75 years of age and older) to evaluate the effects of daily CE (0.625 mg) plus MPA (2.5 mg) on the incidence of probable dementia (primary outcome) compared to placebo.
After an average follow-up of 4 years, the relative risk of probable dementia for CE plus MPA versus placebo was 2.05 (95 percent CI, 1.21 to 3.48). The absolute risk of probable dementia for CE plus MPA versus placebo was 45 versus 22 per 10,000 women-years. Probable dementia as defined in this study included AD, VaD and mixed types (having features of both AD and VaD). The most common classification of probable dementia in the treatment group and the placebo group was AD. Since the ancillary study was conducted in women 65 to 79 years of age, it is unknown whether these findings apply to younger postmenopausal women [see Warnings and Precautions (5.4) and Use in Specific Populations (8.5)].
When data from the two populations were pooled as planned in the WHIMS protocol, the reported overall relative risk for probable dementia was 1.76 (95 percent CI, 1.19 to 2.60). Differences between groups became apparent in the first year of treatment. It is unknown whether these findings apply to younger postmenopausal women [see Warnings and Precautions (5.4) and Use in Specific Populations (8.5)].
-
15 REFERENCES
- Rossouw JE, et al. Postmenopausal Hormone Therapy and Risk of Cardiovascular Disease by Age and Years Since Menopause. JAMA. 2007; 297:1465-1477.
- Hsia J, et al. Conjugated Equine Estrogens and Coronary Heart Disease. Arch Int Med. 2006; 166:357-365.
- Curb JD, et al. Venous Thrombosis and Conjugated Equine Estrogen in Women Without a Uterus. Arch Int Med. 2006; 166:772-780.
- Cushman M, et al. Estrogen Plus Progestin and Risk of Venous Thrombosis. JAMA. 2004; 292:1573-1580.
- Stefanick ML, et al. Effects of Conjugated Equine Estrogens on Breast Cancer and Mammography Screening in Postmenopausal Women With Hysterectomy. JAMA. 2006; 295:1647-1657.
- Chlebowski RT, et al. Influence of Estrogen Plus Progestin on Breast Cancer and Mammography in Healthy Postmenopausal Women. JAMA. 2003; 289:3234-3253.
- Anderson GL, et al. Effects of Estrogen Plus Progestin on Gynecologic cancers and Associated Diagnostic Procedures. JAMA. 2003; 290:1739-1748.
- Shumaker SA, et al. Conjugated Equine Estrogens and Incidence of Probable Dementia and Mild Cognitive Impairment in Postmenopausal Women. JAMA. 2004; 291:2947-2958.
- Jackson RD, et al. Effects of Conjugated Equine Estrogen on Risk of Fractures and BMD in Postmenopausal Women With Hysterectomy: Results From the Women’s Health Initiative Randomized Trial. J Bone Miner Res. 2006; 21:817-828.
- Hendrix SL, et al. Effects of Conjugated Equine Estrogen on Stroke in the Women’s Health Initiative. Circulation. 2006; 113:2425-2434.
-
16 HOW SUPPLIED/STORAGE AND HANDLING
16.1 How Supplied
Estradiol vaginal inserts USP, 10 mcg, are supplied as white to off-white, round biconvex, film-coated unscored inserts debossed with “276” on obverse and “AN” on the reverse. Each estradiol vaginal insert USP, 10 mcg, is contained in a disposable, single-use applicator, packaged in a blister pack. Cartons contain 8 or 18 applicators with inset inserts.
Estradiol vaginal inserts USP, 10 mcg
8 applicators: NDC: 53746-226-21
18 applicators: NDC: 53746-226-23Keep out of reach of children.
-
17 PATIENT COUNSELING INFORMATION
See FDA-Approved Patient Labeling.
17.1 Vaginal Bleeding
Inform postmenopausal women of the importance of reporting vaginal bleeding to their healthcare provider as soon as possible [see Warnings and Precautions (5.3)].
17.2 Possible Serious Adverse Reactions with Estrogen-Alone Therapy
Inform postmenopausal women of possible serious adverse reactions of estrogen-alone therapy including Cardiovascular Disorders, Malignant Neoplasms and Probable Dementia [see Warnings and Precautions (5.2,5.3,5.4)].
17.3 Possible Less Serious but Common Adverse Reactions with Estrogen-Alone Therapy
Inform postmenopausal women of possible less serious but common adverse reactions of estrogen-alone therapy such as headache, breast pain and tenderness, nausea and vomiting.
17.4 Instructions for Use of Applicator
Step 1: Tear off a single applicator.
Step 2: Separate the plastic wrap and remove the applicator from the plastic wrap as shown in Figure A. If after opening the package you see that the insert has come out of the applicator but has not fallen out of the package, carefully put it back into the applicator for insertion. Please keep your hands clean and dry while handling the insert.
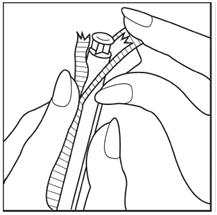
Figure A
Step 3: Hold the applicator so that the finger of one hand can press the applicator plunger as shown in Figure B.
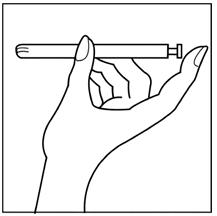
Figure B
Step 4: Next select the best position for vaginal insertion of estradiol vaginal inserts that is most comfortable for you. See suggested reclining Figure C or standing Figure D position illustrated below:
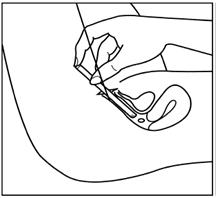
Figure C
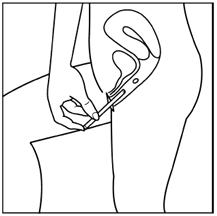
Figure D
Step 5: Using the other hand, guide the applicator gently and comfortably through the vaginal opening (see Figures C and D above). If prior to insertion the insert falls out of the applicator, throw the insert and applicator away and use a new insert-filled applicator.
Step 6: The applicator should be inserted (without forcing) as far as comfortably possible, or until half of the applicator is inside your vagina, whichever is less.
Step 7: Once the insert-filled applicator has been inserted, gently press the plunger until the plunger is fully depressed. This will eject the insert inside your vagina where it will dissolve slowly over several hours.
Step 8: After depressing the plunger, gently remove the applicator and dispose of it the same way you would a plastic tampon applicator. The applicator is of no further use and should be discarded properly. Insertion may be done at any time of the day. It is advisable to use the same time daily for all applications of estradiol vaginal inserts. If you have any questions, please consult your healthcare provider or pharmacist.
Manufactured by:
Amneal Pharmaceuticals of New York, LLC
Brookhaven, NY 11719Rev. 04-2019-04
-
FDA-Approved Patient Labeling
Estradiol (ess-tra-DYE-ole) Vaginal Inserts
Read this PATIENT INFORMATION before you start using estradiol vaginal inserts and read what you get each time you refill your estradiol vaginal inserts prescription. There may be new information. This information does not take the place of talking to your healthcare provider about your menopausal symptoms or your treatment.
What is the most important information I should know about estradiol vaginal inserts
(an estrogen hormone)?- Using estrogen-alone may increase your chance of getting cancer of the uterus (womb)
Report any unusual vaginal bleeding right away while you are using estradiol vaginal inserts. Vaginal bleeding after menopause may be a warning sign of cancer of the uterus (womb). Your healthcare provider should check any unusual vaginal bleeding to find out the cause.
- Do not use estrogen-alone to prevent heart disease, heart attacks, strokes or dementia (decline of brain function)
- Using estrogen-alone may increase your chances of getting strokes or blood clots
- Using estrogen-alone may increase your chance of getting dementia, based on a study of women 65 years of age or older
- Do not use estrogens with progestins to prevent heart disease, heart attack, strokes or dementia
- Using estrogens with progestins may increase your chances of getting heart attacks, strokes, breast cancer, or blood clots
- Using estrogens with progestin may increase your chance of getting dementia, based on a study of women 65 years of age or older
- You and your healthcare provider should talk regularly about whether you still need treatment with estradiol vaginal inserts
What are estradiol vaginal inserts?
Estradiol vaginal inserts are a medicine that contains estradiol (an estrogen hormone) in a vaginal insert.
What are estradiol vaginal inserts used for?
Estradiol vaginal inserts are used after menopause to:
-
Treat menopausal changes in and around the vagina
You and your healthcare provider should talk regularly about whether you still need treatment with estradiol vaginal inserts to control these problems.
Who should not use estradiol vaginal inserts?
Do not start using estradiol vaginal inserts if you:
- Have unusual vaginal bleeding
- Currently have or have had certain cancers
Estrogens may increase the chances of getting certain types of cancers, including cancer of the breast or uterus. If you have or have had cancer, talk with your healthcare provider about whether you should use estradiol vaginal inserts.
- Had a stroke or heart attack
-
Currently have or have had blood clots
-
Currently have or have had liver problems
-
Have been diagnosed with a bleeding disorder
- Are allergic to estradiol vaginal inserts or any of its ingredients
See the list of ingredients in estradiol vaginal inserts at the end of this leaflet.
-
Think you may be pregnant
Tell your healthcare provider:
-
If you have any unusual vaginal bleeding
Vaginal bleeding after menopause may be a warning sign of cancer of the uterus (womb). Your healthcare provider should check any unusual vaginal bleeding to find out the cause.
-
About all of your medical problems
Your healthcare provider may need to check you more carefully if you have certain conditions, such as asthma (wheezing), epilepsy (seizures), diabetes, migraine, endometriosis, lupus, problems with your heart, liver, thyroid, kidneys, or have high calcium levels in your blood.
-
About all the medicines you take
This includes prescription and nonprescription medicines, vitamins and herbal supplements. Some medicines may affect how estradiol vaginal inserts work. Estradiol vaginal inserts may also affect how your other medicines work.
-
If you are going to have surgery or will be on bed rest
You may need to stop using estradiol vaginal inserts.
-
If you are breast feeding
The hormone in estradiol vaginal inserts can pass into your breast milk.
How should I use estradiol vaginal inserts?
Estradiol vaginal inserts are an insert that you place in your vagina with an applicator.
- Take the dose recommended by your healthcare provider and talk to him or her about how well that dose is working for you
- Estrogens should be used at the lowest dose possible for your treatment only as long as needed
You and your healthcare provider should talk regularly (for example, every 3 to 6 months) about the dose you are using and whether you still need treatment with estradiol vaginal inserts.
Step 1: Tear off a single applicator.
Step 2: Separate the plastic wrap and remove the applicator from the plastic wrap as shown in Figure A. If after opening the package you see that the insert has come out of the applicator but has not fallen out of the package, carefully put it back into the applicator for insertion. Please keep your hands clean and dry while handling the insert.
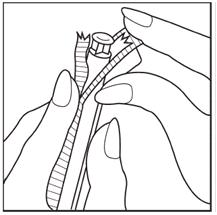
Figure A
Step 3: Hold the applicator so that the finger of one hand can press the applicator plunger as shown in Figure B.
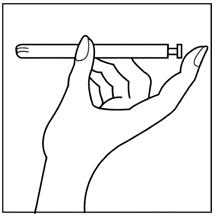
Figure B
Step 4: Next select the best position for vaginal insertion of estradiol vaginal inserts that is most comfortable for you. See suggested reclining Figure C or standing Figure D position illustrated below:
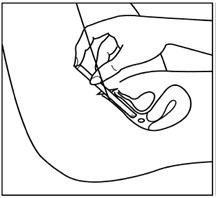
Figure C
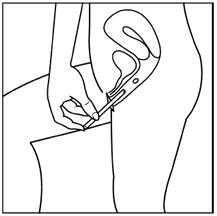
Figure D
Step 5: Using the other hand, guide the applicator gently and comfortably through the vaginal opening (see Figures C and D above). If prior to insertion the insert falls out of the applicator, throw the insert and applicator away and use a new insert-filled applicator.
Step 6: The applicator should be inserted (without forcing) as far as comfortably possible, or until half of the applicator is inside your vagina, whichever is less.
Step 7: Once the insert-filled applicator has been inserted, gently press the plunger until the plunger is fully depressed. This will eject the insert inside your vagina where it will dissolve slowly over several hours.
Step 8: After depressing the plunger, gently remove the applicator and dispose of it the same way you would a plastic tampon applicator. The applicator is of no further use and should be discarded properly. Insertion may be done at any time of the day. It is advisable to use the same time daily for all applications of estradiol vaginal inserts. If you have any questions, please consult your healthcare provider or pharmacist.
Dosage
Estradiol vaginal inserts therapy consists of the following dosing regimen:
One (1) estradiol vaginal insert intravaginally once daily for the first two (2) weeks, then one (1) insert twice weekly (for example Tuesday and Friday) for as long as you use estradiol vaginal inserts.
What are the possible side effects of estradiol vaginal inserts?
Estradiol vaginal inserts are only used in the vagina; however, the risks associated with oral estrogens should be taken into account.
Side effects are grouped by how serious they are and how often they happen when you are treated.
Serious but less common side effects include:
- Heart attack
- Stroke
- Blood clots
- Dementia
- Breast cancer
- Cancer of the lining of the uterus (womb)
- Cancer of the ovary
- High blood pressure
- High blood sugar
- Gallbladder disease
- Liver problems
- Enlargement of benign tumors of the uterus (“fibroids”)
Call your healthcare provider right away if you get any of the following warning signs or any other unusual symptoms that concern you:
- New breast lumps
- Unusual vaginal bleeding
- Changes in vision or speech
- Sudden new severe headaches
- Severe pains in your chest or legs with or without shortness of breath, weakness and fatigue
Less serious, but common, side effects include:
- Headache
- Breast pain
- Irregular vaginal bleeding or spotting
- Stomach or abdominal cramps, bloating
- Nausea and vomiting
- Hair loss
- Fluid retention
- Vaginal yeast infection
These are not all the possible side effects of estradiol vaginal inserts. For more information, ask your healthcare provider or pharmacist for advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
What can I do to lower my chances of a serious side effect with estradiol vaginal inserts?
- Talk with your healthcare provider regularly about whether you should continue using estradiol vaginal inserts.
- If you have a uterus, talk with your healthcare provider about whether the addition of a progestin is right for you.
The addition of a progestin is generally recommended for a woman with a uterus to reduce the chance of getting cancer of the uterus. See your healthcare provider right away if you get vaginal bleeding while using estradiol vaginal inserts.
- Have a pelvic exam, breast exam and mammogram (breast X-ray) every year unless your healthcare provider tells you something else.
If members of your family have had breast cancer or if you have ever had breast lumps or an abnormal mammogram, you may need to have breast exams more often.
- If you have high blood pressure, high cholesterol (fat in the blood), diabetes, are overweight, or if you use tobacco, you may have higher chances for getting heart disease.
Ask your healthcare provider for ways to lower your chances for getting heart disease.
General information about the safe and effective use of estradiol vaginal inserts.
Medicines are sometimes prescribed for conditions that are not mentioned in patient information leaflets. Do not use estradiol vaginal inserts for conditions for which it was not prescribed. Do not give estradiol vaginal inserts to other people, even if they have the same symptoms you have. It may harm them.
Keep estradiol vaginal inserts out of the reach of children.
This leaflet provides a summary of the most important information about estradiol vaginal inserts. If you would like more information, talk with your healthcare provider or pharmacist. You can ask for information about estradiol vaginal inserts that is written for health professionals. You can get more information by calling the toll free number 1-877-835-5472.
What are the ingredients in estradiol vaginal inserts?
Estradiol vaginal inserts are small, white, film-coated inserts containing estradiol. Each insert also contains corn starch, hypromellose, lactose monohydrate and magnesium stearate. The film coating contains hypromellose and polyethylene glycol.
Each estradiol vaginal insert is contained in a disposable applicator, packaged in a blister pack. Cartons contain 8 or 18 applicators with inset inserts.
Store at 20° to 25°C (68° to 77°F); excursions permitted between 15°C to 30°C (59°F to 86°F) [see USP Controlled Room Temperature].
Do not refrigerate.
Manufactured by:
Amneal Pharmaceuticals of New York, LLC
Brookhaven, NY 11719Rev. 11-2017-03
- Using estrogen-alone may increase your chance of getting cancer of the uterus (womb)
- PACKAGE LABEL.PRINCIPAL DISPLAY PANEL
-
INGREDIENTS AND APPEARANCE
ESTRADIOL
estradiol insertProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 53746-226 Route of Administration VAGINAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength ESTRADIOL (UNII: 4TI98Z838E) (ESTRADIOL - UNII:4TI98Z838E) ESTRADIOL 10 ug Inactive Ingredients Ingredient Name Strength STARCH, CORN (UNII: O8232NY3SJ) HYPROMELLOSES (UNII: 3NXW29V3WO) LACTOSE MONOHYDRATE (UNII: EWQ57Q8I5X) MAGNESIUM STEARATE (UNII: 70097M6I30) POLYETHYLENE GLYCOL, UNSPECIFIED (UNII: 3WJQ0SDW1A) Product Characteristics Color WHITE (off-white) Score no score Shape ROUND Size 6mm Flavor Imprint Code AN;276 Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 53746-226-21 8 in 1 CARTON 06/07/2015 1 1 in 1 APPLICATOR; Type 0: Not a Combination Product 2 NDC: 53746-226-23 18 in 1 CARTON 06/07/2015 2 1 in 1 APPLICATOR; Type 0: Not a Combination Product Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA205256 06/07/2015 Labeler - Amneal Pharmaceuticals of New York LLC (123797875) Establishment Name Address ID/FEI Business Operations Amneal Pharmaceuticals of New York, LLC 123797875 ANALYSIS(53746-226) , LABEL(53746-226) , MANUFACTURE(53746-226) , PACK(53746-226)
© 2026 FDA.report
This site is not affiliated with or endorsed by the FDA.