ESTRING- estradiol system
Estring by
Drug Labeling and Warnings
Estring by is a Prescription medication manufactured, distributed, or labeled by Pfizer Laboratories Div Pfizer Inc, Pfizer Inc. Drug facts, warnings, and ingredients follow.
Drug Details [pdf]
- PHYSICIAN'S LEAFLET
-
DESCRIPTION
ESTRING® (estradiol vaginal system) is a slightly opaque ring with a whitish core containing a drug reservoir of 2 mg estradiol. Estradiol, silicone polymers, barium sulfate and silicone fluid (as dispersing agent) are combined to form the ring. When placed in the vagina, ESTRING releases estradiol, approximately 7.5 mcg per day, in a consistent stable manner over 90 days. ESTRING has the following dimensions: outer diameter 55 mm; cross-sectional diameter 9 mm; core diameter 2 mm. One ESTRING should be inserted into the upper third of the vaginal vault, to be worn continuously for three months.
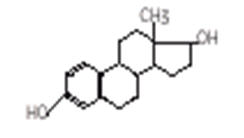
Estradiol is chemically described as estra-1, 3, 5(10)-triene-3, 17β-diol. The molecular formula of estradiol is C18H24O2 and the structural formula is:
The molecular weight of estradiol is 272.39.
-
CLINICAL PHARMACOLOGY
Endogenous estrogens are largely responsible for the development and maintenance of the female reproductive system and secondary sexual characteristics. Although circulating estrogens exist in a dynamic equilibrium of metabolic interconversions, estradiol is the principal intracellular human estrogen and is substantially more potent than its metabolites, estrone and estriol, at the receptor level.
The primary source of estrogen in normally cycling adult women is the ovarian follicle, which secretes 70 to 500 mcg of estradiol daily, depending on the phase of the menstrual cycle. After menopause, most endogenous estrogen is produced by conversion of androstenedione, secreted by the adrenal cortex, to estrone in the peripheral tissues. Thus, estrone and the sulfate conjugated form, estrone sulfate, are the most abundant circulating estrogens in postmenopausal women.
Estrogens act through binding to nuclear receptors in estrogen-responsive tissues. To date, two estrogen receptors have been identified. These vary in proportion from tissue to tissue.
Circulating estrogens modulate the pituitary secretion of the gonadotropins, luteinizing hormone (LH) and follicle stimulating hormone (FSH), through a negative feedback mechanism. Estrogens act to reduce the elevated levels of these hormones seen in postmenopausal women.
Pharmacokinetics
Absorption
Estrogens used in therapeutics are well absorbed through the skin, mucous membranes, and the gastrointestinal (GI) tract. The vaginal delivery of estrogens circumvents first-pass metabolism.
In a Phase I study of 14 postmenopausal women, the insertion of ESTRING (estradiol vaginal system) rapidly increased serum estradiol (E2) levels. The time to attain peak serum estradiol levels (Tmax) was 0.5 to 1 hour. Peak serum estradiol concentrations post-initial burst declined rapidly over the next 24 hours and were virtually indistinguishable from the baseline mean (range: 5 to 22 pg/mL). Serum levels of estradiol and estrone (E1) over the following 12 weeks during which the ring was maintained in the vaginal vault remained relatively unchanged (See Table 1).
The initial estradiol peak post-application of the second ring in the same women resulted in ~38 percent lower Cmax, apparently due to reduced systemic absorption via the treated vaginal epithelium. The relative systemic exposure from the initial peak of ESTRING accounted for approximately 4 percent of the total estradiol exposure over the 12-week period.
The release of estradiol from ESTRING was demonstrated in a Phase II study of 222 postmenopausal women who inserted up to four rings consecutively at three-month intervals. Systemic delivery of estradiol from ESTRING resulted in mean steady state serum estradiol estimates of 7.8, 7.0, 7.0, 8.1 pg/mL at weeks 12, 24, 36, and 48, respectively. Similar reproducibility is also seen in levels of estrone. The systemic exposure to estradiol and estrone was within the range observed in untreated women after the first eight hours.
In postmenopausal women, mean dose of estradiol systemically absorbed unchanged from ESTRING is ~8 percent [95 percent CI: 2.8–12.8 percent] of the daily amount released locally.
TABLE 1: PHARMACOKINETIC MEAN ESTIMATES FOLLOWING SINGLE ESTRING APPLICATION Estrogen Cmax
(pg/mL)Css–48 hr
(pg/mL)Css–4w
(pg/mL)Css–12w
(pg/mL)- * n=14
- † Based on means
Estradiol (E2)
63.2*
11.2
9.5
8.0
Baseline-adjusted E2†
55.6
3.6
2.0
0.4
Estrone (E1)
66.3
52.5
43.8
47.0
Baseline-adjusted E1
20.0
6.2
-2.4
0.8
Distribution
The distribution of exogenous estrogens is similar to that of endogenous estrogens. Estrogens are widely distributed in the body and are generally found in higher concentrations in the sex hormone target organs. Estrogens circulate in the blood largely bound to sex hormone binding globulin (SHBG) and albumin.
Metabolism
Exogenous estrogens are metabolized in the same manner as endogenous estrogens. Circulating estrogens exist in a dynamic equilibrium of metabolic interconversions. These transformations take place mainly in the liver. Estradiol is converted reversibly to estrone, and both can be converted to estriol, which is a major urinary metabolite. Estrogens also undergo enterohepatic recirculation via sulfate and glucuronide conjugation in the liver, biliary secretion of conjugates into the intestine, and hydrolysis in the intestine followed by reabsorption. In postmenopausal women, a significant proportion of the circulating estrogens exist as sulfate conjugates, especially estrone sulfate, which serves as a circulating reservoir for the formation of more active estrogens.
Excretion
Estradiol, estrone, and estriol are excreted in the urine along with glucuronide and sulfate conjugates.
Special Populations
No pharmacokinetic studies were conducted with ESTRING in specific populations, including women with renal or hepatic impairment.
Drug Interactions
No formal drug interactions studies have been done with ESTRING.
In vitro and in vivo studies have shown that systemic estrogens are metabolized partially by cytochrome P450 3A4 (CYP3A4). Therefore, inducers or inhibitors of CYP3A4 may affect estrogen metabolism. Inducers of CYP3A4 such as St. John's Wort (Hypericum perforatum) preparations, phenobarbital, carbamazepine, and rifampin may reduce plasma concentrations of estrogens, possibly resulting in a decrease in systemic effects and/or changes in the uterine bleeding profile. Inhibitors of CYP3A4 such as erythromycin, clarithromycin, ketoconazole, itraconazole, ritonavir and grapefruit juice may increase plasma concentrations of estrogens and may result in side effects.
-
CLINICAL STUDIES
Effects on Vulvar and Vaginal Atrophy
Two controlled studies have demonstrated the efficacy of ESTRING (estradiol vaginal system) in the treatment of postmenopausal urogenital symptoms due to estrogen deficiency.
In a U.S. study where ESTRING was compared with conjugated estrogens vaginal cream, no difference in efficacy between the treatment groups was found with respect to improvement in the physician's global assessment of vaginal symptoms (83 percent and 82 percent of patients receiving ESTRING and cream, respectively) and in the patient's global assessment of vaginal symptoms (83 percent and 82 percent of patients receiving ESTRING and cream, respectively) after 12 weeks of treatment. In an Australian study, ESTRING was also compared with conjugated estrogens vaginal cream and no difference in the physician's assessment of improvement of vaginal mucosal atrophy (79 percent and 75 percent for ESTRING and cream, respectively) or in the patient's assessment of improvement in vaginal dryness (82 percent and 76 percent for ESTRING and cream, respectively) after 12 weeks of treatment.
In the U.S. study, symptoms of dysuria and urinary urgency improved in 74 percent and 65 percent, respectively, of patients receiving ESTRING as assessed by the patient. In the Australian study, symptoms of dysuria and urinary urgency improved in 90 percent and 71 percent, respectively, of patients receiving ESTRING as assessed by the patient.
In both studies, ESTRING and conjugated estrogens vaginal cream had a similar ability to reduce vaginal pH levels and to mature the vaginal mucosa (as measured cytologically using the maturation index and/or the maturation value) after 12 weeks of treatment. In supportive studies, ESTRING was also shown to have a similar significant treatment effect on the maturation of the urethral mucosa.
Endometrial overstimulation, as evaluated in non-hysterectomized patients participating in the U.S. study by the progestogen challenge test and pelvic sonogram, was reported for none of the 58 (0 percent) patients receiving ESTRING and 4 of the 35 patients (11 percent) receiving conjugated estrogens vaginal cream.
Of the U.S. women who completed 12 weeks of treatment, 95 percent rated product comfort for ESTRING as excellent or very good compared with 65 percent of patients receiving conjugated estrogens vaginal cream, 95 percent of ESTRING patients judged the product to be very easy or easy to use compared with 88 percent of cream patients, and 82 percent gave ESTRING an overall rating of excellent or very good compared with 58 percent for the cream.
Women's Health Initiative Trial with Oral Conjugated Estrogen
The Women’s Health Initiative (WHI) estrogen-alone trial enrolled predominantly healthy postmenopausal women to assess the risks and benefits of daily oral conjugated estrogen (CE) (0.625 mg)-alone compared to placebo in the prevention of certain chronic diseases. The primary endpoint was the incidence of coronary heart disease (CHD) (defined as nonfatal MI, silent MI and CHD death), with invasive breast cancer as the primary adverse outcome. A “global index” included the earliest occurrence of CHD, invasive breast cancer, stroke, PE, colorectal cancer, hip fracture, or death due to other cause.
The WHI oral CE-alone trial included 10,739 women (average 63 years of age, range 50 to 79; 75 percent White, 15 percent Black, 6 percent Hispanic, 4 other races), with an average follow-up of 7.1 years. The WHI oral CE-alone trial was stopped early because an increased risk of stroke was observed in the oral CE group. The stroke events were centrally adjudicated. The use of oral CE-alone, compared to placebo, increased the risk for ischemic stroke, and this excess risk was present in all subgroups of women examined.1
No overall difference for centrally adjudicated primary CHD events (nonfatal MI, silent MI and CHD death) and invasive breast cancer incidence were seen in women who received oral CE-alone compared to those who received placebo after an average follow-up of 7.1 years.1,2
The results of the WHI oral CE-alone trial are presented in Table 2.
TABLE 2: Relative Risk and Risk Difference Observed in the WHI Estrogen-Alone Trial at an Average of 7.1 Years of Follow-up*,† Event Relative Ratio (95% CI)‡ Risk Difference
(CE vs placebo/10,000 WYs)- * Adapted from 2013 WHI trial (CE n=5,310, placebo n=5,429). WHI publications can be viewed at www.nhlbi.nih.gov/whi.
- † Results are based on centrally adjudicated data.
- ‡ In the WHI studies, hazard ratios were estimated using Cox proportional hazards models comparing treatment to placebo; however, they are described here as relative risks. Nominal confidence intervals unadjusted for multiple looks and multiple comparisons.
- § Not included in “global index.”
- ¶ Includes metastatic and non-metastatic breast cancer with the exception of in situ cancer.
- # All deaths, except from breast or colorectal cancer, definite or probable CHD, PE or cerebrovascular disease.
- Þ A subset of the events was combined in a “global index,” defined as the earliest occurrence of CHD events, invasive breast cancer, stroke, PE, colorectal cancer, hip fracture, or death due to other causes.
CHD events
Nonfatal MI
CHD death
0.94 (0.78-1.14)
0.97 (0.79-1.21)
1.00 (0.77-1.31)
-3 (55 vs 58)
-1 (44 vs 45)
0 (29 vs 29)
All strokes
1.35 (1.07-1.70)
11 (45 vs 34)
Deep vein thrombosis§
1.48 (1.06-2.07)
7 (23 vs 15)
Pulmonary embolism
1.35 (0.89-2.05)
4 (14 vs 10)
Invasive breast cancer¶
0.79 (0.61-1.02)
-7 (28 vs 35)
Colorectal cancer
1.15 (0.81-1.64)
2 (17 vs 15)
Hip fracture
0.67 (0.46-0.96)
-6 (13 vs 19)
Vertebral fractures§
0.64 (0.44-0.93)
-6 (12 vs 18)
Total fractures§
0.72 (0.64-0.80)
-61 (153 vs 214)
1.03 (0.88-1.21)
3 (80 vs 77)
Global indexÞ
1.03 (0.93-1.13)
4 (208 vs 204)
Women's Health Initiative Memory Study with Oral Conjugated Estrogen
The Women’s Health Initiative Memory Study (WHIMS) estrogen-alone ancillary study of the WHI trial enrolled 2,947 predominantly healthy hysterectomized postmenopausal women 65 to 79 years of age and older to evaluate the effects of daily oral CE (0.625 mg)-alone on the incidence of probable dementia (primary outcome) compared to placebo. In the WHIMS, 45% of the women were 65 to 69 years of age; 36% were 70 to 74 years of age; and 19% were 75 years of age and older. Probable dementia as defined in this study included Alzheimer’s disease (AD), vascular dementia (VaD) and mixed type of dementia (having features of both AD and VaD). The most common classification of probable dementia in the treatment and placebo groups was AD.
In the WHIMS, after an average follow-up of 5.2 years, the relative risk of probable dementia for women in the oral CE-alone group versus the placebo group was 1.49 (95% CI, 0.83-2.66). The absolute risk of probable dementia for oral CE-alone group versus the placebo group was 37 versus 25 cases per 10,000 women-years.
Because WHIMS was conducted in women 65 to 79 years of age, it is unknown whether the findings in WHIMS apply to younger postmenopausal women.3
- INDICATIONS AND USAGE
-
CONTRAINDICATIONS
ESTRING is contraindicated in women with any of the following conditions:
- 1. Abnormal genital bleeding with unknown etiology.
- 2. Known or suspected estrogen-dependent neoplasia.
- 3. Active DVT, PE, or a history of these conditions.
- 4. Active arterial thromboembolic disease (for example, stroke and MI), or a history of these conditions.
- 5. Known anaphylactic reaction or angioedema or hypersensitivity to ESTRING.
- 6. Known liver impairment or disease.
- 7. Protein C, protein S, or antithrombin deficiency, or other known thrombophilic disorders.
-
WARNINGS
1. Endometrial Cancer with Unopposed Estrogen in Women with a Uterus
In ESTRING-treated menopausal women with a uterus with persistent or recurring abnormal genital bleeding of unknown etiology, perform adequate diagnostic measures, including directed or random endometrial sampling when indicated, to assess for endometrial cancer.
There is an increased risk of endometrial cancer with the use of systemic estrogens alone in women with a uterus. The reported endometrial cancer risk among unopposed systemic estrogen users is about 2 to 12 times greater than in non-users and appears dependent on duration of treatment and on estrogen dose. Most studies show no significant increased risk associated with the use of systemically administered estrogens for less than one year. The greatest risk appears to be associated with prolonged use, with increased risks of 15- to 24-fold for 5 to 10 years or more. This risk has been shown to persist for at least 8 to 15 years after systemic estrogen therapy is discontinued. There is no evidence that the use of natural estrogens results in a different endometrial risk profile than synthetic estrogens of equivalent estrogen dose.
Adding a progestogen to estrogen-alone therapy has been shown to reduce the risk of endometrial hyperplasia (possible precursor to endometrial cancer). There is, however, a different risk profile associated with the use of progestogens plus estrogens compared to estrogen-alone regimens.
2. Risks Associated with Concomitant Use of Estrogen Plus Progestogen
If ESTRING is administered with a progestogen, there are possible risks associated with the concomitant use of estrogen with progestogen that differ from those of estrogen-alone regimens. Refer to the prescribing information for progestogens indicated for the prevention of endometrial hyperplasia in nonhysterectomized women receiving estrogens for a discussion of the risks of estrogen and progestogen concomitant therapy.
3. Risks with Systemic Estrogen-Alone Therapy
Systemic absorption occurs with the use of ESTRING, although the exposure is generally lower than that of systemic estrogens indicated for vasomotor symptoms. As such, the relevance or extent of the following risks of systemic estrogens to ESTRING is not known. The following adverse reactions have been reported with systemic estrogen therapy:
Cardiovascular diseases: The Women’s Health Initiative (WHI) estrogen-alone trial reported increased risks of pulmonary embolism (PE), deep vein thrombosis (DVT), and stroke, in postmenopausal women (50 to 79 years of age, average age 63.4 years) during 7.2 years of treatment with daily oral conjugated estrogens (CE) [0.625 mg] relative to placebo. (See CLINICAL STUDIES.)
Breast cancer: In the WHI estrogen-alone trial, after an average follow-up of 7.1 years, daily oral CE-alone was not associated with an increased risk of invasive breast cancer. (See CLINICAL STUDIES.) However, a large meta-analysis including 24 prospective studies of postmenopausal women comparing current use of estrogen-only products with use duration of 5 to 14 years (average of 9 years) versus never use reported a relative risk for breast cancer of 1.33 (95% CI, 1.28 to 1.38).
Ovarian cancer: A large meta-analysis including 17 prospective studies of postmenopausal women compared current use of estrogen-only products versus never user and reported a relative risk for ovarian cancer of 1.37 (95% CI 1.26, 1.50). The duration of hormone therapy use that was associated with an increased risk of ovarian cancer is unknown.4
Others: gallbladder disease requiring surgery, severe hypercalcemia in women with breast cancer and metastases, retinal vascular thrombosis, substantial increases in blood pressure from idiosyncratic reactions, exacerbation of hypertriglyceridemia leading to pancreatitis, cholestatic jaundice, exacerbation of hypothyroidism, fluid retention, hypocalcemia, exacerbation of conditions including hereditary angioedema, asthma, diabetes mellitus, epilepsy, migraine, porphyria, systemic lupus erythematosus, and hepatic hemangiomas.
-
PRECAUTIONS
A. General
1. Location of ESTRING
Some women have experienced moving or gliding of ESTRING within the vagina. Instances of ESTRING being expelled from the vagina in connection with moving the bowels, strain, or constipation have been reported. If this occurs, ESTRING can be rinsed in lukewarm water and reinserted into the vagina by the patient.
2. Vaginal Irritation
ESTRING may not be suitable for women with narrow, short, or stenosed vaginas. Narrow vagina, vaginal stenosis, prolapse, and vaginal infections are conditions that make the vagina more susceptible to ESTRING-caused irritation or ulceration. Women with signs or symptoms of vaginal irritation should alert their physician.
3. Vaginal Infection
Vaginal infection is generally more common in postmenopausal women due to the lack of the normal flora of fertile women, especially lactobacillus, and the subsequent higher pH. Vaginal infections should be treated with appropriate antimicrobial therapy before initiation of ESTRING. If a vaginal infection develops during use of ESTRING, then ESTRING should be removed and reinserted only after the infection has been appropriately treated.
B. Patient Information
Physicians are advised to discuss the PATIENT INFORMATION leaflet with women for whom they prescribe ESTRING.
C. Laboratory Tests
Serum FSH and estradiol levels have not been shown to be useful in the management of moderate to severe symptoms of vulvar and vaginal atrophy.
D. Drug and Laboratory Test Interactions
- 1. Accelerated prothrombin time, partial thromboplastin time, and platelet aggregation time; increased platelet count; increased factors II, VII antigen, VIII antigen, VIII coagulant activity, IX, X, XII, VII-X complex, II-VII-X complex, and beta-thromboglobulin; decreased levels of anti-factor Xa and antithrombin III, decreased antithrombin III activity; increased levels of fibrinogen and fibrinogen activity; increased plasminogen antigen and activity.
- 2. Increased thyroid-binding globulin (TBG) levels leading to increased circulating total thyroid hormone levels, as measured by protein-bound iodine (PBI), T4 levels (by column or by radioimmunoassay) or T3 levels by radioimmunoassay. T3 resin uptake is decreased, reflecting the elevated TBG. Free T4 and free T3 concentrations are unaltered. Women on thyroid replacement therapy may require higher doses of thyroid hormone.
- 3. Other binding proteins may be elevated in serum, (i.e., corticosteroid binding globulin [CBG], sex hormone-binding globulin [SHBG]), leading to increased circulating corticosteroid and sex steroids, respectively. Free hormone concentrations, such as testosterone and estradiol, may be decreased. Other plasma proteins may be increased (angiotensinogen/renin substrate, alpha-1-antitrypsin, ceruloplasmin).
- 4. Increased plasma high-density (HDL) and HDL2 cholesterol subfraction concentrations, reduced low-density (LDL) cholesterol concentration, increased triglycerides levels.
- 5. Impaired glucose tolerance.
E. Carcinogenesis, Mutagenesis, and Impairment of Fertility
Long-term, continuous administration of natural and synthetic estrogens in certain animal species increases the frequency of carcinomas of the breast, uterus, cervix, vagina, testes and liver.
F. Pregnancy
ESTRING should not be used during pregnancy.
There appears to be little or no increased risk of birth defects in children born to women who have used estrogens as an oral contraceptive inadvertently during early pregnancy.
G. Nursing Mothers
ESTRING should not be used during lactation. Estrogen administration to nursing women has been shown to decrease the quantity and quality of the breast milk. Detectable amounts of estrogens have been identified in the breast milk of mothers receiving estrogens. Caution should be exercised when ESTRING is administered to a nursing woman.
H. Pediatric Use
ESTRING is not indicated in children. Clinical studies have not been conducted in the pediatric population.
I. Geriatric Use
There have not been sufficient numbers of geriatric patients involved in studies utilizing ESTRING to determine whether those over 65 years of age differ from younger subjects in their response to ESTRING.
The Women's Health Initiative Study
In the WHI estrogen-alone substudy (daily CE [0.625 mg]-alone versus placebo), there was a higher relative risk of stroke in women greater than 65 years of age. (See CLINICAL STUDIES.)
The Women's Health Initiative Memory Study
In the WHIMS ancillary studies of postmenopausal women 65 to 79 years of age, there was an increased risk of developing probable dementia in women who received oral CE-alone compared to those who received placebo. (See CLINICAL STUDIES.)
Since trial was conducted in women 65 to 79 years of age, it is unknown whether these findings apply to younger postmenopausal women. (See CLINICAL STUDIES.)
-
ADVERSE REACTIONS
See WARNINGS and PRECAUTIONS
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
In the two ESTRING controlled studies, discontinuation of treatment due to an adverse event was required by 5.4 percent of patients receiving ESTRING and 3.9 percent of patients receiving conjugated estrogens vaginal cream. The most common reasons for withdrawal from ESTRING treatment due to an adverse event were vaginal discomfort and gastrointestinal symptoms.
The adverse events reported with a frequency of 3 percent or greater in the two pivotal controlled studies by patients receiving ESTRING or conjugated estrogens vaginal cream are listed in Table 3.
TABLE 3: Adverse Events Reported by 3 Percent or More of Patients Receiving Either ESTRING or Conjugated Estrogens Vaginal Cream in Two Pivotal Controlled Studies ADVERSE EVENT ESTRING
(n = 257)
%Conjugated Estrogens Vaginal Cream
(n = 129)
%Musculoskeletal
Back Pain
6
8
Arthritis
4
2
Arthralgia
3
5
Skeletal Pain
2
4
CNS/Peripheral Nervous System
Headache
13
16
Psychiatric
Insomnia
4
0
Gastrointestinal
Abdominal Pain
4
2
Nausea
3
2
Respiratory
Upper Respiratory Tract Infection
5
6
Sinusitis
4
3
Pharyngitis
1
3
Urinary
Urinary Tract Infection
2
7
Female Reproductive
Leukorrhea
7
3
Vaginitis
5
2
Vaginal Discomfort/Pain
5
5
Vaginal Hemorrhage
4
5
Asymptomatic Genital Bacterial Growth
4
6
Breast Pain
1
7
Resistance Mechanisms
Genital Moniliasis
6
7
Body as a Whole
Flu-Like Symptoms
3
2
Hot Flushes
2
3
Allergy
1
4
Miscellaneous
Family Stress
2
3
Postmarketing Experience
Cases of toxic shock syndrome (TSS) have been reported in women using vaginal rings. TSS is a rare, but serious disease that may cause death. Warning signs of TSS include fever, nausea, vomiting, diarrhea, muscle pain, dizziness, faintness, or a sunburn-rash on face and body.
Vaginal erosion, vaginal ulceration, adherence of the vaginal ring to the vaginal wall:
- Cases of ring adherence to the vaginal wall, making ring removal difficult, have occurred. Some cases have required surgical removal of vaginal rings.
- Cases of vaginal erosion and vaginal ulceration that may manifest as vaginal irritation, erythema. abrasion or spotting have occurred.
Vaginal wall ulceration or erosion should be carefully evaluated. If an ulceration or erosion has occurred, consideration should be given to leaving the ring out and not replacing it until healing is complete in order to prevent the ring from adhering to the healing tissue.
Cases of bowel obstruction and vaginal ring use have been reported. Persistent abdominal complaints consistent with obstruction should be carefully evaluated.
Cases of hypersensitivity have been reported.
The following additional adverse events were reported at least once by patients receiving ESTRING in the worldwide clinical program, which includes controlled and uncontrolled studies. A causal relationship with ESTRING has not been established.
Body as a Whole: allergic reaction
CNS/Peripheral Nervous System: dizziness
Gastrointestinal: enlarged abdomen, vomiting
Metabolic/Nutritional Disorders: weight decrease or increase
Musculoskeletal: arthropathy (including arthrosis)
Psychiatric: depression, decreased libido, nervousness
Reproductive: breast engorgement, breast enlargement, intermenstrual bleeding, genital edema, vulval disorder
Skin/Appendages: pruritus, pruritus ani
Urinary: micturition frequency, urethral disorder
Vascular: thrombophlebitis
Vision: abnormal vision
- OVERDOSAGE
-
DOSAGE AND ADMINISTRATION
One ESTRING (estradiol vaginal system) is to be inserted as deeply as possible into the upper one-third of the vaginal vault. The ring is to remain in place continuously for three months, after which it is to be removed and, if appropriate, replaced by a new ring.
Should the ring be removed or fall out at any time during the 90-day treatment period, the ring should be rinsed in lukewarm water and re-inserted by the patient, or, if necessary, by a physician or nurse.
Retention of the ring for greater than 90 days does not represent overdosage but will result in progressively greater underdosage with the attendant risk of loss of efficacy and increasing risk of vaginal infections and/or erosions.
Instructions for Use
ESTRING (estradiol vaginal system) insertion
The ring should be pressed into an oval and inserted into the upper third of the vaginal vault. The exact position is not critical. When ESTRING is in place, the patient should not feel anything. If the patient feels discomfort, ESTRING is probably not far enough inside. Gently push ESTRING further into the vagina.
ESTRING use
ESTRING should be left in place continuously for 90 days and then, if continuation of therapy is deemed appropriate, replaced by a new ESTRING.
The patient should not feel ESTRING when it is in place and it should not interfere with sexual intercourse. Straining at defecation may make ESTRING move down in the lower part of the vagina. If so, it may be pushed up again with a finger.
If ESTRING is expelled totally from the vagina, it should be rinsed in lukewarm water and reinserted by the patient (or doctor/nurse if necessary).
ESTRING removal
ESTRING may be removed by hooking a finger through the ring and pulling it out.
For patient instructions, see Patient Information.
-
HOW SUPPLIED
Each ESTRING (estradiol vaginal system) contains 2 mg estradiol to deliver 7.5 mcg of estradiol per day over 90 days, and is individually packaged in a heat-sealed rectangular pouch consisting of three layers, from outside to inside: polyester, aluminum foil, and low-density polyethylene, respectively. The pouch is provided with a tear-off notch on one side.
NDC: 0013-1042-01 ESTRING (estradiol vaginal system) delivers 7.5 mcg per day – one vaginal system (contains 2 mg estradiol to deliver 7.5 mcg of estradiol per day over 90 days).
-
REFERENCES
- 1. Manson, J. E., et al Menopausal hormone therapy and health outcomes during the intervention and extended poststopping phases of the Women's Health Initiative randomized trials. JAMA, 310(13): 1353–1368 (2013). https://doi.org/10.1001/jama.2013.278040.
- 2. Anderson GL, et al; Women's Health Initiative Steering Committee. Effects of conjugated equine estrogen in postmenopausal women with hysterectomy: the Women's Health Initiative randomized controlled trial. JAMA. 2004 Apr 14;291(14):1701-12. doi: 10.1001/jama.291.14.1701. PMID: 15082697.
- 3. Espeland MA, Rapp SR, Shumaker SA, Brunner R, Manson JE, Sherwin BB, Hsia J, Margolis KL, Hogan PE, Wallace R, Dailey M, Freeman R, Hays J; Women's Health Initiative Memory Study. Conjugated equine estrogens and global cognitive function in postmenopausal women: Women's Health Initiative Memory Study. JAMA. 2004 Jun 23;291(24):2959-68. doi: 10.1001/jama.291.24.2959. PMID: 15213207.
- 4. Collaborative Group on Epidemiological Studies of Ovarian Cancer; Beral V, Gaitskell K, Hermon C, Moser K, Reeves G, Peto R. Menopausal hormone use and ovarian cancer risk: individual participant meta-analysis of 52 epidemiological studies. Lancet. 2015 May 9;385(9980):1835-42. doi: 10.1016/S0140-6736(14)61687-1. Epub 2015 Feb 13. PMID: 25684585; PMCID: PMC4427760.
- SPL UNCLASSIFIED SECTION
-
PATIENT INFORMATION
ESTRING
(estradiol vaginal system)Read this Patient Information before you start using ESTRING and each time you get a refill. There may be new information. This information does not take the place of talking to your healthcare provider about your menopausal symptoms or your treatment.
What is ESTRING?
ESTRING (estradiol vaginal system) is an off-white, soft, flexible ring with a center that contains 2 mg of estradiol (an estrogen hormone). ESTRING releases estradiol into the vagina in a consistent, stable manner for 90 days. The soft, flexible ring is placed in the upper third of the vagina (by the physician or the patient). ESTRING should be removed after 90 days of continuous use. If continuation of therapy is indicated, the flexible ring should be replaced.
What is ESTRING used for?
ESTRING is used after menopause to treat moderate to severe menopausal changes in and around the vagina.
You and your healthcare provider should talk regularly about whether you still need treatment with ESTRING to control these problems.
Who should not use ESTRING?
Do not start using ESTRING if you:
- have unusual vaginal bleeding
- Vaginal bleeding after menopause may be a warning sign of cancer of the uterus (womb). Your healthcare provider should check any unusual vaginal bleeding to find out the cause.
- currently have or have had certain cancers
- Estrogens may increase the chance of getting certain types of cancers. If you have or had an estrogen-dependent cancer, talk with your healthcare provider about whether you should use ESTRING.
- had a stroke or heart attack
- currently have or have had blood clots
- currently have liver problems
- have been diagnosed with a bleeding disorder
- are allergic to ESTRING or any of its ingredients
- See the list of ingredients in ESTRING at the end of this leaflet.
- think you may be pregnant
- ESTRING is not for pregnant women. If you think you may be pregnant, you should have a pregnancy test and know the results. Do not use ESTRING if the test is positive and talk to your healthcare provider.
What should I tell my healthcare provider before I use ESTRING?
Before you use ESTRING, tell your healthcare provider if you:- have any unusual vaginal bleeding
- Vaginal bleeding after menopause may be a warning sign of cancer of the uterus (womb). Your healthcare provider should check any unusual vaginal bleeding to find out the cause.
- have any other medical conditions
- Your healthcare provider may need to check you more carefully if you have certain conditions, such as asthma (wheezing), epilepsy (seizures), diabetes, migraine, endometriosis, lupus, angioedema (swelling of face and tongue), or problems with your heart, liver, thyroid, kidneys, or have high calcium levels in your blood.
- are going to have surgery or will be on bed rest
- Your healthcare provider will let you know if you need to stop using ESTRING.
- are breast feeding
- The hormone in ESTRING can pass into your breast milk.
Tell your healthcare provider about all the medicines you take including prescription and nonprescription medicines, vitamins, and herbal supplements. Some medicines may affect how ESTRING works. ESTRING may also affect how your other medicines work.
What are the possible side effects of ESTRING?
If you experience any of the following side-effects, immediately remove ESTRING if possible and contact your healthcare provider. If you experience difficulty or pain when trying to remove the ring please do not continue and contact your healthcare provider:
- Cases of toxic shock syndrome (TSS) have been reported in women using vaginal rings. Toxic shock syndrome is a rare but serious illness caused by a bacterial infection. Symptoms of TSS include fever, nausea, vomiting, diarrhea, muscle pain, dizziness, faintness, or a sunburn-like rash on face and body.
- Cases of the vaginal ring becoming attached to the vaginal wall, making ring removal difficult, have occurred. Some women have needed surgery to remove vaginal rings.
- Cases of erosion (wearing away) and ulceration (holes) of the vaginal lining have also occurred. Symptoms of vaginal erosion and ulceration can include vaginal pain or soreness, vaginal bleeding, and redness, swelling, or scrapes in the vagina.
- Cases of bowel obstruction have been reported.
- Severe allergic reactions have been reported including skin rash, giant hives, swelling of the eyelids, face, lips, tongue or throat.
The most frequently reported side effect with ESTRING use is increased vaginal secretions. Many of these vaginal secretions are like those that occur normally prior to menopause and indicate that ESTRING is working. Vaginal secretions that are associated with a bad odor, vaginal itching, or other signs of vaginal infection are NOT normal and may indicate a risk or a cause for concern. Other side effects may include vaginal discomfort, abdominal pain, or genital itching.
What are the possible side effects of estrogens?
Side effects are grouped by how serious they are and how often they happen when you are treated.
Serious, but less common side effects include:
- heart attack
- stroke
- blood clots
- dementia
- breast cancer
- cancer of the lining of the uterus (womb)
- cancer of the ovary
- high blood pressure
- high blood sugar
- gallbladder disease
- liver problems
- changes in your thyroid hormone levels
- enlargement of benign tumors of the uterus ("fibroids")
Call your healthcare provider right away if you get any of the following warning signs or any other unusual symptoms that concern you:
- new breast lumps
- unusual vaginal bleeding
- changes in vision or speech
- sudden new severe headaches
- severe pains in your chest or legs with or without shortness of breath, weakness and fatigue
- memory loss or confusion
Less serious, but common side effects include:
- headache
- breast pain
- irregular vaginal bleeding or spotting
- stomach or abdominal cramps, bloating
- nausea and vomiting
- fluid retention
- vaginal yeast infection
These are not all the possible side effects of ESTRING. For more information, ask your healthcare provider or pharmacist for advice about side effects. Tell your healthcare provider if you have any side effect that bothers you or does not go away.
Call your healthcare provider for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. You may report side effects to Pfizer at 1-800-438-1985.
What can I do to lower my chances of getting a serious side effect with ESTRING?
- Follow carefully the instructions for use.
- Talk with your healthcare provider regularly about whether you should continue using ESTRING.
- See your healthcare provider right away if you get vaginal bleeding while using ESTRING.
- If you have fever, nausea, vomiting, diarrhea, muscle pain, dizziness, faintness, or a sunburn-like rash on face and body, remove ESTRING and contact your healthcare provider.
- Contact your healthcare provider if you have difficulty removing the vaginal ring.
- Have a breast exam and mammogram (breast X-ray) every year unless your healthcare provider tells you something else. If members of your family have had breast cancer or if you have ever had breast lumps or an abnormal mammogram, you may need to have breast examinations more often.
- If you have high blood pressure, high cholesterol (fat in the blood), diabetes, are overweight, or if you use tobacco, you may have higher chances for getting heart disease. Ask your healthcare provider for ways to lower your chances for getting heart disease.
General information about safe and effective use of ESTRING
Medicines are sometimes prescribed for conditions that are not mentioned in patient information leaflets. Do not use ESTRING for conditions for which it was not prescribed. Do not give ESTRING to other people, even if they have the same symptoms you have. It may harm them.
Keep ESTRING out of the reach of children.
This leaflet provides a summary of the most important information about ESTRING. If you would like more information, talk with your healthcare provider or pharmacist. You can ask for information about ESTRING that is written for health professionals. You can get more information by calling the toll free number 1-888-691-6813.
What are the ingredients in ESTRING?
ESTRING (estradiol vaginal system) is a slightly opaque ring with a whitish core containing a drug reservoir of 2 mg estradiol (an estrogen hormone). Estradiol, silicone polymers, barium sulfate and silicone fluid (as dispersing agent) are combined to form the ring.
Storage: Store at controlled room temperature 15° to 25 °C (59 °F to 77 °F).
-
INSTRUCTIONS FOR USE:
How should I use ESTRING?
ESTRING is a local estrogen therapy used after menopause to treat moderate to severe menopausal changes in and around the vagina. ESTRING PROVIDES RELIEF OF LOCAL SYMPTOMS OF MENOPAUSE ONLY.
Estrogens should be used only as long as needed. You and your healthcare provider should talk regularly (for example, every 3 to 6 months) about whether you still need treatment with ESTRING.
ESTRING INSERTION
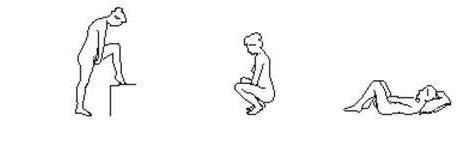
ESTRING can be inserted and removed by you or your doctor or healthcare provider. To insert ESTRING yourself, choose the position that is most comfortable for you: standing with one leg up, squatting, or lying down.
- 1. After washing and drying your hands, remove ESTRING from its pouch using the tear-off notch on the side. (Since the ring becomes slippery when wet, be sure your hands are dry before handling it.)
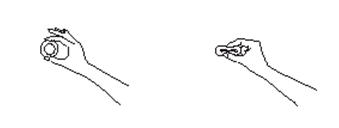
- 2. Hold ESTRING between your thumb and index finger and press the opposite sides of the ring together as shown.
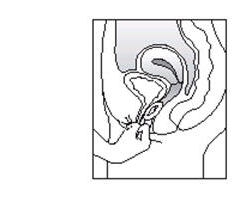
- 3. Gently push the compressed ring into your vagina as far as you can.
ESTRING PLACEMENT
The exact position of ESTRING is not critical, as long as it is placed in the upper third of the vagina.
When ESTRING is in place, you should not feel anything. If you feel uncomfortable, ESTRING is probably not far enough inside. Use your finger to gently push ESTRING further into your vagina.
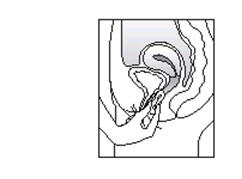
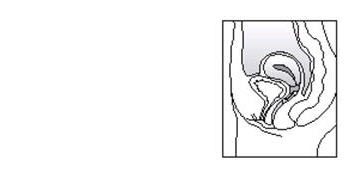
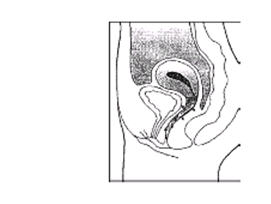
There is no danger of ESTRING being pushed too far up in the vagina or getting lost. ESTRING can only be inserted as far as the end of the vagina, where the cervix (the narrow, lower end of the uterus) will block ESTRING from going any further (See diagram of Female Anatomy).
ESTRING USE
Once inserted, ESTRING should remain in place in the vagina for 90 days.
Most women and their partners experience no discomfort with ESTRING in place during intercourse, so it is NOT necessary that the ring be removed. If ESTRING should cause you or your partner any discomfort, you may remove it prior to intercourse (See ESTRING Removal, below). Be sure to reinsert ESTRING as soon as possible afterwards.
ESTRING may slide down into the lower part of the vagina as a result of the abdominal pressure or straining that sometimes accompanies constipation. If this should happen, gently guide ESTRING back into place with your finger.
There have been rare reports of ESTRING falling out in some women following intense straining or coughing. If this should occur, simply wash ESTRING with lukewarm (NOT hot) water and reinsert it.
ESTRING DRUG DELIVERY
Once in the vagina, ESTRING begins to release estradiol immediately. ESTRING will continue to release a low, continuous dose of estradiol for the full 90 days it remains in place.
It will take about 2 to 3 weeks to restore the tissue of the vagina and urinary tract to a healthier condition and to feel the full effect of ESTRING in relieving vaginal and urinary symptoms. If your symptoms persist for more than a few weeks after beginning ESTRING therapy, contact your doctor or healthcare provider.
One of the most frequently reported effects associated with the use of ESTRING is an increase in vaginal secretions. These secretions are like those that occur normally prior to menopause and indicate that ESTRING is working. However, if the secretions are associated with a bad odor or vaginal itching or discomfort, be sure to contact your doctor or healthcare provider.
ESTRING REMOVAL
After 90 days there will no longer be enough estradiol in the ring to maintain its full effect in relieving your vaginal or urinary symptoms. ESTRING should be removed at that time and replaced with a new ESTRING, if your doctor determines that you need to continue your therapy.
To remove ESTRING:
- 1. Wash and dry your hands thoroughly.
- 2. Assume a comfortable position, either standing with one leg up, squatting, or lying down.
- 3. Loop your finger through the ring and gently pull it out.
- 4. Discard the used ring in a waste receptacle. (Do not flush ESTRING.)
If you have any additional questions about removing ESTRING, contact your doctor or healthcare provider.
LAB-1533-4.0
Revised 4/2026 -
PRINCIPAL DISPLAY PANEL - 2 mg Pouch Label
NDC: 0013-1042-01
Rx onlyEstring®
(estradiol vaginal system)
delivers 7.5 mcg per dayContains one vaginal system
Store at controlled room temperature
15 ºC to 25 ºC (59 ºF to 77 ºF).
DOSAGE AND USE: See accompanying
prescribing information. Package Not Child-Resistant.
Keep out of reach of children.Contains 2 mg estradiol, USP, to deliver 7.5 mcg of
estradiol per day over 90 days.61 31 11
Pfizer
Distributed by Pharmacia & Upjohn Company LLC
A subsidiary of Pfizer Inc., New York, NY 10001
LOT
EXP -
PRINCIPAL DISPLAY PANEL - 2 mg Pouch Carton
NDC: 0013-1042-01
Pfizer
Estring®
(estradiol vaginal system)
delivers 7.5 mcg per dayContains one vaginal system
Rx only
-
INGREDIENTS AND APPEARANCE
ESTRING
estradiol systemProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC: 0013-1042 Route of Administration VAGINAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength ESTRADIOL (UNII: 4TI98Z838E) (ESTRADIOL - UNII:4TI98Z838E) ESTRADIOL 2 mg Inactive Ingredients Ingredient Name Strength BARIUM SULFATE (UNII: 25BB7EKE2E) Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC: 0013-1042-01 1 in 1 CARTON 06/05/2023 1 1 in 1 POUCH; Type 4: Device Coated/Impregnated/Otherwise Combined with Drug Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date NDA NDA020472 06/05/2023 Labeler - Pfizer Laboratories Div Pfizer Inc (134489525) Registrant - Pfizer Inc (113480771)
Trademark Results [Estring]
Mark Image Registration | Serial | Company Trademark Application Date |
|---|---|
 ESTRING 74496606 2086164 Live/Registered |
PFIZER HEALTH AB 1994-03-03 |
 ESTRING 74198624 not registered Dead/Abandoned |
Kabi Pharmacia AB 1991-08-27 |
© 2026 FDA.report
This site is not affiliated with or endorsed by the FDA.